Pediatric emergency case conference Presented by R 3

Pediatric emergency case conference Presented by R 3 李智晃

General and triage information o o o o Chart No. : 7168 xx 9 Date of birth: 85/08/08 Gender: male Body weight: 35 kg Time on arrival: 2006/06/19 PM 16: 15 Vital signs: 36. 3/200/20, BP not measurable 家屬主訴心悸,外院表示tachycardia,建議轉診

Chief complaint and present illness o o C. C: palpitation since AM 10: 00 Present illness n n o Chest tightness and SOB was noted Activity: good No vomiting No cough, no fever Past history: n Similar episode last year

Physical examination o o o HEENT: no active lesion Heart: tachycardia without murmur Chest: clear breathing sound Abdomen: sort and flat Extremities: freely movable Immediate EKG monitoring: tachycardia up to 200/min

Was the patient ill? o PAT n n n Appearance- conscious clear, good activity Breathing- mild tachypnea Circulation- tachycardia, BP not measurable, strong peripheral pulsation, no cold or mottled skin
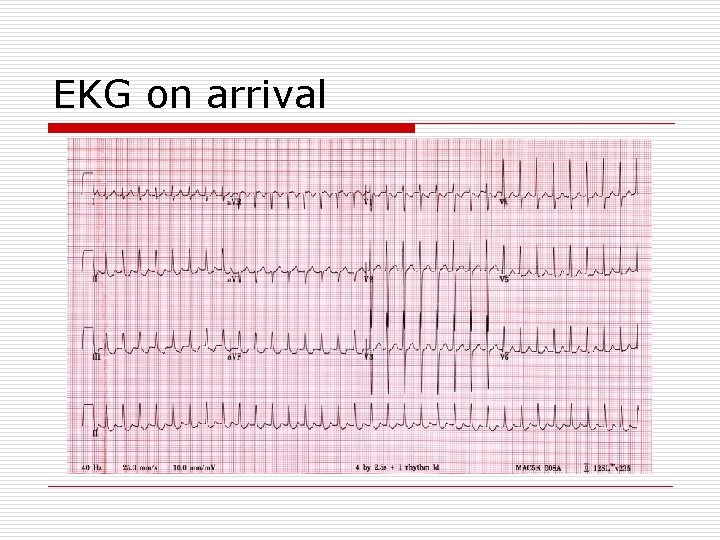
EKG on arrival

Initial management o o o Adenosine 3. 5 mg IV stat On 3 -way lock CBC/DC, CK-MB, Troponin-I, Ca, Na, K, BUN Admission to ward On EKG monitor
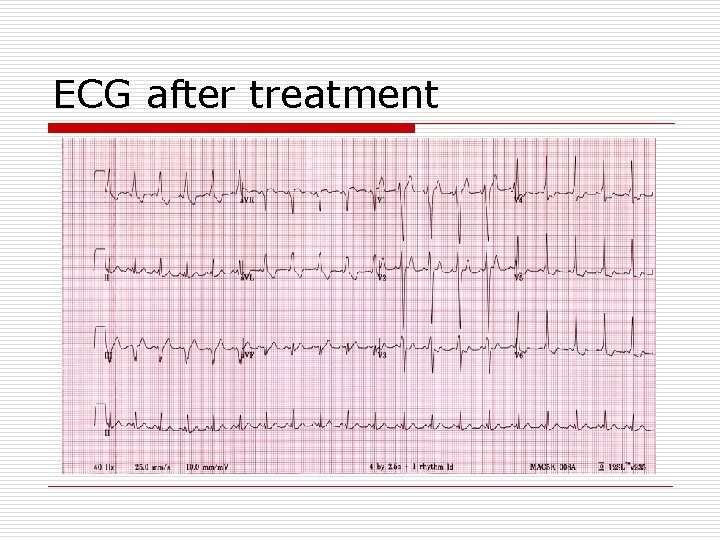
ECG after treatment

Final diagnosis o o Paroxysmal supraventricular tachycardia WPW syndrome

PSVT - Pathophysiology

Introduction and epidemiology o o Prevalence around 1/250 -1/25000 Most common form n n AVRT (including WPW syndrome) AVNRT

AV reentrant tachycardia (including WPW syndrome) o o o presence of an extranodal accessory pathway connecting the atrium and ventricle Antegrade vs. retrograde Antidromic vs. orthodromic
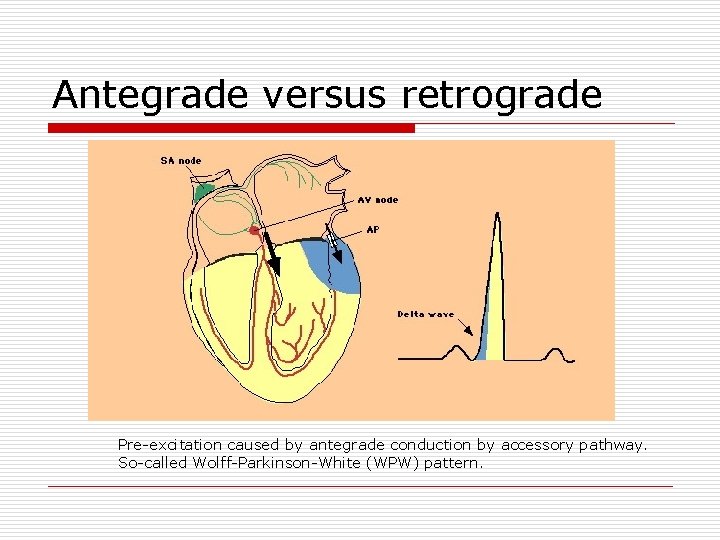
Antegrade versus retrograde Pre-excitation caused by antegrade conduction by accessory pathway. So-called Wolff-Parkinson-White (WPW) pattern.
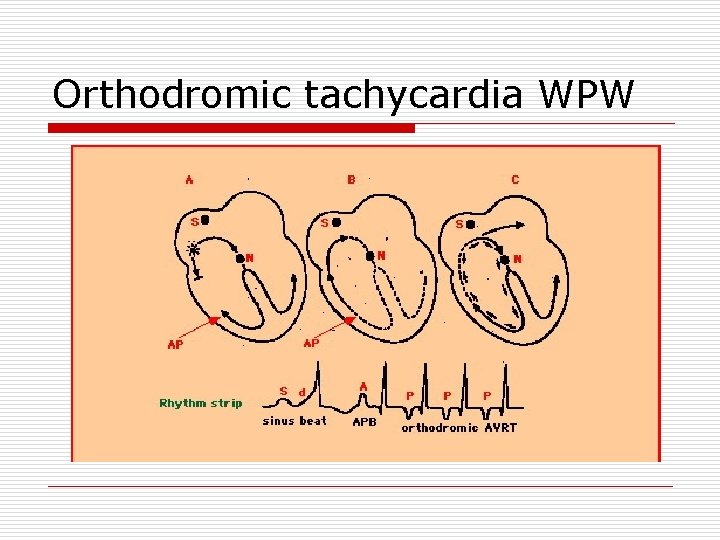
Orthodromic tachycardia WPW
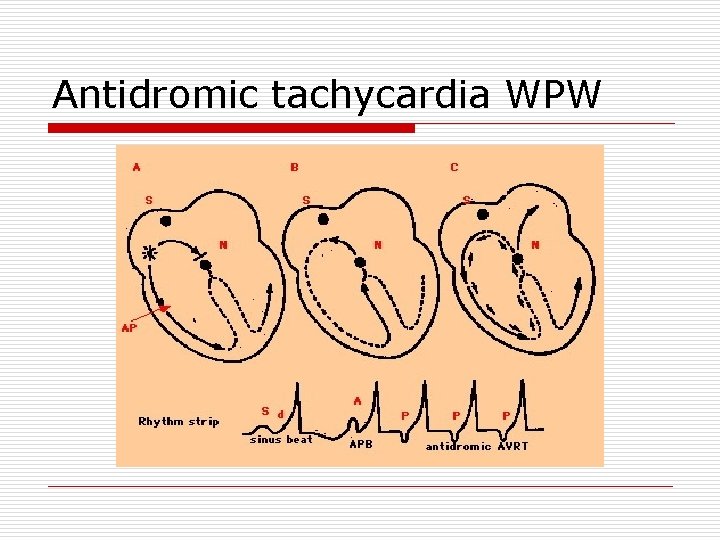
Antidromic tachycardia WPW
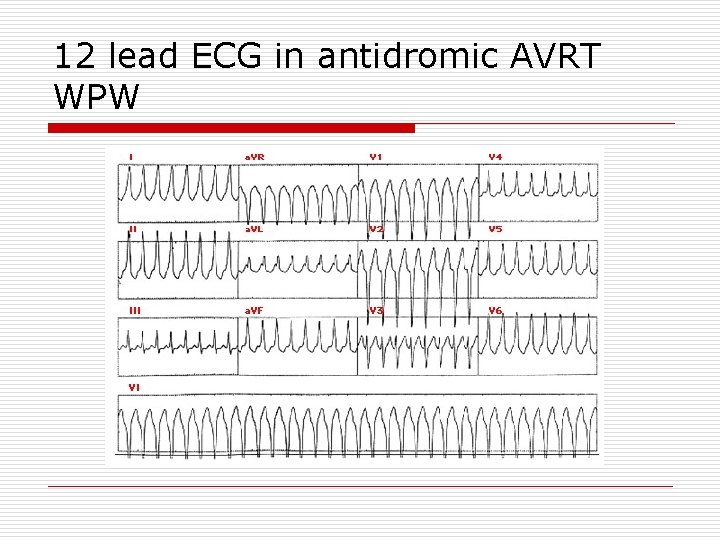
12 lead ECG in antidromic AVRT WPW

PSVT - management
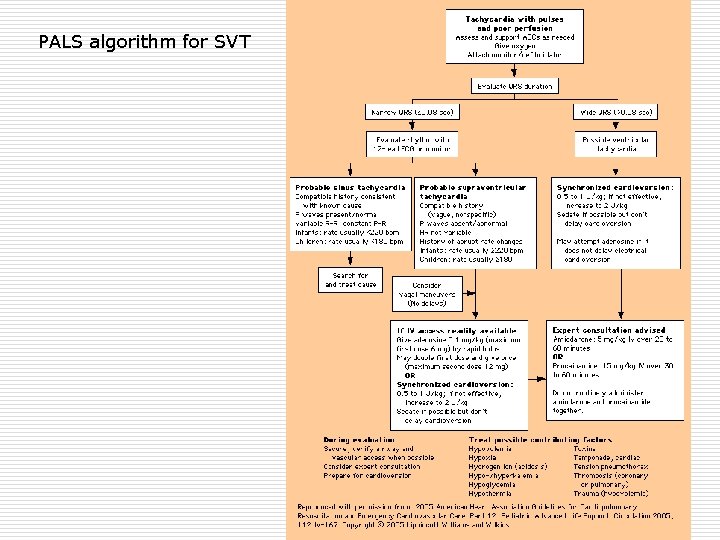
PALS algorithm for SVT

Hemodynamic assessment - PAT o o Appearance- pallor, or decreased level of consciousness Breathing- tachypnea, subcostal retraction, use of accessory muscle Circulation- hypotension, heart failure, signs of shock, . Signs in infants- irritability, tachypnea, and poor feeding.

Hemodynamic unstable o Cardioversion n Direct current cardioversion at 0. 5 to 2. 0 J/kg, synchronized Use pediatric electrode paddles (surface area 21 cm 2) Adequate sedation before the procedure

Diagnostic evaluation o o o History incompatible with sinus tachycardia P waves absent or abnormal Heart rate does not vary with activity The presence of abrupt changes in heart rate Rate usually >220 beats/min in infants and >180 beats/min in children

Vagal maneuvers o o ECG should be continuously monitored Infant and younger children n n o Older children n o Application of a bag filled with ice and cold water over the face for 15 to 30 seconds Rectal stimulation using a thermometer bearing down (Valsalva maneuver) for 15 to 20 seconds Carotid massage and orbital pressure should not be performed in children

Antiarrhythmic drugs o o Used while failure to convert the rhythm with vagal maneuvers Drugs of choice n n n Adenosine Verapamil Procainamide Amiodarone Digoxin was not suggested, especially under the suspicion of WPW syndrome

Adenosine o Mechanism n n n o Interact with A 1 receptor of cardiac muscle Delay of AV nodal conduction Block the re-entry cycle Dosage n n 0. 1 mg/kg, doubled if no response in 2 minutes 0. 05 mg/kg, increase by 0. 05 mg/kg every 2 minutes to total maximal dose of 0. 25 to 0. 35 mg/kg or total 12 mg is given

Verapamil o Mechanism n o Dosage n o to slow AV nodal conduction intravenous infusion in a dose of 0. 1 to 0. 3 mg/kg with a maximum dose of 10 mg Contraindications n n Infant less than one year old Children with heart failure Children suspected with WPW syndrome Children with wide QRS complex

Procainamide o o No IV form in CGMH Mechanism n o inhibiting phase 0 (sodium-dependent) depolarization and slows atrial conduction Dosage n n Loading dose o Infant- 7 to 10 mg/kg is given over 30 to 45 minutes o Oldr children- 15 mg/kg continuous infusion of procainamide starting at 40 to 50 mcg/kg per minute

Amiodarone o o Used for SVT refractory to other anti-arrhythmic agents Can be used safely in patient with WPW syndrome Mechanism n prolongs the refractory period of the AV node and the duration of the action potential and the refractory period of both atrial and ventricular myocardium Dosage n bolus infusion of 5 mg/kg over 20 to 60 minutes, repeated up to a total of 20 mg/kg n Continuous infusion of 10 to 15 mg/kg per day.

Chronic therapy o o ECG after acute episode should be performed to look for evidence of WPW syndrome Medications n o Digoxin Radiofrequency ablation

Reference o Up to date. Ver. 14. 2 n n o Supraventricular tachycardia in children: AV reentrant tachycardia (including WPW) and AV nodal reentrant tachycardia Management of supraventricular tachycardia in children Pediatric advanced life support (PALS), 2 nd edition
- Slides: 29