Pediatric Mortality Morbidity Conference Presented by R 3

Pediatric Mortality & Morbidity Conference Presented by R 3 吳承翰 Supervised by 張孟維 醫師 Moderator 邱德發 主任 1

General Data n n n Date of birth: 2000/10/12 (5 yrs 11 mo) Chart No: 20999721 Gender: female Body weight: 15 kg Time of arrival: 2006/09/19 16: 10 Triage n n 主訴發燒 BT 36. 6℃, HR 125/min, RR 26/min, BP 111 /83 mm. Hg Sat. O 2 98% 2
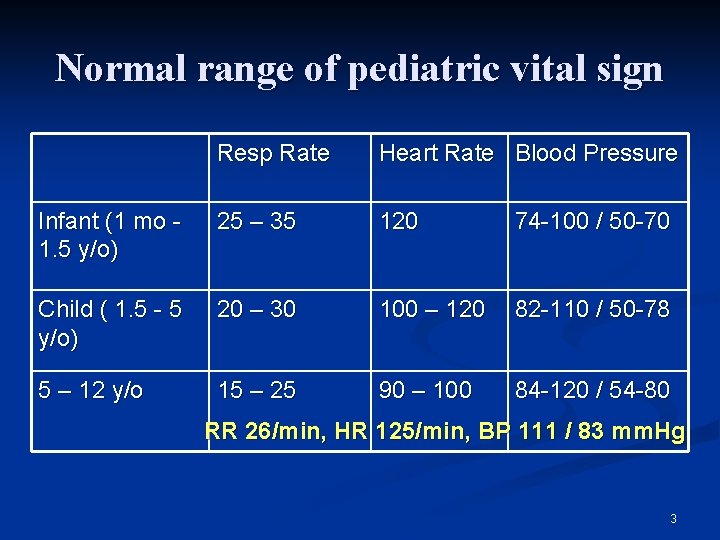
Normal range of pediatric vital sign Resp Rate Heart Rate Blood Pressure Infant (1 mo 1. 5 y/o) 25 – 35 120 74 -100 / 50 -70 Child ( 1. 5 - 5 y/o) 20 – 30 100 – 120 82 -110 / 50 -78 5 – 12 y/o 15 – 25 90 – 100 84 -120 / 54 -80 RR 26/min, HR 125/min, BP 111 / 83 mm. Hg 3

Chief complaint n Fever for 5 days, up to 40 ℃, chillness(+) A n Lethargy Appaerance 1. interactiveness ? 2. consolability? 3. look/gaze? 4. speech/cry? n n n B Mild tachypnea C Pale skin CRT not documented 4

Present illness n n n n Fever with Mild Cough for 5 days Rhinorrhea(-) Activity ↓ with somnolent episodes Abdominal epigastric pain for 3 days, nausea(-), vomitting(-) Decreased urine output Transferred from 壢新 hospital due to bronchopneumonia and abnormal liver function test Past and personal history: not documented 5

Physical examination n General appearance n Weakness (lethargy) n GCS: E 4 V 5 M 6 HEENT n Pupil: 3+/3+ n Throat: not injected Chest n Breathing sound: R’t side ronchi n RHB, tachycardia n n n Abdomen n normoactive bowel sound n Soft, flat Extremity n No specific finding Skin: rash (-), pale 6

What else do you want about Hx and PE ? 7

Present illness Original Hx n Fever with Mild Cough for 5 days, Rhinorrhea( -) n Activity ↓ with somnolent episodes n Epigastric pain for 3 days, nausea(-), vomitting(-) n urine output ↓ More Information needed n Upper airway symptoms, n Dyspena, DOE, orthopnea n CNS symptoms, headache, con’s level ( drowsy ? ) n Character of abd pain, GI symptoms, appetite, shifting pain, pain with movement n Urine color, volume n Myoclonus jerk n Travel Hx, school 8 environment

Physical examination Original PE n General appearance n Weakness, E 4 V 5 M 6 n HEENT n Pupil: 3+/3+ n Throat: not injected n Chest n R’t side ronchi , RHB, tachycardia n Abdomen n Normoactive, Soft, flat n Extremity n No specific finding n Skin: rash (-), pale More thorough PE needed n Detailed NE: including Meningeal signs, IICP signs, focal neurological signs n ENT field: ear drum, mucosa, ulcer n Lymph Node n Cardiopulmonary sign: murmur, rales, resp. accessory muscle, JVE, n Abd: hepatomegaly, Murphy sign, Mcburney point tenderness, knocking pain n petechia 9

Present illness Original Hx n Fever with Mild Cough for 5 days, Rhinorrhea(-) n Activity ↓ with somnolent episodes n Abdominal epigastric pain for 3 days, nausea(-), vomitting(-) n urine output ↓ More Information n Dyspena, DOE n Drowsy, no myoclonic jerk n Persistent dull pain, poor appetite, no shifting pain, no pain with movement, abd. fullness n Deep yellow urine color n No travel Hx 10

Physical examination Original PE n General appearance n Weakness, E 4 V 5 M 6 n HEENT n Pupil: 3+/3+ n Throat: not injected n Chest n R’t side ronchi , RHB, tachycardia n Abdomen n Normoactive, Soft, flat n Extremity n No specific finding n Skin: rash (-), pale More PE n no meningeal signs, no focal neurological signs n normal ear drum, no oral ulcer, no oral vesicles n No palpable lymph node n Bil. rales, mild resp. distress with some intercostal retraction, no JVE, n Abd: lower liver edge, no Murphy sign, no Mcburney point tenderness, no knocking pain, n no petechia 11

Question What is your first impression and management ? 12

Our first impression should include DDx should be considered first n Myocarditis ü Fever, malaise for several days, tachypnea, tachycardia, decreased perfusion, pul. congestion, cong. liver with ab. N LF û Fever course n Bronchopneumonia ü Fever, cough for several days, tachypnea, rhonchi û Epigastralgia, Epigastralgia ab. N LF n Severe sepsis r/o septic shock DDx also considered n n Kawasaki disease Virus n Roseola n Adenovirus n EBV Liver abscess CNS Infection 13

Managements we need to take n n n ABC n O 2 supplement n Fluid supplement depend on skin turgor & volume status Monitor equipment n Oximeter, EKG monitor Lab n CBC/DC, F/S, BUN, Cr, AST, ALP, Bili(T), Troponin I, Na, K, B/C, U/A, venous blood gas n CXR, EKG Rx n Rocephin stat dose for toxic appearance Critical inform 14

Impression at ED 1. 2. 3. bronchopneumonia sepsis, R/O septic shock Hepatitis, cause ? 15

Initial management (16: 22 0 h 12 m) CBC/DC, n CRP, Cr, Na, K, Ca, Cl, Sugar, AST, ALP n Flowcytometry, U/A n B/C, U/C n IVF with D 5 1/4 S run 50 cc/hr n (16: 50 0 H 40 M) n Aq-PCN(300 million u) 0. 5 pc stat + Q 6 H 16
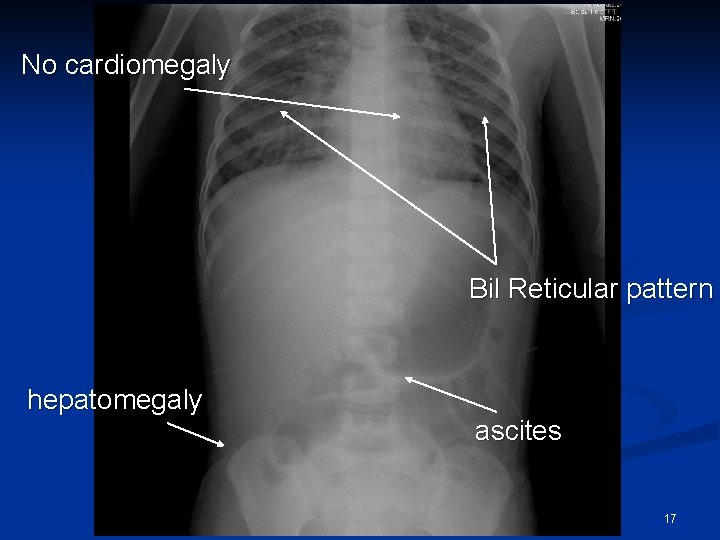
No cardiomegaly Bil Reticular pattern hepatomegaly ascites 17

Hemogram n n n n RBC: 4. 51 million/u. L Hb: 11. 6 g/dl Hct: 34. 7 % MCV: 76. 9 f. L MCH: 25. 7 pg/cell MCHC: 33. 4 g/dl RDW: 14. 2 % Platelet: 38 k/u. L n n n n n WBC: 3600/u. L Atypical-lym: 2. 0 % Myelocyte: 1% Meta-Myelocyte: 2. 0% Segment: 34 % Band: 14% Lymphocyte: 45 % Monocyte: 1. 0 % Eosinophil: 1. 0% 18
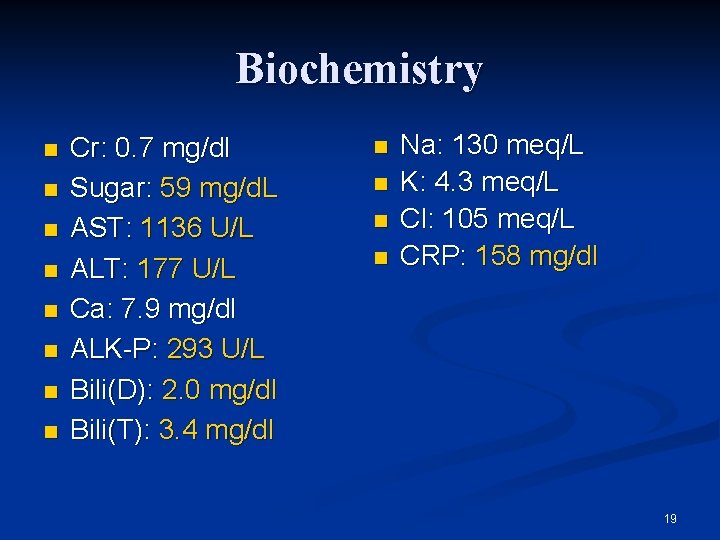
Biochemistry n n n n Cr: 0. 7 mg/dl Sugar: 59 mg/d. L AST: 1136 U/L ALT: 177 U/L Ca: 7. 9 mg/dl ALK-P: 293 U/L Bili(D): 2. 0 mg/dl Bili(T): 3. 4 mg/dl n n Na: 130 meq/L K: 4. 3 meq/L Cl: 105 meq/L CRP: 158 mg/dl 19
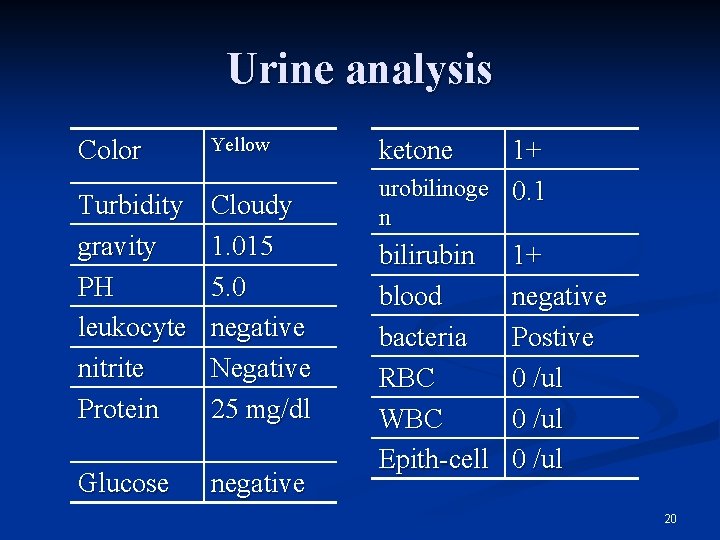
Urine analysis Color Yellow Turbidity gravity PH leukocyte nitrite Protein Cloudy 1. 015 5. 0 negative Negative 25 mg/dl Glucose negative ketone 1+ urobilinoge 0. 1 n bilirubin blood bacteria RBC WBC Epith-cell 1+ negative Postive 0 /ul 20

Do we confirm our DDx ? n n Myocarditis - still can’t be r/o Severe sepsis r/o septic shock n Bronchopneumonia - less likely, pul congestion rather than pneumonic patch n Liver abscess - unlikely n CNS Infection - unlikely 21

What action will you take now ? 22

For this P’t with toxic appearance On critical n ICU admission n Consult CV/CVS for heart survey ( 2 D echo ) and ECMO ( if indicated ) n Virus titer (CMV EBV HIV HSV VZ) n Consider inotropes n 23

(19: 09 3 h 0 m) n HR 123 RR 25 BP 93/62 n Troponin I, CPK, CK-MB Check BP and HR Q 1 H 24

CPK: 65 U/dl n CK-MB: 0. 9 ng/ml n Troponin I: 0. 02 ng/ml n (20: 26 4 h 10 m) n Admitted to ward 25

Ped ward course 09/19 21: 10 BT 37. 8 HR 120 RR 32 BP 92/68 n Admitted to Ped ordinary ward n Acute ill looking n Bil coarse rhonchi; abd distention(+), guarding(+); capillary refilling time > 2 sec n Ward impression n r/o septic shock Abd pain r/o holo-organ perforration Ward plan n N/S resuscitation, antibiotics, DIC profile 26

Ped ward course 09/19 21: 40 n BT 37. 6 HR 133 RR 32 BP 94/58 E 4 V 5 M 6 n Massive coffee ground vomitus n Four limbs cooling n Nasal flaring n N/S 200 cc stat n Transfer to PICU 27
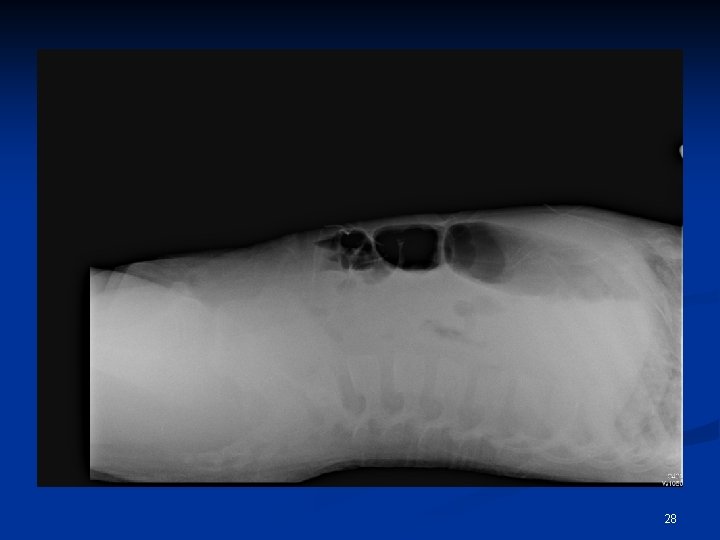
28
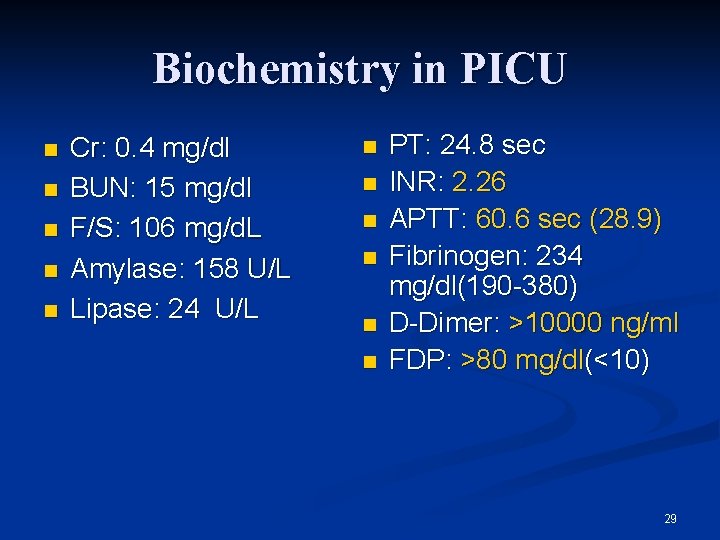
Biochemistry in PICU n n n Cr: 0. 4 mg/dl BUN: 15 mg/dl F/S: 106 mg/d. L Amylase: 158 U/L Lipase: 24 U/L n n n PT: 24. 8 sec INR: 2. 26 APTT: 60. 6 sec (28. 9) Fibrinogen: 234 mg/dl(190 -380) D-Dimer: >10000 ng/ml FDP: >80 mg/dl(<10) 29

PICU course 09/20 (day 2) Vancomycin + Claforan + Metronidazole f/u liver function n Bili(T) 4. 2 Bili(D) 2. 7 n AST/ALT 1342/165 n PT/APTT 27. 1/71. 5 n n n FFP, PLT transfusion Alb supplement n Arrange abd echo n Hepatosplenomegaly, gall bladder wall thickening(7 mm), increased bil renal echogenecity, ascites, bil pleural effusion 30

PICU course 09/20 (day 2) n Consult Infection n VAHS is compatible clinically n Bone marrow aspiration is recommended n IVIG therapy n Consult hematologist for further Tx( VP-16 ) 31

Hemophagocytic lymphohistiocytosis n n HLH is a life-threatening, characterized by fever, hepatosplenomegaly, pancytopenia, hypertriglyceridemia, hypofibrinogenemia and CNS disease, commonly seizures HLH is also known as n autosomal recessive familial hemophagocytic lymphohistiocytosis (FHL), n familial erythrophagocytic lymphohistiocytosis (FEL) n viral-associated hemophagocytic syndrome (VAHS) 32

Diagnostic criteria for HLH Major criteria n fever n splenomegaly n cytopenia involving 2 or more cell lines n Hypertriglyceridemia or hypofibrinogenemia n Hemophagocytosis Alternative criteria n low or abscent natural (NK ) cell activity n serum ferritin > 500 μg / L n Soluble CD 25 > 2400 U / ml 33

PICU course n n n 09/20 (day 2) n IVIG Tx 09/21 (day 3) 00: 20 n E 3 V 2 M 5, tachypnea, Oximeter 80 n O 2 hood change to O 2 mask 50 % 09/21 (day 3) 02: 35 n BT 35. 9 HR 153 RR 40 BP 103/64 Sat 80% n intubation 34
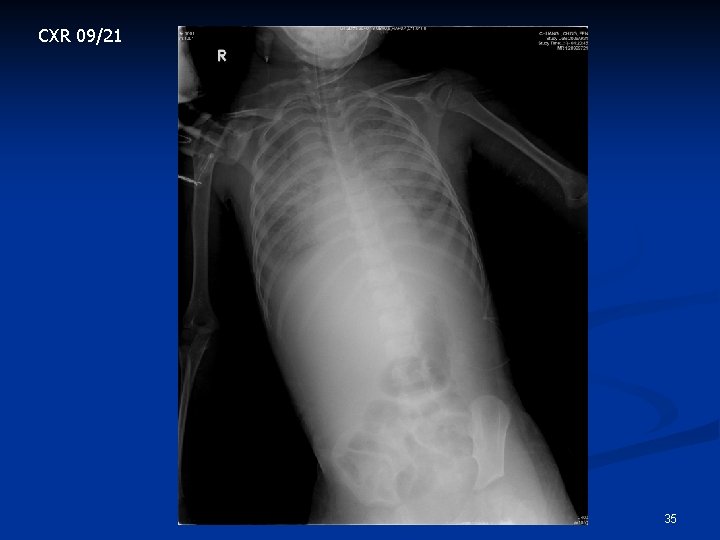
CXR 09/21 35
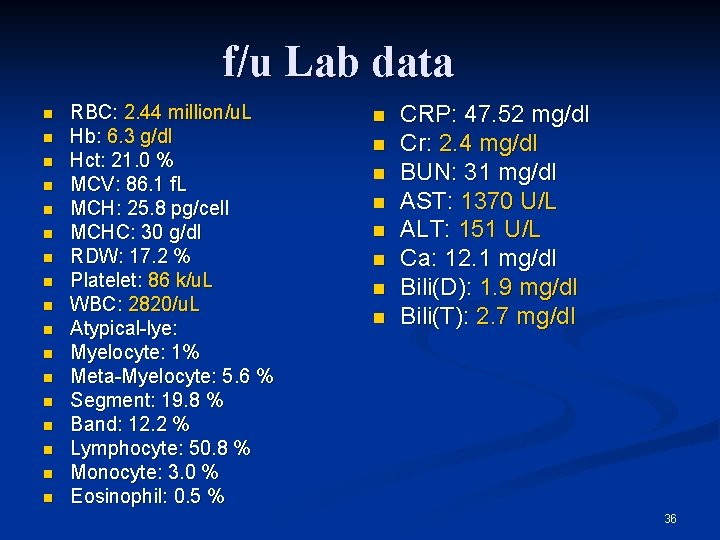

f/u Lab data n n n n n RBC: 2. 44 million/u. L Hb: 6. 3 g/dl Hct: 21. 0 % MCV: 86. 1 f. L MCH: 25. 8 pg/cell MCHC: 30 g/dl RDW: 17. 2 % Platelet: 86 k/u. L WBC: 2820/u. L Atypical-lye: Myelocyte: 1% Meta-Myelocyte: 5. 6 % Segment: 19. 8 % Band: 12. 2 % Lymphocyte: 50. 8 % Monocyte: 3. 0 % Eosinophil: 0. 5 % n n n n CRP: 47. 52 mg/dl Cr: 2. 4 mg/dl BUN: 31 mg/dl AST: 1370 U/L ALT: 151 U/L Ca: 12. 1 mg/dl Bili(D): 1. 9 mg/dl Bili(T): 2. 7 mg/dl 36

PICU course n 09/21 ( day 3 ) 03: 35 weak pulse, low BP n n n Jusomin HAES Dopamine line Bosmine line 09/21 ( day 3 ) 09: 20 Bradycardia, BP undectable n n CPCR Expire at 09: 50 37
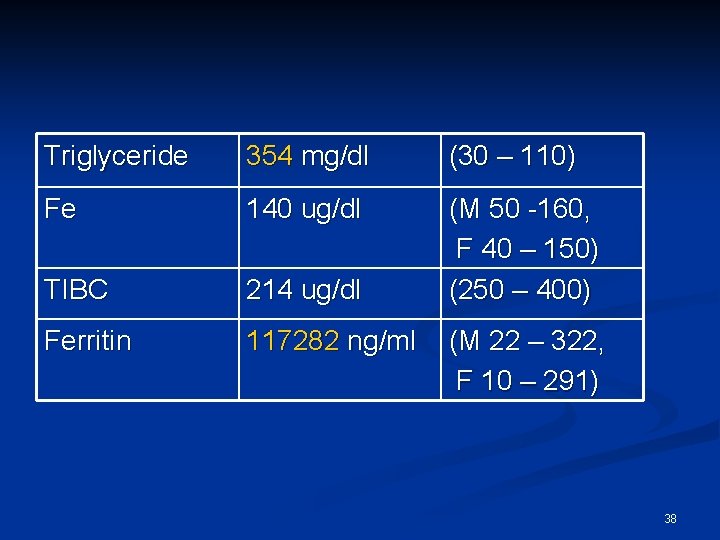
Triglyceride 354 mg/dl (30 – 110) Fe 140 ug/dl TIBC 214 ug/dl (M 50 -160, F 40 – 150) (250 – 400) Ferritin 117282 ng/ml (M 22 – 322, F 10 – 291) 38
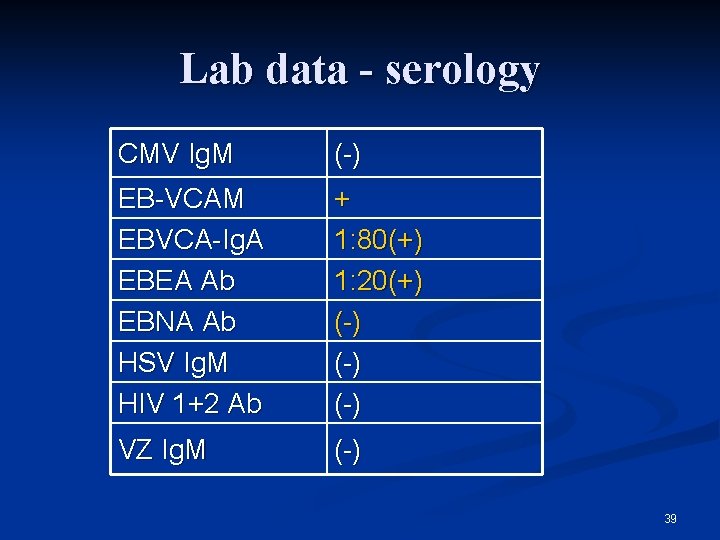
Lab data - serology CMV Ig. M (-) EB-VCAM EBVCA-Ig. A EBEA Ab EBNA Ab HSV Ig. M HIV 1+2 Ab + 1: 80(+) 1: 20(+) (-) (-) VZ Ig. M (-) 39

Blood smear n RBC: no specific change n WBC: Myelo 2% Meta-Myelo 16% Band 44% Seg 7% Lym 18% Aty-Lym 13% n Plt: ↓↓ Bone marrow n Histiocyte proliferation was definite, many showed phagocytosis of blood cells or debris Liver needle biopsy n Consistent with Epstein. Barr viral hepatitis 40

Hemophagocytic lymphohistiocytosis most often affects infants from birth to 18 months of age, but cases in older children and adults have been reported n Initial S/S of HLH are the same as, or mimic, common infections, fever of unknown origin, hepatitis, multiple organ failure syndrome, encephalitis, and even child abuse n 41

Hemophagocytic lymphohistiocytosis PATHOPHYSIOLOGY n HLH may be n familial associated with a number of different infections, autoimmune disorders, n coincident with malignancies n n n Cytokine dysfunction resulting in uncontrolled accumulation of activated Tlymphocytes and activated histiocytes (macrophages) in many organs. 42
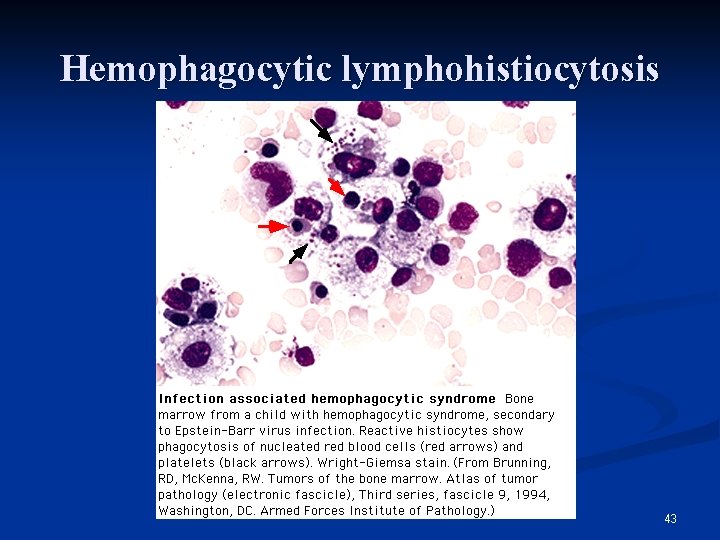
Hemophagocytic lymphohistiocytosis 43

Hemophagocytic lymphohistiocytosis n Treatment n referral to a pediatric hematology-oncology specialist is urgently to initiate immunochemotherapy steroids, immunoglobulin, or cyclosporine n HLH-94 protocol - induction therapy with dexamethasone and etoposide (VP-16), followed by continuous Tx with cyclosporine with pulses of dexamethasone and VP-16 n Hematopoietic cell transplantation — provide the best overall cure rate n 44

Final diagnosis VAHS ( viral-associated hemophagocytic syndrome ) n Virus induced hepatic failure n Pneumonia n 45

Key point Adequate survey and resuscitation in critical children n Pediatric patient with Fever/Cytopenia/MODS should be emphasized in n Infection n Bone marrow/hematology involvement n Consider ICU facility first ! n Consult specialists early if indicated n 46

Thank You ! Questions or comments ? 47
- Slides: 47