Pediatric Gastrointestinal Diseases By Dr Ashraf Radwan MD

Pediatric Gastrointestinal Diseases By Dr. Ashraf Radwan, MD Pediatric Department

Objectives By the end of the chapter the student will be able to: • Know the basic anatomy and physiology of gastrointestinal tract • Describe the etiology, pathophysiology, natural history, and presenting symptoms and signs of the common pediatric gastrointestinal problems. • Choose and interpret the appropriate laboratory and/or imaging studies in gastrointestinal disorders.

Objectives • Plan for initial management of gastrointestinal cases • Assess a patient presenting with gastroenteritis with or without dehydration, including the type and degree of dehydration, as well as any complicating conditions. • Select and calculate the appropriate fluid and electrolyte therapy (oral/IV).
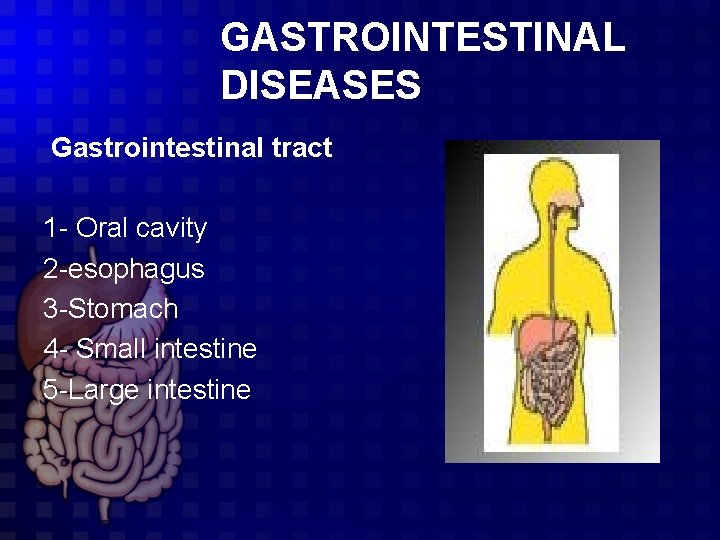
GASTROINTESTINAL DISEASES Gastrointestinal tract 1 - Oral cavity 2 -esophagus 3 -Stomach 4 - Small intestine 5 -Large intestine
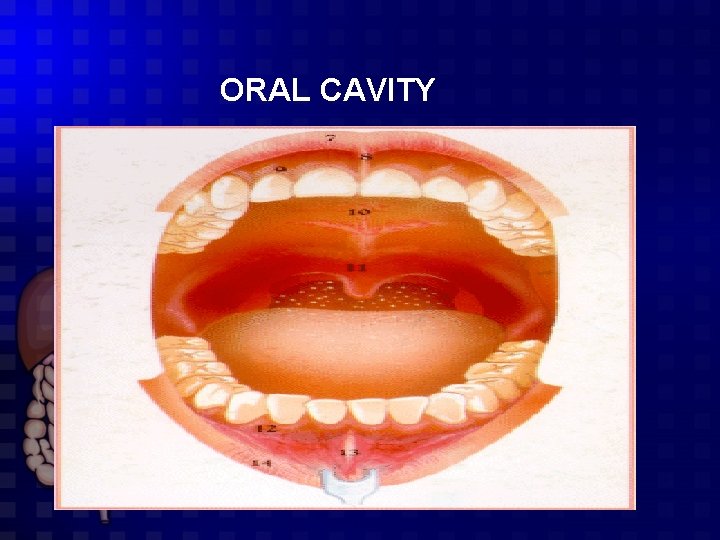
ORAL CAVITY
Functions of the Digestive System • Ingestion of food • Digestion of food into nutrient molecules • Absorption of these nutrient molecules • Eliminate of non digestible wastes
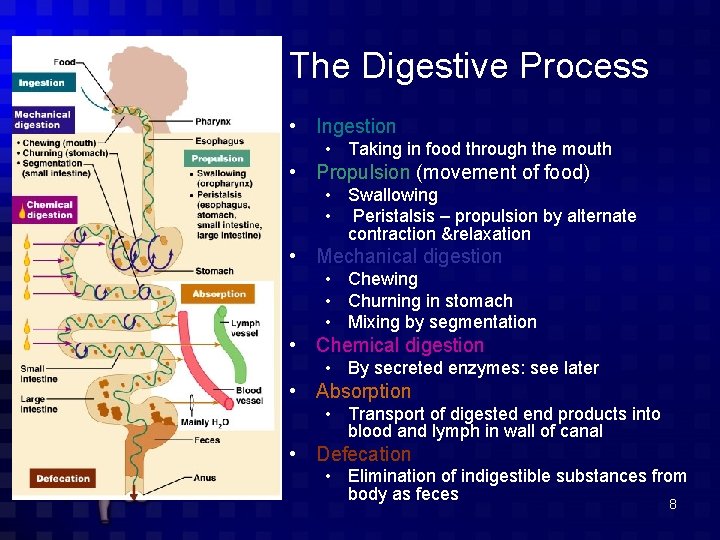
The Digestive Process • Ingestion • Taking in food through the mouth • Propulsion (movement of food) • Swallowing • Peristalsis – propulsion by alternate contraction &relaxation • Mechanical digestion • Chewing • Churning in stomach • Mixing by segmentation • Chemical digestion • By secreted enzymes: see later • Absorption • Transport of digested end products into blood and lymph in wall of canal • Defecation • Elimination of indigestible substances from body as feces 8

ACUTE STOMATITIS
STOMATITIS Definition Inflammation of the oral mucosa

STOMATITIS Causes I- Infections • Viral • Fungal II-Non infectious • Aphthous stomatitis • Trauma • Others
VIRAL STOMATITIS -Herpes simplex virus -Coxsackie viruses Others

HERPETIC STOMATITIS Clinical Manifestations Usually affects children 6 mo to 5 yr of age Symptoms Extremely painful condition with acute onset of - High grade Fever - Oral Pain -Excessive salivation - Refusal of feeding

HERPETIC STOMATITIS Signs 1 -Vesicles Throughout the oral cavity, on the gums, lips, tongue, palate, tonsils, and pharynx. 2 -Ulcers The vesicles progress to form shallow ulcers that may be covered with a yellow-gray membrane. The ulcers are usually multiple and small (1– 3 mm 3 - Cervical lymphadenopathy : submaxillary LN are enlarged &tender Course: self limited in 7 – 14 days
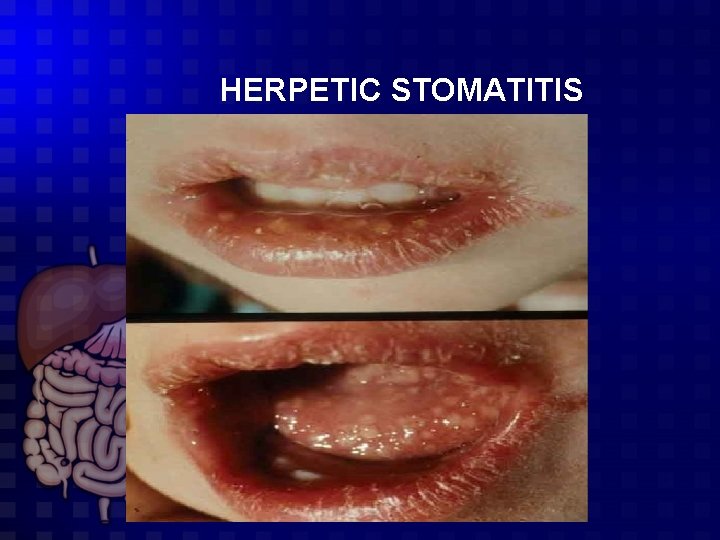
HERPETIC STOMATITIS
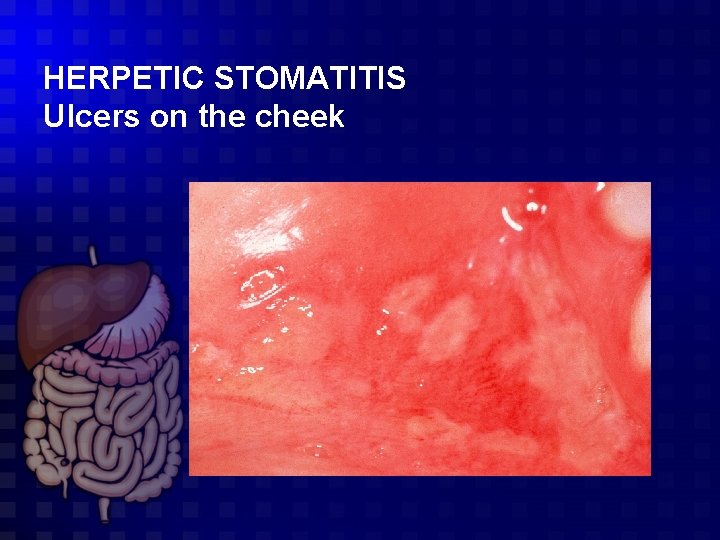
HERPETIC STOMATITIS Ulcers on the cheek

Treatment 1 -symptomatic a- Local and systemic analgesics B-Correction of dehydration c- Soft diet 2 - Antiviral In severe cases oral acyclovir suspension, 20 mg/kg per dose, four times daily for 5 days.
Hand, foot, and mouth disease Etiology Coxsackievirus

Hand, foot, and mouth disease Clinical manifestations usually begins with sore throat and low-grade fever Examinations reveals 1 -Small oral vesicles 2 - Swollen cervical lymph nodes. 3 -Lesions on the hands and feet small vesicles surrounded by a reddish halo. The patient may also develop a few of these vesicles on the fingers, toes, face, buttocks, and legs.
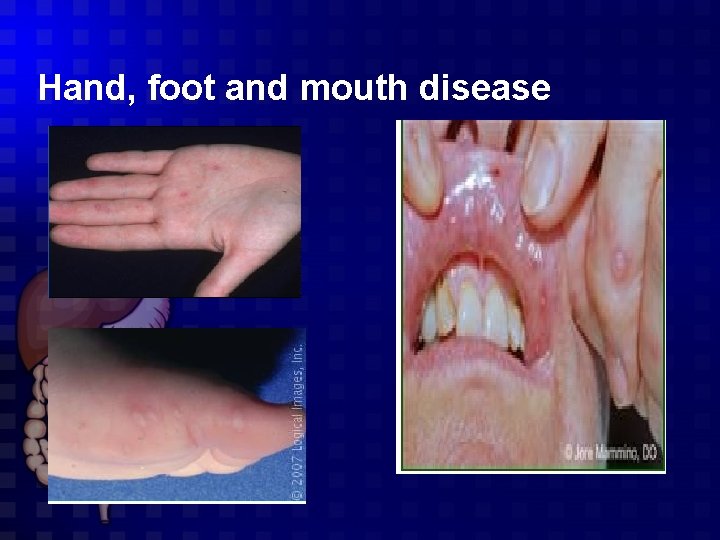
Hand, foot and mouth disease

Treatment The treatment is supportive, as follows • Ensure adequate fluid intake to prevent dehydration • Spicy or acidic substances may cause discomfort • Intravenous hydration may be necessary if the patient has moderate-to-severe dehydration • Fever may be treated with antipyretics • Pain may be treated with acetaminophen or ibuprofen • Direct analgesia may also be applied to the oral cavity via mouthwashes or sprays

Oropharyngeal candidiasis (Thrush) Etiology Candida albicans It is a saprophyte that normally not invasive. It becomes invasive in the presence of certain predisposing factors Oral candidiasis mainly affects newborns and occasionally debilitated infants and older children

Oropharyngeal candidiasis (Thrush) Predisposing factors 1 -Maternal genital infection 2 - Malnutrition 3 -Broad spectrum antibiotics 4 - Immunodeficiency
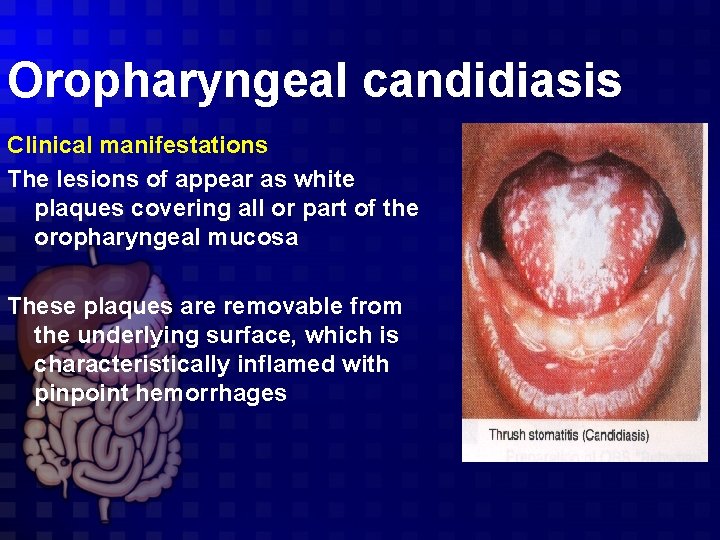
Oropharyngeal candidiasis Clinical manifestations The lesions of appear as white plaques covering all or part of the oropharyngeal mucosa These plaques are removable from the underlying surface, which is characteristically inflamed with pinpoint hemorrhages

Oral candidiasis Treatment I-Antifungal A- Local antifungal -Nystatin oral suspension. -Gentian violet Is effective, but it can severely stain clothing and skin. - Miconazole oral gel B- Systemic antifungal II- Replace any items, such as a pacifier, that may have become contaminated with Candida.
Aphthous Stomatitis Etiology The cause is unknown an allergic or autoimmune basis is suspected.
Aphthous Stomatitis Clinical manifestations 1 - Oral pain 2 - Oral ulcers -Small (3– 10 mm) -usually found on the inner aspect of the lips or on the tongue; rarely they may appear on the tonsils or palate. -last 1– 2 weeks- -Recurrent
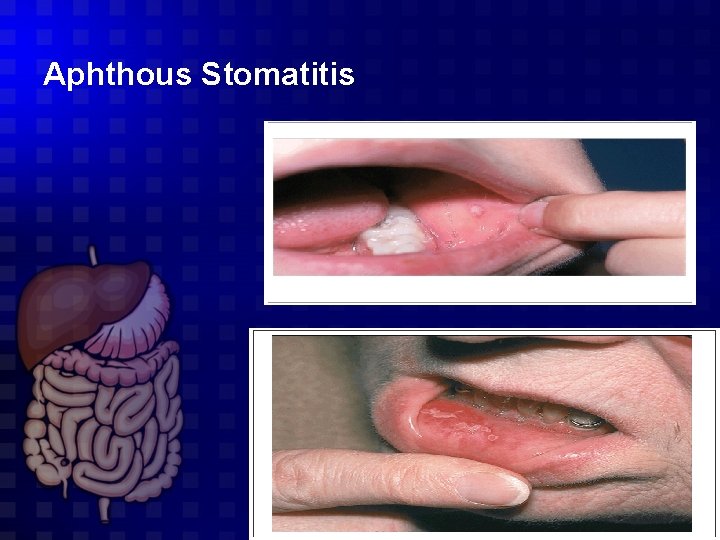
Aphthous Stomatitis
Aphthous Stomatitis Treatment 1 - Diet Eating soft diet, avoiding salty or acidic foods and juices 2 - Systemic analgesics Acetaminophen or ibuprofen. In the presence of oral pain 3 - Local analgesics
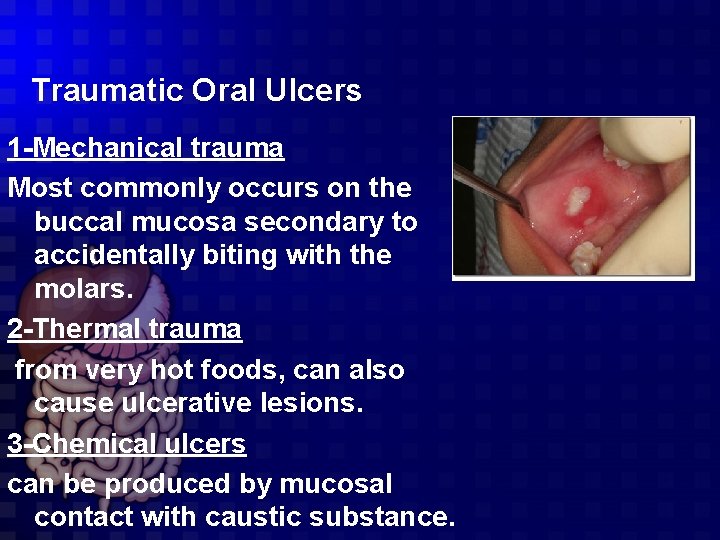
Traumatic Oral Ulcers 1 -Mechanical trauma Most commonly occurs on the buccal mucosa secondary to accidentally biting with the molars. 2 -Thermal trauma from very hot foods, can also cause ulcerative lesions. 3 -Chemical ulcers can be produced by mucosal contact with caustic substance.

VOMITING • Definitions • VOMITING • Forceful expulsion of gastric contents through the mouth. Vomiting is a highly coordinated reflex • RGURGITATION • Non forceful expulsion of foods or secretions from the esophagus or stomach through the mouth

Pathophysiology of Vomiting is a reflex process that begins with violent descent of the diaphragm and constriction of the abdominal muscles with relaxation of the gastric cardia actively forcing the gastric contents back up the esophagus. This process is coordinated in the medularly vomiting center, which is influenced directly by afferent innervations and indirectly by the chemoreceptor trigger zone and higher central nervous system centers.

Causes of vomiting I-Gastrointestinal 1 - Obstructive lesions A-ESOPHAGUS • Esophageal atresia • Esophageal stricture • Achalasia • Others B-STOMACH • Pyloric stenosis • Pyloric stricture • Others

C-SMALL INTESTINE • Duodenal atresia • Malrotation • Volvulus • Postsurgical adhesions • Intussusception • Others D-COLON • Meconium plug • Hirschsprung disease • Colonic atresia • Colonic stenosis • Imperforate anus

2 -Nonobstructive lesions This includes diseases of the upper bowel, pancreas, liver, or biliary tree • Gastritis • Gastroenteritis • Peptic ulcer • Gastroesophageal reflux • Others

II- Nongastrointestinal • Food poisoning • Increased intracranial pressure • Infection (urinary tract , Otitis media , Pertussis • Labyrinthitis • Medications (erythromycin, chemotherapy) • Adrenal insufficiency • Psychogenic • Others III- Cyclic vomiting

Complications of Vomiting 1 -Metabolic • Dehydration • Alkalosis 2 -Malnutrition 3 -Aspiration 4 -Shock

Treatment of Vomiting 1 -Treatment of the cause 2 -IV fluids 3 -Drugs May be needed in cyclic vomiting 4 - Treatment of complications

ESOPHEGEAL ATRESIA Esophageal atresia refers to a congenital anomaly characterized by lack of esophageal patency. One or more tracheoesophageal fistulae may be present between the malformed esophagus and the trachea. • Type A - Esophageal atresia without fistula • Type B - Esophageal atresia with proximal tracheoesophageal fistula • Type C - Esophageal atresia with distal tracheoesophageal fistula • Type D - Esophageal atresia with proximal and distal tracheoesophageal fistulae

Pathophysiology The lack of esophageal patency prevents normal feeding, and may cause infants to aspirate saliva and other secretions which quickly overflow the upper pouch of the obstructed esophagus. If a TEF is present, fluid or gastric secretions from below may flow directly into the tracheobronchial tree.

Clinical manifestations Immediately after delivery the neonate born with esophageal atresia have: 1 -Drooling (mucus and secretions) 2 - Choking If suckling at the breast or bottle is allowed, the baby appears to choke and may have significant respiratory distress. 3 -Vomiting : Repeated with every feed

Diagnosis • In addition to clinical manifestations the following may help in diagnosis • If an oral tube is placed into the esophagus it characteristically becomes blocked 10 -11 cm from the lips and can be confirmed with plain chest x ray • Imaging Esophagogram using water-soluble contrast material • Treatment 1 -Supportive measures • -Aspirations of secretions • - Maintenance of fluids 2 - Surgery It is an emergency
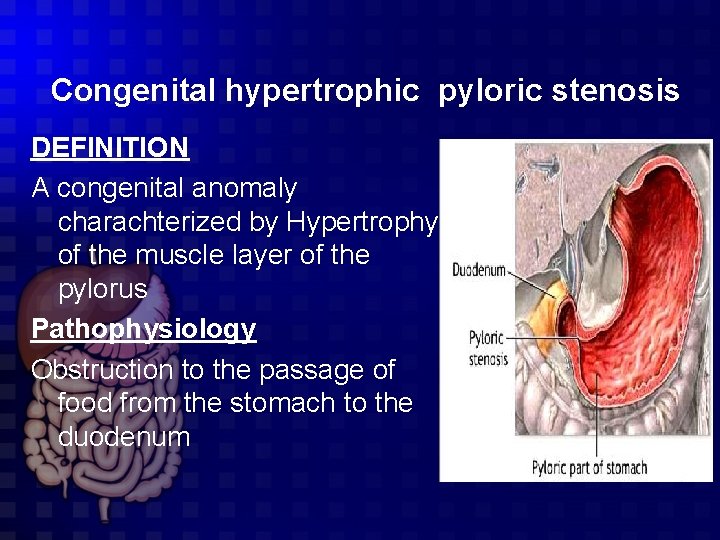
Congenital hypertrophic pyloric stenosis DEFINITION A congenital anomaly charachterized by Hypertrophy of the muscle layer of the pylorus Pathophysiology Obstruction to the passage of food from the stomach to the duodenum

Clinical manifestations 1 -Vomiting -Starts after 2 nd or 3 rd week of life - Projectile -Persistent -Occurs shortly after feeding -Contains only gastric content 2 - Other manifestations - Visible gastric Peristalsis - Pyloric mass - Constipation - Weight loss - Dehydration

Diagnosis 1 -Clinical Manifestations 2 -Immaging -Abdominal sonography -Barium meal a-Dilated stomach b-Narrow pyloric canal (string sign )
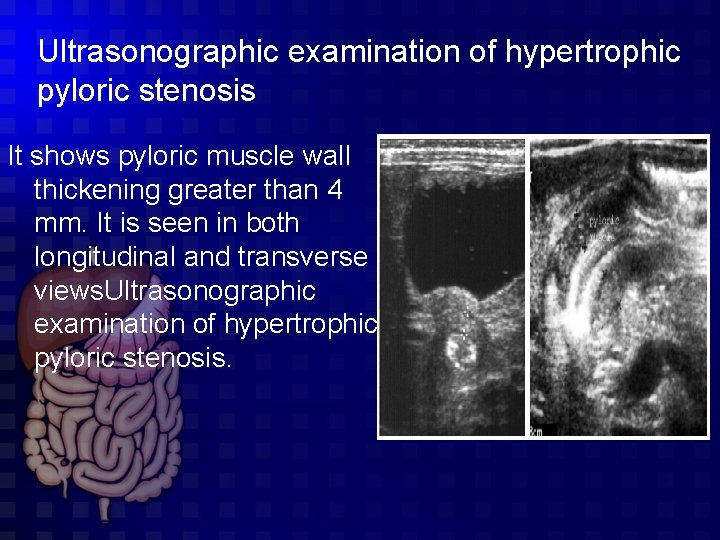
Ultrasonographic examination of hypertrophic pyloric stenosis It shows pyloric muscle wall thickening greater than 4 mm. It is seen in both longitudinal and transverse views. Ultrasonographic examination of hypertrophic pyloric stenosis.
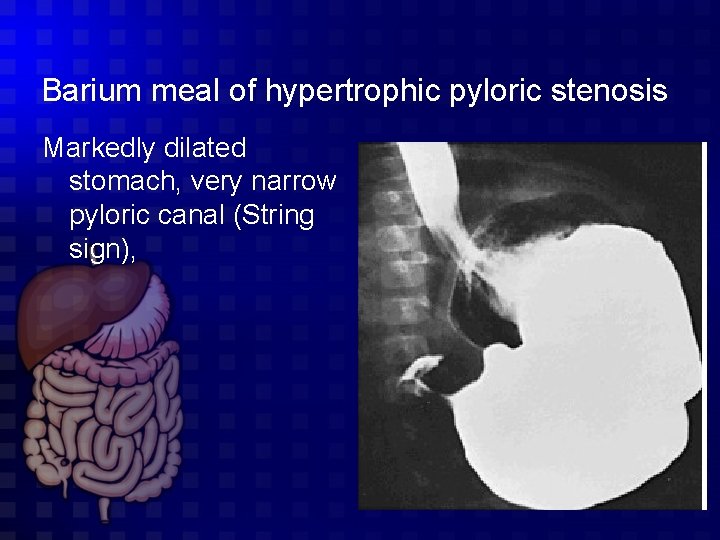
Barium meal of hypertrophic pyloric stenosis Markedly dilated stomach, very narrow pyloric canal (String sign),

Treatment 1 - Medical a-Correction of fluids loss, electrolytes and acid base balance b- Nutritional support 2 -Surgical Pylormyotomy, the undelying antro-pyloric mass is split leaving the mucosal layer intact.

Gastroesophageal reflux Definition It signifies the retrograde movement of gastric contents across the lower esophageal sphincter (LES) into the esophagus Types 1 - physiologic “spitting” regurgitation of normal infants. This is often a developmental process, and resolves with maturity 2 -pathologic (GERD) The episodes of regurgitations are more frequent or persistent, and may produce reflux related complications e. g. , Failure to thrive, esophagitis, esophageal stricture or chronic respiratory disease.

Physiologic regurgitation (Spitting) A normal phenomenon in most newborns - Since birth -Has no effect on growth -Normal bowl habits -Self limited

Gastroesophageal reflux disease Clinical manifestations Infantile GER reflux Usually manifests with 1 -regurgitation (especially postprandially) 2 -signs of esophagitis (irritability, sleep disturbance , choking, gagging) 3 -failure to thrive 4 -respiratory manifestations (obstructive apnea or as stridor ) symptoms resolve spontaneously in the majority by 12– 24 mo. 5 -Sandifer syndrome(posturing with opisthotonus or torticolis) •

GER in Older children Usually have 1 -Regurgitation during the preschool years 2 -Complaints of abdominal and chest pain during adolescence 3 -Airway manifestations frequently related to asthma , laryngitis or sinusitis.

Diagnosis For most of the typical GERD presentations, a thorough history and physical examination suffice to reach the diagnosis initially. Occasionally investigations may be needed this includes 1 -Contrast (usually barium) radiographic study of the esophagus and upper gastrointestinal tract 2 -Intra- esophageal p. H monitoring of the distal esophagus 3 -Endoscopy 4 -Laryngotracheobronchoscopy

Treatment Dietary measures 1 -normalization of feeding techniques, volumes, and frequency. 2 -Thickening of formula with a cereal results in fewer regurgitation episodes 3 -Pharmacotherapy Antacids Histamine-2 receptor antagonists (H 2 RAs) Proton pump inhibitors (PPIs) Prokinetic agents 3 -Avoidance of reflux-inducing foods (tomatoes, chocolate, mint) and beverages (juices, carbonated and caffeinated drinks, ). 4 -Weight reduction for obese patients

Cyclic vomiting A syndrome with numerous episodes of vomiting interspersed with well intervals. 1 -The onset is usually between 2 and 5 yr of age 2 -the frequency of vomiting is variable (average of 12 episodes per yr) 3 -each episode typically lasting 2– 3 days The cause is not exactly known Precipitants include infection, stress, and excitement Idiopathic cyclic vomiting may be a migraine equivalent or it may result from altered intestinal motility
Thank You
- Slides: 56