Pediatric Basic life support Prepared by Ebtesam Ahmed

ﺑﺴﻢ ﺍﻟﻠﻪ ﺍﻟﺮﺣﻤﻦ ﺍﻟﺮﺣﻴﻢ Pediatric Basic life support Prepared by Ebtesam Ahmed Abd Elbaset

Objectives Identifecation and treatment of problems that place the child at risk for cardiac arrest � application of systemic approach to pediatric assesment �

PEDIATRIC BASIC LIFE SUPPORT

resuscitation - It is. Cardiopulmonary an emergency procedures which is performed on person suffering (CPR) cardiac or respiratory arrest. -It is a combination of rescue breathing (mouth-tomouth resuscitation) and chest compressions. CPR can restore circulation of oxygen-rich blood to the brain.
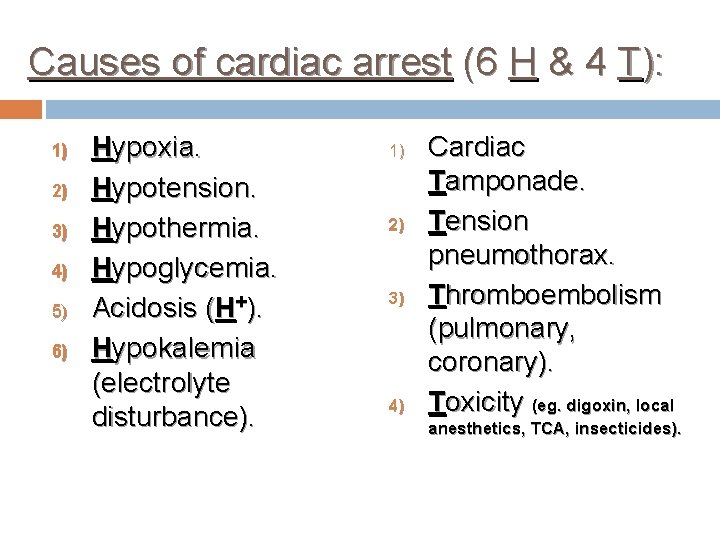
Causes of cardiac arrest (6 H & 4 T): 1) 2) 3) 4) 5) 6) Hypoxia. Hypotension. Hypothermia. Hypoglycemia. Acidosis (H+). Hypokalemia (electrolyte disturbance). 1) 2) 3) 4) Cardiac Tamponade. Tension pneumothorax. Thromboembolism (pulmonary, coronary). Toxicity (eg. digoxin, local anesthetics, TCA, insecticides).
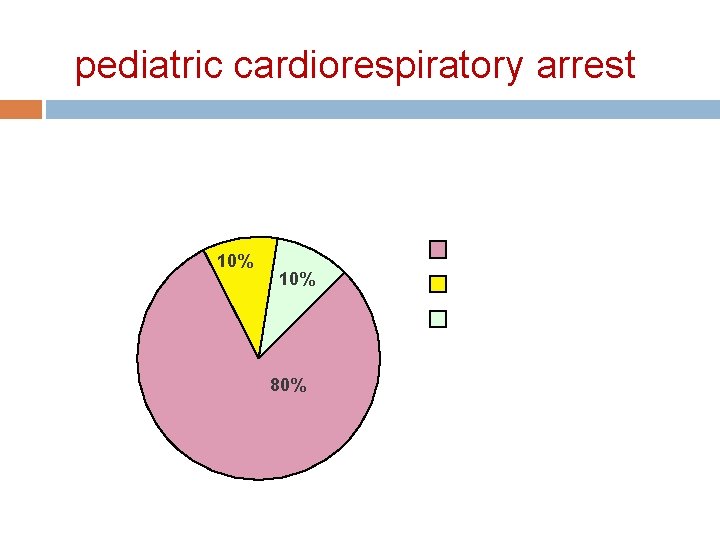
pediatric cardiorespiratory arrest 10% 80% Respiratory Shock Cardiac

The commonest cause of cardiopulmonary arrest in pediatric is respiratory
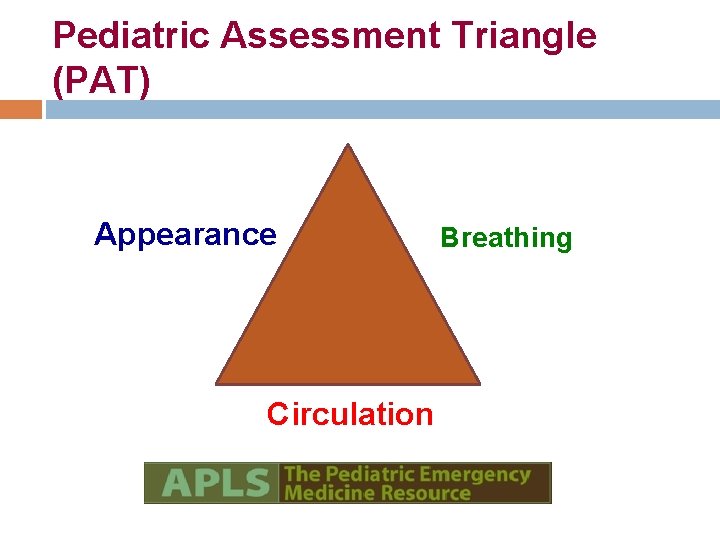
Pediatric Assessment Triangle (PAT) Appearance Circulation Breathing

Appearance Tone Interactiveness Look/Gaze Speech/Cry
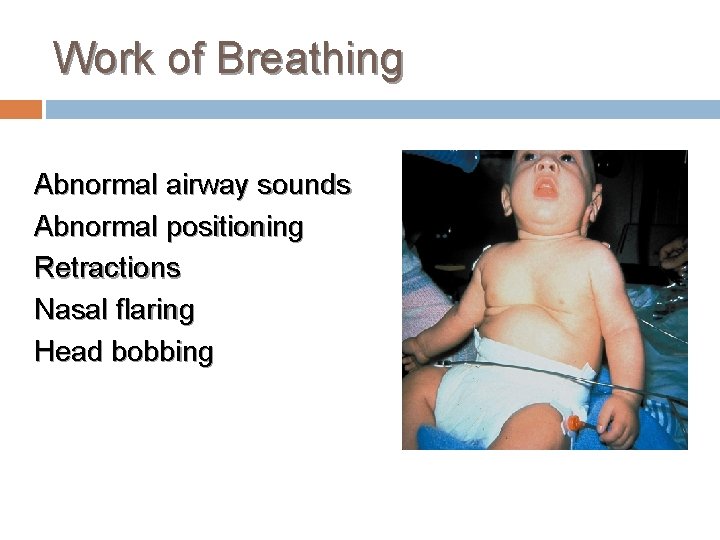
Work of Breathing Abnormal airway sounds Abnormal positioning Retractions Nasal flaring Head bobbing
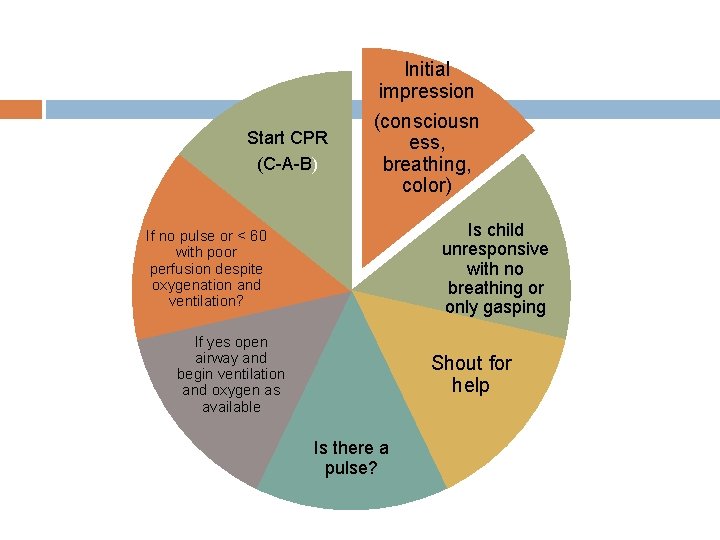
Start CPR (C-A-B) Initial impression (consciousn ess, breathing, color) Is child unresponsive with no breathing or only gasping If no pulse or < 60 with poor perfusion despite oxygenation and ventilation? If yes open airway and begin ventilation and oxygen as available Shout for help Is there a pulse?

Basic Life Support

Change in CPR Sequence: C-A-B Rather Than A-B-C
The 2010 AHA Guidelines for CAB sequence. (chest compressions- airway- breathing)

Pediatric chain of survival 2010

Circulation Objective: Maintain adequate blood flow to vital organs
Circulation-Chest Compressions Indications for chest compression: ❖Absent ❖Heart pulse rate < 60 BPM (or < 80 in infants) with signs of poor perfusion

Where to palpate? � � � The preferred location for checking the pulse depends on the patient’s age as well as the number and skill of the rescuers. • In infants, the brachial pulse is preferred but the femoral pulse can be used alternatively. • In older children and adults, the carotid pulse is preferred but a second or third rescuer may be better able to use the femoral pulse to monitor compressions. � • The brachial artery is palpated just above the elbow, � medial to the biceps. � • The femoral artery is palpated just below the inguinal ligament halfway between the anterior superior iliac spine and the pubic tubercle.
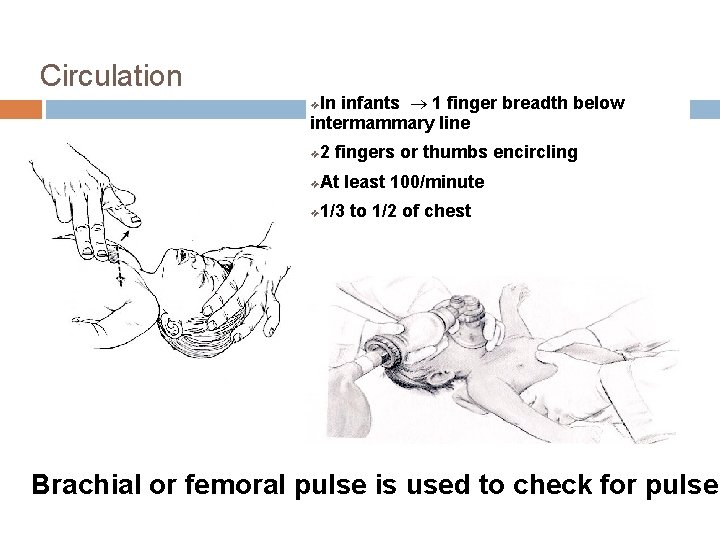
Circulation In infants ® 1 finger breadth below intermammary line ❖ 2 fingers or thumbs encircling ❖ At least 100/minute ❖ 1/3 to 1/2 of chest ❖ Brachial or femoral pulse is used to check for pulse
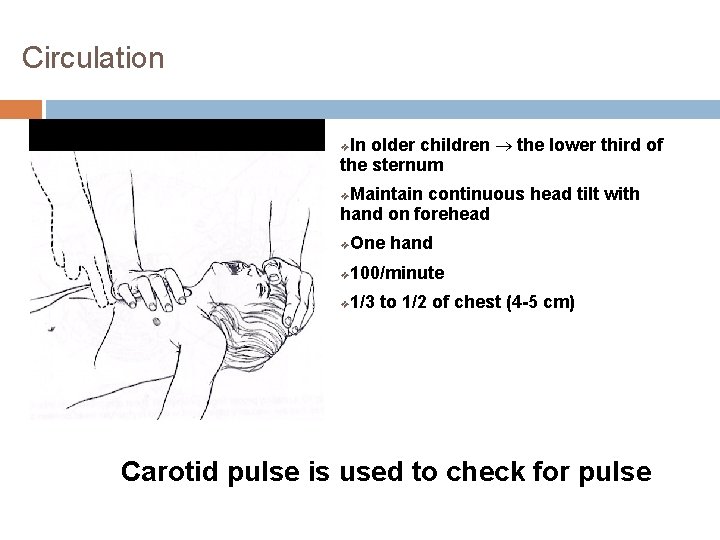
Circulation In older children ® the lower third of the sternum ❖ Maintain continuous head tilt with hand on forehead ❖ One hand ❖ 100/minute ❖ 1/3 to 1/2 of chest (4 -5 cm) ❖ Carotid pulse is used to check for pulse

BEST SIGN OF EFFECTIVE CIRCULATION Pulse with Each Compression
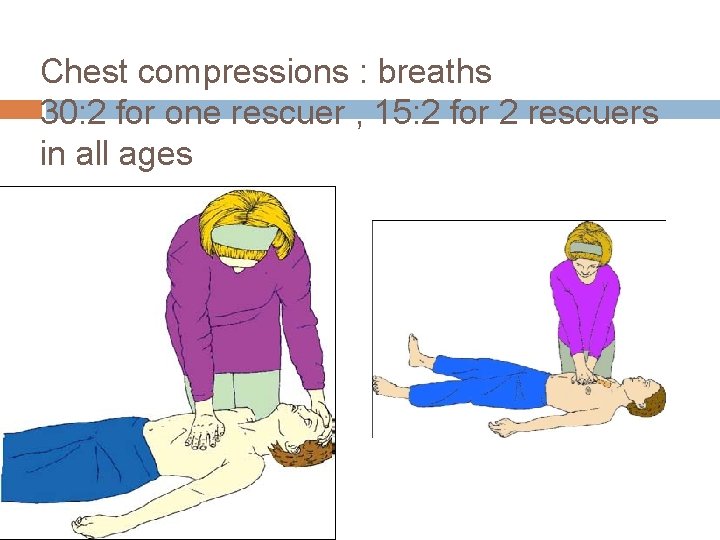
Chest compressions : breaths 30: 2 for one rescuer , 15: 2 for 2 rescuers in all ages

Airway Management OBJECTIVE: Maintain Patent Airway Open Airway Head-tilt/chin-lift method Jaw thrust method with possible neck injury
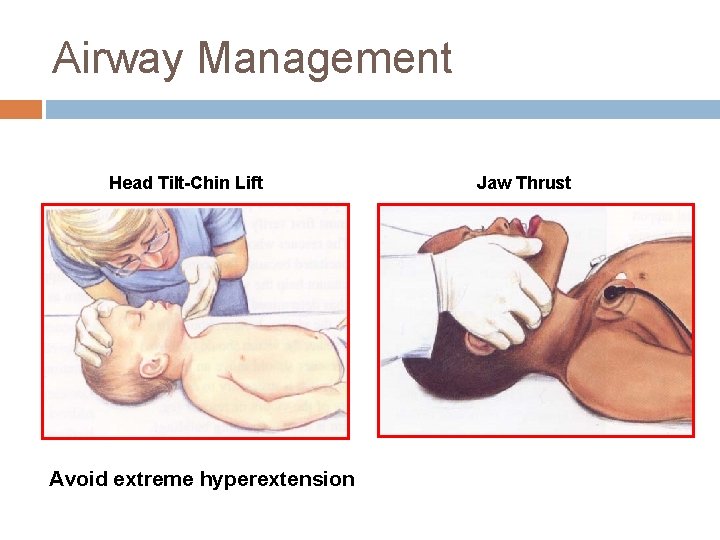
Airway Management Head Tilt-Chin Lift Avoid extreme hyperextension Jaw Thrust
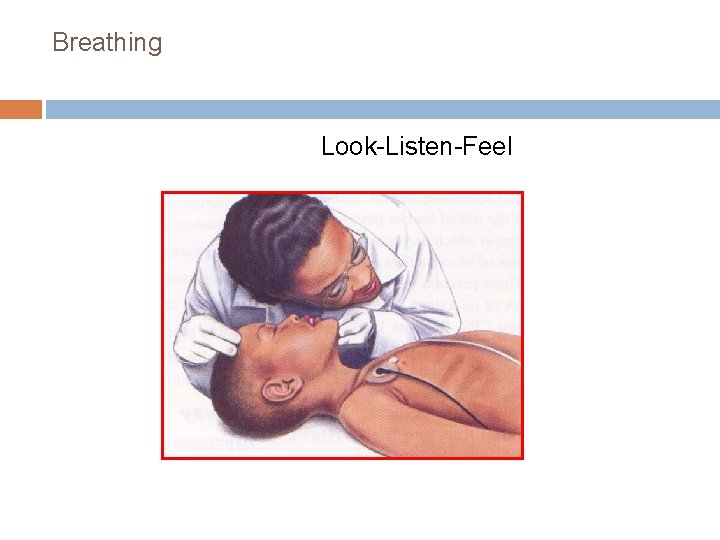
Breathing Look-Listen-Feel

Breathing Objective: Maintain Gas Exchange Rescue Breathing Mouth to mouth/nose-mouth Bag and Mask

Breathing-How much and how fast? Adequate ventilation = adequate volume x adequate rate Volume: enough to cause chest rise over 1 -1. 5 sec Rate: first 2 rescue breathing , then 1220/min synchronized with cardiac compressions at a ratio of 2 -15 if 2 rescuers and 2: 30 if one rescuer
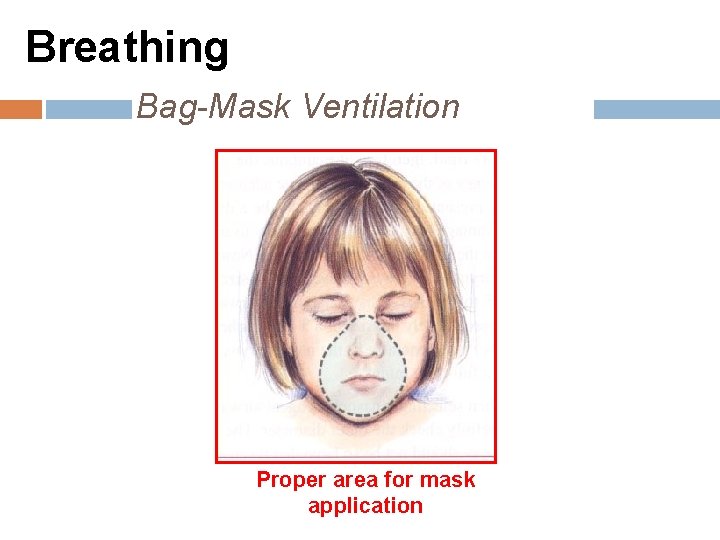
Breathing Bag-Mask Ventilation Proper area for mask application
Breathing Bag-Mask Ventilation

BEST SIGN OF EFFECTIVE VENTILATION Chest Rise

Oxygen therapy
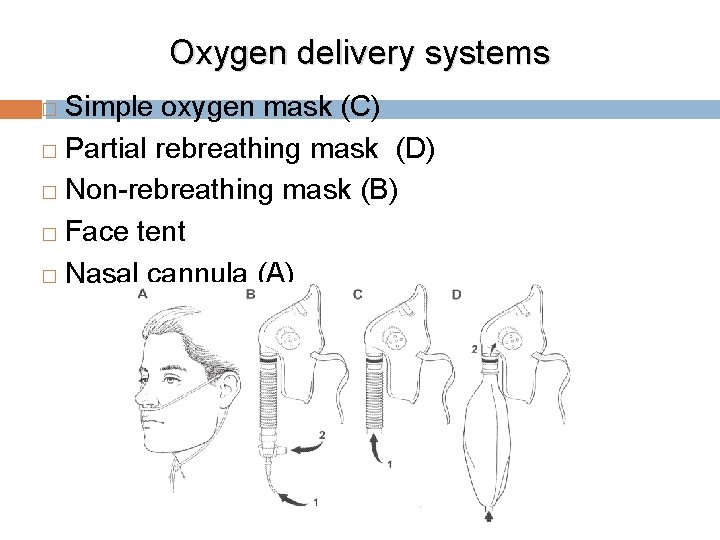
Oxygen delivery systems Simple oxygen mask (C) � Partial rebreathing mask (D) � Non-rebreathing mask (B) � Face tent � Nasal cannula (A) �

Indications of Oxygen Therapy � � � � Cardiac and respiratory arrest Hypoxaemia (Pao 2 < 7. 8 k. Pa, Sao 2 < 90%) Shock Low cardiac output and metabolic acidosis (bicarbonate < 18 mmol/l) Respiratory distress Inadequate tissue perfusion Low haemoglobin concentration septicaemia
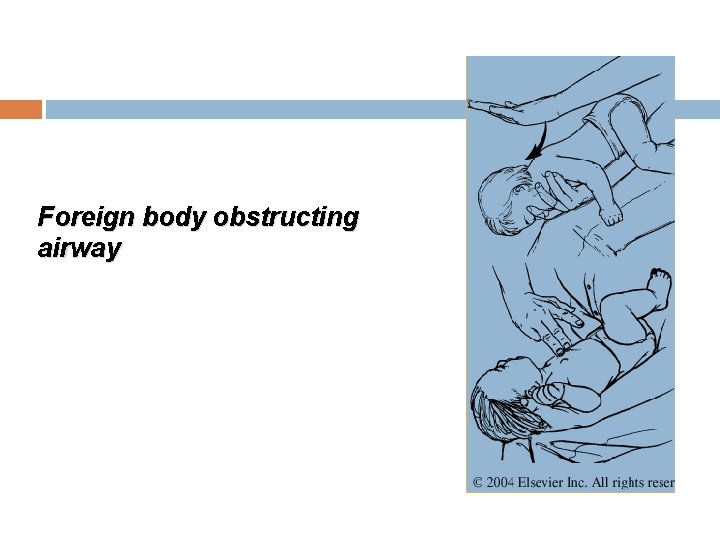
Foreign body obstructing airway
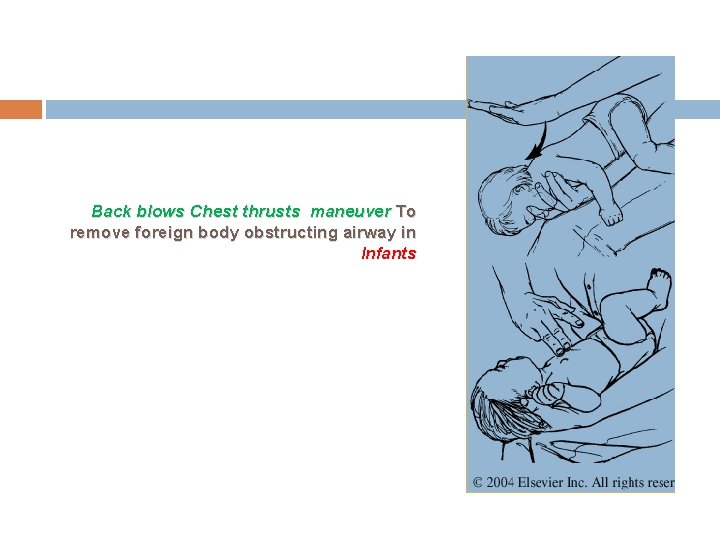
Back blows Chest thrusts maneuver To remove foreign body obstructing airway in Infants

CONSCIOUS CHILDREN: ABDOMINAL THRUSTS ● To remove foreign body obstructing airway In children over one year deliver up to five abdominal thrusts after the second five back blows. ● Use the upright position (Heimlich manoeuvre) manoeuvre if the child is conscious ● Up to five sharp thrusts should be directed upwards toward the diaphragm ● Abdominal thrusts are not recommended in infants because they may cause damage to the abdominal viscera


UNCONSCIOUS CHILDREN: ABDOMINAL THRUSTS ● To remove foreign body obstructing airway in Unconscious children, child must be laid supine and the heel of one hand placed in the middle of the upper abdomen. ● In children over one year deliver up to five abdominal thrusts after the second five back blows.

Thank You
- Slides: 40