Pelvic Floor Health Monica White PT DPT PRCP












- Slides: 16

Pelvic Floor Health Monica White, PT, DPT, PRCP

A little about me Cedar Valley Medical Specialists

What is Pelvic Physical Therapy? • Pelvic floor physical therapy involves treating the pelvic floor muscle group, which is responsible for a variety of functions related to the vagina, bladder and bowels.

Common Conditions I treat • Urinary incontinence, urgency, frequency • Fecal incontinence • Constipation • Postoperative prostatectomy • Postoperative hysterectomy symptoms • prolapse of the bladder, rectum or uterus • Coccyx pain • Irritable bowel syndrome • Pelvic and genital pain • Pain with intercourse • bedwetting in children

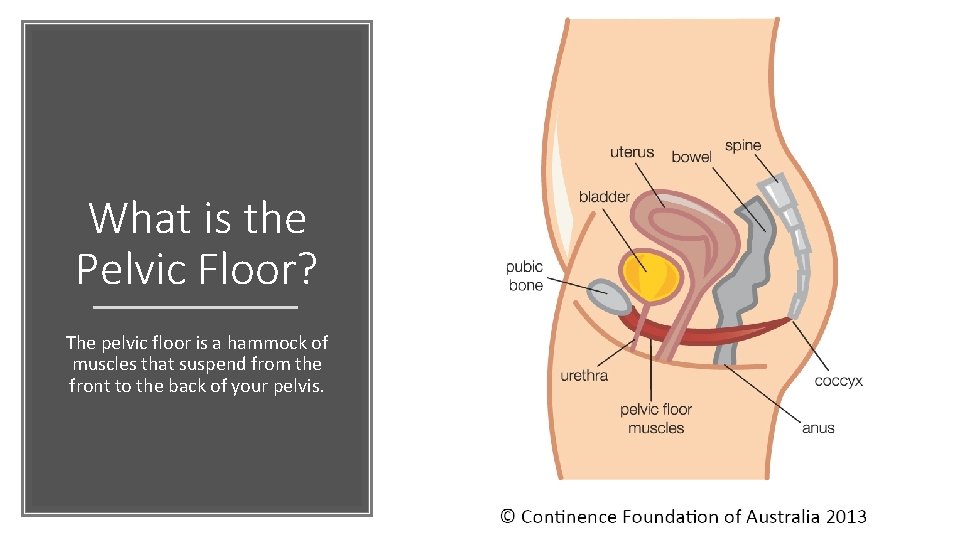
What is the Pelvic Floor? The pelvic floor is a hammock of muscles that suspend from the front to the back of your pelvis.

Pelvic Floor Anatomy

Functions of the Pelvic Floor • Sphincter Control: The pelvic floor muscles contract to prevent incontinence(leaking), relax to allow us to urinate or defecate. • Support of pelvic organs-the pelvic floor forms a shelf holding up your internal organs. ---bladder, uterus, colon • Postural stabilizer-the pelvic floor contracts prior to or with most movements to assist with postural core stabilization • These ‘core’ muscles work to support you during movement like standing

Functions of the Pelvic Floor • Sexual Appreciation-The pelvic floor muscles in women must relax to receive comfortable penetration and deliver babies. They are also very important for arousal and orgasm • Sump Pump-Functional use of these muscles throughout the day helps pump venous and lymphatic fluid around the legs and abdomen back to the heart for circulation

Okay, so what happens when the pelvic floor isn’t functioning properly • Urinary incontinence &/Or fecal incontinence- can be caused by weakness or poor coordination of the pelvic floor muscle • No amount of incontinence is acceptable LADIES!

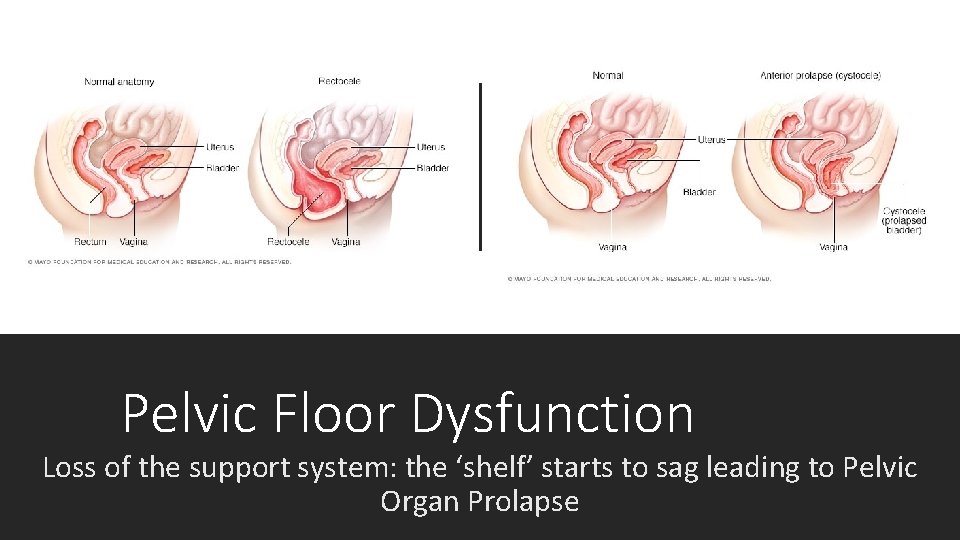
Pelvic Floor Dysfunction Loss of the support system: the ‘shelf’ starts to sag leading to Pelvic Organ Prolapse

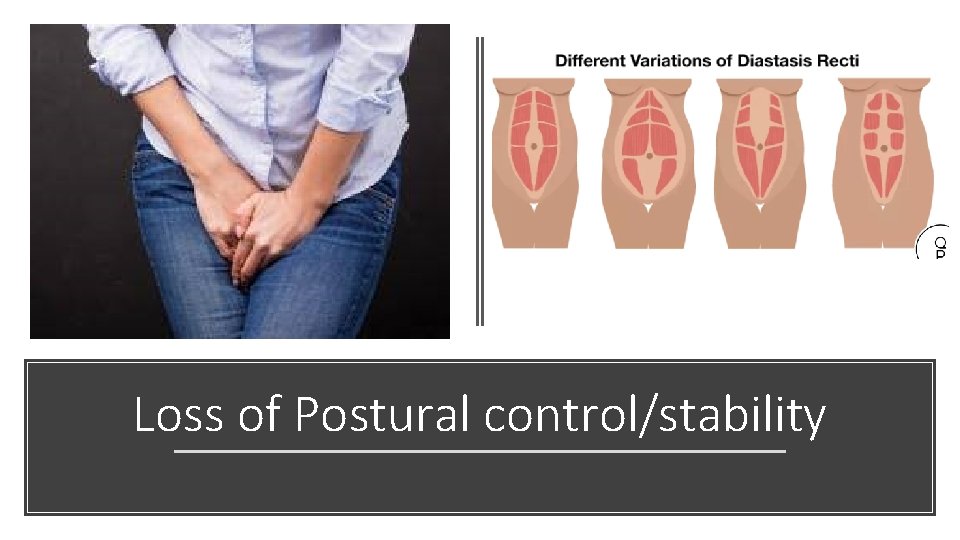
Loss of Postural control/stability

Painful Intercourse

Atrophic Vaginitis • Atrophic vaginitis is a survivorship issue that affects nearly 70% of postmenopausal breast cancer survivors as compared to 50% of postmenopausal women without breast cancer

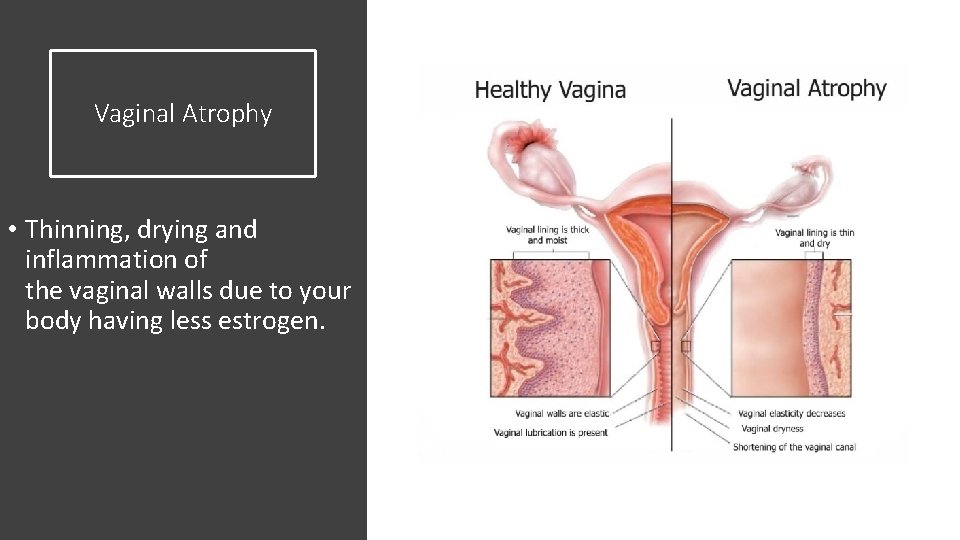
Vaginal Atrophy • Thinning, drying and inflammation of the vaginal walls due to your body having less estrogen.

PT Treatment for Atrophic Vaginitis • Manual therapy • Biofeedback • Use of Vaginal dilators • Education on vaginal moisturizers and lubericants.

TAKE AWAY POINTS • On average it takes a women 6. 5 years to speak to her physician about urinary incontinence • 50% of women that have had 1+ child will have a POP, only 10 -20% seek treatment. Of those that have surgical repairs, 29% will require another surgical repair at some point in their life • Use of biofeedback, manual therapy and vaginal dilators can improve painful sex and even better there are no side effects to these treatments!