Periodontal Plastic Surgery Soft Tissue Grafting Indications and





















- Slides: 42

Periodontal Plastic Surgery Soft Tissue Grafting Indications and Procedures

Objectives • To understand some of the different types of grafts used in Periodontal Plastic Surgery (Mucogingival Surgery) • To understand the indications for the different types of mucogingival surgeries • To show some examples of one of the most common grafting procedures, the FGG and CTG. • To understand when a condition would not benefit from Mucogingival Surgery

Common Questions (FAQ’s): • When is gingival grafting needed and when is it not? • Why do I need it? What happens if I don’t do it? • Does it hurt? • What is the recovery time? • Does it work? Does it have to be redone? • Does brushing too hard cause recession? • How much does it cost?

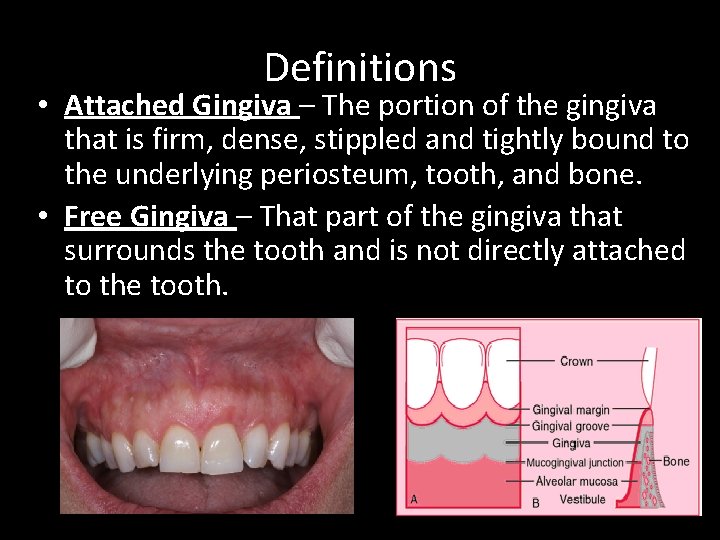
Definitions • Attached Gingiva – The portion of the gingiva that is firm, dense, stippled and tightly bound to the underlying periosteum, tooth, and bone. • Free Gingiva – That part of the gingiva that surrounds the tooth and is not directly attached to the tooth.

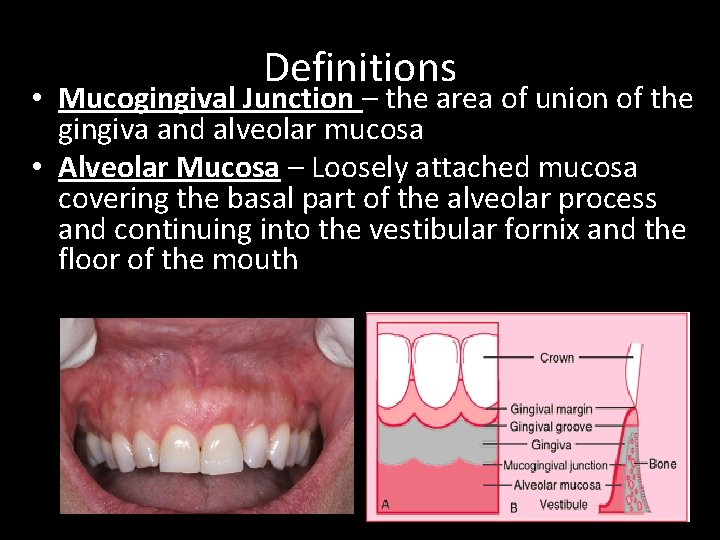
Definitions • Mucogingival Junction – the area of union of the gingiva and alveolar mucosa • Alveolar Mucosa – Loosely attached mucosa covering the basal part of the alveolar process and continuing into the vestibular fornix and the floor of the mouth

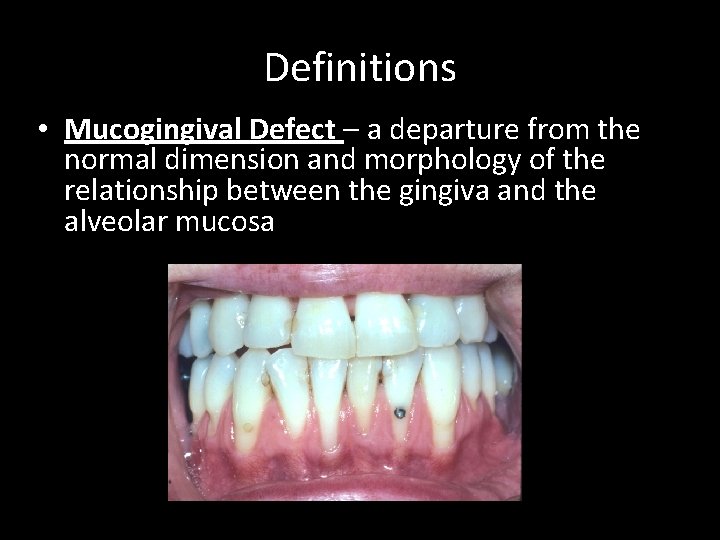
Definitions • Mucogingival Defect – a departure from the normal dimension and morphology of the relationship between the gingiva and the alveolar mucosa

Definitions • Free Gingival Graft (FGG) - A soft tissue graft that is completely detached from one site and transferred to a remote site. No connection with the donor site is maintained • Subepithelial Connective Tissue Graft (CTG) - A detached connective tissue graft that is placed beneath a partial thickness flap. This variation of the free gingival graft provides the tissue graft with a nutrient supply on two surfaces

History of Periodontal Plastic Surgery • 1930’s – Frenectomies and vestibuloplasties • 1948 – First Gingivoplasties • 1956 – Grupe and Warren publish Laterally Positioned Flap • 1963 – Bjorn publishes the Free Gingival Graft • 1982 – P. D. Miller introduces the FGG for root coverage. Fernandez does first CT graft • 1989 – AAP renames Mucogingival Surgery to Periodontal Plastic Surgery

Indications for Perio Plastic Surgery • Gingival Augmentation – Free Gingival Graft – Connective Tissue Graft • Root Coverage – Coronally positioned flap – Semilunar flap – Laterally positioned flap – Double papilla flap – Free Gingival Graft – Connective Tissue Graft – Guided Tissue Regeneration using allograft

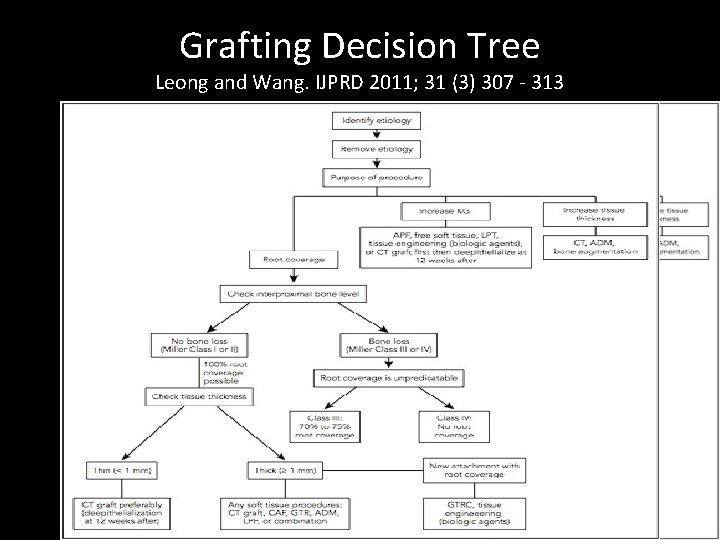
Grafting Decision Tree Leong and Wang. IJPRD 2011; 31 (3) 307 - 313

When is Grafting Needed? • How much keratinized gingivae is needed? – Bowers 1963 – felt that gingival health could be maintained with a narrow zoned of KG (<1 mm) but some was required for healing – Lang & Loe 1968 – suggested 2 mm – Maynard and Wilson 1979 – 5 mm of KG with 3 mm attached when subgingival restorations are planned – Kennedy 1985 – over a 6 year period, patients with inconsistent OH saw recession with thin tissue • Bottom Line: some attached gingiva is necessary for health, but patients with good OH can maintain thin AG.

When is Grafting Needed? • Is the recession progressing? • Is the tooth treatment planned for orthodontic care or prosthetic treatment? • Is there root sensitivity? • Is there difficulty cleaning the root surface by the patient? • Is there an esthetic concern?

Free Gingival Autografts • Indications • To increase keratinized tissue around teeth, implants or crowns • To increase keratinized tissue under removable prostheses • To increase vestibular depth • Disadvantages • • Difficult to achieve root coverage High esthetic demand Large, uncomfortable donor site Graft site, slow uncomfortable healing

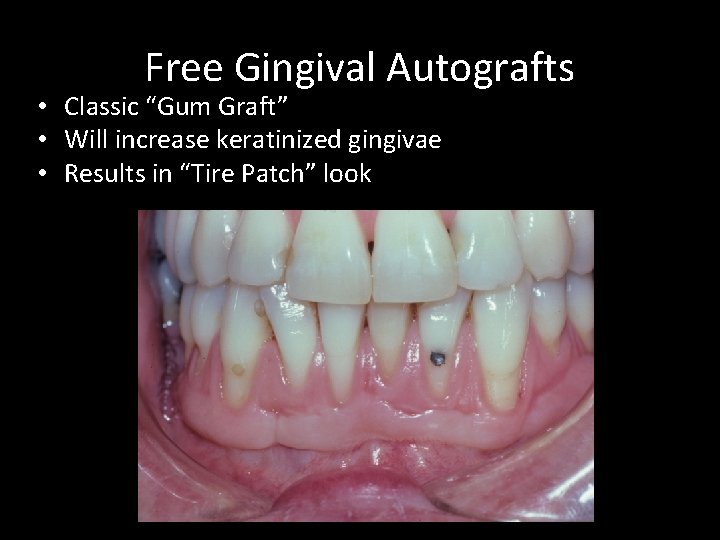
Free Gingival Autografts • Classic “Gum Graft” • Will increase keratinized gingivae • Results in “Tire Patch” look

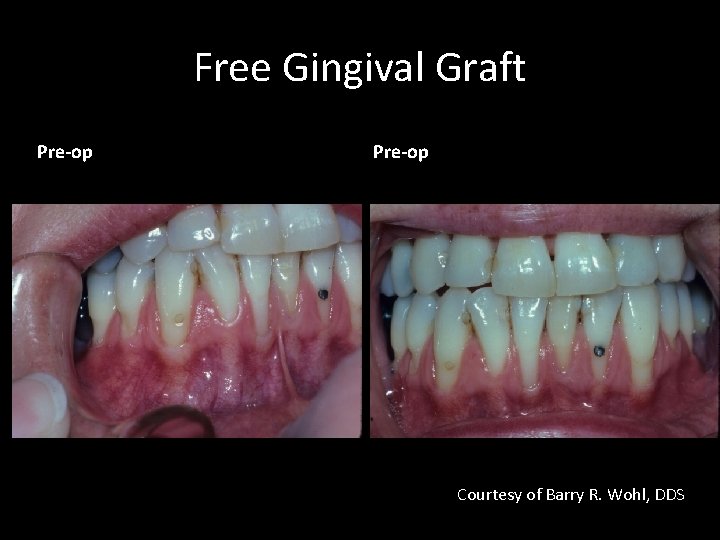
Free Gingival Graft Pre-op Courtesy of Barry R. Wohl, DDS

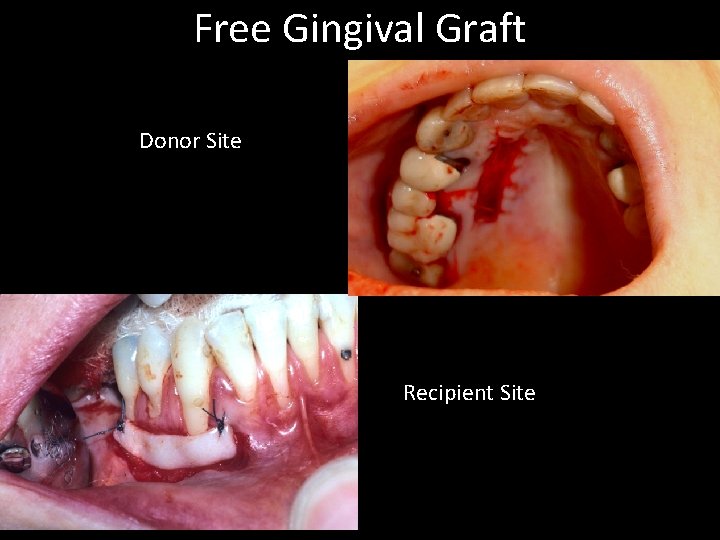
Free Gingival Graft Donor Site Recipient Site

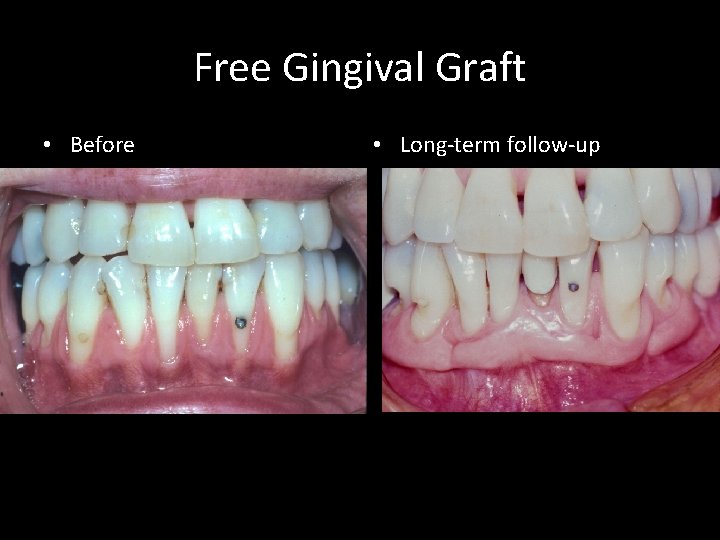
Free Gingival Graft • Before • Long-term follow-up

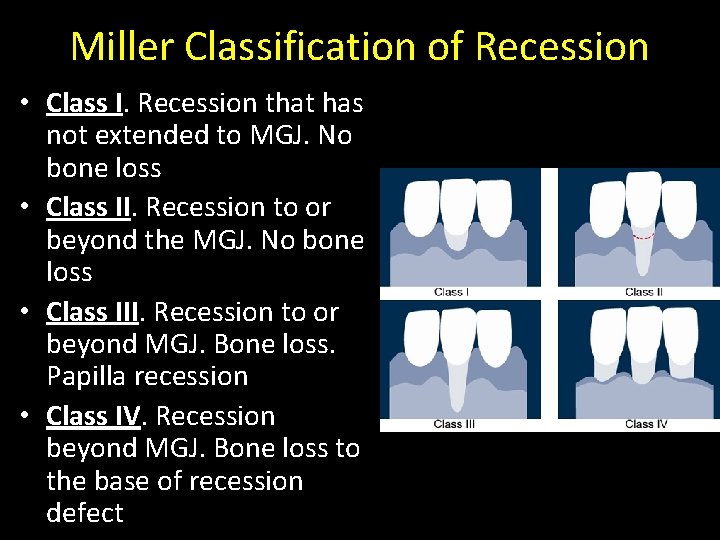
Miller Classification of Recession • Class I. Recession that has not extended to MGJ. No bone loss • Class II. Recession to or beyond the MGJ. No bone loss • Class III. Recession to or beyond MGJ. Bone loss. Papilla recession • Class IV. Recession beyond MGJ. Bone loss to the base of recession defect

Causes and Predisposing Factors in Gingival Recession • Predisposing Factors: – Minimal attached gingiva/thin tissue biotype – Frenum pull / shallow vestibule – Tooth malposition • Precipitating Factors: – Inflammation related to plaque – Restorations adjacent to thin tissue – Occlusal Trauma including orthodontic treatment – Bone loss at an adjacent site

Connective Tissue Graft • Advantages – Very predictable for root coverage – Smaller donor site (than FGG) – Smaller recipient site (than FGG) – Less soreness overall (than FGG) – Uses patient’s own tissue – Excellent esthetics – Can cover multiple, large recessions even on teeth with a previous restorations

Connective Tissue Grafts • Disadvantages – Two surgical sites – Technique sensitive – Bleeding from palate (potential)

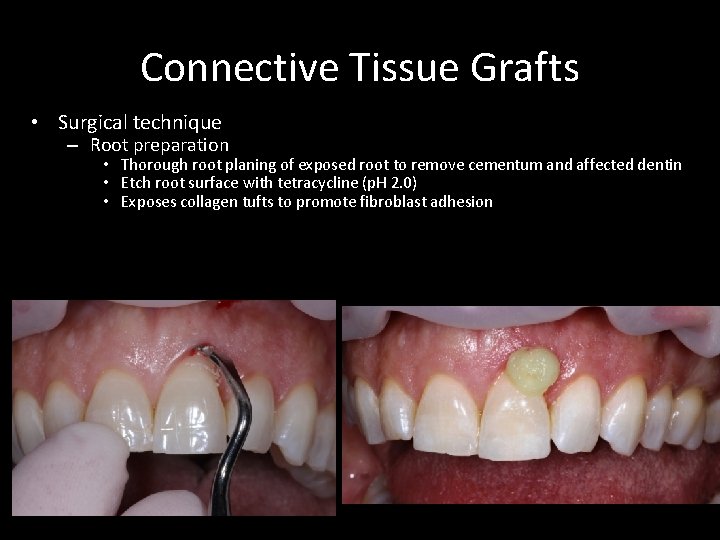
Connective Tissue Grafts • Surgical technique – Root preparation • Thorough root planing of exposed root to remove cementum and affected dentin • Etch root surface with tetracycline (p. H 2. 0) • Exposes collagen tufts to promote fibroblast adhesion

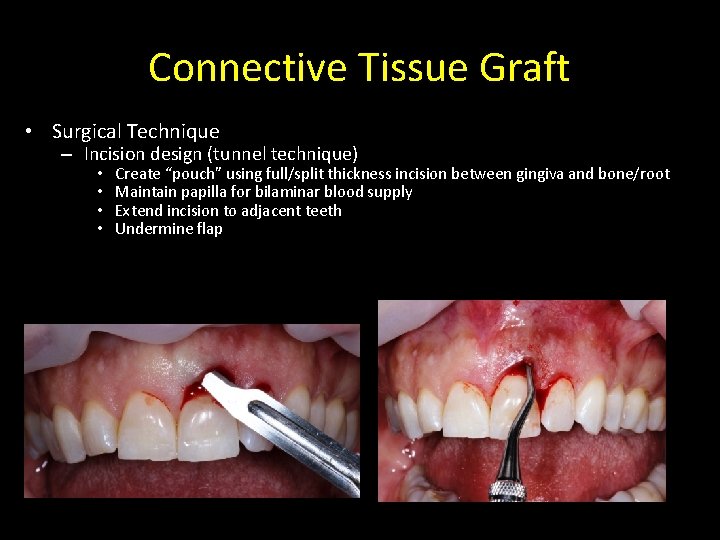
Connective Tissue Graft • Surgical Technique – Incision design (tunnel technique) • • Create “pouch” using full/split thickness incision between gingiva and bone/root Maintain papilla for bilaminar blood supply Extend incision to adjacent teeth Undermine flap

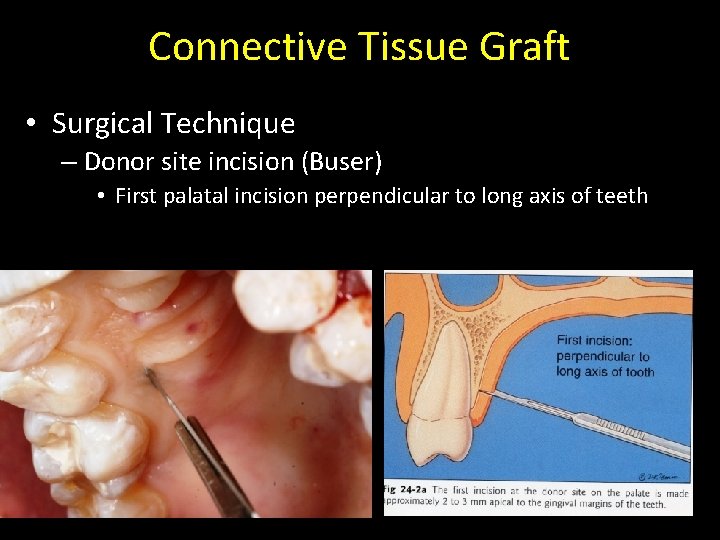
Connective Tissue Graft • Surgical Technique – Donor site incision (Buser) • First palatal incision perpendicular to long axis of teeth

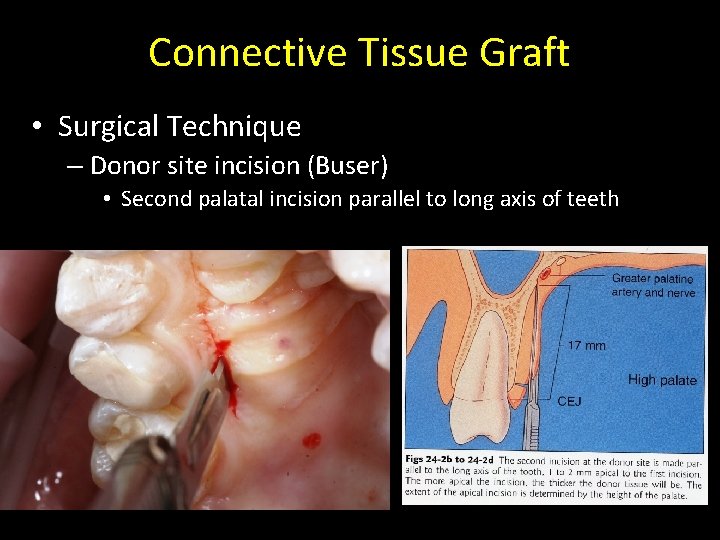
Connective Tissue Graft • Surgical Technique – Donor site incision (Buser) • Second palatal incision parallel to long axis of teeth

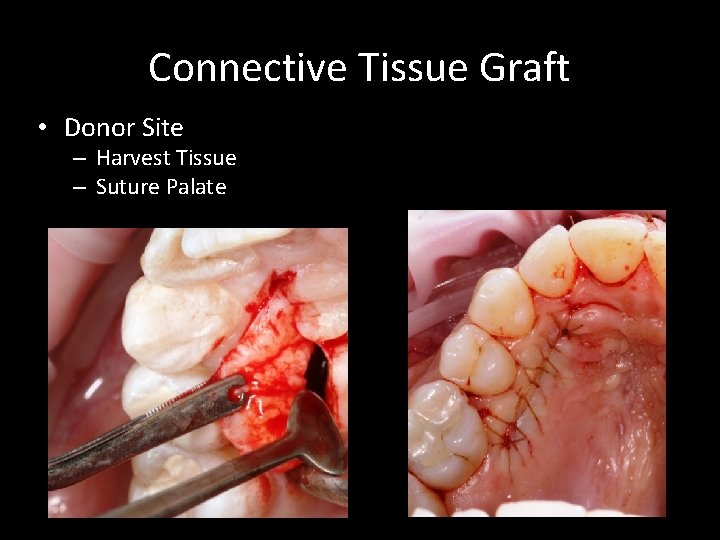
Connective Tissue Graft • Donor Site – Harvest Tissue – Suture Palate

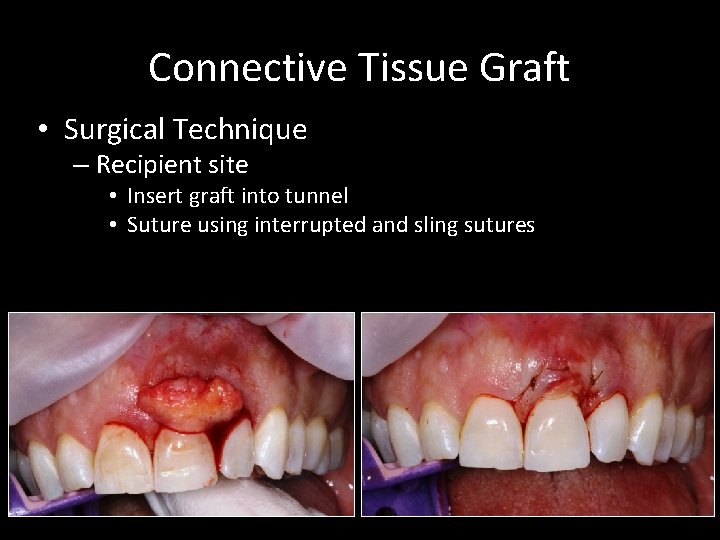
Connective Tissue Graft • Surgical Technique – Recipient site • Insert graft into tunnel • Suture using interrupted and sling sutures

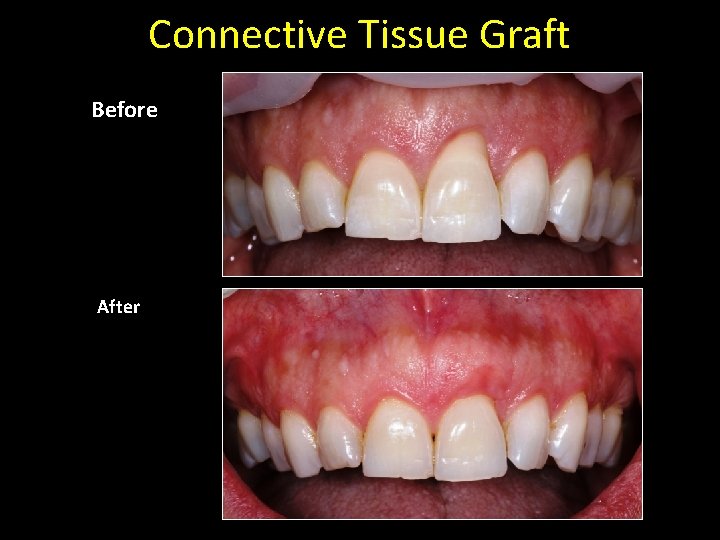
Connective Tissue Graft Before After

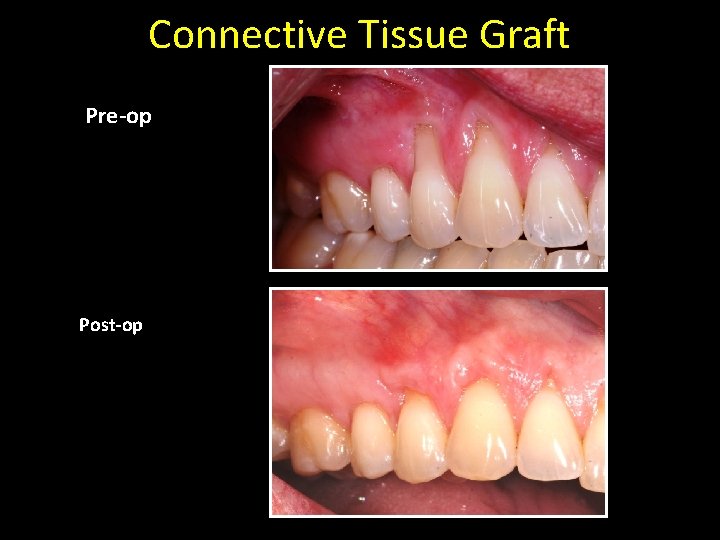
Connective Tissue Graft Pre-op Post-op

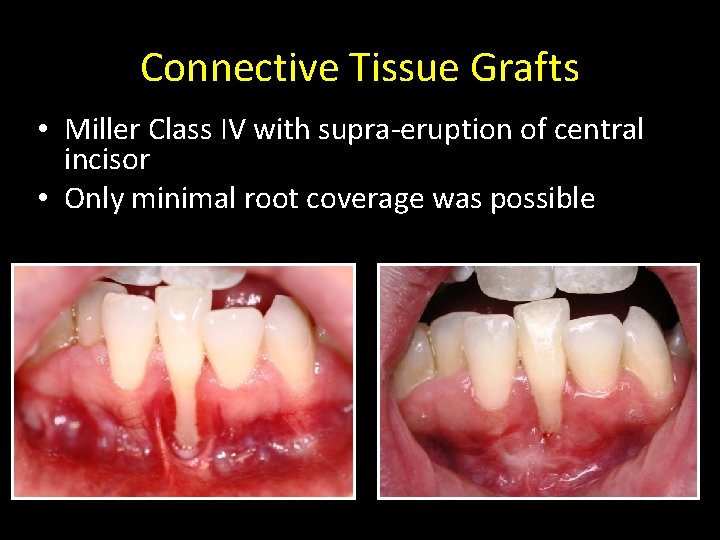
Connective Tissue Grafts • Miller Class IV with supra-eruption of central incisor • Only minimal root coverage was possible

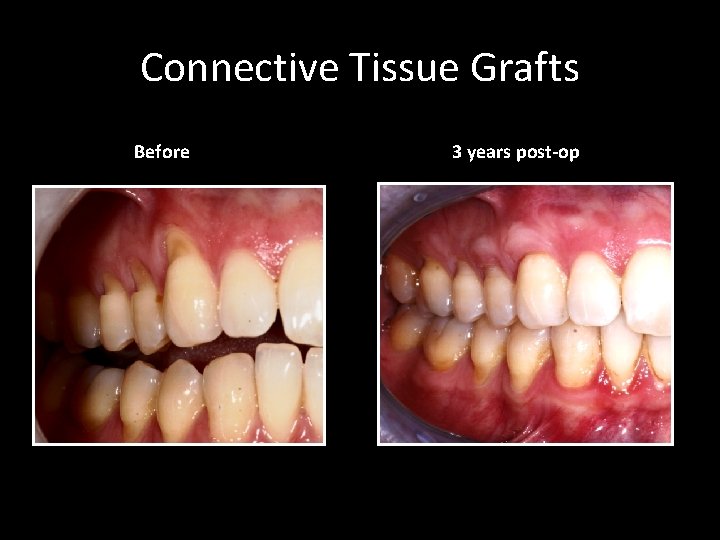
Connective Tissue Grafts Before 3 years post-op

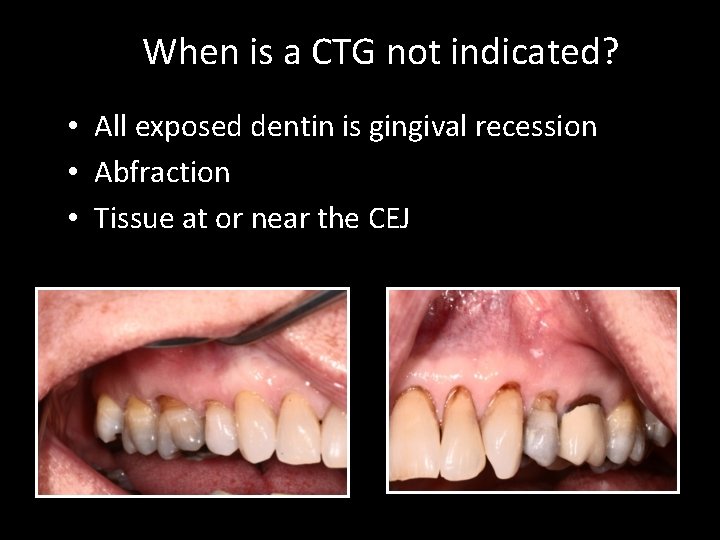
When is a CTG not indicated? • All exposed dentin is gingival recession • Abfraction • Tissue at or near the CEJ

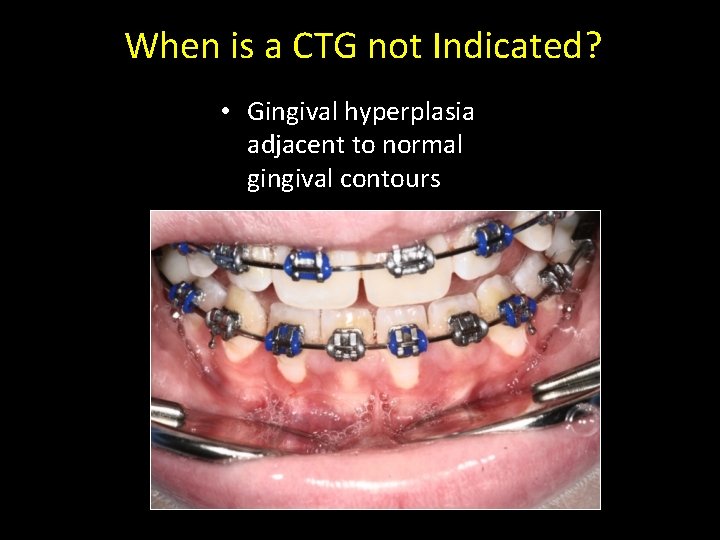
When is a CTG not Indicated? • Gingival hyperplasia adjacent to normal gingival contours

Brushing TOO Hard?

Does brushing cause recession? • Does brushing too hard causes gum recession? Not really…. – Toothbrushing and Gingival Recession. Litonjua, LA, et al. Int Dent J 2003 53(2) a literature review showed no direct relationship between toothbrushing and gingival recession – Trauma from toothbrushing may contribute to recession in a minor way, but other more important factors should be treated first – Abrasion of the hard surfaces of the teeth are likely caused by abrasives in the toothpaste

Does it HURT? • The common perception is that Connective Tissue Grafting is VERY PAINFUL!! – This is often the patient’s perception – This perception is usually the result of hearsay from friends and relatives – The origins probably go back to the days of the Free Gingival Grafts

FEAR

Does it HURT? • Reality – In 20 years of performing CT grafts, very few patients ever complain about significant pain afterwards – Most are pleasantly surprised at how little pain they had – Very little post-op bleeding, swelling or bruising – Of course, everyone’s pain threshold is different…

What is the Recovery Time? • Recovery times vary from individual to individual • Post-op instructions include: – Soft foods for a week – Avoid chewing in the donor or recipient sites if possible for the first week – Bleeding from the palate is possible for the first 24 hours and sometimes longer – Don’t brush the donor site for 1 week; the recipient site for 3 weeks. Chlorhexidine mouthwash in the meantime – Ibuprofen 800 mg 3/day for 2 – 3 days

What is the Recovery Time? • Most patients report some soreness during the first week, but most do not take anything more than the Ibuprofen 800 mg • Some swelling of the recipient site is normal and occasionally some bruising • Sutures resorb in the palate in 2 – 3 days and in about 1 week in the recipient site • Most people resume normal activities either the next day or two days after • Smokers heal more slowly and results are less predictable

Conclusions • Mucogingival defects are very common across all age groups and both genders • Mucogingival defects can be either congenital or acquired with both predisposing and precipitating factors • Periodontal Plastic Surgery can be used to correct mucogingival defects via a variety of methods and techniques • Indications for Periodontal Plastic Surgery can vary depending on rate of progression or the impact of local factors

Thank You! GINGIVAL RECESSION