PEDIATRIC OBESITY AND THE METABOLIC SYNDROME Whitney Brown

PEDIATRIC OBESITY AND THE METABOLIC SYNDROME Whitney Brown, M. D. Division of Pediatric Endocrinology

LECTURE OBJECTIVES Know the BMI percentile cutoffs for pediatric overweight, obesity, and morbid obesity Recall the co-morbidities associated with pediatric obesity Understand that there is no current accepted definition for the metabolic syndrome in pediatrics Be familiar with the laboratory screening recommendations in pediatric obese patients Discuss the treatment options/recommendations for pediatric obesity and some of its co-morbidities

Calories In Calories Out

EPIDEMIOLOGY National Health and Nutrition Examination Survey (NHANES)1 2007 -2008 16. 9% of children (age 2 -19 years) obese 1970 5% In South Carolina— 26. 9% 50% of obese children (>6 years) will become obese adults 2 10% for nonobese children 1 Ogden CL, et al. JAMA. 2010; 303(3): 242– 249 2 Whitaker RC, et al. NEJM. 1997; 337(13): 869 -873
![DEFINING PEDIATRIC OBESITY Body Mass Index (BMI) Weight (kg)/ [height (m)]2 Preferred method for DEFINING PEDIATRIC OBESITY Body Mass Index (BMI) Weight (kg)/ [height (m)]2 Preferred method for](http://slidetodoc.com/presentation_image/5939047c698b5a8332a28bbd197408c2/image-5.jpg)
DEFINING PEDIATRIC OBESITY Body Mass Index (BMI) Weight (kg)/ [height (m)]2 Preferred method for evaluating obesity Age 2 -19 years Correlates strongly with body fat percentage

DEFINING PEDIATRIC OBESITY (CONT. ) 1994 -Expert Committee on Clinical Guidelines for Overweight in Adolescent Preventative Services Overweight BMI > 30 kg/m 2 BMI ≥ 95 th percentile for age and gender “At risk for overweight” BMI ≥ 85 th but ≤ 95 th percentile 2005 -Institute of Medicine Obese BMI > 30 kg/m 2 BMI ≥ 95 th percentile for age and gender

DEFINING PEDIATRIC OBESITY (CONT. ) 2007 -American Academy of Pediatrics Overweight BMI ≥ 85 th but ≤ 95 th percentile Obese BMI > 30 kg/m 2 BMI ≥ 95 th percentile for age and gender Morbidly obese BMI ≥ 99 th percentile If < 2 yo Overweight Weight for lenth ≥ 95 th percentile for age and gender

OBESITY-RELATED CO-MORBIDITIES § Cardiovascular Conditions • Hyperlipidemia • Hypertension (HTN) § Orthopedic Conditions • Blounts Disease • Hip Disorders (SCFE) § Endocrine Conditions • Dysmetabolic Syndrome • Type 2 Diabetes • Impaired Glucose Tolerance • Menstrual Irregularities • Polycystic Ovarian Syndrome • Accelerated Growth § Psychological Conditions • Depression/Self-Esteem • Substance Abuse • Disordered Eating • Discrimination § Pulmonary Conditions • Asthma • Sleep Apnea § Gastrointestinal Conditions • Non-Alcoholic Fatty Liver Disease (NAFLD) • Gallstones

ACCEPTED DEFINITION OF THE METABOLIC SYNDROME IN ADULTS Zimmet P, et al. Diabetes Voice. 2005; 50(3): 31 -33 International Diabetes Federation

WAIST CIRCUMFERENCE 102 cm 88 cm ATP III

PREVALENCE OF THE METABOLIC SYNDROME Overall incidence Age 12 -19 years 3 -4% Age 20 -29 years 6. 7% Adults ≥ 30 years 23. 7% NHANES III (n=2400) Adolescents age 12 -19 years BMI ≥ 95 th percentile 28. 7% BMI 85 th-94 th percentile 6. 1% BMI ≤ 84 th percentile 0. 1% Cook S, et al. Arch Pediatr Adolesc Med. 2003; 157 (8): 821 -827

PEDIATRIC METABOLIC SYNDROME: NEED FOR A STANDARD DEFINITION Reviewed 27 articles 46 unique definitions of pediatric metabolic syndrome Most emulated the NCEP approach BMI or waist circumference Blood pressure Lipid levels Glucose abnormalities Different cut-offs/percentiles were used in the various definitions Ford ES, et al. J Peds. 2008; 152(2): 160 -164
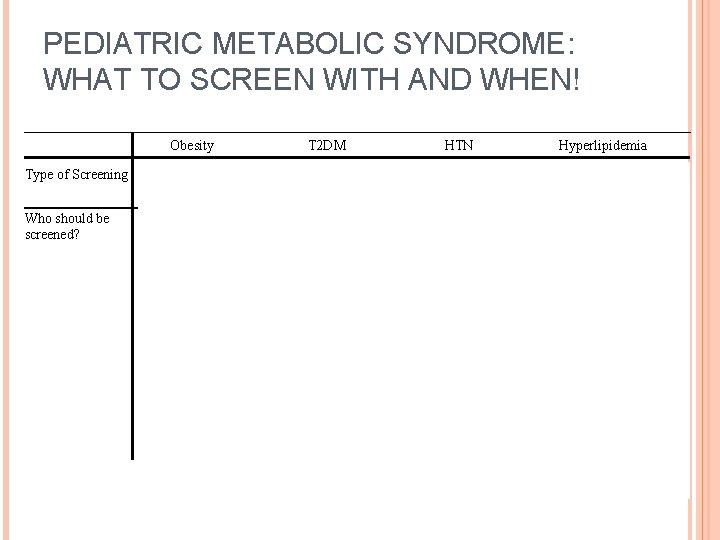
PEDIATRIC METABOLIC SYNDROME: WHAT TO SCREEN WITH AND WHEN! Type of Screening Who should be screened? Obesity BMI All children >2 yo T 2 DM HTN Hyperlipidemia FBG or 2 hr OGTT (? Hb. A 1 c) Measure BP Fasting lipid panel Children ≥ 10 yo All children ≥ 3 yo All children ≥ 2 yo Or IF At onset of puberty Family hx of premature CVD IF OR BMI >85 th %ile If other risk factors present: AND BMI> 95 th percentile ≥ 2 risk factors Diabetes (+)family hx for T 2 DM Smoking Ethnic minority HTN Signs of insulin resistance

Overweight/Obesity Glucose abnormalities Blood pressure Fasting lipid levels • Overweight: BMI ≥ 85 th percentile • Obese: BMI ≥ 95 th percentile • Morbidly BMI ≥ 99 th percentile • ADA criteria • Impaired fasting glucose (IFG) § ≥ 100 but <126 • Impaired glucose tolerance (IGT) § ≥ 140 but <200 • At risk for developing T 2 DM § Hb. A 1 c between 5. 7 and 6. 4% • Norms varying depending on age, height, and gender • Norms very depending on age/gender
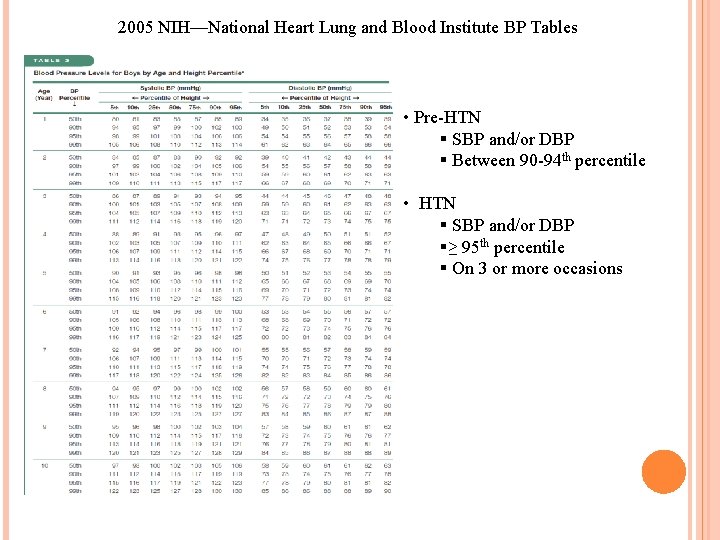
2005 NIH—National Heart Lung and Blood Institute BP Tables • Pre-HTN § SBP and/or DBP § Between 90 -94 th percentile • HTN § SBP and/or DBP §≥ 95 th percentile § On 3 or more occasions
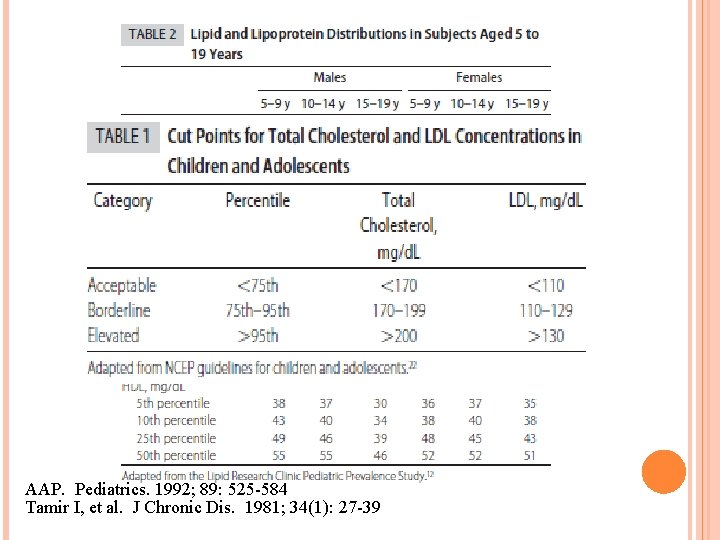
AAP. Pediatrics. 1992; 89: 525 -584 Tamir I, et al. J Chronic Dis. 1981; 34(1): 27 -39

OFF THE RECORD: No accepted definition of pediatric metabolic syndrome Clinically I use: BMI ≥ 85 th percentile plus ≥ 2 of the following HDL <10 th percentile (~40 mg/d. L) TG >95 th percentile IGT or IFG BP ≥ 90 th percentile

EVALUATION OF PEDIATRIC OBESITY

HISTORY Complete dietary history Meals/snacks Portion sizes Dining out Fried food Drinks Complete physical activity history PE Activity outside of school Intensity Number of hours per day TV, video games, computer, talking/texting on phone ROS Geared toward the co-morbidities associated with obesity
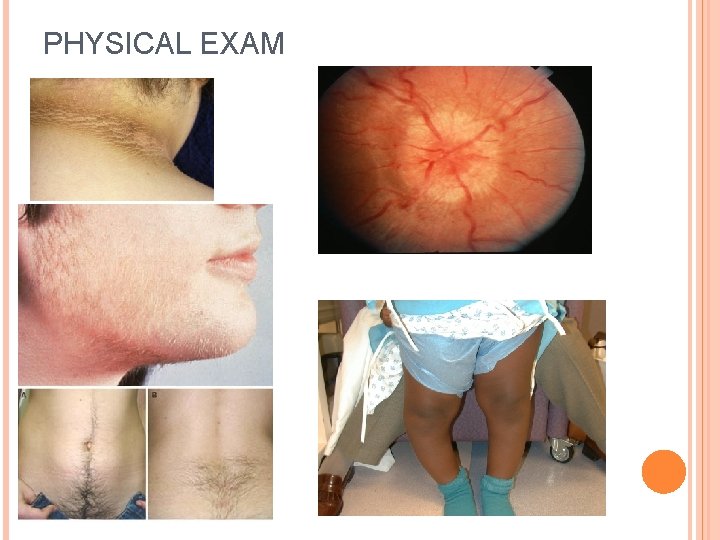
PHYSICAL EXAM
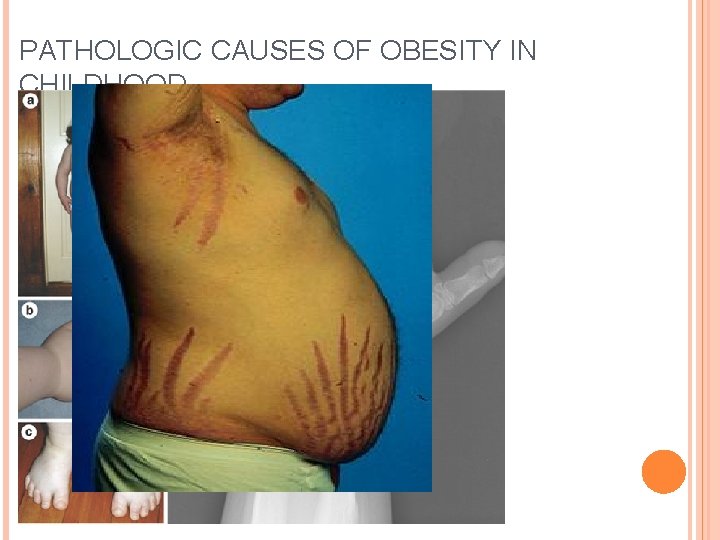
PATHOLOGIC CAUSES OF OBESITY IN CHILDHOOD Pseudohypoparathyroidism Albright Hereditary Osteodystrophy Cushing syndrome Laurence Moon or Bardet-Biedel syndrome Prader Willi syndrome MC-4 R mutation Congenital leptin deficiency POMC mutation Fragile X syndrome Trisomy 21
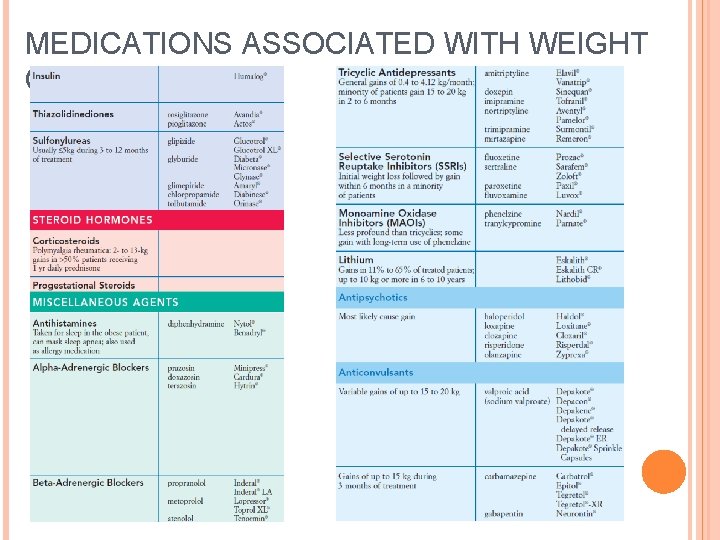
MEDICATIONS ASSOCIATED WITH WEIGHT GAIN

LAB SCREENING RECOMMENDATIONS Overweight with no risk factors: Fasting lipid panel Overweight with risk factor(s): Fasting lipid panel AST/ALT Fasting glucose Obese (± risk factors) Fasting lipid panel AST/ALT Fasting glucose BUN/Cr Risk Factors: • Family Hx of obesity-related diseases • Elevated BP • Elevated lipid levels • Tobacco use
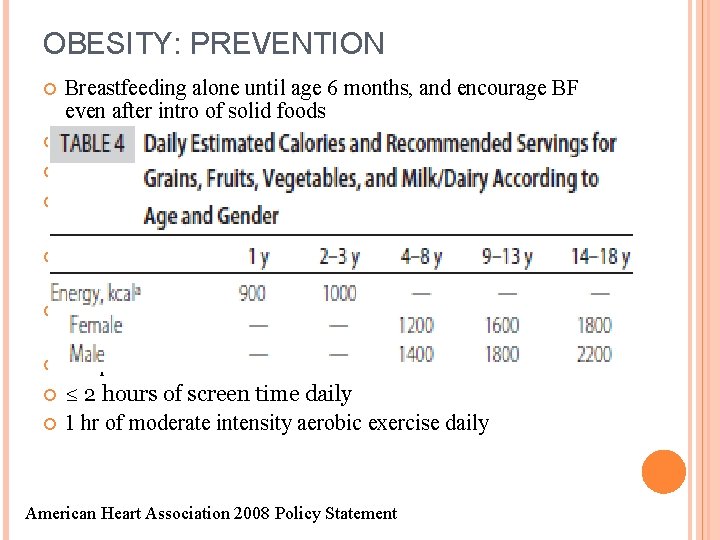
OBESITY: PREVENTION Breastfeeding alone until age 6 months, and encourage BF even after intro of solid foods Do not skip meals Eat meals as a family; Dining out ≤ 2 x/week Avoid high sugar beverages Drink 3 -4 8 -oz glasses of skim milk daily ≤ 12 oz of 100% fruit juice daily Ca and Vit D fortified Portion sizes should be limited to the amount of recommended calories for age Keep TVs and other electronics out of bedrooms ≤ 2 hours of screen time daily 1 hr of moderate intensity aerobic exercise daily American Heart Association 2008 Policy Statement

OBESITY: TREATMENT STAGES Prevention (P) All children Promotion and support for: Breastfeeding Family meals Limited screen time Regular physical activity Yearly BMI monitoring When 3 - 6 months of SWM fails BMI between the 85 th - 94 th percentiles Comprehensive Multidisciplinary Intervention (CMI) Prevention Plus (PP) More frequent visits with an MD and a dietician May include exercise and behavioral specialists Tertiary Care Intervention BMI ≥ 99 th percentile with associated comorbidities SWM and CMI failed 5 servings of fruits and vegetables/day 2 hours or less of screen time 1 hour or more of physical activity 0 sugared drinks Incudes everything else plus: Meal replacements Pharmacotherapy Bariatric surgery Structured Weight Management (SWM) If PP fails BMI is between 95 th - 98 th percentiles More frequent follow-up with written diet and exercise plans Barlow SE and the AAP Expert Committee. Pediatrics. 2007; 120(4): S 164 -S 192
HEALTHY LIFESTYLES CLINIC: PALMETTO HEALTH RICHLAND Individual Group education Session

Breakfast Everyday 5 servings of fruits/veggies 3 structured meals daily ≤ 2 hrs daily of TV/video time ≥ 1 hr/day of moderate activity Almost no high sugar beverages

OBESITY: PHARMACOTHERAPY Orlistat (Xenical or Alli) Metformin FDA-approved for children ≥ Not FDA approved for obesity 12 yo Inhibits GI lipases Dose: 120 mg TID For T 2 DM During or up to 1 hr after meal MVI 2 hrs before or after orlistat GI side effects common Approved in children ≥ 10 yo Metformin ER FDA approved ≥ 17 yo Major effects: ↓ hepatic gluconeogenesis ↑ peripheral insulin sensitivity

METFORMIN (CONT. ) Starting dose 500 mg Qday, increased to a max of 1000 mg BID Titrating slow can limit GI-side effects MVI with vit B 12 Contraindictaed in: Renal failure Chronic hypoxic states Use of radiocontrast dye Very rare side effects: decreased platelet aggregation and hemolytic anemia Check BUN/Cr and CBC Before initiation Every 2 years

METFORMIN USE IN PEDIATRIC OBESITY Review of 5 RCTs from 2001 -2008 Children age 6 -19 years (n=320) All trials lasted 6 months Metformin 1000 -2000 mg/day or placebo BMI reduction of 1. 42 kg/m 2 Improved insulin sensitivity Need larger, long term studies Park MH, et al. Diabetes Care. 2009; 32(9): 1743 -1745

ELEVATED LDL: TREATMENT RECOMMENDATIONS Recommended LDL Concentrations for Pharmacologic Treatment of Children and Adolescents 10 years and Older Patient Characteristics Recommended Cut Points No other risk factors for CVD LDL concentration is persistently > 190 mg/d. L despite diet therapy Other risk factors present, including obesity HTN, tobacco use, or positive family hx LDL concentration is persistently > 160 mg/d. L despite diet therapy or premature CVD Children with diabetes mellitus Pharmacologic treatment should be considered when LDL concentration is ≥ 130 mg/d. L Daniels SR, et al. Pediatrics. 2008; 122: 198 -208

HYPERLIPIDEMIA PHARMACOTHERAPY

FISH OIL: COROMEGA

STAGES OF PEDIATRIC HTN Normal < 90 th percentile Pre-hypertension ≥ 90 th percentile and < 95 th percentile Stage 1 hypertension ≥ 95 th percentile and ≤ 99 th percentile +5 mm. Hg Stage 2 hypertension > 99 th percentile + 5 mm. Hg

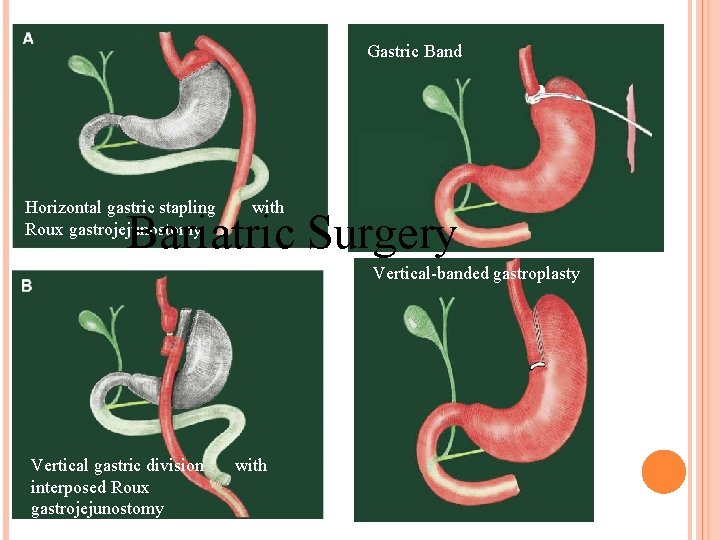
Gastric Band Horizontal gastric stapling with Roux gastrojejunostomy Bariatric Surgery Vertical-banded gastroplasty Vertical gastric division with interposed Roux gastrojejunostomy

OPTIONS FOR OBESITY MANAGEMENT: BARIATRIC SURGERY ASBS 2004 Consensus Statement � Adolescent candidates BMI ≥ 40 kg/m 2 BMI of 35. 0 kg/m 2 to 39. 9 kg/m 2 in the presence of severe comorbidities Type 2 diabetes Life-threatening cardiopulmonary problems Severe sleep apnea � Pickwickian syndrome � Obesity-related cardiomyopathy � Obesity-induced physical problems interfering with a normal lifestyle � Joint disease treatable but for the obesity Body size problems precluding or severely interfering with Employment � Family function � Ambulation � Buchwald, H. Surgery for Obesity and Related Diseases. 2005; 1: 371– 381

BARIATRIC SURGERY (CONT. ) Adolescent candidates (cont. ) � Puberty complete � Obtained 95% of predicted adult stature � Need to understand that: Long term efficacy and potential adverse consequences related to decreased absorption of nutrients unknown Degree of recidivism remains unknown Buchwald, H. Surgery for Obesity and Related Diseases. 2005; 1: 371– 381
AN UPDATE ON 73 US OBESE PEDIATRIC PATIENTS TREATED WITH LAPAROSCOPIC ADJUSTABLE GASTRIC BANDING: COMORBIDITY RESOLUTION AND COMPLIANCE DATA NYU Division of Pediatric Surgery � First 73 patients to undergo lapband Aged 13 to 17 years (mean 15. 8 ± 1. 2 years) 54 females and 19 males Mean preop wt: 298 lb, with a BMI 48 kg/m 2 Mean estimated wt loss post-op: 6 months: 35% ± 16% 1 year: 57% ± 23% 2 years: 61% ± 27% Nadler, EP, et al. J Pediatr Surg. 2008 Jan; 43(1): 141 -6

AN UPDATE ON 73 US OBESE PEDIATRIC PATIENTS TREATED WITH LAPAROSCOPIC ADJUSTABLE GASTRIC BANDING: COMORBIDITY RESOLUTION AND COMPLIANCE DATA (CONT. ) Complications � Band slippage (6) Gastric perforation (1) � Symptomatic hiatal hernias (3) � Asymptomatic iron deficiency (13) � Asymptomatic vitamin D deficiency (4) � Mild subjective hair loss (14) Nadler, EP, et al. J Pediatr Surg. 2008 Jan; 43(1): 141 -6

FINAL THOUGHTS Childhood obesity has reached epidemic proportions There is no current accepted definition for pediatric metabolic syndrome Mainstay of treatment is DIET/EXERCISE counseling The counseling should start in early childhood and BEGINS with the caregivers Pediatrician or Family practitioner Consider referral to weight management program After age ≥ 6 years if Prevention and prevention plus fail BMI ≥ 95 th percentile with co-morbidity BMI ≥ 99 th percentile

ANY QUESTIONS?
- Slides: 42