Peripheral Arterial Disease Critical Limb Ischemia Pedal Approach

Peripheral Arterial Disease & Critical Limb Ischemia Pedal Approach to Infratibial Occlusion Nelson Lim Bernardo, MD Director, Peripheral Vascular Laboratory Medstar Heart Institute at Washington Hospital Center Washington, D. C.

Nelson L. Bernardo, MD Honoraria: Abbott Vascular Cook Group Incorporated Cordis Corporation Covidien Medtronic, Inc. Terumo Cardiovascular Systems Group

Faculty Disclosure • Abbott Vascular – Training Site • Cook Medical – Training Site • Cordis Endovascular – Training Site • Covidien/e. V 3 – Training Site • Medtronic – Training Site • No conflict of interest related to this presentation • Non-IFU use of devices will be discussed

Endovascular Intervention in 2013: • Percutaneous Endovascular Intervention of below -the-knee (BTK) arterial occlusive disease, especially in critical limb ischemia (CLI), has been gaining a lot of ground Ø Ø Growing patient population – patients with diabetes mellitus, awareness Utility/success of PEI in limb salvage and/or limb preservation

PEI of BTK Occlusions: • Approximately 15 -20% of patients with complex tibio-peroneal arterial occlusive disease cannot be crossed with an antegrade approach using vascular access from the common femoral artery • Retrograde pedal artery access is an alternative to allow successful ‘crossing’ of the lesion and eventual recanalization

Retrograde Pedal Approach: Advantages • Patient is supine (comfort) • High success rate of crossing CTOs Ø ‘Distal’ cap of occlusion may be ‘softer’ • Can work from above and below to cross lesions and deliver therapy • Less access site bleeding (good hemostasis)

Retrograde Pedal Approach: Disadvantages • Access of pedal artery is more difficult Ø Requires training, i. e. ‘learning curve’ Ø Experience • Small vessel caliber Ø Avoid injury of vessel Ø Small sized sheath (3 F) or ‘bare-back’ delivery of catheters/devices – limits the device/catheters that can be delivered

Retrograde BTK - Pedal Artery Access: 1. Anterior tibial artery Ø Dorsalis pedis artery (distal anterior tibial A) Ø Proximal anterior tibial artery 2. Posterior tibial artery Ø Distal (proximal segment of plantar vessels) Ø Mid segment of the vessel 3. Distal peroneal artery (+/- through interosseous ligament)

Vasculature of the L. E. : Arterial System Venous System

Retrograde BTK - Pedal Artery Access: • Techniques - ‘Imaging’ guidance for Pedal Artery Access: Ø Surgical Ø X-ray - ‘Open’ cutdown Fluoroscopy - Angiography, Roadmapping Ø Duplex Ultrasound guidance

Retrograde Pedal Access: Surgical • ‘Open’ surgical cutdown Ø Cutdown - direct visualization of the artery Ø Direct puncture of the artery, i. e. dorsalis pedis artery Right Foot • Cons: Ø Surgical incision site to manage Ø ? ? hemostasis

Retrograde Pedal Access: Fluoro guidance • X-ray Fluoroscopy guidance Ø Angiography +/- ‘road-map’ Ø Vessel wall calcification Peroneal • Cons: Ø The artery is entered ‘blindly’ Ø Radiation, + Contrast agent DP Needle

Retrograde Pedal Access: Ultrasound guidance • In the lower extremity, each artery is accompanied by corresponding two (2) veins - Use ultrasound and doppler to dileneate • Imaging views for needle ‘entry’ Ø Transverse (Short axis) Ø Longitudinal (Long axis)

Retrograde Pedal Access: Ultrasound guidance • In the lower extremity, each artery is accompanied by corresponding two (2) veins - Use ultrasound and doppler to dileneate • Imaging views for needle ‘entry’ Ø Transverse (Short axis) Ø Longitudinal (Long axis)

Retrograde Pedal Access: Foot Positioning ‘Frog-leg’ position + Dorsiflexion Plantar Flexion Dorsalis pedis, distal AT artery ‘Frog-leg’ position PT artery, Peroneal artery PT artery

Retrograde Pedal Access: Posterior Tibial A. Artery Vein

Retrograde PT Artery Access: Technique Confirmed arterial doppler-flow signal

Retrograde PT Artery Access: Technique Application of local anesthesia Confirmed arterial doppler-flow signal Insertion of micropuncture needle

Retrograde PT Artery Access: Technique Look for “Tenting” of the vessel wall • Needle approaching Posterior Tibial Artery

Retrograde PT Artery Access: Technique • Needle entering Posterior Tibial Artery • Blood return micropuncture needle
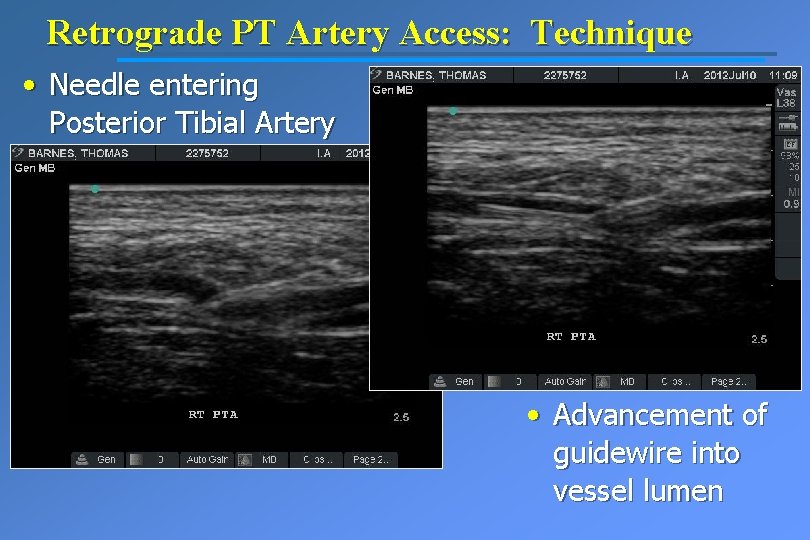
Retrograde PT Artery Access: Technique • Needle entering Posterior Tibial Artery • Advancement of guidewire into vessel lumen

Retrograde Pedal Artery Access: • Access with the first puncture Ø to prevent spasm Ø to avoid vascular injury • Adequate anti-coagulation (i. e. Heparin) • “Anti-spasm” cocktail Ø Nitroglycerin Ø Ca++ channel blocker – Verapamil, Nicardipine

Retrograde DP Access: Sheath Mgt 21 G Micropuncture needle in right DP artery 4 F Micropuncture sheath + Tuohy-Borst/Co-pilot in right DP artery

Retrograde Pedal Access: Access Site Mgt • Management of Access Site-Sheath Options: 1) ‘Bare-back’ over guidewire with balloon catheter or support catheter v Vessel wall trauma with repeated entry

Retrograde Pedal Access: Access Site Mgt • Management of Access Site-Sheath Options: 1) ‘Bare-back’ over guidewire with balloon catheter or support catheter v Vessel wall trauma with repeated entry 2) Use of the Micropuncture introducer sheath v No need to exchange out; attach Tuohy. Borst/Copilot control valve v Inner diameter = 2. 9 F (can accommodate the entire length of Cook CXI 0. 018” support catheter)

Retrograde Pedal Access: Access Site Mgt • Management of Access Site-Sheath Options: 1) ‘Bare-back’ over guidewire with balloon catheter or support catheter v Vessel wall trauma with repeated entry 2) Use of the Micropuncture introducer sheath v No need to exchange out; attach Tuohy. Borst/Copilot control valve v Inner diameter = 2. 9 F (can accommodate the entire length of Cook CXI 0. 018” support catheter)

Retrograde Pedal Access: Access Site Mgt • Management of Access Site-Sheath Options: 1) ‘Bare-back’ over guidewire with balloon catheter or support catheter v Vessel wall trauma with repeated entry 2) Use of the Micropuncture introducer sheath v No need to exchange out; attach Tuohy. Borst/Copilot control valve v Inner diameter = 2. 9 F (can accommodate the entire length of Cook CXI 0. 018” support catheter) 3) ‘Dedicated’ 3 F pedal access sheath

Retrograde Pedal Artery Access: Hemostasis • Manual compression (external) Ø ? ? compromise distal outflow

Retrograde Pedal Artery Access: Hemostasis • Manual compression (external) Ø ? ? compromise distal outflow • Mechanical compression (external) Ø Use of blood pressure cuff Ø Use of TR-band – Over left distal PT artery access site

Retrograde Pedal Access: Hemostasis • Balloon occlusion (internal) 2. 0 -mm diameter Balloon catheter Balloon inflation x 5 minutes

Retrograde Pedal Access: Hemostasis • Balloon occlusion (internal) 2. 0 -mm diameter Balloon catheter Balloon inflation x 5 minutes

KL: Successful CLI revascularization Good hemostasis Post: 2 -vessel run-off

Montero-Baker, M. , et. al. J Endovasc Ther 2008; 15: 594 -604. Retrograde Approach for Pop/TP Occlusions • Single Center Registry Ø September 2006 to December 2007 Ø 62/343 limbs (17. 8%) failed antegrade revascularization 51 limbs retrograde recanalization 45/51 (88. 2%) – pedal access 6/51 (11. 8%) – trans-collateral Ø Overall success = 86. 3% (44/51)

Montero-Baker, M. , et. al. J Endovasc Ther 2008; 15: 594 -604. Retrograde Approach for Pop/TP Occlusions • Complications: Ø Major 1 (1. 9%) - pedal access site occlusion (DP) Ø Minor (without clinical consequence) 3 (5. 9%) - arterial perforation 1 (1. 9%) - pedal hematoma

Pedal Approach to Infratibial Occlusions • In the percutaneous endovascular treatment of below-the-knee (BTK) arterial occlusive disease, the technique of retrograde pedal artery access is essential in an interventionalist’s armamentarium. • Pedal access has definitely changed the playing field in the approach & has improved the treatment of BTK arterial occlusive disease.

Peripheral Arterial Disease & Critical Limb Ischemia Thank You
- Slides: 36