Pediatric Palliative Care and EndofLife Care Nicole C



























- Slides: 29

Pediatric Palliative Care and End-of-Life Care Nicole C. Hahnlen, BS, RN Hummingbird Program Clinical Coordinator Caring for Kids.

Philosophy and Principles of Palliative Care • Hospice Caring for Kids.

Palliative Care Curative Focus: Disease-Specific Treatments Palliative Focus: Comfort / Supportive Treatments Caring for Kids. Bereavement Support

General Principles of Palliative Care for Children • Palliative care can occur simultaneously with curative care • Child and family viewed as unit of care • Attention to physical, psychological, social and spiritual needs Caring for Kids.

General Principles of Palliative Care for Children • Interdisciplinary team approach • Ongoing assessment and clarification of desires/priorities important • Quality of life is subjective Caring for Kids.

Model of Quality of life • Physical Well-Being • Psychological Well-Being • Social Well-Being • Spiritual Well-Being Ferrell, et al, 1991 Caring for Kids.

Physical Well-Being • Pain • Multiple other symptoms • Impact on family caregivers Caring for Kids.

Psychological Well-Being • Wide range of emotions and concerns • Meaning of illness • Coping Caring for Kids.

Social Well-Being • Relationship/role description • Caregiver burden • Financial concerns • Impact on siblings Caring for Kids.

Spiritual Well-Being • Religion and spirituality • Seeking meaning • Hope vs. despair • Importance of ritual Caring for Kids.

Psychological Physical Functional Ability Strength/Fatigue Sleep & Rest Nausea Appetite Constipation Pain Anxiety Depression Enjoyment/Leisure Pain Distress Happiness Fear Cognition/Attention Quality of Life Spiritual Social Financial Burden Caregiver Burden Roles & Relationships Affection/Sexual Function Appearance Caring for Kids. Adapted from Ferrell, et al. 1991 Hope Suffering Meaning of Pain Religiosity Transcendence

Epidemiology • Approximately 500, 000 children cope with lifethreatening conditions annually in the United States 1 • Over 50, 000 infants and children die annually in the United States 2 1. Himelstein BP et al. N Eng J Med 2004; 350: 1752 2. Hoyert DL et al. Pediatrics 2006; 117: 168 Caring for Kids.

Leading Causes of Infant Death • • • Congenital & Chromosomal Anomalies Disorders related to SGA & LBW SIDS Maternal Complications of Pregnancy Complications of Placenta, Cord & Membranes Respiratory Distress Accidents Bacterial Sepsis Diseases of the Circulatory System Intrauterine Hypoxia & Birth Asphyxia Martin JA et al. Pediatrics 2005; 115: 619 Caring for Kids.

Leading Causes of Childhood Death (1 - 19 years old) • • • Accidents (unintentional injuries) Assault (homicide) Malignant Neoplasms Intentional Self Harm (suicide) Congenital & Chromosomal Anomalies Diseases of Heart Chronic Lower Respiratory Diseases Influenza and Pneumonia Septicemia Cerebrovascular Diseases Martin JA et al. Pediatrics 2005; 115: 619 Caring for Kids.

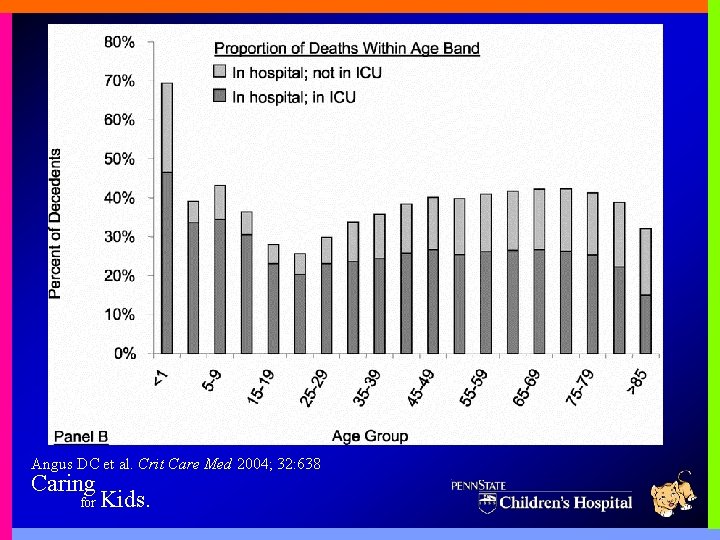
Angus DC et al. Crit Care Med 2004; 32: 638 Caring for Kids.

Contrasting Goals of Intensive Care and Palliative Care Intensive Care • To fight death • To cure • To prolong life at all costs Caring for Kids. Palliative Care • To promote physical, psychological, spiritual, and social comfort • To promote the acceptance of death as an outcome

Mode of Death in the Pediatric Intensive Care Unit • The most common mode of death in the pediatric intensive care unit (PICU) is the limitation or withdraw of life sustaining therapy (LST) Vernon DD et al. Crit Care Med 1993; 21: 1798 Mink RB et al. Pediatrics 1992; 89: 961 Caring for Kids.

Types of LST Forgone • • Mechanical Ventilation Vasoactive Infusions Renal Replacement Therapies Invasive Catheters Extracorporeal Membrane Oxygenation Antibiotics Intravenous Fluids Feeds Caring for Kids.

Factors Important to Parents’ Decisions to Forgo LST • • • Quality of life Likelihood of improvement Pain or discomfort Unlikely to survive hospitalization What I believe my child would have wanted Information the staff provided Caring for Meyer EC et al. Crit Care Med 2002; 30: 226 Kids.

Factors Important to Parents’ Decisions to Forgo LST, continued • • • Religious/spiritual beliefs Child’s appearance or behavior Advice of hospital staff Attitudes of hospital staff Advice of family and friends Financial costs Caring for Meyer EC et al. Crit Care Med 2002; 30: 226 Kids.

Reasons for Clinicians Limiting or Withdrawing LST • No benefit - Imminent death • Excessive burden - Unacceptable decrement in quality of life • No relational benefit - Survival with severe neurologic dysfunction • Diagnosis • Acute versus chronic disease Caring for Kids. Randolph AG et al. Crit Care Med 1997; 25: 435 Levetown M et al. JAMA 1994; 272; 1271 Keenan HT et al. Crit Care Med 2000; 28: 1590

Reasons for Clinicians Limiting or Withdrawing LST, continued • • • Perceived benefit Prognosis Family preference Probability of survival Functional status or Quality of life Caring for Kids. Randolph AG et al. Crit Care Med 1997; 25: 435 Levetown M et al. JAMA 1994; 272; 1271 Keenan HT et al. Crit Care Med 2000; 28: 1590

Physicians’ Responsibilities & the Decision Making Process • Inform the patient & family when end of life discussions need to occur because treatment no longer confers benefit & should be forgone • Provide the patient & family with adequate information about therapeutic and diagnostic benefits • Elicit questions and ascertain whether or not information and advice is understood • Ascertain the patient’s & family’s personal values and goals of therapy • Provide advice about which option to choose • Documents orders & progress notes in the medical record AAP Committee on Bioethics Pediatrics 1994; 93: 532 Caring for Kids.

Role of the Nurse • The importance of presence • Maintaining a realistic perspective • Nurses as the safety net Caring for Kids.

The Ideal Decision Making Process • Is shared between the caregiver team, patient, & family • Reaches a consensus on a medical plan that is in accordance with the values and choices of the patient and family • Begins early during the ICU admission with a multidisciplinary meeting which: – Uses nontechnical language – Allows ample time for questions – Considers the patient’s & family’s personal values and goals of therapy • Is one of negotiation • Is documented Thompson BT et al Crit Care Med 2004; 32: 1781 Caring for Kids.

Improving the Quality of End-of. Life Care in the PICU Parents’ priorities and recommendations include: – – – Honest and complete information Ready access to staff Communication and coordination of care Emotional expression and support by staff Preservation of the integrity of the parent-child relationship Faith Meyer EC et al. Pediatrics 2006; 117: 649 Caring for Kids.

The Hummingbird Program at Penn State Children’s Hospital • A consultative service that provides comprehensive medical, emotional, social, and spiritual support to the children and families facing life-threatening, complex medical conditions. Caring for Kids.

Hummingbird Program Goals: • To support the medical, emotional, social and spiritual needs of children with life-threatening complex medical conditions and their families • To assist in communication, navigation and coordination of care between various inpatient and community specialists and healthcare services • To assist patient and families in decision making regarding various treatment options • To assist patients and families in defining and meeting their goals and wishes thereby enhancing quality of life Caring for Kids.

The Hummingbird Program at Penn State Children’s Hospital Any child with a complex medical condition and the following criteria may qualify for help from the Hummingbird program: • The condition causes significant pain, emotional, social, or physical distress • The condition causes fragmentation of medical care and communication • The condition disrupts the ability to perform age appropriate life activities • The condition results infrequent emergency department visits, hospitalizations, or prolonged length of hospital stay • The condition requires assistance with complex decision-making and determination of medical goals of care Caring for Kids.