Perioperative seizures Dr S Parthasarathy MD DA DNB

Perioperative seizures Dr. S. Parthasarathy MD. , DA. , DNB, MD (Acu), Dip. Diab. DCA, Dip. Software statistics- Phd Mahatma Gandhi Medical college and research institute , puducherry , India

Definition • A seizure can be defined as the clinical manifestation of an abnormal and excessive discharge of neurones, seen as alteration of consciousness, motor, sensory or autonomic events. • Epilepsy is defined as recurrent (two or more) epileptic seizures unprovoked by any immediately identifiable cause. • Epilepsy includes seizures but seizures ? ?

Incidence • Only epilepsy – incidence • 0. 5 – 1 % • But peri operative seizures – incidence ? ? • EEG monitoring in potential patients ? ? • It can also miss ? ?

Classification • General • Partial • Unclassified

Causes • • • Epilepsy Tumours Infections Metabolic Alcohol Stroke • Its Same

Differential diagnosis • • Syncope Migraine Narcolepsy Non epileptic seizures

Investigations • • EEG CT scan MRI PET scan

How does it relate to us ? ? • Sudden seizures – periop • Epilepsy – anaesthetic considerations • ICU status epilepticus
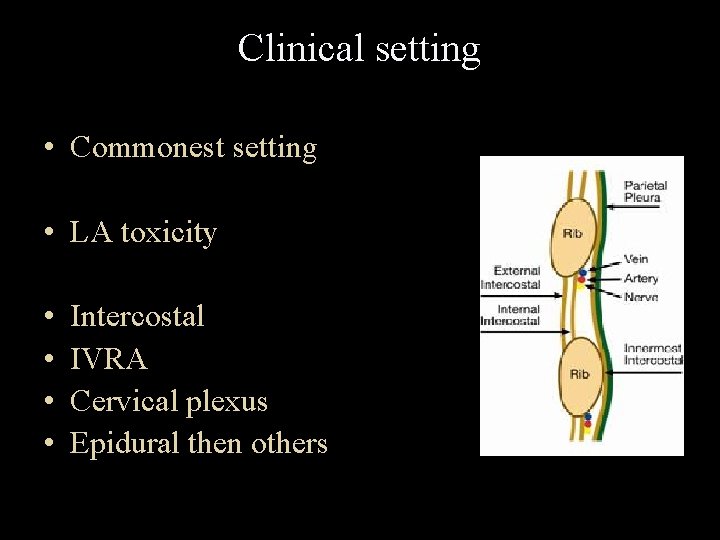
Clinical setting • Commonest setting • LA toxicity • • Intercostal IVRA Cervical plexus Epidural then others

Test dose • There may be premonitory symptoms, such as peri oral tingling, or feelings of dissociation following a test dose. • Epinephrine ? ? • Catheter malfunction • Catheter position change • Axillary ? ? • Field blocks

Maximum dose for infiltration (mg/kg) • • Lidocaine 3 - 4 With adrenaline 7 Bupivicaine 2 With adrenaline 3 Prilocaine 6 With adrenaline/octapressin 8 Additive

Basic treatment • • Airway Oxygen Ventilate Support • Other than benzodiazepines
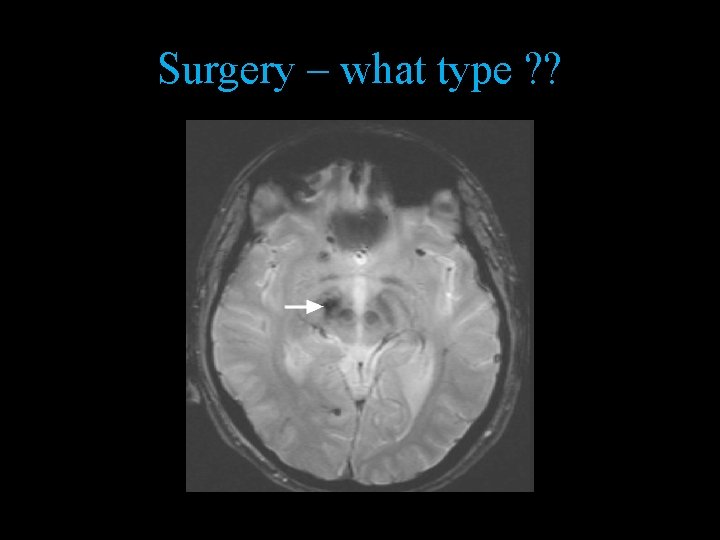
Surgery – what type ? ?
What Type of Surgery Places the Patient at Risk for Seizures? • Neuro surgery 20 % • • Leave alone head injury Supratentorial tumors Cerebral abscess 90 % Drainage 15 – 20 % • Preop seizure history -- incidence is very much higher

CAROTID AND CARDIAC SURGERY • Clamping • Emboli • Stents and tubes

Other surgeries • extensive bowel surgeries • Burns and plastic surgeries • Gut obstruction • Fluid shifts – seizures

• Electrolytes • Clinical settings

Hyponatremia – usually 115 is cut off • • TURP syndrome Extensive bowel surgeries Other scopies where irrigation is done Plastic and burn reconstruction – massive fluid shifts Drugs like diuretics Water intoxication SIADH. Vomiting Renal and hepatic disorders

Hypocalcemia • • Low albumin; abnormal acid-base status and electrolytes; drugs used during the peri-operative period transfusion of large volumes of citrated blood; Parathyroid surgeries , thyroid , CPBs Sepsis , CRF Calcium chelators in radiographic contrast

Eclampsia

In pregnant – other than • Epilepsy, eclampsia, drugs • Posterior reversible encephalopathy • Amniotic fluid embolism • Cortical vein thrombosis

Intraop seizures – wrong drugs • Tranexemic acid into the intrathecal space


In an ICU • Seizures • • Posttraumatic brain injury CNS infections Endocrine and metabolic disorders Drugs or toxins

Seizure prone electrolyte disturbances • • • Hyponatremia Hypokalemia Hypocalcemia Hypoglycemia and hyperglycemia Hypomagnesemia

Drugs • • Amphetamine SSRIs Tricyclics Levodopa Deriphyllin Phencyclidine Withdrawal of antiepileptics Methergin

Alcohol related • hyponatremia, hypomagnesemia, or hypoglycemia • Thiamine

Anesthesia related • • • Tramadol Pethidine , etomidate Enflurane , sevo Atracurium Flumezanil • Ketamine methohexital ? ? , propofol • Hypocapnia ? ?
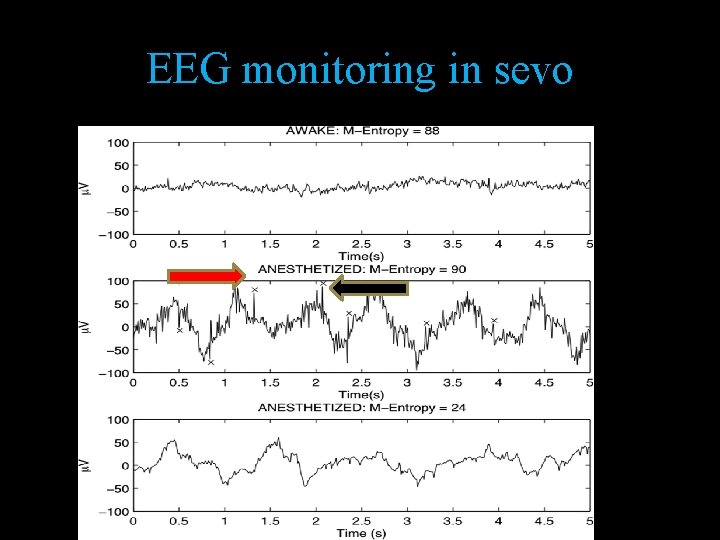
EEG monitoring in sevo

Other settings • • Renal failure --- erythropeitin ? ? Hepatic failure Hypothyroidism Hashimato s • Inciting factors • Fever , infection , sleeplessness

Reflex Anoxic Seizures and Anaesthesia • What is this ? ? • ocular pressure, venepuncture, accidental trauma and fear • Young female school children • Grand mal like • EEG changes may not be present

What should we do • • Patient Should not fall Oxygen Bag and mask Two IV lines Glucose Thiamine Benzodiazepines

Settings at a glance • • Local anaesthetic toxicity TURP Eclampsia Neuro surgeries CPBs Drug intake Drug withdrawal

Post operative period • Postoperative generalized shaking is usually because of shivering, which may be thermoregulatory or non-thermoregulatory. • The latter is thought to be secondary to the effects of volatile anaesthetics, pain or both.

Pseudoepileptic seizures • • • common in the postoperative period. resemble tonic–clonic seizures NO abnormal electrical discharges history of convulsions and/or psychosomatic illness. flamboyant, last longer than 90 s , asynchronous limb movements, side-to-side head movements, closed eyes (including a resistance to eye opening). There is no cyanosis or post-ictal period may be incontinence or tongue-biting. Seizures may settle with reassurance. Plasma prolactin concentrations tend to be raised after epileptic seizures and normal after pseudo-seizures.


In fits • • • Case ? ? Massive fluid shifts Epileptic Systemic illness Drugs, alcohol Hypoxemia Electrolytes , blood glucose, RFT, LFT CT brain Oxygenation, benzodiazepines

Status epilepticus • The traditional definition of status epilepticus as a seizure lasting or recurring without regaining of consciousness over a 30 min period is primarily useful for epidemiological purposes. • Can we wait for 30 minutes ? ? • In clinical practice, most convulsive seizures abate within 2– 3 min and a seizure that continues for more than 5 min has a low chance of terminating spontaneously.

Physiological changes • • Increased cerebral metabolism Increased blood flow, increased glucose and lactate concentration Increased catecholamine secretion • 30 – 60 minutes • hyponatraemia, potassium imbalance, • evolving metabolic acidosis, consumptive coagulopathy, rhabdomyolysis, and multi-organ • failure

Stages • • Premonitory (0 -5 min) Early (5 -10 minutes) Established ( 10 – 30 minutes ) Refractory ( 30 – 60 minutes)

• Pre-monitory stage (out of hospital or first 5 min) • BUCCAL OR RECTAL MIDAZ

Early stage (first 5– 10 min) • • Iv ACCESS OXYGEN GLUCOSE , THIAMINE BENZODIAZIPINES

Established CSE (5– 30 min) • • Phenytoin Phenobarbital Valproate levetiracetam

Refractory status (30– 60 min) • Refractory CSE (RSE), where SE continues in spite of administration of two AEDs (e. g. benzodiazepines and phenytoin), is associated with a high risk of complications. • These include tachyarrhythmias, pulmonary oedema, hyperthermia, rhabdomyolysis, and aspiration pneumonia.


To continue till ? ? • Maximal therapy should be maintained until 12 – 24 h after the last clinical or electrographic seizure, after which the dose should be tapered. If seizures recur, therapy can be re-instituted or altered

Non-convulsive status epilepticus • Impaired consciousness • Automatism • EEG patterns

Summarize • • Status definition Complications Stages Treatment

- Slides: 49