Pediatric Overweight and Obesity Wendy Novoa M S

Pediatric Overweight and Obesity Wendy Novoa, M. S. November 14, 2006

Overview • • • Obesity Trends and Prevalence Definition of Overweight and Obesity Causes of Overweight and Obesity Medical and Psychosocial Complications Empirically Supported Treatments Project STORY

Trends and Prevalence
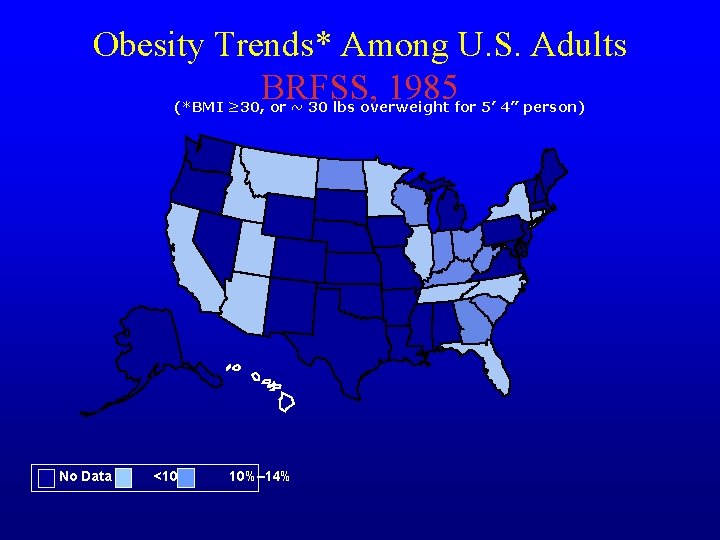
Obesity Trends* Among U. S. Adults BRFSS, 1985 (*BMI ≥ 30, or ~ 30 lbs overweight for 5’ 4” person) No Data <10% 10%– 14%
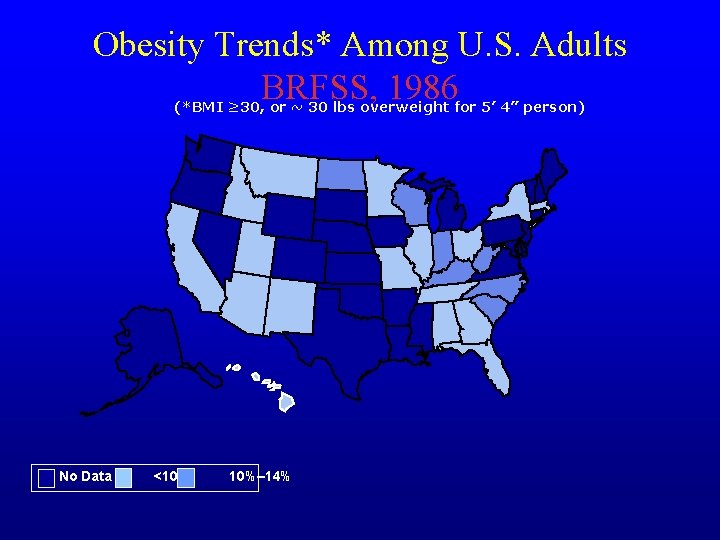
Obesity Trends* Among U. S. Adults BRFSS, 1986 (*BMI ≥ 30, or ~ 30 lbs overweight for 5’ 4” person) No Data <10% 10%– 14%
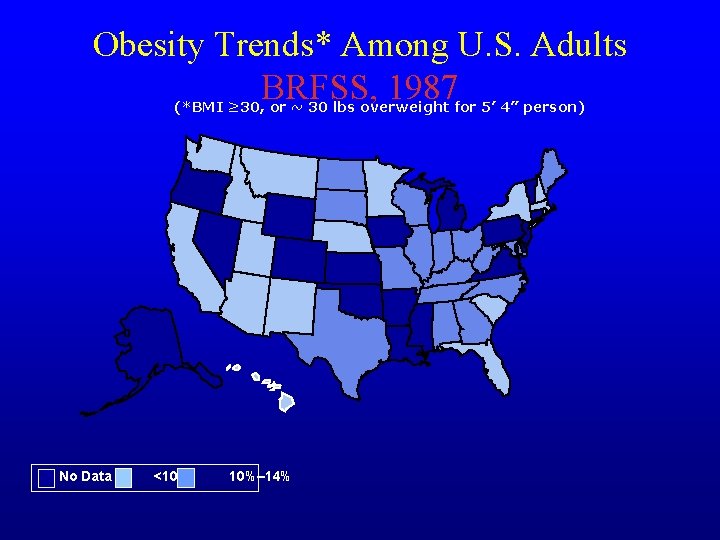
Obesity Trends* Among U. S. Adults BRFSS, 1987 (*BMI ≥ 30, or ~ 30 lbs overweight for 5’ 4” person) No Data <10% 10%– 14%
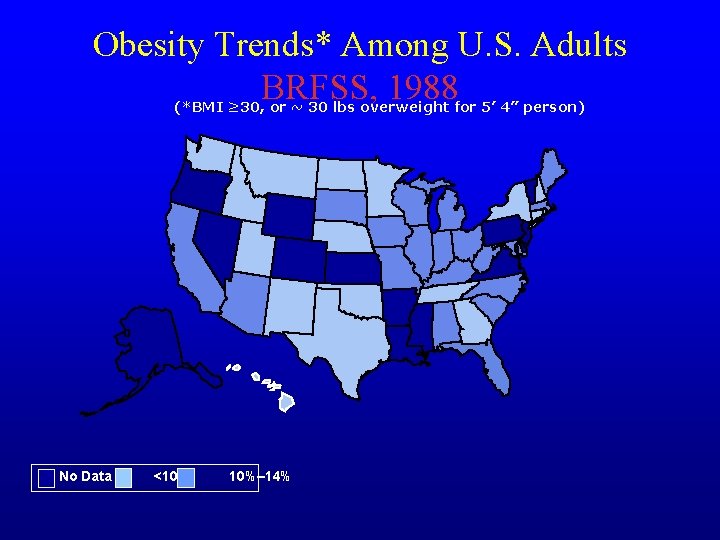
Obesity Trends* Among U. S. Adults BRFSS, 1988 (*BMI ≥ 30, or ~ 30 lbs overweight for 5’ 4” person) No Data <10% 10%– 14%
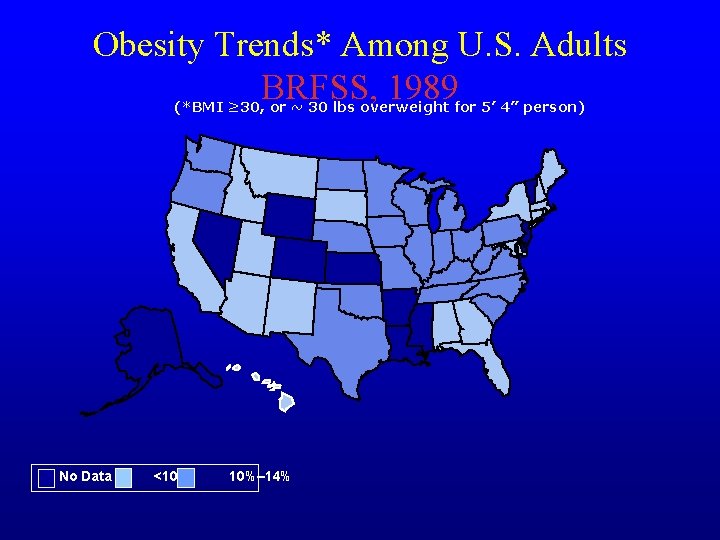
Obesity Trends* Among U. S. Adults BRFSS, 1989 (*BMI ≥ 30, or ~ 30 lbs overweight for 5’ 4” person) No Data <10% 10%– 14%
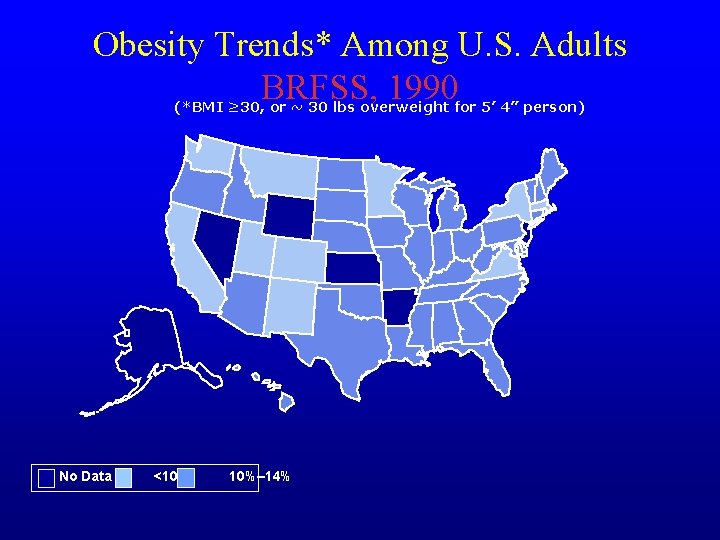
Obesity Trends* Among U. S. Adults BRFSS, 1990 (*BMI ≥ 30, or ~ 30 lbs overweight for 5’ 4” person) No Data <10% 10%– 14%
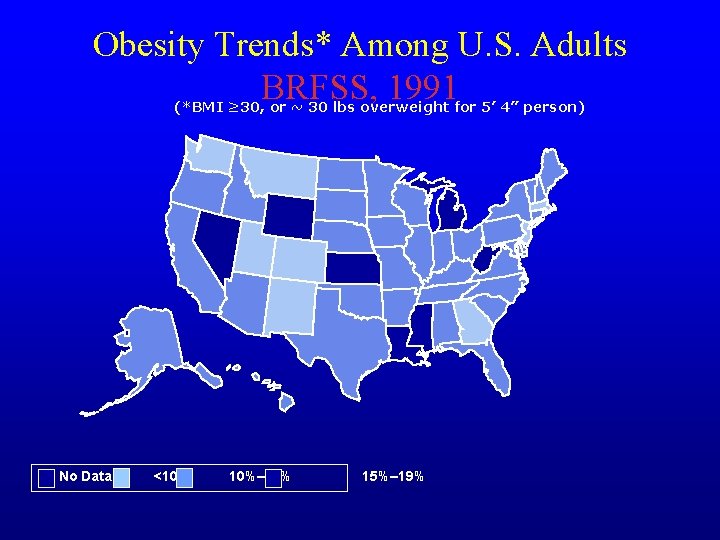
Obesity Trends* Among U. S. Adults BRFSS, 1991 (*BMI ≥ 30, or ~ 30 lbs overweight for 5’ 4” person) No Data <10% 10%– 14% 15%– 19%
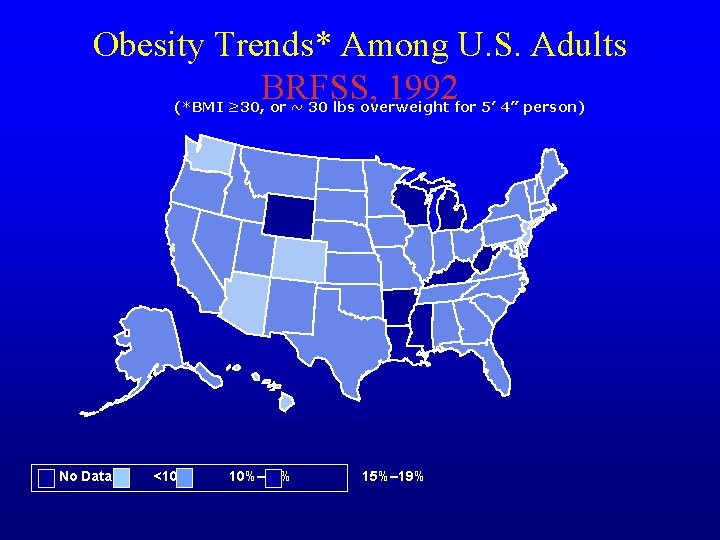
Obesity Trends* Among U. S. Adults BRFSS, 1992 (*BMI ≥ 30, or ~ 30 lbs overweight for 5’ 4” person) No Data <10% 10%– 14% 15%– 19%
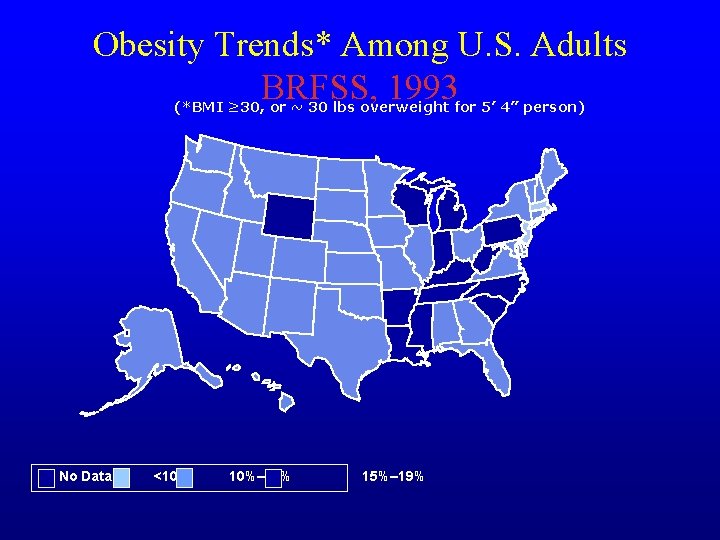
Obesity Trends* Among U. S. Adults BRFSS, 1993 (*BMI ≥ 30, or ~ 30 lbs overweight for 5’ 4” person) No Data <10% 10%– 14% 15%– 19%
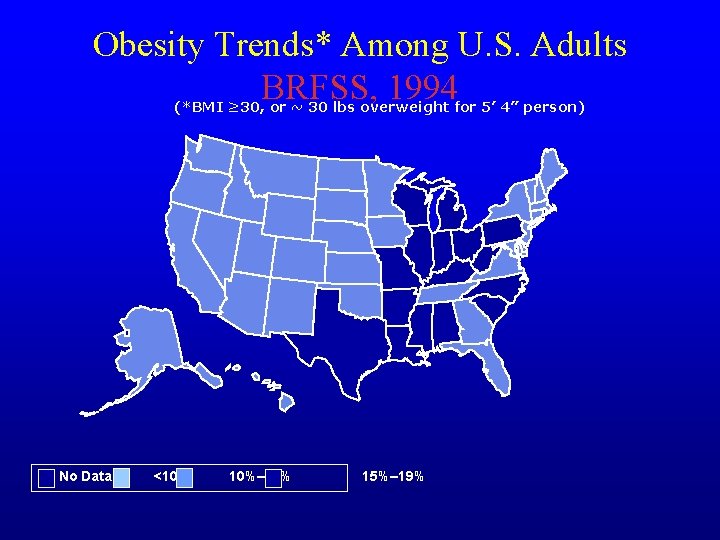
Obesity Trends* Among U. S. Adults BRFSS, 1994 (*BMI ≥ 30, or ~ 30 lbs overweight for 5’ 4” person) No Data <10% 10%– 14% 15%– 19%
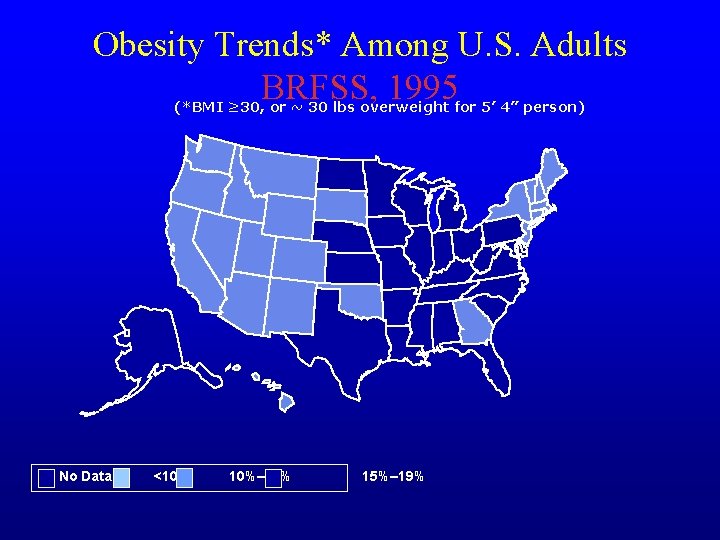
Obesity Trends* Among U. S. Adults BRFSS, 1995 (*BMI ≥ 30, or ~ 30 lbs overweight for 5’ 4” person) No Data <10% 10%– 14% 15%– 19%
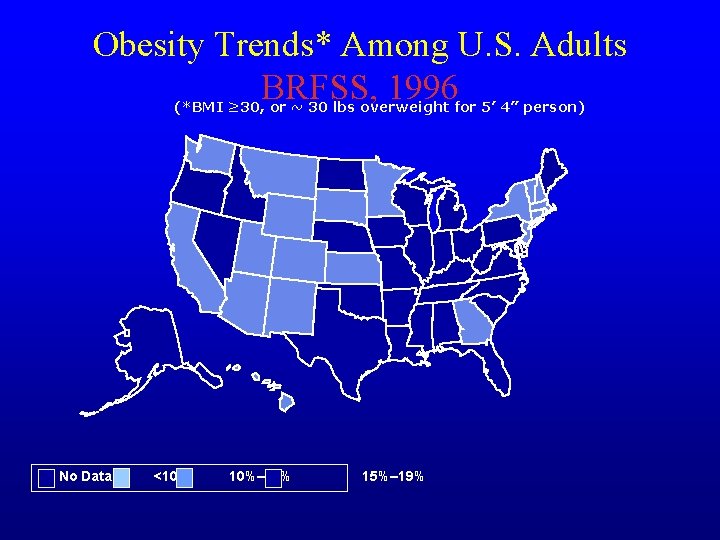
Obesity Trends* Among U. S. Adults BRFSS, 1996 (*BMI ≥ 30, or ~ 30 lbs overweight for 5’ 4” person) No Data <10% 10%– 14% 15%– 19%
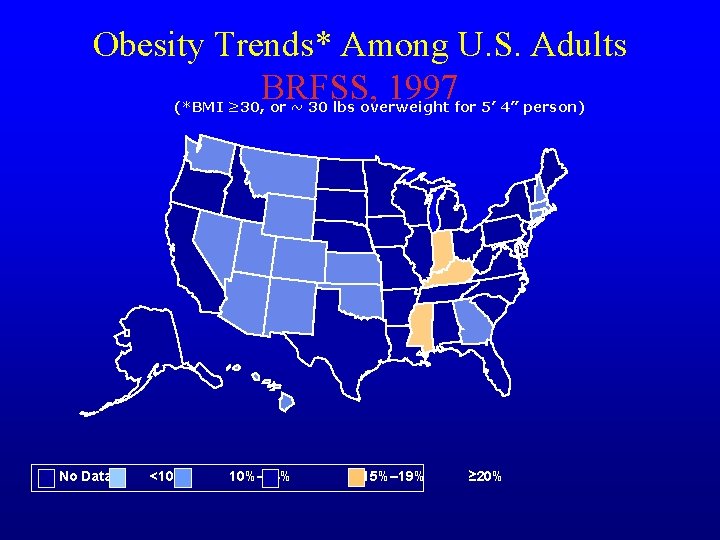
Obesity Trends* Among U. S. Adults BRFSS, 1997 (*BMI ≥ 30, or ~ 30 lbs overweight for 5’ 4” person) No Data <10% 10%– 14% 15%– 19% ≥ 20%
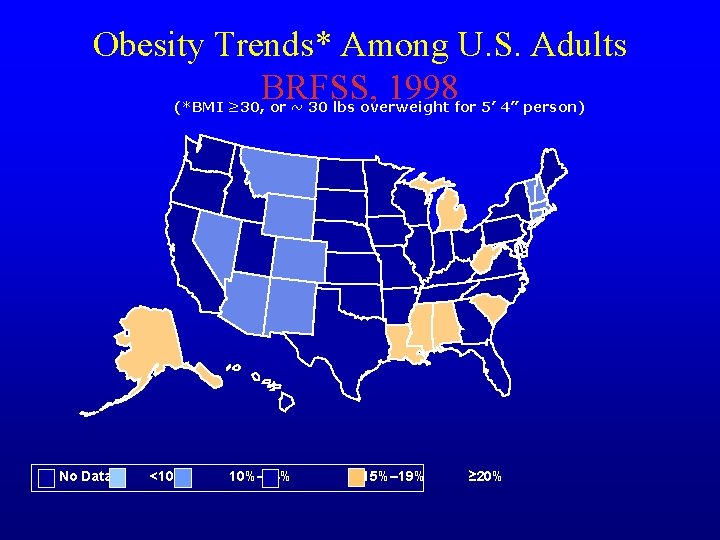
Obesity Trends* Among U. S. Adults BRFSS, 1998 (*BMI ≥ 30, or ~ 30 lbs overweight for 5’ 4” person) No Data <10% 10%– 14% 15%– 19% ≥ 20%
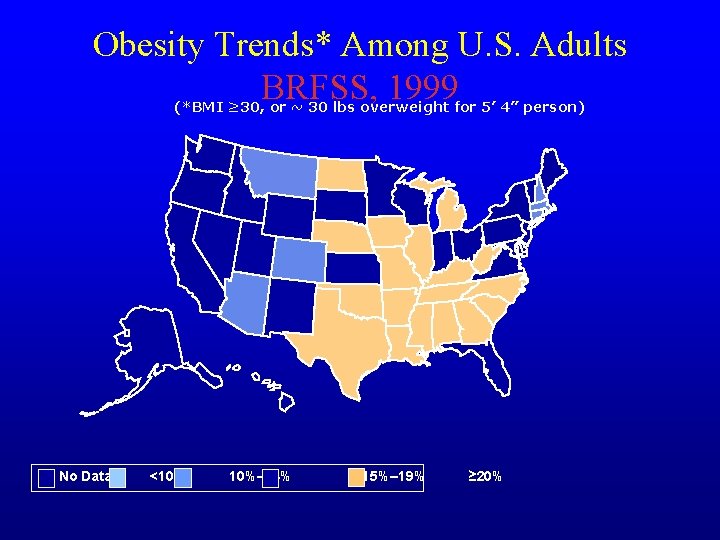
Obesity Trends* Among U. S. Adults BRFSS, 1999 (*BMI ≥ 30, or ~ 30 lbs overweight for 5’ 4” person) No Data <10% 10%– 14% 15%– 19% ≥ 20%
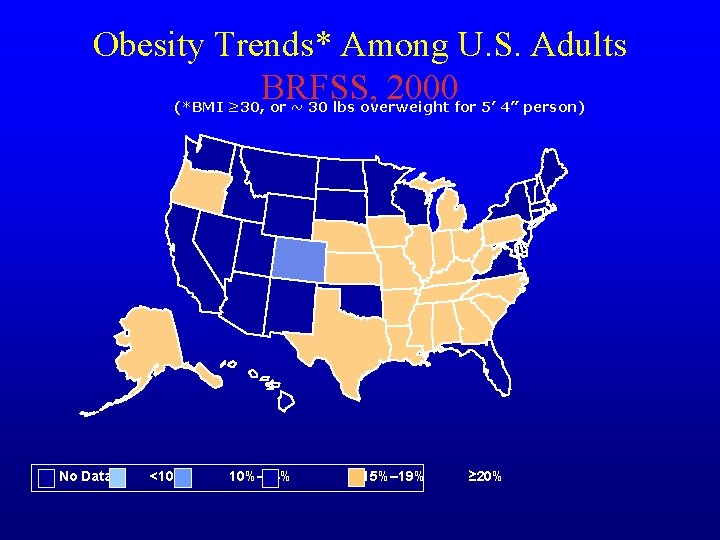
Obesity Trends* Among U. S. Adults BRFSS, 2000 (*BMI ≥ 30, or ~ 30 lbs overweight for 5’ 4” person) No Data <10% 10%– 14% 15%– 19% ≥ 20%
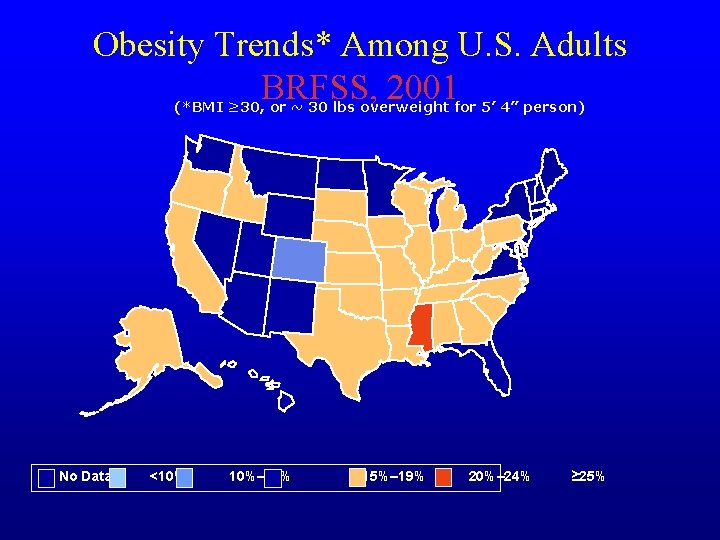
Obesity Trends* Among U. S. Adults BRFSS, 2001 (*BMI ≥ 30, or ~ 30 lbs overweight for 5’ 4” person) No Data <10% 10%– 14% 15%– 19% 20%– 24% ≥ 25%
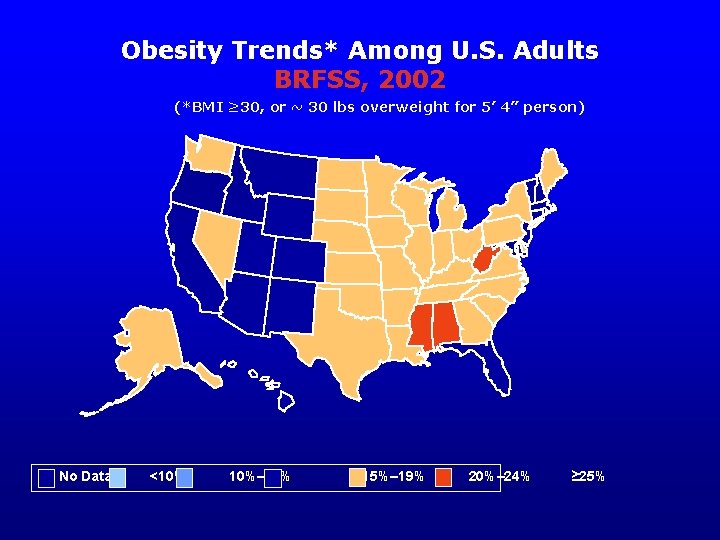
Obesity Trends* Among U. S. Adults BRFSS, 2002 (*BMI ≥ 30, or ~ 30 lbs overweight for 5’ 4” person) No Data <10% 10%– 14% 15%– 19% 20%– 24% ≥ 25%
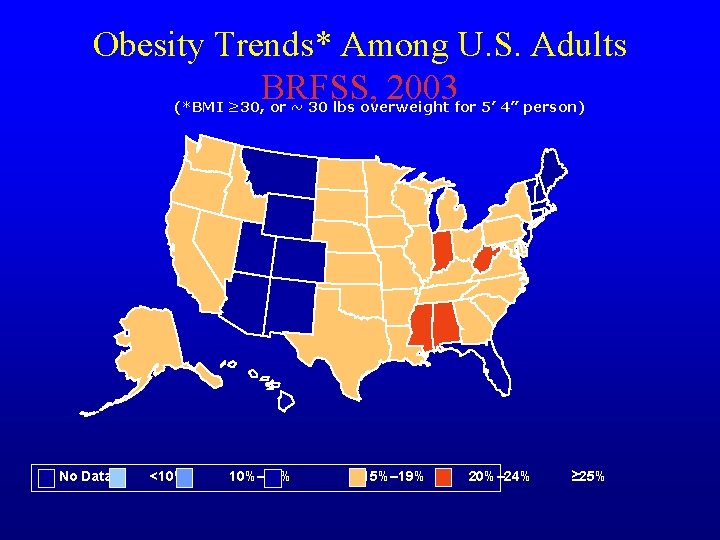
Obesity Trends* Among U. S. Adults BRFSS, 2003 (*BMI ≥ 30, or ~ 30 lbs overweight for 5’ 4” person) No Data <10% 10%– 14% 15%– 19% 20%– 24% ≥ 25%
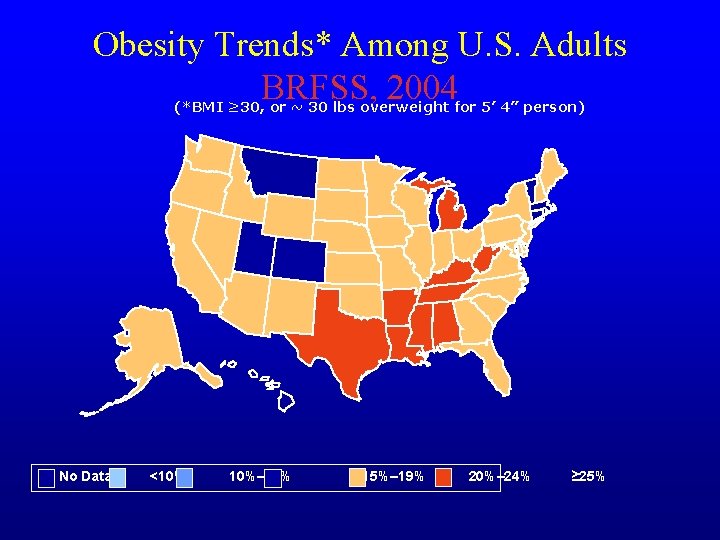
Obesity Trends* Among U. S. Adults BRFSS, 2004 (*BMI ≥ 30, or ~ 30 lbs overweight for 5’ 4” person) No Data <10% 10%– 14% 15%– 19% 20%– 24% ≥ 25%
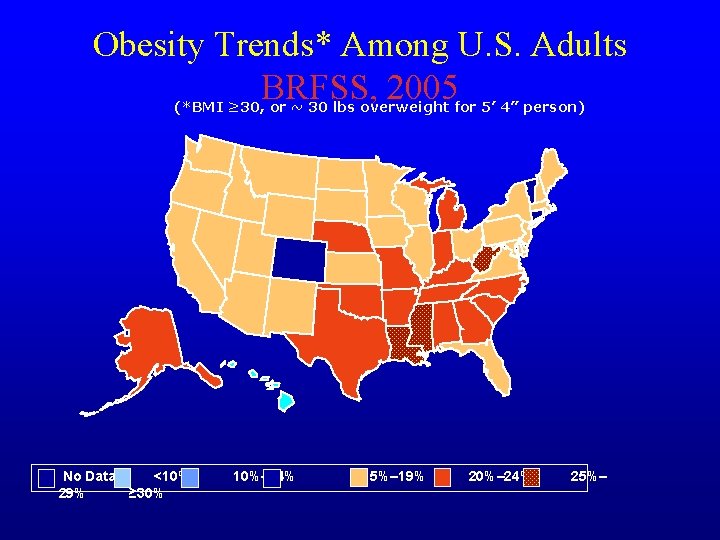
Obesity Trends* Among U. S. Adults BRFSS, 2005 (*BMI ≥ 30, or ~ 30 lbs overweight for 5’ 4” person) No Data <10% 29% ≥ 30% 10%– 14% 15%– 19% 20%– 24% 25%–
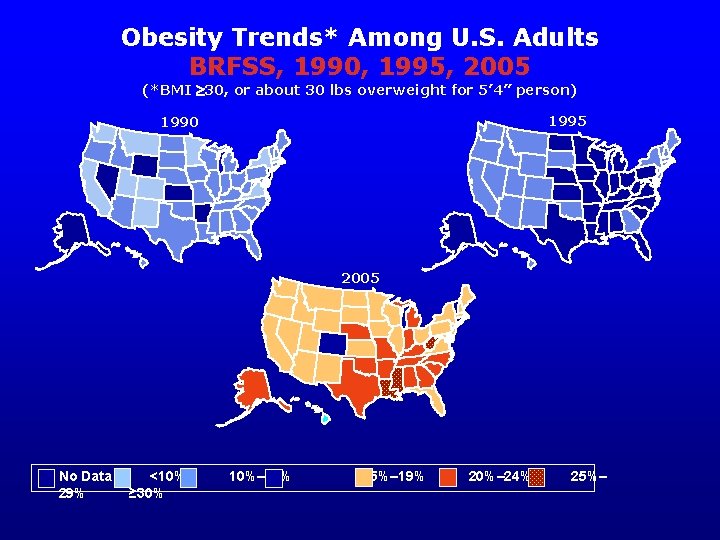
Obesity Trends* Among U. S. Adults BRFSS, 1990, 1995, 2005 (*BMI 30, or about 30 lbs overweight for 5’ 4” person) 1995 1990 2005 No Data 29% <10% ≥ 30% 10%– 14% 15%– 19% 20%– 24% 25%–

Obesity and Overweight in Children and Adolescents • Prevalence – 33% overweight (85 th-95 th percentile) – 16% obese (at or above 95 th percentile) – Children in rural areas have a 54. 7% increased risk of obesity

Prevalence • Doubled among children 6 -11 and tripled among adolescents 12 -17 from 1976 -1980 to 1999 -2000 (Dietz, 2004) • 1999 -2000 data indicate that 31% of children and adolescents are overweight and 16% are obese (Hedley, et al. , 2004) • Black and Mexican American children disproportionately affected (Dietz, 2004)

Higher Prevalence in Rural Areas • Research suggests that children in rural areas have a 54. 7% increased risk of obesity compared to urban children • Despite increased risk, many individuals living in rural areas are medically underserved due to: – – Limited health promotion programs Higher rates of poverty Higher percentages of patients without health insurance Lower numbers of health care providers

In Florida • 60% of Florida adults are overweight or obese (CDC BRFSS, 2004) • 26% of Florida high-school students are overweight or at risk of becoming overweight (CDC YRBSS, 2003) • 21% of non-Hispanic white adults, 33% of non. Hispanic black adults, and 26% of Hispanic adults in Florida are obese (CDC BRFSS, 2004) • 28% of low-income children between 2 and 5 years of age in Florida are overweight or at risk of becoming overweight (CDC Ped. NSS, 2003)

Costs • State specific obesity attributable medical expenditures: $87 million – $7. 7 billion (Ogden et al. , 2006) • Between 1979 -1980, the number of obesity and obesity-related hospital discharges tripled (Goran, Ball, & Cruz, 2003)

Definition of Overweight and Obesity

Definition for Adults • Definition of Obesity and Overweight in Adults* – – BMI under 18. 5: Underweight BMI 18. 6 -24. 9: Healthy weight BMI 25 -29. 9: Overweight BMI 30 or higher: Obese *Although BMI correlates with the amount of body fat, BMI does not directly measure body fat. Some people, such as athletes, may have a BMI that identifies them as overweight even though they do not have excess body fat

What is BMI? • Body Mass Index (BMI) = weight (kg)/height (m)2 • BMI is a screening tool, not a diagnostic tool • In children, BMI is gender and age specific, so BMI-for-age is used • No gender or age distinctions are made for adult BMI calculations (CDC, 2005)

Advantages of BMI-for-age • Correlates with clinical risk factors for cardiovascular disease • Compares well with measures of body fat • Recommended by expert committees to evaluate overweight status in children and adults • Tracks well into adulthood (CDC, 2005)

Link to Adult Obesity • Overweight in children associated with more severe obesity among adults • Some studies suggest up to 80% of overweight adolescents become obese adults • An increased risk exists for girls (Dietz, 2004)
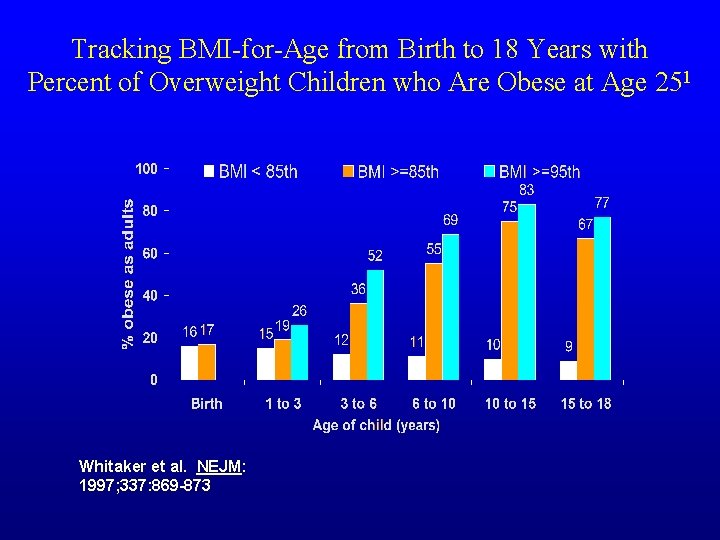
Tracking BMI-for-Age from Birth to 18 Years with Percent of Overweight Children who Are Obese at Age 251 Whitaker et al. NEJM: 1997; 337: 869 -873

Definition for Children and Adolescents • Definition of Obesity and Overweight in Children and Adolescents: – Sex and Age-specific BMI – Obese is at or above 95 th percentile, based on revised CDC growth charts – Overweight is at or above 85 th percentile (U. S. Department of Health and Human Services, 2001)

CDC Growth Charts • Percentile curves that illustrate the distribution of selected body measurements in U. S. children • The 1977 growth charts were developed by the National Center for Health Statistics as a clinical tool for health professionals to determine if the growth of a child is adequate • The 1977 charts were adopted by the World Health Organization for international use (CDC, 2005)

CDC Growth Charts • The 2000 CDC growth charts represent the revised version of the 1977 NCHS growth charts • The revised growth charts consist of 16 charts, 8 for boys and 8 for girls (CDC, 2005)
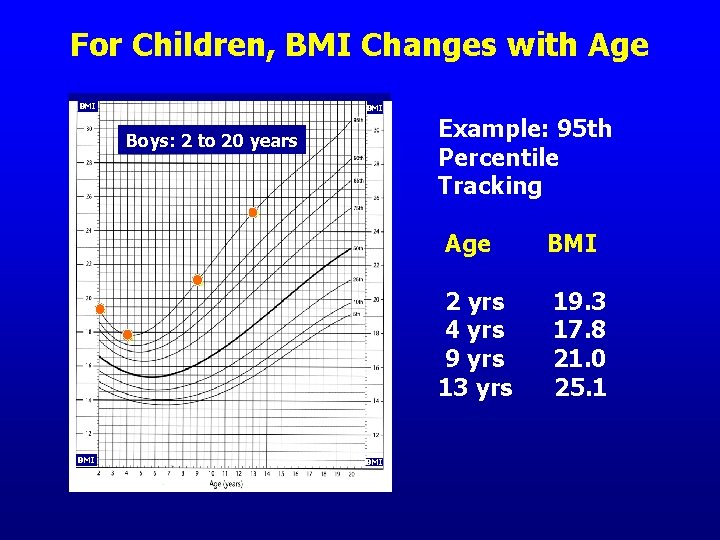
For Children, BMI Changes with Age BMI Example: 95 th Percentile Tracking Boys: 2 to 20 years BMI Age BMI 2 yrs 4 yrs 9 yrs 13 yrs 19. 3 17. 8 21. 0 25. 1


Can you see risk? • This boy is 3 years, 3 weeks old • Is his BMI-for-age in the >85 th to <95 th percentile? • Is he at risk for overweight? Photo from UC Berkeley Longitudinal Study, 1973
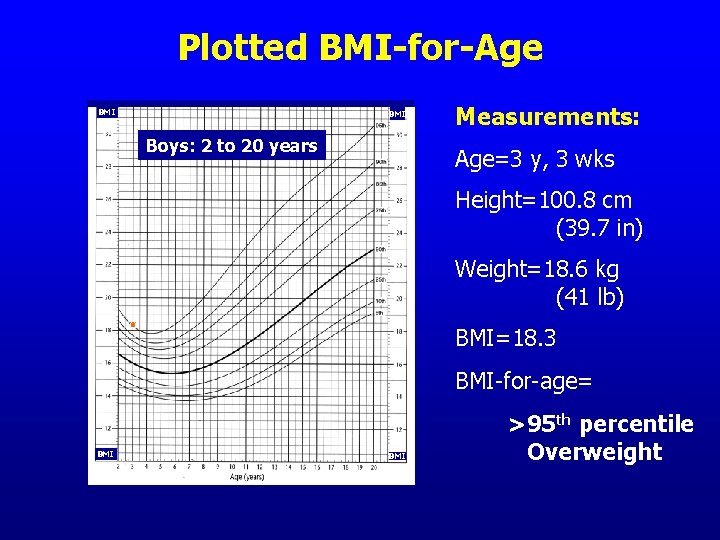
Plotted BMI-for-Age BMI Boys: 2 to 20 years Measurements: Age=3 y, 3 wks Height=100. 8 cm (39. 7 in) Weight=18. 6 kg (41 lb) BMI=18. 3 BMI-for-age= BMI >95 th percentile Overweight

Can you see risk? • This girl is 4 years, 4 weeks old • Is her BMI-for-age in the >85 th to <95 th percentile? • Is she at risk for overweight? Photo from UC Berkeley Longitudinal Study, 1974
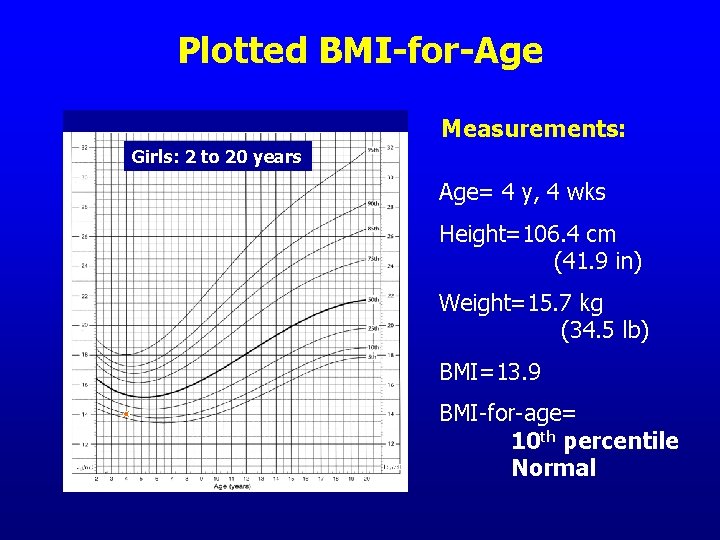
Plotted BMI-for-Age BMI Girls: 2 to 20 years BMI Measurements: Age= 4 y, 4 wks Height=106. 4 cm (41. 9 in) Weight=15. 7 kg (34. 5 lb) BMI=13. 9 BMI BMI-for-age= 10 th percentile Normal

Causes

Causes for Overweight • Overweight and obesity result from an energy imbalance. This involves eating too many calories and not getting enough physical activity • Body weight is the result of genes, metabolism, behavior, environment and culture • Behavior and environment are the greatest areas for prevention and treatment actions (CDC, 2005)

Causes for Overweight "Despite obesity having strong genetic determinants, the genetic composition of the population does not change rapidly. Therefore, the large increase in. . . [obesity] must reflect major changes in non-genetic factors. " * * from Hill, J. O. , & Trowbridge, F. L. (1998) Childhood obesity: future directions and research priorities. Pediatrics. Supplement: 571

Toxic Environment "We take Joe Camel off the billboard because it is marketing bad products to our children, but Ronald Mc. Donald is considered cute. How different are they in their impact, in what they're trying to get kids to do? " -Kelly Brownell, Yale University

Toxic Environment • Encourages overeating and inactivity while at the same time discriminates against overweight or obese individuals • Greater access to pre-packaged, calorie dense foods anytime, anywhere • Portion sizes have increased over last 20 yrs.

COFFEE 20 Years Ago Today Coffee (with whole milk and sugar) Mocha Coffee (with steamed whole milk and mocha syrup) 45 calories 8 ounces How many calories are in today's coffee?

COFFEE 20 Years Ago Today Coffee (with whole milk and sugar) 45 calories 8 ounces Mocha Coffee (with steamed whole milk and mocha syrup) 350 calories 16 ounces Calorie Difference: 305 calories

BAGEL 20 Years Ago 140 calories 3 -inch diameter Today How many calories are in this bagel?

BAGEL 20 Years Ago 140 calories 3 -inch diameter Today 350 calories 6 -inch diameter Calorie Difference: 210 calories

CHEESEBURGER 20 Years Ago 333 calories Today How many calories are in today’s cheeseburger?

CHEESEBURGER 20 Years Ago Today 333 calories 590 calories Calorie Difference: 257 calories

SODA 20 Years Ago 85 Calories 6. 5 ounces Today How many calories are in today’s portion?

SODA 20 Years Ago 85 Calories 6. 5 ounces Today 250 Calories 20 ounces Calorie Difference: 165 Calories

CHEESECAKE 20 Years Ago 260 calories 3 ounces Today How many calories are in today’s large portion of cheesecake?

CHEESECAKE 20 Years Ago 260 calories 3 ounces Today 640 calories 7 ounces Calorie Difference: 380 calories

CHICKEN CAESAR SALAD 20 Years Ago 390 calories 1 ½ cups Today How many calories are in today’s chicken Caesar salad?

CHICKEN CAESAR SALAD 20 Years Ago 390 calories 1 ½ cups Today 790 calories 3 ½ cups Calorie Difference: 400 calories

Child and Adolescent Nutrition • Less than 40% of children and adolescents in the United States meet the U. S. dietary guidelines for saturated fat (US Dpt. of Agriculture, 1998) • Almost 80% of young people do not eat the recommended number of servings of fruits and vegetables (Grunbaum et al. , 2003) • Only 39% of children ages 2– 17 meet the USDA’s dietary recommendation for fiber (found primarily in dried beans and peas, fruits, vegetables, and whole grains) (Lin et al. , 2001)

Child and Adolescent Nutrition • 85% of adolescent females do not consume enough calcium (NIH, 1997) • During the last 25 years consumption of milk has decreased 36% among adolescent females (Cavadini et al. , 2000) • From 1978 to 1998, average daily soft drink consumption almost doubled among adolescent girls, increasing from 6 oz to 11 oz, and almost tripled among adolescent boys, from 7 oz to 19 oz. (US Dpt. of Agriculture, 1998)

Physical Activity • Overweight children average 3, 000 less steps per day than normal weight children (Tudor-Locke et al. , 2004) • 71% of 9 th graders but only 40% of 12 th graders enrolled in a physical education class in 2003 (Grunbaum et al. , 2004)

Physical Activity • The percentage of high school students who attended physical education classes daily decreased from 42% in 1991 to 25% in 1995 • In 2003, 38% of 9 th graders but only 18% of 12 th graders attended a daily physical education class • Among the 56% of students who are enrolled in a physical education class, 80% exercised or played sports for 20 minutes or more during an average class (Grunbaum et al. , 2004)

Secondary Complications

Risks of Obesity and Overweight • 60% of overweight children have at least one risk factor for cardiovascular disease, 25% have at least two risk factors: – BP – Hyperlipidemia – Hyperinsulinemia • Increased risk of endocrine and pulmonary problems, orthopedic, gastroenterological, and neurological difficulties (Strauss, 1999)

Risks of Obesity and Overweight • Type 2 Diabetes account for 8 -45% of all new cases of diabetes (Dietz, 2004) • Risk factors of Type 2 Diabetes include: – increased body fat and abdominal fat – insulin resistance – ethnicity (greater risk in African-American, Hispanic, and Native American children) – onset of puberty (Goran, Ball, & Cruz, 2003) • Prevalence of metabolic syndrome increased with the severity of obesity – Reached 50% in severely obese youngsters – Each half-unit increase in BMI was associated with 1. 55 odds ratio increased risk of metabolic syndrome (Weiss, et al. , 2004)

Obesity and Overweight in Children and Adolescents • Medical Complications: – – – – Endocrine Pulmonary Orthopedic Gastroenterological Neurological Cardiovascular Metabolic Syndrome • Psychosocial Complications: – – Social Stigmatization Teasing Depression Psychosocial Maladjustment – Body Image – Body Dissatisfaction – Self-Esteem

Self-Esteem • Women who were overweight as older adolescents were less likely to be married, had less education, and lower household income than women who had not been overweight at 7 -year-follow-up (Gortmaker, Must, Perrin, Sobol, & Deitz, 1993) • Body dissatisfaction reported in girls as young as 9 years old, and internalization of “thin ideal” predicted to be a critical influence on development of body dissatisfaction (Sands & Wardle, 2003)

Social Stigmatization • Replicated a 1961 study • Found rates of stigmatization is getting worse • 458, 5 th and 6 th grade children ranked drawings of students about how much they liked the student in the picture • Students were overweight, disabled, and “normal” (normal weight or no disability) • Students ranked the overweight child lowest • Girls ranked the overweight student lower than boys (Latner & Stunkard, 2003)

Body Image • Consistently replicated finding that obese children have a more negative body image than their peers (French et al. , 1995; Manus & Killeeen, 1995) • 13601, 9 -12 graders compared self-reported suicidal ideation and attempts to perceived weight and BMI (calculated from self-reported ht and wt) • Negative body image was a risk factor for suicidal ideation even when BMI was controlled for • In other words, perceptions of weight were more important than actual weight with regard to mood and suicide risk (Eaton et al. , 2005)

Self-Esteem • Mixed results in previous literature including: – Lower self-esteem than non-obese peers – No differences – Those that find lower self-esteem is not significantly lower in obese populations when body image is controlled for (Gortmaker, 1993; French et al. , 1995; Manus & Killeeen, 1995; Strauss, 2000)

Self-Esteem • Higher body weight related to lower Physical Appearance subscale scores and mean self-concept (O’Dea & Abraham, 1999) • Decreases in physical and social functioning for overweight vs. non-overweight children (Williams, Wake, Hesketh, 2005)

Self-Esteem • Emphasis of slimness was most strongly linked to: – Body dissatisfaction – Disordered eating – Global self-esteem • An emphasis on popularity and hours spent watching television related to body dissatisfaction • Sport participation seemed to serve as a protective function (Tiggemann, 2001)

Self-Esteem • Current research indicates lower than normal weight peers – Higher body weight students had lower ratings of global selfconcept – Overweight 9 -10 year old students experienced significant declines in self-esteem over 4 years • Why is this important? – Positive self-esteem associated with positive adjustment and functioning while negative self-esteem associated with behavior disorders and negative or depressed mood

Why lower Self-Esteem? • Developmental Changes: – Self-esteem gets lower with increasing age (Strauss, 2000) • Ethnic differences: – White females report lower self-esteem than African American females (Strauss, 2000) • Parental concern: – Obese 10 to 16 year olds more significantly correlated with self-esteem problems than did BMI (Stradmeijer et al. , 2000) – Lower body esteem in 5 yr old girls associated with higer parental concern about weight, independent of actual weight (Davison & Birch, 2001)

Why lower Self-Esteem? • Teasing: – Predictive of lower self-esteem and poorer body image for females and males (Gleason et al. , 2000) • Body image: – Females at greater risk for self-esteem problems due to importance of for self-esteem, but risks increasing for males (Manus & Killeeen, 1995) • Locus of Control: – 9 -11 yr old children reported lower self-esteem if they believed they were responsible for their overweight compared to those who didn’t believe they were responsible (Pierce & Wardle, 1997)

Why lower Self-Esteem? • Increased discrepancy between media images and average individual in the U. S. – 20 yrs. ago the average model was only 8% thinner than the average American, today is 23% thinner – If life size, Barbie would be 5’ 6” tall, 110 lbs. and measure 39, 18, 33 • Back too weak to hold up chest, waist too narrow to hold more than ½ a liver and few centimeters of bowels • Diet industry alone worth estimated $100 billion a year – Overwhelmed with messages about weight loss, negative images of fat and “fat” people

Unsafe (and ineffective) Potential Consequences • A large number of high school students use unsafe methods to lose or maintain weight • A nationwide survey found that during the 30 days preceding the survey: – 13% of students went without eating for one or more days – 6% had vomited or taken laxatives – 9% had taken diet pills, powders, or liquids without the advice of their physicians (Grunbaum et al. , 2003)

Pediatric Weight Management Programs

Pediatric Obesity and Weight Management Programs • Essential components include: – – Behavioral goals (dietary and physical activity) Medical goals to reduce secondary complications Gradual, permanent weight loss Parent involvement • Empirically Supported Treatments exist • Epstein’s Stop Light program • Golan’s program

Effects of Weight Management Programs • Adolescents in weight loss camps showed significant: – Decrease in body dissatisfaction – Increase in global self-worth, athletic competence, and physical appearance (Walker, Gately, Bewick, & Hill, 2003) • Children 10 -15 yo in weight management program with no significant change in average weight or BMI showed a significant: – Decrease in self-concept – Greatest changes in self-concept score (Cameron, 1999)

Program Recommendations • Surgeon General Recommendations: – Recommend Public Health Response settings • • Families and Communities Schools Health Care Media and Communication (U. S. Department of Health and Human Services, 2001)

Program Recommendations • Expert Committee Recommendations: – Children w/BMI 85 th percentile should undergo tx – Tx should include assessment of readiness to engage in program, assessment of diet and physical activity habits, primary goal should be healthy eating and activity – Tx should begin early, involve families, and institute permanent changes – Parenting skills are foundation for successful intervention w/gradual targeted increases in activity and targeted reductions in high-fat, high-calorie foods – Ongoing support for families after initial weightmanagement programs (Barlow & Dietz, 1998)

Empirically Supported Treatments • Chambless Criteria for Well Established Txs – Minimum of 2 well-designed between group studies demonstrating efficacy of a particular treatment when compared to psychological placebo or alternative treatment – Equivalent to an already established treatment – Inclusion of treatment manuals – Clear definition of sample characteristics – Treatment effects must be demonstrated by at least two investigators (Jelalian & Saelens, 1999)

Empirically Supported Treatments • Criteria for inclusion: – • Studies with children and adolescents that targeted weight loss as a primary objective or reported information through quantitative or illustrative presentation of weight loss if other outcomes were primary interest Criteria for exclusion: – – Conducted primarily in school setting Conducted with special populations Used medication trials Included participants older than 18 years old (Jelalian & Saelens, 1999)

Studies for Children • 26 studies • Comprehensive behavioral treatment targeting eating and physical activity is superior to wait-list control or nutrition education alone • 4 studies by Epstein and colleagues document long-term maintenance of loss up to 10 years • Components include: – – – – Targeted diet combined with lifestyle or aerobic activity Parental inclusion Behavior modification Self-monitoring of diet and activity Stimulus control Contingency management Parent training (Jelalian & Saelens, 1999)

Studies for Adolescents • 7 studies • “Promising interventions” exist: – 1) At least one well-controlled study and another less rigorously controlled study by a separate investigator, – 2) 2 or more well-controlled studies w/small numbers, or – 3) 2 or more well-controlled studies by the same investigator (Jelalian & Saelens, 1999)

Studies for Adolescents • Overlap in inclusion of behavioral modification of diet, but: – Not as well developed – No rigorously conducted study documenting that outpatient obesity treatment is superior to wait-list control or instruction only • Mixed Group (Children and Adolescents or nonstated) – 9 studies (Jelalian & Saelens, 1999)

Traffic Light Diet • 13 of 26 Childhood studies were by Epstein • Empirically supported with multiple studies demonstrating significant weight loss that is maintained up to 10 years post treatment • Tx implementation that includes teaching children and parents how to label foods as “green, yellow, and red” foods based on calorie and nutrient density • Tx also includes developing healthy eating and activity environment for children, behavior change techniques, and maintenance of behavior change (Epstein et al. , 2000; Epstein et al. , 2001)

More Epstein…… • Evaluated problem solving in obesity treatment and found that additional problem solving did not add to effectiveness beyond standard family-based treatments (Epstein et al. , 2000) • Compared emphasizing fruit and vegetable intake vs. fat and sugar intake and found significantly greater decreases in % overweight in fruit and vegetable intake group (Epstein et al. , 2001) • Compared stimulus control to reinforcement to target sedentary behavior, found to be equivalent methods (Epstein et al. , 2004)

Golan’s Alternative Approach • “Health-centered” Approach • 60 children 7 -12 years old in a family-based health -centered approach targeting only parents vs. children-only control group • Demonstrated 29% reduction in children’s overweight vs. 20. 2% reduction in children-only group 7 yr follow-up • At 7 yr follow-up, 2 children from child-only condition exhibited eating disordered symptoms, no children from parent-only condition exhibited eating disordered symptoms (Golan & Crow, 2004)

Primary Care Program • 4 -month behavioral weight control program initiated in a primary care setting and extended through telephone and mail contact • Treatment group had better change in BMI and higher use of behavioral skills than in control group • No significant difference between groups for energy intake, percentage calories from fat, physical activity, sedentary behavior, and problematic weight-related or eating behaviors (Saelens, et al. , 2002)

Planet Health • School-based multidisciplinary intervention for 2 years with session focused on: – – Decreasing television viewing Decreasing consumption of high-fat foods Increasing fruit and vegetable intake Increasing moderate and vigorous physical activity • Female obesity reduced compared to controls, no difference among boys (Gortmaker et al. , 1999) • Also had reduced risk of using self-induced vomiting/laxatives or diet pills to control weight in past 30 days (Austin et al. , 2005)

PACE+ for Adolescents • Patient-Centered Assessment and Counseling for Exercise • 117 adolescents 11 -18 years recruited from pediatric and adolescent clinics • Receive interactive computer counseling, provider counseling, and extended follow-up • Intervention targets: – – Moderate physical activity Vigorous physical activity Fat intake Fruit and vegetable intake • All outcomes except physical activity improved over time, extended interventions (mail or telephone) showed no greater outcomes (Patrick et al. , 2001)

Cost Effectiveness of Programs • • 24 families randomized to group + individualized tx or group tx only All groups included: – – – • Traffic Light Diet Physical Activity Self-monitoring Stimulus Control Reinforcement Group treatment alone is more cost effective than mixed group plus individual format (Goldfield, et al. , 2001)

Weight Management Programs and Self-Esteem • Epstein and Golan – No data on self-esteem rates or changes for participants • Negative Changes – Cameron, 1999 • No significant weight loss • Positive Changes – Savoye et al. , 2005 • Increased at post, but back to baseline at follow-up – Walker et al. , 2003 & Gately et al. , 2005 • Increased during a camp setting • Significant weight loss • No follow-up data

Why the Change in Self-Esteem? • Weight loss – • Behavioral goals – – • Decreasing consumption of high fat and high calorie foods Increasing physical activity levels Locus of Control – – • Large focus during programs on “losing weight” Locus of Control: An individual’s belief regarding their control over personal outcomes Limited data on pediatric obesity and locus of control All hypotheses, none yet examined in a pediatric weight management program

Obesity and Locus of Control in Children • Pierce and Wardle (1997) Findings – Examined the belief systems of 9 -11 year old overweight children – Children who indicated they felt their overweight was due to internal causal beliefs (“I eat too much” or “I don’t exercise enough”) were strongly and negatively correlated to self-esteem – Children who indicated that they felt their overweight was due to external causes (“It runs in my family” or “A medical cause”) were strongly and positively correlated to self-esteem

Project STORY

Project STORY • Project Sensible Treatment of Obesity Rural Youth (STORY) • 4 month pediatric weight management program • Delivered in 3 “waves” in rural counties in north central Florida • Interventions delivered in Cooperative Extension Office

Participants • Data from larger study • Participants – 90 overweight children and their parent(s) – 8 -13 years old from 4 rural counties • Inclusion/Exclusion Criteria – Child at or above 85 th percentile – Participating parent living in home primarily or equally responsible for food purchasing and meal preparation – No condition contraindicating participation in a weight management program such as dietary and exercise restrictions – See proposal for additional criteria

Intervention Groups • Basic Program – Modified Stop-Light Program – Use of red, yellow, green classification – Physical activity targets and goals – Self-esteem and body image addressed – Behavioral modification techniques to help parents and children reach these goals

Intervention Groups • Behavioral Family Intervention (BFI) – Simultaneous but separate child and parent treatment groups • Behavioral Parent Intervention (BPI) – Parent only treatment group where parents encouraged to serve as child’s interventionist at home • Weight List Control Group (WLC) – Will receive BFI condition after the 6 -month follow-up

Project STORY Goals 1) Decrease consumption of high fat and high calorie foods with modified version of “Stop Light Program” 2) Increase physical activity with pedometers and daily physical activity logs 3) Address Self-Esteem and Body Image with specific interactive lessons

Summary • Pediatric Obesity is a major Public Health Concern • Prevalence will only rise in “toxic environment” • Early intervention and prevention is critical to prevent medical, psychosocial, and disease-related costs • Empirically supported treatments for children are available with long term maintenance • Self-Esteem should be monitored and targeted in overweight and obese individuals • More research is needed with adolescents • Effective program components, cost effectiveness, and media messages are among the next directions for the field of research

Questions?
- Slides: 109