PERFORMING TACTICAL COMBAT CASUALTY CARE Tactical Combat Casualty

PERFORMING TACTICAL COMBAT CASUALTY CARE

Tactical Combat Casualty Care 1. BAD TACTICS CAN GET EVERYONE KILLED. 2. BAD TACTICS CAN CAUSE THE MISSION TO FAIL.

Timing is Everything The Right Things To Do AND The Right Time to Do Them


Introduction About 90 percent of combat deaths occur on the battlefield before the casualties reach a medical treatment facility (MTF). Most of these deaths cannot be prevented by you or the medic. Examples: Massive head injury, massive trauma to the body.
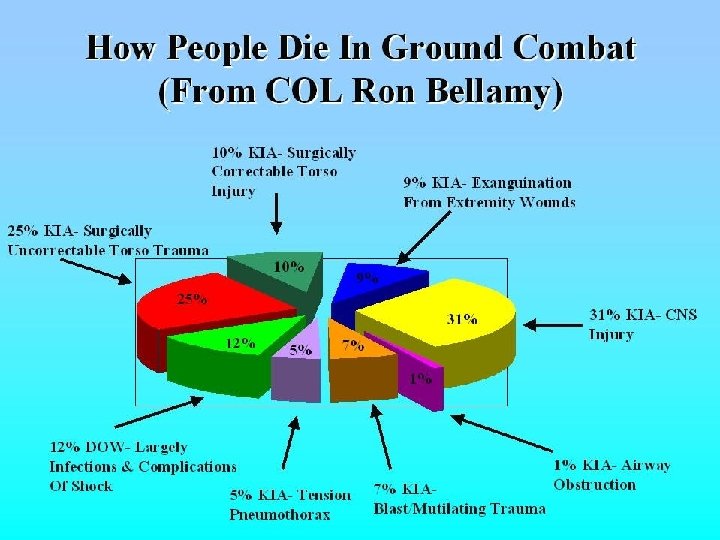
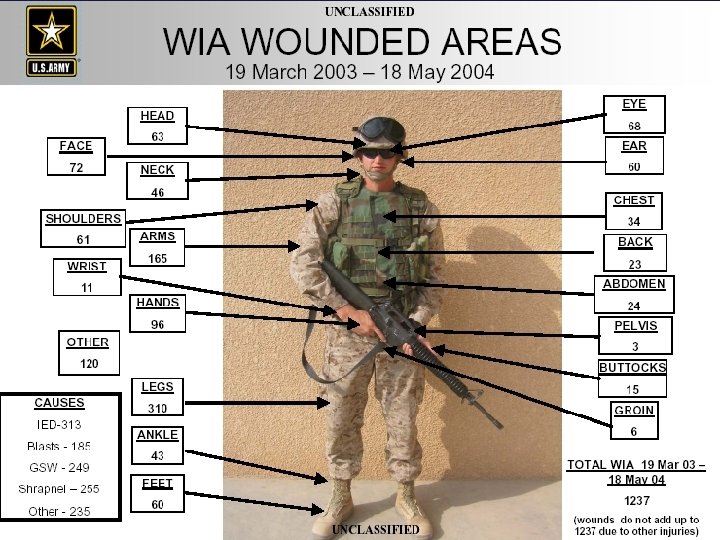

About 15 percent of the casualties that die before reaching a medical treatment facility can be saved if proper measures are taken. Stop severe bleeding (hemorrhaging) Relieve tension pneumothorax Restore the airway

In the Vietnam conflict, over 2500 soldiers died due to hemorrhage from wounds to the arms and legs even though the soldiers had no other serious injuries. These soldiers could have been saved by applying pressure dressings and tourniquets to stop the bleeding.

Combat Lifesaver • Functioning as a Combat Lifesaver is your secondary mission. • Your primary mission is still your combat duties. • You should render care only when such care does not endanger your primary mission.

Tactical Context • Incoming fire • Darkness • Environmental factors • Casualty transport problems • Delays to definitive care • Command decisions

Tactical Combat Casualty Care 3 Distinct Phases • Care Under Fire • Tactical Field Care • Combat Casualty Evacuation Care

The three goals of Tactical Combat Casualty Care (TCCC) are: 1. Save preventable deaths 2. Prevent additional casualties 3. Complete the mission

This approach recognizes a particularly important principle: – To perform the correct intervention at the correct time in the continuum of combat care – A medically correct intervention performed at the wrong time in combat may lead to further casualties

Care Under Fire • Care rendered by the medic or first responder at the scene of the injury while still under effective hostile fire • Very limited as to the care you can provide

Tactical Field Care • Care rendered once you are no longer under effective hostile fire • You and the casualty are safe and you are free to provide casualty care (primary mission is complete)

Combat Casualty Evacuation Care • Care rendered during casualty evacuation • Additional medical personnel and equipment may have been pre-staged and available at this stage of casualty management

Care Under Fire

The Toohey Amendment “I also expect the casualties to continue to return fire as long as they are able to do so. ” CDR Pat Toohey Commanding Officer SEAL Team Four

Care Under Fire • “The best medicine on any battlefield is fire superiority” • Medical personnel’s firepower may be essential in obtaining tactical fire superiority • Attention to suppression of hostile fire will minimize the risk of additional injuries or casualties

Care Under Fire • If the casualty can function, direct him to return fire, move to cover, and administer self-aid • If unable to return fire or move to safety and you cannot assist, tell the casualty to “play dead” • Communicate the medical situation to the team leader • Use cover/concealment such as smoke

Care Under Fire • No attention to the airway at this point because of the need to move casualty to cover quickly • If the casualty has severe bleeding from a limb or has an amputation, apply a tourniquet Improved First Aid Kit

Care Under Fire • Hemorrhage from extremities is the 1 st leading cause of preventable combat deaths • Prompt use of tourniquets to stop the bleeding may be life-saving in this phase

OIF Fatality • • Marine shot in leg in Iraq Pulsatile femoral artery bleeding Corpsman arrived 10 minutes later Attempted to use hemostatic material failed • IV attempted - failed • Tourniquet finally applied • Casualty died

Combat Application Tourniquet (CAT) WINDLASS OMNI TAPE BAND WINDLASS STRAP
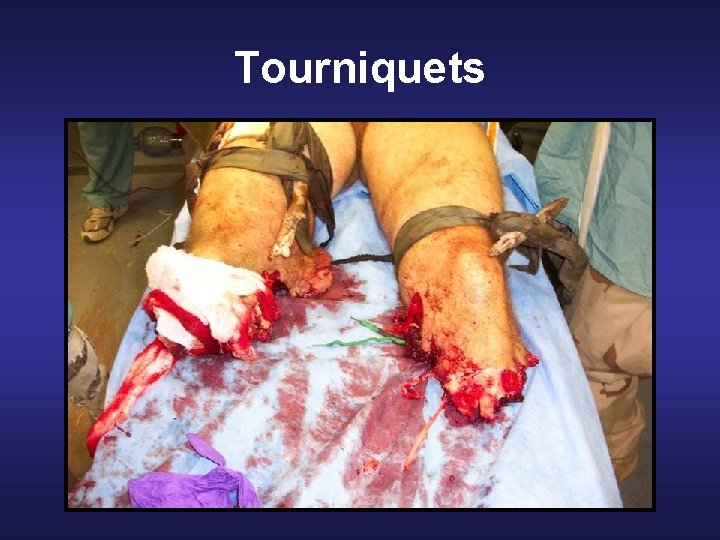
Tourniquets

Care Under Fire • Reassure the casualty • If unresponsive, move the casualty and his mission-essential equipment to cover as the tactical situation permits

Tactical Field Care

Tactical Field Care • Perform tactical field care when you and the casualty are not under direct enemy fire. • Recheck bleeding control measures if they were applied while under fire.

Tactical Field Care If a victim of a blast or penetrating injury is found without a pulse, respirations, or other signs of life, DO NOT attempt CPR performers may get killed Mission gets delayed Casualty stays dead…

Tactical Field Care Casualties with confused mental status should be disarmed immediately of both weapons and grenades.

Determine Level of Consciousness AVPU system A The casualty is alert, knows who he is, the date, where he is, and so forth. V The casualty is not alert, but does respond to verbal commands. P The casualty responds to pain, but not verbal commands. U The casualty is unresponsive (unconscious). Recheck every 15 minutes

Tactical Field Care • Initial assessment is the ABCs – Airway – Breathing – Circulation

Tactical Field Care: Airway • Open the airway with a chin-lift or jaw-thrust maneuver • If unconscious and spontaneously breathing, insert a nasopharyngeal airway • Place the casualty in the recovery position
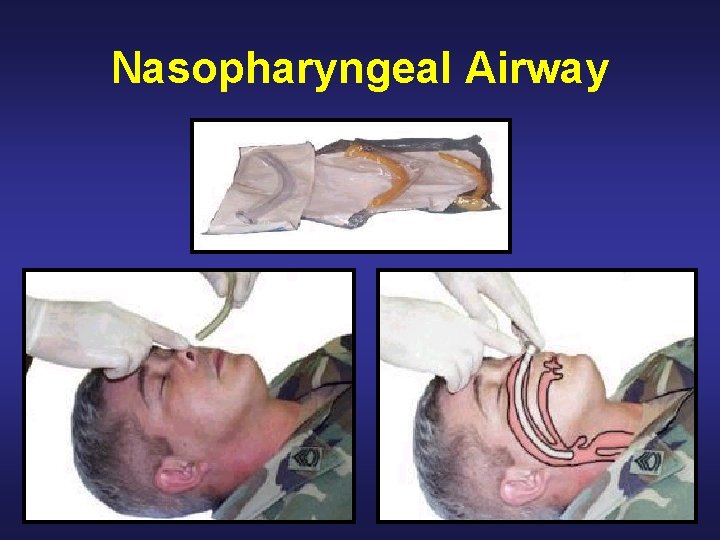
Nasopharyngeal Airway
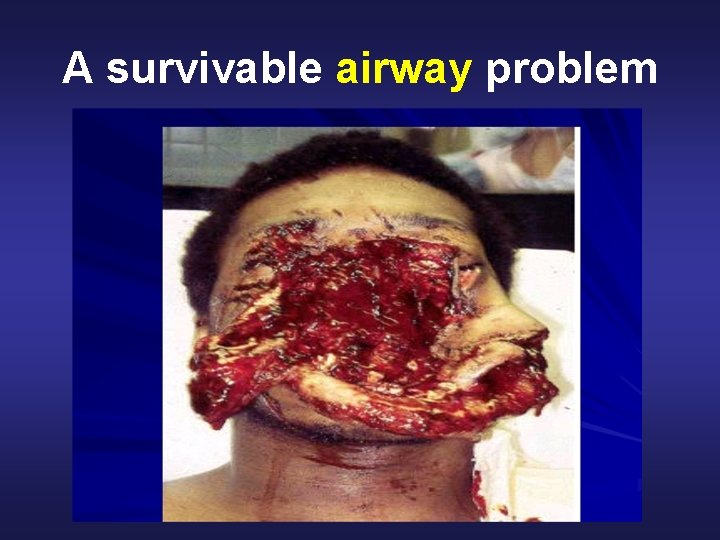
A survivable airway problem

Tactical Field Care: Breathing • Traumatic chest wall defects should be closed quickly with an occlusive dressing without regard to venting one side of the dressing • Also may use an “Asherman Chest Seal” • Place the casualty in the sitting position if possible.
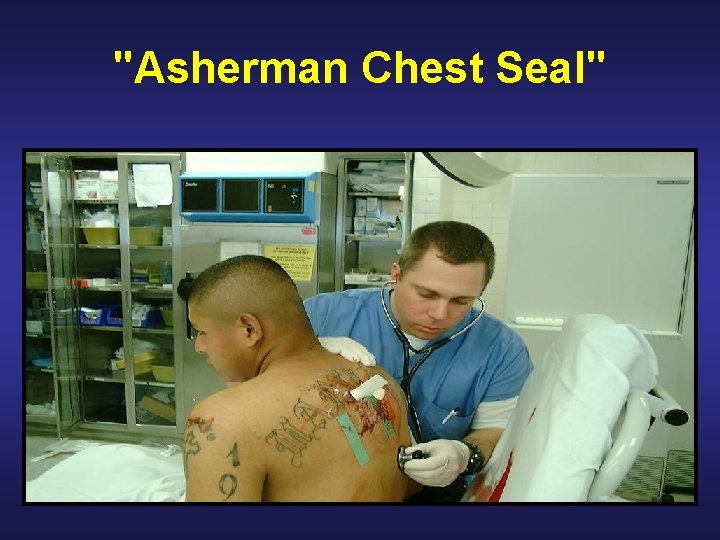
"Asherman Chest Seal"
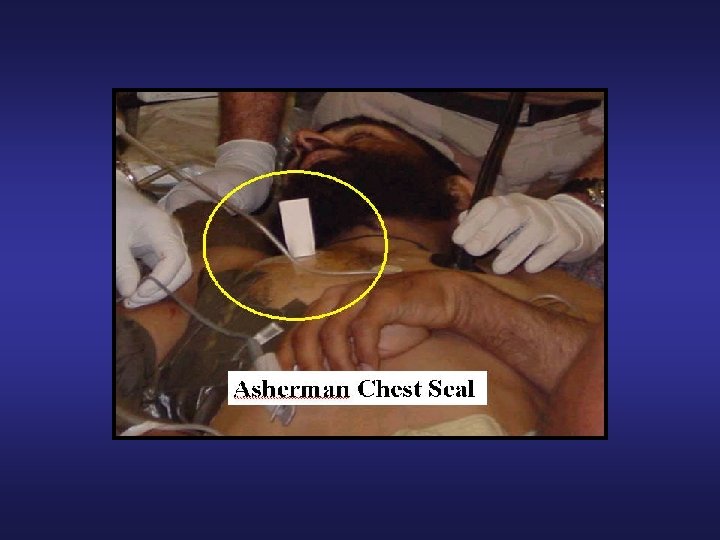

Tactical Field Care: Breathing • Progressive respiratory distress in the presence of unilateral penetrating chest trauma should be considered tension pneumothorax • Tension pneumothorax is the 2 nd leading cause of preventable death on the battlefield • Cannot rely on typical signs such as shifting trachea, etc. • Needle chest decompression is life-saving
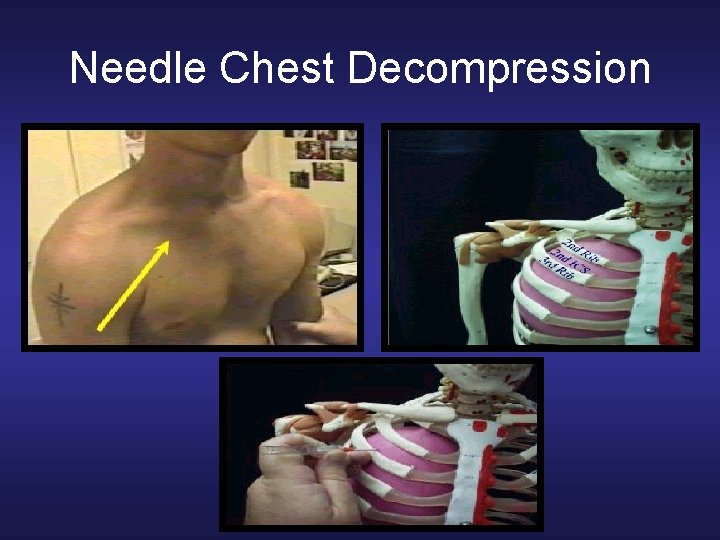
Needle Chest Decompression

Tactical Field Care: Circulation • Any bleeding site not previously controlled should now be addressed • Only the absolute minimum of clothing should be removed, although a thorough search for additional injuries must be performed

Tactical Field Care: Circulation • Apply a tourniquet to a major amputation of the extremity • Apply an emergency trauma bandage and direct pressure to a severely bleeding wound • If a tourniquet was previously applied, consider changing to a pressure dressing and/or using hemostatic dressings (Hem. Con) or hemostatic powder (Quik. Clot) to control any additional hemorrhage

Chitosan Hemostatic Dressing • Apply directly to bleeding site and hold in place 2 minutes • If dressing is not effective in stopping bleeding after 4 minutes, remove original and apply a new dressing

Chitosan Hemostatic Dressing • Additional dressings cannot be applied over ineffective dressing • Apply a battle dressing/bandage to secure hemostatic dressing in place • Hemostatic dressings should only be removed by responsible persons after evacuation to the next level of care

Tactical Field Care: Shock • Hypovolemic shock results when there is a sudden decrease in the amount of fluid in the casualty’s circulatory system. • Heat stroke, diarrhea, and dysentery can also cause hypovolemic shock. • The casualty may also have internal bleeding, such as bleeding into the abdominal or chest cavities.

Tactical Field Care: IV fluids • FIRST, STOP THE BLEEDING! • IV access should be obtained using a single 18 gauge catheter because of the ease of starting • A saline lock may be used to control IV access in absence of IV fluids • Ensure IV is not started distal to a significant wound

Reasons NOT to Start IVs on All Combat Casualties • Minimize interference with combatants who can continue to participate in the engagement • Conserve limited IV fluid supplies • Attend to casualties with more severe wounds • Avoid delaying tactical movement - waiting 5 minutes to start an IV may get 5 members of your team killed
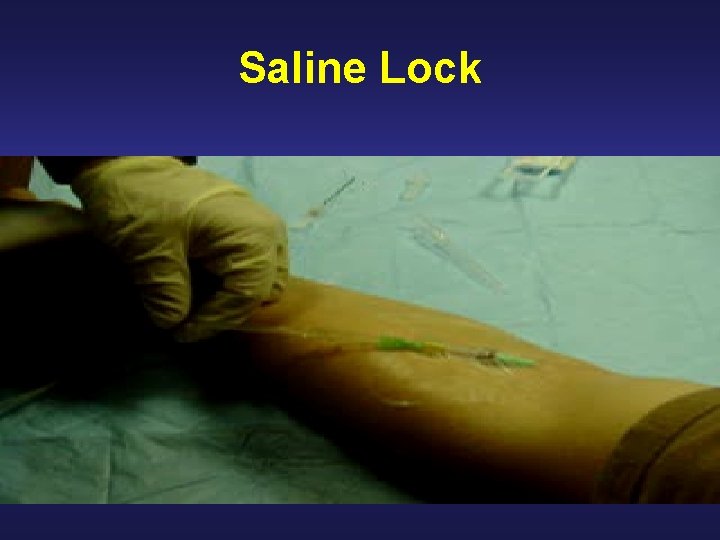
Saline Lock

Tactical Field Care: Additional injuries • Splint fractures as circumstances allow while verifying pulse and prepare for evacuation • Administer the Soldier’s Combat Pill Pack
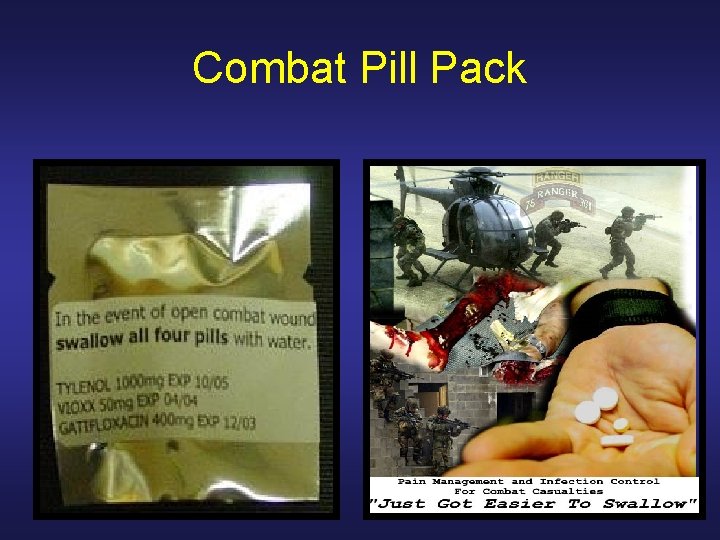
Combat Pill Pack

Warning! • Do not take aspirin, ibuprofen (Motrin) or related medications while in theater • Interfere with blood clotting • Increase risk of fatal hemorrhage if wounded

Tactical Field Care: • Communicate: Let your unit leader know the casualty’s condition: Will casualty return to duty? Does the casualty require medical evac to save life or limb? Non-medical evac? • Initiate a Field Medical Card (DD Form 1380) • Monitor the casualty: Airway, breathing, bleeding, and IV infusion

Combat Casualty Evacuation Care

Casevac Care • If the casualty requires evacuation, prepare the casualty • Use a blanket to keep the casualty warm • If the casualty is to be evacuated by medical transport, you may need to prepare and transmit a MEDEVAC request
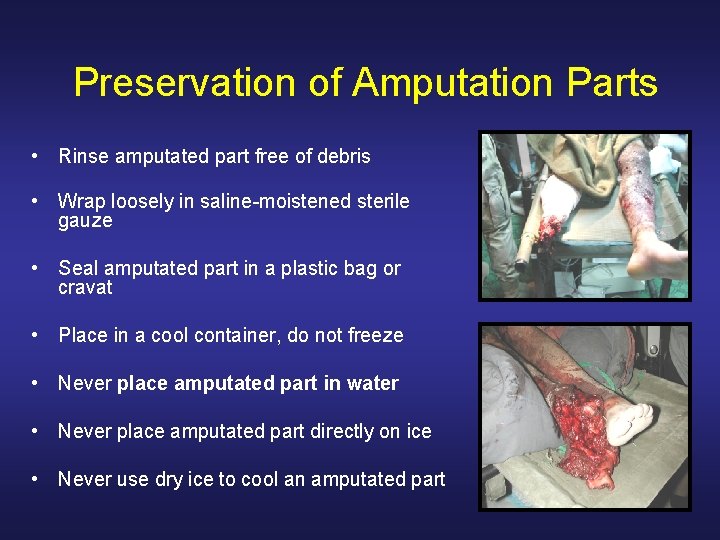
Preservation of Amputation Parts • Rinse amputated part free of debris • Wrap loosely in saline-moistened sterile gauze • Seal amputated part in a plastic bag or cravat • Place in a cool container, do not freeze • Never place amputated part in water • Never place amputated part directly on ice • Never use dry ice to cool an amputated part

Casevac Care • Use a SKED litter or improvised litter if the casualty must be moved to a casualty collection point • If transported by a non-medical vehicle (CASEVAC), you may need to arrange the vehicle to accommodate the casualty • If an unconscious casualty is transported on a non-medical vehicle, you may need to accompany the casualty and render additional care as needed • Restock your aid bag when possible

Summary • There are three categories of casualties on the battlefield: 1. Soldiers who will live regardless 2. Soldiers who will die regardless 3. Soldiers who will die from preventable deaths unless proper life-saving steps are taken immediately (7 -15%)
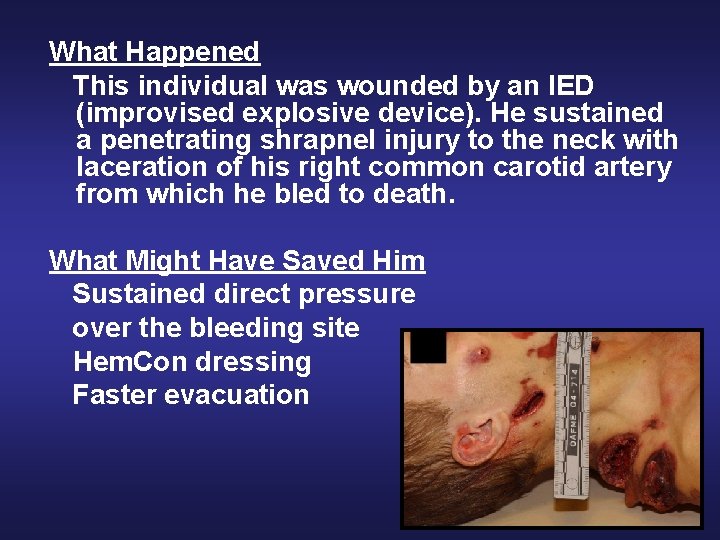
What Happened This individual was wounded by an IED (improvised explosive device). He sustained a penetrating shrapnel injury to the neck with laceration of his right common carotid artery from which he bled to death. What Might Have Saved Him Sustained direct pressure over the bleeding site Hem. Con dressing Faster evacuation
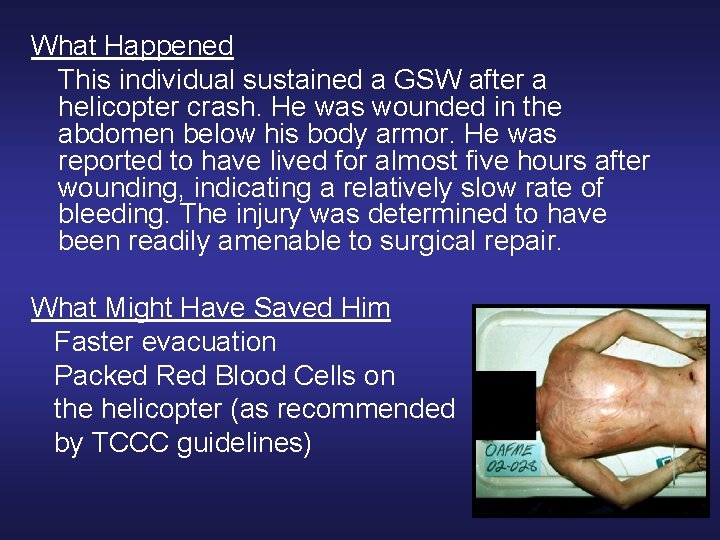
What Happened This individual sustained a GSW after a helicopter crash. He was wounded in the abdomen below his body armor. He was reported to have lived for almost five hours after wounding, indicating a relatively slow rate of bleeding. The injury was determined to have been readily amenable to surgical repair. What Might Have Saved Him Faster evacuation Packed Red Blood Cells on the helicopter (as recommended by TCCC guidelines)
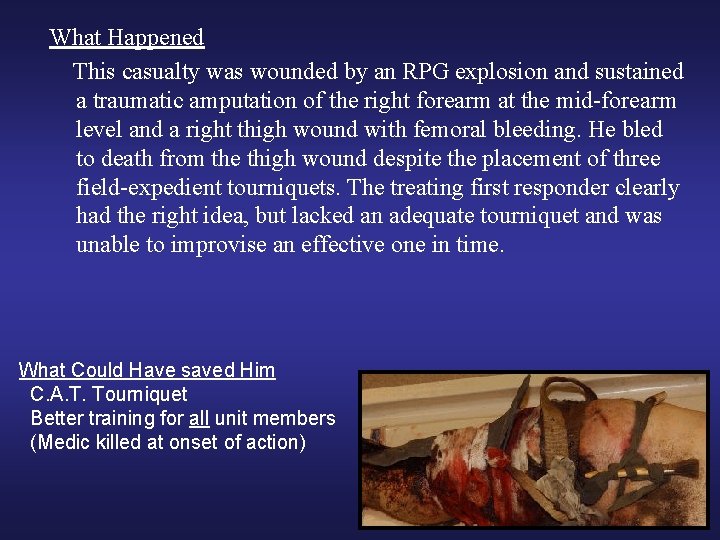
What Happened This casualty was wounded by an RPG explosion and sustained a traumatic amputation of the right forearm at the mid-forearm level and a right thigh wound with femoral bleeding. He bled to death from the thigh wound despite the placement of three field-expedient tourniquets. The treating first responder clearly had the right idea, but lacked an adequate tourniquet and was unable to improvise an effective one in time. What Could Have saved Him C. A. T. Tourniquet Better training for all unit members (Medic killed at onset of action)

What Happened This casualty sustained a gunshot wound to his upper thigh at an anatomic location too high for effective use of a tourniquet. What Could Have Saved Him Sustained direct pressure on the wound or Pressure on the femoral artery at the pressure point or Hem. Con dressing and Faster evacuation

TCCC in IRAQ The adoption and implementation of the principles of TCCC by the medical platoon of TF 1 -15 IN in OIF 1 resulted in overwhelming success. Over 25 days of continuous combat with 32 friendly casualties, many of them serious, we had 0 KIAs and 0 Died From Wounds, while simultaneously caring for a significant number of Iraqi civilian and military casualties.

TCCC in IRAQ (cont) This success should serve as a model for other conventional combat units throughout the army involved in Level 1 treatment. The principles of TCCC are well-researched and proven effective and should be the foundation of the treatment of battlefield casualties. CPT Michael Tarpey Battalion Surgeon 1 -15 IN 20 January 2005

Summary “If during the next war you could do only two things, (1) place a tourniquet and (2) treat a tension pneumothorax, then you can probably save between 70 and 90 percent of all the preventable deaths on the battlefield. ” -COL Ron Bellamy

QUESTIONS?
- Slides: 67