Pediatric Airway Management H HOSSEINI MD Airway anatomy



































- Slides: 88

Pediatric Airway Management H. HOSSEINI MD

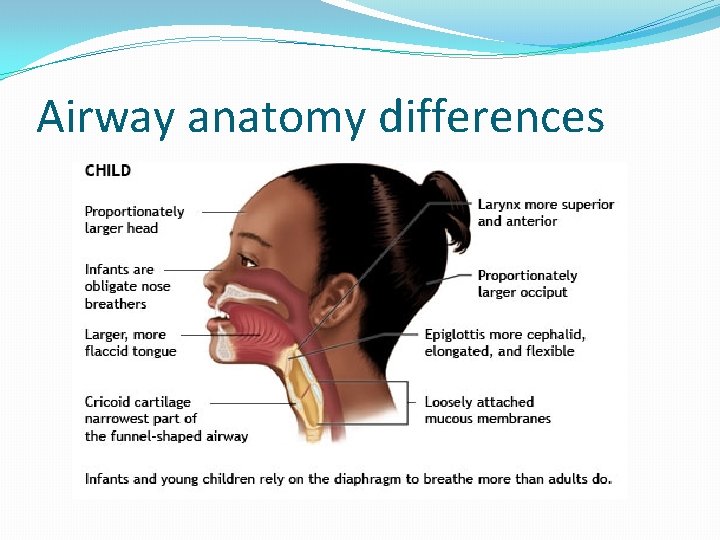
Airway anatomy differences

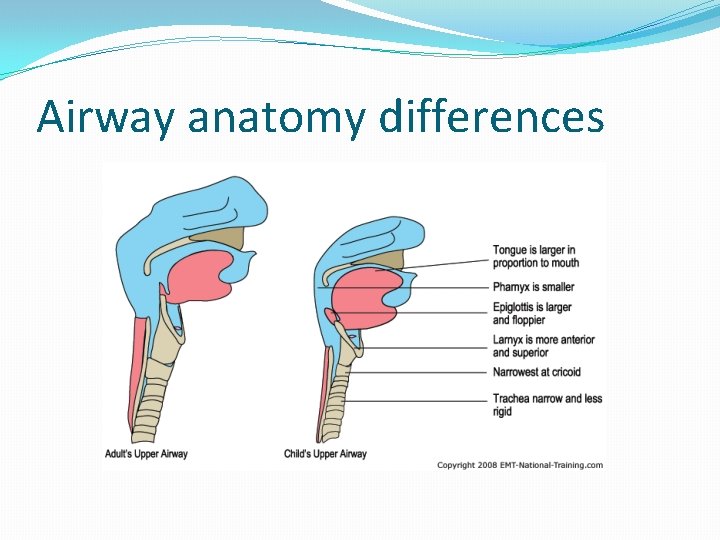
Airway anatomy differences

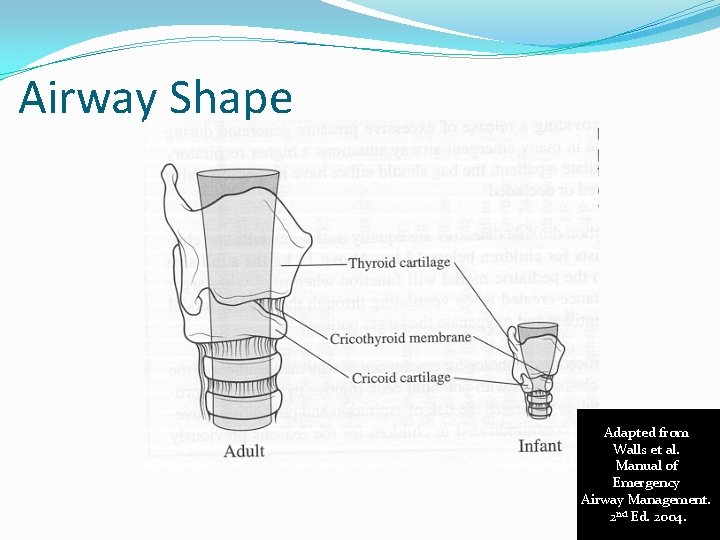
Airway Shape Adapted from Walls et al. Manual of Emergency Airway Management. 2 nd Ed. 2004.

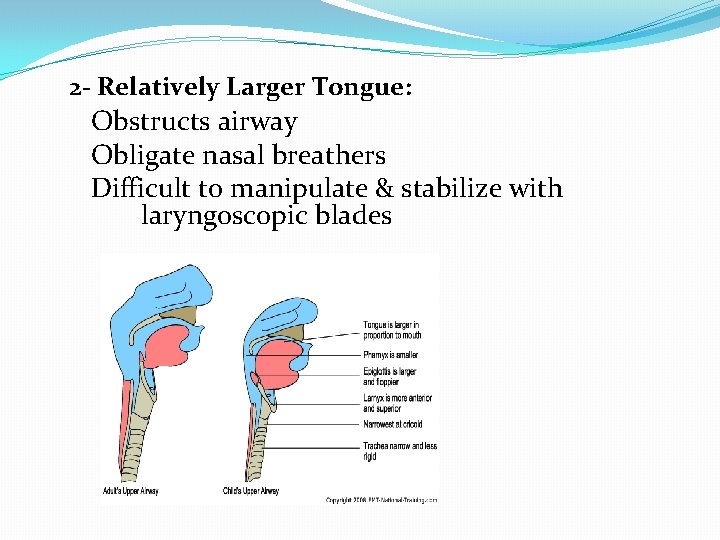
2 - Relatively Larger Tongue: Obstructs airway Obligate nasal breathers Difficult to manipulate & stabilize with laryngoscopic blades

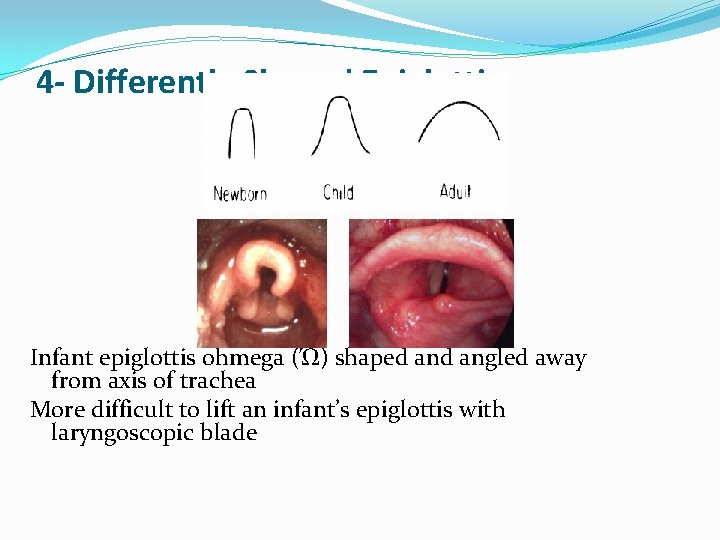
4 - Differently Shaped Epiglottis Infant epiglottis ohmega (Ώ) shaped angled away from axis of trachea More difficult to lift an infant’s epiglottis with laryngoscopic blade

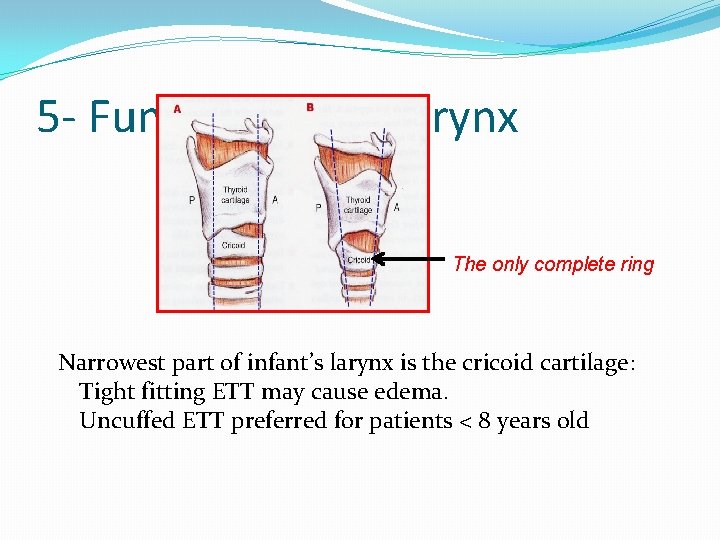
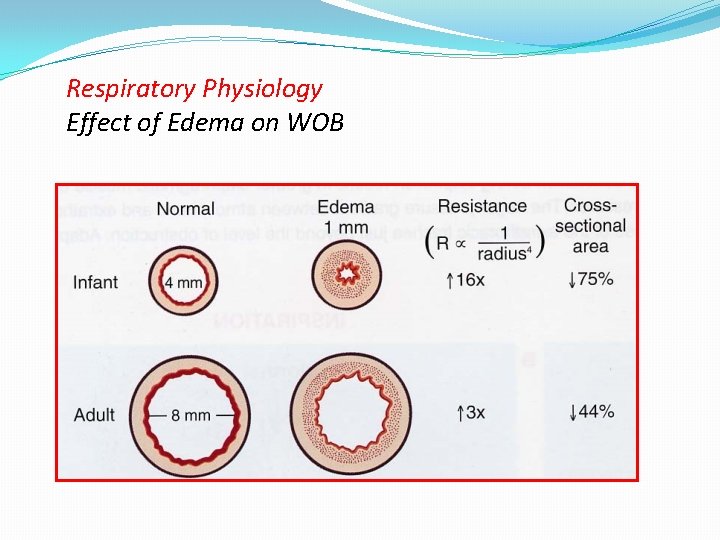
5 - Funnel shaped larynx The only complete ring Narrowest part of infant’s larynx is the cricoid cartilage: Tight fitting ETT may cause edema. Uncuffed ETT preferred for patients < 8 years old


Recently, the concept of the child having a funnelshaped airway with the cricoid as the narrowest portion of the airway has been challenged. Based on bronchoscopic images, Dalal and colleagues (2009) suggest for infants and children the glottis, not the cricoid, may be the narrowest portion.

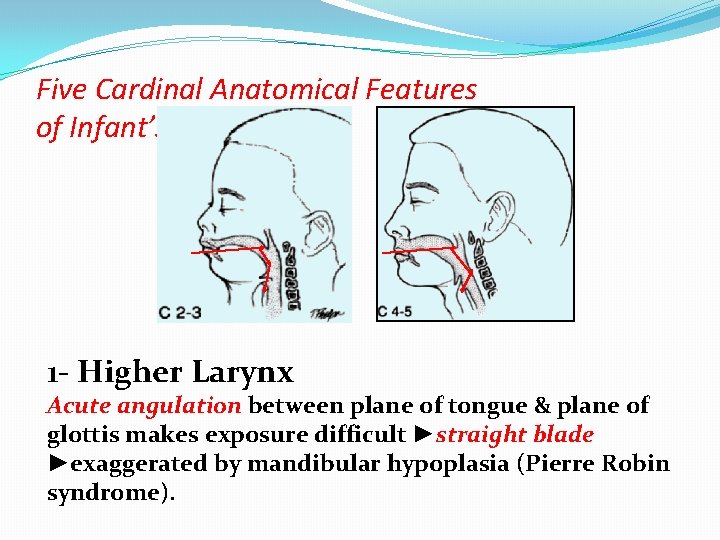
Five Cardinal Anatomical Features of Infant’s Larynx 1 - Higher Larynx Acute angulation between plane of tongue & plane of glottis makes exposure difficult ►straight blade ►exaggerated by mandibular hypoplasia (Pierre Robin syndrome).

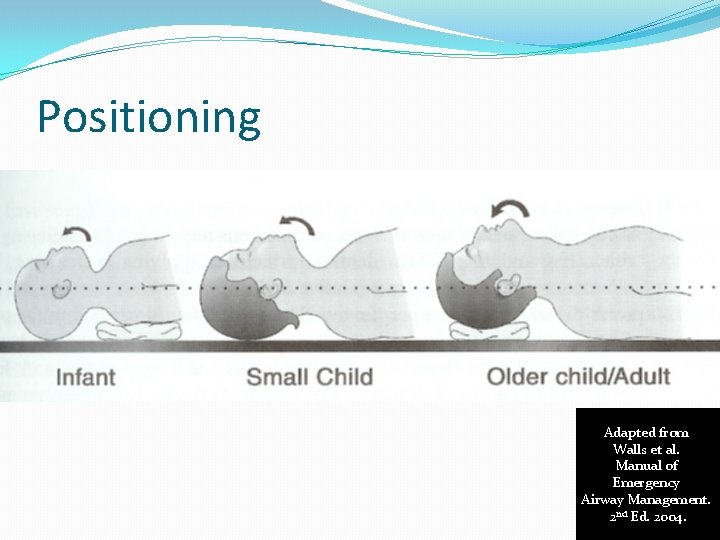
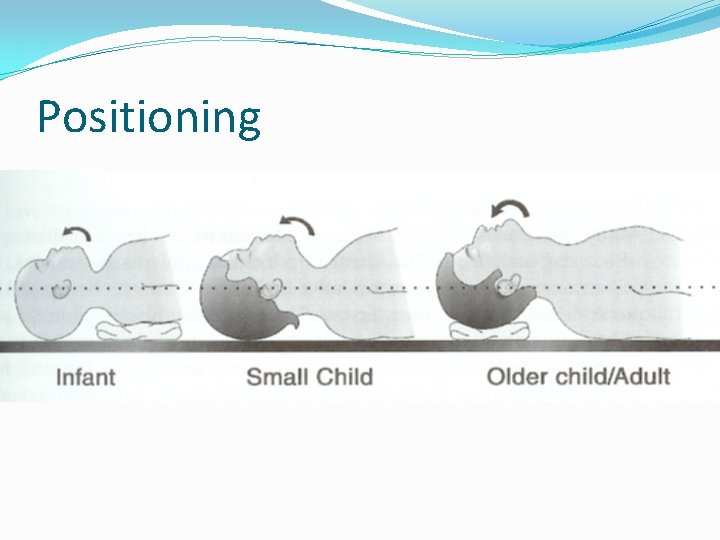
Positioning Adapted from Walls et al. Manual of Emergency Airway Management. 2 nd Ed. 2004.

3 - Anteriorly Angulated Vocal Cords: The anterior attachment of vocal cords are lower than posterior attachment ► difficulty in nasal intubations where “blindly” placed ETT lodges in the anterior commissure rather than in the trachea.

Respiratory Physiology Obligate nasal breathers q Immaturity of coordination between respiratory efforts and oropharyngeal motor/sensory input. q During quiet respiration, the tongue rests against the roof of the mouth.

Respiratory Physiology Respiratory Parameters q High metabolic rate (5 -8 ml/kg/min) q Tidal volume (6 -7 ml/kg/min) q High respiratory rate (40 -60 breaths/min) q High alveolar ventilation (130 ml/kg/min) q Lung compliance is less while chest wall compliance is more than those in adults {reduced FRC and atelectasis} ►PEEP.

Respiratory Physiology Effect of Edema on WOB

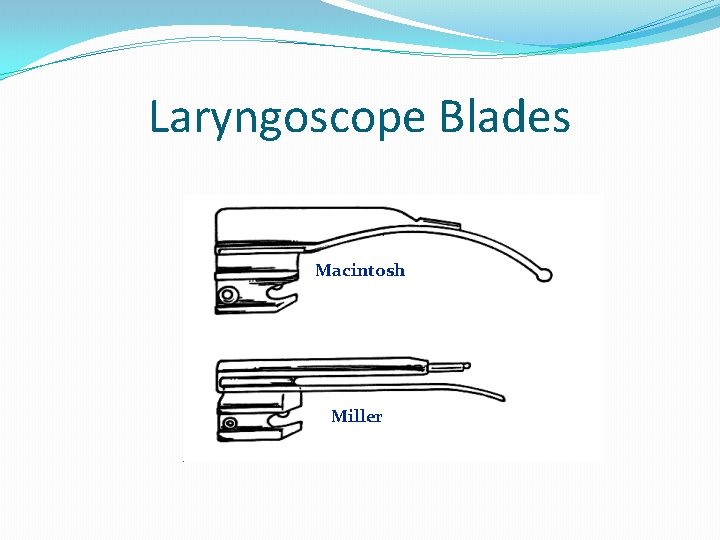
Laryngoscope Blades Macintosh Miller


Using The Miller Blade Better in younger children with a floppy epiglottis Straight Laryngoscope Blade – used to pick up the epiglottis

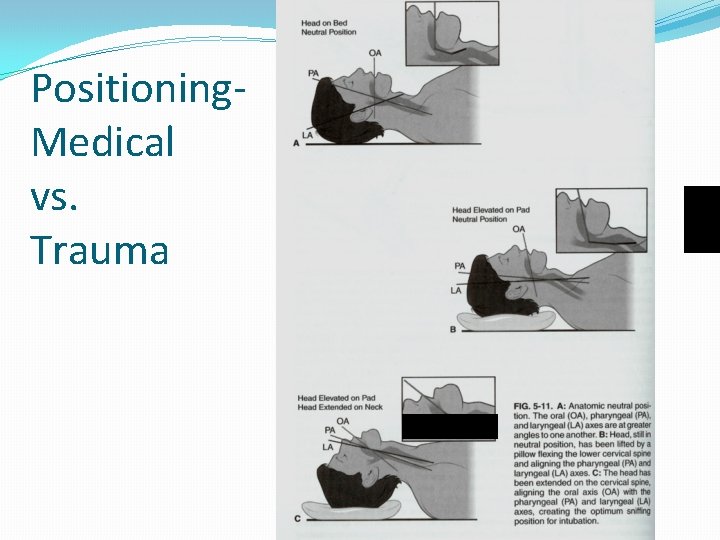
Intubation Positioning �Goal is to align three axes �OA/PA/LA �Medical positioning �Head tilt chin lift �Towels (older = head, younger = shoulders) �Trauma positioning �Manual in-line stabilization

Positioning. Medical vs. Trauma

Positioning

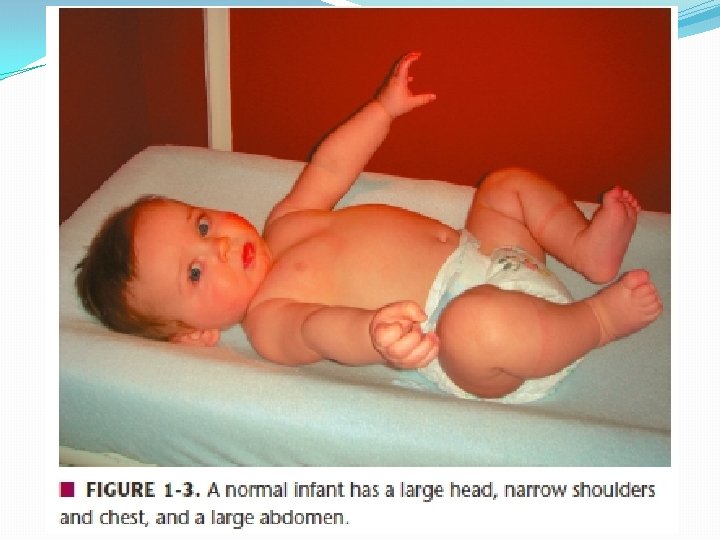
Intubation Approach �Remember, much different than adults �Externally �Larger head/occiput �Head flexes forward and can obstruct �Internally �Larger tongue �Friable tissues �Different angles and shapes

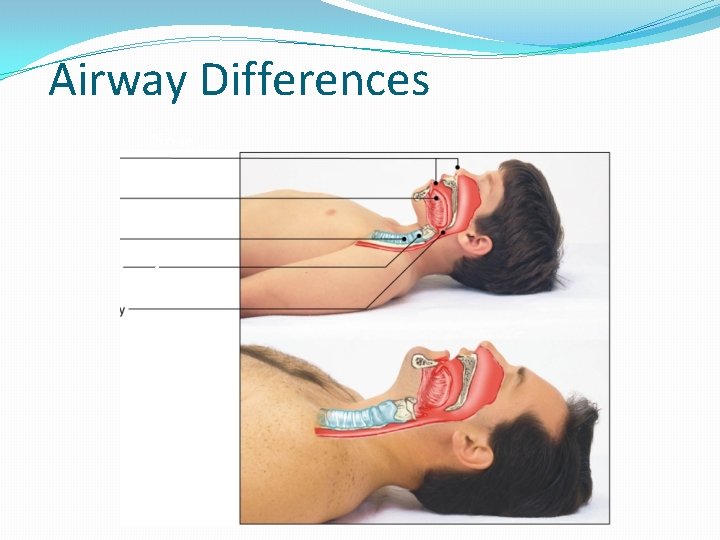
Airway Differences Nose Tongue Trachea Cricoid Airway

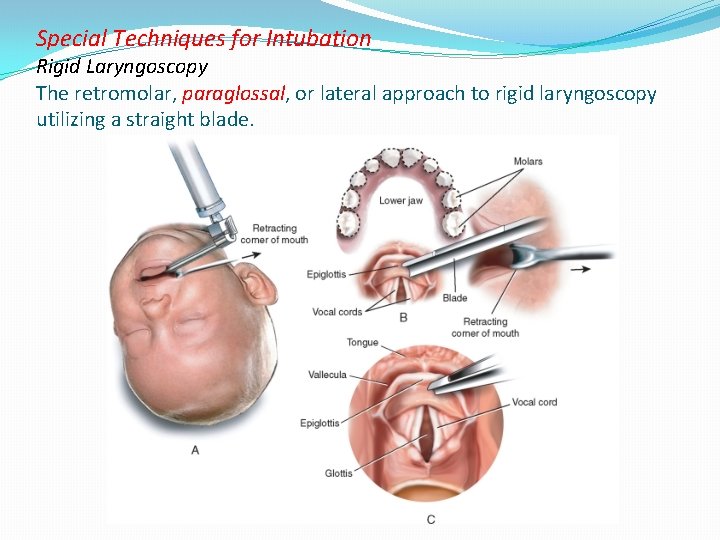
Special Techniques for Intubation Rigid Laryngoscopy The retromolar, paraglossal, or lateral approach to rigid laryngoscopy utilizing a straight blade.

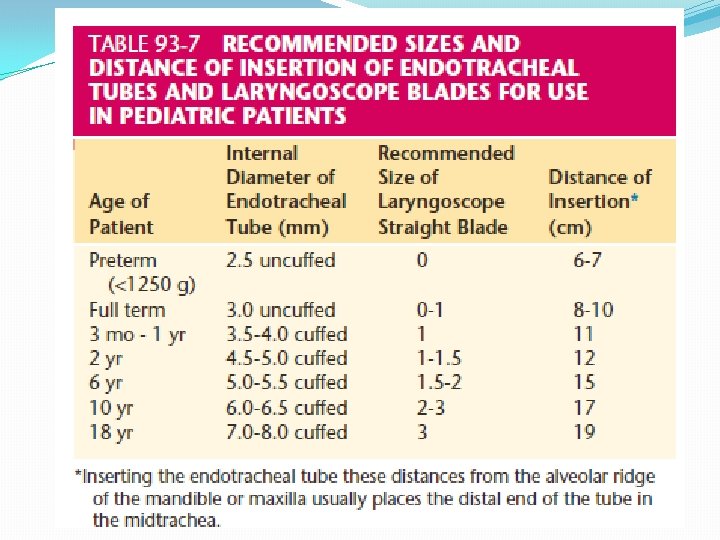
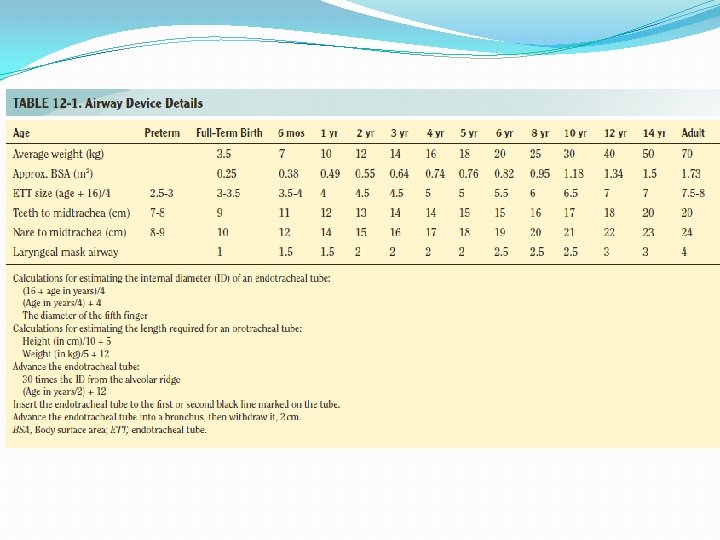
ET Tube sizes �Age kg �Newborn � 3 mos � 1 yr � 2 yrs 3. 5 6. 0 10 12 � Children > 2 years: �ETT size: �ETT depth (lip): ETT Length (lip) 3. 5 9 3. 5 10 4. 0 11 4. 5 12 Age/4 + 4 Age/2 + 12

Equipment choosing �Other methods for choosing ET tubes Uncuffed tubes (in mm): Cuffed tubes: age 4 + 4 Uncuffed size - 0. 5

Tube Placement �ETT depth – use the black line � (Age in years/2) + 12 �ETT internal diameter x 3



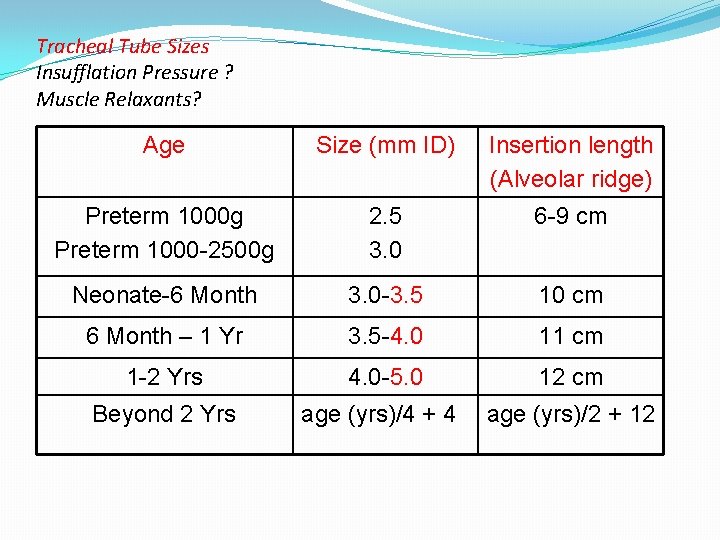
Tracheal Tube Sizes Insufflation Pressure ? Muscle Relaxants? Age Size (mm ID) Insertion length (Alveolar ridge) Preterm 1000 g Preterm 1000 -2500 g 2. 5 3. 0 6 -9 cm Neonate-6 Month 3. 0 -3. 5 10 cm 6 Month – 1 Yr 3. 5 -4. 0 11 cm 1 -2 Yrs 4. 0 -5. 0 12 cm Beyond 2 Yrs age (yrs)/4 + 4 age (yrs)/2 + 12

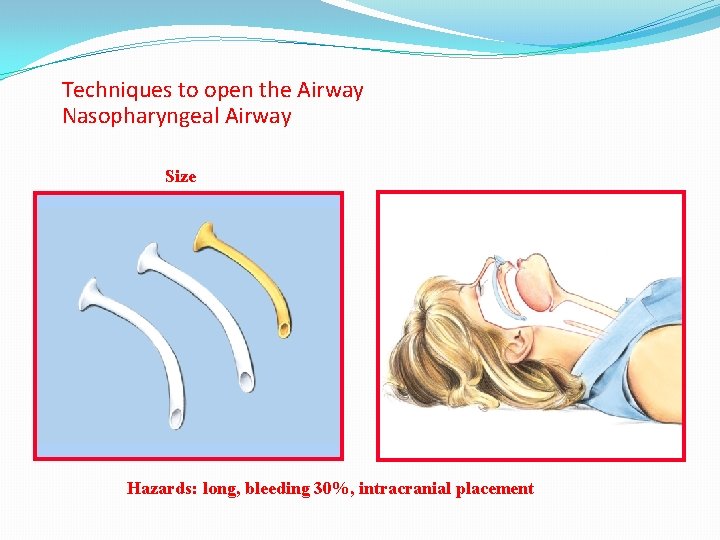
Techniques to open the Airway Nasopharyngeal Airway Size Hazards: long, bleeding 30%, intracranial placement

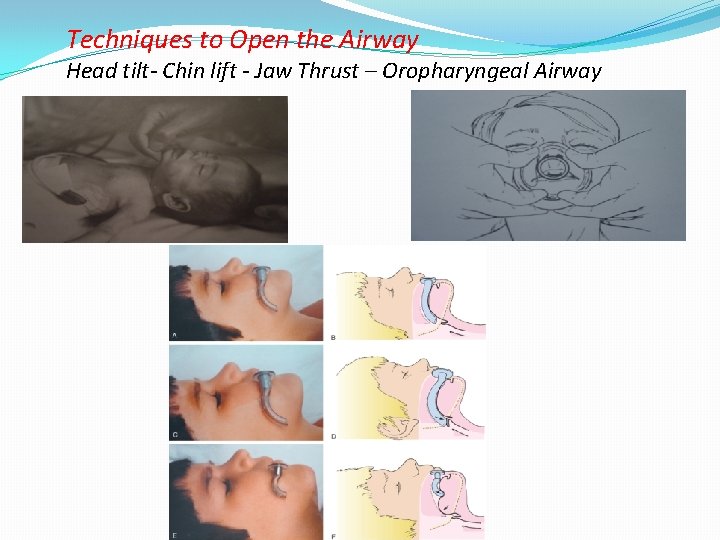
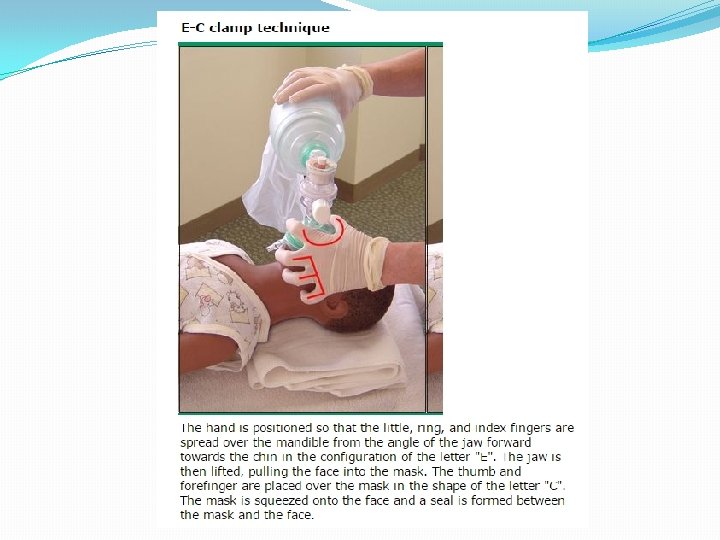
Techniques to Open the Airway Head tilt- Chin lift - Jaw Thrust – Oropharyngeal Airway

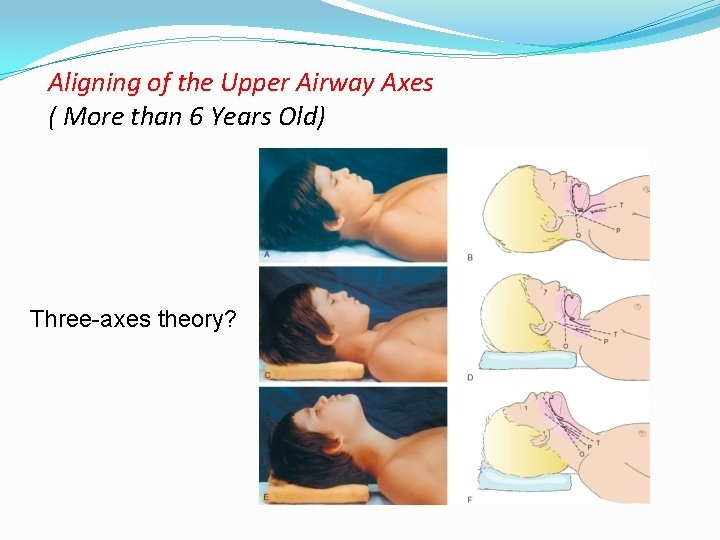
Aligning of the Upper Airway Axes ( More than 6 Years Old) Three-axes theory?

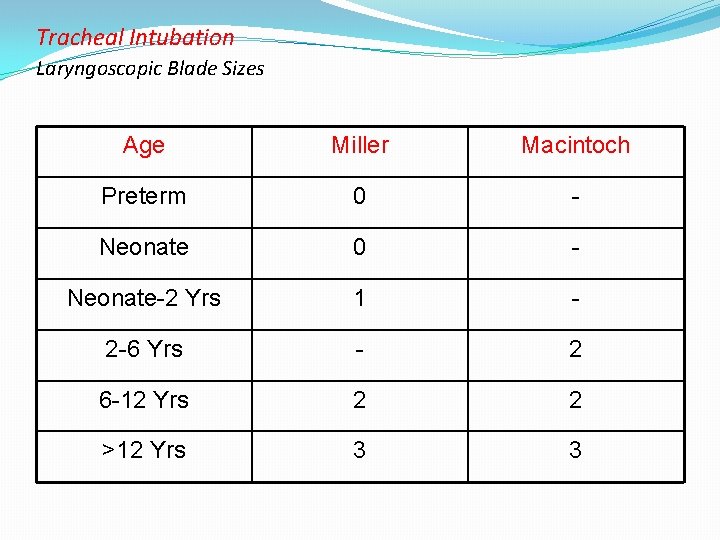
Tracheal Intubation Laryngoscopic Blade Sizes Age Miller Macintoch Preterm 0 - Neonate-2 Yrs 1 - 2 -6 Yrs - 2 6 -12 Yrs 2 2 >12 Yrs 3 3

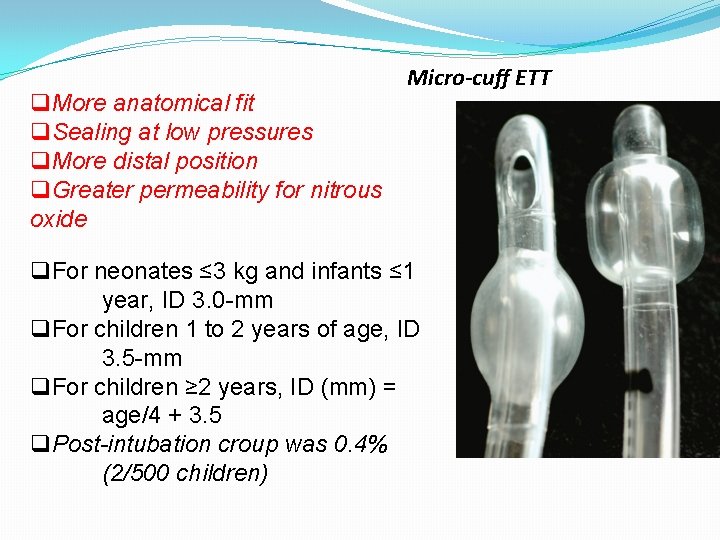
q. More anatomical fit q. Sealing at low pressures q. More distal position q. Greater permeability for nitrous oxide Micro-cuff ETT q. For neonates ≤ 3 kg and infants ≤ 1 year, ID 3. 0 -mm q. For children 1 to 2 years of age, ID 3. 5 -mm q. For children ≥ 2 years, ID (mm) = age/4 + 3. 5 q. Post-intubation croup was 0. 4% (2/500 children)

Endotracheal tubes fabricated without the Murphy eye are known as Magill tubes, whereas those that have this opening are called Murphy tubes. However, there are potential disadvantages to the presence of a Murphy eye on an endotracheal tube, including a tendency for accumulation of secretions and the possibility that a stylet, catheter, or bronchoscope may get stuck, requiring the removal of the entire assembly.

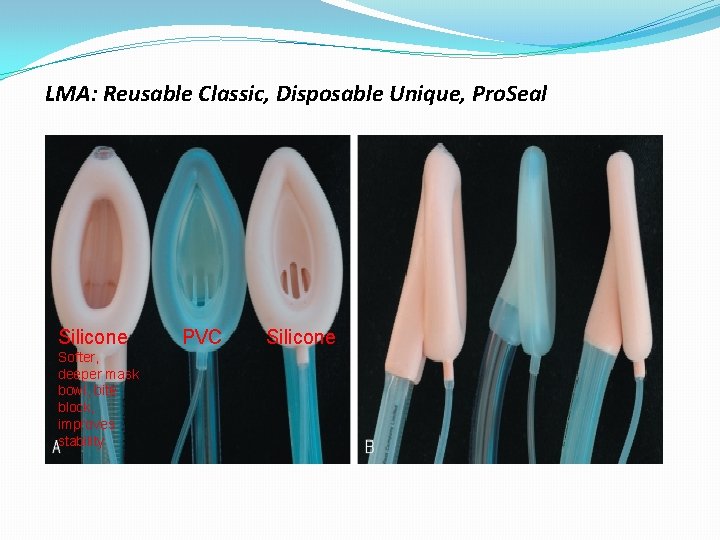
LMA: Reusable Classic, Disposable Unique, Pro. Seal Silicone Softer, deeper mask bowl, bite block, improves stability PVC Silicone


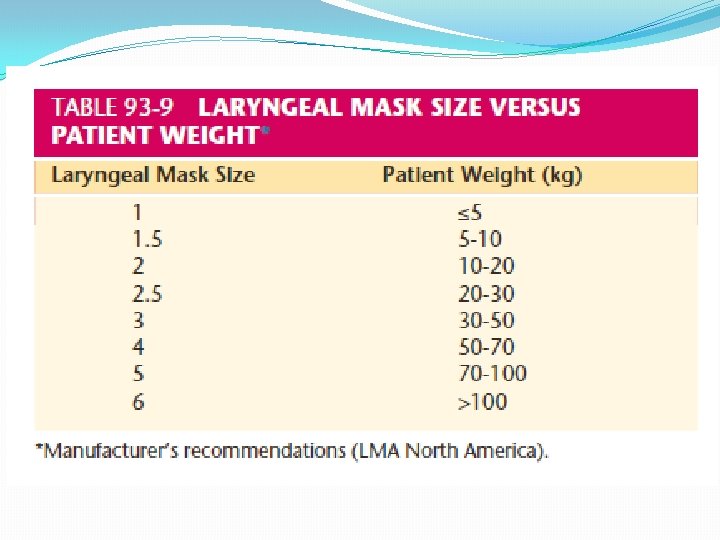
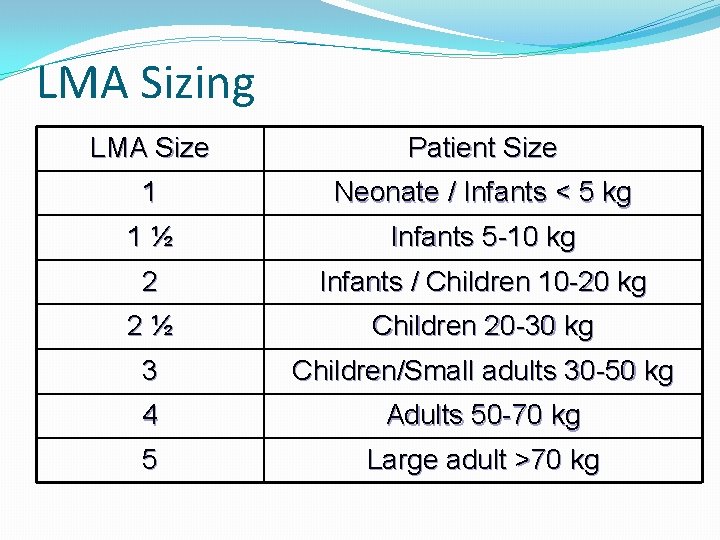
LMA Sizing LMA Size Patient Size 1 Neonate / Infants < 5 kg 1½ Infants 5 -10 kg 2 Infants / Children 10 -20 kg 2½ Children 20 -30 kg 3 Children/Small adults 30 -50 kg 4 Adults 50 -70 kg 5 Large adult >70 kg

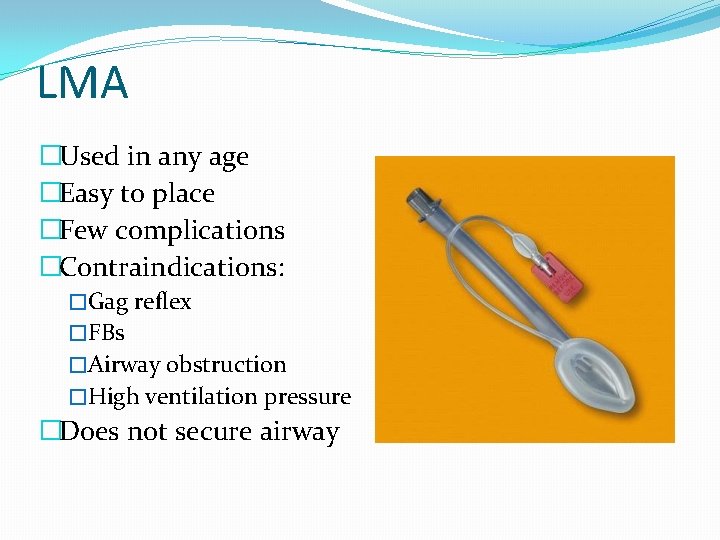
LMA �Used in any age �Easy to place �Few complications �Contraindications: �Gag reflex �FBs �Airway obstruction �High ventilation pressure �Does not secure airway


Following its blind passage through the oral cavity, the proper seating of an LMA is generally heralded by a slight rise of the device when the mask’s cushion is inflated with air. Care should be taken to use the minimal effective inflation pressure for the cuff, typically up to 60 cm. H 2 O. The routine use of a manometer is advocated

The more cephalad anterior position of the larynx of a child as compared with an adult has prompted the use of an alternate insertion technique in children. In this case, the LMA is inserted with its cushion placed against the hard palate. The device is then rotated through 180 degrees until the cushion is seated at the laryngeal inlet. This method for the insertion of an LMA appears to be especially useful in preschool and young school-age children.

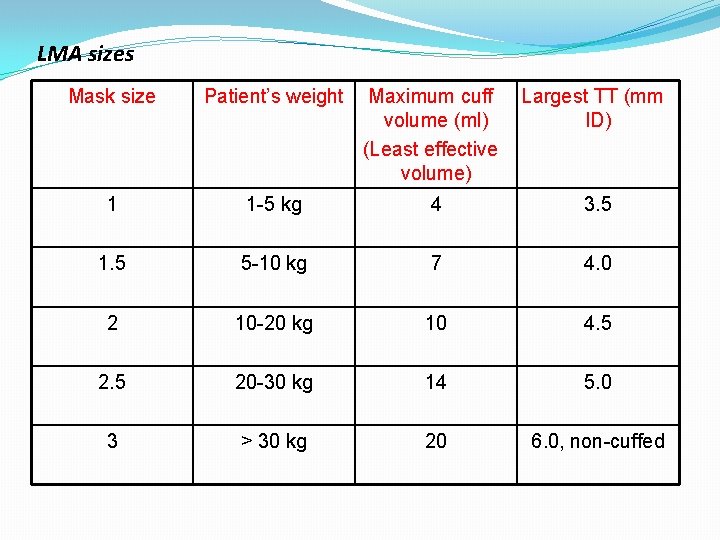
LMA sizes Mask size Patient’s weight Maximum cuff volume (ml) (Least effective volume) Largest TT (mm ID) 1 1 -5 kg 4 3. 5 1. 5 5 -10 kg 7 4. 0 2 10 -20 kg 10 4. 5 20 -30 kg 14 5. 0 3 > 30 kg 20 6. 0, non-cuffed


Causes of Difficult Airway Congenital Anomalies Tumors Infection Musculoskeletal Problems

q Loose or missing teeth. q Size and configuration of palate. q Size and configuration of mandible (side view). q Location of larynx in relation to the mandible. q Presence of inspiratory stridor : epiglottitis, croup, extrathoracic foreign body. q Both inspiratory and expiratory stridor: aspirated foreign body, vascular ring, or large esophageal foreign body. q Prolonged expiration: lower airway disease? q Baseline oxygen saturation in room air.

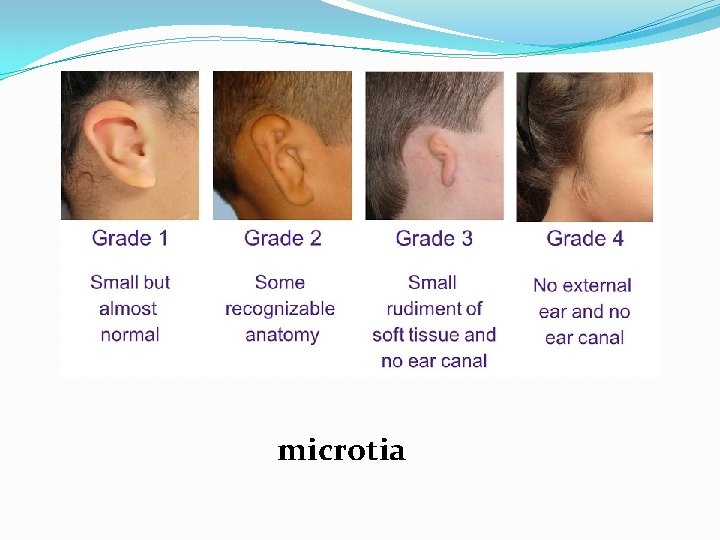
q Bilateral microtia (ear deformity easily notable) is associated with mandibular hypoplasia & difficulty in visualizing the laryngeal inlet (42%) & with unilateral microtia (2. 5%). q Are there congenital anomalies that may fit a recognizable syndrome? The finding of one anomaly mandates a search for others.

microtia

q. Musculoskeletal Problems Ankylosis of jaw, cervical spine Unstable or dislocated cervical vertebrae Wired jaw Cervical cord tumor Halo traction apparatus Facial trauma, fractures, laceration, burns

Evaluation of the Upper Airway (Diagnostic Testing) q X-ray, MRI and CT. Radiologic airway examination in a child with a compromised airway must be undertaken only when there is no immediate threat to the child's safety and only in the presence of skilled and appropriately equipped personnel able to manage the airway. q Endoscopic evaluation (flexible fiberoptic endoscopy) q Arterial blood gas analysis (chronic airway obstruction with respiratory acidosis)

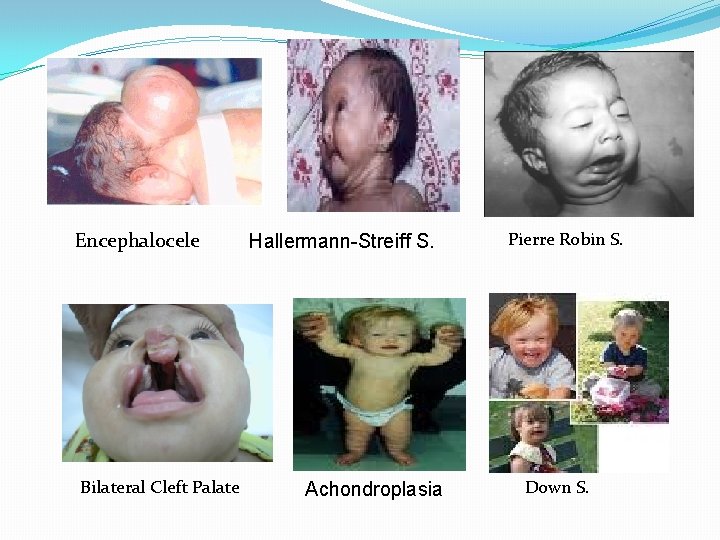
Encephalocele Bilateral Cleft Palate Hallermann-Streiff S. Achondroplasia Pierre Robin S. Down S.

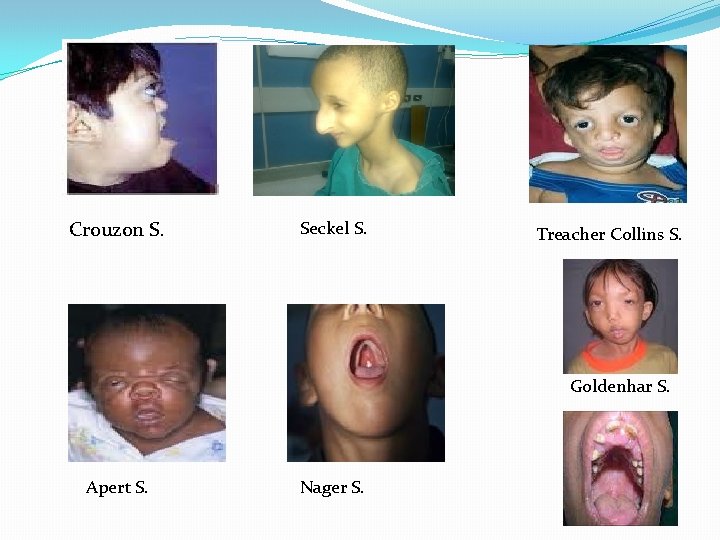
Crouzon S. Seckel S. Treacher Collins S. Goldenhar S. Apert S. Nager S.

Mucopolysaccaridosis Type IH (Hurler) Type 1 H/S (Hurler-Scheie) Type II Hunter Type III (Sanfilippo)

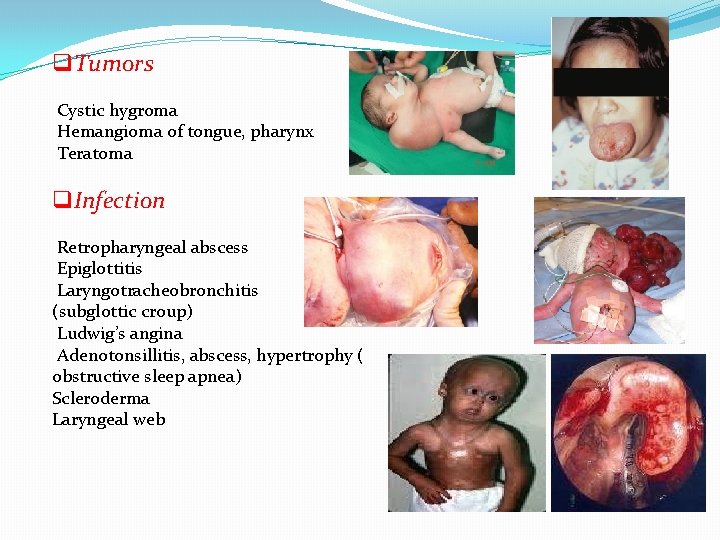
q. Tumors Cystic hygroma Hemangioma of tongue, pharynx Teratoma q. Infection Retropharyngeal abscess Epiglottitis Laryngotracheobronchitis (subglottic croup) Ludwig’s angina Adenotonsillitis, abscess, hypertrophy ( obstructive sleep apnea) Scleroderma Laryngeal web


I-LMA �Only sizes 3, 4, 5 �Same rules and sizing as LMA �Need special armored tube for intubation �New similar devices exist �Leave LMA portion in place in field

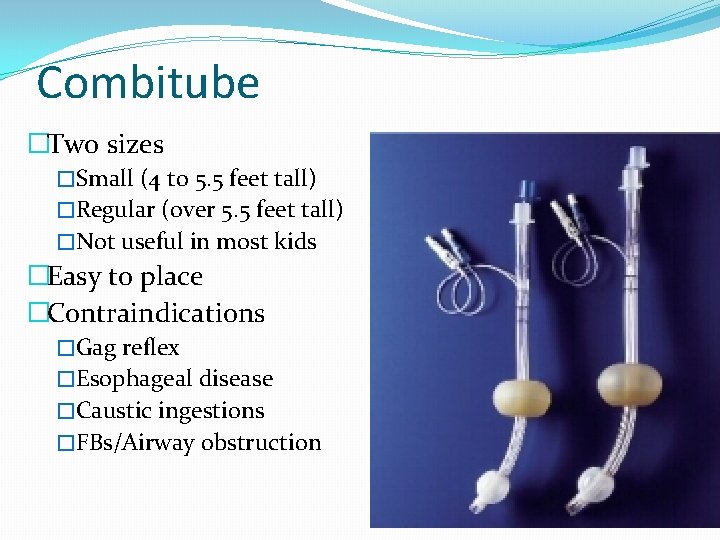
Combitube �Two sizes �Small (4 to 5. 5 feet tall) �Regular (over 5. 5 feet tall) �Not useful in most kids �Easy to place �Contraindications �Gag reflex �Esophageal disease �Caustic ingestions �FBs/Airway obstruction





Bougie �Replaces stylet �Able to use with poor view �Feel tracheal rings �Feel carina �Intubate over it �Keep blade in place �Two person technique �Need to practice

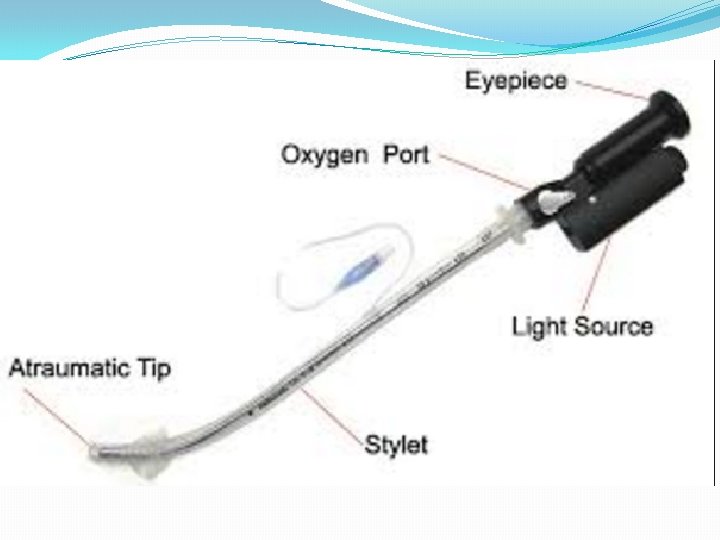
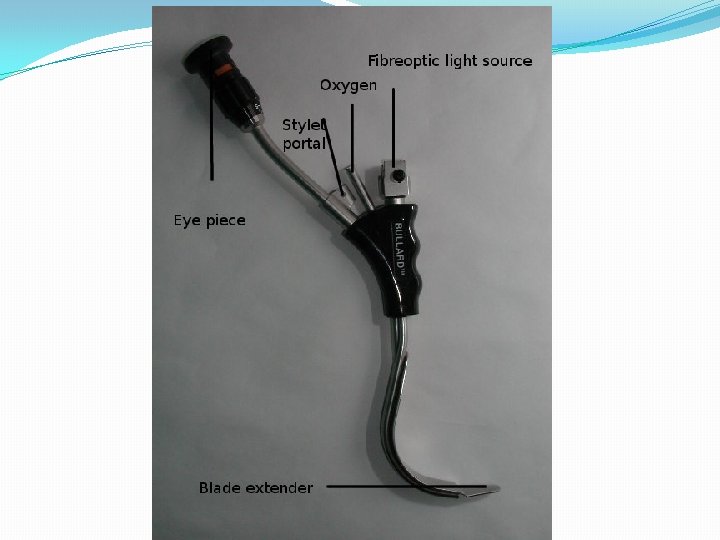
Other Toys �Lighted stylet �Flexible fiberoptic scopes �Rigid fiberoptic scopes �Bullard �Shikani �Video laryngoscopy



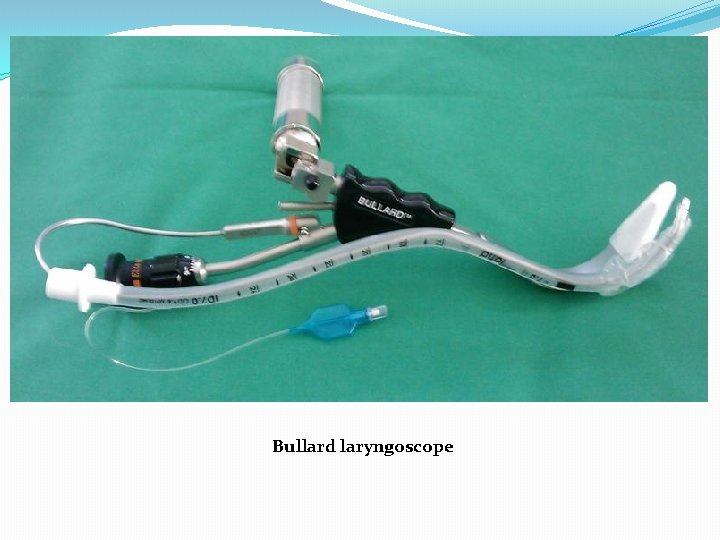
Bullard laryngoscope

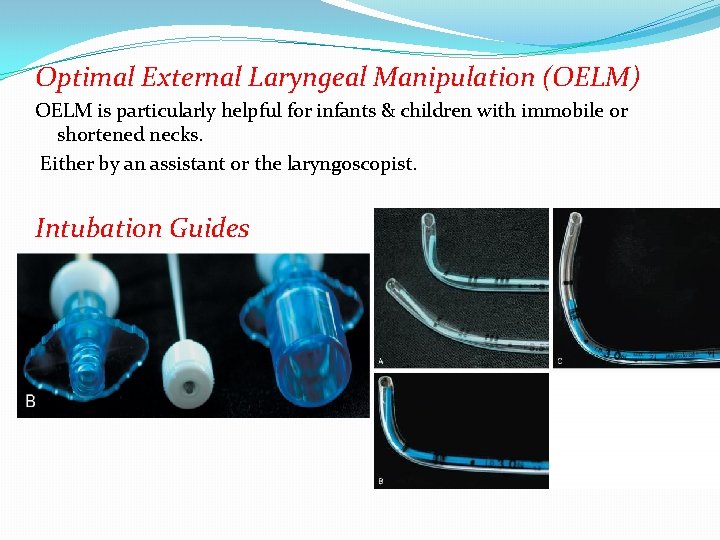
Optimal External Laryngeal Manipulation (OELM) OELM is particularly helpful for infants & children with immobile or shortened necks. Either by an assistant or the laryngoscopist. Intubation Guides

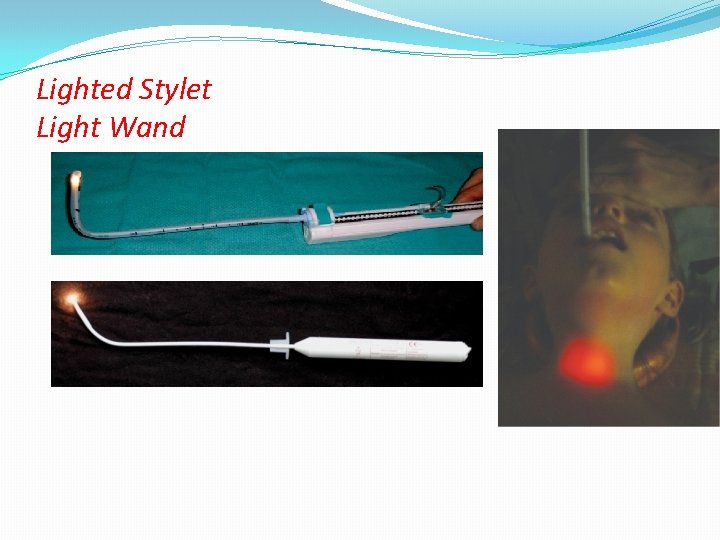
Lighted Stylet Light Wand


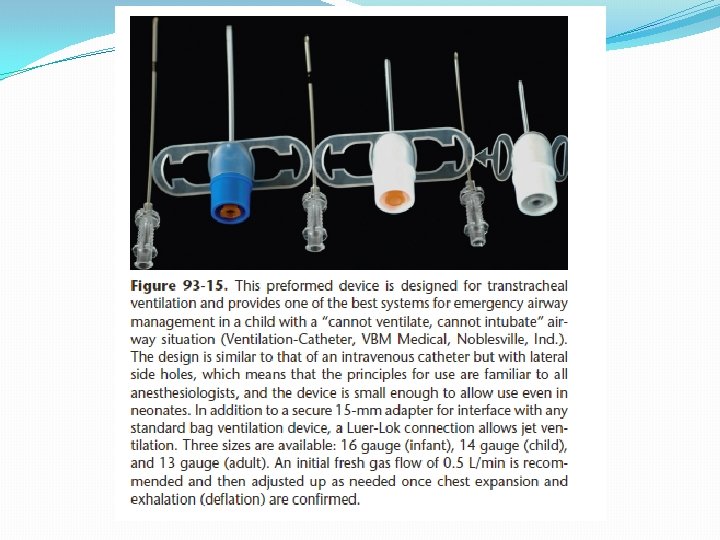
TTJV

Glidescope Video Laryngoscope

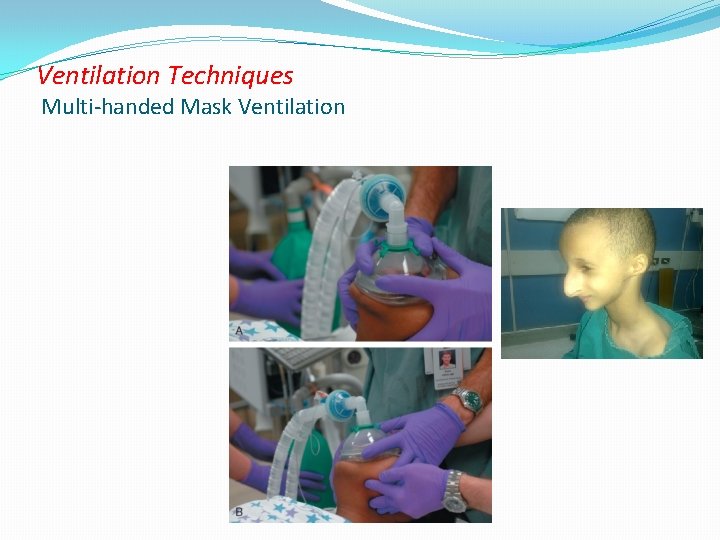
Ventilation Techniques Multi-handed Mask Ventilation


Intubation through LMA (Blind)

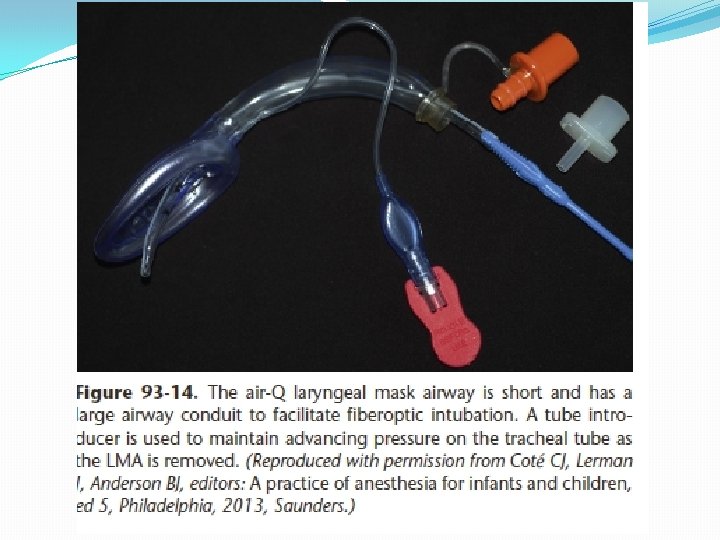
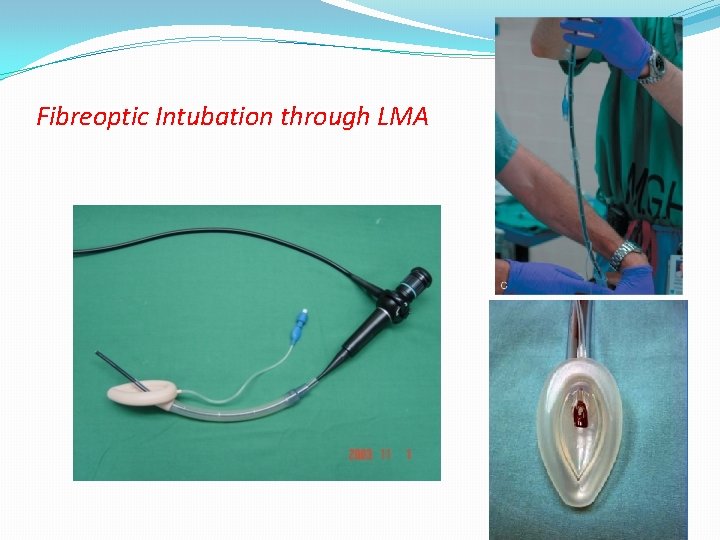
Fibreoptic Intubation through LMA

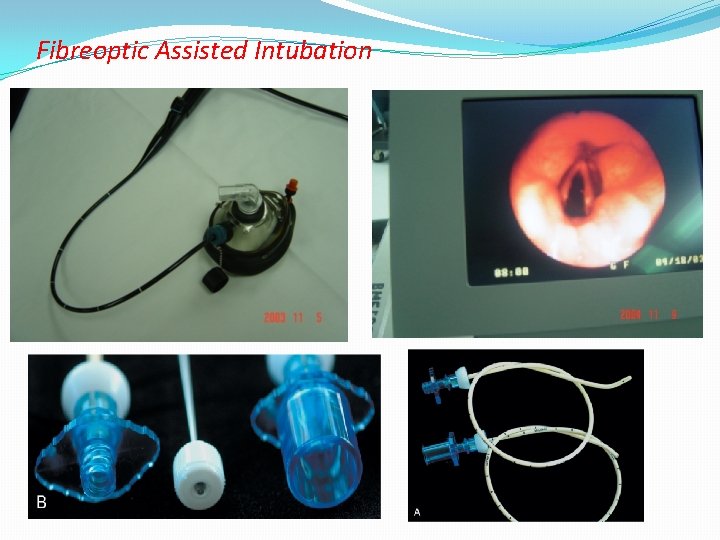
Fibreoptic Assisted Intubation

Surgical Airways Cricothyrotomy �Indications (only if >10 years old) �Failed airway �Failed ventilation �Predictors of difficulty �Previous neck surgery �Obesity �Hematoma or infection

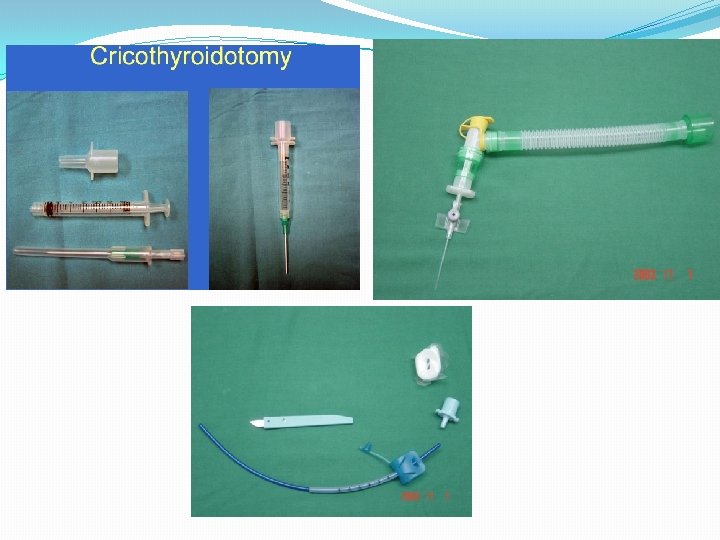
Cricothyrotomy Techniques Open �Locate CTM �Stabilize larynx/prep �Incise skin �Vertical �Horizontal through CTM �Insert spacer/dilator �Insert cuffed tube �Check breath sounds Closed �Locate CTM �Stabilize larynx/prep �Insert needle �Direct inferiorly �Insert guidewire �Remove needle �Small skin incision �Insert dilators/UC tube �Check breath sounds

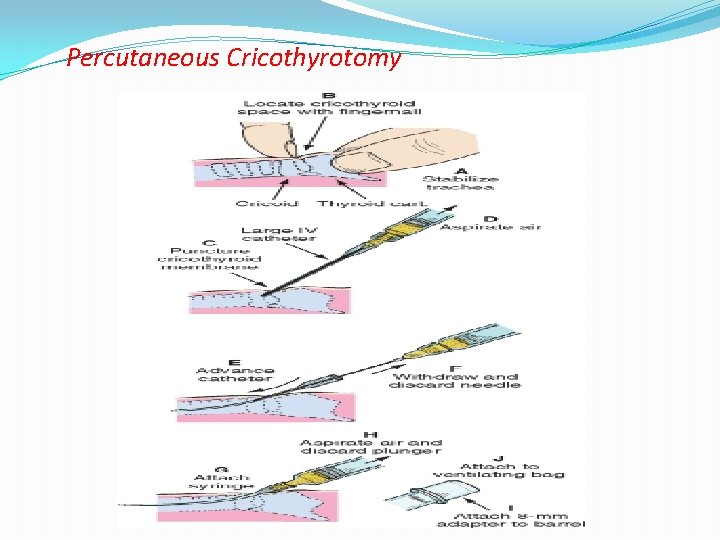
Percutaneous Cricothyrotomy


q. Percutaneous needle cricothyrotomy provides only a mean for oxygen insufflation and does not reliably provide adequate ventilation. q. If glottic or subglottic pathology is not suspected, LMA placement to establish ventilation may be appropriately attempted first.

Cricothyrotomy Complications �Bleeding �Laryngeal or tracheal injury �Infection �Pneumomediastinum �Subglottic stenosis

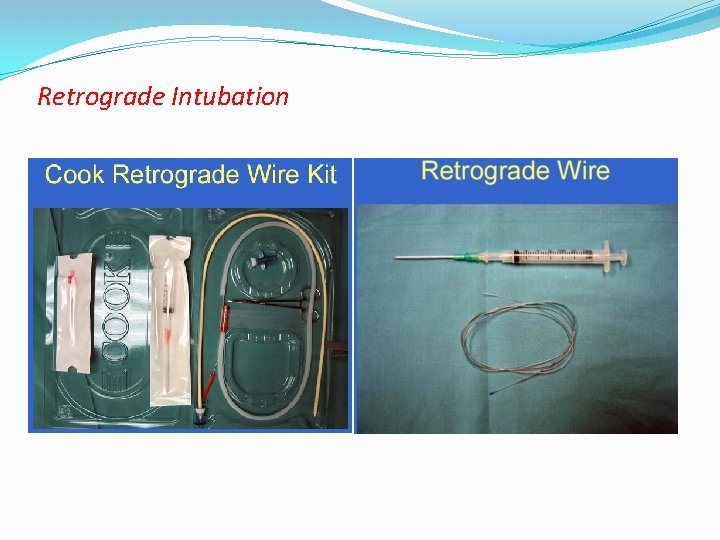
Retrograde Intubation

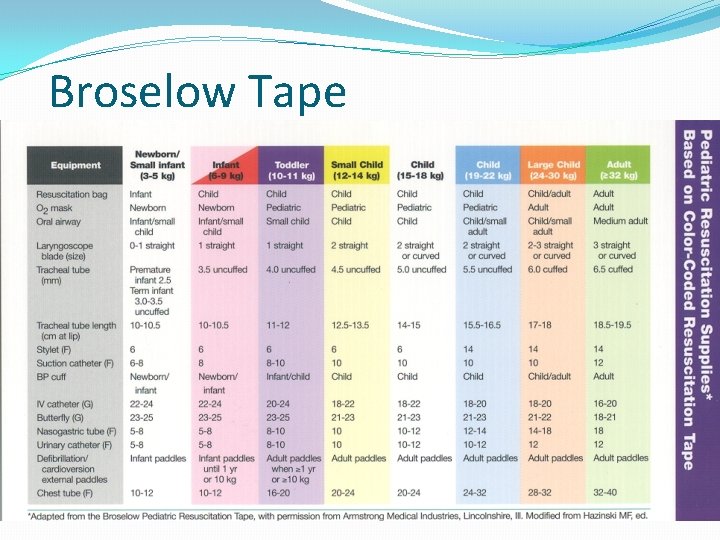
Broselow Tape � 8 color codes (6 -36 kg) �Broselow-Luten Emergency System �Color-coded bags with equip �Quicker, more efficient

Broselow Tape �Equipment sizes �Airway adjuncts �Intubation equip �Oxygen delivery �Vascular access �Defibrillation �NGT, suction caths �BP cuff �Chest tubes �Foley �Medications �Antiarrhythmics �Arrest medications �Anticonvulsants �Overdose meds �Increased ICP meds �Induction agents �Paralytics �Vasopressors �IV drips

Broselow Tape

THANK YOU