Pediatric Cervical Hodgkins Lymphoma Diagnosed by Ultrasoundguided Core

Pediatric Cervical Hodgkin’s Lymphoma Diagnosed by Ultrasoundguided Core Needle Biopsy A case report Chi-Maw Lin, MD Department of Otolaryngology, Head and Neck Surgery, National Taiwan University Hospital, Yunlin Branch 2017. 11. 02

Hodgkin’s lymphoma • The most common pediatric H&N malignancy (31% of total pediatric malignancies) • > 80% present with cervical lymphadenopathy • Traditionally, H&N lymphoma is diagnosed by open excisional biopsy. However, ultrasound-guided core needle biopsy (US-CNB) may also sample sufficient tissues for lymphoma diagnosis to prevent surgery

Case presentation • A 12 y/o boy with a right painless neck mass > 2 wks • PE revealed one fixed and firm cervical mass, measuring 6*3 cm, at right level IV cervical region • No history of fever, night sweats, or body weight loss • Blood work revealed an elevated white cell count (14, 480/m. L) with 79% segments and 13. 5% lymphocytes. Hb 11. 7 g/d. L, PLT 463, 000/m. L
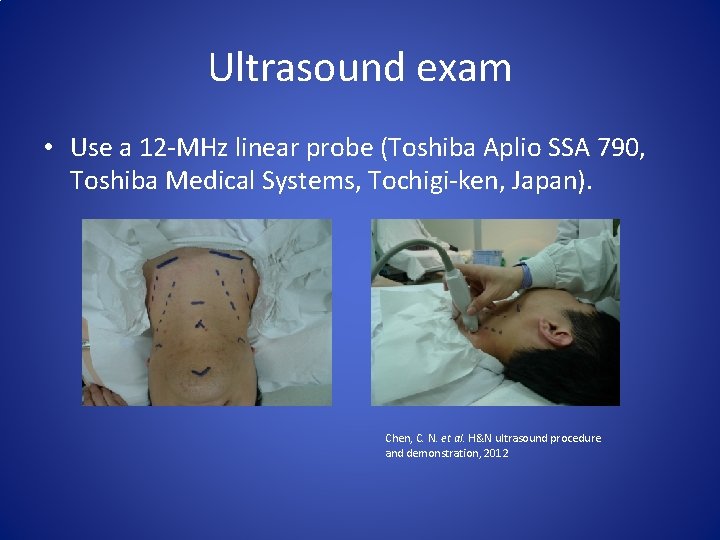
Ultrasound exam • Use a 12 -MHz linear probe (Toshiba Aplio SSA 790, Toshiba Medical Systems, Tochigi-ken, Japan). Chen, C. N. et al. H&N ultrasound procedure and demonstration, 2012
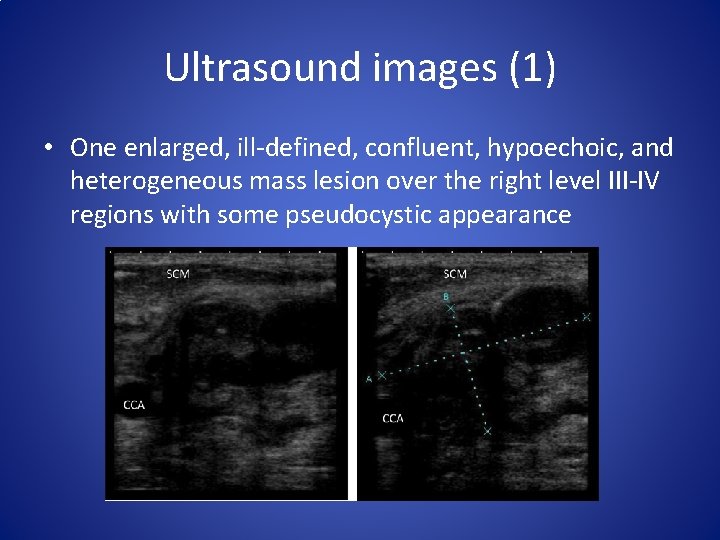
Ultrasound images (1) • One enlarged, ill-defined, confluent, hypoechoic, and heterogeneous mass lesion over the right level III-IV regions with some pseudocystic appearance
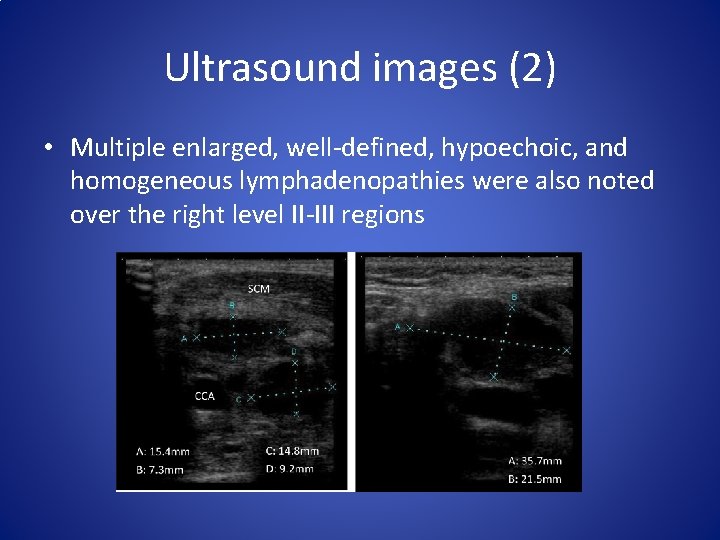
Ultrasound images (2) • Multiple enlarged, well-defined, hypoechoic, and homogeneous lymphadenopathies were also noted over the right level II-III regions
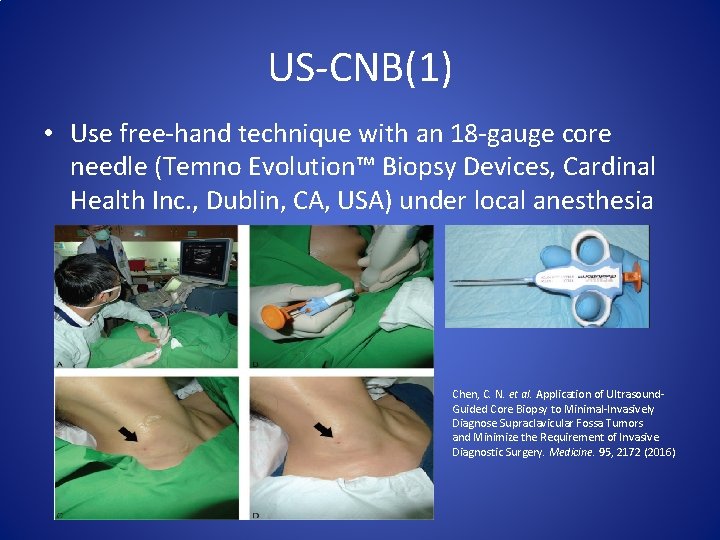
US-CNB(1) • Use free-hand technique with an 18 -gauge core needle (Temno Evolution™ Biopsy Devices, Cardinal Health Inc. , Dublin, CA, USA) under local anesthesia Chen, C. N. et al. Application of Ultrasound. Guided Core Biopsy to Minimal-Invasively Diagnose Supraclavicular Fossa Tumors and Minimize the Requirement of Invasive Diagnostic Surgery. Medicine. 95, 2172 (2016)
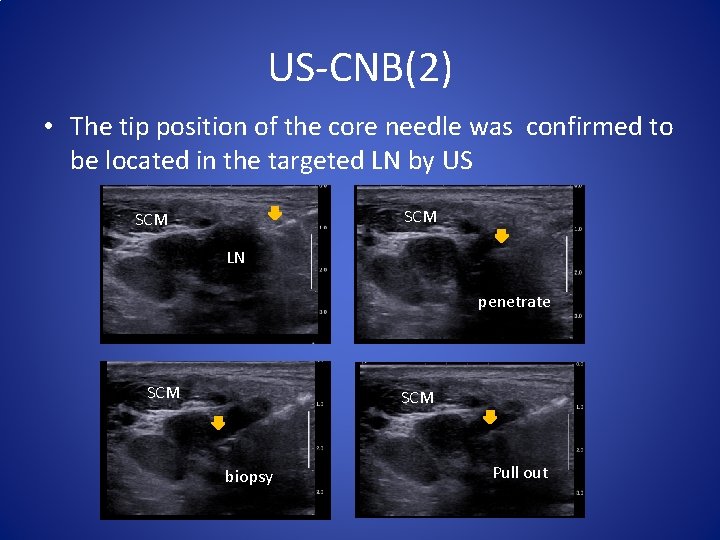
US-CNB(2) • The tip position of the core needle was confirmed to be located in the targeted LN by US SCM LN LN penetrate SCM biopsy Pull out
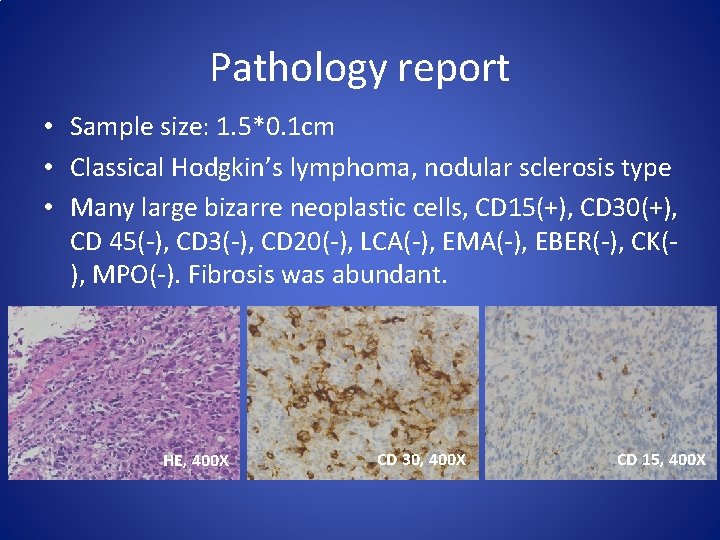
Pathology report • Sample size: 1. 5*0. 1 cm • Classical Hodgkin’s lymphoma, nodular sclerosis type • Many large bizarre neoplastic cells, CD 15(+), CD 30(+), CD 45(-), CD 3(-), CD 20(-), LCA(-), EMA(-), EBER(-), CK(), MPO(-). Fibrosis was abundant. HE, 400 X CD 30, 400 X CD 15, 400 X
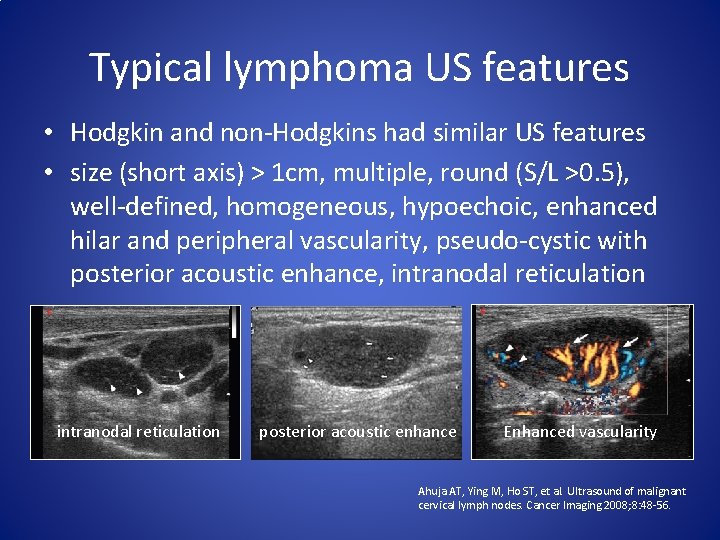
Typical lymphoma US features • Hodgkin and non-Hodgkins had similar US features • size (short axis) > 1 cm, multiple, round (S/L >0. 5), well-defined, homogeneous, hypoechoic, enhanced hilar and peripheral vascularity, pseudo-cystic with posterior acoustic enhance, intranodal reticulation posterior acoustic enhance Enhanced vascularity Ahuja AT, Ying M, Ho ST, et al. Ultrasound of malignant cervical lymph nodes. Cancer Imaging 2008; 8: 48 -56.
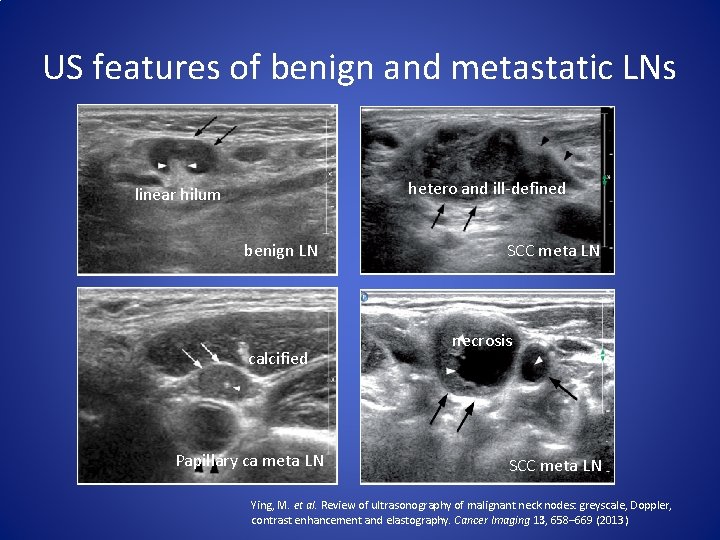
US features of benign and metastatic LNs hetero and ill-defined linear hilum benign LN calcified Papillary ca meta LN SCC meta LN necrosis SCC meta LN Ying, M. et al. Review of ultrasonography of malignant neck nodes: greyscale, Doppler, contrast enhancement and elastography. Cancer Imaging 13, 658– 669 (2013)
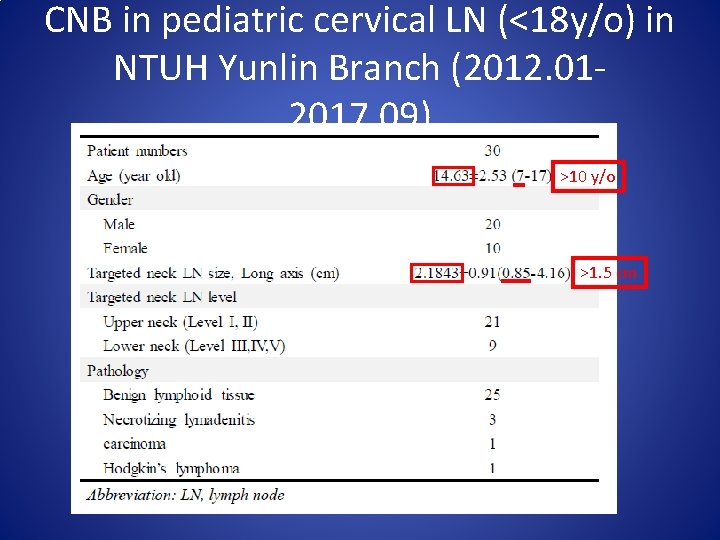
CNB in pediatric cervical LN (<18 y/o) in NTUH Yunlin Branch (2012. 012017. 09) >10 y/o >1. 5 cm

Advantages and ability of US-CNB • • Prevent surgical settings and risks FNA seldom give final diagnosis of lymphoma CNB could fully classify lymphoma in 38 -96% Burke et al. : 31/37 (84%) of diffuse large B-cell lymphoma conclusively diagnosed by CNB but only 8/16 (50%) of Hodgkin’s lymphoma

Disadvantages and risks of US-CNB • Harder to approach target LN than FNA – Difficult to perform CNB in small LN < 1 cm (long axis) – Harder to penetrate skin and subcutaneous tissue – Still need local anesthesia • If the patient is too young and incorporated (e. g. <10 y/o), CNB is hard to perform • Bleeding risk: minimal, if sparing great vessels • Tumor seeding risk: minimal

Conclusions • Though US-CNB cannot fully classify lymphoma, especially Hodgkin’s lymphoma, it is still an effective method giving us sufficient diagnosis information most of the time, and is an appropriate first-line method for the diagnosis of cervical LNs • Suitable candidates: – – Age > 10 y/o Cooperated Suspect malignancy, esp lymphoma Target LN size > 1. 5 cm

Thank you for your attentions
- Slides: 16