Pediatric Case Study By Sarah Iske Elliot Hospital

Pediatric Case Study By: Sarah Iske

Elliot Hospital • Elliot Health System (EHS) is the largest provider of comprehensive healthcare services in Southern New Hampshire. • Established in 1890, Elliot Hospital offers Southern New Hampshire communities caring, compassionate and professional patient service. • 296 -bed acute care facility located in Manchester.

Upon Admission… • Initial Screening Questions: • Have you lost weight in the past 3 -6 months? If yes, how much? • Has there been no nutritional intake for greater than five days? • Difficulty swallowing? • Non-healing wound or pressure sore? • Admitted on nutrition support (TF/TPN)? • Malnutrition Universal Screening Tool (MUST) Score: • BMI >20 = score 0, 18. 5 -20 = score 1, <18. 5= score 2

Elliot Registered Dietitians • Prioritize all new patients • Perform an initial assessment • • Estimate nutrition requirements Determine level of care Create nutrition diagnosis statements Determine nutrition status Determine goal of therapy Create intervention Monitor and evaluate • Re-evaluate every 1 -7 days • Provide nutrition educations • Coordinate care with medical staff and attend rounds/pre-rounds

Initial Screening • Initial Screening Questions: • Have you lost weight in the past 3 -6 months? If yes, how much? NO • Has there been no nutritional intake for greater than five days? NO • Difficulty swallowing? aspiration precaution • Non-healing wound or pressure sore? NO • Admitted on nutrition support (TF/TPN)? YES
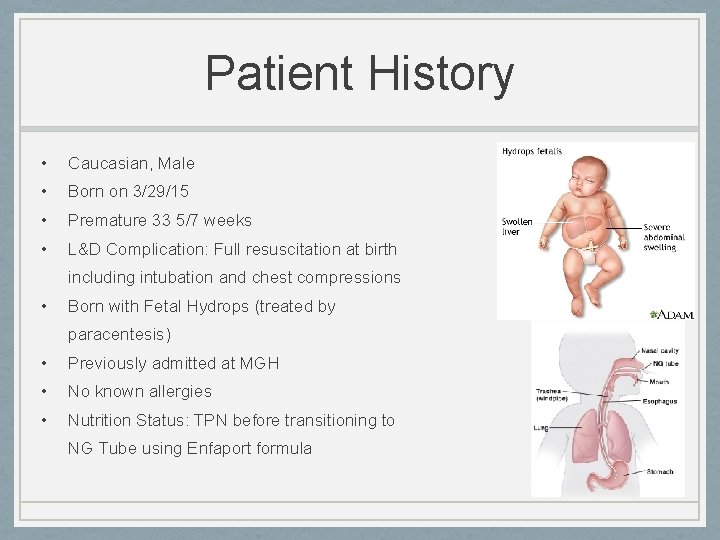
Patient History • Caucasian, Male • Born on 3/29/15 • Premature 33 5/7 weeks • L&D Complication: Full resuscitation at birth including intubation and chest compressions • Born with Fetal Hydrops (treated by paracentesis) • Previously admitted at MGH • No known allergies • Nutrition Status: TPN before transitioning to NG Tube using Enfaport formula

Social History • Lives with parents and 4 year old sister • Apartment is not baby safe • Planning to move to a new apartment • Family doesn’t have a car • Medical team concerned about Mom-infant bond

Anthropometrics from Medical Chart • Birth Weight: 3. 2 kg • Length since admission: 52 – 59 cm • Weight since admission: 4. 87 – 6. 38 kgs • BMI: 18. 33 kg/m 2

Elliot Problem List 1. Chylothorax/Chylous Ascites • d/t Noonan’s Syndrome? 2. Hypogammaglobulinemia 3. Hypercoagulability 4. Chronic Lung Disease (CLD) 5. Iatrogenic Drug Withdrawl
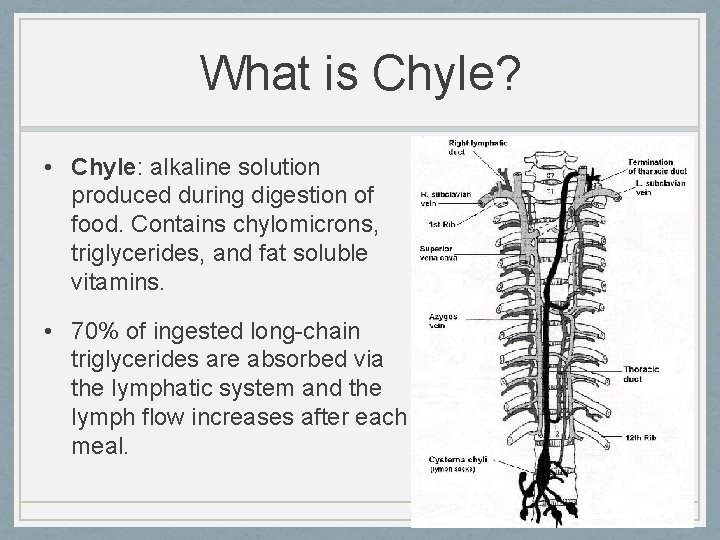
What is Chyle? • Chyle: alkaline solution produced during digestion of food. Contains chylomicrons, triglycerides, and fat soluble vitamins. • 70% of ingested long-chain triglycerides are absorbed via the lymphatic system and the lymph flow increases after each meal.
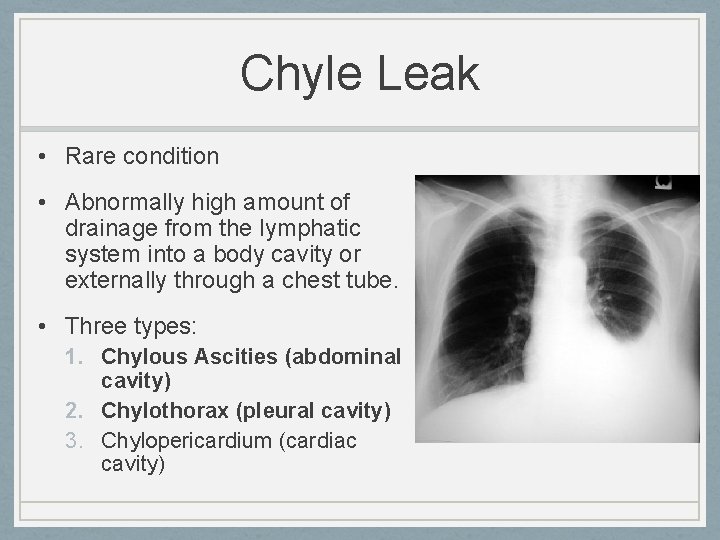
Chyle Leak • Rare condition • Abnormally high amount of drainage from the lymphatic system into a body cavity or externally through a chest tube. • Three types: 1. Chylous Ascities (abdominal cavity) 2. Chylothorax (pleural cavity) 3. Chylopericardium (cardiac cavity)

Causes of Chyle Leaks • Select malignancies (60%) • Lymphoma • Mediastinal lymph node metastasis • Carcinomas (gastric, ovarian, colon) • Trauma (25%) • Congenital abnormalities • Cirrhosis • Diagnosis confirmed by lab assessment: • Lipid content of the leak is greater than the lipid content of plasma. • Protein content of the leak is 50%+ greater than the protein content of plasma.

Complications of Chyle Leaks • Symptoms: dyspnea, tachypnea, cough, chest pain, abdominal distention. • Malnutrition • Depletion of nutrients (fat, protein, fat soluble vitamins, albumin, lymphocytes) • Increased risk for immunosuppression with potential risk for pneumonia and sepsis. • Hypovolemia (2. 5 L losses/day) • Metabolic acidosis • Electrolyte imbalance (hypernatremia, hypocalcemia) • Hemodynamic instability

Treatment of Chyle Leaks • Surgical Treatment • Swift closure • Medical Treatment: • Goal = spontaneous closure • Paracentesis • Reducing the amount of chyle (diuresis with a fat-modified enteral diet) • Treating the underlying cause • Nutrition support • Goal: decrease production of chyle, replace fluid and electrolytes, and maintain or replete nutrition status

Nutritional Management Two Options: 1. Enteral Nutrition/Oral Nutrition • Very low fat or fat free elemental formula/diet • 2 -5% of energy from essential fatty acids to prevent deficiency • <10 g of LCT a day • Multivitamin/Mineral supplement • High Protein (fat free protein supplement) • MCT oil supplementation 2. NPO with Parenteral Nutrition • Attempt EN or Oral feedings first • Only if unable to use gut, intolerance to oral or EN feeds, or failure of EN or oral diet to close chyle leak.
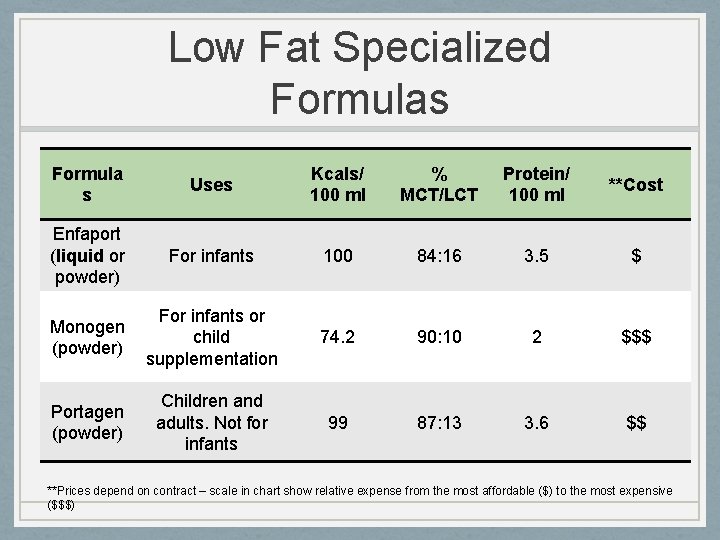
Low Fat Specialized Formulas Formula s Uses Kcals/ 100 ml % MCT/LCT Protein/ 100 ml **Cost Enfaport (liquid or powder) For infants 100 84: 16 3. 5 $ Monogen (powder) For infants or child supplementation 74. 2 90: 10 2 $$$ Portagen (powder) Children and adults. Not for infants 99 87: 13 3. 6 $$ **Prices depend on contract – scale in chart show relative expense from the most affordable ($) to the most expensive ($$$)
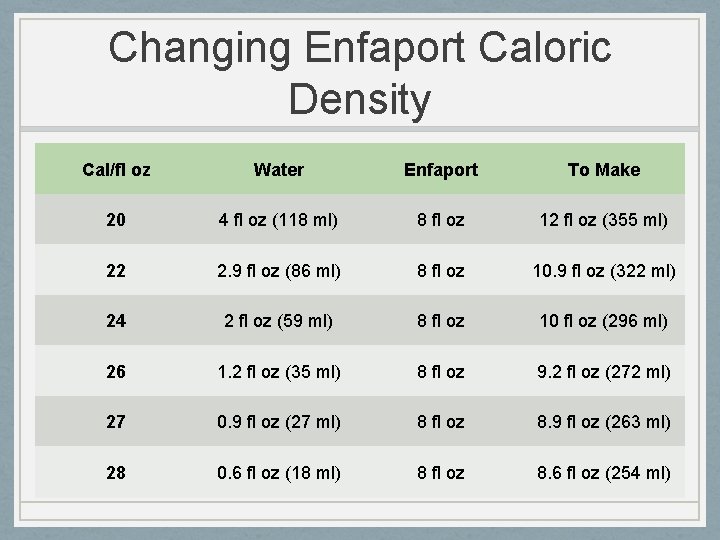
Changing Enfaport Caloric Density Cal/fl oz Water Enfaport To Make 20 4 fl oz (118 ml) 8 fl oz 12 fl oz (355 ml) 22 2. 9 fl oz (86 ml) 8 fl oz 10. 9 fl oz (322 ml) 24 2 fl oz (59 ml) 8 fl oz 10 fl oz (296 ml) 26 1. 2 fl oz (35 ml) 8 fl oz 9. 2 fl oz (272 ml) 27 0. 9 fl oz (27 ml) 8 fl oz 8. 9 fl oz (263 ml) 28 0. 6 fl oz (18 ml) 8 fl oz 8. 6 fl oz (254 ml)

Noonan’s Syndrome (Also called Turner Syndrome) • An autosomal dominant congenital disorder that affects both males and females • Mutations in the PTPN 11, SOS 1, RAF 1, KRAS, NRAS and BRAF genes that provide instructions for making proteins. • Characterized by: mildly unusual facial characteristics, short stature, heart defects, blood clotting problems, skeletal malformations. • Affects 1 in 1, 000 to 2, 500 people • Testing: Molecular genetic tests (or gene tests) that study single genes or short lengths of DNA to identify variations or mutations that lead to a genetic disorder. • Patients results were inconclusive. • Nutrition Management: No specific nutrition management. • Treatment: Based on individual signs and symptoms. Any cardiac or respiratory treatment is similar to treatment in general population.

Hypercoagulability • Increased risk for blood clots developing in the arteries and veins. • In most cases, treatment is only needed when a blood clot develops in a vein or artery. • Anticoagulants decrease the blood’s ability to clot and prevent the formation of additional clots. • Warfarin (Coumadin) • Heparin (IV or subcutaneous) • Fondaparinux (Arixtra)

Secondary to Chylothorax/Fetal Hydrops: Hypogammaglobulinemia • A deficiency of gamma globulins and especially antibodies in the blood causing immunosuppression. • Other causes: medications, nephrotic syndrome, intestinal lymphangiectasia, B-cell lineage malignancies, severe burns, and dystrophic myotonia. • Normal ranges for Ig. G are 176 - 601 mg/d. L for 2 -3 month old baby • Treated with replacement therapy of immunoglobulin G (Ig. G) through IVIG or SCIG

Chronic Lung Disease (CLD) • A general term for long-term respiratory problems in premature babies. The lungs of newborn babies are fragile and are easily damaged. Injury causes inflammation and scarring leading to breathing difficulties. • Causes: 1. Prematurity 2. Low amounts of surfactant 3. Oxygen use 4. Mechanical ventilation 5. Maternal womb infection 6. A family history of asthma 7. Development of an infection during or shortly after birth • Symptoms: • Respiratory distress (rapid breathing, flaring of the nostrils, grunting, chest retractions) • Continued need for mechanical ventilation or oxygen after a premature baby reaches 36 weeks gestation • Treatment: • Oxygen • Mechanical ventilation • Surfactant replacement • Medications: Bronchodilators, Steroids, Diuretics, Antibiotics • Nutrition for proper growth
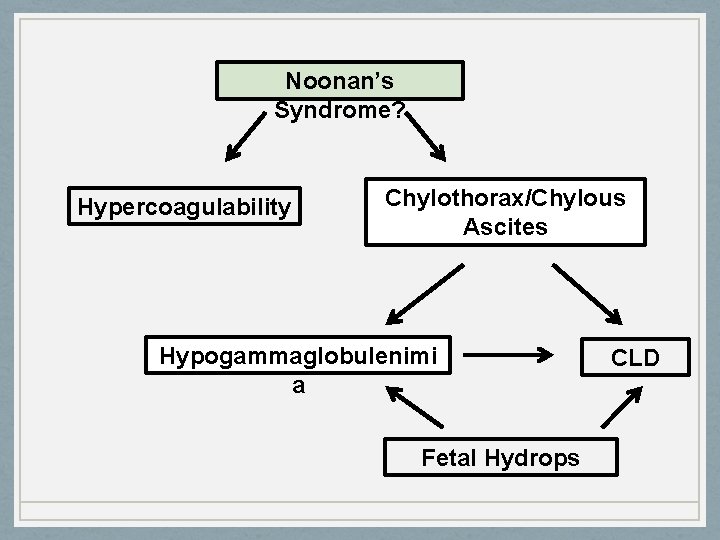
Noonan’s Syndrome? Hypercoagulability Chylothorax/Chylous Ascites Hypogammaglobulenimi a Fetal Hydrops CLD
Patient Admission 6/5 • Admitted to NICU • Weight: 4. 87 kgs • Current Problems: CLD, Chylothorax/chylous ascities, hypercoagulability, hypogammaglobulinemia, possible Noonan’s Syndrome. • On NCPAP for CLD • Chylothorax/Chylous Ascites – resolving on current diet • Continue Enfaport 26 cal/oz TF regimen 135 -140 ml/kg/day • No PO allowed d/t respiratory status • IVC/RA junction clot (hypercoagulability) • NAS scoring system for drug withdrawl • Practicing comfort measures: supportive positioning, pacifier, and sucrose per unit policy.
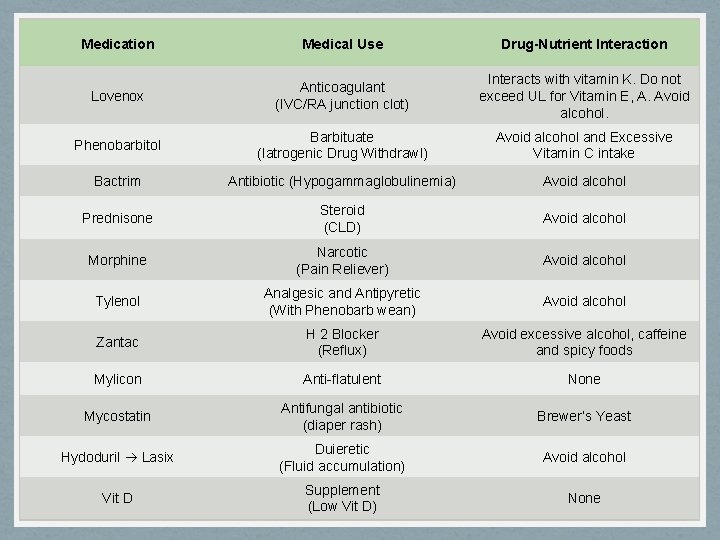
Medication Medical Use Drug-Nutrient Interaction Lovenox Anticoagulant (IVC/RA junction clot) Interacts with vitamin K. Do not exceed UL for Vitamin E, A. Avoid alcohol. Phenobarbitol Barbituate (Iatrogenic Drug Withdrawl) Avoid alcohol and Excessive Vitamin C intake Bactrim Antibiotic (Hypogammaglobulinemia) Avoid alcohol Prednisone Steroid (CLD) Avoid alcohol Morphine Narcotic (Pain Reliever) Avoid alcohol Tylenol Analgesic and Antipyretic (With Phenobarb wean) Avoid alcohol Zantac H 2 Blocker (Reflux) Avoid excessive alcohol, caffeine and spicy foods Mylicon Anti-flatulent None Mycostatin Antifungal antibiotic (diaper rash) Brewer’s Yeast Hydoduril Lasix Duieretic (Fluid accumulation) Avoid alcohol Vit D Supplement (Low Vit D) None

Initial NICU Nutrition Assessment 6/9 • Weight: 5. 225 kgs • Diet: NPO • Nutrition Support: NG tube of Enfaport 24 cal/oz @ 135 ml/kg over 1 hr via pump. Decreased from 26 • cals/oz d/t large weight gain. Vit D labs requested. Abnormal at 18 ng/ml – added 400 IU Vit D • Estimated Nutrition Needs: • Energy: 110 – 120 kcal/kg for corrected to term/post term based on estimated enteral needs. • Protein: 3 -4 gm for corrected to term/recovery needs based on estimated enteral needs. • Yield of current TF: 135 mls/kg provides 564 kcals/day, 108 kcals/kg and 3. 5 gm protein/kg/day. • Nutrition Diagnosis: • Altered GI function related to chylothorax evidenced by need for specialized low chain fatty acid formula • (Enfaport) Delayed/impaired oral feeding related to hx of prematurity and extensive medical/respiratory support as evidenced by NPO status/full TF dependence at this time. • No Malnutrition Identified • Goal of Therapy: • Promote ~0. 025 -0. 035 kgs/day weight gain • Promote proportionate growth velocity • Check TF daily and Reassess in 7 days • Labs: Glucose 96, BUN 16, Creat 0. 4, Na 134, K 3. 3

Enfaport Formula Calculation Nutrition Support: NG tube of Enfaport 24 cal/oz @ 135 ml/kg over 1 hr via pump. • Energy Requirements: 110 – 120 kcal/kg and 3 -4 gm protein • Weight: 5. 225 kg • 24 cals/oz x 30 ml/oz = 720 mls/ 5. 225 kg = 137. 7 ml/kg • 135 ml/kg x 5. 225 kg = ~705 ml • 705 ml/ 30 ml/oz = 23. 5 ounces x 24 cals/oz = 564 kcals • 564 kcals / 5. 2 kg = 108 kcals/kg • 705 mls x 0. 026 gm protein/ml = 18. 33 gms protein • 18. 33 grams protein/ 5. 2 kg = 3. 5 gm protein/kg • Yield of current TF: 135 mls/kg provides 564 kcals/day, 108 kcals/kg and 3. 5 gm protein/kg/day.

Updates 6/10 -6/16 • Labs: Glucose 99, BUN 15, Creat 0. 2, Na 134, K 4. 3 • TF remains at 135 -140 ml/kg/day with Enfaport 24 cal/oz over 1 hr via pump and no PO intake • NAS score daily • Plan for gradual wean off phenobarbitol • Weights checked daily – 0. 395 kg weight increase • Stooling well for age • Prednisolone for respiratory issues d/c’ed
Nurtition Re-Eval 6/16 • Weight: 5. 62 kgs • Diet: NPO • Nutrition Support: NG tube of Enfaport 22 cal/oz @ 130 ml/kg over 1 hr via pump. Decreased from 24 cals/oz d/t large weight gain. • Diuretic also adjust for weight gain and fluid accumulation may be source of weight gain. • Estimated Nutrition Needs: • Energy: 100 – 110 kcal/kg for corrected to term/post term based on estimated enteral needs. • Protein: 2. 2 -3 gm for corrected to term/recovery needs based on estimated enteral needs. • Yield of current TF: 130 mls/kg provides 535 kcals/day, 95 kcals/kg and 3. 4 gm protein/kg/day. • Nutrition Diagnosis: • Altered GI function related to chylothorax evidenced by need for specialized low chain fatty acid formula (Enfaport) • Delayed/impaired oral feeding related to hx of prematurity and extensive medical/respiratory support as evidenced by NPO status/full TF dependence at this time. • Check TF daily and Reassessment in 7 days

Updates 6/17 – 6/24 • Transferred to the PICU from NICU • On the TF with Enfaport but cleared by MD to trial PO intake. • Noticed increased WOB, nasal flaring, head bobbing • Plan to have SLP evaluate • Labs: Glucose 85, BUN 10, Creat 0. 14, Na 133, K 4. 3 • Multiple loose stools • Not weaning from respiratory support as expected • Hold PO when attempting to wean

SLP Evaluation • Noted immature suck of 4 -5 sucks and then a breathing break. • Tires quickly after 15 minutes and sucks decrease to 3 before breathing break. • Risk of aspiration is very high! • Plan: Allow PO feeds with slow flow nipple d/t no evidence of aspiration • Recommendations: SLP Therapy and Modified Barrium Swallow • Modified Barium Swallow findings: at very high risk for aspiration given issues with feedings, respiratory needs, and delay in developmental milestones.

Nutriton Re-Eval 6/24 • Weight: 5. 9 kgs • Diet: NPO • Nutrition Support: NG tube of Enfaport 22 cal/oz @ 130 ml/kg over 1 hr via pump. • If weight gain suboptimal, can increase TF to meet low end needs of 100 kcals/kg. • Promote ~ 20 -25 g/day weight gain • Estimated Nutrition Needs: • Energy: 100 – 110 kcal/kg for corrected to term/post term based on estimated enteral needs. • Protein: 2. 2 -3 gm for corrected to term/recovery needs based on estimated enteral needs. • Yield of current TF: 130 mls/kg provides 562 kcals/day, 95 kcals/kg and 3. 4 gm protein/kg/day. • Nutrition Diagnosis: • Altered GI function related to chylothorax evidenced by need for specialized low chain fatty acid formula (Enfaport) • Delayed/impaired oral feeding related to hx of prematurity and extensive medical/respiratory support as evidenced by NPO status/full TF dependence and SLP evaluation. • Check TF daily and Reassessment in 7 days • GI consultation planned today

GI Consultation • Aspiration will continue to worsen lung function and prevent alveolar growth • Possible PEG placement • Possible Nissen Fundoplication to protect airway • Plan to continue NG tube feeds and we reevaluate when closer to d/c and respiratory status improves
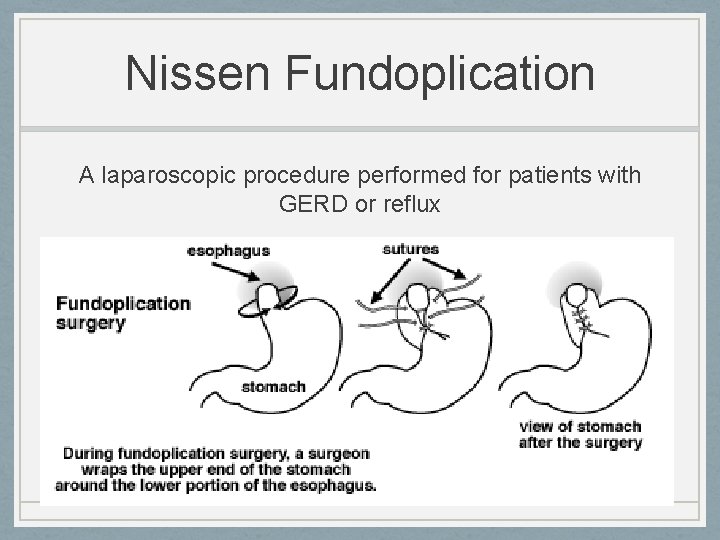
Nissen Fundoplication A laparoscopic procedure performed for patients with GERD or reflux

Updates 6/25 – 6/29 • Low weight gain – increased TF from 95 ml q 3 to 100 ml q 3 • Yield of Enteral Nutrition: 800 mls of Enfaport 22 kcals/ounce will yield 587 calories/day 98 kcals/kg and 20 grams protein/day. • 98% energy needs and 3. 3 gm Pro/kg/day • Multiple, loose stools • Had episode of 2 emesis after feeding • Patient discovered to have inguinal hernia – reduced by MDs. • Labs: Glucose 93, BUN 11, Creat 0. 31, Na 136, K 4. 4

Nutrition Re-Eval 6/30 • Weight: 6 kgs • Diet: NPO • Nutrition Support: NG tube of Enfaport 22 cal/oz @ 100 ml q 3 Estimated Nutrition Needs: • Energy: 100 – 110 kcal/kg for corrected to term/post term based on estimated enteral needs. • Protein: 2. 2 -3 gm for corrected to term/recovery needs based on estimated enteral needs. • Yield of Enteral Nutrition: 800 mls of Enfaport 22 kcals/ounce will yield 587 calories/day 98 kcals/kg and 20 grams protein/day or 3. 5 gm protein/kg. • Nutrition Diagnosis: • Altered GI function related to chylothorax evidenced by need for specialized low chain fatty acid formula (Enfaport) • Delayed/impaired oral feeding related to hx of prematurity and extensive medical/respiratory support as evidenced by NPO status/full TF dependence and SLP evaluation. • Check TF daily and Reassessment in 7 days

Updates 6/31 – 7/6 • Parents are more involved in patient care – learning how to use feeding pump. • Plan for hernia repair with PEG placement when respiratory status improves. • Of all options (NG, GT/fundo, G-J) chose G-J because feeds will be postpyloric and will protect airway. • Planned for 7/7 • Abnormal Lab 7/1: Ig. G 140 mg/d. L – given IVIG (last dose on 7/6) • Average ranges between 176 -601 for 2 -3 month old • Weaned off NC • Vomit x 2 (likely related to NGT position) • Poor weight gain: TF increased from 100 ml q 3 to 105 ml q 3 of Enfaport 22 kcals/ounce • Provides 840 mls , 616 calories/day and 22 grams protein

Nutrition Re-Eval 7/6 • Weight: 6. 195 kgs • Diet: NPO • • Estimated Nutrition Needs: • • Energy: 100 – 110 kcal/kg for corrected to term/post term based on estimated enteral needs. Protein: 2. 2 -3 gm for corrected to term/recovery needs based on estimated enteral needs. Yield of Enteral Nutrition: 840 mls of Enfaport 22 kcals/ounce will yield 616 calories/day 99 kcals/kg and 22 grams protein/day providing 99% of energy needs and 3. 5 gms protein/kg/day Nutrition Diagnosis: • • • Nutrition Support: NG tube of Enfaport 22 cal/oz @ 105 ml q 3 Altered GI function related to chylothorax evidenced by need for specialized low chain fatty acid formula (Enfaport) Delayed/impaired oral feeding related to hx of prematurity and extensive medical/respiratory support as evidenced by NPO status/full TF dependence and SLP evaluation. GJ tube placement and hernia repair planned for 7/8 • With J tube in place, switch to continuous feeds and consider goal rate of 35 ml/hr for 24 hrs to provide 840 ml, 616 kcals (99 kcals/kg current weight), 22 grams protein. • Once established, may wish to shorten TF rate to 20 hours daily (44 ml/hr) for more motility at home • Monitor and Evaluate: new feeding tube, TF restart, events/plans for surgery • Check TF daily and Reassessment in 2 -4 days
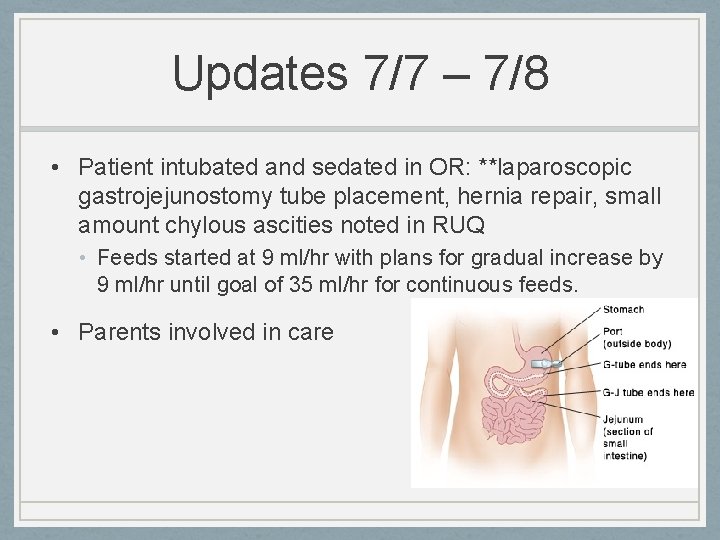
Updates 7/7 – 7/8 • Patient intubated and sedated in OR: **laparoscopic gastrojejunostomy tube placement, hernia repair, small amount chylous ascities noted in RUQ • Feeds started at 9 ml/hr with plans for gradual increase by 9 ml/hr until goal of 35 ml/hr for continuous feeds. • Parents involved in care

Nutrition Re-Eval 7/9 • Weight: 6. 38 kgs • Diet: NPO • Nutrition Support: GJ tube of Enfaport 22 cal/oz @ 35 ml/hr • Estimated Nutrition Needs: • Energy: 100 – 110 kcal/kg for corrected to term/post term based on estimated enteral needs. • Protein: 2. 2 -3 gm for corrected to term/recovery needs based on estimated enteral needs. • Yield of Enteral Nutrition: 840 mls of Enfaport 22 kcals/ounce will yield 616 calories/day 97 kcals/kg and 22 grams protein/day providing 97% of energy needs and 3. 4 gms protein/kg/day • Nutrition Diagnosis: • Altered GI function related to chylothorax evidenced by need for specialized low chain fatty acid formula (Enfaport) • Delayed/impaired oral feeding related to hx of prematurity and extensive medical/respiratory support as evidenced by NPO status/full TF dependence and SLP evaluation • Check TF daily and Reassessment in 2 -4 days
Updates 7/10 – 7/12 • Possible d/c on 7/13 • Home feeding equipment delivered • Officially weaned off phenobarbitol

Nutrition Re-Eval 7/12 • Weight: 6. 38 kgs • Diet: NPO • Nutrition Support: GJ tube of Enfaport 22 cal/oz @ 35 ml/hr • Estimated Nutrition Needs: • Energy: 100 – 110 kcal/kg for corrected to term/post term based on estimated enteral needs. • Protein: 2. 2 -3 gm for corrected to term/recovery needs based on estimated enteral needs. • Yield of Enteral Nutrition: 840 mls of Enfaport 22 kcals/ounce will yield 616 calories/day 97 kcals/kg and 22 grams protein/day providing 97% of energy needs and 3. 4 gms protein/kg/day • Nutrition Diagnosis: • Altered GI function related to chylothorax evidenced by need for specialized low chain fatty acid formula (Enfaport) • Delayed/impaired oral feeding related to hx of prematurity and extensive medical/respiratory support as evidenced by NPO status/full TF dependence nd SLP evaluation • Check TF daily and Reassessment in 2 -4 days • Monitoring and Evaluation: May want to measure head circumference prior to discharge and once well established, may wish to shorten TF to 20 hrs daily for 42 ml/hr for more mobility at home.

Updates 7/12 – 7/13 • G tube flushing, J tube not flushing • Attempted flushing with warm water • Cleared with warm water and cola • Parents received full training of formula prep and feeding tube/pump instructions. • Also given recipe for clearing clogged tube • Labs: Ig. G re-checked - at 281 mg/dl • Average ranges between 176 -601 for 2 -3 month old

Discharge Summary 7/13 • Active problems: CLD, hypercoagulability, hypogammaglobulinemia • Resolved problems: drug withdrawal, Chlythorax/Chylous ascites managed with Enfaport • Medications: Vit D, hydrodiuril, zantac, and bactrim • Outpatient Care: • Noonan’s Syndrome? F/U genetics testing at MGH • Plan for flow cytometry for Ig. G levels • Referrals for hematology, GI, pulmonary, cardiology

Questions? ?

References Sources: 1. Vogt, Annelie M. , and Rebecca Brody. "Nutritional Management of Chyle Leaks. " Support Line 31. 3. 2. http: //www. stanfordchildrens. org/en/topic/default? id=chronic-lung-disease-90 -P 02348 3. http: //www. uofmhealth. org/health-library/hw 179354 4. http: //emedicine. medscape. com/article/136471 -overview 5. http: //primaryimmune. org/about-primary-immunodeficiencies/specific-disease-types/transient-hypogammaglobulinemia-of-infancy/ ? ? 6. http: //www. ohsu. edu/xd/outreach/occyshn/training-education/upload/Infant-Pediatric-Formulas-Alisa-de-De. Weese. pdf 7. http: //www. merriam-webster. com/medical/hypogammaglobulinemia 8. http: //ghr. nlm. nih. gov/condition/noonan-syndrome 9. http: //www. ncbi. nlm. nih. gov/gtr/conditions/C 0028326/ 10. http: //my. clevelandclinic. org/services/heart/disorders/hypercoagstate 11. http: //costellosyndromeusa. org/2013 Resources/Tools%20 To%20 Help%20 Your%20 Childs%20 Nutrition%20 -%20 Karjoo%202013. pdf 12. http: //www. fodsupport. org/documents/Monogenarticle 6. 07. pdf 13. http: //www. nutricia. ie/products/view/monogen 14. http: //www. nlm. nih. gov/medlineplus/ency/article/003544. htm 15. http: //www. ext. colostate. edu/pubs/foodnut/09361. html 16. http: //www. nlm. nih. gov/medlineplus/druginfo/meds/a 682007. html 17. http: //edis. ifas. ufl. edu/pdffiles/HE/HE 77600. pdf 18. Mead Johnson Nutrition Pediatric Product handbook 19. https: //rarediseases. info. nih. gov/gard/10955/noonan-syndrome/resources/8 20. http: //www. nlm. nih. gov/medlineplus/ency/article/007308. htm 21. https: //my. clevelandclinic. org/health/treatments_and_procedures/hic_Fundoplication_Procedure_for_Children 22. http: //www. stanfordchildrens. org/en/topic/default? id=chronic-lung-disease-90 -P 02348 23. https: //www. healthcare. uiowa. edu/path_handbook/Appendix/Heme/PEDIATRIC_NORMALS. html Pictures: • http: //www. crosscanadarounds. ca/html/feb_07/images/figure%203. jpg • http: //www. meddean. luc. edu/lumen/Med. Ed/Radio/curriculum/IPM/PCM/86 a. jpg • http: //media. omedix. com/Healthwise/n 5551311. jpg
- Slides: 45