Pediatric Airway Management Jennifer Oliverio RRT BSc Clinical

Pediatric Airway Management Jennifer Oliverio RRT, BSc Clinical Educator Respiratory Services Alberta Children’s Hospital

A & P Characteristics of Newborn Respiratory System • Infant lung is a unique structure not a mini- adult lung • Airways, distal lung tissue and pulmonary capillary bed continue to grow and develop after birth • General pattern is laid down at birth but upper and lower airways continue to change • Alveoli development complete and adult anatomy by 810 years of age • Ossification of ribs and sternum complete by 25 years of age 2

Nose • Obligatory nasal breathing • Poor tolerance to obstruction Tongue • Relatively Large • Neck extension may not relieve obstruction 3

Head • Relatively large • Anterior flexion may cause airway obstruction Epiglottis • Relatively large and U- shaped • More susceptible to trauma • Forms more acute angle with vocal cords 4

Larynx • More anterior and cephalad • Intubation more difficult Cricoid • Narrowest portion of airway • ↑ resistance with airway edema or infection • Acts as “cuff” during tracheal intubation 5

Trachea • Small diameter (6 mm), high compliance • ↑ resistance with airway edema or infection • Collapses easily with neck hyperflexion or hyperextension Alveoli • ↑ closing capacity • No pores of Kohn • ↑ air trapping and ↓ collateral circulation of air 6

Pulmonary Vessels • ↑ pulmonary vascular resistance (PVR) • Very sensitive to constriction by hypoxia, acidosis and hypercarbia Chest Wall • • • ↑ compliance due to weak rib cage ↑ A-P diameter Horizontal ribs Breathing is all diaphragmatic FRC determined solely by elastic recoil of lungs Chest wall collapses with -ve pressures 7

WOB • Weak resp muscles • ↑ RR = early sign of resp distress Regulation of Breathing • Response to ↓ O 2/ ↑ CO 2 minimal • Tolerates hypoxia poorly 8

Airway assessment • Best to 1 st look from afar. Infants and small children don’t like strangers hard to assess baseline after they are upset. • Is the chest moving? • Can you hear breath sounds? • Are there any abnormal airway sounds (e. g. . Stridor, snoring)? • Is there increased respiratory effort with retractions or respiratory effort with no airway or breath sounds? 9

Airway Management • Simple things to improve airway patency • Suction nose and oropharynx • Reposition child/ allow child to assume position of comfort • head-tilt-chin lift/ jaw thrust • Use airway adjuncts- NPA/ OPA 10

Oral & Nasopharyngeal Suctioning • Clean technique • Negative pressure of 80 to 120 mm. Hg. Test suction level on regulator prior to suctioning • Nasal and oral suction can be performed with same catheter • May result in hypoxia, ↓ HR (vagal), bronchospasm, larygospasm, atelectasis 11

Suction supplies • • Clean gloves Suction regulator, canister, tubing Normal saline in cup Yankauer and appropriate suction catheter Neonates 5 -6 Fr Infants 6 -8 Fr Older kids 10 Fr 12

Nasopharyngeal Suction • Measure length from pt’s earlobe to tip of nose • Keep pass <10 sec. • Document: pt assessment prior to procedure, time of procedure, amount and type of secretions, pt’s response 13

Positionning • If pt has preferred position let them remain in that position e. g. tripod • Repositioning can greatly improve airway patency • Manual airway maneuvers can also help open the airway (head tilt-chin lift/ jaw thrust) 14

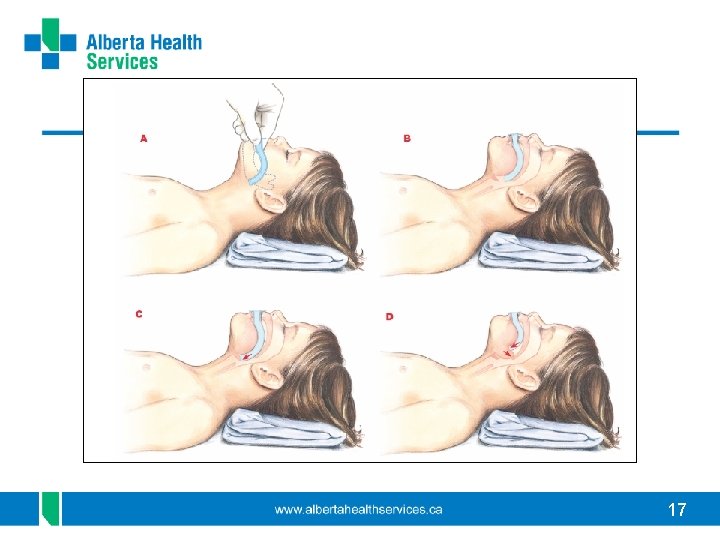
Oral Pharyngeal Airways (OPA) • Only for use in UNCONSCIOUS pt with no intact cough/gag reflex • Holds tongue and soft hypopharyngeal structures away from posterior pharynx • Still need good head and jaw position to maintain airway patency • Suction airway prn • Never tape in place 15

Choosing correct OPA • Place OPA against side of face. With flange at the corner of the mouth the tip should reach angle of the jaw • Too small: will not adequately displace tongue • Too large: may obstruct larynx and/ or interfere with mask fit if BVM required 16
17

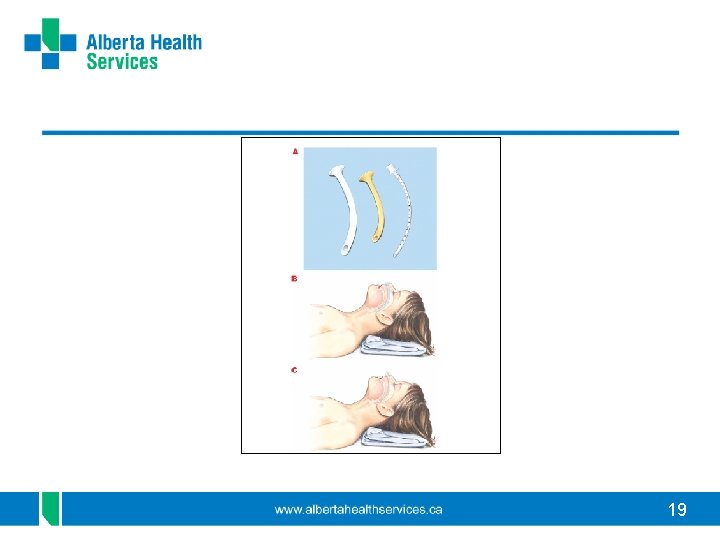
Nasopharyngeal Airways • Soft plastic pre-made or shortened ETT • Provides unobstructed path for airflow between nares and pharynx • Can use in conscious/ semi-conscious pt • Small internal diameter so must be evaluated frequently and suctioned prn to maintain patency 18
19

If these don’t work… • Pt may require more advanced interventions to establish a patent airway • CPAP • Intubation 20

Breathing • • • RR Effort Tidal volume Airway and lung sounds Sp. O 2 21
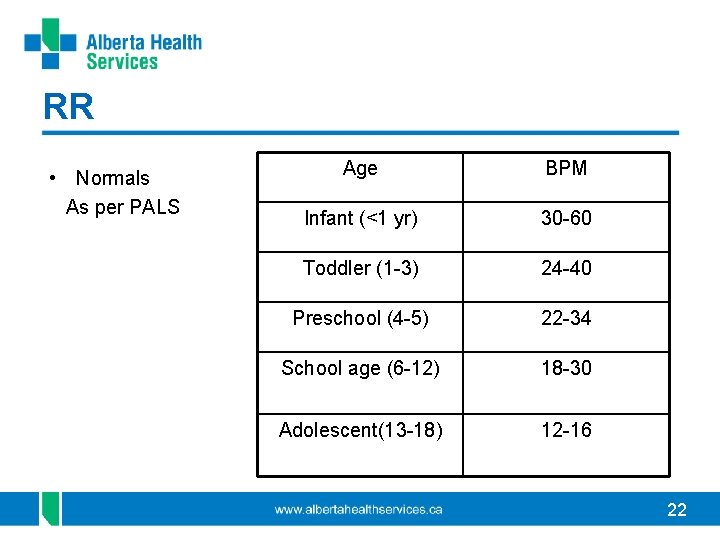
RR • Normals As per PALS Age BPM Infant (<1 yr) 30 -60 Toddler (1 -3) 24 -40 Preschool (4 -5) 22 -34 School age (6 -12) 18 -30 Adolescent(13 -18) 12 -16 22

RR • Best to evaluate prior to hands-on assessment • Excitement, anxiety, exercise, pain, fever, agitation can all ↑ RR • ↓ RR with acutely ill child or with ↓ LOC = ++ cause for concern • > 60 in any age is cause for concern 23

Effort • Signs of ↑’d respiratory Effort – Nasal flaring – Chest retractions – Head bobbing • Chin lifts and neck extends during I • Chin falls forward during E – Seesaw respirations • Chest retracts and abdomen expands during I, reversed during E • Very Inefficient= quickly leads to fatigue – Grunting • Child exhales vs partially closed glottis in an effort to keep small airways open 24

Auscultation • Same landmarking and principals as with adults • BUT…smaller size and sound is transmitted much more easily throughout the infant chest. 25

Bag-Mask Ventilation • Indicated when the pt’s spontaneous breathing effort is inadequate despite patent airway • Can provide adequate oxygenation and ventilation until definitive airway control is obtained • Can be as effective as ventilation through ETT 26
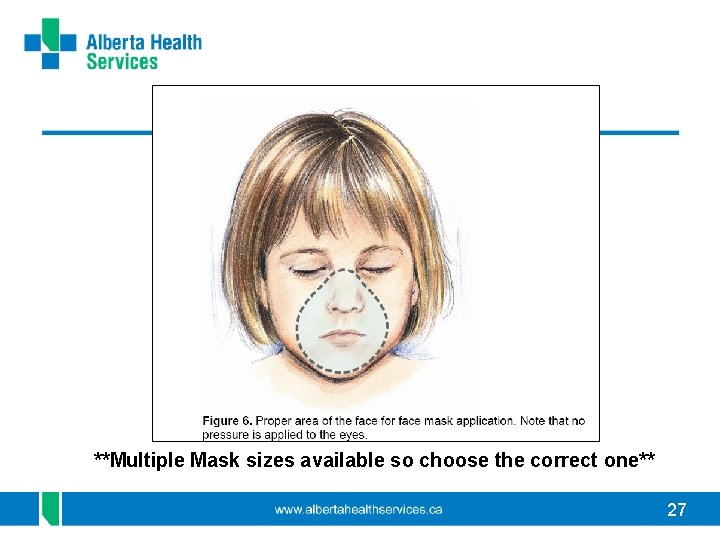
**Multiple Mask sizes available so choose the correct one** 27

Bagging Units • 3 sizes: Age Volume (ml) Infant 500 Child 1000 Adolescent 2000 28

Testing the bagging unit • Check all components before use to ensure proper function. Ideally as part of your daily safety checks. • Occlude pt outlet and outflow, squeeze bag ensure no tears/leaks • Check that PEEP valve works (2 L) • Ensure connection to wall O 2 and adequate flow • Proper size mask with cuff inflated 29

Bagging 1. Position pt: sniffing position 30
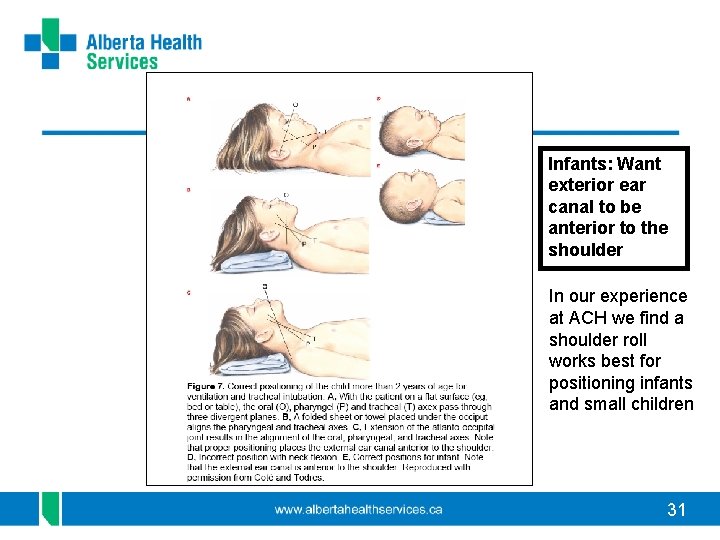
Infants: Want exterior ear canal to be anterior to the shoulder In our experience at ACH we find a shoulder roll works best for positioning infants and small children 31

Bagging 1. 2. Position pt: sniffing position Open airway and seal mask to face using E-C technique. You may need OPA. 32

33

Bagging 1. 2. 3. Position pt: sniffing position Open airway and seal mask to face using E-C technique. You may need OPA. Squeeze bag with other hand to deliver tidal volume and produce chest rise. Careful to not over-ventilate! 34

2 person BMV • One person uses both hands to open airway and maintain tight mask-to-face seal • 2 nd person bags 35

Monitor effectiveness of Ventilation • • Visible chest rise with each breath Sp. O 2 ETCO 2 HR BP Pt responsiveness Air entry on auscultation 36

If ventilation is not effective… • • • Reposition pt. Reposition airway. OPA. Verify proper mask size and placement Suction airway Check O 2 source and flow Check bag and mask for function/leaks Treat gastric inflation 37

Indications for intubation • • Respiratory distress Apnea Self-extubation Upper airway obstruction or the potential to develop upper airway obstruction • Actual or potential decrease in airway protection (compromised neurological function) • Need to eliminate/ reduce WOB (e. g. cardiac pt) • Inadequate ventilation and/or oxygenation 38

Preparing for Intubation • Appropriate ETT for >1 yo: (age/4) + 4 Term infant: 3. 0 -3. 5 ID 6 mo: 3. 5 -4. 0 ID 1 yo: 4. 0 -4. 5 ID • Cuffed ETT’s for pt’s > 8 yo • If you anticipate need for high PEEP or PIP may want to use cuffed ETT with <8 yo. Use ½ size smaller ETT. • Remember SOAPME 39

SOAPME Suction equipment: yaunkauer, catheters, regulator/canister/tubing, Oxygen: O 2 flowmeter, preoxygenate 2 -3 min, manual resuscitator bag with mask Airway equipment: ETT, stylet, syringe (cuffed ETT), laryngoscope and blade, lubricating gel, OPA Position, pharmacy, personnel: supine, rolls for positioning, bed height up Monitors ETCO 2 detector 40

Post-Intubation • • • ETCO 2 assessment for confirmation of placement Auscultation for bilateral air entry Placement of ETT documented ETT secured with tapes CXR to confirm placement Place pt on ventilator 41

Acute deterioration post-intubation • Remember DOPE D Displaced ETT may be in trachea or in right or left mainstem bronchus O Obstruction of ETT Secretions, blood, pus, foreign body, kinked ETT P Pneumothorax Simple Tension E Equipment failure Disconnection of O 2 source, leak in vent circuit, loss of power/ vent malfunction 42

Tube Position • Remember: Endotracheal tube position follows chin • Pt positioning ++ important. Often need shoulder roll to keep chin neutral. • CXR need to be done with neutral, midline head position (RRT should be called) – Chin low- tube low – Chin high- tube high 43

Uncuffed ETT’s • May have issues with leak • Better success with Pressure modes of ventilation with a tube leak • Position of pt can affect amount of leak • If having difficulty with ventilation or oxygenation may need to upsize ETT or Δ to cuffed ETT • Short term fix: NS soaked nasal packing packed around ETT. DO NOT CUT the gauze. 44

Cuffed ETT • Important to assess cuff inflation Qshift • > 8 yo can follow adult VAP guidelines • 25 -30 cm H 2 O inflation pressure • < 8 yo MOV with pressure < 20 cm H 2 O often quite a bit lower than 20 • Cuff is circumferential in a growing airway! 45

Suctioning ETT • Suction frequency depends on ETT size and pt needs: • 4. 0 i. d. and smaller- a minimum of Q 8 H unless • otherwise ordered • 4. 5 i. d. and greater- prn or as ordered • All pt’s need for suction should be assessed hourly and prn Sterile suctioning Suction depth should only be 0. 5 cm past the end of ETT • Determine suction depth by using suction guide or match number on catheter to number on ETT and advance 0. 5 cm. 46

Assessing need for suction • Clinical assessment of pt will determine frequency of suctioning. Many factors influence the need for suction including but not limited to: – ETT Size – Changes in vital signs – Adventitious breath sounds – ↓ breath sounds/ chest movement – ↓ Sp. O 2 – Visible secretions in ETT – Respiratory distress – Coughing – ↑Tc. CO 2/ Et. CO 2 – ↑ PIP – Worsening ABG/CBG 47

Selecting suction catheter • Use largest size that can pass easily down the ETT • Ideally not larger than half the diameter of ETT to avoid causing atelectasis • TIP: choose double the ETT e. g. 4. 0 i. d. ETT choose 8 Fr suction catheter 48

Wall suction Use lowest possible setting Age negative pressure (mm. Hg) < 1 yo 60 -80 1 -12 yo 80 -120 13 -17 yo 100 -150 49

Instillation • Normal saline unless otherwise ordered • Should occur prn not routinely • For <10 FR you can use sterile NS syringe as there is no one-way valve in instillation port. For >12 Fr you will need pink NS nebule. • Recommended amounts: Age Volume < 1 yo* 0. 5 -1. 0 m. L 1 -12 yo 0. 5 -3. 0 m. L 13 -18 yo 0. 5 -5. 0 m. L *total volume is especially important to limit and document in infants and small children 50

Suction Guide • Should be filled out at the bedside for all ETT < 4. 5 and all pediatric tracheostomy pt’s regardless of tube size • Suction ½ cm farther than marked length to clear end of ETT unless otherwise ordered (e. g. TEF repair) 51
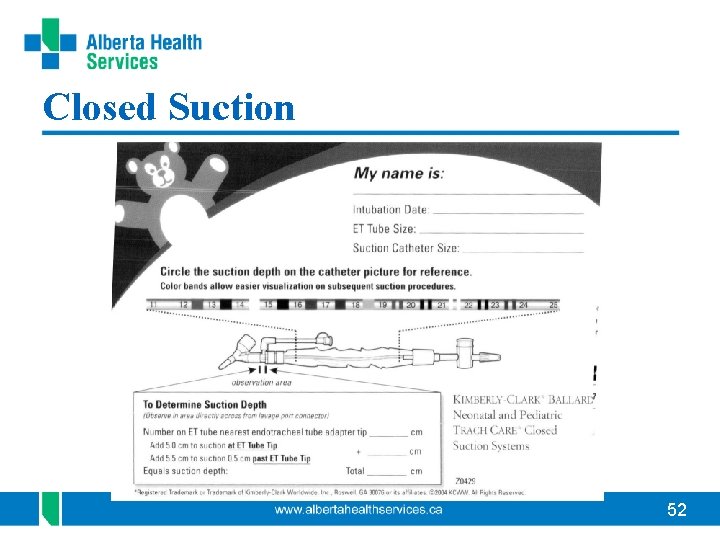
Closed Suction 52

53

Patient Preparation • • • Assess pt visually and auscultate, note monitor readings Determine need for sedation/ analgesia Ensure ETT tapes are secure Explain procedure to pt/ parents Pre- oxygenate and give meds as required Position pt 54

Closed Suction • Ensure suction is on and set appropriately • Ensure bagging unit attached to O 2, adequate flow, and intact • Attach sterile syringe with appropriate instillation solution to instillation port • Securely hold ETT with one hand insert catheter to appropriate depth with the other • Apply continuous suction while slowly withdrawing the catheter • Flush catheter by instilling into instillation port while applying suction • Allow pt to re-oxygenate at least 30 sec between passes 55

Post-Suctioning • • • Turn suction control to locked position Remove instillation syringe and cap instillation port Disconnect suction tubing and cap end Reasess pt Document: – Time – Initial assessment – Amount of suctioning required – Amount and type of secretions – Amount and type of instillation – Pt response 56
- Slides: 56