PeriOperative Created by Cindy Lutkenhaus MSN RNCOB CHAPTERS


Peri-Operative Created by: Cindy Lutkenhaus, MSN, RNC-OB CHAPTERS 18, 19, 20 Fall 2015

Pre-operative Interview pt- psychosocial and physical assessment- Risk Factors Health History Current Rx meds, OTC, and herbal supplements, ALLERGIES Pre-op teaching. TCDB SCD or VTE preventative What to expect in OR to reduce anxiety Placement of IV NPO status Common pre-op meds p. 329

Pre-operative Informed consent Nurse SCIP can witness signature only. Informed of risks/benefits by Doctor Measures (surgical care improvement protocol) Hair clipped, not shaved. Antibiotic 30 -60 minutes prior to surgery, DC’d 24 hrs after operation Urinary catheter removed within 24 hrs of surgery Prevent VTE Give beta-blockers if currently on this med

Pre-operative Common Death/ Fears permanent disability Postponement Alteration in body image/Mutilation Pain Anesthesia Disruption of life

Nursing Assessment Cardiovascular • system Report Any cardiac problems so they can be monitored during the intraoperative period Use of cardiac drugs Presence of pacemaker/ICD • 12 -lead electrocardiogram (ECG) • Coagulation studies Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Assessment Respiratory system • Inquire about recent airway infections Procedure could be cancelled because of increased risk of laryngo/bronchospasm or decreased Sa. O 2 • History of dyspnea, coughing, hemoptysis, COPD or asthma High • risk for atelectasis and hypoxemia Smokers should be encouraged to quit 6 weeks before procedure Decreases Greater • risk of complications years and number of packs = greater risk Sleep apnea, obesity, and airway deformities affect respiratory function Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Assessment Nervous • system Evaluation of neurologic functioning Vision or hearing loss can influence results of informed consent Cognitive deficits can affect informed consent and cause adverse outcomes during and after surgery Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Assessment Genitourinary system • History of urinary or renal diseases • Renal dysfunction contributes to Fluid and electrolyte imbalances Increased Impaired Altered risk of infection wound healing response to drugs and their elimination Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Assessment Genitourinary system • Renal function tests • Note problems voiding, and inform operative team • Assess women for possibility of pregnancy Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Assessment Hepatic system • Liver detoxifies many anesthetics and adjunctive drugs • Hepatic dysfunction may increase risk of postoperative complications Integumentary system • History of skin and musculoskeletal problems • History of pressure ulcers Extra padding during procedure Affects • postoperative healing Body art, tattoos, piercings Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Assessment Musculoskeletal system • Identify joints affected with arthritis • Mobility restrictions may affect positioning and ambulation • Bring mobility aids to surgery • Report problems affecting neck or lumbar spine to ACP (anesthesia care provider) Can affect airway management and anesthesia delivery Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Assessment Endocrine system • Patients with diabetes mellitus are especially at risk for: Hypo/hyperglycemia Ketosis Cardiovascular Delayed alterations wound healing Infection Serum or capillary glucose tests morning of surgery (baseline) Clarify with physician or ACP regarding insulin dose Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Assessment Endocrine system • Patients with thyroid dysfunction Hyper-/hypothyroidism poses surgical risks because of altered metabolic rate Verify • with ACP about giving thyroid medications Patients with Addison’s disease Abruptly stopping replacement corticosteroids could cause Addisonian crisis Stress of surgery may require increased dose of IV corticosteroids Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Assessment Immune system • Patients with history of compromised immune system or use of immunosuppressive drugs can have Delayed wound healing Increased risk for infection Fluid and electrolyte status- Usually NPO • Vomiting, diarrhea, or difficulty swallowing can cause imbalances • Identify drugs that alter F and E status Diuretics • Evaluate serum electrolyte levels Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Assessment Nutritional status • Obesity (Person of Size) Stresses cardiac and pulmonary systems Increased risk of wound dehiscence, infection, and incisional hernia Slower recovery from anesthesia Slower wound healing • Provide extra padding to underweight patients to prevent pressure ulcers • May be protein and vitamin deficient • Identify dietary habits that may affect recovery (e. g. , caffeine) Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Management Preoperative teaching • Patient right to know what to expect and how to participate Increases Reduces • patient satisfaction fear, anxiety, stress, pain, and vomiting Limited time available Address needs of highest priority Include information focused on safety Provide written material Anxiety and fear can hinder learning Give priority to patient’s concerns Must be documented and reported to postoperative nurses Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Management Preoperative teaching • Teach deep breathing, coughing, and early ambulation as appropriate • Inform if tubes, drains, monitoring devices, or special equipment will be used postoperatively • Provide surgery-specific information • Basic information before arrival Time and place Fluid and food restrictions Need for enema Need for shower Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Management Legal • preparation All required forms are signed and in chart Informed Blood consent transfusions Advance Power directives of attorney Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Management Consent for surgery • Informed consent must include Adequate disclosure Understanding Voluntarily and comprehension given consent Surgeon responsible for obtaining consent • Nurse may obtain and witness signature • Verify patient has understanding • Permission may be withdrawn at any time Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Management Consent • for surgery Medical emergency may override need for consent Legally appointed representative of family may consent if patient is • Minor • Unconscious • Mentally incompetent Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Management Void before surgery • Prevents involuntary elimination under anesthesia or during early postoperative recovery • Before medication administration Preoperative medication • Benzodiazepines • Anticholinergics • Opioids • Antiemetics • Antibiotics Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Management Transportation to the OR • Via stretcher or wheelchair • Communication “handoff” Situation Background Assessment Recommendation Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Physical Environment Holding area National Patient Safety Goals (NPSGs) require a preprocedure process, including: Verification Required of relevant documentation blood products and equipment Diagnostic and radiology test Procedure site marked Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Surgical Team Perioperative nurse Is a registered nurse (RN) Prepares Serves as patient advocate throughout surgical experience Maintains room with team patient safety, privacy, dignity, confidentiality Circulating nurse Not scrubbed, gowned, or gloved Remains in unsterile field Documents (charts) Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Surgical Team Scrub nurse (LVN, CST) Follows designated hand scrub procedure Gowned and gloved in sterile attire Remains in sterile field Passes Copyright © 2014 by Mosby, an imprint of Elsevier Inc. instruments and implements other technical functions during procedure

Nursing Management preparation Surgical attire worn by all persons entering OR suite Electrical Aseptic Copyright © 2014 by Mosby, an imprint of Elsevier Inc. Room and mechanical equipment checked for proper function technique practiced when placing instruments Counts Functions of team members delineated

Nursing Management Patient patient transported into OR after preparation Sufficient number of staff to lift, guide, and prevent patient falls, as well as injury to staff Persons of size Caution with monitor leads, IVs, and catheters Wheels locked Copyright © 2014 by Mosby, an imprint of Elsevier Inc. Transferring

Nursing Management Basic aseptic technique Center of sterile field is site of surgical incision Only sterilized items in sterile field Protective equipment Face shields, caps, gloves, aprons, and eyewear Assisting anesthesia care provider Know location of emergency equipment and drugs in the OR Circulating nurse may place monitoring devices on patient Remain at patient’s side to ensure safety Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Management Safety considerations Fire Smoke particles Universal Surgical protocol time-out To prevent wrong site, wrong surgery, wrong patient. Copyright © 2014 by Mosby, an imprint of Elsevier Inc. TIME OUT prior to each surgery/procedure - all staff must agree. ID pt, procedure, surgical site, informed consent

Nursing Management Positioning of patient Correct skeletal alignment Prevent pressure on nerves, skin, bony prominences, or eyes Provide for adequate thoracic excursion Accessibility of operative site Administration Maintenance and monitoring of anesthetic agents of airway Prevent occlusion of arteries and veins Provide modesty in exposure Recognize and respect needs such as pain or deformities Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Nursing Management Closely monitor temperature Apply warming blankets Bair Hugger blankets or gowns Increased risk of infection, impaired wound healing Preparing Scrub or clean around the surgical site with antimicrobial agents Use a circular motion from clean to dirty area Allow surgical site to fully dry Hair may be removed with clippers prior to scrub Copyright © 2014 by Mosby, an imprint of Elsevier Inc. Preventing hypothermia

Nursing Management surgery Perioperative nursing data set (PNDS) reflects standards of nursing care in any perioperative setting Care plans in the OR ACP and perioperative team member take patient to PACU and give report Handoff procedure Copyright © 2014 by Mosby, an imprint of Elsevier Inc. After

Gerontologic Considerations Assess drugs should be carefully titrated for poor communication Risk from tape, electrodes, and warming/cooling blankets Osteoporosis and osteoarthritis Perioperative hypothermia Copyright © 2014 by Mosby, an imprint of Elsevier Inc. Anesthetic

Catastrophic Events in the OR Anaphylactic reactions Manifestation may be masked by anesthesia Meds Latex Vigilance and rapid intervention are essential Symptoms include hypotension, tachycardia, bronchospasm, pulmonary edema Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Catastrophic Events in the OR Malignant hyperthermia Rare inherited metabolic disorder Hyperthermia with rigidity of skeletal muscles Often occurs with exposure to succinylcholine, especially in conjunction with inhalation agents Usually occurs under general anesthesia but may also occur in recovery Treatment dantrolene, cold IV fluids and irrigation Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Catastrophic Events in the OR Malignant hyperthermia Tachycardia Tachypnea Hypercarbia Ventricular dysrhythmias Rise in body temperature NOT an early sign Can result in cardiac arrest and death Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Post Anesthesia Care (PACU) Post-operative Anesthesia provider and circulator SBAR to PACU nurse assessment important because detects and manages post-op complications Emergence Delirium (Neuro comp, hypoxia, anesthesia, pain or ET tube) Examples of post-op complications: ? ? Maintain safety is still a large concern Managing Rewarm pain pt

Postoperative Period Begins immediately after surgery PACU is located adjacent to OR Minimizes Provides transport immediate access to anesthesia and OR personnel Nursing care focus • Protecting patient • Preventing complications post- surgical procedure Copyright © 2014 by Mosby, an imprint of Elsevier Inc. •

PACU Admission Report management Anesthetic medications used Other medications received Blood loss Fluid replacement Urine output Intraoperative Unexpected course anesthetic events or reactions Unexpected surgical events Vital signs and trends Results of intraoperative laboratory tests Copyright © 2014 by Mosby, an imprint of Elsevier Inc. Intraoperative

Postoperative Assessment Patency Artificial ECG airway Breathing RR and quality Breath sounds Supplemental oxygen Continuous pulse oximetry monitoring Vital signs Peripheral pulses Capillary refill Skin color and temperature Copyright © 2014 by Mosby, an imprint of Elsevier Inc. Circulation Airway

Postoperative Assessment LOC/ Glasgow Coma Scale Orientation Sensory and motor status Pupil size and reaction Genitourinary Intake (IV fluids) Output (urine and NG) Estimated loss (EBL) blood Copyright © 2014 by Mosby, an imprint of Elsevier Inc. Neurologic

Postoperative Assessment Gastrointestinal sounds NG—Verify placement to suction or clamped Nausea site Dressing CDI Pain Incisional Copyright © 2014 by Mosby, an imprint of Elsevier Inc. Bowel Surgical

Postoperative Complications • Airway obstruction • Hypoxemia • Atelectasis • Aspiration • Bronchospasm • Hypoventilation Copyright © 2014 by Mosby, an imprint of Elsevier Inc. Respiratory

Nursing Interventions to Prevent Respiratory Complications therapy Cough and deep breathing Change patient position every 1– 2 hours Early mobilization Adequate hydration Parenteral Chest or oral physical therapy Pain management Copyright © 2014 by Mosby, an imprint of Elsevier Inc. Oxygen

Splinting With a Pillow or Blanket Copyright © 2014 by Mosby, an imprint of Elsevier Inc.

Postoperative Complications Cardiovascular Syncope Hypertension Dysrhythmias VTE Frequent vital signs monitoring Continuous ECG monitoring Adequate fluid replacement Assess surgical site for bleeding Copyright © 2014 by Mosby, an imprint of Elsevier Inc. Hypotension,

Postoperative Complications Emergence Delayed delirium emergence Anxiety Postoperative Alcohol cognitive dysfunction (POCD) withdrawal delirium Copyright © 2014 by Mosby, an imprint of Elsevier Inc. Neurologic/Psychologic

Nursing Interventions to Prevent Neuropsychologic Complications Monitor oxygen levels with pulse oximetry Fluid and electrolyte balance Adequate nutrition Oxygen therapy Sleep Pain management Reversal agents (Phase I) Proper bowel and bladder functioning Assess for anxiety and depression Monitor mobility status and activity status for safety Alcohol protocols

Nursing Interventions to Prevent Pain and Discomfort Copyright © 2014 by Mosby, an imprint of Elsevier Inc. Analgesics • Epidural catheter • Patient-controlled analgesia (PCA) •

• Passive warming • Active warming • Oxygen therapy • Opioids • Meticulous asepsis • Coughing/deep breathing Copyright © 2014 by Mosby, an imprint of Elsevier Inc. Nursing Interventions to Prevent Hypothermia and Fever

Postoperative Complications Nausea/vomiting Abdominal distension Postoperative Delayed Hiccups ileus gastric emptying Copyright © 2014 by Mosby, an imprint of Elsevier Inc. Gastrointestinal

Nausea/vomiting Antiemetics/prokinetics NG suction as ordered Adequate hydration Assess bowel function Presence Is of bowel sounds/flatulence the patient hungry? Early mobilization Copyright © 2014 by Mosby, an imprint of Elsevier Inc. Nursing Interventions to Prevent GI Complications

Postoperative Complications Urinary Retention • Oliguria • Infection (CAUTI) Monitor urine output Adequate Remove hydration urinary catheter when no longer indicated Normal positioning for elimination Bladder scan/straight catheter per orders Copyright © 2014 by Mosby, an imprint of Elsevier Inc. •
Postoperative Complications Surgical Site Infection Copyright © 2014 by Mosby, an imprint of Elsevier Inc. Surgical site/wounds • Surgical site infection (SSI) • Hematoma • Dehiscence Assess the wound Note drainage color, consistency, and amount Assess effect of position changes on wound/drain tube drainage Signs/symptoms (S/S) of infection Ordered prophylactic antibiotics Maintain glycemic control

Modified Aldrete Scoring System to assess transition from PACU to discharge Discontinuation motor function A Copyright © 2014 by Mosby, an imprint of Elsevier Inc. Used of anesthesia to return of protective reflexes and score of 9 or 10 indicates readiness for transfer or discharge to the next phase of recovery
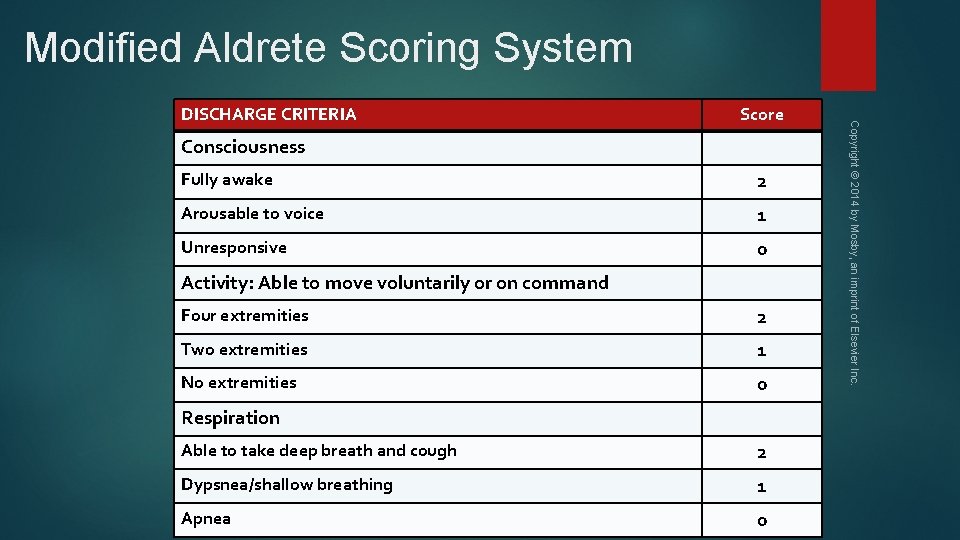
Modified Aldrete Scoring System Score Consciousness Fully awake 2 Arousable to voice 1 Unresponsive 0 Activity: Able to move voluntarily or on command Four extremities 2 Two extremities 1 No extremities 0 Respiration Able to take deep breath and cough 2 Dypsnea/shallow breathing 1 Apnea 0 Copyright © 2014 by Mosby, an imprint of Elsevier Inc. DISCHARGE CRITERIA
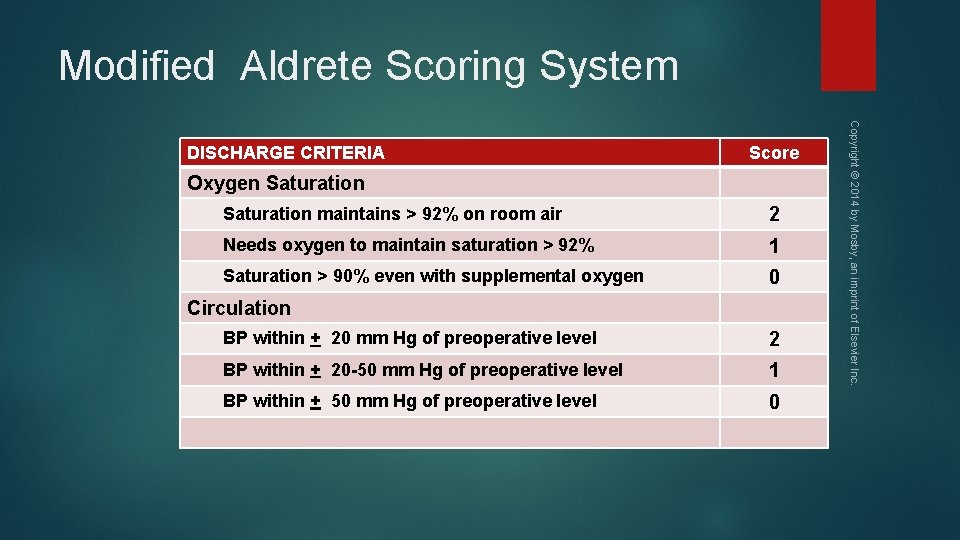
Modified Aldrete Scoring System Score Oxygen Saturation maintains > 92% on room air 2 Needs oxygen to maintain saturation > 92% 1 Saturation > 90% even with supplemental oxygen 0 Circulation BP within + 20 mm Hg of preoperative level 2 BP within + 20 -50 mm Hg of preoperative level 1 BP within + 50 mm Hg of preoperative level 0 Copyright © 2014 by Mosby, an imprint of Elsevier Inc. DISCHARGE CRITERIA

PACU Discharge Criteria airway Patient awake Hemodynamic • stability BP and HR, sinus rhythm No respiratory depression Oxygen Pain saturation > 90% management Condition N/V, of surgical site (no excessive bleeding) Bowel Sounds Copyright © 2014 by Mosby, an imprint of Elsevier Inc. Patent

Discharge Criteria from PACU Hemodynamic and comfort management Condition of surgical site and dressings/drainage tubes Fluid/hydration Mobility status—can ambulate if not contraindicated Emotional Patient status (voided if appropriate) status safety needs Significant other interactions Copyright © 2014 by Mosby, an imprint of Elsevier Inc. Pain stability

Gerontologic Considerations Postoperative Patient Altered Drug vascular function toxicity Mental Pain respiratory function status changes control Copyright © 2014 by Mosby, an imprint of Elsevier Inc. Decreased
- Slides: 61