Periodontal medicine When you have eliminated the impossible

Periodontal medicine

“When you have eliminated the impossible, whatever remains, however improbable, must be the truth!!”

FOCAL INFECTION ACUTE PHASE REACTANTS CARDIOVASCULAR DISEASE DIABETES PRETERM LOW BIRTH WEIGHT RESPIRATORY DISEASES RHEUMATOID ARTHRITIS OBESITY

DEFINITION Offenbacher (1996) defined periodontal medicine as a rapidly emerging branch of periodontology focusing on the wealth of new data establishing a strong relationship between periodontal health or disease and systemic health or disease This establishes a two way relationship!! The impact of oral infection on systemic health.

Because of : - Extensive microbial plaques Chronic nature Exuberant local and systemic host response to the microbial assault HYPOTHESIS

History… Ancient Civilizations – Hebrew Book – Sefer haolsmot o maaseh tovia Hippocrates described a patient of ‘rheumatism’ whose arthritis was cured by the extraction of a tooth. Roman physician Galen (166 -201 A. D. ) – Head is the source of all ills. In 1768, Thomas Berdmore in A Treatise on the disorders and deformities of the teeth and gums described the relation between teeth and the entire body

ORAL SEPSIS …. Modern times Miller, a dentist working with Koch published an article titled “The human mouth as a focus of Infection” (1891) “Bacterial infections can produce a metastatic abscess, thus periodontal disease, tonsils and uterus formed the foci of infection” William Hunter 1900 – “oral sepsis as a cause of disease” 1902 – Colyer suggested “Better no teeth than septic ones”. Charles Mayo of Mayo Clinic advocated the Focal infection theory

ACUTE PHASE REACTANTS Host response to variety of injuries like bacterial, viral or parasitic infections, mechanical or chemical trauma, ischemic necrosis or malignant growth. Macrophage is the cell responsible for initiating the response. Characteristic features. . fever, neutrophilia, increased (muscle) protein catabolism, activation of the complement and coagulation pathways, hormonal changes, and induction of acute-phase proteins
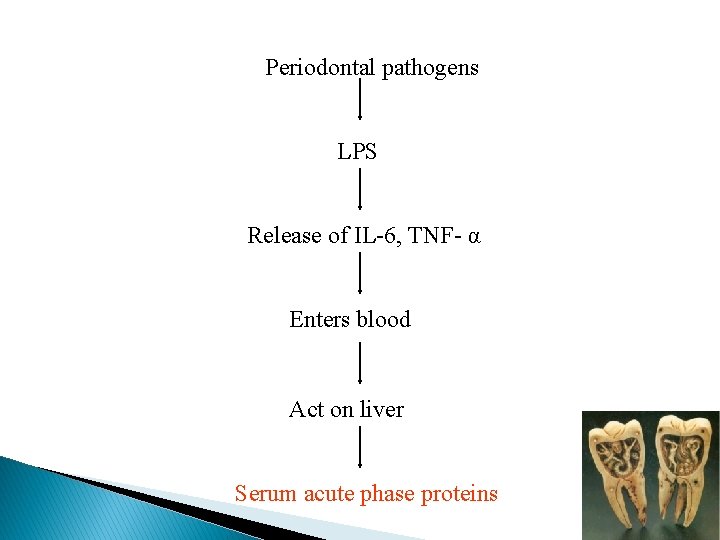
Periodontal pathogens LPS Release of IL-6, TNF- α Enters blood Act on liver Serum acute phase proteins
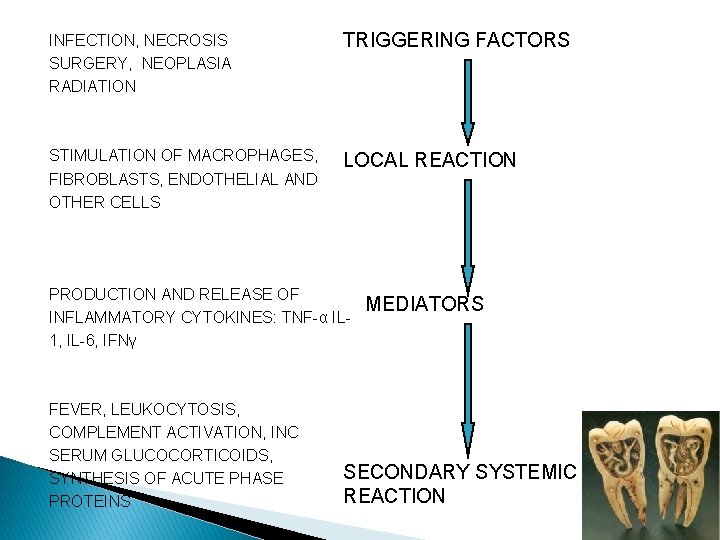
INFECTION, NECROSIS SURGERY, NEOPLASIA RADIATION TRIGGERING FACTORS STIMULATION OF MACROPHAGES, FIBROBLASTS, ENDOTHELIAL AND OTHER CELLS LOCAL REACTION PRODUCTION AND RELEASE OF INFLAMMATORY CYTOKINES: TNF-α IL 1, IL-6, IFNγ FEVER, LEUKOCYTOSIS, COMPLEMENT ACTIVATION, INC SERUM GLUCOCORTICOIDS, SYNTHESIS OF ACUTE PHASE PROTEINS MEDIATORS SECONDARY SYSTEMIC REACTION


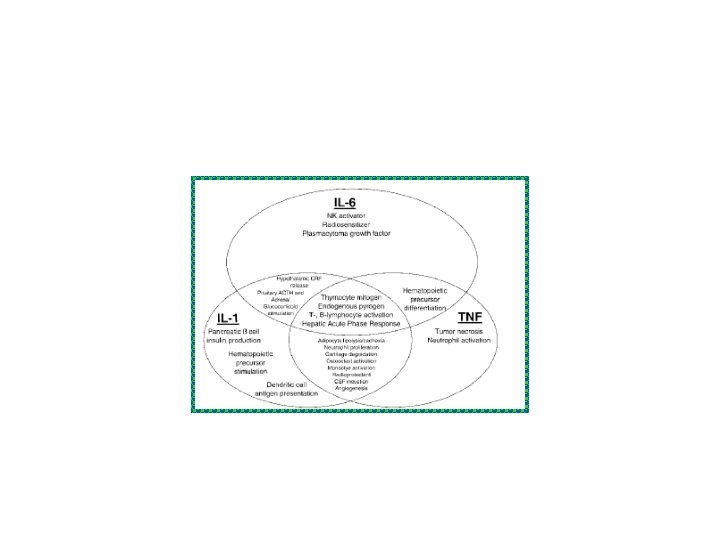


Acute phase proteins Strong … • C reactive protein • Serum Amyloid A • alpha 2 macroglobulin C reactive protein Serum Amyloid A Complement C 3 Moderate • haptoglobin • Fibrinogen • Alpha 1 anti trypsin Weak • Complement C 3 • Ceruloplasmin Type 1(IL-1) Type 2(IL-6) Fibrinogen Haptoglobulin Anti chymotrypsin
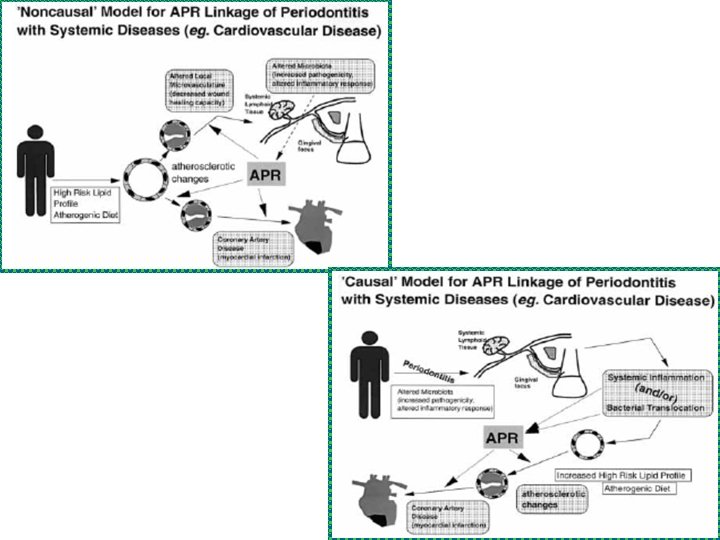
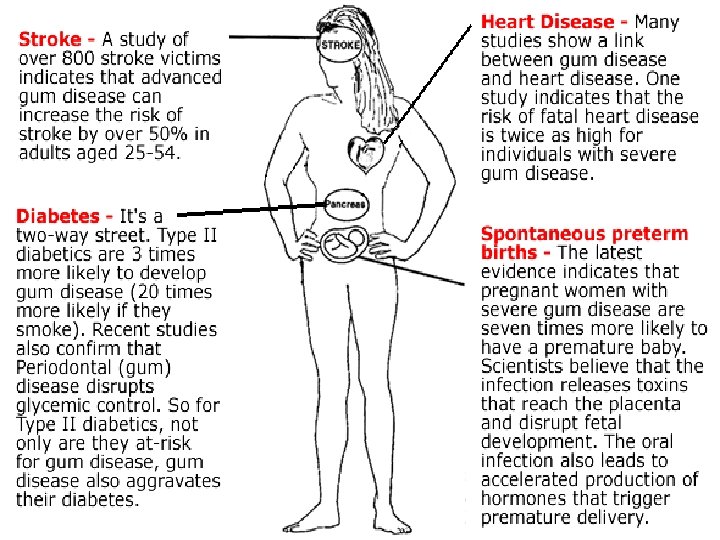

PERIODONTAL DISEASE AND CVD WHO statistics indicate that in 1995, CVD were responsible for 20% of deaths worldwide, numbering 14 million people. Principle cause of death in developed countries – accounts for 50% of deaths while in developing countries accounting for 16% of deaths.

CVD and Atherosclerosis – A progressive degenerative condition involving large and medium sized arteries. Atheromatous plaques composed of lysed cells, cholesterol ester crystals, foam cells occlude the artery or cause infarction …
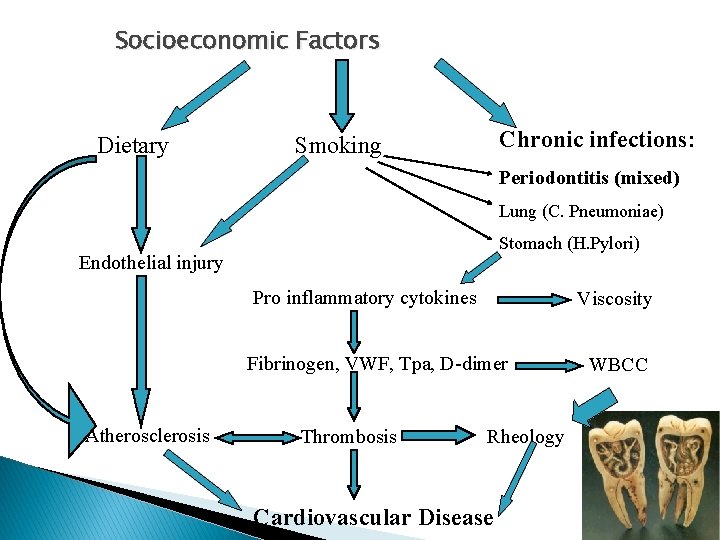
Socioeconomic Factors Dietary Chronic infections: Smoking Periodontitis (mixed) Lung (C. Pneumoniae) Stomach (H. Pylori) Endothelial injury Pro inflammatory cytokines Viscosity Fibrinogen, VWF, Tpa, D-dimer Atherosclerosis Thrombosis Rheology Cardiovascular Disease WBCC
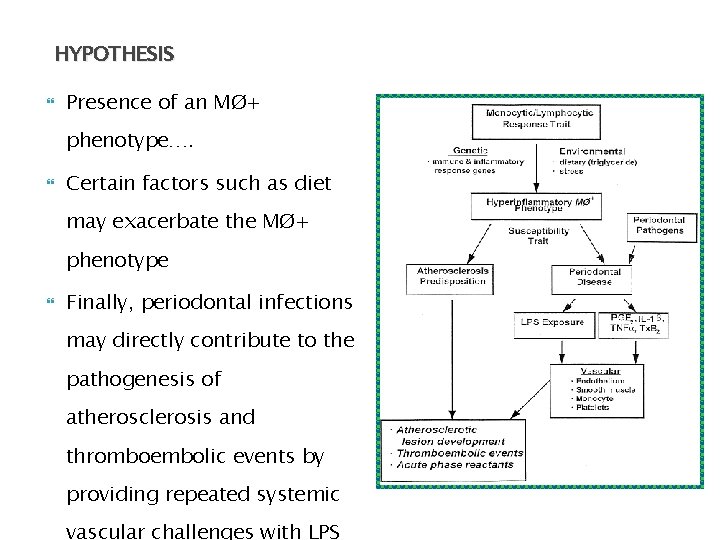
HYPOTHESIS Presence of an MØ+ phenotype…. Certain factors such as diet may exacerbate the MØ+ phenotype Finally, periodontal infections may directly contribute to the pathogenesis of atherosclerosis and thromboembolic events by providing repeated systemic vascular challenges with LPS

Association between CVD and Periodontitis as measured in M. I patients, patients with Stroke and CHD…. Positive. . Mattilla and Neiminen – 1989 De. Stefano – 1993 Beck - JP 1996 Grau and Buggle - 1997

MECHANISMS Factor VIII activity and its cofactors (Von Willebrand factor antigen) – were associated with poor dental status, linking chronic dental infection with increased thrombogenicity. Mattila - 1997 Individuals with periodontitis had significantly elevated leukocyte counts and circulating fibrinogen. Lowe GD -1992 Platelets bind to strains of Strep. Sanguis, a common component of supragingival plaque and result in thrombus formation. (PAAP) • Herzberg et al 1996

MECHANISMS Infection produces a hypercoagulable state and increased blood viscosity; INFECTION LIPOPOLYSACCHARIDES INFLAMMATORY MEDIATORS INCREASED BLOOD VISCOSITY CHANGES IN TUNICA MEDIA AND ADVENTITIA ATHEROSCLEROSIS ARTERIAL THICKENING
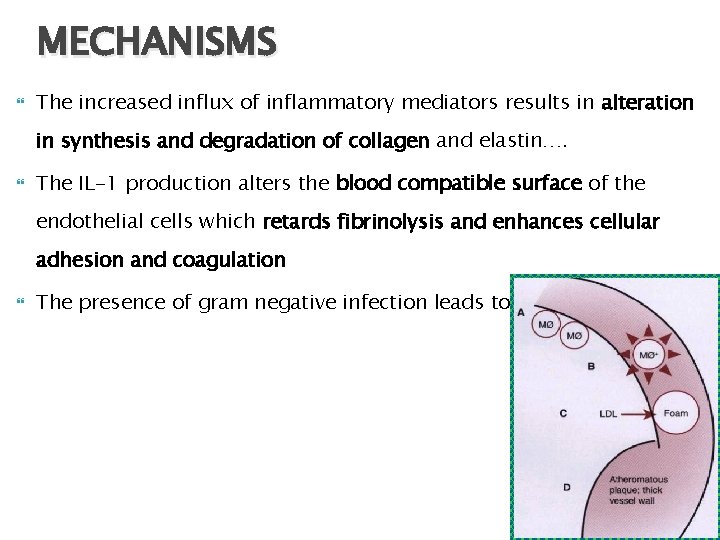
MECHANISMS The increased influx of inflammatory mediators results in alteration in synthesis and degradation of collagen and elastin…. The IL-1 production alters the blood compatible surface of the endothelial cells which retards fibrinolysis and enhances cellular adhesion and coagulation The presence of gram negative infection leads to bacteremia.
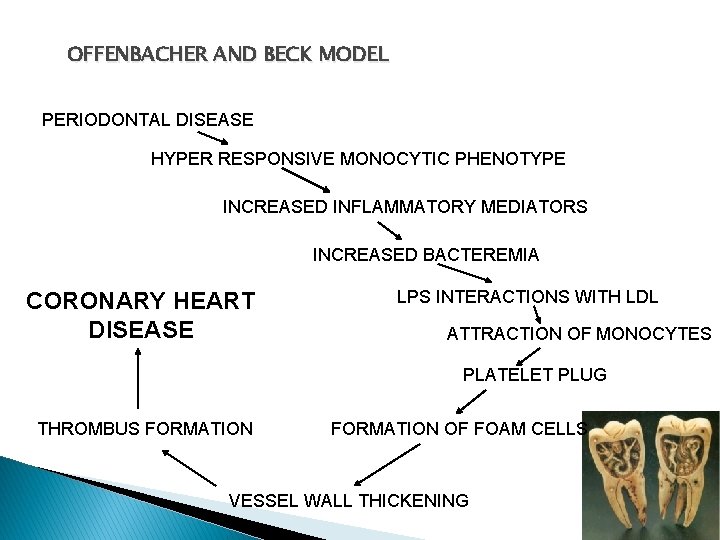
OFFENBACHER AND BECK MODEL PERIODONTAL DISEASE HYPER RESPONSIVE MONOCYTIC PHENOTYPE INCREASED INFLAMMATORY MEDIATORS INCREASED BACTEREMIA CORONARY HEART DISEASE LPS INTERACTIONS WITH LDL ATTRACTION OF MONOCYTES PLATELET PLUG THROMBUS FORMATION OF FOAM CELLS VESSEL WALL THICKENING

Scannapieco F, Bush R &Paju S ’ 03 systematic review …. 1, 526 articles scanned … 31 ONLY modest association Several studies showed no association Absence of a standard definition & measures Large scale epidemiologic studies and intervention trials required….

Summary Periodontal and cardiovascular diseases share many risk factors. The chronicity of periodontal infections provides a rich source of microbial and host products. Two main processes providing a causative link include; lipopolysaccharide and monocyte-related responses.

PERIODONTITIS AND DIABETES Pathogenic aspects!! 17 million people affected by Diabetes Periodontitis recognized as the 6 th major complication (Loe H 1993) TYPE I and TYPE II; Impaired glucose tolerance, gestational diabetes and drug or chemical induced diabetes. Characterized by hyperglycemia, hyperlipidemia and assoc complications. 5 classic major complications include; microangiopathy, nephropathy, neuropathy, macrovascular disease and delayed wound healing
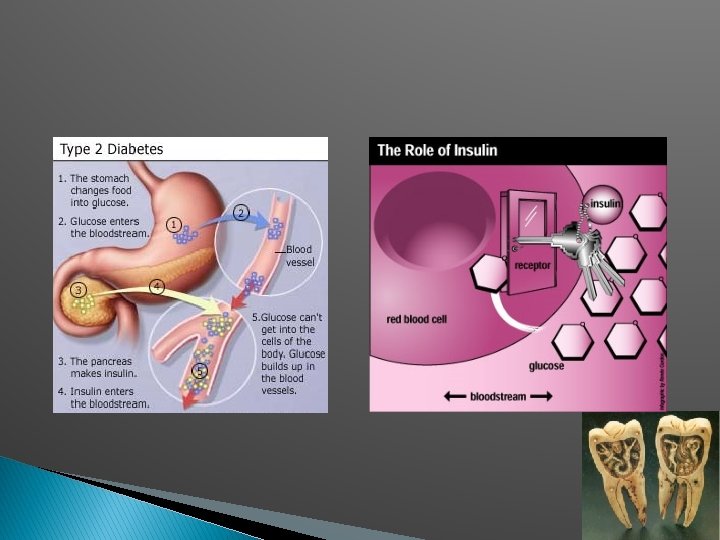

� � Hypothesis – severe periodontitis in persons with NIDDM increases the conc of glycated Hb in serum. Data were collected from Gila river indian community – Pima tribe – prevalence of 50% - highest reported in the world. Poor glycemic control defined – occurrence of glycated Hb of 9% or more at follow up. Results suggested that severe periodontitis at baseline was assoc with increased risk of having poor glycemic control at follow up 2 or more years later. � Shlossman – JADA 1990 � Elimination of periodontal inflammation. � Grossi’ 96…. Effect of periodontal treatment on glycated Hb levels

hyperglycemia and its Direct consequences Increased production of sorbitol and fructose by the enzyme aldose reductase. Polymorphisms. . Aldose reductase gene (Engerman’ 93) Inhibitors. . No effects on complications Diacylglycerol and it’s importance …production of protein kinase Cbeta (Koya’ 97)

Indirect consequences Nonenzymatic glycation and oxidation, the Schiff bases and Amadori products. (reversible) The best-known of these products is glycosylated hemoglobin A 1 c whose measurement is used as a clinical barometer of glucose control over weeks to months Complex rearrangement leads to the formation of Advanced Glycation End products (AGE). These include carboxymethyl (lysine), pentosidine, pyralline and methyglyoxal. Recent investigations reveal that AGEs can also form in response to an inflammatory milieu (Anderson 1999)

Indirect consequences � AGEs result in significant alteration of normal cellular composition and structure. � Alters the function of ECM components, � Affect the collagen stability and vascular integrity. � Monocytes, macrophages and endothelial cells possess high affinity receptors for AGEs. � the AGEs have a direct effect on the cell surfaces. RAGE…. STRUCTURE � Binding sites for AGEs…. . RAGE � Consists of a 332 amino acid region containing a “V” type domain and two “C” domains followed by hydrophobic transmembrane and finally a highly charged cytosolic tail of 42 amino acids, essential for signal transduction.

EFFECTS OF RAGE � ü ü Endothelial cells: � Smooth Muscle Cells Present at low levels, inc. on cellular perturbation ü Binding lead to increased migration and activation, which may have Increased permeability of the endothelial lining important implications in vascular ü Increased expression of VCAM � Mononuclear Phagocytes: � increased chemotaxis of the macrophages. Fibroblasts: ü Binding led to reduced production of ü ü increased release of TNF-α perturbations and injury. Type I collagen m. RNA

Studies of RAGE Schmidt (1996) demonstrated that AGEs accumulate in human diabetic gingiva as compared to nondiabetics. Lalla (1998) demonstrated that diabetic mice injected with P. gingivalis strains showed more periodontal destruction than non diabetic mice The diabetic patients showed greater periodontal destruction as compared to non diabetics. (Mealey et al, Genco et al) Thus suggesting that accumulation of AGEs might play a role in pathogenesis of periodontal disease.
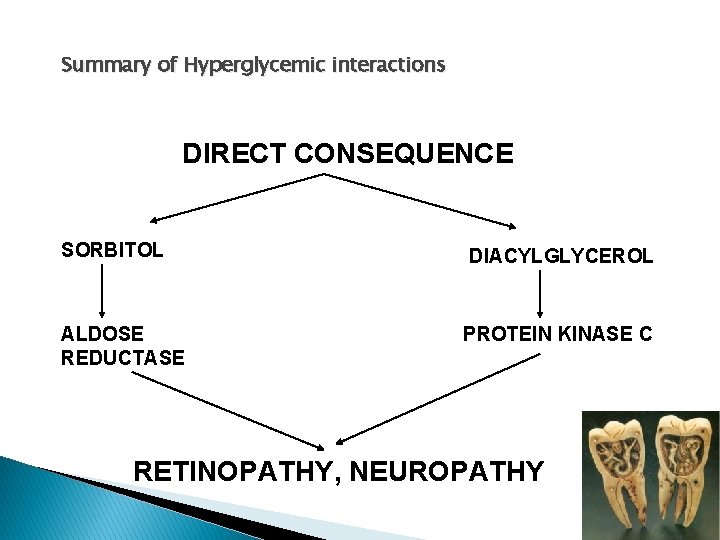
Summary of Hyperglycemic interactions DIRECT CONSEQUENCE SORBITOL DIACYLGLYCEROL ALDOSE REDUCTASE PROTEIN KINASE C RETINOPATHY, NEUROPATHY
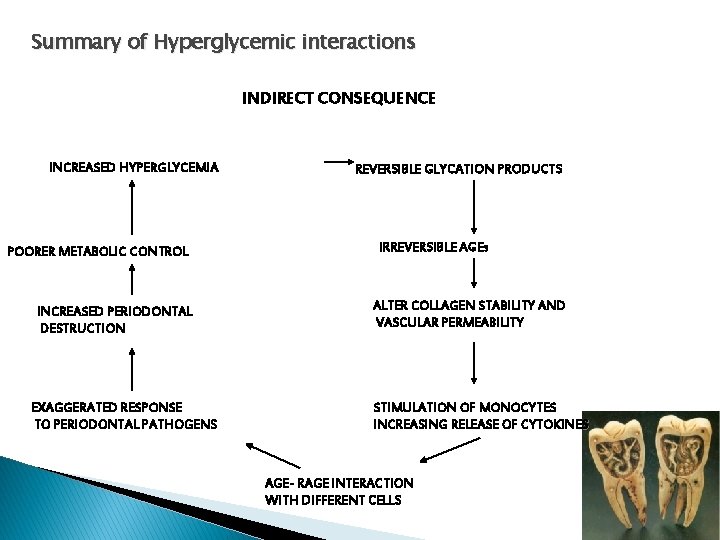
Summary of Hyperglycemic interactions INDIRECT CONSEQUENCE INCREASED HYPERGLYCEMIA POORER METABOLIC CONTROL INCREASED PERIODONTAL DESTRUCTION EXAGGERATED RESPONSE TO PERIODONTAL PATHOGENS REVERSIBLE GLYCATION PRODUCTS IRREVERSIBLE AGEs ALTER COLLAGEN STABILITY AND VASCULAR PERMEABILITY STIMULATION OF MONOCYTES INCREASING RELEASE OF CYTOKINES AGE- RAGE INTERACTION WITH DIFFERENT CELLS
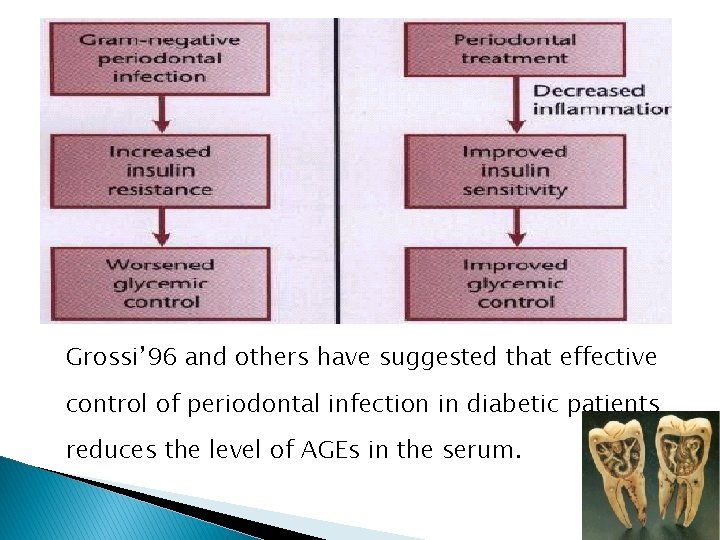
Grossi’ 96 and others have suggested that effective control of periodontal infection in diabetic patients reduces the level of AGEs in the serum.

DIABETES, PERIODONTITIS AND LIPID METABOLISM
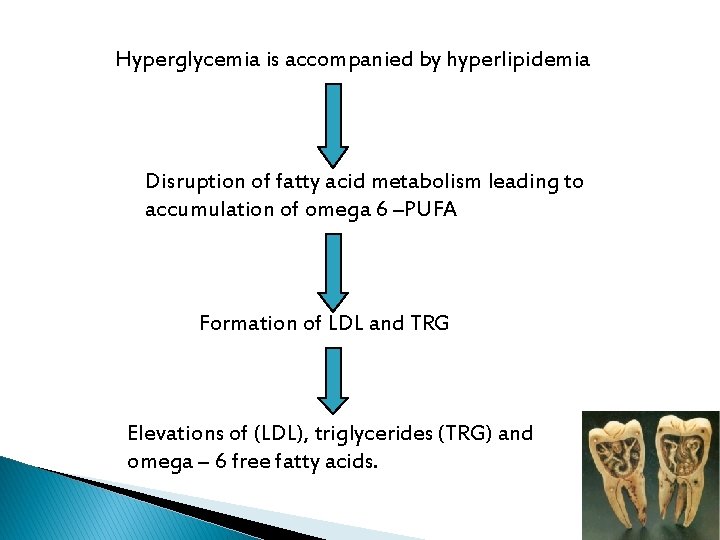
Hyperglycemia is accompanied by hyperlipidemia Disruption of fatty acid metabolism leading to accumulation of omega 6 –PUFA Formation of LDL and TRG Elevations of (LDL), triglycerides (TRG) and omega – 6 free fatty acids.

Conversion of PUFA to active metabolites is impaired because of reduced 6 -desaturase enzyme activity brought about by insulin deficiency. Present on the surface of the membrane of cells Pociot (1993), Offenbacher (1994), Yalda (1994) Salvi (1997 and 1998) have shown the existence of a hyper responsive monocytic phenotype which has been postulated to be related to hyperlipidemia

Periodontitis as a risk factor!! Earlier studies could not document a role of infection causing hyperlipidemia (Lopes 1990). Recent studies have documented a positive relationship between infection and hyperlipidemia Samra (1996) found that periodontal infections induced profound changes in the plasma concentration of cytokines and hormones leading to a catabolic state characterized by hypertriglyceridemia and lipid oxidation Casey (1993) demonstrated that chronic low level exposure to gram negative LPS could induce a similar response

� Also the increased presence of cytokines (for e. g. periodontal disease) stimulates the production of ACTH by modifying the hypothalamic-pituitary-adrenal axis resulting in elevated levels of (FFA), LDL and TRG – Gwosdow – 1990. � There is evidence of enhanced hepatic lipogenesis, increased adipose lipolysis, increased synthesis and reduced clearance of TRG. � There is reduction in the lipoprotein lipase activity
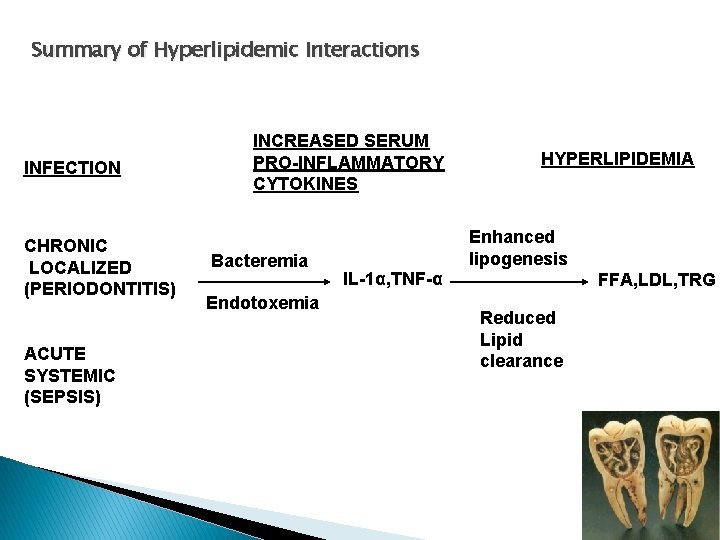
Summary of Hyperlipidemic Interactions INFECTION CHRONIC LOCALIZED (PERIODONTITIS) ACUTE SYSTEMIC (SEPSIS) INCREASED SERUM PRO-INFLAMMATORY CYTOKINES Bacteremia Endotoxemia IL-1α, TNF-α HYPERLIPIDEMIA Enhanced lipogenesis FFA, LDL, TRG Reduced Lipid clearance

IACOPINO AND CUTLER HYPOTHESIS PERIODONTAL DISEASE HYPER RESPONSIVE MONOCYTIC TRAIT ENHANCED PROD OF PRO-INFLAMMATORY CYTOKINES ELEVATION OF SERUM LIPID LEVELS INCREASED SEVERITY OF DIABETES
PRETERM LOW BIRTH WEIGHT AND PERIODONTAL DISEASE

WHAT IS PRETERM? NORMAL GESTATION TIME IS 40 WEEKS. Birth at Lesser than 37 weeks is called as preterm delivery WHAT IS LOW BIRTH WEIGHT? • International definition adopted at the 29 th WHA in 1976 is birth weight less than 2500 g is termed low birth weight

Preterm distribution

• Maternal age less than 17 or greater than 34 Surviving infants are at years increased risk of developing • Low socio-economic status : • Inadequate prenatal care • Drug abuse Respiratory distress syndrome • Malnutrition Anemia • Alcohol and tobacco use Jaundice • Diabetes • Genitourinary tract infections Mental retardation • Hypertension and multiple pregnancies. Cerebral palsy Impaired sight and hearing Intracranial hemorrhage Malnutrition Congestive heart failure Epilepsy Learning disabilities and impaired lung function. • In spite of this wide range of risk factors, about 25% of PLBW cases remain unexplained. This has motivated further research into the causes of PLBW.
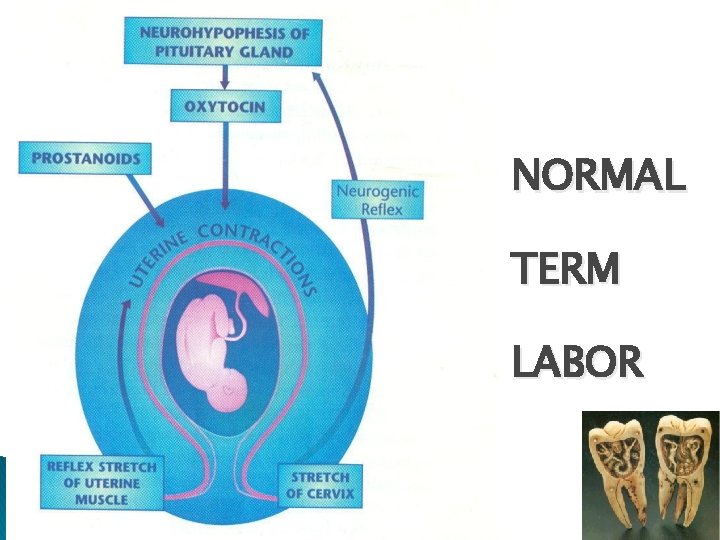
NORMAL TERM LABOR
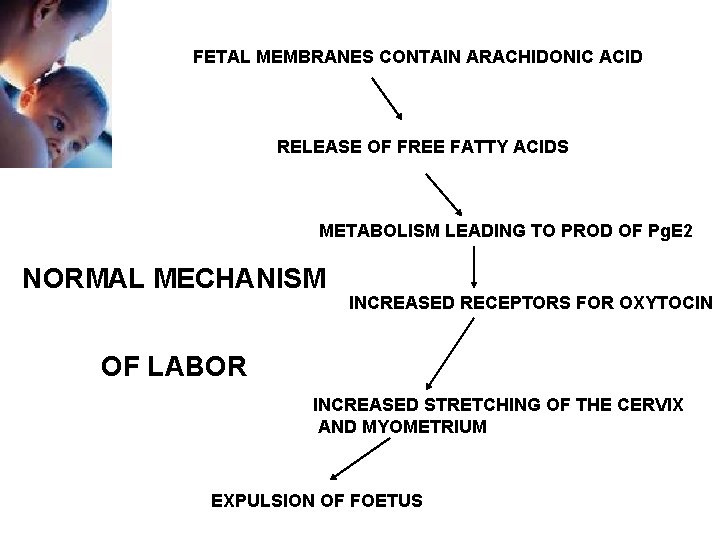
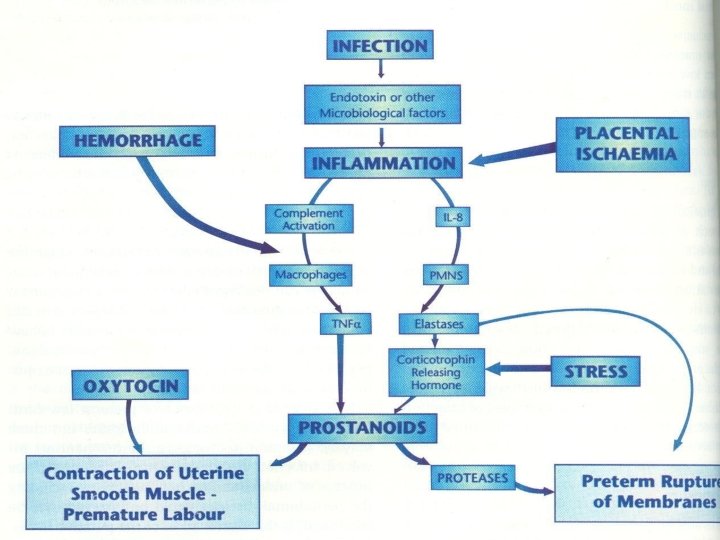
FETAL MEMBRANES CONTAIN ARACHIDONIC ACID RELEASE OF FREE FATTY ACIDS METABOLISM LEADING TO PROD OF Pg. E 2 NORMAL MECHANISM INCREASED RECEPTORS FOR OXYTOCIN OF LABOR INCREASED STRETCHING OF THE CERVIX AND MYOMETRIUM EXPULSION OF FOETUS
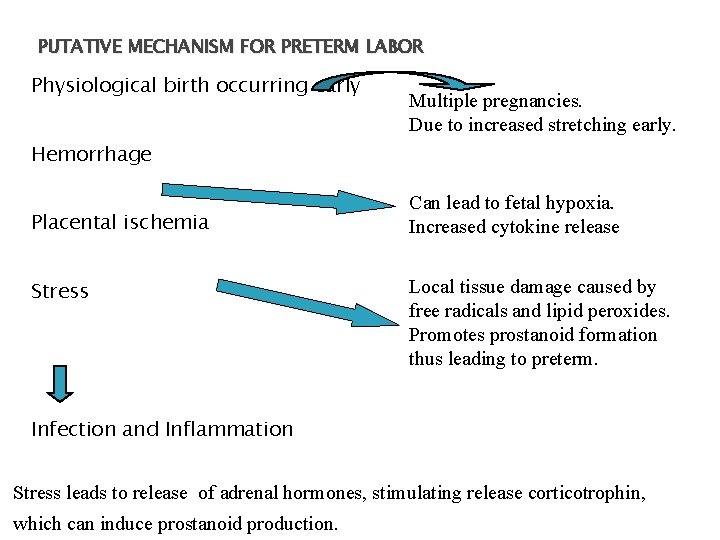
PUTATIVE MECHANISM FOR PRETERM LABOR Physiological birth occurring early Multiple pregnancies. Due to increased stretching early. Hemorrhage Placental ischemia Stress Can lead to fetal hypoxia. Increased cytokine release Local tissue damage caused by free radicals and lipid peroxides. Promotes prostanoid formation thus leading to preterm. Infection and Inflammation Stress leads to release of adrenal hormones, stimulating release corticotrophin, which can induce prostanoid production.
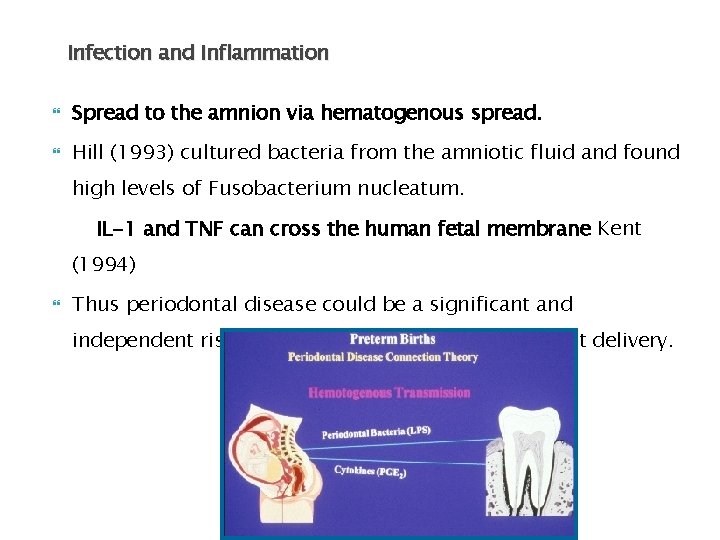
Infection and Inflammation Spread to the amnion via hematogenous spread. Hill (1993) cultured bacteria from the amniotic fluid and found high levels of Fusobacterium nucleatum. IL-1 and TNF can cross the human fetal membrane Kent (1994) Thus periodontal disease could be a significant and independent risk factor for pre term low birth weight delivery.

PLBW and Periodontal Infections � Galloway who in 1931 postulated that periodontal disease may provide sufficient infectious microbial challenge causing potentially harmful effects on the pregnant mother and developing fetus. � Studies by Collins et al, published in 1994 and 1995 showed that experimentally induced periodontitis in pregnant hamsters can retard fetal growth � Offenbacher and team….

They hypothesized that periodontal infections, which serve as resevoirs for Gram-negative anaerobic organisms, lipopolysaccharide (LPS, endotoxin), and inflammatory mediators including PGE 2 and TNF-α may pose a potential threat to the fetal-placental unit. The research team consisted of periodontists, obstetriciangynecologists and epidemiologists.

When no analysis tecniques were used to control for other variables, periodontal disease increased the risk for PLBW by almost 6 times. After adjusting for these variables, periodontal disease increased the risk of being a PLBW case by more than 7 fold. Although the sample size of this study was relatively small, the results indicated that periodontal disease contributed to more cases of PLBW than the use of either tobacco or alcohol.

18% of PLBW cases possibly due to periodontal diseases represents 45000 cases each year. Findings mean that all pregnant women should be given a comprehensive periodontal evaluation and all active periodontal lesions should be treated and controlled.

PERIODONTAL DISEASE AND RESPIRATORY DISEASE Lower respiratory infections were the 3 rd most common cause of death by 1990 (causing more than 4. 3 million deaths) COPD was the 6 th leading cause of mortality (causing 2. 2 million deaths) Harvard School of Public Health – Lancet 1997
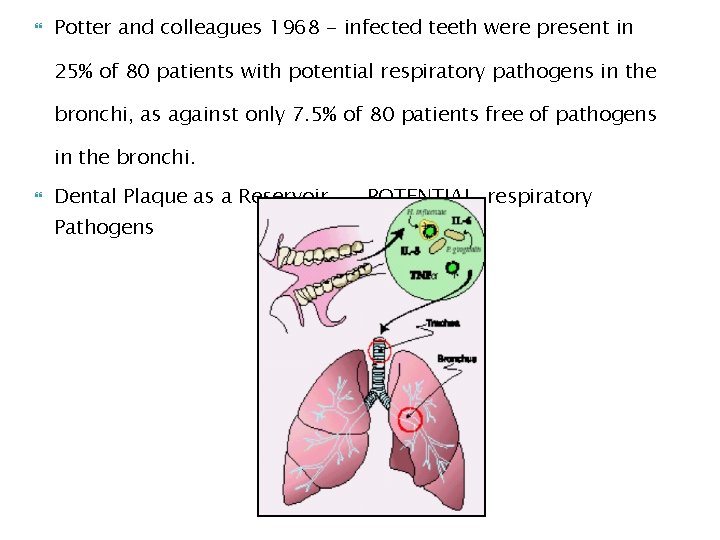
Potter and colleagues 1968 - infected teeth were present in 25% of 80 patients with potential respiratory pathogens in the bronchi, as against only 7. 5% of 80 patients free of pathogens in the bronchi. Dental Plaque as a Reservoir…. POTENTIAL respiratory Pathogens
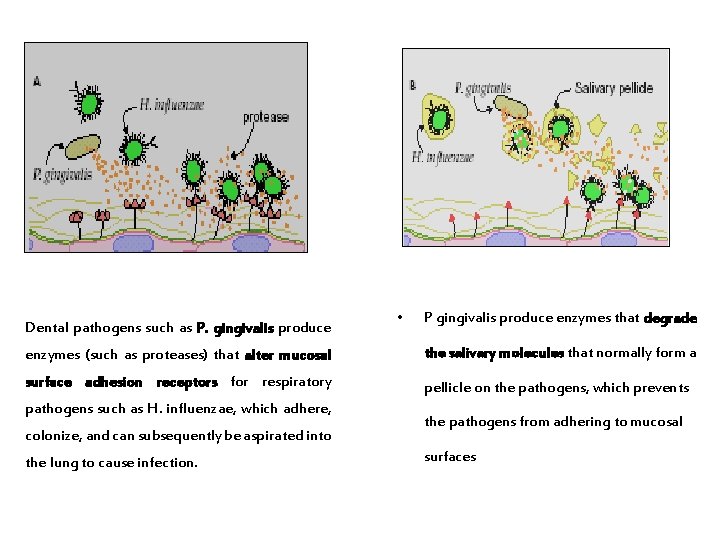
Dental pathogens such as P. gingivalis produce • P gingivalis produce enzymes that degrade enzymes (such as proteases) that alter mucosal the salivary molecules that normally form a surface adhesion receptors for respiratory pellicle on the pathogens, which prevents pathogens such as H. influenzae, which adhere, colonize, and can subsequently be aspirated into the lung to cause infection. the pathogens from adhering to mucosal surfaces
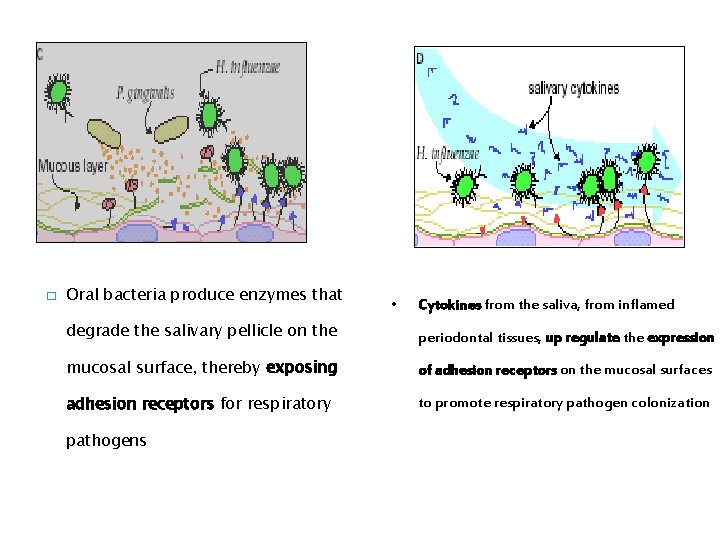
� Oral bacteria produce enzymes that • Cytokines from the saliva, from inflamed degrade the salivary pellicle on the periodontal tissues, up regulate the expression mucosal surface, thereby exposing of adhesion receptors on the mucosal surfaces adhesion receptors for respiratory to promote respiratory pathogen colonization pathogens

� Scannapieco FA, (2001) evaluated the potential associations between chronic respiratory disease and periodontal disease by analyzing data from the (NHANES III). � Subjects with a history of COPD had more periodontal attachment loss than subjects without COPD. � Subjects with mean attachment loss (MAL) > or = 3. 0 mm had a higher risk of COPD than those having MAL < 3. 0 mm. � SMOKING…. . Effect modifier…

Scannapieco FA, (2003) - Searches were performed for articles published in English from 1966 through March 2002. Of the initial 1, 688 studies identified, 36 satisfied all inclusion criteria and were read. They found : - A variety of oral interventions improving oral hygiene through mechanical and/or topical chemical disinfection or antibiotics reduced the incidence of nosocomial pneumonia by an average of 40%. Several studies demonstrated a potential association between periodontal disease and COPD.

Azarpazhooh, Leake’ 06… review of Respiratory & Oral conection 728 articles scanned… 19 articles met the inclusion criteria Conclusion … fair evidence (Odds ratio=1. 2 -9. 6) Pnuemonia & Periodontitis Poor evidence (OR< 2) COPD & Periodontitis Good evidence intervention helps in reduction of nosocomial Pnuemonia

Obesity and periodontal disease Obese Japanese subjects… (Shimazaki et al’ 98) HDL < 60 mg…. ‘Metabolic syndrome’ Upper body obesity…. Younger more than older individuals. . Change in microflora…

pathogenesis Affects host immunity Adipocytokines… TNF- alpha PAI-1 expressed in visceral fat… blood stasis… pdl disease Leptin stimulates the cytokine production Hyperlipidemia… risk factor for Periodontitis (Noack’ 00 ) Katz et al ’ 02… higher CPI code… higher TRG & LDL

Rheumatoid arthritis …. Chronic destructive inflammatory disease… Association shown…. (Kasser’ 97, Mercado’ 01)
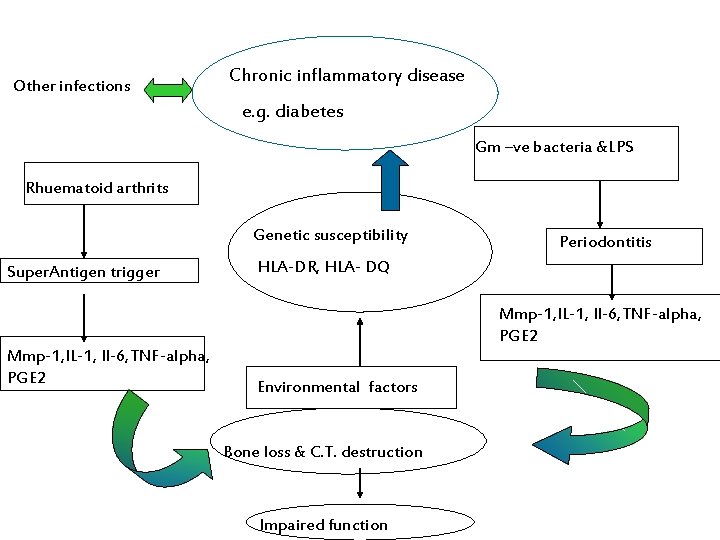
Other infections Chronic inflammatory disease e. g. diabetes Gm –ve bacteria &LPS Rhuematoid arthrits Genetic susceptibility Super. Antigen trigger Periodontitis HLA-DR, HLA- DQ Mmp-1, IL-1, Il-6, TNF-alpha, PGE 2 Environmental factors Bone loss & C. T. destruction Impaired function

NSAID’s…. . Treatment… DMARD’s…. . Gold, methotrexate ( Novak’ 84) Cox-2 inhibitors…

READ FURTHER FROM : Clinical Periodontology; Carranza X edition Periodontal medicine; PERIO 2000; 2000. Brian Mealey; Influence of periodontal infections on systemic health, Perio 2000; 1999; 21: 197 -209
- Slides: 72