Pericardial stentless bioprosthesis Preliminary results of a modified

Pericardial stentless bioprosthesis Preliminary results of a modified procedure for implantation Y. De Bruyne, B. El Nakadi & M. Joris Hopitaux civils du CPAS de Charleroi, Belgium.
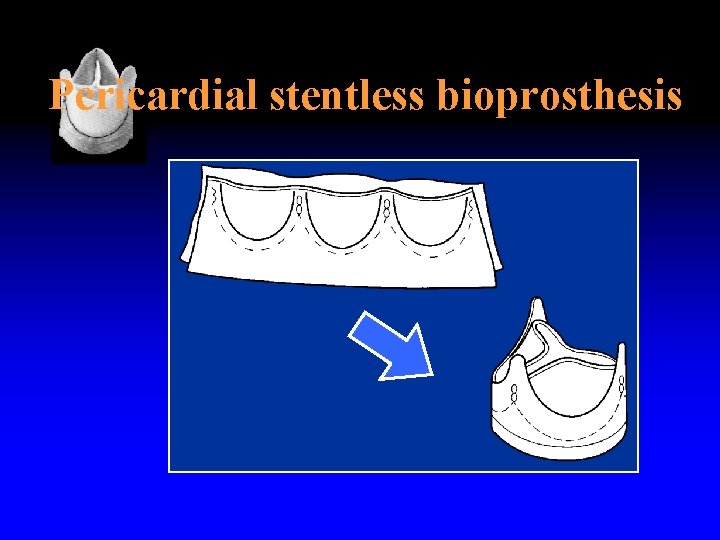
Pericardial stentless bioprosthesis

Pericardial stentless bioprosthesis • • 37 patients Male / female: 26/11 Age: 68 ± 6 ( 53 - 83 ) Aortic valve lesions: Stenosis: 16 Regurgitation: 10 Mixed: 11 • Endocarditis: 5 (43%) (27%) (13%)
Pericardial stentless bioprosthesis Operative data – Size of implanted valves: • 21 mm 1 • 23 mm 7 • 25 mm 12 • 27 mm 17 – Associated procedures: • CABG 13 • Mitral repair 1

Pericardial stentless bioprosthesis Operative groups • Group A: Classical – Classical subcoronary implantation (8/37) • Group B: Banding – Addition of peri-aortic banding (19/37) • Group C: Vascular prosthesis – Association with replacement of a dilated ascending aorta (10/37)

Pericardial stentless bioprosthesis Group A: Classical • 8 patients • Regurgitation: 1 mild 1 severe ( reoperated ) Reconsideration of the operative technique
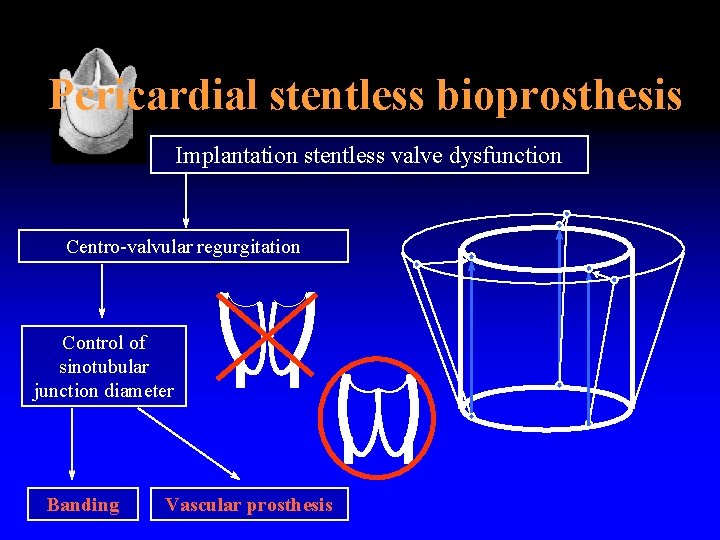
Pericardial stentless bioprosthesis Implantation stentless valve dysfunction Centro-valvular regurgitation Control of sinotubular junction diameter Banding Vascular prosthesis
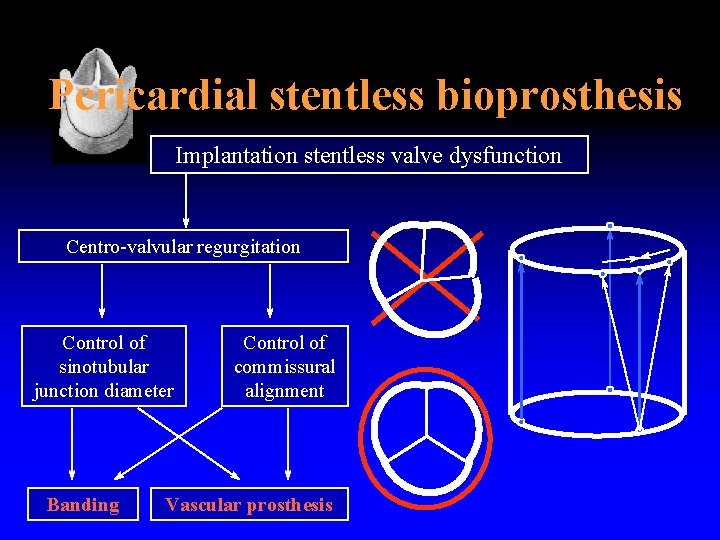
Pericardial stentless bioprosthesis Implantation stentless valve dysfunction Centro-valvular regurgitation Control of sinotubular junction diameter Banding Control of commissural alignment Vascular prosthesis
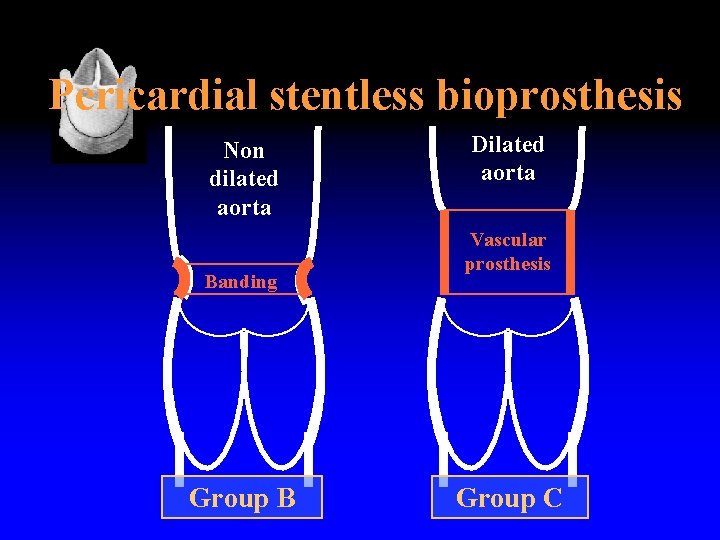
Pericardial stentless bioprosthesis Non dilated aorta Banding Group B Dilated aorta Vascular prosthesis Group C
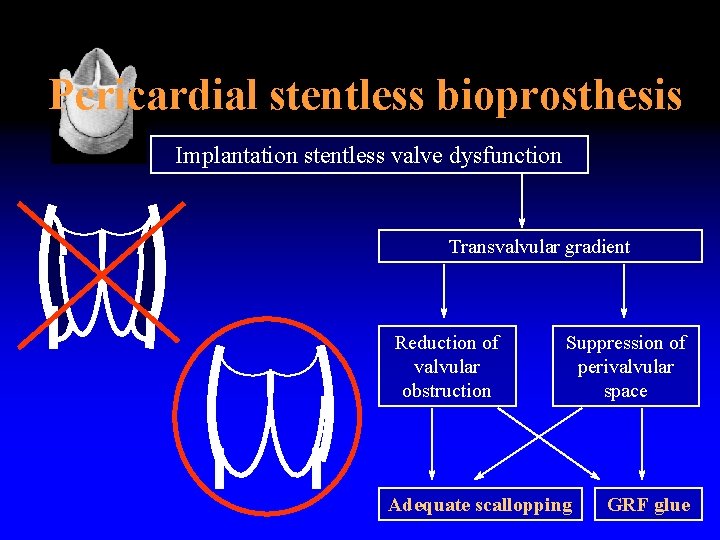
Pericardial stentless bioprosthesis Implantation stentless valve dysfunction Transvalvular gradient Reduction of valvular obstruction Suppression of perivalvular space Adequate scallopping GRF glue
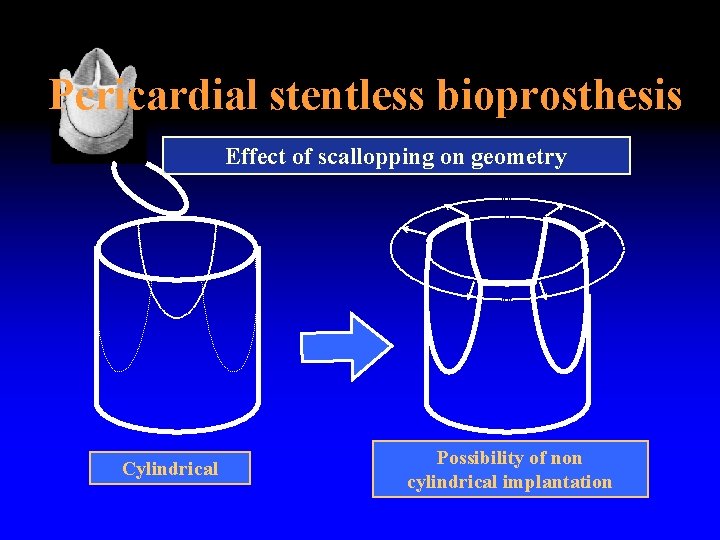
Pericardial stentless bioprosthesis Effect of scallopping on geometry Cylindrical Possibility of non cylindrical implantation
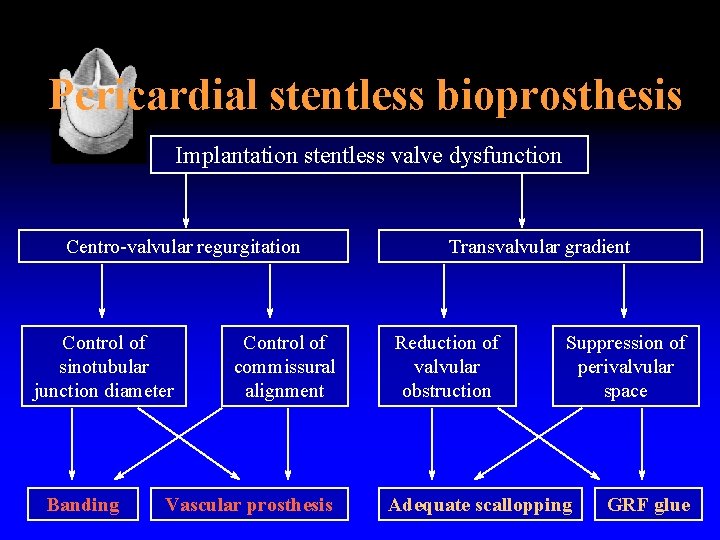
Pericardial stentless bioprosthesis Implantation stentless valve dysfunction Centro-valvular regurgitation Control of sinotubular junction diameter Banding Control of commissural alignment Vascular prosthesis Transvalvular gradient Reduction of valvular obstruction Suppression of perivalvular space Adequate scallopping GRF glue

Pericardial stentless bioprosthesis Group B: Banding (19 patients ) • S-shaped aortotomy • Aortic wall extensively freed of calcifications • Size of the prosthesis defined by the diameter of the aortic annulus • Trimming of the inferior rim of the prosthesis • Inflow suture line: 3 running sutures (Baratt-Boyes) • Scallopping of the three sinuses • Outflow suture line: 3 running sutures

Pericardial stentless bioprosthesis Group B: Banding (19 patients ) • Dacron strip length : C = 3, 5 * [prosthesis diameter] (perimeter + aortic wall thickness) • GRF Glue • Extra-aortic knots of the distal suture line anchoring the Dacron banding • Closure of the aortotomy • Fastening of the banding

Pericardial stentless bioprosthesis Group C: Vascular prosthesis (10 patients ) • Dilated ascending aorta (more than 40 mm) • Transsection at the sinotubular junction • Valve replacement (± plicatures of the aortic wall) • Vascular prosthesis (1 mm larger than the valve) • Proximal running suture supporting the valvular commissures • Distal running suture line

Pericardial stentless bioprosthesis Cross-clamping time
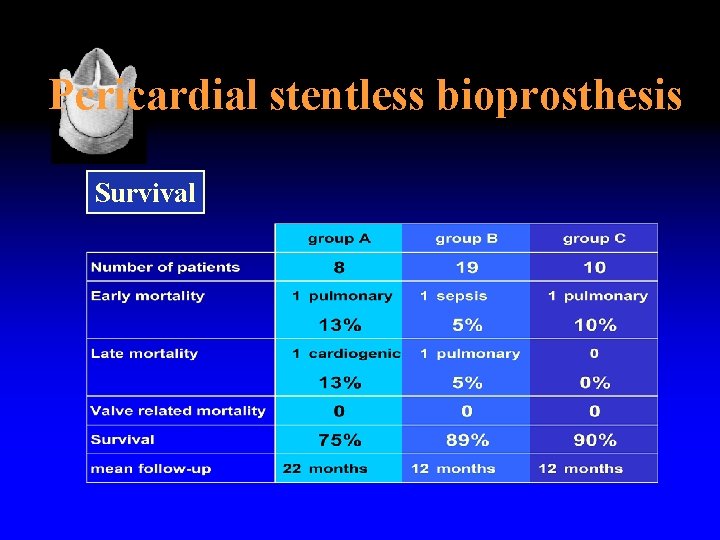
Pericardial stentless bioprosthesis Survival
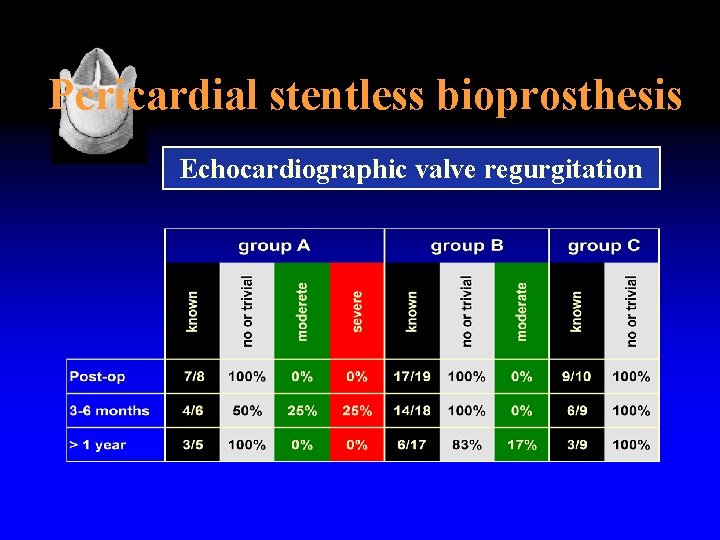
Pericardial stentless bioprosthesis Echocardiographic valve regurgitation

Pericardial stentless bioprosthesis Conclusion • The pericardial stentless bioprosthesis can be used in any pathologic condition requiering aortic valve replacement. • An appropriate peri-aortic banding seems to secure an adequate geometrical valve implantation. • Combined replacement of the aortic valve and a part of the ascending aorta seems to be a good alternative for a root replacement.

Pericardial stentless bioprosthesis Echocardiographic valve regurgitation
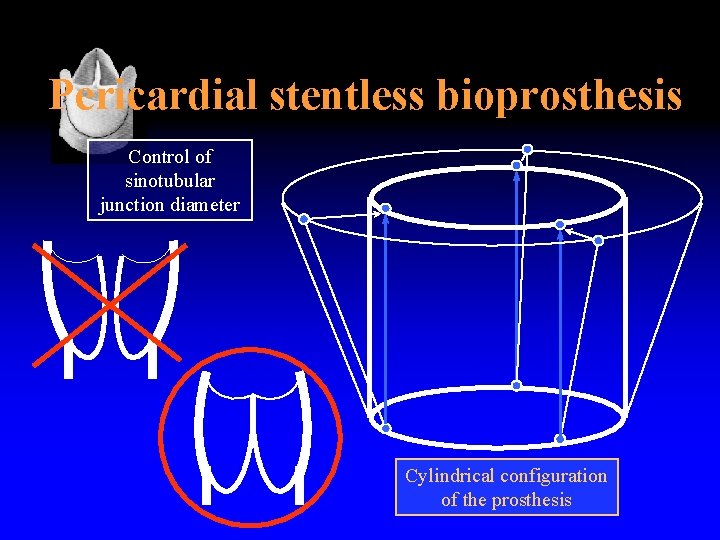
Pericardial stentless bioprosthesis Control of sinotubular junction diameter Cylindrical configuration of the prosthesis
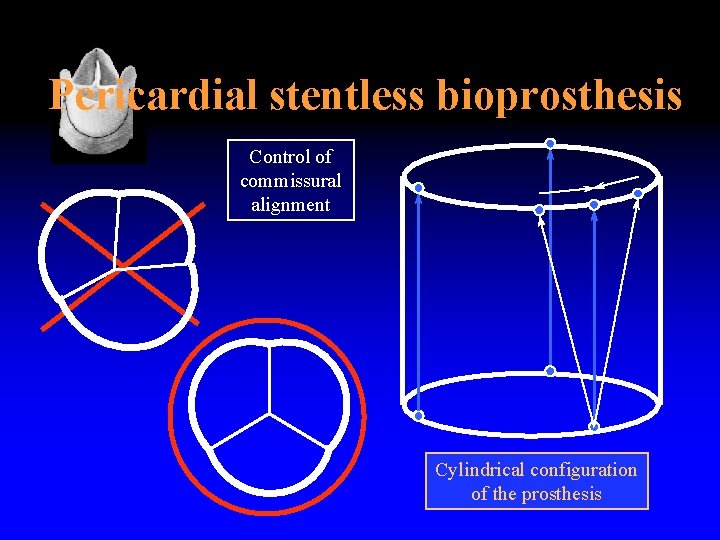
Pericardial stentless bioprosthesis Control of commissural alignment Cylindrical configuration of the prosthesis
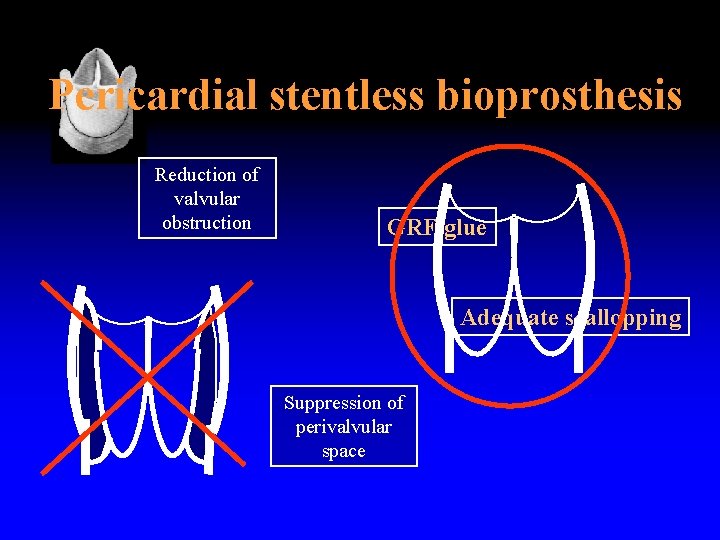
Pericardial stentless bioprosthesis Reduction of valvular obstruction GRF glue Adequate scallopping Suppression of perivalvular space

Pericardial stentless bioprosthesis Follow-up
- Slides: 24