Periodontal Microbiology q Human fetus is sterile but

Periodontal Microbiology

q Human fetus is sterile but after passing through birth canal it acquires vaginal and fecal microorganisms q By 2 nd day Anaerobic flora can be detected in infant edentulous mouth 10/28/2020 Dr Saif Khan 2

q Within 2 nd week a nearly mature microbiota is established in the gut of newborn q After weaning(>2 yrs), entire human microbial flora formed by complex collection of more than 400 types of bacteria. 10/28/2020 Dr Saif Khan 3
Oral cavity is an “Open growth system” ORAL CAVITY 10/28/2020 COMMUNICATES WITH OROPHARYNX Dr Saif Khan OPEN GROWTH SYSTEM 4
Oral cavity divided into 5 major niches Intraoral, Supragingival hard surface(teeth, Implants, restoration, and prosthesis) Periodontal/Periimplant pocket (with its crevicular fluid, the root cementum or implant surface, and pocket epithelium) Buccal epithelium, palatal epithelium, and epithelium of the floor of the mouth Dorsum of the tongue Tonsil 10/28/2020 Dr Saif Khan 5

q Most species colonize on all above described niches with the exception of spirochetes q Adherence of bacteria to oral epithelial cells is directly related to its virulence 10/28/2020 Dr Saif Khan 6

q. Teeth and Implants are unique from a microbiological point of view for two reason – Provide hard, non-shedding surface that allows for the development of extensive structured baterial deposit – Form a unique ectodermal interruption q. A special seal of epithelium and connective tissue exists between external enviroment and internal part of body 10/28/2020 Dr Saif Khan 7

q. Teeth are primary habitat for periopathogens q. Thus teeth can be considered as “Port of entry for Periopathogens q. Cariogenic species like S mutans remain restricted to solid surfaces and are called “obligate periphyte” 10/28/2020 Dr Saif Khan 8

Dental Plaque Dental plaque is a specific, amorphous, granular deposit which accumulates on the surface of teeth, dental restoration and dental calculus. - -Glickmann 10/28/2020 Dr Saif Khan 9

WHO defnition “Dental plaque is a specific but highly variable entity resulting from growth and colonization of micro-organisms on surfaces of teeth, restoration and soft- tissue consisting of various species microorganisms entangled in extracellular matrix. ” 10/28/2020 Dr Saif Khan 10

Dental plaque • Defined clinically as structured, reselient, yellowish-grayish substance that adhere tenaciously to the intraoral hard surface, including removable and fixed restoration. • Plaque is primarily composed of bacteria in matrix of salivary glycoproteins and extracellular polysaccharides • 1 gm of dental plaque(wet weight) contains 1011 bacteria 10/28/2020 Dr Saif Khan 11

No of bacteria in Supragingival plaque on single tooth – 109 Gingival Crevice- 103 Deep periodontal pocket- 108 More than 500 distinct microbial species are found in dental plaque Non bacterial microorganism found in plaque include Mycoplasma species, yeasts, Protozoa and Viruses 10/28/2020 Dr Saif Khan 12
Dental plaque is broadly Classified into Supragingival Plaque Subgingival Plaque 10/28/2020 Dr Saif Khan 13
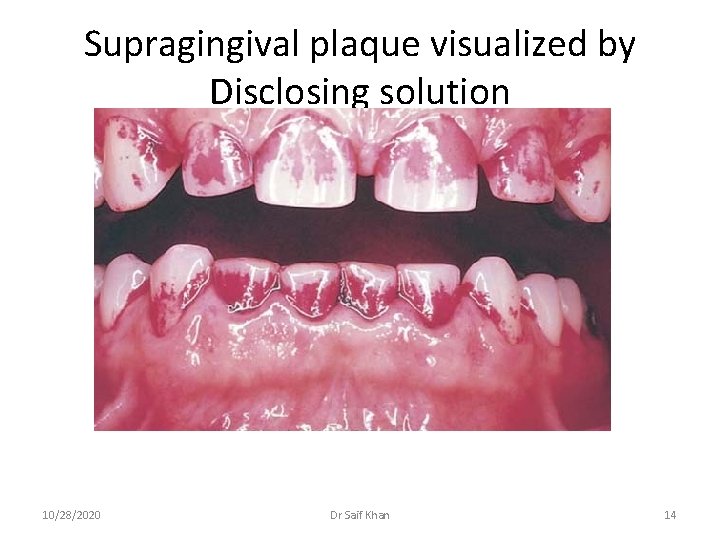
Supragingival plaque visualized by Disclosing solution 10/28/2020 Dr Saif Khan 14

Supragingival Plaque Marginal Plaque Subgingival plaque 10/28/2020 • Multilayered accumulation of bacterial morphotypes. Gm+ve Cocci & short rods predominate at tooth surface whereas Gm-ve rods and filaments as well as spirochetes predominate at the outer surface • At this location filamentous microorganisms dominate but cocci and rods also occur • Dominated by Gm+ve rods and cocci including S mitis, S sangius, A viscosus, A nnaeslundi and Eubacterium Species • Differs in composition from supragingival plaque because of local availability of blood products and low oxygen tension. Gm-ve Anaerobes and Spirochetes predominate Dr Saif Khan 15
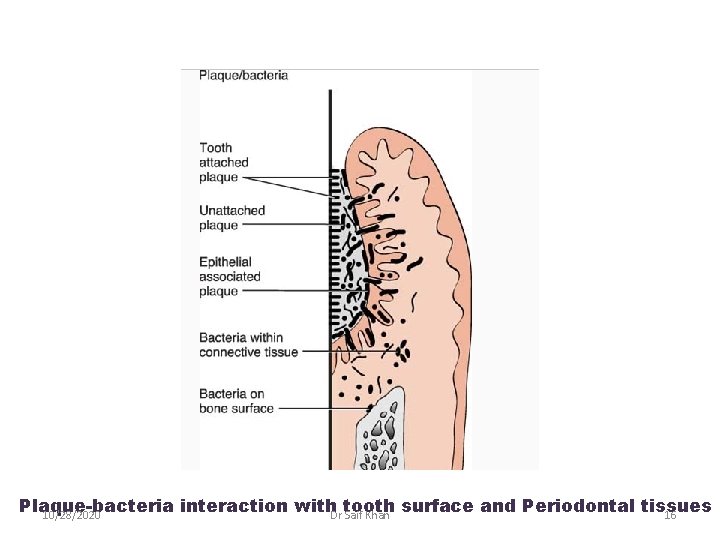
Plaque-bacteria interaction with. Dr Saif Khan tooth surface and Periodontal tissues 10/28/2020 16
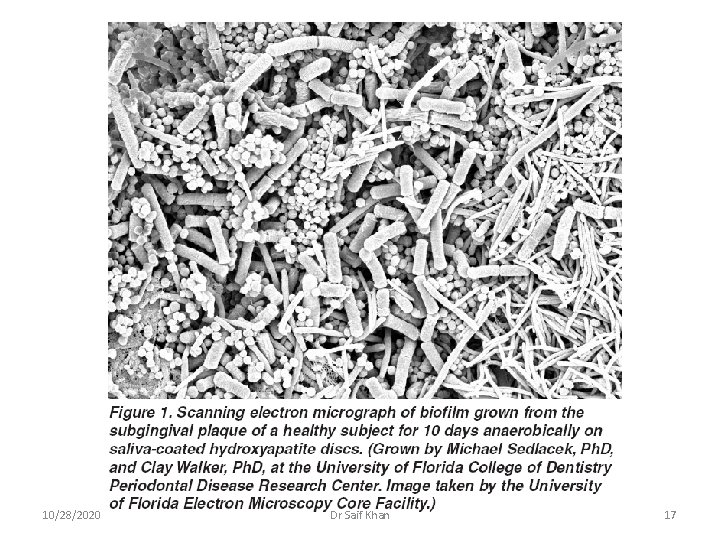
10/28/2020 Dr Saif Khan 17
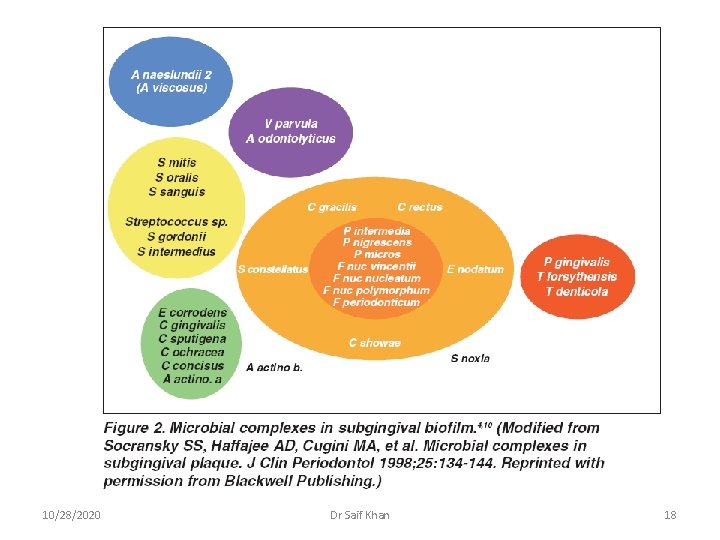
10/28/2020 Dr Saif Khan 18

The enviromental paramaters of subgingival region is different from supragingival region – Gingival crevice is bathed by GCF which may contains many substances that bacteria may use as nutrients – Low oxygen tension in the subgingival area – Host inflammatory cells and mediators have considerable influence on establishment and growth of bacteria 10/28/2020 Dr Saif Khan 19

The apical border of the plaque mass is separated from junctional epitheliun by a layer of host leukocytes and the bacteria of this apical-tooth associated region show an increased concentration of Gm-ve rods 10/28/2020 Dr Saif Khan 20

Dental Plaque as a Biofilm • Biofilm is a highly organized structure • Consists of microcolonies of bacterial cells randomly distributed in a shaped matrix or glycocalyx. • Lower plaque layer are dense in which microbes are bound together in polysaccharide matrix with other organic and inorganic materials 10/28/2020 Dr Saif Khan 21

• On top of lower layer, loose layer can be seen which can extend into surrounding medium (for teeth and saliva) • The fluid layer bordering the biofilm has a stationary sublayer and a fluid layer in motion • Nutrient components penetrate this fluid medium by molecular diffusion 10/28/2020 Dr Saif Khan 22

• The dental plaque biofilm has open fluid filled channels running across the plaque mass • Act as primitive “circulating system” 10/28/2020 Dr Saif Khan 23

Intercellular Matrix • Organic Constituent- Consists of – Polysacchrides, Proteins, Glycoprotein & Lipid – Albumin derived from GCF – Lipid material consists of debris from the membranes of disrupted bacterial & Host cells and possibly Food debris – Glycoprotein from saliva important component of pellicle – Polysacchrides produced by bacteria of which Dextran is most predominant form & play major role in maintaining integrity of Biofilm 10/28/2020 Dr Saif Khan 24

Inorganic component • Predominantly Ca and P • Trace minerals Na, K and F • Source of inorganic constituent of supragingival plaque is primarily saliva • As mineral content increases plaque calcifies to Calculus • Inorganic portion of subgingival fluid are derived from crevicular fluid • F content of plaque is basically derived from external sources such as floridinated toothpaste, rinses, water etc 10/28/2020 Dr Saif Khan 25

Plaque formation at Ultrastructural level 1. Formation of Pellicle – Thin, saliva derived layer – Consists of Glycoprotein (mucins), Proline rich protein, Phosphoproteins (Statherin), Histidine rich proteins, enzymes – Forms within seconds of prophylaxis – Forms by selective adsorption of enviromental macromolecules – Mechanism involved in pellicle formation include Vanderwall forces & Hydrophobic forces 10/28/2020 Dr Saif Khan 26

10/28/2020 Dr Saif Khan 27
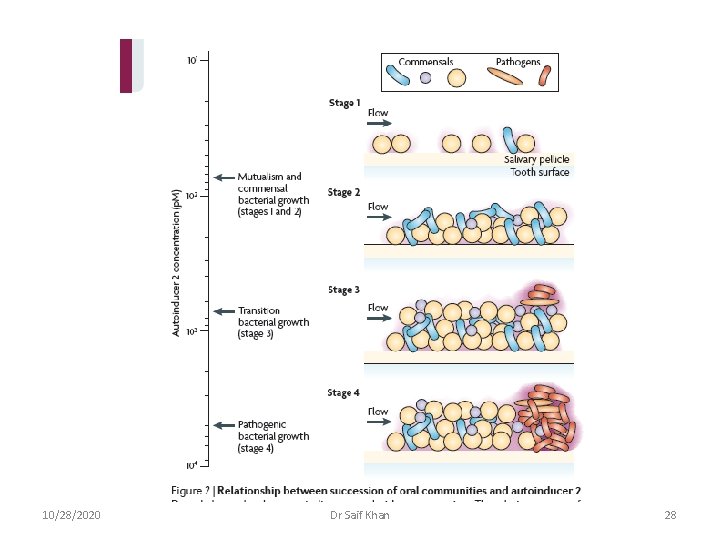
10/28/2020 Dr Saif Khan 28

2. Initial Adhesion and attachment of bacteria Phase I : Transport to the surface • • • Initial contact of bacterium to tooth surface Random contacts through Brownian movement (40μm/hr) Through Active bacterial movement Phase II: Initial Adhesion • Reversible adhesion • Interaction b/w bacteria and surface at certain distance (50 nm) through long range and short range forces • Including Vanderwall attractive and electrostatic repulsive forces • Gibbs total energy GTOT = GA + GE • GTOT is a function of separation distance between negatively charged particle and negatively charged surface in a medium ionic suspension (saliva) • For most bacteria reversible binding takes place 5 -20 nm from surface 10/28/2020 Dr Saif Khan 29
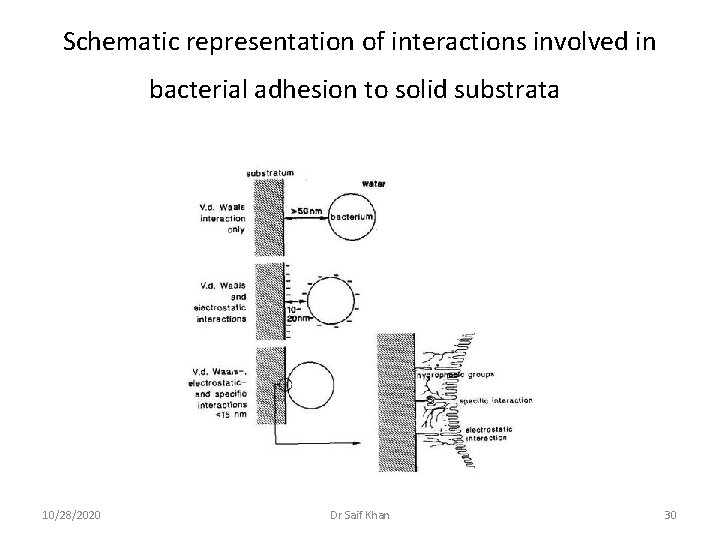
Schematic representation of interactions involved in bacterial adhesion to solid substrata 10/28/2020 Dr Saif Khan 30
Phase III: Attachment • • • After intial adhesion firm adhesion is established by specific interactions (covalent, ionic or hydrogen Rough surfaces are more conducive for attachment as bacteria are better protected against sheer force leading change from reversible to irreversible bonding The bonding between bacteria and pellicle is mediated by by specific extracellular protein components Bacteriu m Complimentary Receptor(protein, glycoprotein or polysacchride) on the pellicle eg; Streptococci (S sangius) early colonizer binds to acidic proline-rich proteins, also α-amylase and sialic acid 10/28/2020 Dr Saif Khan 31

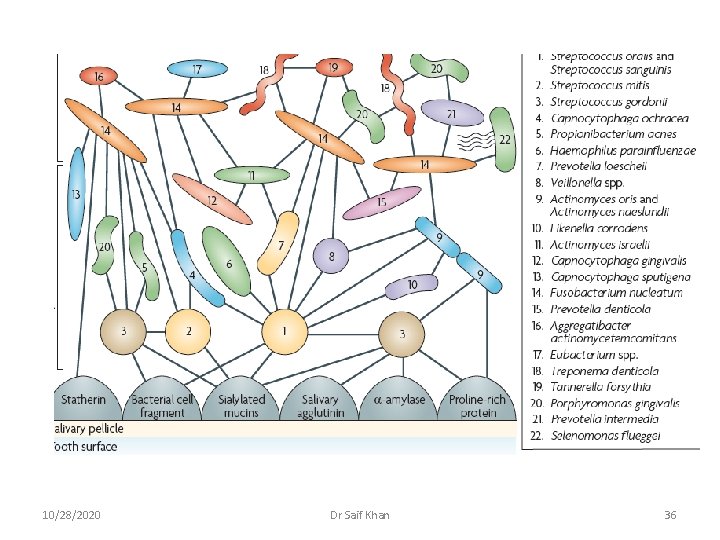
3. Colonization and plaque maturation Primary Colonizers: Streptococci and Actinomycetes Secondary Colonizers: P intermedia, P loescheii, Capnocytophaga, F nucleatum, P gingivalis 10/28/2020 Dr Saif Khan 32

Ø All oral bacteria possess surface molecule or receptor which foster cell to cell interaction Ø Highly specific stereo chemical interaction of proteins and carbohydrate molecules located on bacterial cell surfaces leading to Coaggregation Ø Most Co aggregation are among strains of different genera are mediated by Lectin like adhesins and inhibited by Lactose and other galactosides 10/28/2020 Dr Saif Khan 33

Examples of Co-aggregation v Fusobacterium nucleatum with steptocooci sangius, Prevotella loescheii with A viscosus v Capnocytophaga ochraceus with A viscosus v Intrageneric co-aggregation in streptocooci 10/28/2020 Dr Saif Khan 34
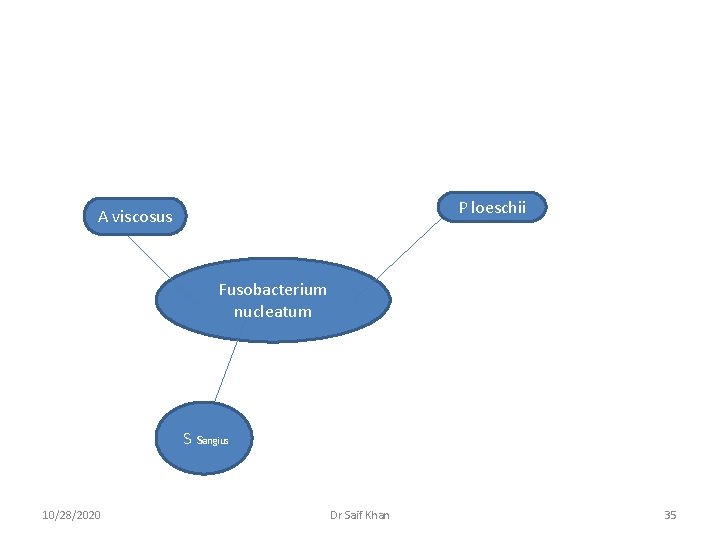
P loeschii A viscosus Fusobacterium nucleatum S sangius 10/28/2020 Dr Saif Khan 35
10/28/2020 Dr Saif Khan 36

Growth dynamics of Dental Plaque • First 2 -8 hrs, adherent pioneering streptococci saturate the salivary pellicular binding sites and cover 3 -30% of enamel surface • After 1 day the term Biofilm is fully deserved because organization takes place in it • After 3 days plaque growth increases at rapid rate and then slows down 10/28/2020 Dr Saif Khan 37

• There is shift towards more anaerobic and gramnegative flora, including an influx of Fusobacteria, filaments, Spiral forms and spirochetes • In ecological shift within of the biofilm, there is a transition from the early aerobic environment characterized by Gm+ve facultative species to a highly oxygen- deprived environment in which Gm -ve anaerobic microorganism predominate 10/28/2020 Dr Saif Khan 38

Topography of Supragingival Plaque • Early plaque formation follow typical topograhic pattern with initial growth along gingival margin and interdental space • Later furthere is extension in coronal direction • This pattern changes when tooth contains surface irregularities such as grooves, cracks, perikymata, or pits • Surface irregularities can give rise to “individualized plaque growth pattern 10/28/2020 Dr Saif Khan 39

Surface Microroughness • Rough intraoral surface (crown, implant abutments, denture bases)accumulate and retain more plaque and calculus in terms of thickness area and colony forming unit • [Ra=0. 2µ] is threshold for surface roughness above which bacterial adhesion is facilitated 10/28/2020 Dr Saif Khan 40

Individual variables influencing plaque formation q. Heavy(fast) plaque formers § Rapid plaque formers demonstrate higher proportion of Gm-ve rods (35% vs 17%) in 14 -day old plaque q. Light (slow) plaque formers 10/28/2020 Dr Saif Khan 41

Intersubject variation in plaque formation can be explained by factors such as • • • Diet Food Smoking Presence of copper amalgam Tongue& palate brushing Colloid stability of bacteria in the saliva Antimicrobial factors present in saliva Chemical composition of the Pellicle Retention depth of dentogingival area 10/28/2020 Dr Saif Khan 42

Variation within the Dentition Early plaque formation occurs faster in • lower jaw compared to upper • Molar areas • Buccal tooth surfaces as compared to oral sites (esp in upper jaw) • Interdental region compared to buccal or oral surfaces 10/28/2020 Dr Saif Khan 43

Impact of Gingival inflammation • Early invivo plaque formation is more rapid on tooth surfaces facing inflamed gingival margins than those adjacent to healthy gingival margins • Increase in crevicular fluid production enhances plaque formation 10/28/2020 Dr Saif Khan 44

Impact of Age Recent studies show that subject’s age does not influence de novo plaque formation 10/28/2020 Dr Saif Khan 45

Spontaneous tooth cleaning • Firm attachment between bacteria and surface this is unlikeky • Even occlusal part of molars, plaque remains after chewing fibrous food • Only negligible differences in plaque extension could be observed 10/28/2020 Dr Saif Khan 46

De novo subgingival plaque formation v. Recent studies suggest that complex subgingival microbiota, including most periopathogens, is established within 1 week after abutment insertion v. Smooth abutments[Ra<0. 2µ] were found to harbour less bacteria than less ones, with a slightly higher density of coccoids (i. e nonpathogenic) cell 10/28/2020 Dr Saif Khan 47
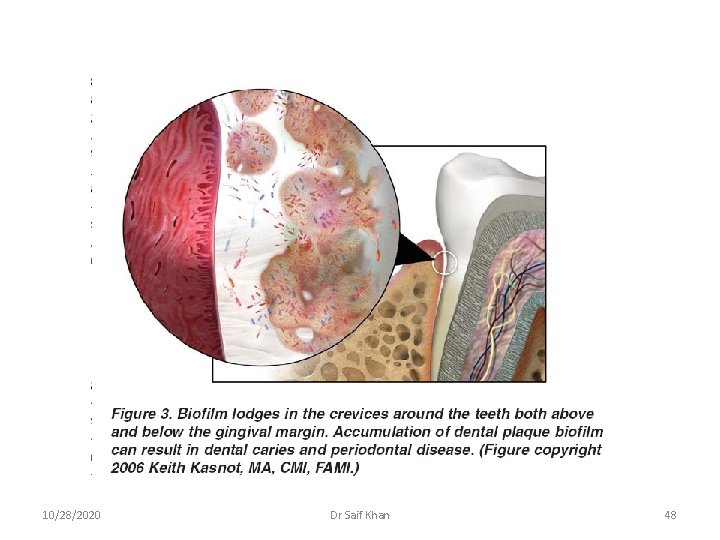
10/28/2020 Dr Saif Khan 48

Physiological properties of Dental Plaque q The transition from Gm+ve to Gm-ve microorganism observed in structural development of plaque is paralled by physiologic transition in the developing plaque q Early colonizers use oxygen and lower redox potential of the environment which then favors growth of anaerobic species 10/28/2020 Dr Saif Khan 49

q Early colonizers use sugar as energy source and saliva as carbon source q Bacteria which predominate in mature plaque or late colonizers are Asaccharolytic and use amino acids and small peptides as energy source q Lactate and formate are by products of metabolism of streptococci and actinomycetes may be used by other microorganism 10/28/2020 Dr Saif Khan 50

q Hemin a breakdown product from host hemoglobin is important in metabolism of P gingivalis q Increase in steroid hormone is associated with increase in proportions of Prevotella intermedia in subgingival plaque 10/28/2020 Dr Saif Khan 51
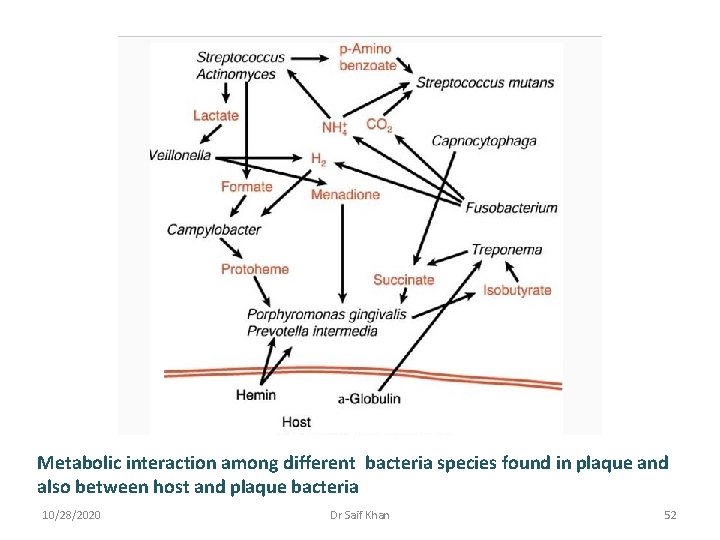
Metabolic interaction among different bacteria species found in plaque and also between host and plaque bacteria 10/28/2020 Dr Saif Khan 52

Ecological plaque Hypothesis q Given by Marsh & Co- Workers in 1990 q Total amount of dental Plaque and the specific microbial composition of plaque contribute to transition from health to disease q Health –associated dental plaque microflora is considered to be relatively stable overtime and in state of dynamic equilibrium or “ microbial homeostasis ” 10/28/2020 Dr Saif Khan 53

Ecological plaque Hypothesis q Change in nutrient status of a periodontal pocket or q Chemical and physical changes to habitat can lead over growth of pathogens Eg: Increase in GCF flow can lead to enrichment of proteolytic species(periopathogens) by providing essential nutrients such as heme containing molecules 10/28/2020 Dr Saif Khan 54
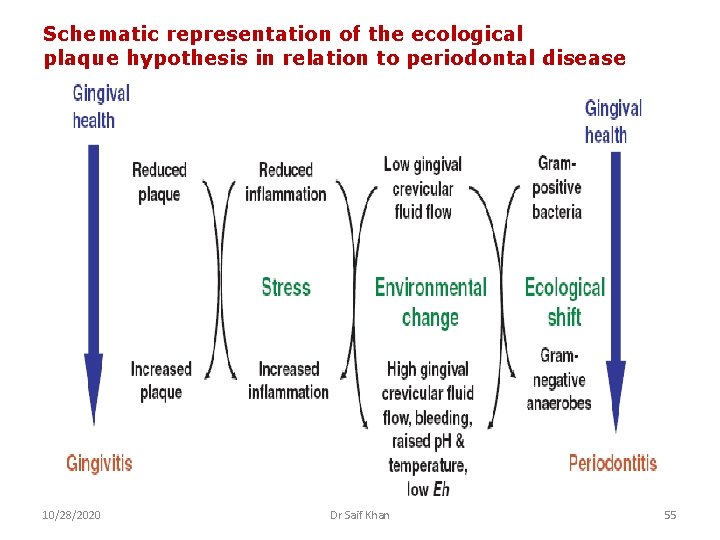
Schematic representation of the ecological plaque hypothesis in relation to periodontal disease 10/28/2020 Dr Saif Khan 55
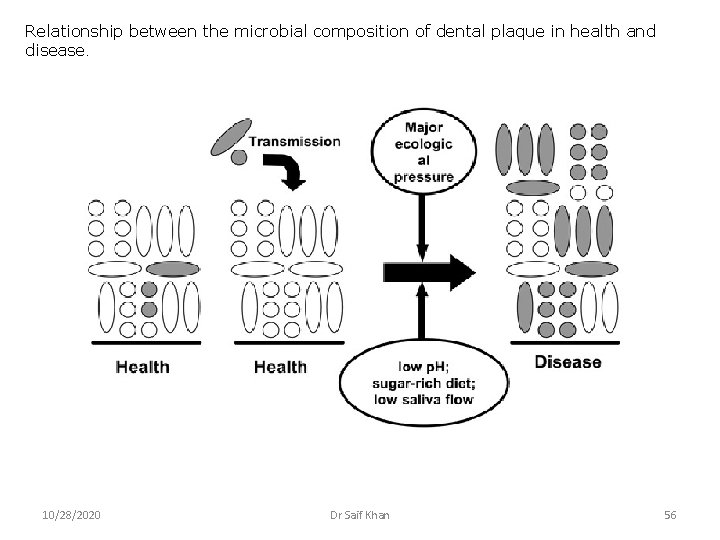
Relationship between the microbial composition of dental plaque in health and disease. 10/28/2020 Dr Saif Khan 56

Non- specific plaque hypothesis q Periodontal disease results from elaboration of noxious products from entire plaque flora q Large amount of plaque produces large amount of noxious product that would overwhelm host’s defense 10/28/2020 Dr Saif Khan 57

q Control of periodontal disease depend on control of amount of plaque deposit q The current standard treatment of periodontitis still focuses on the removal of plaque and its product founded on non-specific plaque hypothesis 10/28/2020 Dr Saif Khan 58

Non-specific plaque hypothesis has been discarded because q Some individuals with considerable amount of plaque and calculus as well as gingivitis never developed destructive periodontitis q Individuals with periodontitis demonstrated considerable site specificity in pattern of disease q Individuals with very less plaque developed destructive periodontal disease as in Aggressive periodontitis 10/28/2020 Dr Saif Khan 59

Specific plaque Hypothesis q States that only certain plaque is pathogenic q And its pathogenecity depends on presence of or increase in specific microorganism 10/28/2020 Dr Saif Khan 60

Plaque harboring specific bacterial pathogen results in periodontal disease because these organism produce substance that mediate the destruction of host tissue Eg: A actinomycetemcomitans as pathogen in localized aggressive periodontitis 10/28/2020 Dr Saif Khan 61

Specific Bacterial behaviour in Biofilm: Antibiotic resistance q Microorganisms in biofilm are 1000 to 1500 times more resistant to antibiotics than in their planktonic stage q The mechanism of this increased resistance differs from species to species, from antibiotic to antibiotic, and for biofilm growing in different habitats 10/28/2020 Dr Saif Khan 62

Resistance of bacteria to antibiotics is affected by their • • • Nutritional status Growth rate Temparature p. H Prior exposure to subeffective concentration of anti microbial agents 10/28/2020 Dr Saif Khan 63

q. Also slower growth of bacterial species in biofilm is another important mechanism of antibiotic resistance q. Biofilm matrix although not significant barrier in itself to diffusion of antibiotics but have certain properties to resist diffusion q. Biofilm act as ion-exchange resin removing antibiotics from solution 10/28/2020 Dr Saif Khan 64

q. Also extracellular enzymes such as β lactamases, formaldehyde lyase and formaldehyde dehydrogenase may become trapped and concentrated in the extracellular matrix thus inactivating some antibiotics(especially positive charged hydrophilic antibiotics) 10/28/2020 Dr Saif Khan 65

q Some antibiotics such as Macrolide which are positive charged but hydrophobic are unaffected by this process 10/28/2020 Dr Saif Khan 66

“Super-resistant” bacteria have been identified within a biofilm and these cells have multidrugresistant pump that can extrude antimicrobials from the cell 10/28/2020 Dr Saif Khan 67

Quorum Sensing q Bacteria in biofilm communicate with each other q This involves the regulation of expression of specific genes through accumulation of signalling compounds that mediate intercellular communication q When these signalling compounds reach a threshold level(quorum cell density) gene expression is activated 10/28/2020 Dr Saif Khan 68

• Quorum sensing seems to play a role in expressing genes for antibiotic resistance and encouraging growth of beneficial species to the biofilm and discouraging the growth of competitors 10/28/2020 Dr Saif Khan 69
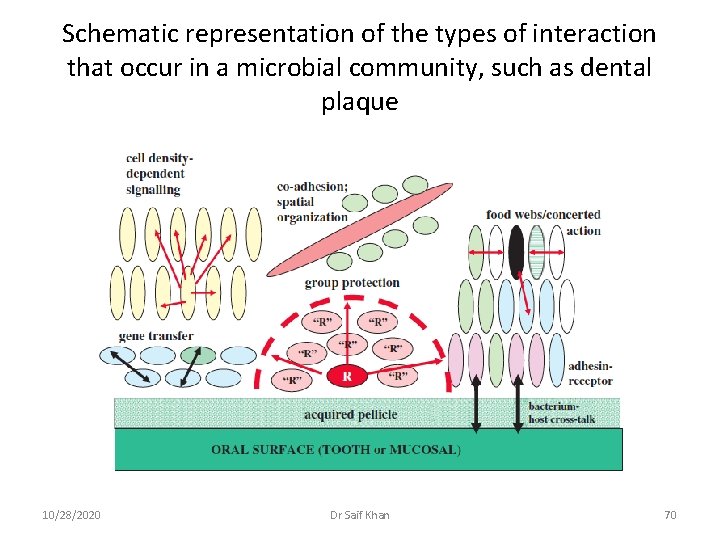
Schematic representation of the types of interaction that occur in a microbial community, such as dental plaque 10/28/2020 Dr Saif Khan 70

High density of bacterial cells in biofilm facilitates the exchange of genetic information among cell of the same species and genera through; 1. Conjugation (sex pilus) 2. Transformation (movement of small pieces of DNA from enviroment into bacterial chromosome) 3. Plasmid tranfer 4. Transposon transfer (DNA sequence which can change sequence within the genome) 10/28/2020 Dr Saif Khan 71
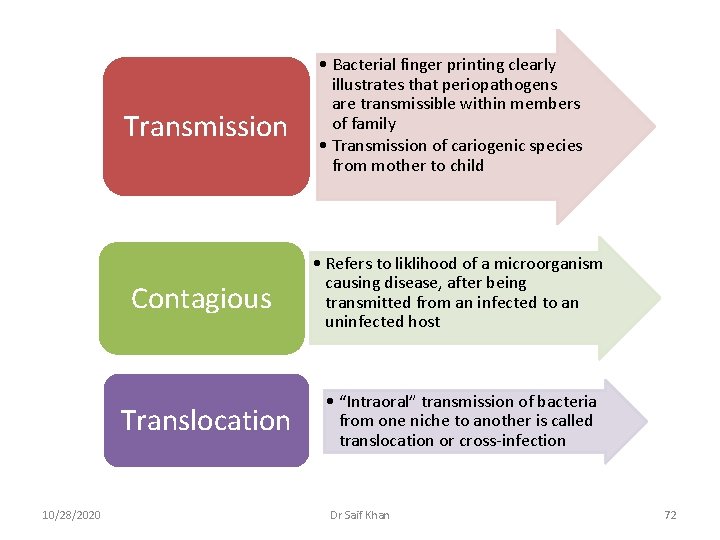
Transmission 10/28/2020 • Bacterial finger printing clearly illustrates that periopathogens are transmissible within members of family • Transmission of cariogenic species from mother to child Contagious • Refers to liklihood of a microorganism causing disease, after being transmitted from an infected to an uninfected host Translocation • “Intraoral” transmission of bacteria from one niche to another is called translocation or cross-infection Dr Saif Khan 72

Translocation and Mechanical Debridement • To reduce chance of intraoral transmission, one stage, Full mouth disinfection has been introduced by Leuven group in the 1990 s • This strategy attempts to eradicate, or atleast suppress, periopathogens in short time not only from the periodontal pockets, but also from all their intraoral habitats(mucous membrane, tongue, and saliva) 10/28/2020 Dr Saif Khan 73

One stage, Full mouth disinfection q Full mouth scaling and root planning within 24 hrs to reduce number of subgingival pathogenic organisms q Subgingival irrigation of all pockets with 1% chlorhexidine gel to kill remaining bacteria q Tongue brushing with an antiseptic to suppress the bacteria in the niche q Mouth rinsing with antiseptic to reduce the bacteria in the saliva and on the tonsil 10/28/2020 Dr Saif Khan 74

Benefits of the One stage, Full mouth disinfection • Pocket depth reduction • Gain in clinical attachment level • Microbiologic shift 10/28/2020 Dr Saif Khan 75

The current concept on etiology of Periodontitis considers three factors that determine whether active periodontitis will occur 1. Susceptible Host 2. Presence of a Pathogenic species 3. Absence or small numbers of beneficial species 10/28/2020 Dr Saif Khan 76
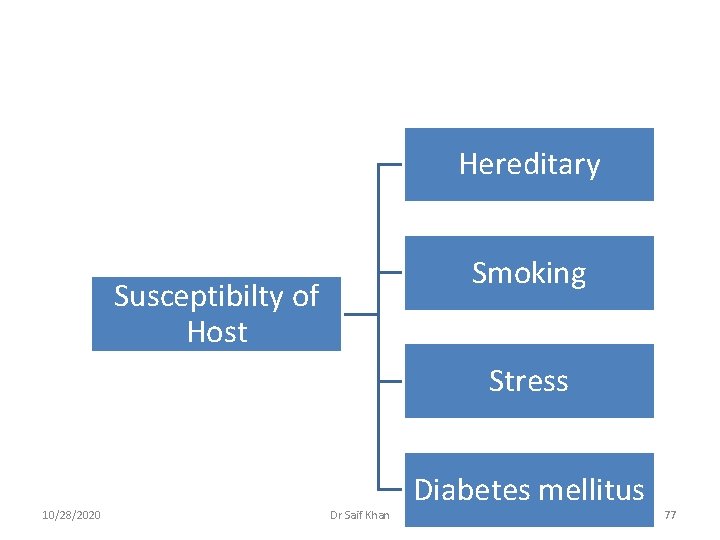
Hereditary Smoking Susceptibilty of Host Stress 10/28/2020 Dr Saif Khan Diabetes mellitus 77
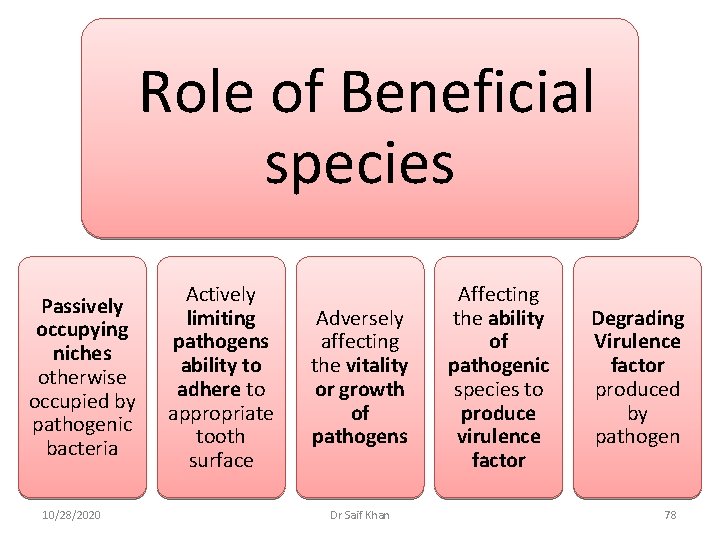
Role of Beneficial species Passively occupying niches otherwise occupied by pathogenic bacteria 10/28/2020 Actively limiting pathogens ability to adhere to appropriate tooth surface Adversely affecting the vitality or growth of pathogens Dr Saif Khan Affecting the ability of pathogenic species to produce virulence factor Degrading Virulence factor produced by pathogen 78

Beneficial species such as S sangius, Veillonella parvula and C ochreus are typically found in higher number at periodontal sites with no attachment loss where as lower in number where there is active periodontal destruction 10/28/2020 Dr Saif Khan 79

Criteria for identification of Periodontal pathogen Kochs Postulates Given by Robert Koch as classic criteria by which microorganims are judged causative v Must be routinely isolated from diseased individual v Must be grown in pure culture in laboratory v Must produce similar disease when inoculated in susceptible laboratory animal v Must be recovered from lesions in diseased laboratory animal Streptococcus mutans has been shown to follow Koch’s postulate as an etiologic agent of dental caries 10/28/2020 Dr Saif Khan 80

koch’s criteria are difficult to apply in periodontal disease because of 3 reasons 1. Inability to culture all the microorganism that have been associated with disease (eg: spirochetes) 2. The difficulties inherent in defining and culturing sites of active disease 3. Lack of good animal model for study of Periodontitis 10/28/2020 Dr Saif Khan 81

Socransky criteria • Proposed criteria by which periodontal microorganism may be judged to be potential pathogens 1. Must be associated with disease, as evident by increase in the number of organisms at diseased sites 2. Must be eliminated or decreased in sites that demonstrate clinical resolution of disease with treatment 3. Must demonstrate a host response, in the form of an alteration in the host cellular or humoral immune response 4. Must be capable of causing disease in experimental animal model. 5. Must demonstrate virulence factors responsible for enabling the microorganism to cause destruction of periodontal tissue 10/28/2020 Dr Saif Khan 82

Microorganism associated with specific periodontal disease q Fewer coccal cells and more motile rods and spirochetes are found in diseased state than healthy sites by means of phase-contrast or dark-field microscopy q Almost all periodontal pathogens except Campylobacter rectus are immobile q Bacteria from healthy periodontal sites consists of gram +ve facultative rods and cocci 10/28/2020 Dr Saif Khan 83

Periodontal Health q Gm+ve facultative species of genera Streptococcus and Actinomycetes(S sangius, S mitis, A viscosus, A naeslundi) q Small proportions of Gm-ve species are also found (P intermedia, F nucleatum, Capnocytophaga, C ochareus) 10/28/2020 Dr Saif Khan 84

Gingivitis Micro biota of Dental –plaque induced gingivitis(chronic gingivitis) consists of equal proportions of § Gm+ve(56%) & Gm-ve(44%) species § Facultative(59%) & anaerobic(51%) microorganisms § Predominant Gm+ve microorganisms are S sangius, S mitis, S intermedius, S oralis, A viscosus, A naeslundii and P micros 10/28/2020 Dr Saif Khan 85

The predominant Gm-ve microorganisms are F nucleatum, P intermedia, V parvula as well as Haemophilus, Campylobacter and Capnocytophaga Pregnancy associated gingivitis is acute inflammation of gingivae associatedin pregnancy. There is increase in steroid hormones in crevicular fluid and dramatic increase in Prevotella intermedia which uses steroid as growth factor 10/28/2020 Dr Saif Khan 86

Chronic periodontitis q Microscopic examination of plaque from sites with chronic gingivitis consistently revealed elevated proportions of spirochetes q Cultivation of plaque microorganisms from sites chronic periodontitis have reveal high percentages of anaerobic(90%) and gram negative (75%) bacterial species 10/28/2020 Dr Saif Khan 87

q Bacteria most often cultivated include P. gingivalis , T. forsythus, C rectus, E corrodens, F. nucleatum, A actinomycetemcomitans, P micros, Treponema and Eubacterium q C rectus, P gingivalis, P intermedia, F nucleatum & T forsythia are elevated in active sites 10/28/2020 Dr Saif Khan 88

v Detectable levels of P gingivalis, P intermedia, T forsythia, C rectus and A actinomycetemcomitans are associated with disease progression and their elimination by therapy is associated with improve clinical outcome 10/28/2020 Dr Saif Khan 89

Also recent studies have documented association between chronic periodontitis and viral microrganisms of Herpes group, most notably Epstein barr virus-1 (EBV-1) and Human cytomegalovirus (HCMV) are associated with putative pathogens P gingivalis, T forsythia, P intermedia and T denticola 10/28/2020 Dr Saif Khan 90
Microbial Shift during disease Gm +ve to Gm -ve Cocci Rods Spirochetes Nonmotile to Obligate anaerobes Facultative anaerobes 10/28/2020 Dr Saif Khan 91

Localized Aggressive Periodontitis q A actinomycetemcomitans compose of 90% of total cultivable microbiota q P gingivalis, E corrodens, C rectus, F nucleatum, B capillus, Eubacterium brachy, Capnocytophaga sp and Spirochetes are also found in significant levels q Herpes viruses, including EBV-1 and HCMV have been associated with LAP 10/28/2020 Dr Saif Khan 92

Necrotizing Periodontal disease q Microbiologic studies indicate high levels of Prevotella intermedia and especially Spirochetes in NUG lesions q Spirochetes penetrate deep into necrotic tissue and unaffected connective tissue 10/28/2020 Dr Saif Khan 93

Periimplantitis q Inflammatory process affecting the tissue around an already osseointegrated implant resulting in loss of supporting bone q Healthy periimplant pockets are characterised by high proportions of coccoid cells, low anaerobic/aerobic ratio, low number of gram anaerobic species and low detection frequency for periodontal pathogens 10/28/2020 Dr Saif Khan 94

• Species such as A actinomycetencomitans, P gingivalis, T forsythia, P micros, C rectus, Fusobacterium and Capnocytophaga are isolated from failing sites but also can be detected from healthy sites • Other species such as Pseudomonas aeruginosa, enterobacteriaceae, Candida albicans, Staphlycocci are also detected around implants 10/28/2020 Dr Saif Khan 95

Microbial specificity in Periodontitis • There is no “black-or-white” situation; most pathogens might be present, but do not necessarily have to be present for specific form of periodontitis • Microbial composition can not be used to differentiate different forms of periodontal disease 10/28/2020 Dr Saif Khan 96

Most pathogens can also be detected in healthy subjects with frequencies ranging from 10% to 85%. This automatically reduces the specificity of microbiologic testing in periodontology 10/28/2020 Dr Saif Khan 97
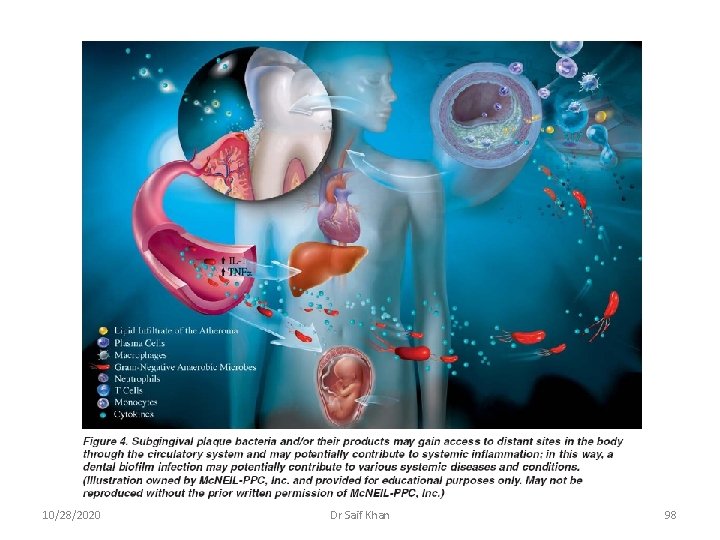
10/28/2020 Dr Saif Khan 98
- Slides: 98