Pediatric Airway Management SNOHOMISH COUNTY EMS OBJECTIVES Anatomy

Pediatric Airway Management SNOHOMISH COUNTY EMS

OBJECTIVES Anatomy Physiology Equipment Establish respiratory distress present Technique Post intubation management Pitfalls and Pearls Difficult airway

ANATOMY Unique <2 years old Approaches normal adult airway by 8 years old Glottic opening high and anterior C 1, transitions to C 3/4, then C 5/6 by adulthood More soft tissue, less tone
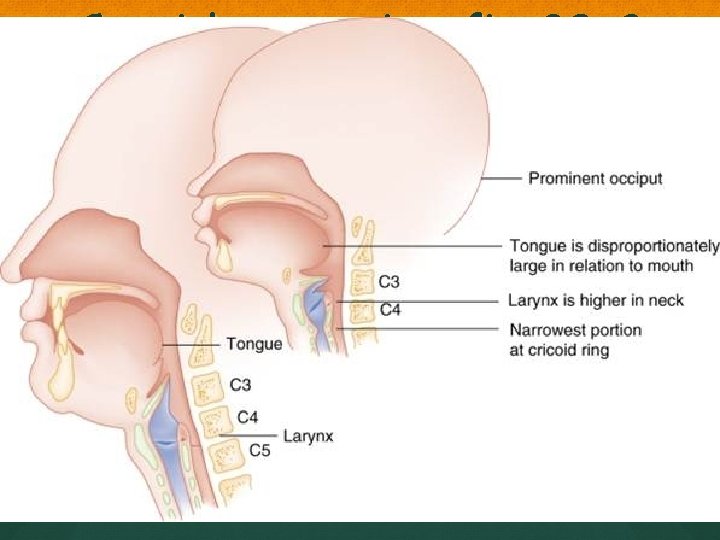
Consider copying fig 20 -2 p 270 here

ANATOMY Large tongue in relation to oral cavity Large tonsils and adenoids that can bleed (no blind nasotracheal intubations) Angle of epiglottis to laryngeal opening more acute

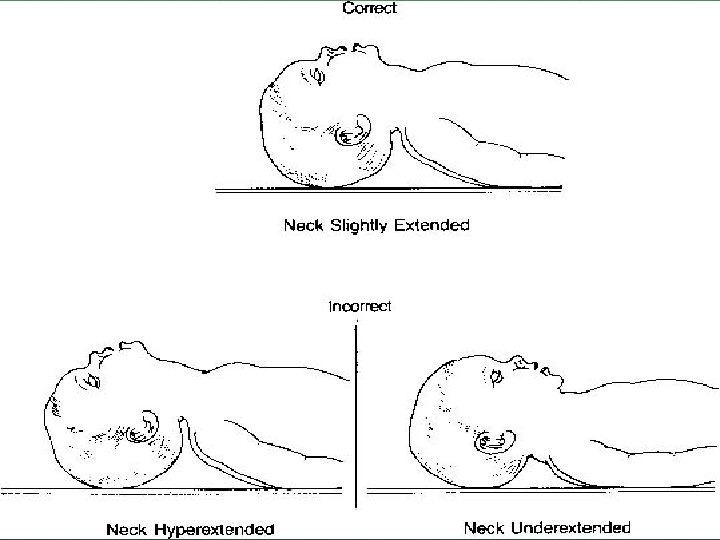
ANATOMY Large occiput/cranium flexes the neck Avoid further neck flexion Use sniffing position Neck flexed, head extended
ANATOMY Small cricothyroid membrane <3 -4 years old almost nonexistant >8 similar to adults No surgical cricothyroidotomy <8 Cricoid ring most narrow part of airway (below vocal cords)

PHYSIOLOGY Smaller floppy upper airway more likely to obstruct and more susceptible to swelling Resistance is inversely proportional to radius R 1/r 4 th power Small decrease in airway size=large increase in airway resistance

PHYSIOLOGY Crying increases the work of breathing 32 times Basal O 2 requirement 2 x that of adults FRC (functional residual capacity) 40% of adults Only half the alveoli of adults Overall, less reserve and faster desaturations

EQUIPMENT Length based systems Decrease errors Eliminate remembering and completing mathematical equations Organize equipment
BROSELOW SYSTEM
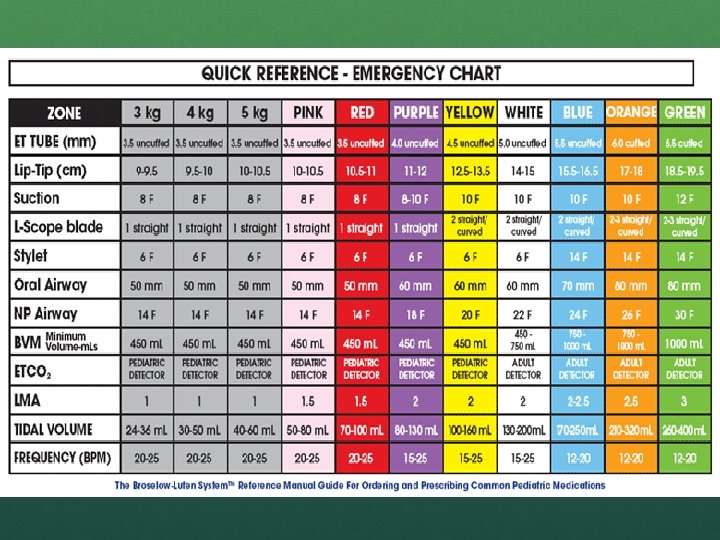

EQUIPMENT Self inflating bags smallest 450 ml Pop off valves that may have to be closed Newborn equipment different than peds (0 blades, <50 mm oral airways, 250 ml BVM, 3 -0 tubes)

RESPIRATORY DISTRESS Rapid 30 second assessment T one I nteractive C onsolablity L ook/track S peech/cry

RESPIRATORY DISTRESS Altered mental status Nasal flaring Head bobbing Accessory muscle use Grunting
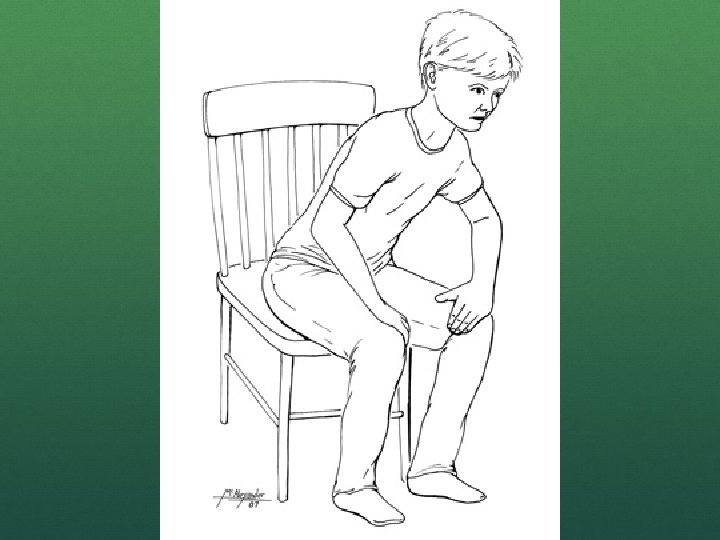
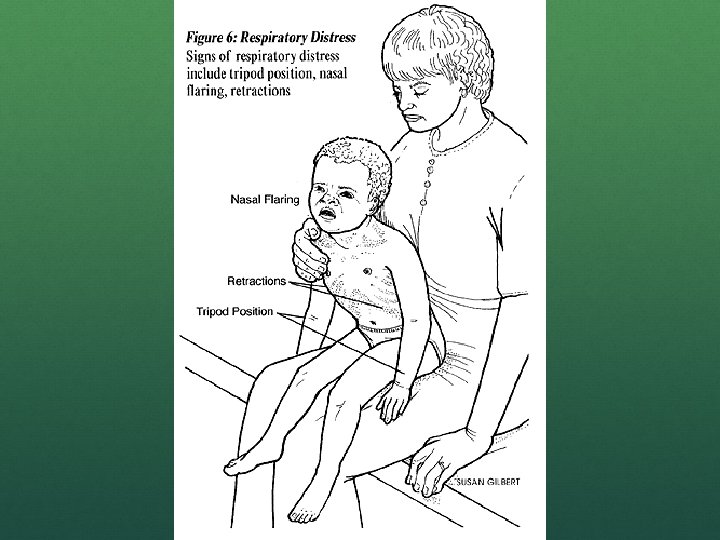

RESPIRATORY DISTRESS You must undress the patient Retractions Substernal Intercostal Supraclavicular Suprasternal

RESPIRATORY DISTRESS Infants are nose breathers Secretions can impeded air flow Bulb syringe nasal suction may alleviate this

RESPIRATORY FAILURE Impending respiratory arrest All of the above signs diminish Respiratory rate diminishes Mental status diminishes Child becomes quiet Mottling may develop

TECHNIQUE MEDICATIONS Succinylcholine Dose higher at 1. 5 mg/kg Etomidate 0. 3 mg/kg Fentanyl 1 -3 mcg/kg consider for age >10 and head injury

TECHNIQUE MEDICATIONS Vecuronium 0. 1 mg/kg Rocuronium 1 mg/kg

TECHNIQUE MEDICATIONS Atropine Routine use not recommended Should be available and prepared in case it is needed (more common in children <1) 0. 02 mg/kg

TECHNIQUE HEAD POSITION Sniffing position Slight anterior displacement of neck (pulling chin up) Small infants may require elevation of shoulders with a towel to counteract a large occiput flexing head Older children may require a towel under the head Goal is to align ear canal anterior to shoulders Head tilt chin lift or Jaw thrust (trauma patients)
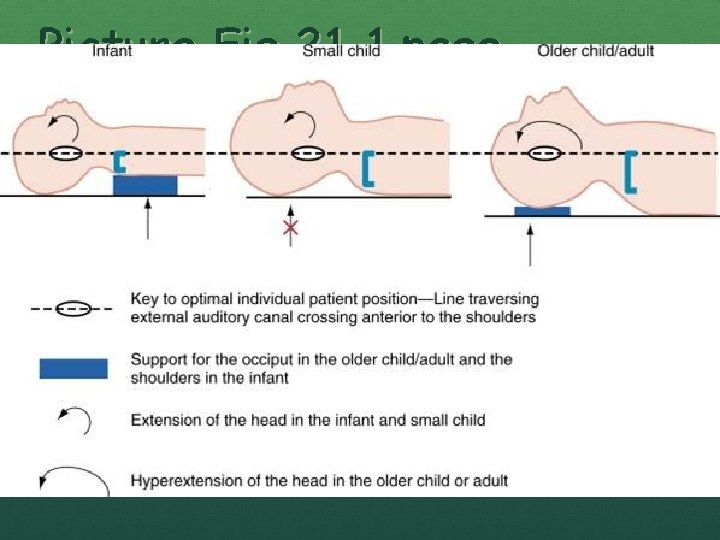
Picture Fig 21 -1 page 284

TECHNIQUE OXYGEN SUPPLEMTATION Oxygen may be delivered by Blow by Nasal cannula Face mask Forcing the child to struggle with nasal cannula oxygen increase oxygen demand Blow by may suffice

TECHNIQUE BVM alone may suffice for short transports Pediatric airway obstruction usually amenable to BVM The extra thoracic trachea is collapsible in children, so with increased negative pressure from inspiration during obstruction, obstruction may become worse and BVM may help

TECHNIQUE BVM Don’t compress submental tissue Hold angle of mandible Use C-Clamp technique (solo) Use 2 providers when possible Don’t put pressure on eyes (causes vagal response)

TECHNIQUE BVM Normal tidal volume 8 -10 ml/kg Watch for adequate chest rise Squeeze-Release to allow for exhalation Only use enough force to see chest rise 8 -10 BPM code, 12 -20 alive (monitor end tidal CO 2)

TECHNIQUE BVM Avoid gastric insufflation Avoid excessive peak inspiratory pressure Ventilate slowly and watch for chest rise Slight cricoid pressure (excessive will compress trachea in peds)

TECHNIQUE BLADES Follow Broselow guide Miller straight blade better until about age 5 Lifts disproportionately large epiglottis out of way

TECHNIQUE CRICOID PRESSURE Insufficient evidence to routinely recommend cricoid pressure during intubation (as opposed to BVM)

TECHNIQUE LAYNGEAL MANIPULATION Use as needed Frequently: B ackward U pward R ightward P ressure

TECHNIQUE TUBES Use Broselow guide Be prepared with tubes 0. 5 mm larger and smaller Narrowest part of airway is below cords If tight, use smaller tube If large air leak, use larger tube or same size tube with cuff Small air leak, no worries if adequate chest rise, O 2 sat, end tidal CO 2

TECHNIQUE TUBES Cuffed tubes Are OK Cuff pressure needs to be monitored (20 -25 cm water) Don’t have to be inflated In general, go a size smaller if using cuffed tube for size <6. 0 Too large a tube/too high cuff pressure)=laryngeal tracheal stenosis which can develop rapidly

TECHNIQUE TUBES Tube insertion depth Follow Broselow 3 x size of tube (4. 0 ETT=12 cm insertion length at teeth) Secure tube, immobilize neck, as short trachea predisposes to moving tube too far in with neck flexion, and out with neck extension

TECHNIQUE CONFIRM PLACEMENT Tube fogging B/L breath sounds Silent epigastrum End Tidal CO 2 Pulse ox

TECHNIQUE END TIDAL CO 2 Peds detectors up to 15 kg (adult detectors have too much dead space in circuit) Adult detectors over 15 kg (peds detectors will cause too much resistance

TECHNIQUE END TIDAL CO 2 In cardiac arrest: If <10 -15 mm. Hg, focus on improving CPR and avoid over ventilation An abrupt and sustained increase may signal return of spontaneous circulation In non arrest: Titrate to clinical condition (35 -45 unless head injury/impending herniation 25 -30)

POST INTUBATION MANAGEMENT Adequate sedation Benzodiazepines Diazepam 0. 2 mg/kg (max 10 mg/dose) Lorazepam 0. 05 mg/kg (max 2 mg/dose) Midazolam 0. 1 mg/kg (max 2 mg/dose) Opiates Fentanyl 1 -3 mcg/kg (max 50 mcg/dose) Morphine 0. 05 -0. 2 mg/kg (max 5 mg/dose) Paralytics as needed Rocuronium 1 mg/kg Vecuronium 0. 1 mg/kg

POST INTUBATION MANAGEMENT Problems D isplacement of tube (confirm placement) O obstruction of tube (pass suction catheter) P neumothorax E quipment failure (unhook from vent, check O 2)

PITFALLS AND PEARLS Performance anxiety Equipment stocking and testing Troubleshooting Periodic training and practice

DIFFICULT AIRWAY Infectious disease causes Noninfectious causes including trauma Congenital abnormalities

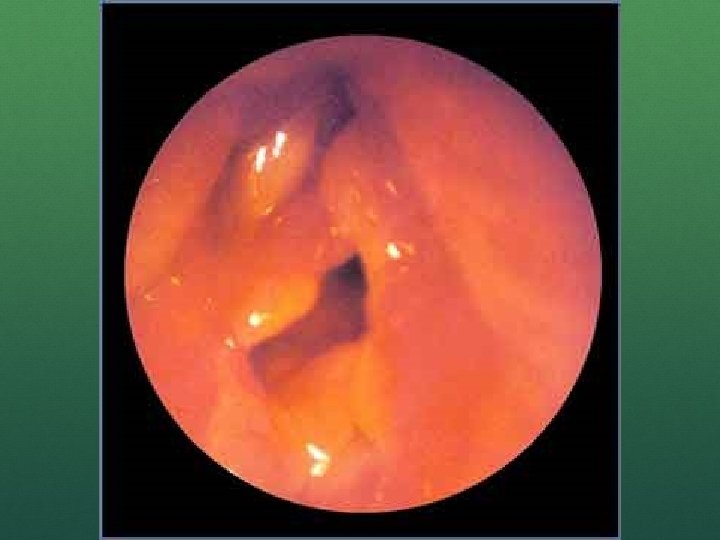
DIFFICULT AIRWAY INFECTIOUS DISEASE Epiglottitis Croup Retropharyngeal abscess Bacterial Tracheitis Ludwig’s angina

DIFFICULT AIRWAY INFECTIOUS DISEASE Small changes in airway diameter have a large impact on airway resistance Crying increases work of breathing 32 times Don’t “over treat”

EPIGLOTTITIS If stable, leave patient with parent in position of comfort 2 person bag valve mask ventilation can be sufficient If needed, intubation can be attempted with a smaller than predicted tube Push on chest to try to see bubbles coming from airway if visualization obstructed One of the few indications for needle cricothyrotomy if all else fails
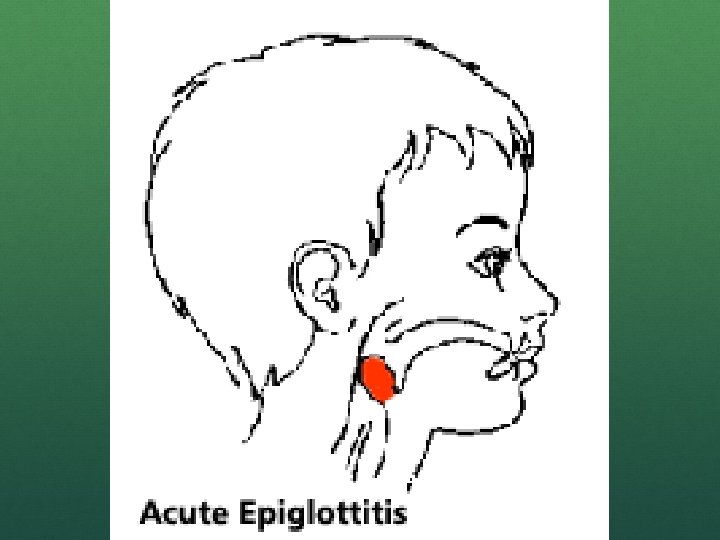
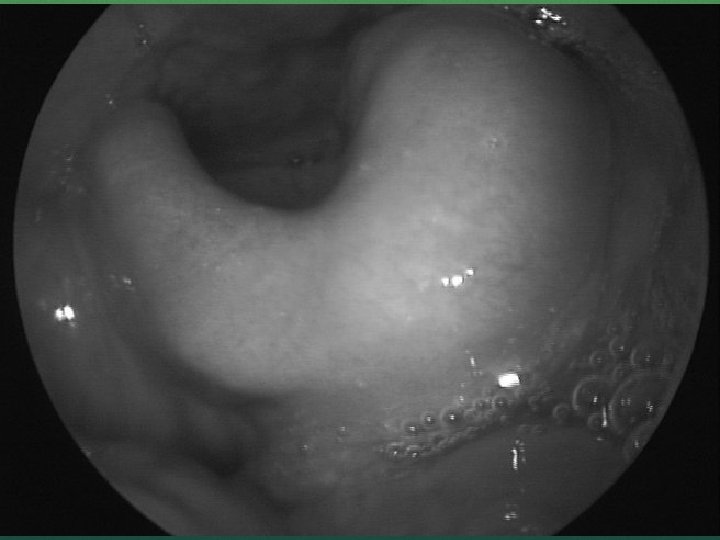

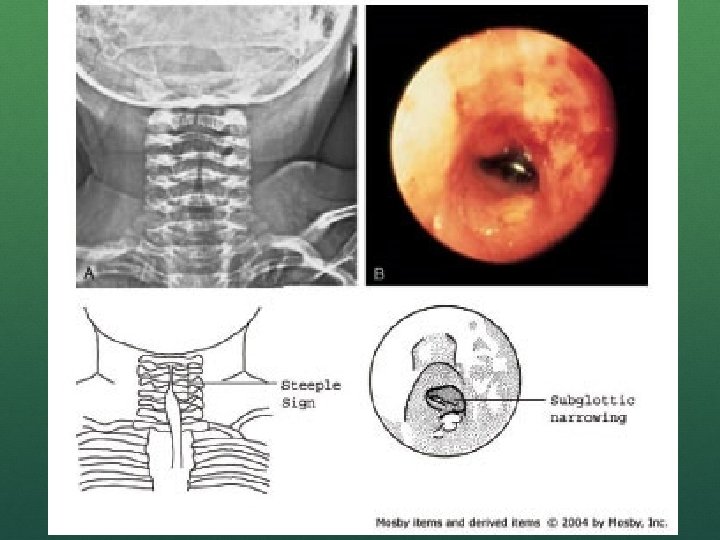
CROUP Subglottic narrowing Tube may fit through cords, but then get snug Use smaller than expected tube BVM can work, but requires 2 people and possible high pressure

DIFFICULT AIRWAY NONINFECTIOUS DISEASE Foreign body Burns Anaphylaxis Caustic ingestion Trauma

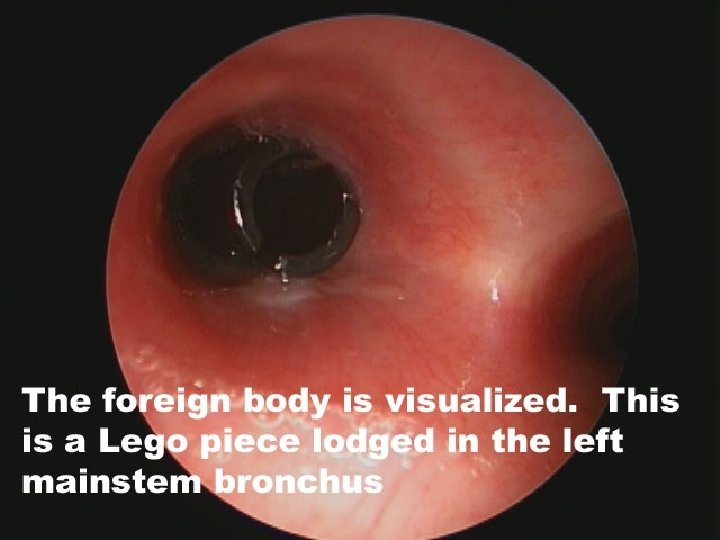
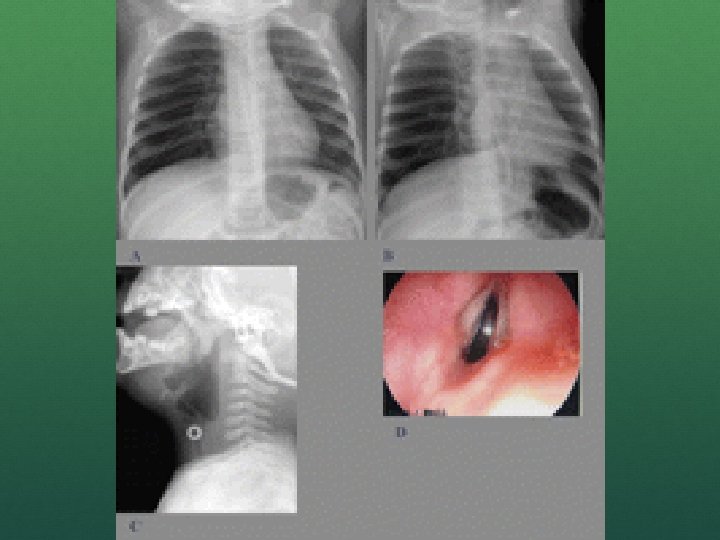
FOREIGN BODY Conscious Consider doing nothing if patient stable Back blows less than age 1 year Heimlich (age greater than 1) Unconscious BVM may work Direct laryngoscopy Removal of object Push it down and move the tube back to normal position Needle cricothyrotomy will only work if obstruction is above the cricothyrotomy level (you should see it but can’t remove it)

BURNS, ANAPHYLAXIS, CAUSTIC INGESTIONS, TRAUMA If condition is decompensating and/or not responding to treatment, consider early intervention Should consider medications first in anaphylaxis

CONGENITAL ABNORMALITITES Don’t try unless you have to May be more reasonable to support until respiratory failure/arrest has occurred Treat for causes of respiratory distress

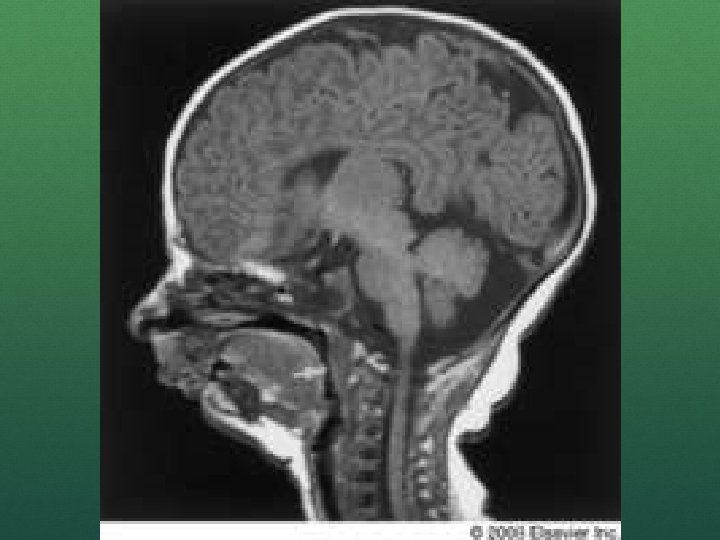
CONGENITAL ABNORMALITITES MICROGNATHIA Small mandible reduces the space to which the tongue and soft tissue can be displaced out of your way

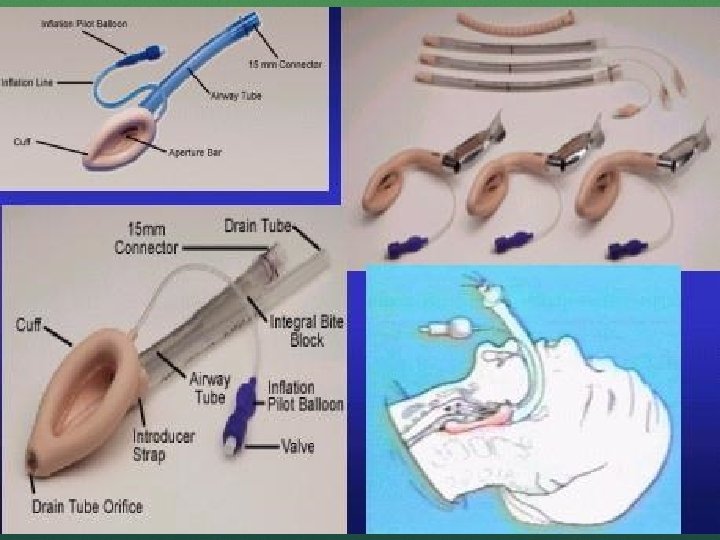
DIFFICULT AIRWAY ADJUNCTS LMA Needle cricothyrotomy Combitube/King LT

DIFFICULT AIRWAY LMA Can be used in all ages In small infants more complications Causes obstruction with relatively large epiglottis Easy to lose adequate seal with movement Air leaks Recommend inserting upside down and rotating it as advanced back Not foreign bodies, caustics, burns

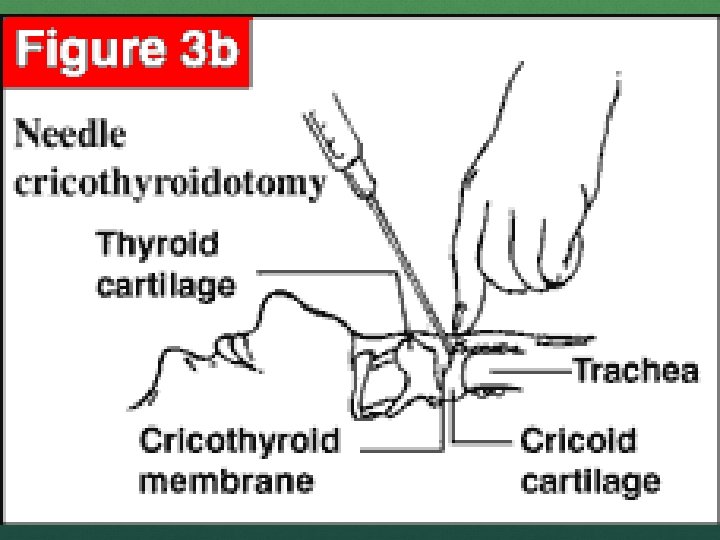
NEEDLE CRICOTHYROTOMY For use when you cant intubate or ventilate For use in children <8 -10 years old Not helpful for croup or distal foreign bodies

NEEDLE CRICOTHYROTOMY Extend head, towel under shoulders Identify landmarks Insert catheter (14 g) over the needle at a 30 degree angle directed toward feet Aspirate air Slide catheter off needle and remove needle Attach 3 mm ETT adapter and begin BV

NEEDLE CRICOTHYROTOMY Will require excessive force due to small catheter diameter Pop off valve should be disabled Does not protect airway Does not allow for adequate ventilation, only oxygenation

NEEDLE CRICOTHYROTOMY Complications Inappropriate needle placement Inadequate ventilation (hypercarbia and acidosis) Obstruction of small catheter Subcutaneous emphysema

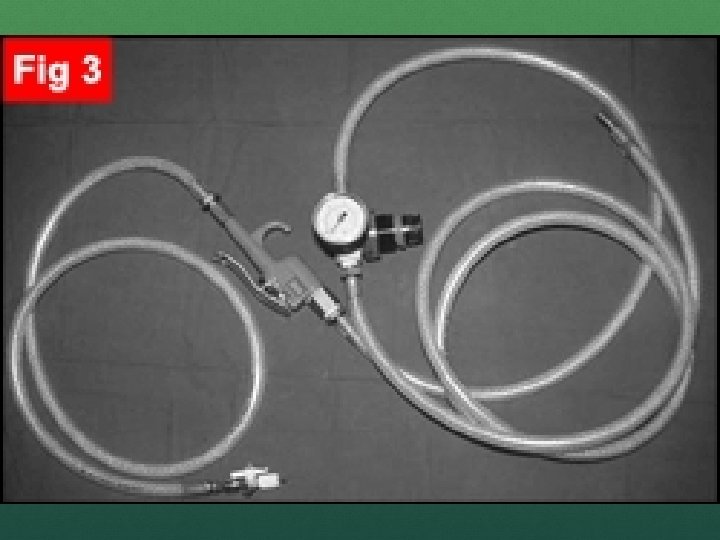
NEEDLE CRICOTHYROTOMY TTV For use >5 years Supraglottic patency required to allow for exhalation (air stacking) Barotrauma Start with 20 PSI and adjust to chest rise Requires no more than of 1 second inspiration, then 3 seconds to exhale Nasal/oral airway should be placed as well

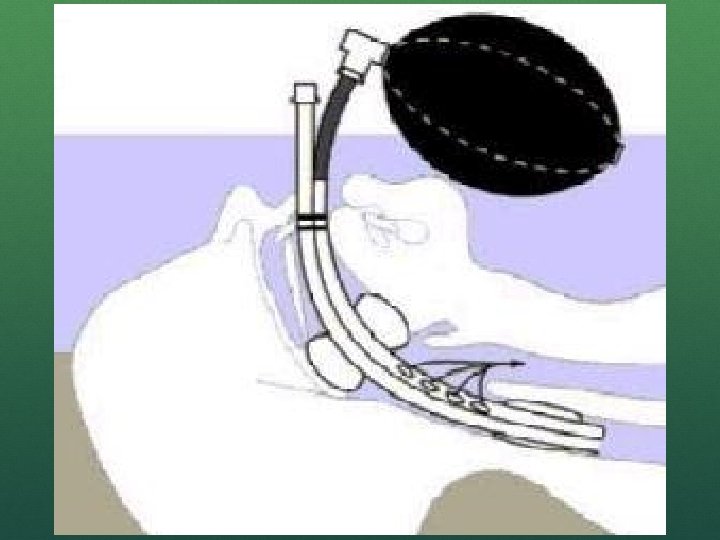
COMBITUBE/KING LT Double/single lumen tube designed to be place in esophagus Must be 4 ft tall for small Combitube May not protect against aspiration Not for caustic ingestion or significant esophageal pathology
- Slides: 74