Pediatric Patellar Instability Conservative Management and Outcomes Daniel

Pediatric Patellar Instability Conservative Management and Outcomes Daniel W. Green , M. D. , M. S. , F. A. C. S. Hospital for Special Surgery Lindsay Schlichte, M. S. Hospital for Special Surgery
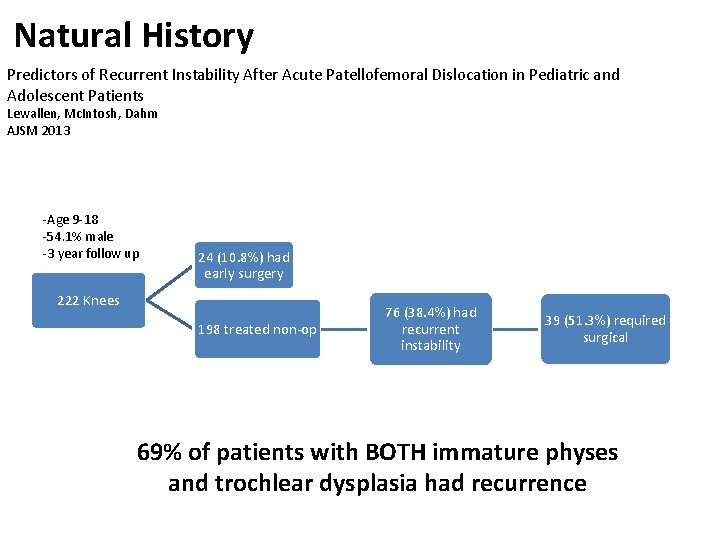
Natural History Predictors of Recurrent Instability After Acute Patellofemoral Dislocation in Pediatric and Adolescent Patients Lewallen, Mc. Intosh, Dahm AJSM 2013 -Age 9 -18 -54. 1% male -3 year follow up 24 (10. 8%) had early surgery 222 Knees 198 treated non-op 76 (38. 4%) had recurrent instability 39 (51. 3%) required surgical 69% of patients with BOTH immature physes and trochlear dysplasia had recurrence
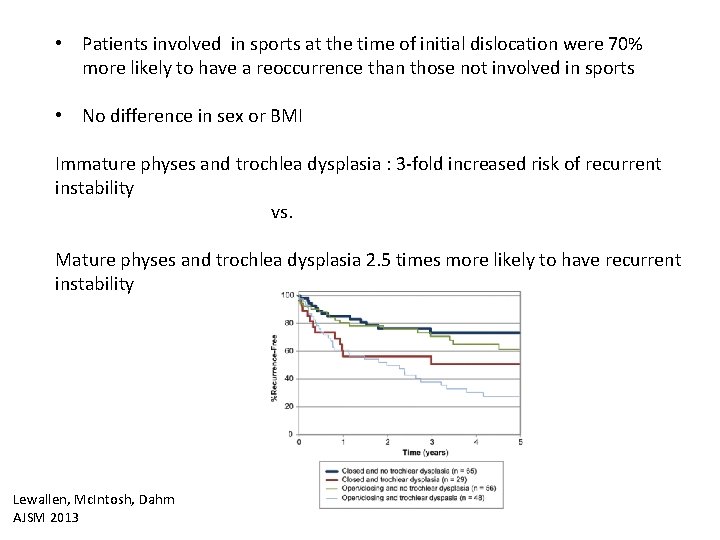
• Patients involved in sports at the time of initial dislocation were 70% more likely to have a reoccurrence than those not involved in sports • No difference in sex or BMI Immature physes and trochlea dysplasia : 3 -fold increased risk of recurrent instability vs. Mature physes and trochlea dysplasia 2. 5 times more likely to have recurrent instability Lewallen, Mc. Intosh, Dahm AJSM 2013
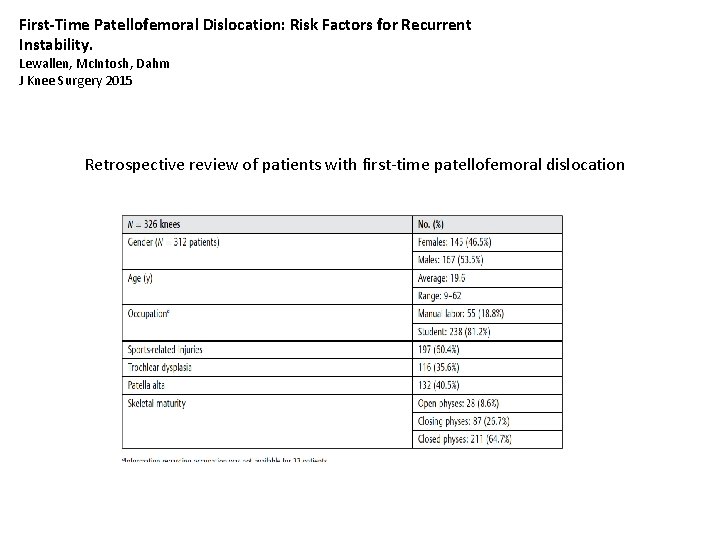
First-Time Patellofemoral Dislocation: Risk Factors for Recurrent Instability. Lewallen, Mc. Intosh, Dahm J Knee Surgery 2015 Retrospective review of patients with first-time patellofemoral dislocation
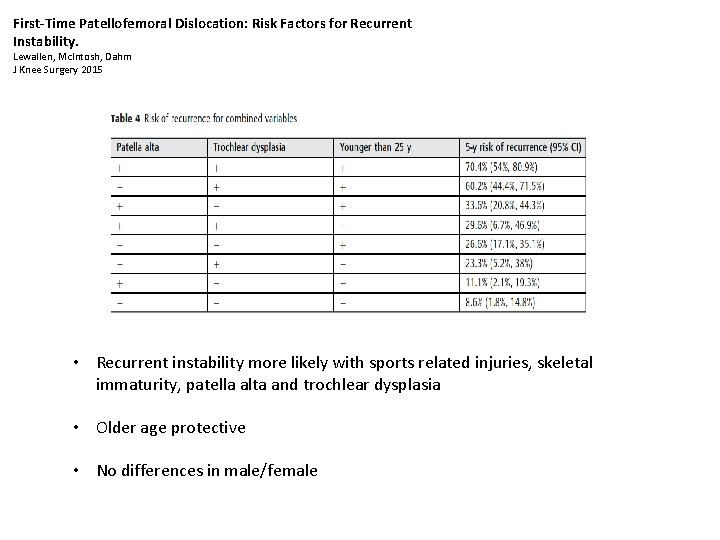
First-Time Patellofemoral Dislocation: Risk Factors for Recurrent Instability. Lewallen, Mc. Intosh, Dahm J Knee Surgery 2015 • Recurrent instability more likely with sports related injuries, skeletal immaturity, patella alta and trochlear dysplasia • Older age protective • No differences in male/female
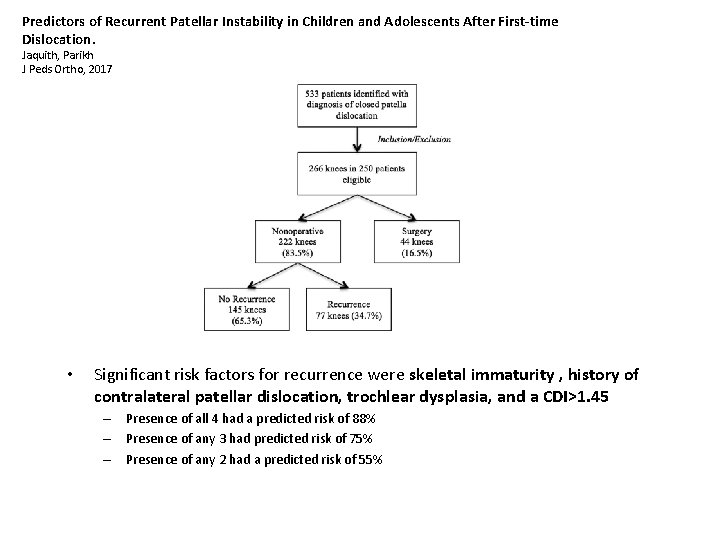
Predictors of Recurrent Patellar Instability in Children and Adolescents After First-time Dislocation. Jaquith, Parikh J Peds Ortho, 2017 • Significant risk factors for recurrence were skeletal immaturity , history of contralateral patellar dislocation, trochlear dysplasia, and a CDI>1. 45 – Presence of all 4 had a predicted risk of 88% – Presence of any 3 had predicted risk of 75% – Presence of any 2 had a predicted risk of 55%

Patellar Instability Severity Score Which patellae are likely to redislocate? Balcarek, Oberthür, Hopfensitz et. , al Knee Surg Sports Traumatol Arthrosc 2014 • • 61 patients Ages 9 -51 (Median 19) All had initial non-op treatment Within 24 months • 40 (65. 6%) experienced redislocation Identified risk factors for recurrent lateral patellar dislocations to create a Patellar Instability Severity Score

Assessed: • • • Age at primary dislocation Gender Affected side BMI Odds ratio with regards to patellar Bilateral instability Physical activity (baecke’s redislocation questionnaire) Grade of trochlear dysplasia Patellar height Tibial tuberosity-trochlear groove (TT-TG) distance Patellar tilt Which patellae are likely to redislocate? Balcarek, Oberthür, Hopfensitz et. , al Knee Surg Sports Traumatol Arthrosc 2014 “Patellar Instability Severity Score”: • Age* • Bilateral Instabilty • Severity of Trochlear dysplasia* • Patella Alta • TT-TG Distance • Patellar tilt* Total possible score = 7 *=significant

Applied to study population: Redislocation group: median = 4 (range 2 -7) No redislocation group: median = 3 (range 1 -6) Scoring Odds Ratio for early episode of patellar redislocation was nearly 5 times higher for the patient who scored 4 -7 than for those who scored 1 -3 However- still small differences between those who experienced a redislocation and those who did not • example: median TT-TG difference: • Redislocation: 16 (range 7 -27) • None: 14 (range 8 -24) Which patellae are likely to redislocate? Balcarek, Oberthür, Hopfensitz et. , al Knee Surg Sports Traumatol Arthrosc 2014 Balcarek et. , al.
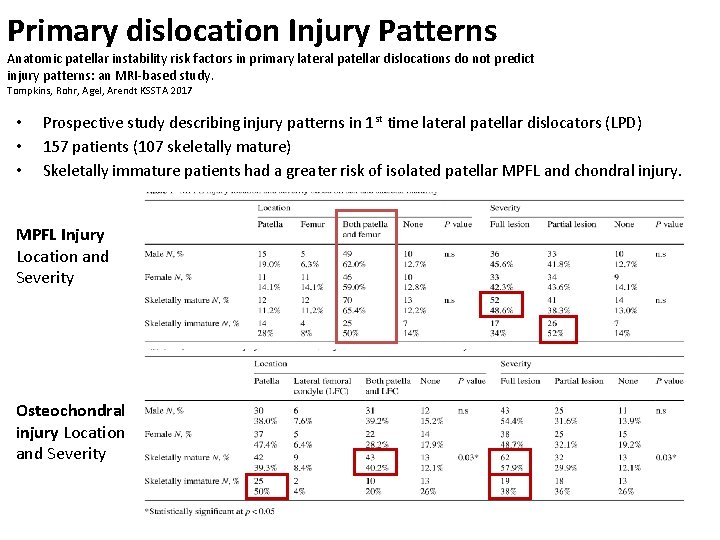
Primary dislocation Injury Patterns Anatomic patellar instability risk factors in primary lateral patellar dislocations do not predict injury patterns: an MRI-based study. Tompkins, Rohr, Agel, Arendt KSSTA 2017 • • • Prospective study describing injury patterns in 1 st time lateral patellar dislocators (LPD) 157 patients (107 skeletally mature) Skeletally immature patients had a greater risk of isolated patellar MPFL and chondral injury. MPFL Injury Location and Severity Osteochondral injury Location and Severity

Trochlear Dysplasia Definitions for presented studies • Lewallen et al. , 2013: Dejour Classification § 4 grade: low grade (type A) high grade (types B-D) • Lewallen et al. , 2015: Dejour Classification § 4 grade: low grade (type A) high grade (types B-D) • Jaquith et al. , 2017: Dejour Classification § 4 grade: low grade (type A) high grade (types B-D) • Balcarek et al. , 2014: Dejour Classifcation § 4 grade: low grade (type A) high grade (types B-D) • Tompkins et al. , 2017: Trochlear depth <3 mm

Conservative Treatment First patellar dislocation: from conservative treatment to return to sport Respizzi, Cavallin Stage 1 Stage 2 Stage 3 Stage 4 • Resolution of pain, swelling and inflammation • Recovery of joint motion and flexibility • Recovery of muscle strength • Recovery of motor patterns and coordination • Recovery of the sport-specific athletic action and return to sporting activity Stage 5

Conservative vs. Surgical Treatment • Earlier studies: support surgery for those who fail conservative treatment – Buchner, Baudendistel, Sabo et. , al. 2005 – Nikku, Nietosvaara, Aalto et. , al 2004 • More recent RCTs highlight the higher rates of recurrent instability in the athletic pediatric population undergoing conservative treatment – Nwachakwu, Schairer, Green et. , al. 2016 – Regalado, Lintula, Kokki et. , al. 2016 – Bitar, Alexandre Carneiro, et al. 2012
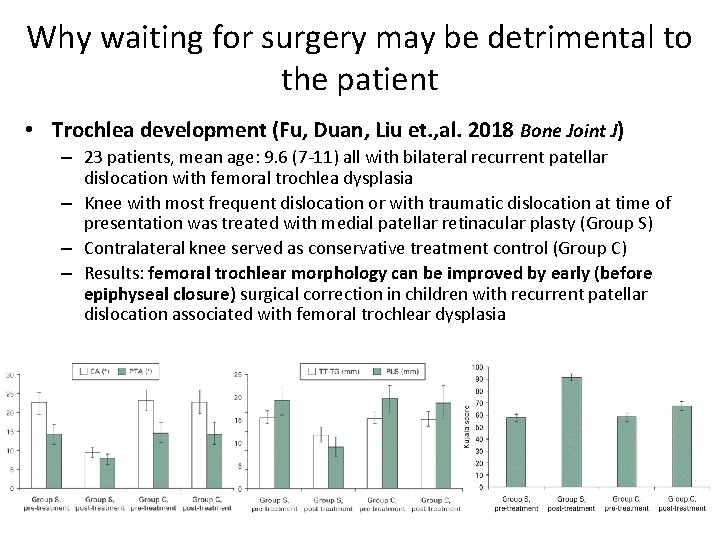
Why waiting for surgery may be detrimental to the patient • Trochlea development (Fu, Duan, Liu et. , al. 2018 Bone Joint J) – 23 patients, mean age: 9. 6 (7 -11) all with bilateral recurrent patellar dislocation with femoral trochlea dysplasia – Knee with most frequent dislocation or with traumatic dislocation at time of presentation was treated with medial patellar retinacular plasty (Group S) – Contralateral knee served as conservative treatment control (Group C) – Results: femoral trochlear morphology can be improved by early (before epiphyseal closure) surgical correction in children with recurrent patellar dislocation associated with femoral trochlear dysplasia

Why waiting for surgery may be detrimental to the patient • More dislocations = more cartilage injury= more long term pain (even after the instability is surgically corrected) Cartilage status in knees with recurrent patellar instability using magnetic resonance imaging T 2 relaxation time value. Chen, Li, Wang et. , al. KSSTA 2015 – 113 patients with patellar instability – 50 healthy controls – CT and MRI to measure joint anatomy and cartilage status respectively – MRI: • 32 patients were determined to have cartilage defects • Remaining 81: T 2 relaxation time value was significantly higher than that of the control group on the middle or medial sites of the patellar cartilage – CT: • Patellar instability group showed greatly abnormal anatomy of the PF joint compared to controls
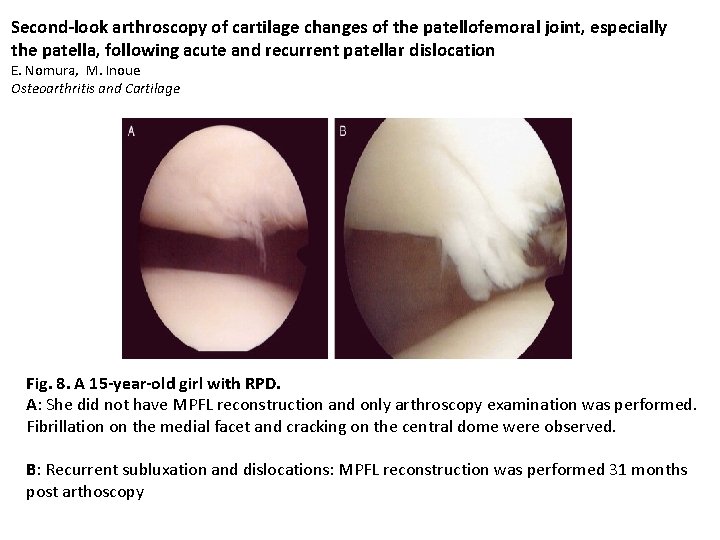
Second-look arthroscopy of cartilage changes of the patellofemoral joint, especially the patella, following acute and recurrent patellar dislocation E. Nomura, M. Inoue Osteoarthritis and Cartilage Fig. 8. A 15 -year-old girl with RPD. A: She did not have MPFL reconstruction and only arthroscopy examination was performed. Fibrillation on the medial facet and cracking on the central dome were observed. B: Recurrent subluxation and dislocations: MPFL reconstruction was performed 31 months post arthoscopy
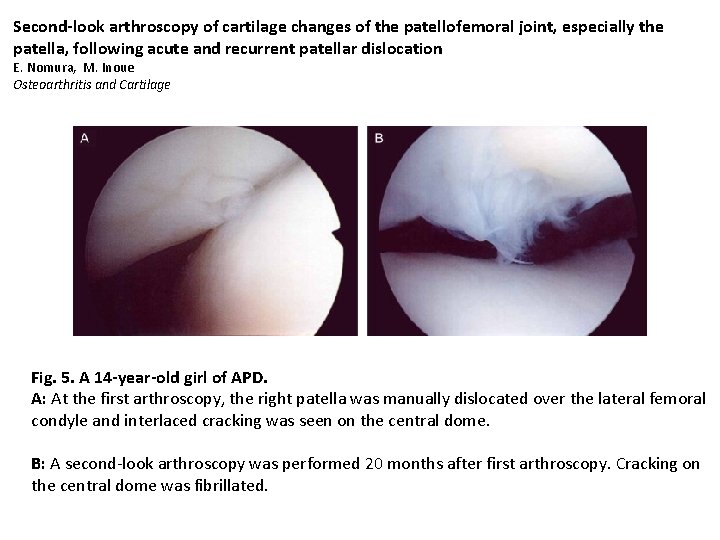
Second-look arthroscopy of cartilage changes of the patellofemoral joint, especially the patella, following acute and recurrent patellar dislocation E. Nomura, M. Inoue Osteoarthritis and Cartilage Fig. 5. A 14 -year-old girl of APD. A: At the first arthroscopy, the right patella was manually dislocated over the lateral femoral condyle and interlaced cracking was seen on the central dome. B: A second-look arthroscopy was performed 20 months after first arthroscopy. Cracking on the central dome was fibrillated. 17

Recent developments in evaluation and treatment of lateral patellar instability Zimmerer, Sobau, Balcarek Journal of Experimental Orthopedics 2018 • 15% to 72% of patients treated non-op – Patients without reoccurrence often reported not restoring their pre-injury function • High risk of patellofemoral arthritis after non-op treatment of lateral patellar dislocations • Paradigm shift from conservative to primary op treatment • However: reduced re-dislocations not yet reflected in the clinical results • Individual clinical decision-making approach, taking each individual risk of re-dislocation into account

Thank You! Daniel W Green, MD greendw@hss. edu Lindsay Schlichte, M. S.

• • • • Lewallen, L. W. , Mc. Intosh, A. L. , & Dahm, D. L. (2013). Predictors of recurrent instability after acute patellofemoral dislocation in pediatric and adolescent patients. The American journal of sports medicine, 41(3), 575 -581. Lewallen, L. , Mc. Intosh, A. , & Dahm, D. (2015). First-time patellofemoral dislocation: risk factors for recurrent instability. The journal of knee surgery, 28(04), 303 -310. Balcarek, P. , Oberthür, S. , Hopfensitz, S. , Frosch, S. , Walde, T. A. , Wachowski, M. M. , . . . & Stürmer, K. M. (2014). Which patellae are likely to redislocate? . Knee Surgery, Sports Traumatology, Arthroscopy, 22(10), 2308 -2314. Buchner, M. , Baudendistel, B. , Sabo, D. , & Schmitt, H. (2005). Acute traumatic primary patellar dislocation: long-term results comparing conservative and surgical treatment. Clinical Journal of Sport Medicine, 15(2), 62 -66 Jaquith, Bradley P. , and Shital N. Parikh. "Predictors of recurrent patellar instability in children and adolescents after first-time dislocation. " Journal of Pediatric Orthopaedics 37. 7 (2017): 484 -490. Nwachukwu, B. U. , So, C. , Schairer, W. W. , Green, D. W. , & Dodwell, E. R. (2016). Surgical versus conservative management of acute patellar dislocation in children and adolescents: a systematic review. Knee Surgery, Sports Traumatology, Arthroscopy, 24(3), 760 -767. Regalado, G. , Lintula, H. , Kokki, H. , Kröger, H. , Väätäinen, U. , & Eskelinen, M. (2016). Six-year outcome after non-surgical versus surgical treatment of acute primary patellar dislocation in adolescents: a prospective randomized trial. Knee Surgery, Sports Traumatology, Arthroscopy, 24(1), 6 -11. Fu, K. , Duan, G. , Liu, C. , Niu, J. , & Wang, F. (2018). Changes in femoral trochlear morphology following surgical correction of recurrent patellar dislocation associated with trochlear dysplasia in children. Bone Joint J, 100(6), 811 -821. Chen, X. , Wang, W. , Xin, H. , Wang, Y. , & Wang, J. (2015). Cartilage status in knees with recurrent patellar instability using magnetic resonance imaging T 2 relaxation time value. Knee Surgery, Sports Traumatology, Arthroscopy, 23(8), 2292 -2296. Nomura, E. , & Inoue, M. (2005). Second-look arthroscopy of cartilage changes of the patellofemoral joint, especially the patella, following acute and recurrent patellar dislocation. Osteoarthritis and cartilage, 13(11), 1029 -1036. Zimmerer, A. , Sobau, C. , & Balcarek, P. (2018). Recent developments in evaluation and treatment of lateral patellar instability. Journal of experimental orthopaedics, 5(1), 3. Bitar AC, Demange MK, D’Elia CO, Camanho GL. Traumatic patellar dislocation: nonoperative treatment compared with MPFL reconstruction using patellar tendon. The American journal of sports medicine. 2012 Jan; 40(1): 114 -22. Tompkins MA, Rohr SR, Agel J, Arendt EA. Anatomic patellar instability risk factors in primary lateral patellar dislocations do not predict injury patterns: an MRI-based study. Knee Surgery, Sports Traumatology, Arthroscopy. 2018 Mar 1; 26(3): 677 -84.
- Slides: 20