Pediatric Academic Societies Meeting 2017 Department Poster Presentations





- Slides: 7

Pediatric Academic Societies Meeting 2017 Department Poster Presentations San Francisco, CA 5/6 -5/9/17 Lewis M. Fraad Department of Pediatrics, NYC Health + Hospitals Jacobi, Albert Einstein College of Medicine, Bronx, NY

Are Parents Who Identify their Children as Having a Low-Acuity Illness Willing to Accept Alternative Transportation to a Pediatric Emergency Department? Gonzalo A. Manzano MD, Stephen M. Blumberg MD Lewis M. Fraad Department of Pediatrics (Emergency Medicine), NYC Health + Hospitals/Jacobi, Albert Einstein College of Medicine, Bronx, NY The authors have documented no financial relationships to disclose or conflicts of interest (COIs) to resolve Results Background Methods • Emergency Medical Services (EMS) faces several challenges: Ø Increasing number of patients Ø Rising costs Ø Frequent transport requests for non-life-threatening medical complaints • EMS is exploring alternative non-emergency transportation modes, such as medical vans and taxis • In order for these alternatives to be practical, patients and caregivers must be: Ø Able to identify low-acuity illnesses that would be appropriate for non-emergency modes of transportation Ø Willing to accept these alternatives • Previous research has shown that: Ø Most adults would accept alternative transportation for their own medical care Ø Parents of children with higher acuity illness would not be willing to accept alternative transportation • There is limited evidence examining these issues in urban pediatric lowacuity patients • The survey examined: Ø Demographics Ø Modes of arrival to the PED Ø Parental perception of the child’s severity of illness (dichotomized Likert scale: 1 -3=not sick, 4 -5=sick) Ø Parental acceptance of alternative transportation in the future (dichotomized Likert scale: 1 -2=acceptable, 3 -5=not acceptable) Ø Parental acceptance of waiting up to one hour for alternative transportation (dichotomized Likert scale: 1 -2=acceptable, 3 -5=not acceptable) • Among parents who identified their child as having low-acuity illnesses, we calculated the percentage who were willing to accept alternative modes of transportation to the PED • Determined the association of acceptance of taxi in the future, regardless of whether or not the family presented to the PED via ambulance • To determine the percentage of parents who recognize that their child has a low-acuity illness and are willing to accept alternative transportation to the pediatric emergency department (PED) Methods • We administered a voluntary, anonymous survey to parents and guardians accompanying low-acuity pediatric patients who presented to an urban PED via any method of transportation Inclusion Criteria • Triage Emergency Severity Illness scores of 4 and 5 • Able to read and understand English or Spanish Exclusion Criteria • More than one patient per family • Previous participation in the study • Transported via ambulance from another facility or institution (school) • Of these, 433 (77%) parents stated an alternative mode of transportation with a taxi would be acceptable Results • N=811 surveys completed Parental Perception of Child’s Severity of Illness Characteristics Child age: Median Years (IQR) 4 (2, 9) Gender: Male n (%) 445 (55) Race/Ethnicity: n (%) Hispanic African-American Asian White 422 (52) 246 (30) 60 (7) 56 (7) Distance: Median Miles Home to PED (IQR) 2. 4 (1. 8, 3. 3) Driver’s License: None n (%) 471 (58) Mode of Arrival to the PED: n (%) Taxi Driving Public transportation Ambulance Ride from friend/relative Walking 244 (30) 182 (22) 155 (19) 136 (17) 54 (7) 40 (5) Chief Complaint: n (%) Fever Extremity pain Rash 196 (24) 103 (13) 100 (12) Parental Acceptance of Alternative Transportation Objective • 564 (70%) parents perceived their child had a low-acuity illness Not Sick Yes 433 177 No 131 65 • The acceptance of a taxi was not significantly associated with whether or not the family presented to the PED via ambulance [OR=0. 80 (95%CI 0. 53 -1. 22)] • 148 (18%) parents stated it would be reasonable to wait at home up to one hour for an alternative mode of transportation Conclusion • The majority of parents in this study are able to identify their child as having a low-acuity illness Ø Most of these parents would be willing to accept alternative transportation to the PED • There was no significant relationship between acceptance of an alternative mode of transportation in the future and current mode of arrival to the PED

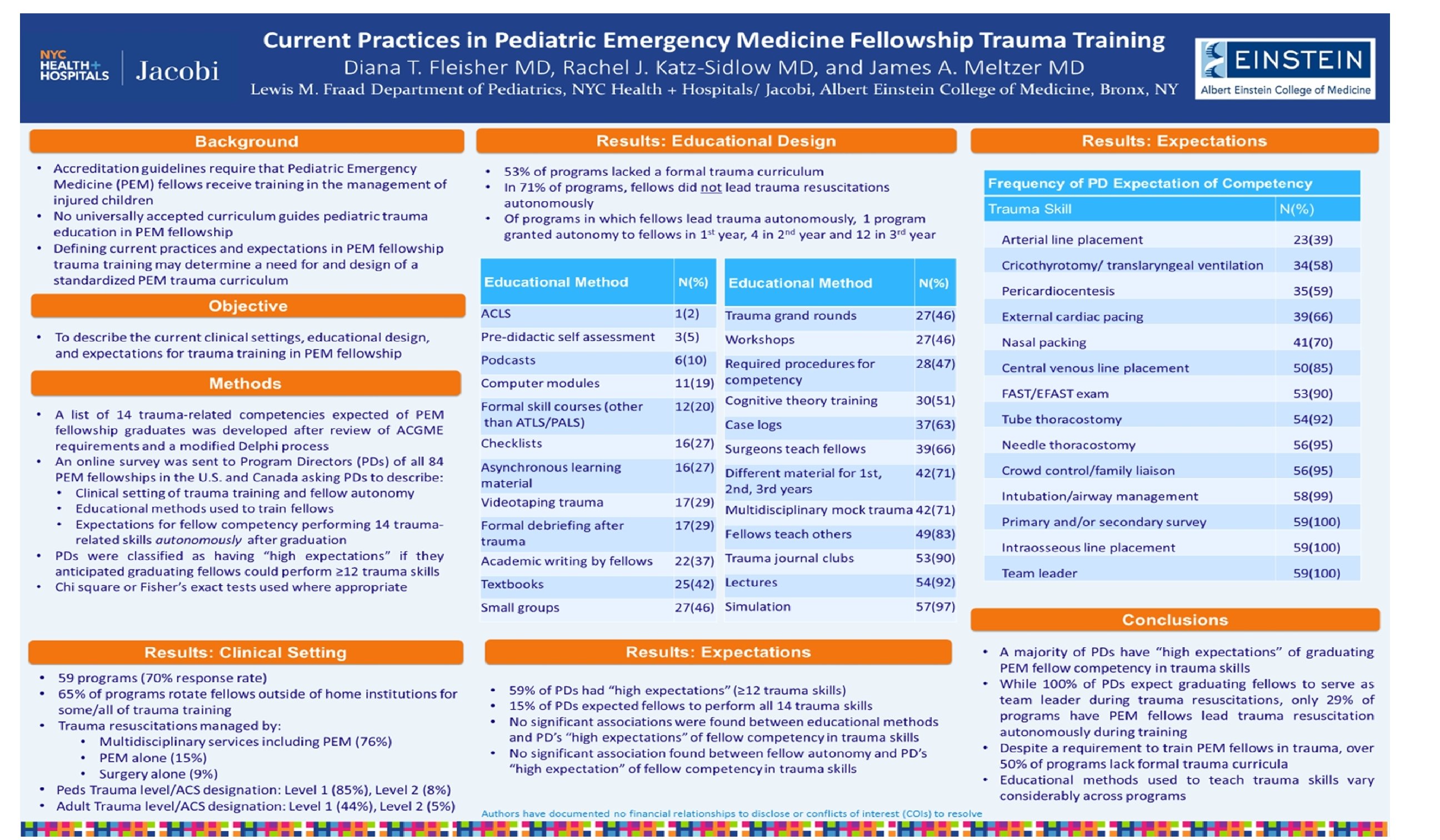
The Association Between the Asthma Predictive Index (API) and Clinical Response to Asthma Therapy in Young Children With Recurrent Wheezing in an Asthma-Endemic Population Danielle B. Barrocas MD, Sandra Cunningham, MD Lewis M. Fraad Department of Pediatrics, NYC Health + Hospitals/ Jacobi, Albert Einstein College of Medicine, Bronx, NY The authors have documented no financial relationships to disclose or conflicts of interest (COIs) to resolve Results Background Methods • The treatment of infants and toddlers with recurrent wheezing remains a challenge • Several phenotypes of infant wheezers have been described, however, no approach to clinically distinguish these in the acute setting has been established • The Asthma Predictive Index (API) is a tool that helps predict a child’s likelihood of developing asthma based on major and minor criteria (Figure) • No studies to date have looked for an association between the API and response to asthma treatment in this age group. • A separate blinded investigator recorded RDAI and vitals every 30 minutes for 2 hours • CBCs from the past 6 months were obtained from the medical record to evaluate for eosinophilia • The primary outcome, the Respiratory Assessment Change Score (RACS), is the sum of the changes in RDAI and respiratory rate • Median RACS at 60 and 120 minutes (m) and admission rate were compared between API-Positive and API-Negative groups • A RACS of ≥ 3 was considered to be clinically significant Results Outcomes API Positive API Negative P value RACS at 60 minutes, median (IQR) 4 (1, 6) 6 (1, 9) 0. 10 RACS at 120 minutes, median (IQR) 5 (1, 8) 7 (4, 10) 0. 41 Change in RDAI at 60 minutes, median (IQR) 4 (1, 6) 5 (1, 7) 0. 43 Change in RDAI at 120 minutes, median (IQR) 5 (1, 7) 5 (3, 9) 0. 22 Admission rate, n (%) 6 (18) 5 (31) 0. 30 Asthma Predictive Index* 1 of 2 MAJOR Criteria OR 2 of 3 MINOR Criteria Physician diagnosis of asthma in a parent Physician diagnosis of allergic rhinitis Physician diagnosis of eczema Wheezing apart from colds Eosinophilia (≥ 4%) *Adapted from Castro-Rodriguez, 2000 50 patients enrolled • Mean age 14 months (SD +/- 6) • 50 (100%) received at least 2 nebulized albuterol treatments • 26 (52%) received corticosteroids • 34 (68%) were classified as API-Positive • 38 (76%) met at least one API criterion; of these 14 (37%) met both major criteria Objective • To determine if children <2 years with recurrent wheezing and a positive API are more likely to have clinical improvement following standard asthma therapy compared to those with a negative API Demographics And Group Characteristics API-Positive n=34 API-Negative n=16 22 (65) 10 (63) 14 15 9 (27) 6 (38) 19 (56) 5 (31) 5 (15) 2 (13) Cockroaches 10 (29) 5 (31) Dust 23 (72) 14 (88) 17 (50) 9 (56) 99. 7 100. 8 8 7 Male, n (%) Mean age, months Methods • Prospective observational study of wheezing children <2 years presenting to the PED with a history of at least one prior wheezing episode and a baseline Respiratory Distress Assessment Instrument (RDAI) score ≥ 4 • Patients were classified as API-Positive or API-Negative based on a parental survey • Bronchodilators and steroids were administered at the discretion of the treating physician Race, n (%): African American Hispanic Household exposures, n (%): Cigarette smoke Received corticosteroids, n (%) Baseline temperature, °F, median Baseline RDAI, median Conclusions • API classification did not differentiate those who responded to asthma therapy from those who did not in our sample • The majority of subjects in our cohort had improved respiratory scores after asthma therapy, and the majority had risk factors for asthma • The use of respiratory scoring as a measure of response to therapy may be a limitation of this study • Other environmental factors that are not included in the API may play a role in our population’s overall responsiveness to asthma therapy


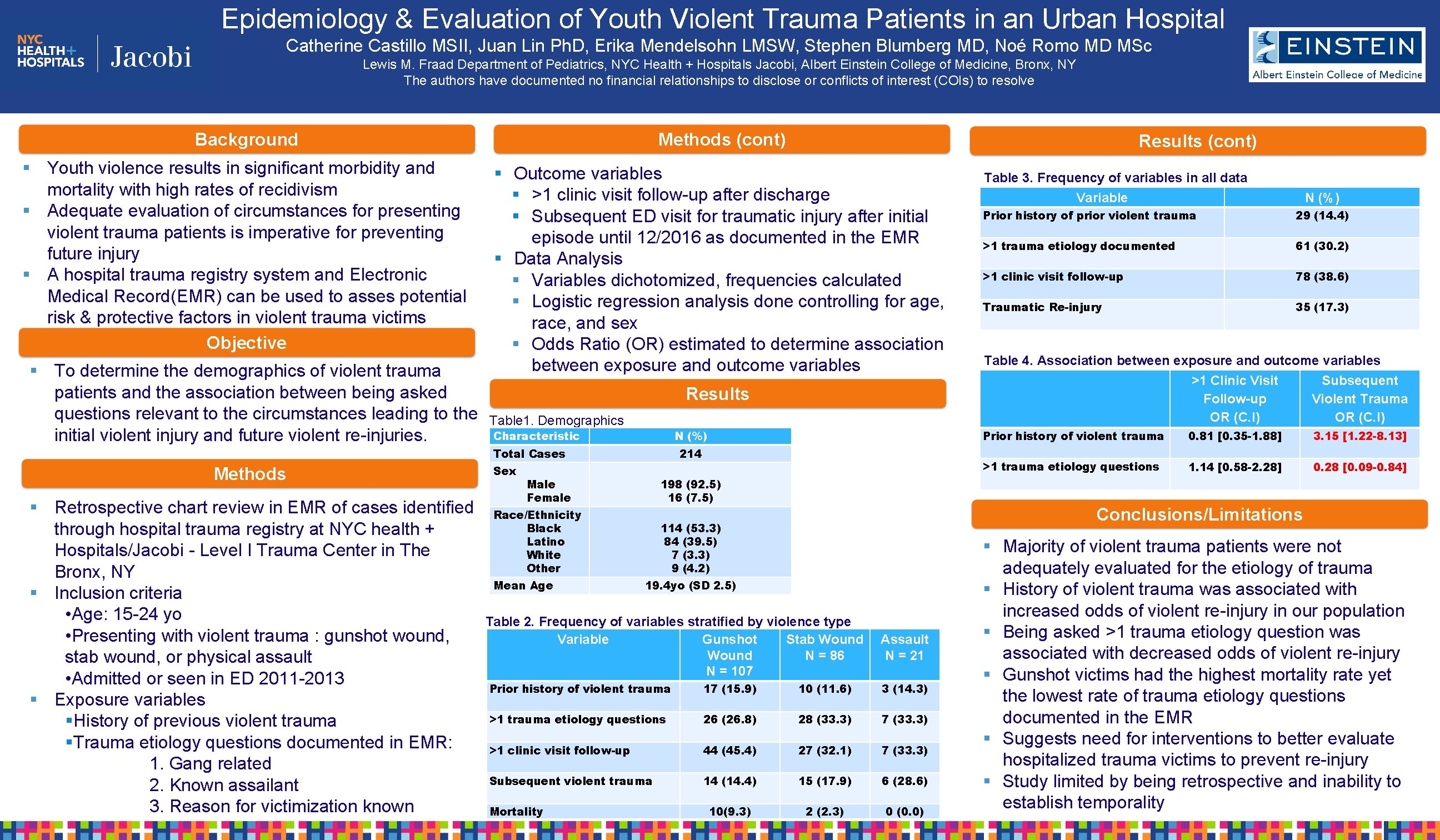
Epidemiology & Evaluation of Youth Violent Trauma Patients in an Urban Hospital Catherine Castillo MSII, Juan Lin Ph. D, Erika Mendelsohn LMSW, Stephen Blumberg MD, Noé Romo MD MSc Lewis M. Fraad Department of Pediatrics, NYC Health + Hospitals Jacobi, Albert Einstein College of Medicine, Bronx, NY The authors have documented no financial relationships to disclose or conflicts of interest (COIs) to resolve Background Methods (cont) § Youth violence results in significant morbidity and mortality with high rates of recidivism § Adequate evaluation of circumstances for presenting violent trauma patients is imperative for preventing future injury § A hospital trauma registry system and Electronic Medical Record(EMR) can be used to asses potential risk & protective factors in violent trauma victims Objective § Outcome variables § >1 clinic visit follow-up after discharge § Subsequent ED visit for traumatic injury after initial episode until 12/2016 as documented in the EMR § Data Analysis § Variables dichotomized, frequencies calculated § Logistic regression analysis done controlling for age, race, and sex § Odds Ratio (OR) estimated to determine association between exposure and outcome variables § To determine the demographics of violent trauma patients and the association between being asked questions relevant to the circumstances leading to the initial violent injury and future violent re-injuries. Results Table 1. Demographics Characteristic N (%) Total Cases Methods § Retrospective chart review in EMR of cases identified through hospital trauma registry at NYC health + Hospitals/Jacobi - Level I Trauma Center in The Bronx, NY § Inclusion criteria • Age: 15 -24 yo • Presenting with violent trauma : gunshot wound, stab wound, or physical assault • Admitted or seen in ED 2011 -2013 § Exposure variables §History of previous violent trauma §Trauma etiology questions documented in EMR: 1. Gang related 2. Known assailant 3. Reason for victimization known Results (cont) Sex 214 Male Female 198 (92. 5) 16 (7. 5) Race/Ethnicity Black Latino White Other Mean Age N (%) Prior history of prior violent trauma 29 (14. 4) >1 trauma etiology documented 61 (30. 2) >1 clinic visit follow-up 78 (38. 6) Traumatic Re-injury 35 (17. 3) Table 4. Association between exposure and outcome variables >1 Clinic Visit Subsequent Follow-up Violent Trauma OR (C. I) Prior history of violent trauma 0. 81 [0. 35 -1. 88] 3. 15 [1. 22 -8. 13] >1 trauma etiology questions 1. 14 [0. 58 -2. 28] 0. 28 [0. 09 -0. 84] Conclusions/Limitations 114 (53. 3) 84 (39. 5) 7 (3. 3) 9 (4. 2) 19. 4 yo (SD 2. 5) Table 2. Frequency of variables stratified by violence type Variable Gunshot Stab Wound N = 86 N = 107 Assault N = 21 Prior history of violent trauma 17 (15. 9) 10 (11. 6) 3 (14. 3) >1 trauma etiology questions 26 (26. 8) 28 (33. 3) 7 (33. 3) >1 clinic visit follow-up 44 (45. 4) 27 (32. 1) 7 (33. 3) Subsequent violent trauma 14 (14. 4) 15 (17. 9) 6 (28. 6) 10(9. 3) 2 (2. 3) 0 (0. 0) Mortality Table 3. Frequency of variables in all data Variable § Majority of violent trauma patients were not adequately evaluated for the etiology of trauma § History of violent trauma was associated with increased odds of violent re-injury in our population § Being asked >1 trauma etiology question was associated with decreased odds of violent re-injury § Gunshot victims had the highest mortality rate yet the lowest rate of trauma etiology questions documented in the EMR § Suggests need for interventions to better evaluate hospitalized trauma victims to prevent re-injury § Study limited by being retrospective and inability to establish temporality

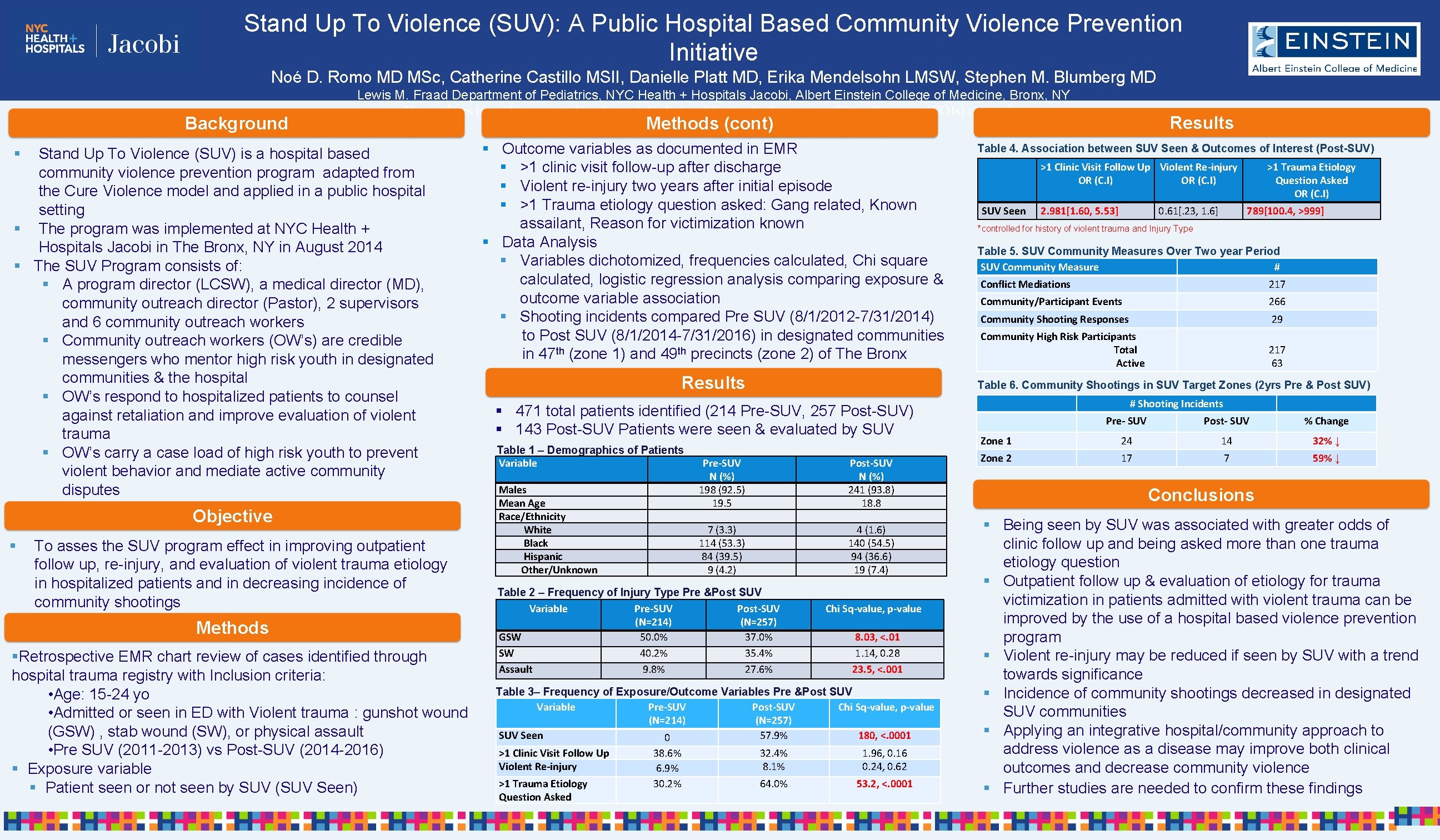
Stand Up To Violence (SUV): A Public Hospital Based Community Violence Prevention Initiative Noé D. Romo MD MSc, Catherine Castillo MSII, Danielle Platt MD, Erika Mendelsohn LMSW, Stephen M. Blumberg MD Background Lewis M. Fraad Department of Pediatrics, NYC Health + Hospitals Jacobi, Albert Einstein College of Medicine, Bronx, NY The authors have documented no financial relationships to disclose or conflicts of interest (COIs) to resolve § Stand Up To Violence (SUV) is a hospital based community violence prevention program adapted from the Cure Violence model and applied in a public hospital setting § The program was implemented at NYC Health + Hospitals Jacobi in The Bronx, NY in August 2014 § The SUV Program consists of: § A program director (LCSW), a medical director (MD), community outreach director (Pastor), 2 supervisors and 6 community outreach workers § Community outreach workers (OW’s) are credible messengers who mentor high risk youth in designated communities & the hospital § OW’s respond to hospitalized patients to counsel against retaliation and improve evaluation of violent trauma § OW’s carry a case load of high risk youth to prevent violent behavior and mediate active community disputes Objective § To asses the SUV program effect in improving outpatient follow up, re-injury, and evaluation of violent trauma etiology in hospitalized patients and in decreasing incidence of community shootings Methods §Retrospective EMR chart review of cases identified through hospital trauma registry with Inclusion criteria: • Age: 15 -24 yo • Admitted or seen in ED with Violent trauma : gunshot wound (GSW) , stab wound (SW), or physical assault • Pre SUV (2011 -2013) vs Post-SUV (2014 -2016) § Exposure variable § Patient seen or not seen by SUV (SUV Seen) Results Methods (cont) § Outcome variables as documented in EMR § >1 clinic visit follow-up after discharge § Violent re-injury two years after initial episode § >1 Trauma etiology question asked: Gang related, Known assailant, Reason for victimization known § Data Analysis § Variables dichotomized, frequencies calculated, Chi square calculated, logistic regression analysis comparing exposure & outcome variable association § Shooting incidents compared Pre SUV (8/1/2012 -7/31/2014) to Post SUV (8/1/2014 -7/31/2016) in designated communities in 47 th (zone 1) and 49 th precincts (zone 2) of The Bronx Results Males Mean Age Race/Ethnicity White Black Hispanic Other/Unknown Pre-SUV N (%) 198 (92. 5) 19. 5 Post-SUV N (%) 241 (93. 8) 18. 8 7 (3. 3) 114 (53. 3) 84 (39. 5) 9 (4. 2) 4 (1. 6) 140 (54. 5) 94 (36. 6) 19 (7. 4) Table 2 – Frequency of Injury Type Pre &Post SUV Variable Pre-SUV Post-SUV (N=214) (N=257) GSW 50. 0% 37. 0% SW 40. 2% 35. 4% Assault 9. 8% 27. 6% Chi Sq-value, p-value 8. 03, <. 01 1. 14, 0. 28 23. 5, <. 001 Table 3– Frequency of Exposure/Outcome Variables Pre &Post SUV Variable Pre-SUV Post-SUV Chi Sq-value, p-value (N=214) (N=257) SUV Seen 57. 9% 180, <. 0001 0 >1 Clinic Visit Follow Up Violent Re-injury >1 Trauma Etiology Question Asked 38. 6% 6. 9% 30. 2% >1 Clinic Visit Follow Up Violent Re-injury OR (C. I) SUV Seen 2. 981[1. 60, 5. 53] 0. 61[. 23, 1. 6] >1 Trauma Etiology Question Asked OR (C. I) 789[100. 4, >999] *controlled for history of violent trauma and Injury Type Table 5. SUV Community Measures Over Two year Period SUV Community Measure # Conflict Mediations 217 Community/Participant Events 266 Community Shooting Responses 29 Community High Risk Participants Total Active 217 63 Table 6. Community Shootings in SUV Target Zones (2 yrs Pre & Post SUV) § 471 total patients identified (214 Pre-SUV, 257 Post-SUV) § 143 Post-SUV Patients were seen & evaluated by SUV Table 1 – Demographics of Patients Variable Table 4. Association between SUV Seen & Outcomes of Interest (Post-SUV) 32. 4% 8. 1% 1. 96, 0. 16 0. 24, 0. 62 64. 0% 53. 2, <. 0001 # Shooting Incidents Pre- SUV Post- SUV % Change Zone 1 24 14 32% ↓ Zone 2 17 7 59% ↓ Conclusions § Being seen by SUV was associated with greater odds of clinic follow up and being asked more than one trauma etiology question § Outpatient follow up & evaluation of etiology for trauma victimization in patients admitted with violent trauma can be improved by the use of a hospital based violence prevention program § Violent re-injury may be reduced if seen by SUV with a trend towards significance § Incidence of community shootings decreased in designated SUV communities § Applying an integrative hospital/community approach to address violence as a disease may improve both clinical outcomes and decrease community violence § Further studies are needed to confirm these findings

See You at PAS!!!