PELVIC INFLAMMATORY DISEASE CONTENTS OBJECTIVES INTRODUCTION DEFINITION AND

PELVIC INFLAMMATORY DISEASE

CONTENTS OBJECTIVES INTRODUCTION, DEFINITION AND EPIDEMIOOGY AETIOLOGY NATURAL DEFECES PREDISPOSING FACTORS PATHOPHYSIOLOGY/MODE OF SPREAD APPROACH DIAGNOSIS CRITERIA AND DIFFERENTIALS CHRONIC PID AND PELVIC TB SEVERITY SCORING SEQUELAE PREVENTION FINAL WORDS AND OBJECTIVES REVIEW BIBLOGRAPHY

INTRO. AND DEF. AND EPID is a syndrome in which there is usually an ascending spread of microorganisms from the lower genital tract to the upper genital tract. 8% of all admissions at gynae Ward at the Korle-Bu teaching Hospital(Ghana). Occurs in 11% of women of reproductive age (USA) 25% occurs in teenage girls
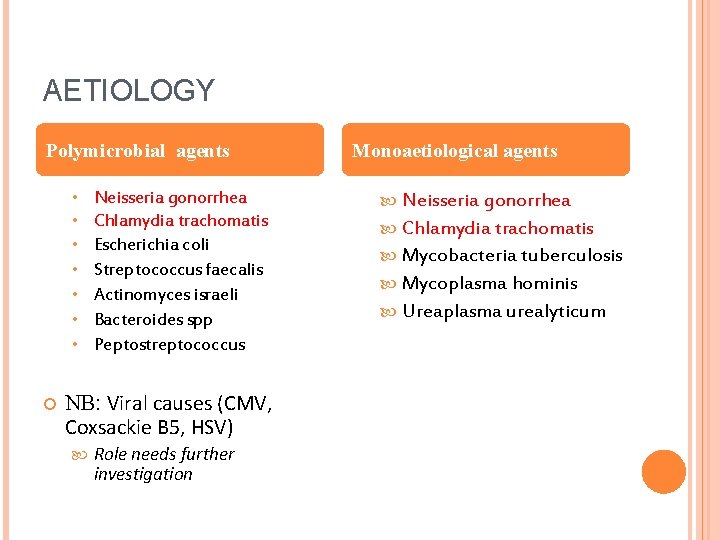
AETIOLOGY Polymicrobial agents • • Neisseria gonorrhea Chlamydia trachomatis Escherichia coli Streptococcus faecalis Actinomyces israeli Bacteroides spp Peptostreptococcus NB: Viral causes (CMV, Coxsackie B 5, HSV) Role needs further investigation Monoaetiological agents Neisseria gonorrhea Chlamydia trachomatis Mycobacteria tuberculosis Mycoplasma hominis Ureaplasma urealyticum

NATURAL DEFENCES AGAINST SPREAD OF INFECTION 1. 2. 3. 4. Vulva (introitus closure; fungicidal apocrine gland secretions) Vagina (lactobacilli produce acid) Cervix (closure of cervix by bacteriolytic mucous plug) Endometrium (regular shedding)

PREDISPOSING FACTORS Sexual activity(multiple partners) History of prior STI Age IUCD (2 to 9 -fold incr risk) Douching Smoking Iatrogenic [HSG, D/C] Previous history of PID

PATHOPHYSIOLOGY AKA SPREAD Ascending infection Uterine muscular activity Vectors(spermatozoa) Intra-uterine manipulation(IUCD, HSG, D&C Menstruation/miscarraige/childbirth Haematogenous spread [pelvic TB] Contiguous spread [acute appendicitis or acute diverticulitis]

APPROACH HISTORY ü ü 1. Asymptomatic Symptomatic: mild to toxic Abdominal pain (90%) – dull, aching or crampy, bilateral, and constant; it usu begins a few days after the onset of the last menstrual period and tends to be accentuated by motion, exercise, or coitus with about 7 days duration; associated with dysuria, dyspareunia & dysmenorhoea 2. Abnormal vaginal discharge (75%) EXAMINATION 1. Fever >38°c 2. Tachycardia 3. Low abdominal tenderness with features of peritonitis 4. Cervical excitation tenderness 5. Bilateral adnexal tenderness 6. Palpable mass on pelvic examination Bleeding/abnormal discharge on vaginal examination 3. Irregular vaginal bleeding (35 – 40%) 4. Fever, nausea & vomiting 7.

DIAGNOSIS CRITERIA All 3 of these : Lower abdominal tenderness Adnexal tenderness Cervical excitation tenderness and at least 1 of the following 1. 2. 3. 4. 5. Case surveillance definition of chlamydia or gonorrhoea infection Temperature ≥ 38ºC Leucocytosis > 10, 000 wbc/mm 3 Abnormal cervical or vaginal mucopurulent discharge Elevated ESR and CRP 6. Purulent material in peritoneal cavity obtained by culdocentesis or laparoscopy Pelvic abscess or inflammatory complex on bimanual examination or ultrasonography Patient is a sexual contact of a person known to have gonorhoea, chlamydia or non-gonococcal urethritis 7. 8.

DIFFERENTIALS Acute Appendicitis Adnexal tumours Ectopic Pregnancy Endometriosis Interstitial Cystitis Ovarian cysts Ovarian Torsion Ectopic Pregnancy Ovarian Tumour

INVESTIGATIONS 1. Hematological 2. Microbiology 3. FBC, ESR, C-reactive protein NB: preg test r/o ectopic pregnancy vaginal wet mount (increased white cell) endocervical swab urethral, rectal & oropharyngeal swabs esp if gonorrhoea is suspected Imaging techniques A) Ultrasonography (Transvaginal) - thickened fluid filled tubes (cogwheel sign) - free fluid in pouch of Douglas - demonstrates adnexal mass or abscess - has poor sensitivity (81%) and specificity (78%)
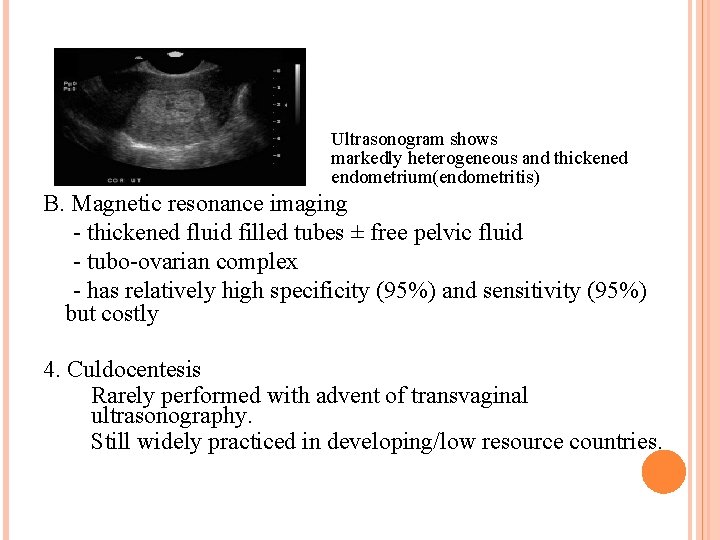
Ultrasonogram shows markedly heterogeneous and thickened endometrium(endometritis) B. Magnetic resonance imaging - thickened fluid filled tubes ± free pelvic fluid - tubo-ovarian complex - has relatively high specificity (95%) and sensitivity (95%) but costly 4. Culdocentesis Rarely performed with advent of transvaginal ultrasonography. Still widely practiced in developing/low resource countries.

5. Laparascopy Gold standard for diagnosis Minimal visual criteria : i. hyperaemia of external tubal surface ii. Oedema of the tubal wall iii. Sticky exudate on tubal surface and/or from the fimbriated end when patent 6. Endometrial biopsy histopathologic diagnosis of endometritis; Endometrial biopsy is approximately 90% specific and 90% sensitive. CDC recommend it in women undergoing laparoscopy with no visible signs of salpingitis. requires specialized skills

TREATMENT Choice of antibiotic should be guided by : 1. Patient’s information 2. Severity of signs & symptoms 3. Knowledge of the drug (*criminal offence*) Broadly: - Medical (33 -75% success used alone) - Surgical (simple drainage, adhesiolysis, and copious irrigation or unilateral adnexectomy, ect if possible – 15 -20% cases it is required) NB: IUCD removal?

INDICATIONS FOR HOSPITALIZATION AND INPATIENT CARE Uncertain diagnosis Surgical emergencies (eg. When acute appendicitis and ectopic preg are not definitely excluded) Pelvic abscess is suspected Severe illness The patient is pregnant Patient is unable to follow or tolerate outpatient Regimen Previous failure with outpatient management(after 72 hrs) Patient is prepubertal/nulliparous(admit in order to preserve her fertility and improve her compliance) Immunodeficiency (eg, patients with HIV infection who have a low CD 4 count or patients who are using immunosuppressive medications)

ANTIBIOTIC RX. OUTPATIENT Regimen INPATIENT Regimen A Ceftriaxone 250 mg intramuscularly (IM) once as a single dose plus Doxycycline 100 mg orally twice daily for 14 days Metronidazole 500 mg orally twice daily for 14 days (if vaginitis suspected) Regimen B Cefoxitin 2 g IM once as a single dose concurrently with probenecid 1 g orally in a single dose Doxycycline 100 mg orally twice daily for 14 days Metronidazole 500 mg orally twice daily for 14 days (suspected vaginitis) Regimen A Cefoxitin 2 g IV every 6 hours or cefotetan 2 g IV every 12 hours plus Doxycycline 100 mg orally or IV every 12 hours Regimen B Clindamycin 900 mg IV every 8 hours plus Gentamicin IV in a loading dose of 2 mg/kg, followed by a maintenance dosage of 1. 5 mg/kg q 8 h

CONTACT TRACING 75% of men with chlamydia or non-specific urethritis will be asymptomatic Women Rx for PID must abstain from coitus until their partner is checked and Rx Examine and Rx all sexual contacts in the 60 days preceeding onset of symptoms

CHRONIC PID Implies presence of tissue changes in tubes, ovaries, and parametrieum Long term benefits of antibiotics questionable Surgical procedures such as adhesiolysis, adnexetomy and/or TAH may be applicable Symptomatic relief with analgesia

PELVIC TUBERCULOSIS M. TB used to be a notorious cause of pelvic infection, but incidence waned down with advent of antibiotics. Re-emerge especially in developing world due to increase immunosupression. Primary site of infection is lungs, via lymphohematogenous route pelvic structures gets affected(chronic salpingitis, endometritis and peritonitis). Common presentation is infertility and mestrual disorders(oligo-/amenorrhoea and menorrhagia) Extremely dense adhesions seen. ZN-stain for AFB; samples from endometrial and peritonial biopsies; Laparoscopy is also useful in dx of pelvic TB. Rx usually is mainly medical with varying combination of anti-TB drugs. Surgery indicated in cases of unresolved masses with medical Rx.
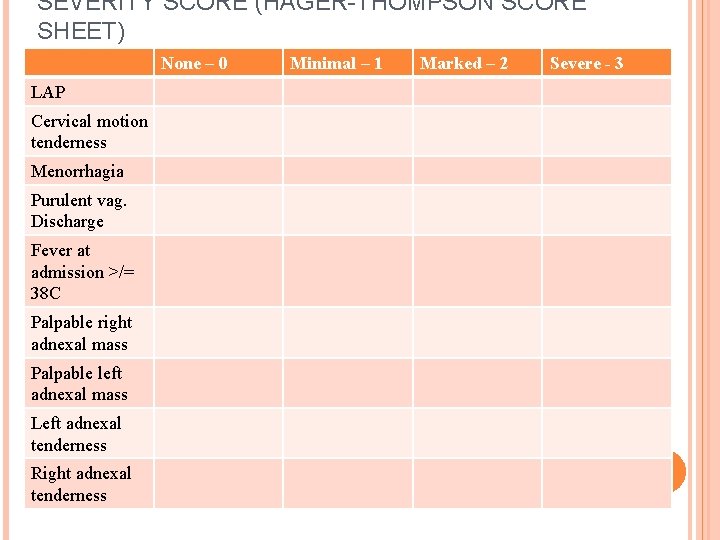
SEVERITY SCORE (HAGER-THOMPSON SCORE SHEET) None – 0 LAP Cervical motion tenderness Menorrhagia Purulent vag. Discharge Fever at admission >/= 38 C Palpable right adnexal mass Palpable left adnexal mass Left adnexal tenderness Right adnexal tenderness Minimal – 1 Marked – 2 Severe - 3

SEQUELAE/CONSEQUENCIES Repeat infection Once (20%) Twice (56%) Chronic abdominal pain(15 -20%) Ectopic pregnancy: 7 -fold incr in incidence Infertility: the risk is one episode is 11%, two in 34%, three in 54%. Peritonitis Fitz-Hugh-Curtis syndrome Mortality

PREVENTION Primary Improved education Avoid risky sexual behaviour Pre-operative antibiotic cover for vaginal procedures Barrier contraceptives Adequate treatment of STIs and lower GTIs Topical vaccines and lactobacilli suppositories(research) Secondary – proper and early diagnosis and mgt of upper genital tract infection to prevent progress and complications Tertiary – mgt of complications NB: BLT not preventive measure Rx of sexual partners

ABNORMAL UTERINE BLEEDING Change in frequency, duration and amount of menstrual bleeding

DEFINITIONS Normal menses Every 28 days Mean +/- 7 days duration is 4 days. More than 7 days is abnormal.

Normal Menses AVERAGE BLOOD LOSS WITH MENSTRUATION IS 35 -50 CC. 95% OF WOMEN LOSE <60 CC.
DEFINITIONS Menorrhagia: Prolonged bleeding > 7 days or > 80 cc occurring at regular intervals.

FREQUENCY OF AUB Menorrhagia occurs in 9 -14% of healthy women. Most common Gyn disorder of reproductive age women

DEFINITIONS Metrorrhagia: Uterine bleeding occurring at irregular but frequent intervals.

DEFINITIONS Menometrorrhagia: Prolonged uterine bleeding occurring at irregular intervals.

DEFINITIONS Oligomenorrhea: • Reduction in frequency of menses • Between 35 days and 6 months.

DEFINITIONS AMENORRHEA: • Primary amenorrhea • Secondary amenorrhea Ø No menses for 3 -6 months

PRIMARY AMENORRHEA • No menses by age 13 • No secondary sexual development No menses by age 15 Secondary sexual development present

DEFINITIONS Menarche average Menopause average 12. 43 years age 51. 4 years Ovulatory cycles for over 30 years

MENSTRUAL BLEEDING STOPS IF: Prostaglandins cause contractions and expulsion Endometrial healing and cessation of bleeding with increasing estrogen

SYSTEMIC ETIOLOGIES Coagulation ITP Von. Willebrand’s defects

ROUTINE SCREENING FOR COAGULATION DEFECTS SHOULD BE RESERVED FOR THE YOUNG PATIENT WHO HAS HEAVY FLOW WITH THE ONSET OF MENSTRUATION. Comprehensive Gynecology, 4 th edition

VON WILLEBRAND’S DISEASE IS THE MOST COMMON INHERITED BLEEDING DISORDER WITH A FREQUENCY OF 1/800 -1000. Harrison’s Principles of Internal Medicine, 14 th edition

HYPOTHYROIDISM CAN BE ASSOCIATED WITH MENORRHAGIA OR METRORRHAGIA. THE INCIDENCE HAS BEEN REPORTED TO BE 0. 3 -2. 5%. Wilansky, et al. , 1989

MOST COMMON CAUSES OF REPRODUCTIVE TRACT AUB Pre-menarchal Foreign body Reproductive Gestational age event Post-menopausal Atrophy

REPRODUCTIVE TRACT CAUSES Gestational events Malignancies Benign Atrophy Leiomyoma Polyps Cervical lesions Foreign body Infections

REPRODUCTIVE TRACT CAUSES Gestational events Abortions Ectopic pregnancies Trophoblastic disease IUP

FIGO SYSTEM PALM-COEIN Polyp Adenomyosis Leiomyoma Malignancy and hyperplasia Coagulopathy Ovulatory disorders Endometrium Iatrogenic Not classified

REPRODUCTIVE TRACT CAUSES OF BENIGN ORIGIN Uterine Vaginal or labial lesions Cervical lesions Urethral lesions GI

REPRODUCTIVE TRACT CAUSES OF BENIGN ORIGIN Uterine Pregnancy Leiomyomas Polyps Hyperplasia Carcinoma

PROPOSED ETIOLOGIES OF MENORRHAGIA WITH LEIOMYOMA Increased vessel number Increased endometrial surface area Impeded uterine contraction with menstruation Clotting less efficient locally Wegienka, et al. , 2003

LEIOMYOMA IN ANY LOCATION IS ASSOCIATED WITH INCREASED RISKS OF GUSHING OR HIGH PAD/TAMPON USE. Wegienka, et al. , 2003

REPRODUCTIVE TRACT CAUSES OF BENIGN ORIGIN Uterine Vaginal or labial lesions Carcinoma Sarcoma Adenosis Lacerations Foreign body

REPRODUCTIVE TRACT CAUSES OF BENIGN ORIGIN Uterine Vaginal or labial lesions Cervical lesions Polyps Condyloma Cervicitis Neoplasia
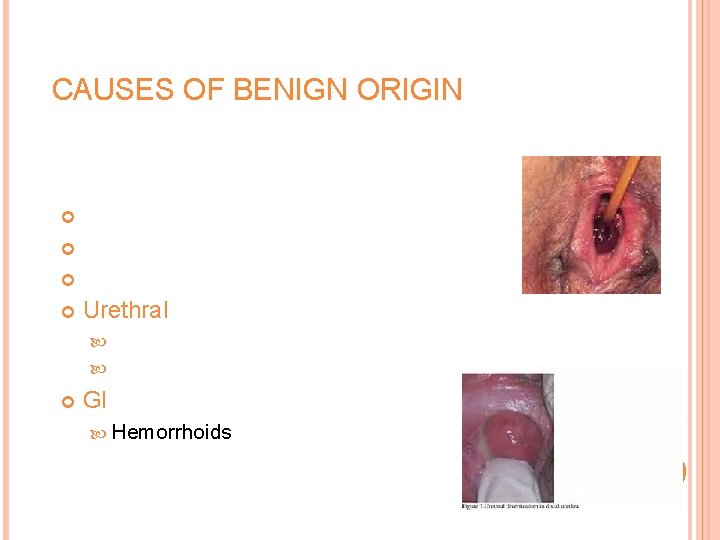
CAUSES OF BENIGN ORIGIN Uterine Vaginal or labial lesions Cervical lesions Urethral Caruncle Diverticulum GI Hemorrhoids

IATROGENIC CAUSES OF AUB Intra-uterine device Oral and injectable steroids Psychotropic drugs MAOI’s

Physiology of Abnormal Uterine Bleeding WITH ANOVULATION A CORPUS LUTEUM IS NOT PRODUCED AND THE OVARY THEREBY FAILS TO SECRETE PROGESTERONE.

HOWEVER, ESTROGEN PRODUCTION CONTINUES, RESULTING IN ENDOMETRIAL PROLIFERATION AND SUBSEQUENT AUB.

PGE 2 VASODILATION PGF 2Α VASOCONSTRICTION Progesterone is necessary to increase arachidonic acid, the precursor to PGF 2α. With decreased progesterone there is a decreased PGF 2α/PGE 2 ratio.

EVALUATION AND WORK -UP: EARLY REPRODUCTIVE YEARS/ADOLESCENT Thorough history Screen for eating disorder Labs: CBC, PT, PTT, FSH, TSH, h. CG

EVALUATION AND WORK -UP: WOMEN OF REPRODUCTIVE AGE h. CG, LH/FSH, CBC, TSH Cervical cultures U/S Hysteroscopy EMB

EVALUATION AND WORK -UP: POST-MENOPAUSAL WOMEN Transvaginal EMB U/S

BIBLOGRAPGY Ten teachers – Gynecology 18 th Edition Obstetrics and Gynecology – Akin Agboola (? Edition) Obstetrics and Gynecology Handbook – Kwame (? Edition) Med. Scape 2014 PID – Dr. Patrick`s lecture 2012 PID case Presentation 2014 – Mr. Kitabu Jammeh (Medical Student, 9 th Cohort, UTG)
- Slides: 57