PERIMENOPAUSE MENOPAUSE By Bonnie Hill CNM ARNP NCMP

PERIMENOPAUSE & MENOPAUSE By Bonnie Hill, CNM, ARNP, NCMP

Bonnie Hill, CNM, ARNP, NCMP Gynecology Franciscan Women’s Health Associates 1618 S J Street Tacoma, Wa 98407 253 -274 -7501 bonniehillcnm@chifranciscan. org

Menopause: permanent cessation of menstrual periods resulting from ovarian function, usually because of aging. Postmenopause: when the woman has not had a period for one year Perimenopause: menopausal transition including the one year of amenorrhea prior to menopause. Typically starts 8 to 10 years before menopause Premature menopause: cessation of menses before the age of 40 DEFINITIONS

Menopause: When Women Give Birth to Themselves

Is it a disease?

No! It is the natural progression of aging that affects everything!

Why is it important?

Women are living a third of their life after menopause In 2010 there were an estimated 50 million postmenopausal women You will be taking care of them! A women’s life expectancy in the Western world is estimated 80. 8 years
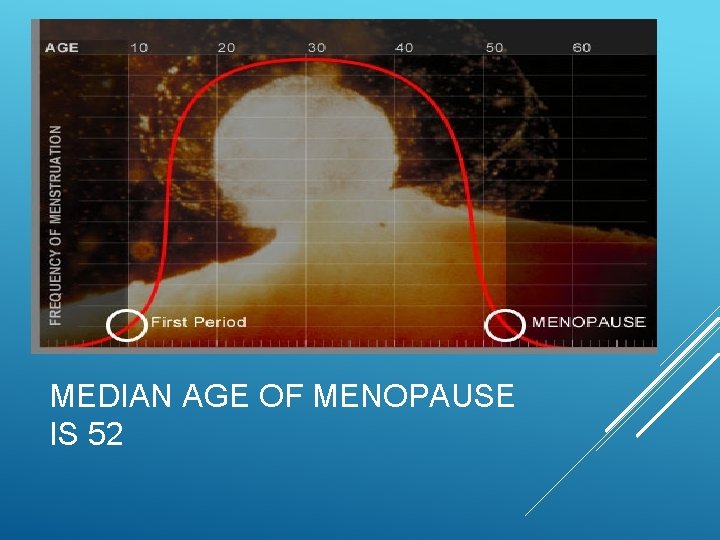
MEDIAN AGE OF MENOPAUSE IS 52

95% woman have transitioned through menopause by the age of 56

Follicular phase of the menstrual cycle shortens with aging Menstrual cycles become irregular because of fluctuating gonadotropins (FSH) from the anterior pituitary gland Decrease sensitivity to gonadotropin stimulation due to follicular attrition leading to anovulatory cycles Estradiol levels remain normal/high due to continued response to FSH & peripheral conversion of androstenedione to testosterone, estradiol and estrone. Women can still get pregnant! PHYSIOLOGY: PERIMENOPAUSE

Follicles depleted, ovary unresponsive to increased FSH, estradiol levels decrease, no more periods The woman can no longer achieve a pregnancy Peripheral conversion of androstenedione now produces circulating estrogens in the form of estrone, estradiol Important to note that hormone fluctuations still occur within the first 5 years after menopause with possible release of senescent egg PHYSIOLOGY: POSTMENOPAUSE

A. R. 52 year woman comes in to your office for her annual exam and tells you her menstrual cycles use to occur every 28 days but the last 6 months they have been occurring every 2124 days. Medical and Surgical Hx: Hypothyroid for which she takes 50 mcg Synthroid OBGYN Hx: G 3 P 2, reports no contraception Social Hx: Married, works fulltime for a nonprofit. She exercises regularly and is nonsmoker. Kids are in college. Family Hx: Mother with heart disease and osteoporosis PE completely normal CASE STUDY

ARE YOU CONCERNED ABOUT HER MENSTRUAL CYCLES?

No Reassure her the bleeding pattern is physiological Counsel her menstrual changes are one of the first signs of hormones shifting in the body and that she is perimenopausal Inform her 50% of women in the US transition through menopause by the age of 52. 95% are done menstruating by the age of 56 Give her menopause resources-North American Menopause Society’s (NAMS) website Dr Christiene Northrup’s Book, The Wisdom of Menopause WHAT ABOUT CONTRACEPTION?

Recommend during the perimenopause until menopause confirmed May consider Progestin only pill or nonhormonal method since > 50. Starting her on combination pills ok as long as there are no risk factors increasing her risk for stroke and blood clot. Mirena IUD excellent choice-if inserted at 45 or later, ok to keep in for 7 years (off label use)

In general nonhormonal contraception can be stopped 1 year after the last menstrual period in women over the age of 50 In women >45 with 1 year amenorrhea still have 210% chance of menstruation. These women can stop contraception after 2 years of amenorrhea Natural sterility can be assumed after the age of 55 in amenorrheic women

WHAT ORGANS ARE AFFECTED?

Integumentary-skin becomes dry, acne flares, eyes become dry, hair loses shine, coronal hair loss, chin and upper lip hair Cardiovascular- decreased blood flow to vascular beds, increase nitric oxide, vasoconstriction, angiotension-converting enzyme decreases Gastrointestinal- decrease secretion of hydrochloric acid secretion impacting digestion. Musculoskeletal- loss of muscle mass, central obesity, loss of pelvic floor tone, bone loss Genitourinary-urinary frequency, urgency, incontinence, dyspareunia, vaginal atrophy, vaginal dryness, vaginitis, sexual dysfunction Psychological-depression, grief, anxiety Endocrine- insulin resistance-menopause is diabetogenic ALL OF THEM!

Cognition- current evidence shows verbal memory loss occurs initially through menopausal transition, regained in postmenopause Important to normalize this for women Estrogen has a direct affect on memory and frontal cortex functioning Studies suggest vasomotor symptoms correlate with memory performance raising the question if hormone therapy might affect memory during menopausal transition Counsel women with significant vasomotor symptoms that memory might improve with estrogen Keep lipids in normal range and exercise, no alcohol COGNITION

COMMON SYMPTOMS OF MENOPAUSE
HOT FLASHES! ��

Typically occurs the first 5 to 10 years around menopause but in some women may last well into their 70 s. Change in the hypothalmic thermoregulatory center Impact on women variable Verify vasomotor instability due to hormonal fluctuations, check TSH, CBC and CMP CAUSES

Estrogen works! FDA approved formulations for menopausal symptoms Start with non-oral bio-identical formulations if at all possible to lower risk for blood clot and stroke Patch, gel, spray, ring Compounded formulations TREATMENT

Minivelle and Vivelle Dot, 0. 025, 0. 0375, 0. 075, 0. 1 patch, twice per week. Dot matrix technology so ok to cut the patch in 1/2 Climara, 0. 025, 0. 0375, 0. 05, 0. 6, 0. 075, 0. 1 patch, weekly, some women may need to change it every 5 days. Alora, 0. 025, 0. 075, 0. 1 twice per week Estraderm, 0. 05, 0. 1 twice per week Various generics FDA APPROVED TRANSDERMAL PATCHES-17 B-ESTRADIOL-MG E 2/DAY

Divigel, 0. 25, 0. 5, 1. 0 Estrogel, Elestrin, 0. 75 0. 52 FDA APPROVED TRANSDERMAL GELS (MG E 2/DAY)

Evamist, 1. 53 mg. E 2/day FDA APPROVED TRANSDERMAL SPRAY

Femring, 0. 05 mg/day for 90 days, 0. 01 mg/day for 90 days This is also indicated for moderate to severe vulvar and vaginal atrophy due to menopause FDA APPROVED RINGS

Climara-Pro, 0. 045 E (17 B etstradiol)+ 0. 015 mg P (levonorgestrel) once/week. Good option for recently postmenopausal women with uterus Combi. Patch, 0. 05 mg E (17 B estradiol) + 0. 014 P (norethindrone acetate) 2/week. FDA APPROVED COMBINATION ESTROGEN-PROGESTOGEN PATCHES

Estrace (17 B-estradiol), 0. 5, 1. 0, 2. 0 Various 17 B estradiol generics Premarin (conjugated estrogen), 0. 3, . 045, 0. 625, 0. 9, 1. 25 Enjuvia (synthetic conjugated estrogen), 0. 3, 0. 45, 0. 0625, 0. 9, 1. 25 Menest (esterified estrogen), 0. 3, 0. 625, 1. 25, 2. 5(administer cyclically, usually in perimenopausal women) FDA APPROVED ORAL ESTROGEN-MG/DAY

Prometrium (micronized progesterone), 100 mg/day, 200 mg (administer cyclically) This is a bioidentical progesterone, check peanut allergy Norethindrone, 2. 5 mg, 10 mg (administer cyclically) Provera (medroxyprogesterone acetate), 2. 5 mg, 10 mg (administer cyclically) Caution in women with hyperlipidemia FDA APPROVED PROGESTINS

Vaginal formulations: Prochieve 1 applicator per vagina QOD x 6 doses Crinolone 4%- 8% gel, containing 45 mg progesterone, 1 applicator per vagina QOD x 6 doses PROGESTERONE/PROGESTIN OFF LABEL USE

Premphase (conjugated estrogens + medroxyprogesterone acetate) 0. 625 mg E + 5. 0 mg P (2 tablets: E days 1 -14, E+P days 15 -28. This is an oral continuous-cyclic regime. Appropriate for perimenopausal women Prempro (conjugated estrogens + medroxyprogesterone acetate) 0. 3 mg or 0. 45 mg E + 1. 5 mg P. Femhrt (ethinyl estradiol + norethindrone acetate), 2. 5 ug E + 0. 5 mg P, 5 ug E + 1 mg P Activella (17 B-estradiol + norethindrone acetate), 0. 5 mg E + 0. 1 mg P, 1 mg E + 0. 5 mg P Angeliq (17 B-estradiol + drospirenone), 1 mg E + 0. 5 mg P, 0. 5 mg E + 0. 25 mg P Prefest ( 17 B-estradiol + norgestimate), 1 mg E and 1 mg E+ 0. 09 P – E alone for 3 days followed by E+P for 3 days, repeated continuously FDA APPROVED ORAL COMBINATION ESTROGENPROGESTOGEN

Duavee (conjugated estrogen + bazedoxifene), 0. 45 mg E + 20 mg bazedoxifene OTHER FDA APPROVED TREATMENT FOR HOT FLASHES

Estrogen and progesterone increase risk for blood clots in lungs and legs similar to OCPs, patches and rings This risk is rare in healthy women 50 -59 Increased risks for breast cancer when estrogen & progesterone used continuously for 5 or more years-breast cancer risk decreases when hormones stopped Use of estrogen alone for 7 years did not increase breast cancer risk RISKS IDENTIFIED FROM WHI

Clinicians follow WHI recommendations right nowlowest dose of hormones that provide vasomotor symptom relief for the shortest period of time However there is a body of research that shows stopping hormone therapy may increase a woman’s risk for cardiovascular disease (Dr Howard Hodis atherosclerosis research) and dementia (Dr Pauline Maki’s research) Health cell phenomena, age and timing of hormone initiation RECENT RESEARCH

Therapy individualized to the woman Consider the woman’s quality of life Her personal risk factors-age, time since menopause, risk for blood clots, heart disease stroke and breast cancer BOTTOM LINE

P. C. is a 48 year old G 1 P 1 perimenopausal woman who comes in to your office stating she is miserable because she wakes up at night with hot flashes. They are a cause of embarrassment for her at work. Med/Surg Hx: Left oophorectomy 5 years ago for dermoid cyst No medical problems Family Hx: Father with colon cancer and mother with osteoporosis with fragility fractures Social Hx: Smoker Mirena IUD for contraception BP 120/70, BMI 29 Thyroid: nonenlarged without nodules Lymphatics: Negative adenopathy Heart: RRR no murmer Lungs: clear to auscultation, easy excursion Abdominal Exam: Nontender all quadrants, negative organomegaly, girth>35 cm CASE STUDY

CONSIDERATIONS?

WHI tells us that estrogen decreases a woman’s risk for colon cancer and osteoporosis

I placed her on 0. 05 mg estrogen patch, Minivelle 2 times per week Rotate sites, buttocks best, mineral oil removes adhesive Informed her hormones usually do not take hot flashes away completely, but frequency and intensity start to decrease in a month, significantly better in 3 months Patient followed up in 4 weeks, sleeping better, having less hot flashes I renewed the patch for one year Made sure current with mammogram CLINICAL MANAGEMENT

What Why about progesterone? is it important?

Increased risk uterine cancer when estrogen used without progesterone or progestins (7/1000 risk decreases to <1/1000 Not an issue in women with hysterectomy Decrease rare recurrence endometriosis-therefore sometimes prescribed with estrogen in women with history hysterectomy and endometriosis

Cycle perimenopausal woman, estrogen patch 2 times per week, add progesterone /progestins 10 days of the cycle, days 16 -25 This regulates cycles and helps decrease uterine cancer risk especially in obese women Mirena IUD Once the woman transitions through menopause, change progesterone/progestin to daily if she has a uterus TREATMENT PERIMENOPAUSE

Uterine cancer risk of unopposed estrogen is 7/1, 000, check the endometrium annually with ultrasound and or endometrial biopsy. Document informed consent Consider Mirena IUD Consider compounding formulations MANAGEMENT: SHE CAN NOT TOLERATE PROGESTERONE/PROGESTINS

Make sure dosage is at least 50 mg daily. Check the endometrium annually with pelvic ultrasound, and if >5 mm, perform an endometrial biopsy. Patient needs information that we do not know if non FDA approved progesterone protects the uterus from cancer when taking estrogen TREATMENT: NON FDA APPROVED COMPOUNDED PROGESTERONE

Not FDA approved Not recommended by ACOG, NAMS due to lack of data attesting to safety, concern about dose, therapeutic effect Women need to be informed of these concerns Informed consent Beauty of them is able to titrate to symptoms Comes in cream, tincture, troche or capsules Biest (80% estriol, 20% estradiol, can be 50/50 Triest 80% estriol, 10% estradiol, 10% estrone Progesterone capsules, tincture and cream Testosterone capsules, cream DHEA capsules, cream TREATMENT: COMPOUNDED PREPARATIONS

WHAT IF ESTROGEN CONTRAINDICATED?

Clonidine patch 0. 05 mg – 0. 1 mg patch Brisdelle (Paroxetine) 7. 5 mg po daily (Not recommended in women on tamoxifem due to inhibition of enzyme converting tamoxifem to active metabolite) Paroxetine 10 -25 mg daily (off label use) Venlafaxine (Effexor) 37. 5 mg for the first week, increase to 75 mg. Can titrate to 150 mg daily Off label use of other SSRI, SRNI (fluoxetine and sertraline did not show significant reduction hot flashes. Escitalopram 10 -20 mg, Citalapram 10 -20 mg, Desvenlafaxine 100 -150 mg Gabapentin 300 mg daily can increase to tid slowly FDA NONHORMONAL TREATMENT OPTIONS:

NAMS 2015 Position Statement of Nonhormonal management of menopause-associated vasomotor symptoms Relizen- Swedish flower pollen extract, allergenic husk removed, order through website Relizen. com Cognitive Behavioral Therapy Clinical Hypnosis Stellate Ganglion Block-bupivicaine injections into this area C-6 and T 2 region Phytoestrogens- in particular soy TREATMENT: NON HORMONAL OPTIONS

Weight loss-getting and keeping BMI in a normal range Regular exercise Yoga Stop smoking Increase water intake Eliminating alcohol, caffeine, spicy foods Dressing in layers, cool room at night Accupuncture TREATMENT: LIFESTYLE

GENITOURINARY SYNDROME OF MENOPAUSE (GSM)
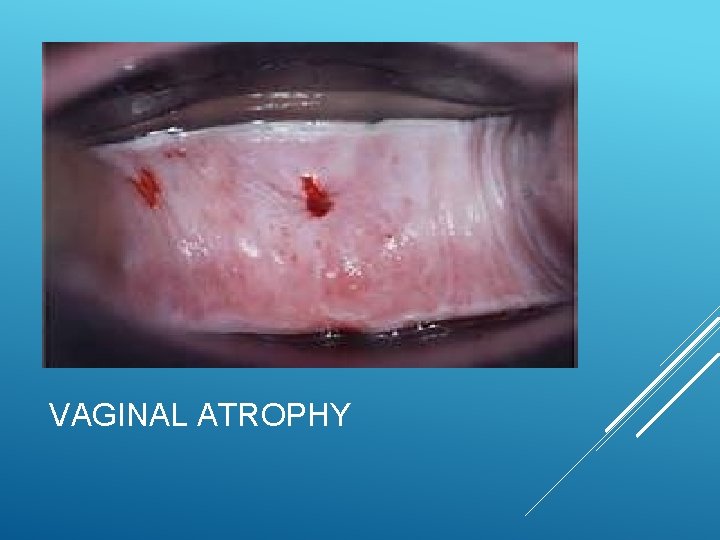
VAGINAL ATROPHY
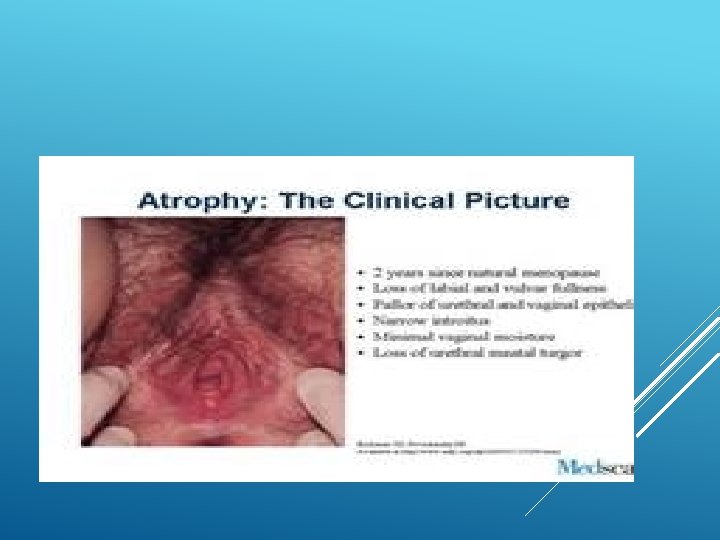
UROGENITAL CHANGES

Drop in estrogen impacts the structural and functional integrity of the urogenital area Decreased fat and hair distribution in bilateral labia majorum Thinning labia minora Decreased blood flow to the area Shortened and narrowed vaginal canal Decreased lubrication Vaginal atrophy progressively gets worse with time WHAT HAPPENS?

Decreased vestibular sensitivity Decreased sexual arousal Increase in vaginal PH Increase BV infections Atrophy of the bladder and urethral tissues Increased UTI, urinary urge and stress incontinence
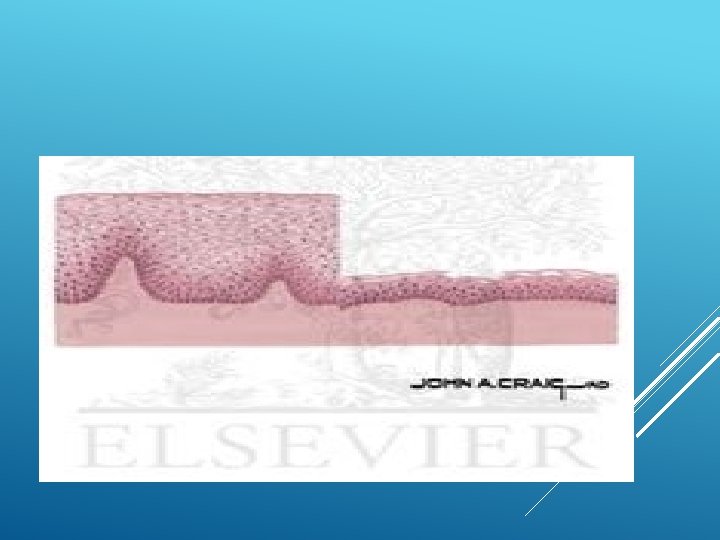
VAGINAL CHANGES


Vaginal dryness, itching, pain, burning, odor Decreased lubrication Dyspareunia Loss of libido Urinary urgency, frequency, dysuria Recurrent UTI Urinary urge and stress incontinence SYMPTOMS

Vagifem 10 mcg 1 per vagina qhs 1 st 2 weeks then 2 times per week Estrace or premarin cream 1 gram per vagina 2 times per week Estring 7. 5 mcg estradiol/24 hours Black box warning will be removed in near future Osphena SERM 60 mg daily-risk blood clot and stroke, no greater risk than hormone therapy FDA APPROVED TREATMENT VAGINAL ATROPHY

Estriol 1 -2 mg vaginal suppositories DHEA vaginal suppositories Cannibus vaginal suppositories OFF LABEL TREATMENT

Replens OTC 1 applicator per vagina qod Lubrigyn OTC vaginal moisturizer-can be used daily Luvena OTC vaginal moisturizer-can be used daily NONHORMONAL TREATMENTS
SAMPLES

T. W is a 57 G 0 P 0 year old woman who tells you she can not have sex with her husband due to pain and vaginal dryness. Medical History: Breast cancer Surgical History: Bilateral mastectomy Family History: Mother with breast cancer, diagnosed at age 70 Social history: Married, does not work, previous smoker, raised husbands children from previous marriage PE: Narrow introitus, skin pale and dry. Speculum exam (pediatric speculum) vaginal canal dry, no ruggae, bleeds easily, petechiae noted, dark yellow discharge, nulliparous cervix A: Dyspareunia due to severe vulvovaginal atrophy CASE STUDY

Would you give her estrogen? WHAT IS YOUR PLAN?

MAYBE

Retrospective studies of Durna et al (2002) and Le. Ray (2012) suggest local vaginal estrogen therapy may not place breast cancer survivors at risk for recurrence Give the woman information about nonhormonal vaginal moisturizers and vaginal estrogens. Make sure oncology ok with vaginal estrogen prescription if bret cancer history Inform the woman it takes 3 -6 months before dyspareunia decreases

Heart Disease Diabetes Osteoporosis Cancer: lung, breast, colon MEDICAL RISKS

30 % of women die of cardiovascular disease after menopause, 4% die of breast cancer

#1 cause of mortality in postmenopausal woman Exercise, 6 days per week minimum 30 minutes Keep BMI within normal range, GET FIT Keep waist circumference < 35 Mediterranean or DASH diet Stop smoking Love and laughter every day 4 ounces red wine daily CARDIOVASCULAR DISEASE

Love Relationships, community Massage Regular exercise Counselor Energy healers EMOTIONAL HEALTH

Risks: PCOS, GDM, BMI > 25, family history, age Increased insulin resistance in post menopausal women, in part due to testosterone Intervene when pre-diabetic, PCOS & GDM diagnosis Exercise Keep BMI within normal range, FIT BODY Eliminate white poisons from the diet DIABETES

The most common cause of morbidity in postmenopausal women OSTEOPOROSIS

Silent skeletal disorder characterized by compromised bone strength predisposing a woman to fracture Primary osteoporosis caused by bone loss associated with aging Secondary osteoporosis caused by other diseasesie malabsorption, prolonged steroid exposure DEFINITION

World Health Organization defines osteoporosis when Dexa scan T score -2. 5 Can be a clinical diagnosis when there is a fragility fracture-even with a normal T score DIAGNOSIS

Osteoclasts promote bone resorption (breakdown) by stimulating enzymes and acids that dissolve bone minerals and proteins Osteoblasts promote bone formation by creating bone matrix consisting of collagen that becomes calcified resulting in mineralized bone In normal bone remodeling bone resorption is balanced with bone formation Bone loss results when there is an imbalance between bone resorption and formation Menopause results in rapid loss of bone mass due to loss of 17 B-estradiol that inhibits osteoclast activity Greatest bone loss is within the first 5 years after menopause transition, after which bone loss stabilizes PATHOPHYSIOLOGY

Screen with Dexa scan at the age of 50 in women with risk factors: low body weight personal history of fractures family history of osteoporosis (women’s risk increases when there is a fragility fracture) smoking, excessive alcohol intake long term use of glucocorticoids USPSTF recommendation: screen all postmenopausal women at age 65 FRAX-tool to assess fracture risk incorporating Dexa scan results. Helps with treatment decisions EVALUATION

Primary goal of treatment is to lower risk for fracture TREATMENT

Bisphonates Estrogen agonist/antagonist Calcitonin Parathyroid hormone RANK lignand inhibitor Others in clinical trials FDA APPROVED TREATMENT OPTIONS

Weight bearing exercise Lifting weights Stop smoking and minimize alcohol intake Vitamin D, calcium, trace minerals Yoga for balance and core strengthening OTHER IMPORTANT RECOMMENDATIONS

Second leading cause of death from cancer Annual mammograms and SBE BRa. CA screening Keep BMI within normal range Adequate Vitamin D Alcohol, smoking Exercise BREAST CANCER

Vegetable based diet Fiber 25 grams per day Regular exercise Regular bowel movements Colonoscopy screening age 50 Stop smoking Family history, genetic screening Estrogen COLON CANCER

PSYCHOLOGICAL IMPACT

Grief Changing relationships Coming to terms with mortality Legacy Intention TRANSITION: EMBRACING THE CRONE-STEPPING INTO WISDOM

“Life isn’t about finding yourself. It is about creating yourself. ” GEORGE BERNARD SHAW


Connect with spirit Important! Nurture the spirit on a regular basis SPIRITUAL HEALTH

COMMUNITY

SERVICE

PASSION!

North American Society (NAMS) Womento. Women. org The Wisdom of Menopause by Dr Christine Northrup Estrogen, the Natural Way by Nina Shandler The Virgin Diet Younger Next Year (pink version) Fit Body, Fit Soul by Brant Secunda and Mark Allen RESOURCES FOR WOMEN

THANK-YOU!
- Slides: 92