Penumbra Imaging in Acute Stroke Is it Useful

Penumbra Imaging in Acute Stroke: Is it Useful? Lawrence R. Wechsler, M. D. Professor and Chair, Department of Neurology University of Pittsburgh

Lawrence R. Wechsler, MD § Ownership Interest (Stocks, Stock Options or Ownership Interest) – Neuro Interventional Therapeutic
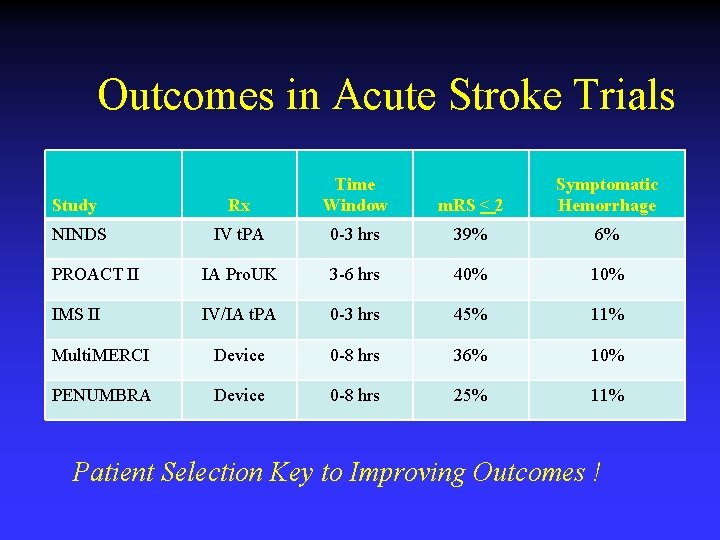
Outcomes in Acute Stroke Trials Study Rx Time Window m. RS < 2 Symptomatic Hemorrhage NINDS IV t. PA 0 -3 hrs 39% 6% PROACT II IA Pro. UK 3 -6 hrs 40% 10% IMS II IV/IA t. PA 0 -3 hrs 45% 11% Multi. MERCI Device 0 -8 hrs 36% 10% PENUMBRA Device 0 -8 hrs 25% 11% Patient Selection Key to Improving Outcomes !
Acute Stroke Therapy: Penumbra
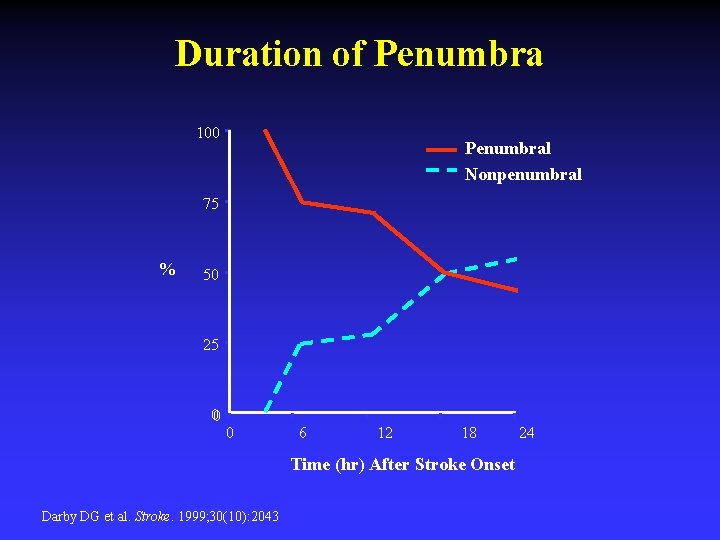
Duration of Penumbra 100 Penumbral Nonpenumbral 75 % 50 25 0 0 6 12 18 Time (hr) After Stroke Onset Darby DG et al. Stroke. 1999; 30(10): 2043 24
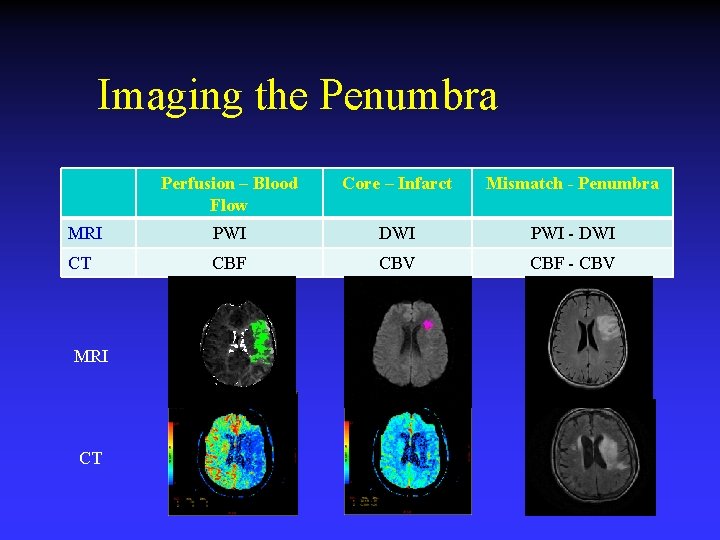
Imaging the Penumbra Perfusion – Blood Flow Core – Infarct Mismatch - Penumbra MRI PWI DWI PWI - DWI CT CBF CBV CBF - CBV MRI CT
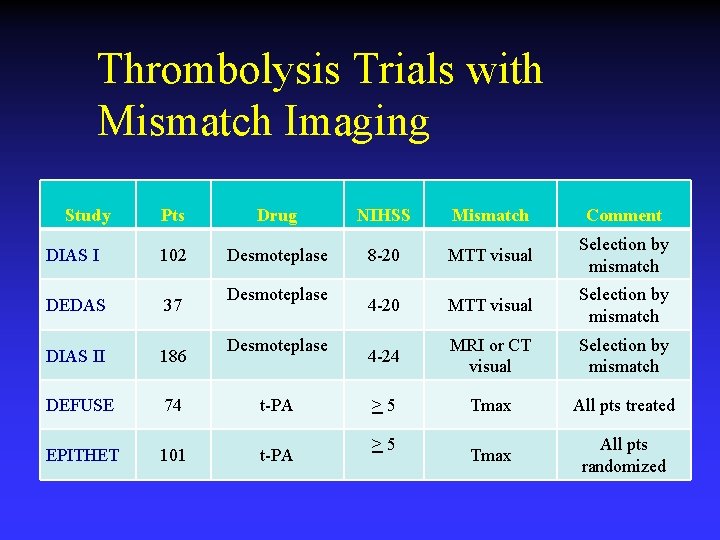
Thrombolysis Trials with Mismatch Imaging Study Pts Drug NIHSS Mismatch Comment DIAS I 102 Desmoteplase 8 -20 MTT visual Selection by mismatch DEDAS 37 4 -20 MTT visual Selection by mismatch DIAS II 186 4 -24 MRI or CT visual Selection by mismatch DEFUSE 74 t-PA >5 Tmax All pts treated EPITHET 101 t-PA Tmax All pts randomized Desmoteplase >5
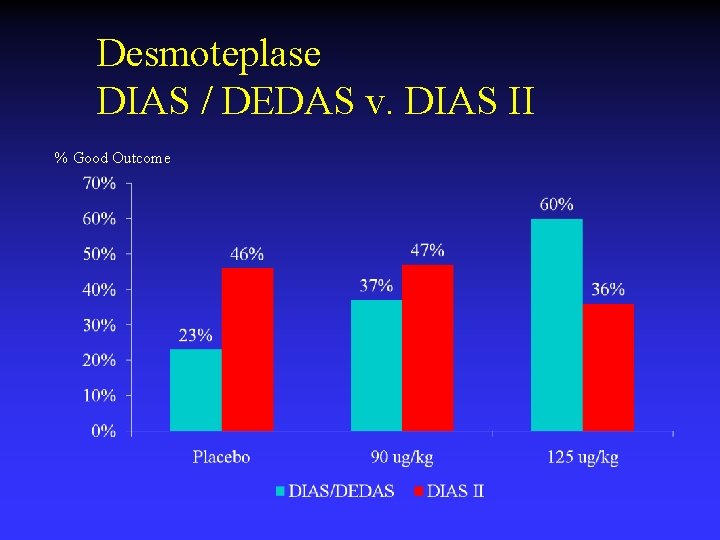
Desmoteplase DIAS / DEDAS v. DIAS II % Good Outcome
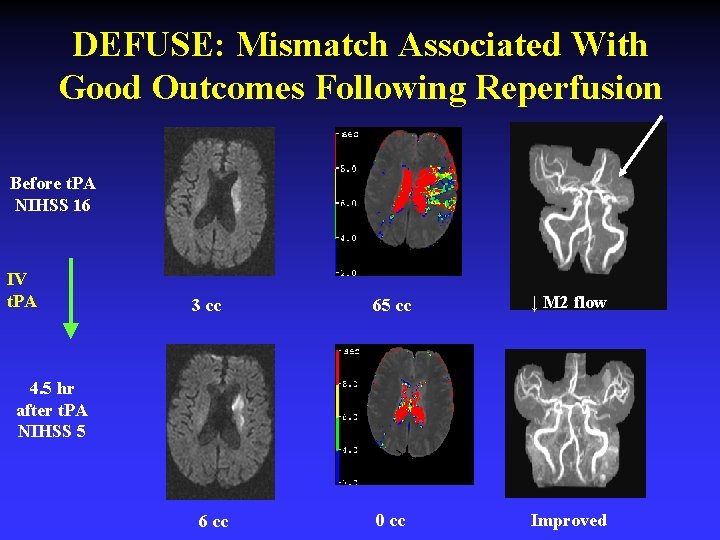
DEFUSE: Mismatch Associated With Good Outcomes Following Reperfusion Before t. PA NIHSS 16 IV t. PA 3 cc 65 cc ↓ M 2 flow 0 cc Improved 4. 5 hr after t. PA NIHSS 5 6 cc
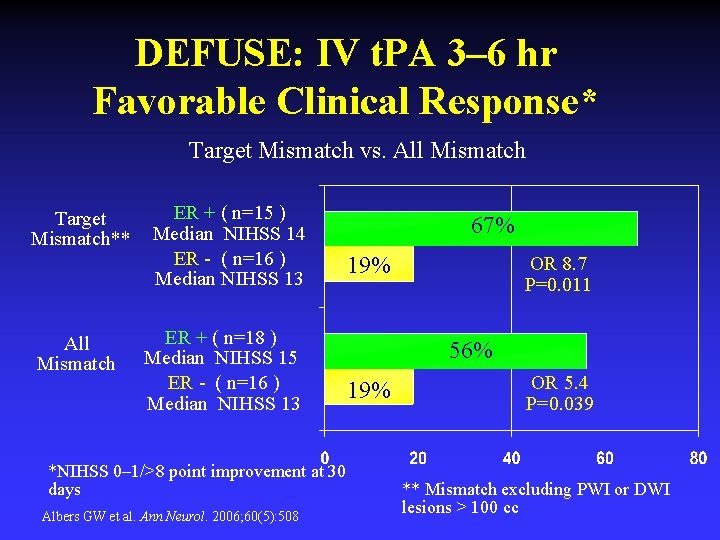
DEFUSE: IV t. PA 3– 6 hr Favorable Clinical Response* Target Mismatch vs. All Mismatch Target Mismatch** All Mismatch ER + ( n=15 ) Median NIHSS 14 ER - ( n=16 ) Median NIHSS 13 ER + ( n=18 ) Median NIHSS 15 ER - ( n=16 ) Median NIHSS 13 *NIHSS 0– 1/>8 point improvement at 30 days Albers GW et al. Ann Neurol. 2006; 60(5): 508 67% 19% OR 8. 7 P=0. 011 56% 19% OR 5. 4 P=0. 039 ** Mismatch excluding PWI or DWI lesions > 100 cc
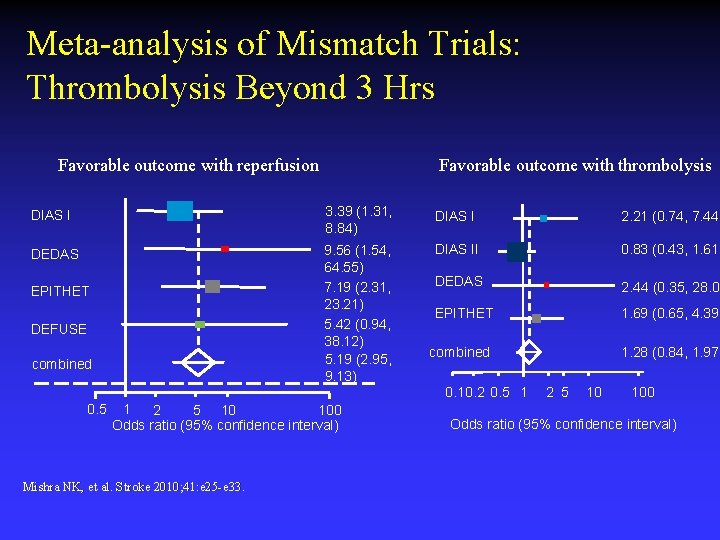
Meta-analysis of Mismatch Trials: Thrombolysis Beyond 3 Hrs Favorable outcome with reperfusion Favorable outcome with thrombolysis DIAS I 3. 39 (1. 31, 8. 84) DIAS I 2. 21 (0. 74, 7. 44) DEDAS 9. 56 (1. 54, 64. 55) 7. 19 (2. 31, 23. 21) 5. 42 (0. 94, 38. 12) 5. 19 (2. 95, 9. 13) DIAS II 0. 83 (0. 43, 1. 61) DEDAS 2. 44 (0. 35, 28. 02 EPITHET 1. 69 (0. 65, 4. 39) combined 1. 28 (0. 84, 1. 97) EPITHET DEFUSE combined 0. 10. 2 0. 5 1 2 5 10 100 Odds ratio (95% confidence interval) Mishra NK, et al. Stroke 2010; 41: e 25 -e 33. 2 5 10 100 Odds ratio (95% confidence interval)
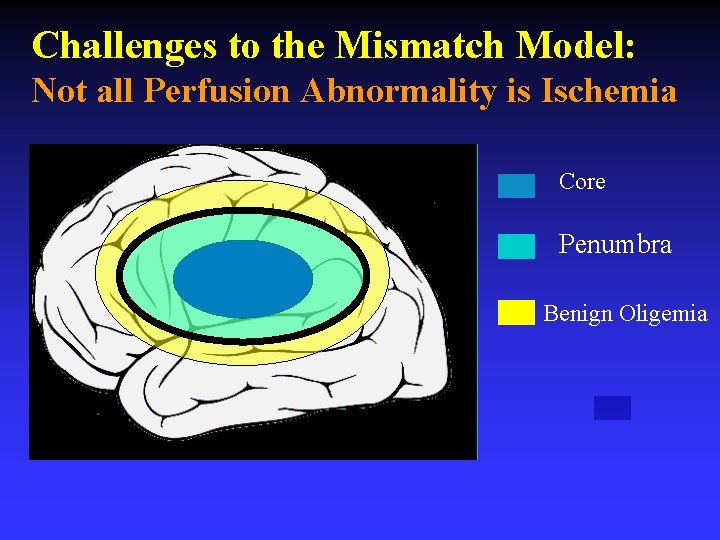
Challenges to the Mismatch Model: Not all Perfusion Abnormality is Ischemia Core Penumbra Benign Oligemia
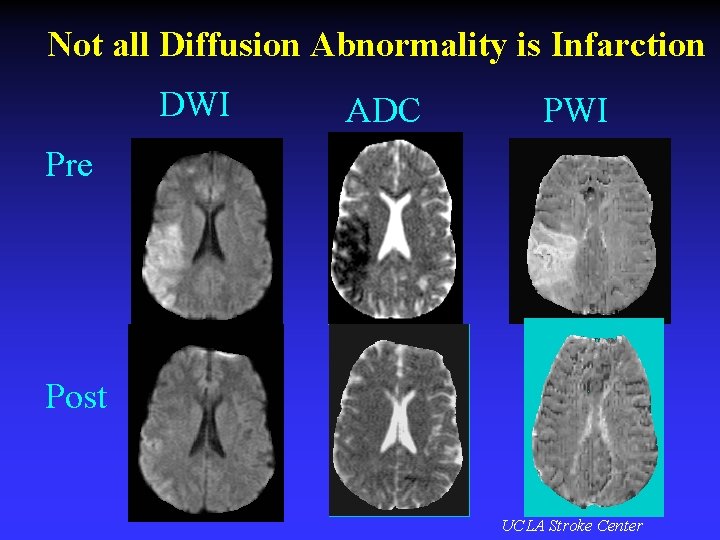
Not all Diffusion Abnormality is Infarction DWI ADC PWI Pre Post UCLA Stroke Center
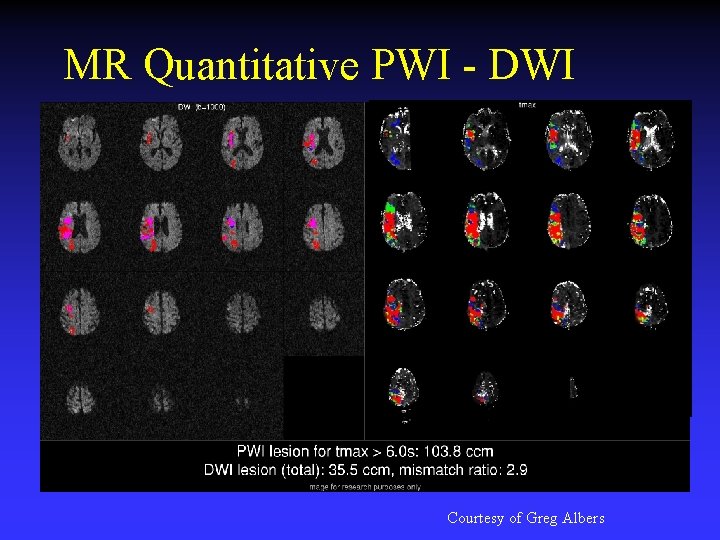
MR Quantitative PWI - DWI Courtesy of Greg Albers

Reversible Pattern • Perfusion MR or CT • Sufficiently reduced to cause infarction if not reperfused • Salvage with reperfusion • Diffusion / CBV • Infarction not large enough to cause severe deficit • Exclude malignant pattern

Summary • Key to improving outcomes is patient selection • Penumbra imaging may identify patients likely to benefit from intervention and those likely to be harmed • Additional time for penumbra imaging must be justified by improved outcomes
- Slides: 16