PEDIATRIC ACUTE KIDNEY INJURY Sunee Panombualert M D

PEDIATRIC ACUTE KIDNEY INJURY Sunee Panombualert, M. D. Department of Peditric, Faculty of Medicine, Khon Kaen University, Thailand

Outline 1. Diagnosis and definitions of AKI 2. Evaluation of causes of AKI 3. Management of AKI Fluid resuscitate Blood pressure management Diuretics Nutrition Renal replacement therapy
Acute kidney injury (AKI) Previously called acute renal failure Rapid (over hours to days) and usually reversible decline in GFR Acute, impairment of kidney function, manifest by changes in urine output and blood chemistries, portend serious clinical consequences

AKI definitions AKI is defined as any of the following: Increase in SCr by > 0. 3 mg/dl within 48 hours or Increase in SCr to > 1. 5 times baseline, which is known or presumed to have occurred within the prior 7 days or Urine volume < 0. 5 ml/kg/h for 6 hours.
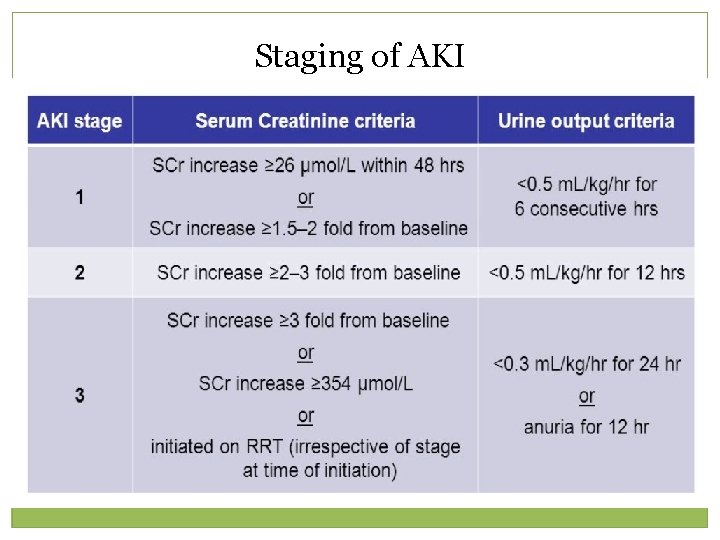
Staging of AKI
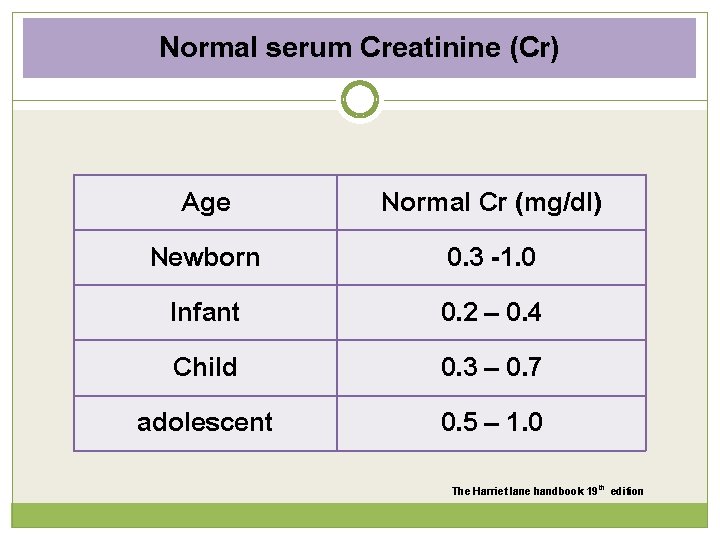
Normal serum Creatinine (Cr) Age Newborn Infant Child adolescent Normal Cr (mg/dl) 0. 3 -1. 0 0. 2 – 0. 4 0. 3 – 0. 7 0. 5 – 1. 0 The Harriet lane handbook 19 th edition

ESTIMATED CREATININE CLEARANCE e. GFR / e. Cr. Cl = (ml/min/1. 73 m 2) 0. 413 x Ht (cm) Cr (mg/dl) Pediatrics 1976; 58: 259 -263. J Am Soc Nephrol 2009; 20: 629 -637.

Evaluation of Kidney Function in the Acute Care Setting Case: You are asked to see a 5 -year-old boy with PUV and known chronic kidney disease (CKD; baseline Scr 2. 0 mg/d. L) who is admitted with urosepsis. Admission Scr concentration was 2. 3 mg/d. L and increased to 2. 6 mg/d. L the following day. Question 1: Which statement regarding his kidney function is correct? a) Using the MDRD (Modification of Diet in Renal Disease) Study equation, his estimated GFR (e. GFR) is 34 m. L/min/ 1. 73 m 2 b) Use of the CKD-EPI (CKD Epidemiology Collaboration) equation is more appropriate for this patient, and his e. GFR is 32 m. L/min/1. 73 m 2 c) Using the Cockcroft-Gault formula, his creatinine clearance is 20 to 32 m. L/min d) His e. GFR cannot be calculated because his Scr concentration is not stable
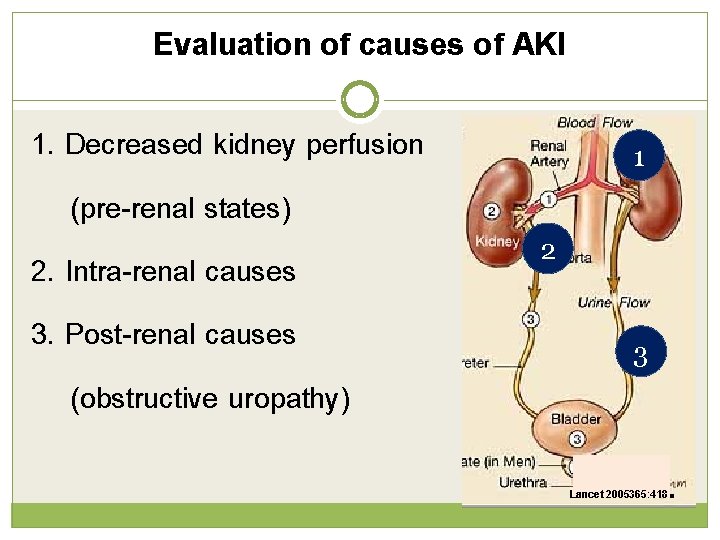
Evaluation of causes of AKI 1. Decreased kidney perfusion (pre-renal states) 2. Intra-renal causes 3. Post-renal causes (obstructive uropathy) 1 2 3 Lancet 2005365: 418 .
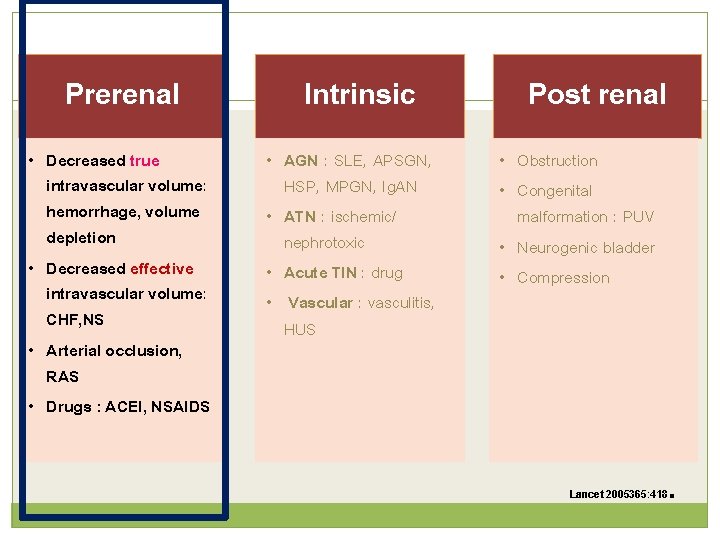

Prerenal • Decreased true intravascular volume: hemorrhage, volume depletion • Decreased effective intravascular volume: CHF, NS • Arterial occlusion, RAS • Drugs : ACEI, NSAIDS Intrinsic • AGN : SLE, APSGN, HSP, MPGN, Ig. AN • ATN : ischemic/ nephrotoxic • Acute TIN : drug • Vascular : vasculitis, HUS Post renal • Obstruction • Congenital malformation : PUV • Neurogenic bladder • Compression Lancet 2005365: 418 .
Decreased kidney perfusion (pre-renal states) Hypovolemia : Increased losses (hemorrhage, burns, massive vomiting or diarrhea), poor oral intake Reduced cardiac output : Heart failure, cardiac tamponade, massive pulmonary embolism Renal vasomodulation/shunting : Medications (NSAID, ACEi/ARB, cyclosporine, iodinated contrast), hypercalcemia, hepatorenal syndrome, abdominal compartment syndrome Systemic vasodilation : Sepsis, SIRS, hepatorenal syndrome
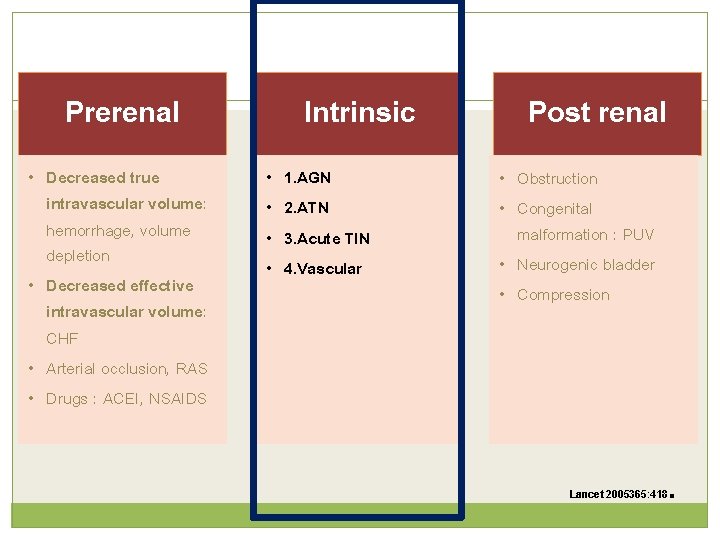

Prerenal • Decreased true intravascular volume: hemorrhage, volume depletion • Decreased effective intravascular volume: CHF • Arterial occlusion, RAS • Drugs : ACEI, NSAIDS Intrinsic • • 1. AGN 2. ATN 3. Acute TIN 4. Vascular Post renal • Obstruction • Congenital malformation : PUV • Neurogenic bladder • Compression Lancet 2005365: 418 .

Intra-renal causes Glomerular: Rapidly progressive (crescentic) GN: anti–glomerular basement membrane immune complex diseases: Ig. A nephropathy, postinfectious, lupus, mixed cryoglobuminemia with MPGN pauciimmuneglomerulonephritis: ANCAassociatedvasculitides: GPA, MPA, EGPA(Churg-Strauss) ANCA-negative nephrotic-range proteinuria with associated AKI: HIV-associated nephropathy (secondary FSGS) Other causes of nephrotic-range proteinuria that commonly associate with AKI: minimalchangediseasewith. ATN/AIN Membranous nephropathy+crescentic. GNorrenal vein thrombosis; myeloma +multiple different pathologies, but in particular light chain cast nephropathy
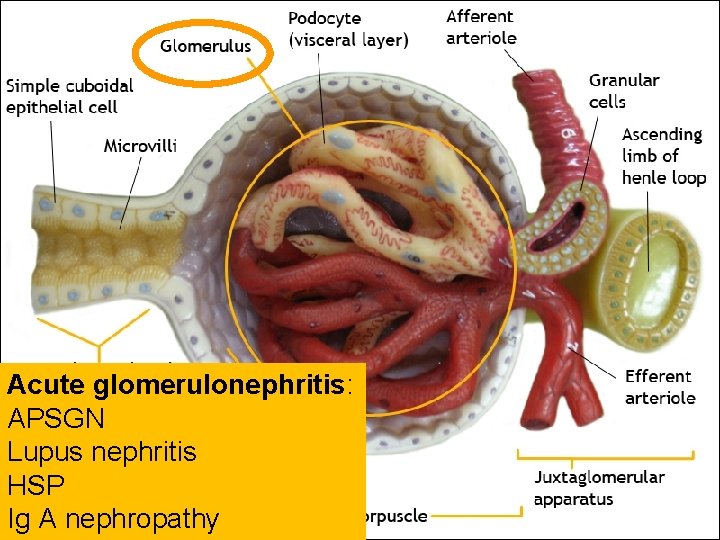
Acute glomerulonephritis: APSGN Lupus nephritis HSP Ig A nephropathy

Tubulo-interstitium AIN: medications, infection, lymphoproliferative disease Pigment nephropathy: rhabdomyolysis (myoglobin), massive hemolysis (hemoglobin) Crystal nephropathy: uric acid (tumor lysis), acyclovir, sulfonamides, protease inhibitors (indinavir, azatanavir), methotrexate, ethylene glycol, acute phosphate nephropathy, oxalate nephropathy, myelomaassociated AKI (cast nephropathy) ATN: ischemia (shock, sepsis), inflammatory (sepsis, burns), medications Osmotic nephrosis in setting of sucrose, mannitol and hydroxyethyl starch use
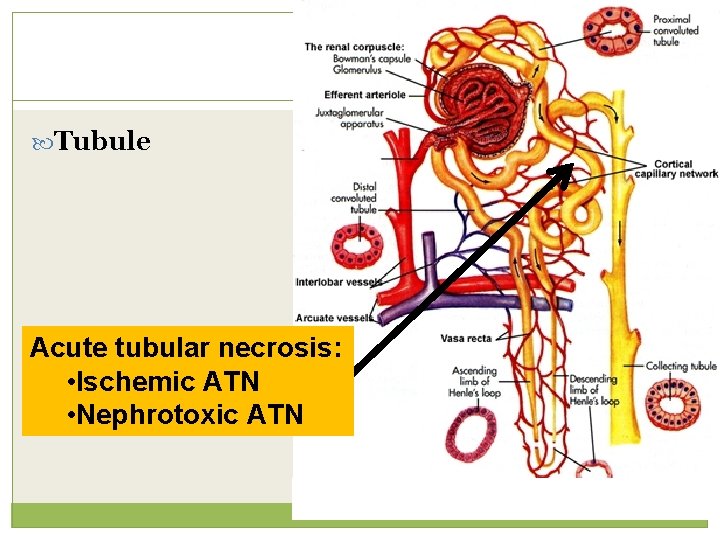
Tubule Acute tubular necrosis: • Ischemic ATN • Nephrotoxic ATN
Intrinsic renal disease Acute tubular necrosis Ischemic ATN : shock, post cardiac arrest, severe hypoxia, prolong dehydration Nephrotoxic ATN: Exogenous : antibiotic, radio contrast agents, cisplatin, heavy metals Endogenous : Intratubular pigment: hemoglobin, myoglobin Intratubular crystals: uric acid, oxalate Lancet 2005365: 418 .

Medications Commonly Associated With ATN Aminoglycosides (tobramycin, gentamycin) NSAIDs (ibuprofen, naproxen, celecoxib) ACEI (captopril, lisinopril, benazepril, ramipril) ARB (losartan, valsartan, candesartan, irbesartan) Amphotericin Cisplatin Foscarnet Iodinated contrast Pentamidine Tenofovir Zolendronic acid
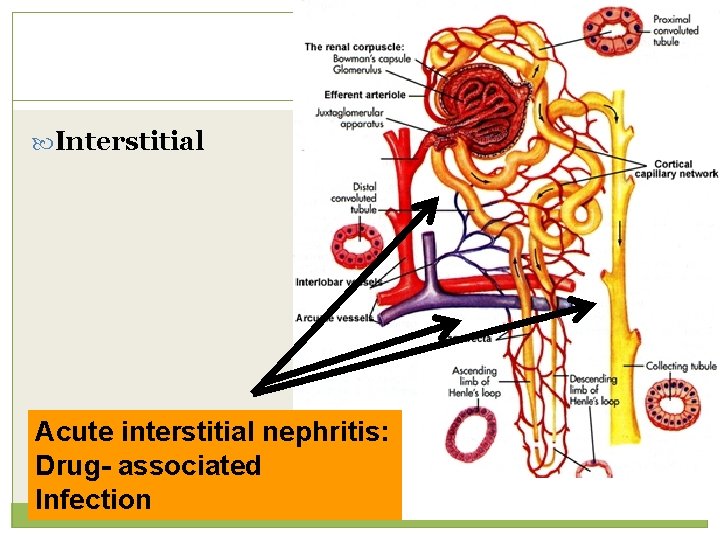
Interstitial Acute interstitial nephritis: Drug- associated Infection
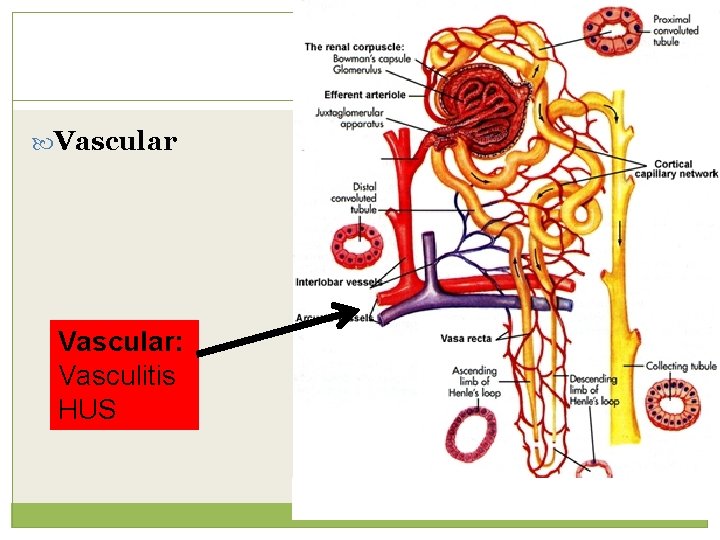
Vascular: Vasculitis HUS

Intra-renal causes Vascular: Renal artery stenosis, arterial/venous cross- clamping Microvascular: Thrombotic microangiopathies (TTP, HUS, a. HUS, DIC, APS, malignant hypertension, scleroderma renal crisis, preeclampsia/HELLP syndrome, drug-induced), cholesterol emboli
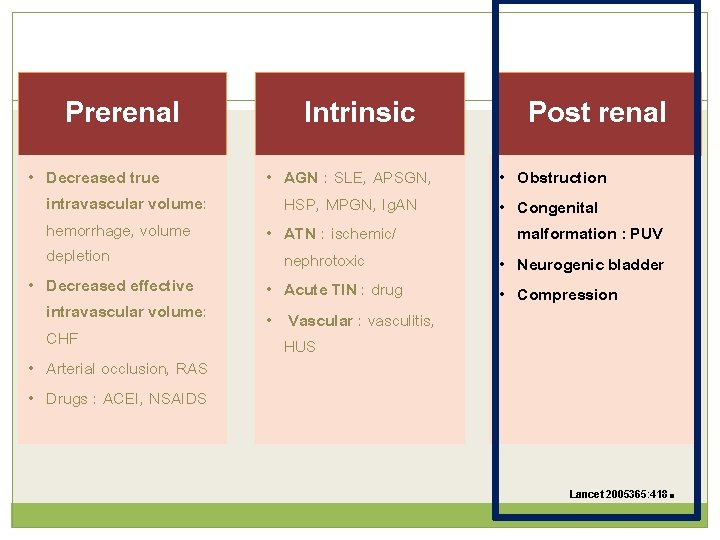

Prerenal • Decreased true intravascular volume: hemorrhage, volume depletion • Decreased effective intravascular volume: CHF • Arterial occlusion, RAS • Drugs : ACEI, NSAIDS Intrinsic • AGN : SLE, APSGN, HSP, MPGN, Ig. AN • ATN : ischemic/ nephrotoxic • Acute TIN : drug • Vascular : vasculitis, HUS Post renal • Obstruction • Congenital malformation : PUV • Neurogenic bladder • Compression Lancet 2005365: 418 .

Post-renal causes Bladder outlet: Posterior urethral valve Ureteral: Bilateral obstruction (or unilateral with one kidney): stones, malignancy, retroperitoneal fibrosis Renal pelvis: Papillary necrosis (NSAIDs), stones
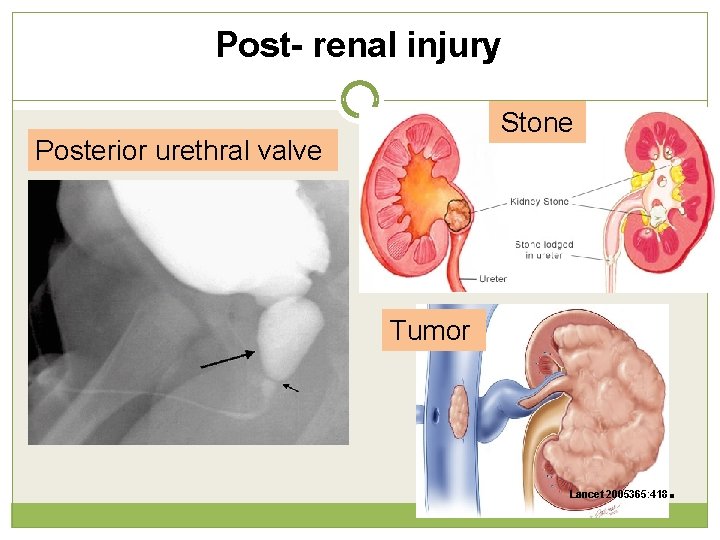
Post- renal injury Stone Posterior urethral valve Tumor Lancet 2005365: 418 .
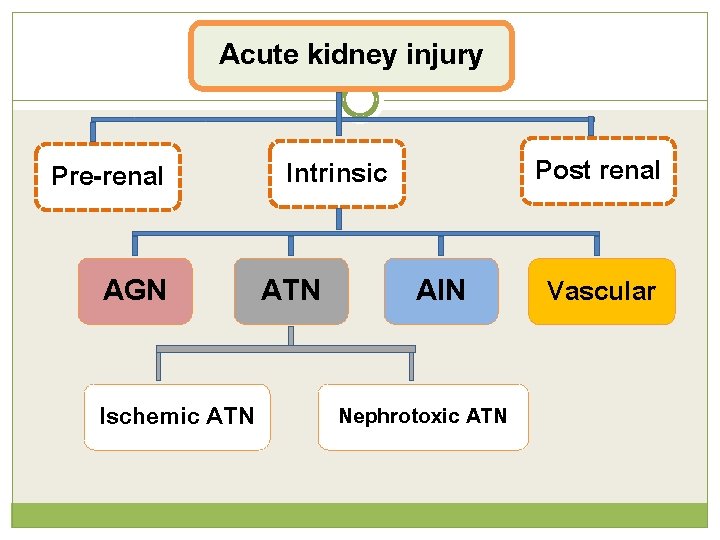
Acute kidney injury Pre-renal AGN Ischemic ATN Post renal Intrinsic ATN AIN Nephrotoxic ATN Vascular
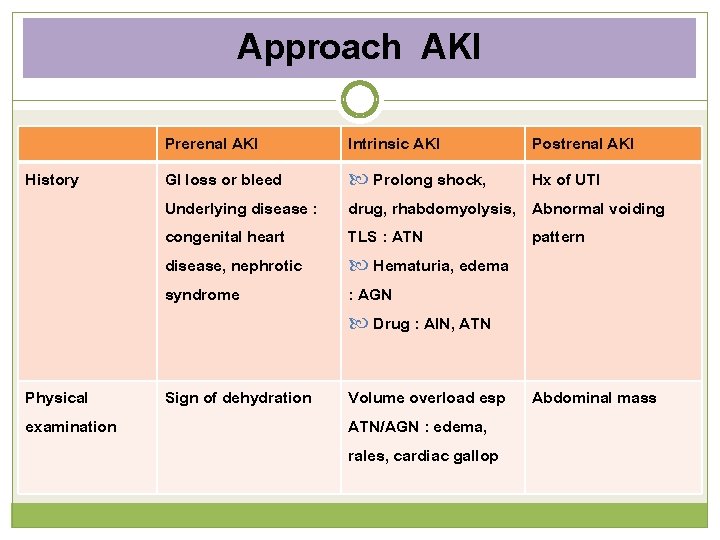
Approach AKI History Physical examination Prerenal AKI GI loss or bleed Underlying disease : congenital heart disease, nephrotic syndrome Intrinsic AKI Prolong shock, drug, rhabdomyolysis, TLS : ATN Hematuria, edema : AGN Drug : AIN, ATN Postrenal AKI Hx of UTI Abnormal voiding pattern Sign of dehydration Volume overload esp ATN/AGN : edema, rales, cardiac gallop Abdominal mass
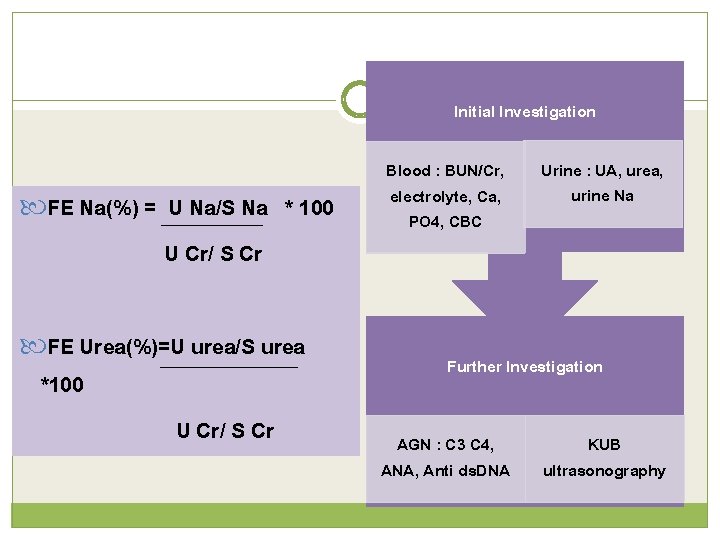
Initial Investigation FE Na(%) = U Na/S Na * 100 U Cr/ S Cr FE Urea(%)=U urea/S urea *100 U Cr/ S Cr Blood : BUN/Cr, electrolyte, Ca, PO 4, CBC Urine : UA, urea, urine Na Further Investigation AGN : C 3 C 4, ANA, Anti ds. DNA KUB ultrasonography
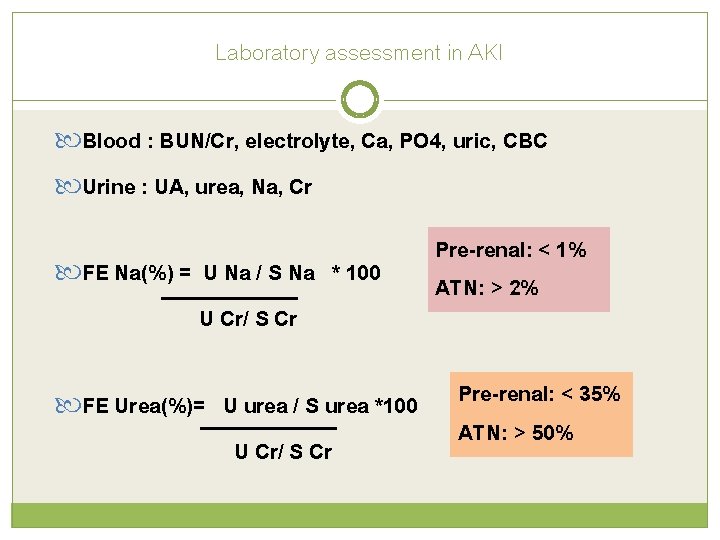

Laboratory assessment in AKI Blood : BUN/Cr, electrolyte, Ca, PO 4, uric, CBC Urine : UA, urea, Na, Cr FE Na(%) = U Na / S Na * 100 U Cr/ S Cr FE Urea(%)= U urea / S urea *100 U Cr/ S Cr Pre-renal: < 1% ATN: > 2% Pre-renal: < 35% ATN: > 50%
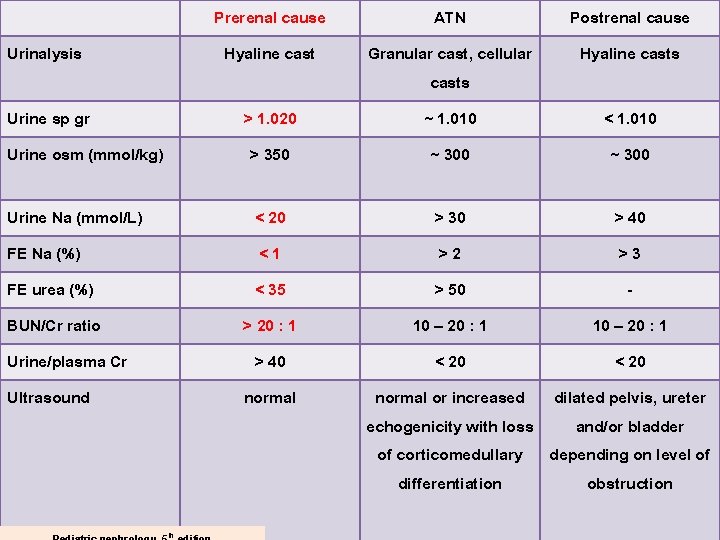
Urinalysis Prerenal cause ATN Postrenal cause Hyaline cast Granular cast, cellular casts ~ 1. 010 ~ 300 Hyaline casts Urine sp gr Urine osm (mmol/kg) > 1. 020 > 350 Urine Na (mmol/L) FE Na (%) FE urea (%) BUN/Cr ratio Urine/plasma Cr Ultrasound < 20 <1 < 35 > 20 : 1 > 40 normal th < 1. 010 ~ 300 > 30 > 40 >2 >3 > 50 10 – 20 : 1 < 20 normal or increased dilated pelvis, ureter echogenicity with loss and/or bladder of corticomedullary depending on level of differentiation obstruction
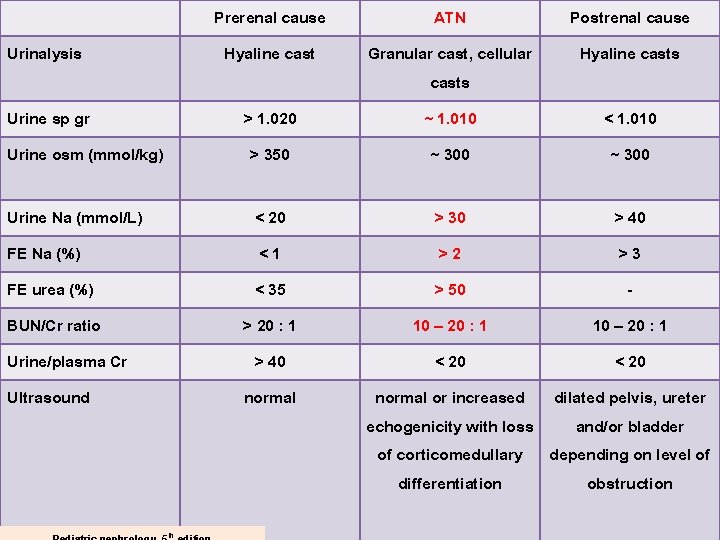
Urinalysis Prerenal cause ATN Postrenal cause Hyaline cast Granular cast, cellular casts ~ 1. 010 ~ 300 Hyaline casts Urine sp gr Urine osm (mmol/kg) > 1. 020 > 350 Urine Na (mmol/L) FE Na (%) FE urea (%) BUN/Cr ratio Urine/plasma Cr Ultrasound < 20 <1 < 35 > 20 : 1 > 40 normal th < 1. 010 ~ 300 > 30 > 40 >2 >3 > 50 10 – 20 : 1 < 20 normal or increased dilated pelvis, ureter echogenicity with loss and/or bladder of corticomedullary depending on level of differentiation obstruction
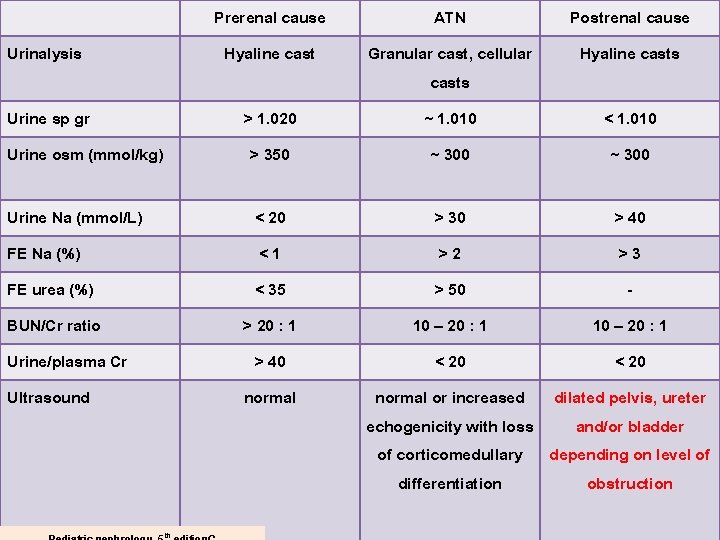
Urinalysis Prerenal cause ATN Postrenal cause Hyaline cast Granular cast, cellular casts ~ 1. 010 ~ 300 Hyaline casts Urine sp gr Urine osm (mmol/kg) > 1. 020 > 350 Urine Na (mmol/L) FE Na (%) FE urea (%) BUN/Cr ratio Urine/plasma Cr Ultrasound < 20 <1 < 35 > 20 : 1 > 40 normal th < 1. 010 ~ 300 > 30 > 40 >2 >3 > 50 10 – 20 : 1 < 20 normal or increased dilated pelvis, ureter echogenicity with loss and/or bladder of corticomedullary depending on level of differentiation obstruction
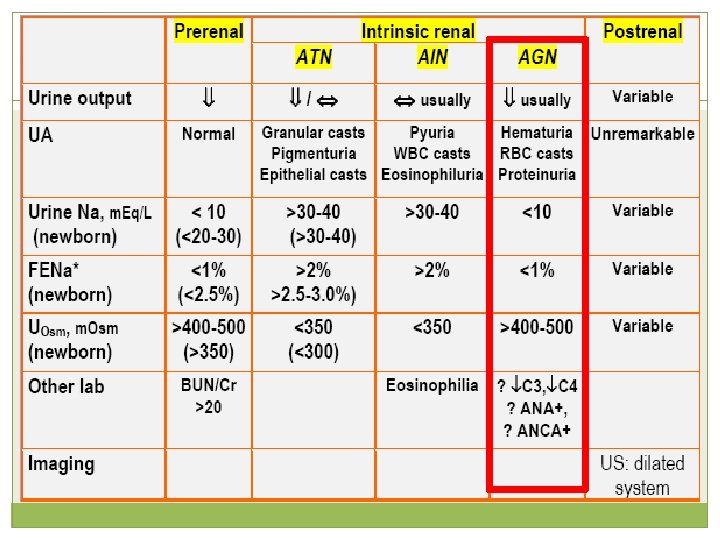
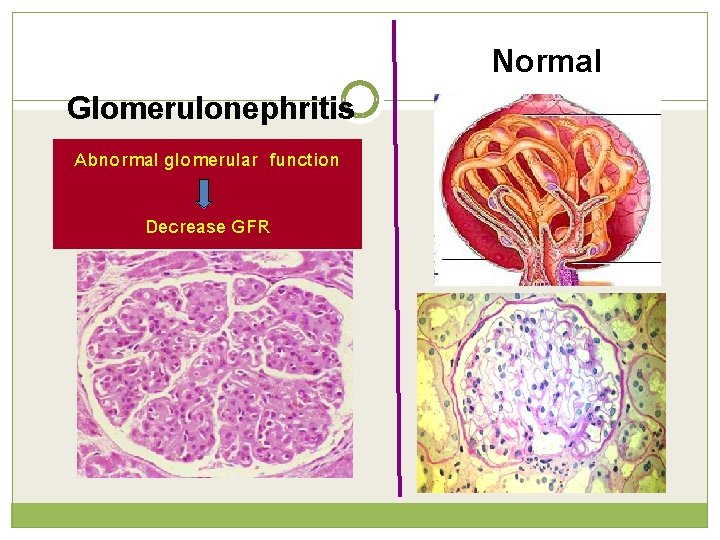
Glomerulonephritis Abnormal glomerular function Decrease GFR Normal
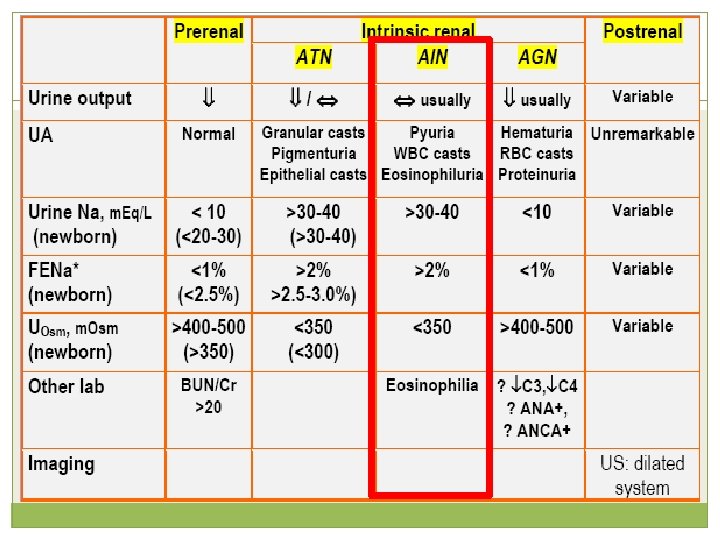
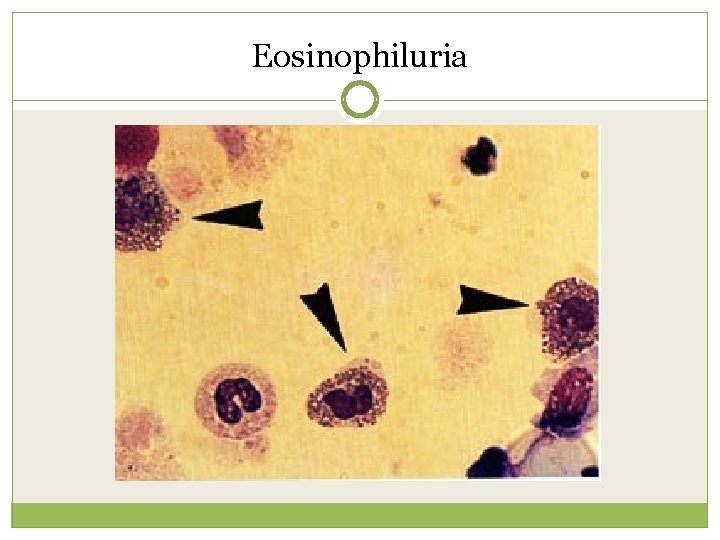
Eosinophiluria
Management of AKI Fluid Electrolytes Hypertension disturbance Treatment causes Drugs Nutritions Dialysis

Management : Fluid Pre-renal: Fluid loss : fluid rehydration, blood transfusion Heart failure : fluid restriction, inotropic drug, diuretics Intrinsic renal cause: AGN: fluid & salt restriction, diuretic(furosemide) ATN: Depends on phase of ATN

Clinical course : ATN 3 Phases of ATN Oliguric phase : 1 -2 weeks Diuretic phase : replace urine ml/ml Recovery phase Pediatric nephrology, 6 th edition
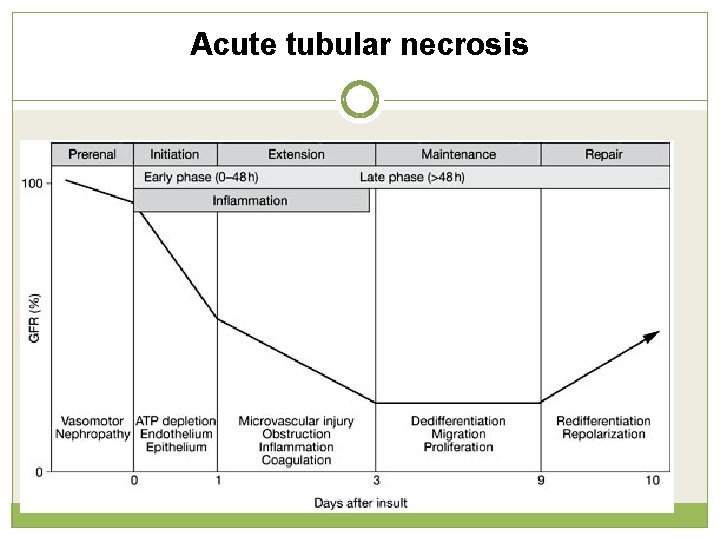
Acute tubular necrosis

Fluid management : oliguria Restrict fluid = ISL+ urine output + ongoing loss Insensible water loss = • 300 -400 ml/m 2/day • 30 -40 ml/kg in neonate GI loss CSF Third space loss Diuretic change oliguric to non-oliguric phase Pediatric nephrology, 6 th edition
Management : post-renal AKI Correct obstruction After release obstruction Post-obstructive diuresis Close observe vital signs, urine output Replace fluid & electrolyte

Electrolyte and acid-base balance Hyponatremia: fluid restriction, symptomatic 3% Na. Cl Hyperkalemia: Kayexalate or Kalimate, bicarbonate, insulin+glucose, beta 2 -agonist Hyperphosphatemia: PO 4 -binder(Ca. CO 3), restrict PO 4, avoid aluminum containing compounds Hypocalcemia : calcium supplement Metabolic acidosis: 7. 5%Na. HCO 3, sodamint Pediatric nephrology, 6 th edition

Management hyperkalemia Monitor ECG : if change 10%calcium gluconate 2. Decrease K intake/ remove cause : low K diet, off aldactone, ACEI 3. Shift of K from extracellular to intracellular compartment : Na. HCO 3, insulin, salbutamol 4. Remove K from body 1. • • • Ca+/Na+ polystyrene sulfonate Furosemide diuretic Dialysis
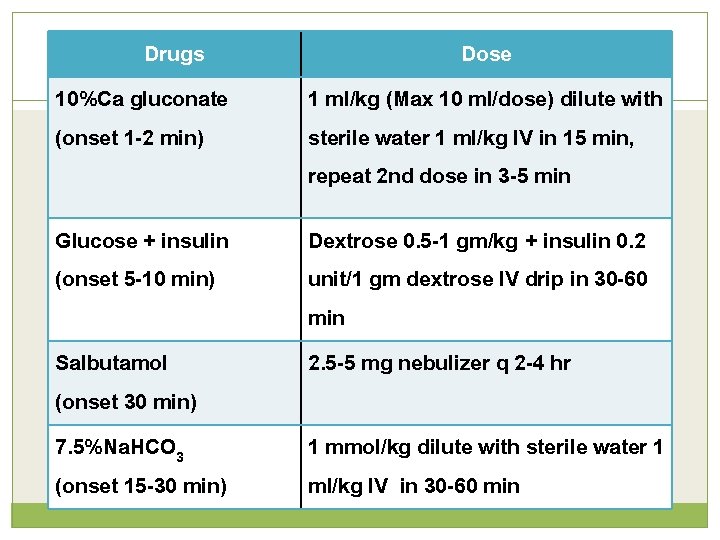
Drugs 10%Ca gluconate (onset 1 -2 min) Dose 1 ml/kg (Max 10 ml/dose) dilute with sterile water 1 ml/kg IV in 15 min, repeat 2 nd dose in 3 -5 min Glucose + insulin (onset 5 -10 min) Dextrose 0. 5 -1 gm/kg + insulin 0. 2 unit/1 gm dextrose IV drip in 30 -60 min 2. 5 -5 mg nebulizer q 2 -4 hr Salbutamol (onset 30 min) 7. 5%Na. HCO 3 (onset 15 -30 min) 1 mmol/kg dilute with sterile water 1 ml/kg IV in 30 -60 min
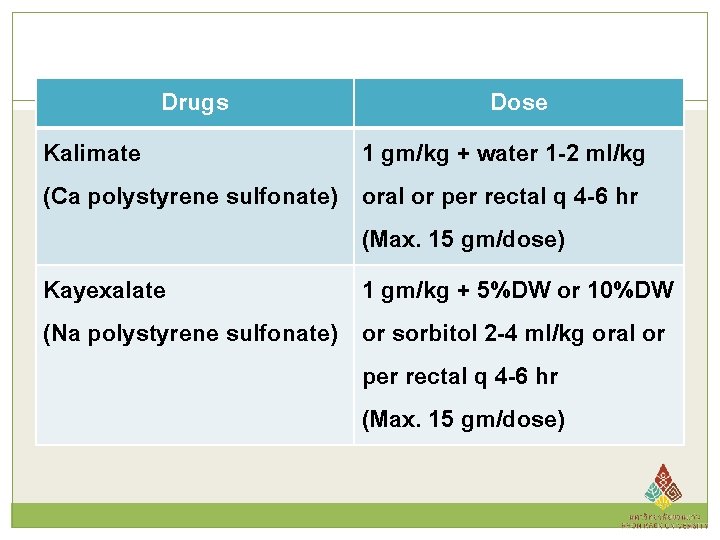
Drugs Dose Kalimate 1 gm/kg + water 1 -2 ml/kg (Ca polystyrene sulfonate) oral or per rectal q 4 -6 hr (Max. 15 gm/dose) Kayexalate 1 gm/kg + 5%DW or 10%DW (Na polystyrene sulfonate) or sorbitol 2 -4 ml/kg oral or per rectal q 4 -6 hr (Max. 15 gm/dose)

Dialysis indications Fluid overload Symptoms of uremia Severe hyperkalemia Severe metabolic acidosis Severe hyperphosphatemia (especially if accompanied by hypocalcemia) Prevention or treatment of tumor lysis syndrome and removal of toxins (ingestions or inborn errors of metabolism)

Mode of dialysis Hemodialysis Peritoneal dialysis CRRT (Continuous Renal Replacement Therapy)
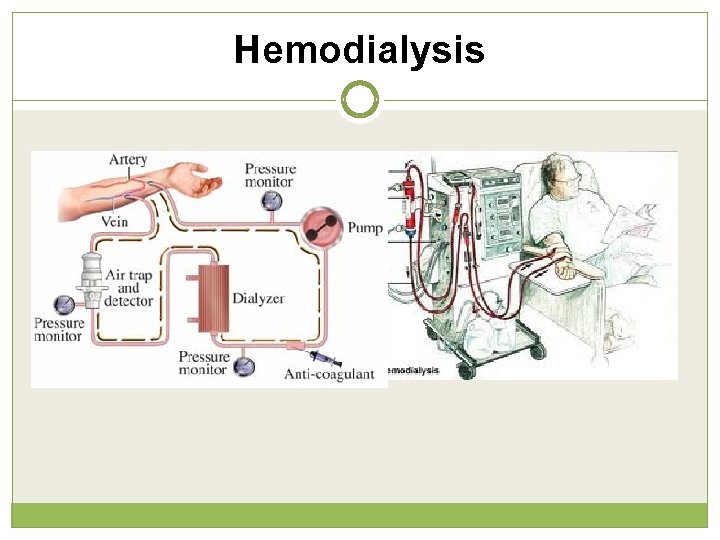
Hemodialysis
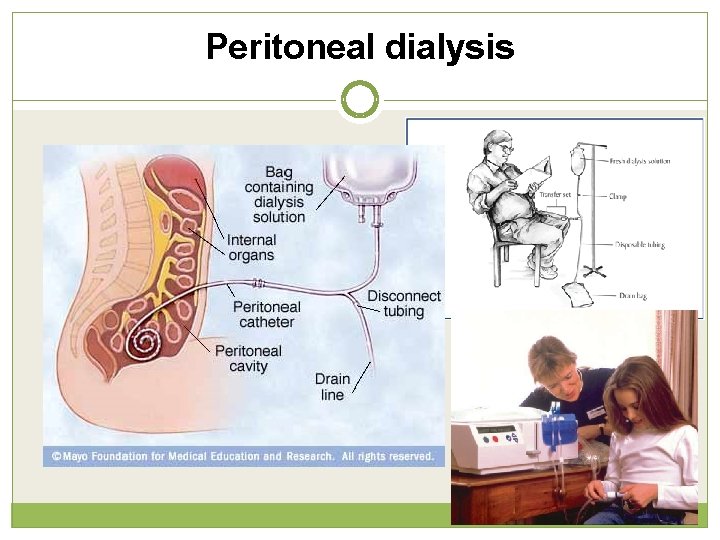
Peritoneal dialysis
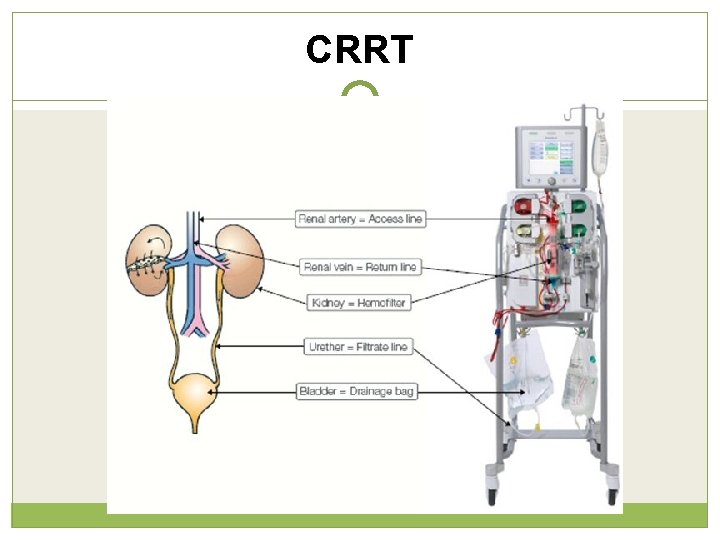
CRRT

- Slides: 51