PCA Based Tumor Classification Algorithm PCA based Algorithm

PCA Based Tumor Classification Algorithm PCA based Algorithm for Longitudinal Brain Tumor Stage And Classification & Dynamical Modeling of Tumor Dynamical Modeling Of Tumor Decay in response to VB-111 Virotherapy Amy W. Daali Ph. D. Defense Spring 2015 Electrical and Computer Engineering Department University of Texas at San Antonio

Outline • Motivation • Research Background • Proposed Approach : • Classification Algorithm • Mathematical Model • Results • Conclusion • Future work • Publications

Contributions •
Motivation • Research focus on deadly brain cancer : Glioblastoma • Highly malignant, cannot be cured : cells reproduce quickly, supported by a large network of blood vessels Gliomas Glioblastoma Ependymomas • Glioblastomas represent 54% of all gliomas Oligodendrogliomas

Needs in Neuro-Oncology & Our Research § Need to detect the stage of the tumor to predict the progression of brain cancer and patient survival § Developed novel principal component analysis (PCA) based tumor classification of a large temporal MRI brain scans § Investigate the efficacy of VB-111 clinically on solid tumors § Quantified the effect of VB-111 in the presence of TNF-α at the tumor microenvironment

Research Background § Magnetic Resonance Imaging Experiment § Data Description § Biological Background on VB-111 mechanism
MRI Experiment • Intracranial xenograft

Data Description •
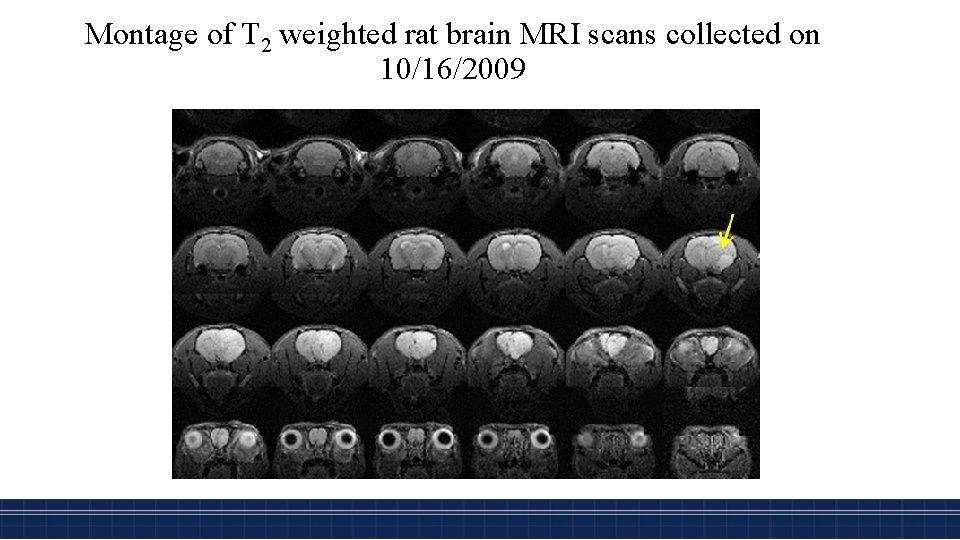
Montage of T 2 weighted rat brain MRI scans collected on 10/16/2009
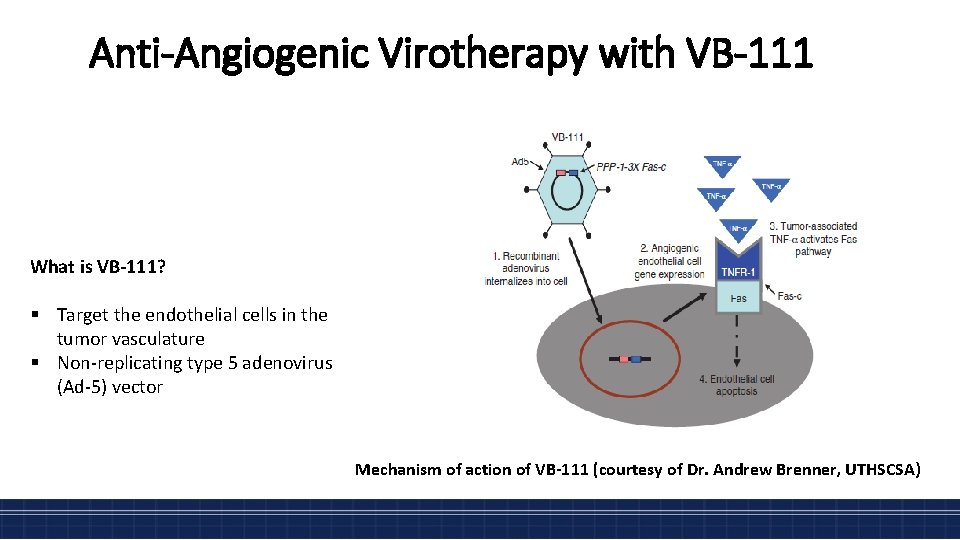
Anti-Angiogenic Virotherapy with VB-111 What is VB-111? § Target the endothelial cells in the tumor vasculature § Non-replicating type 5 adenovirus (Ad-5) vector Mechanism of action of VB-111 (courtesy of Dr. Andrew Brenner, UTHSCSA)
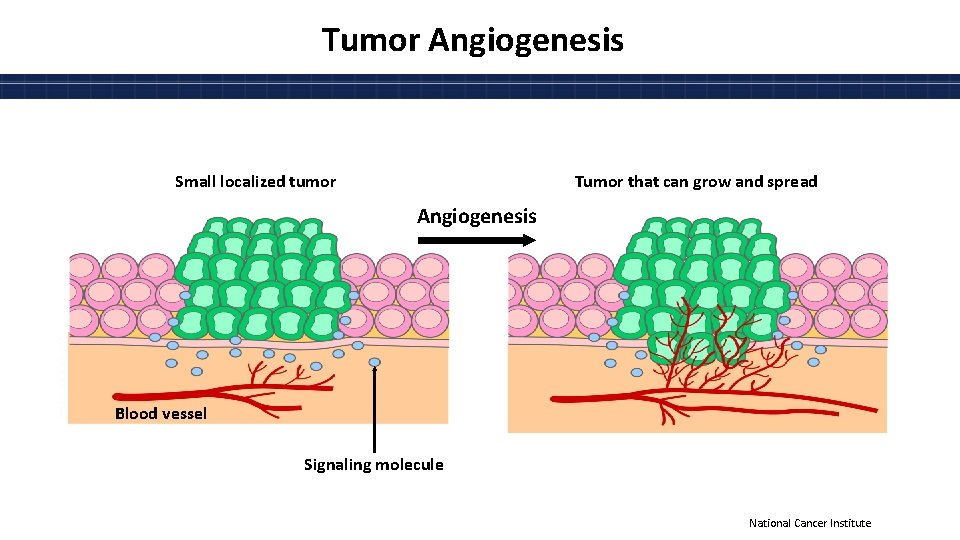
Tumor Angiogenesis Small localized tumor Tumor that can grow and spread Angiogenesis Blood vessel Signaling molecule National Cancer Institute
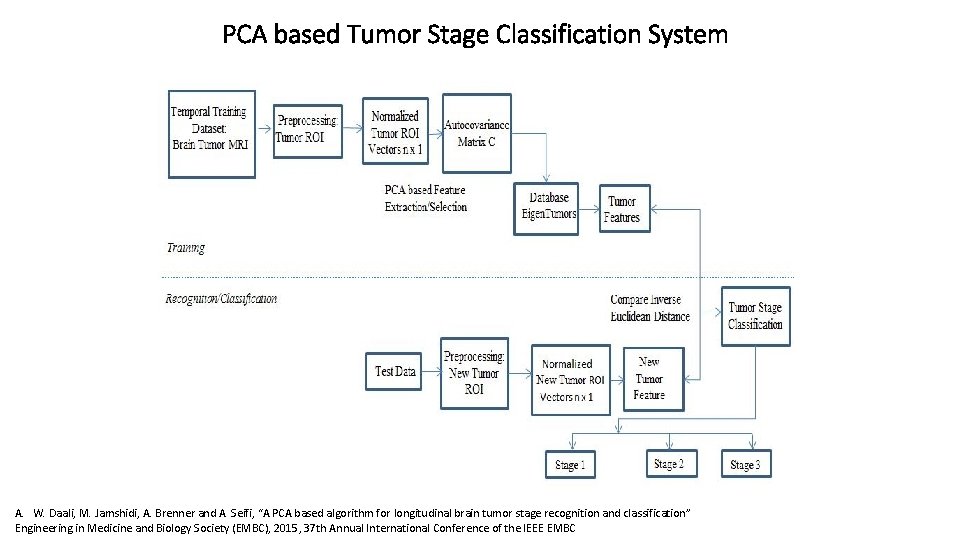
PCA based Tumor Stage Classification System A. W. Daali, M. Jamshidi, A. Brenner and A. Seifi, “A PCA based algorithm for longitudinal brain tumor stage recognition and classification” Engineering in Medicine and Biology Society (EMBC), 2015, 37 th Annual International Conference of the IEEE EMBC
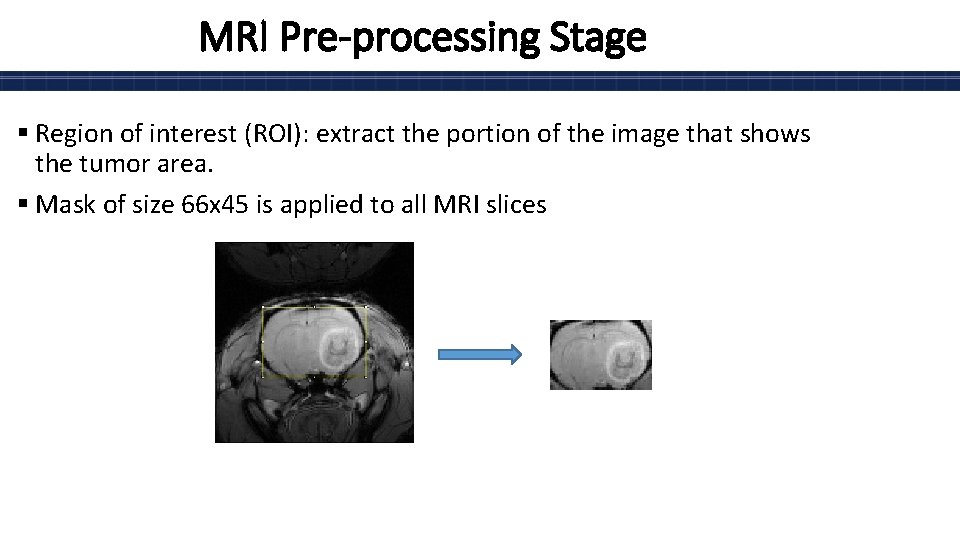
MRI Pre-processing Stage § Region of interest (ROI): extract the portion of the image that shows the tumor area. § Mask of size 66 x 45 is applied to all MRI slices
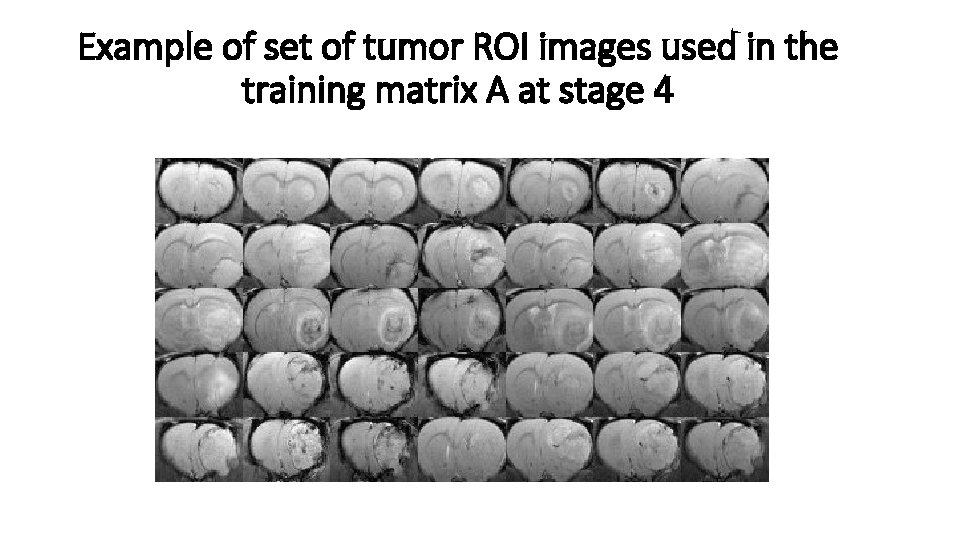
Example of set of tumor ROI images used in the training matrix A at stage 4

Applying PCA on Tumor ROI images •

Top 10 Eigen. Tumors § Keep only the Eigentumors with largest eigenvalues that retain highest information about the input data (top 33 ) § These Eigentumors are what they call the principle components of the dataset

Inverse Euclidean Classifier •
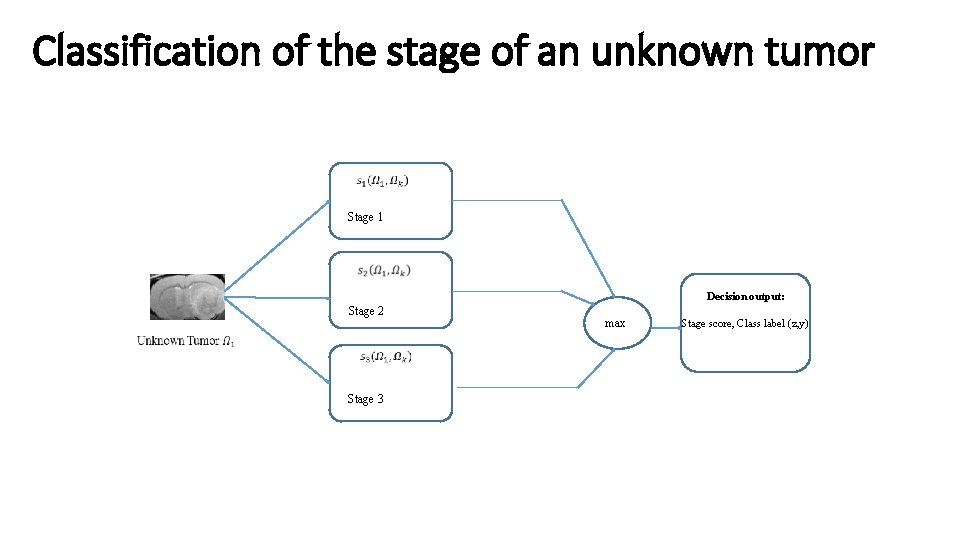
Classification of the stage of an unknown tumor Stage 1 Stage 2 Stage 3 max Decision output: Stage score, Class label (z, y)
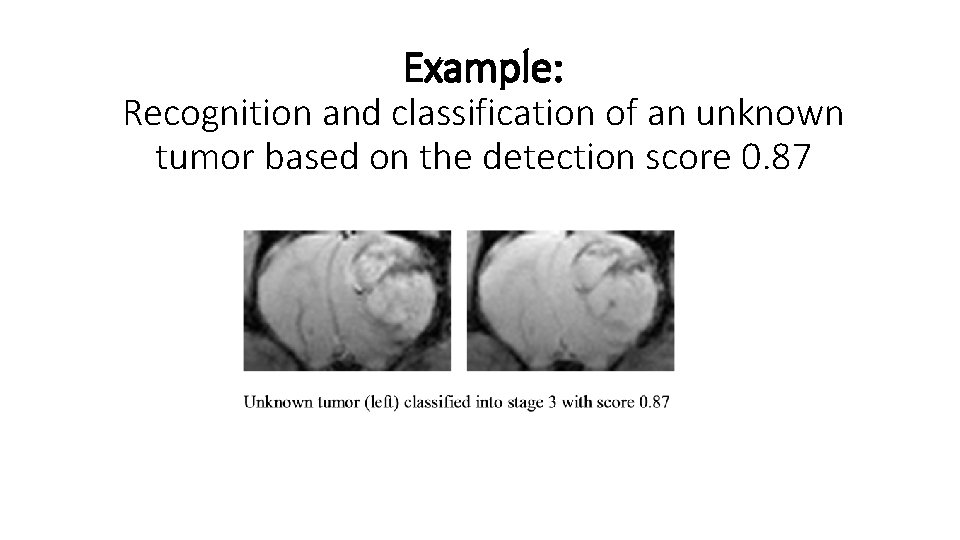
Example: Recognition and classification of an unknown tumor based on the detection score 0. 87

Classifier Performance Ground Truth Stage 1 MRI scan Detection Score Stage 1 Stage 2 Stage 3 1 0. 98 0. 65 0. 58 2 0. 80 0. 48 0. 47 3 0. 75 0. 53 0. 50 4 0. 81 0. 75 0. 64 5 0. 98 0. 64 0. 63 Sensitivity Stage 2 98. 70% 1 0. 95 0. 98 0. 76 2 0. 51 0. 78 0. 55 3 0. 50 0. 67 0. 55 4 0. 58 0. 90 0. 58 5 0. 47 0. 71 0. 53 Sensitivity Stage 3 Sensitivity 95. 80% 1 0. 46 0. 56 0. 99 2 0. 49 0. 78 0. 98 3 0. 52 0. 82 0. 95 4 0. 58 0. 53 0. 98 5 0. 69 0. 59 0. 72 94. 01%

Needs in Neuro-Oncology & Our Research § Need to detect the stage of the tumor to predict the progression of brain cancer and patient survival § Developed novel principal component analysis (PCA) based tumor classification of a large temporal MRI brain scans § Investigate the efficacy of VB-111 clinically on solid tumors § Quantifying the effect of VB-111 in the presence of TNF-α at the tumor microenvironment

Phase 1 study Results • By Brenner, et al. at Cancer Therapy & Research Center, UTHSCSA • Single dose of VB-111 in 33 patients with solid tumors Increased survival rate • No existing model to quantify the effect of VB-111 on tumor system We propose: • Novel mathematical model for antiangiogenic treatments effects of VB-111 on tumor cells

Proposed Mathematical Model -Key Components • Tumor cells • Cytokine tumor necrosis factor (TNF-α ): protein mediators of immune responses, important role in cancer immunotherapies • Effector Cells (T cells, Natural killer cells) • Therapeutic protein Fas-c
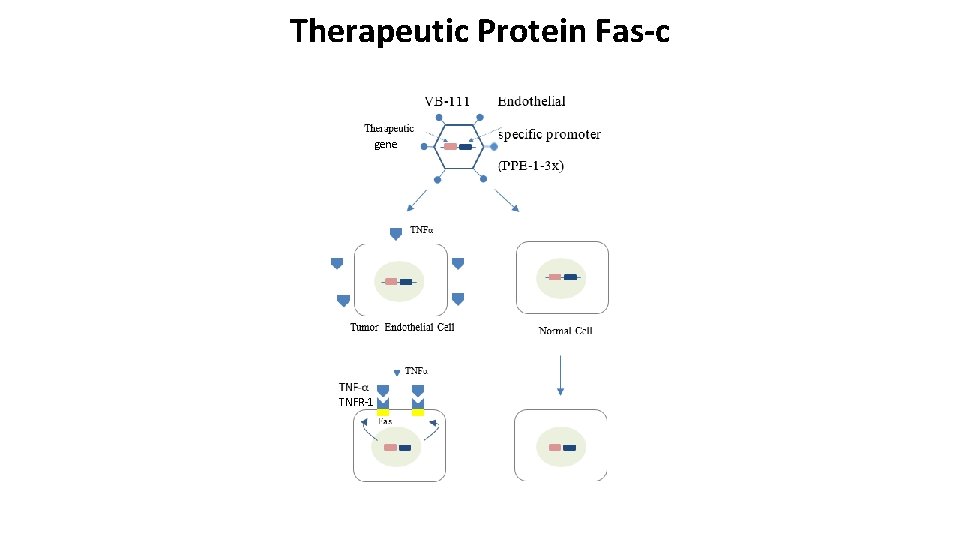
Therapeutic Protein Fas-c gene TNFR-1
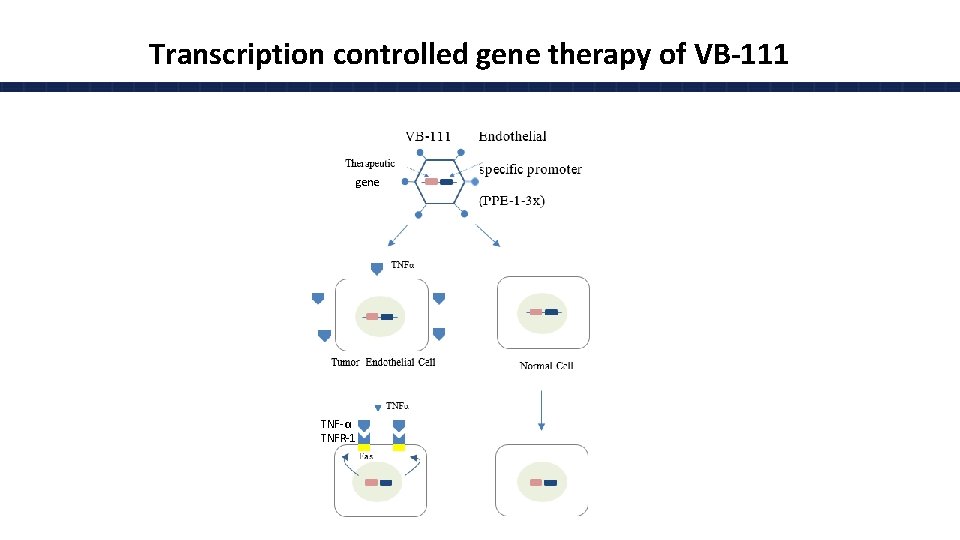
Transcription controlled gene therapy of VB-111 gene TNF-α TNFR-1
Goal Confirm & investigate the following biological results: 1. Confirm therapeutic effect of Fas-c on tumor cells 2. Explore how the production of TNF-α changes with tumor antigenicity c 3. Investigate whether TNF-α is dysregulated under the presence of tumor and determine if VB-111 treatment correct this dysregulation 4. Determine if effector cells behave differently when ad-5 is administered
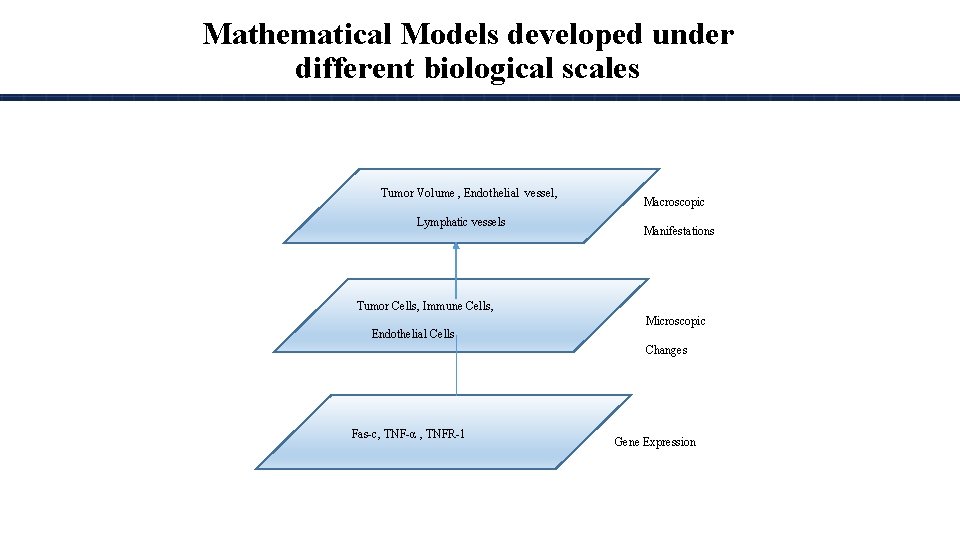
Mathematical Models developed under different biological scales Tumor Volume , Endothelial vessel, Lymphatic vessels Macroscopic Manifestations Tumor Cells, Immune Cells, Endothelial Cells Microscopic Changes Fas-c, TNF-α , TNFR-1 Gene Expression
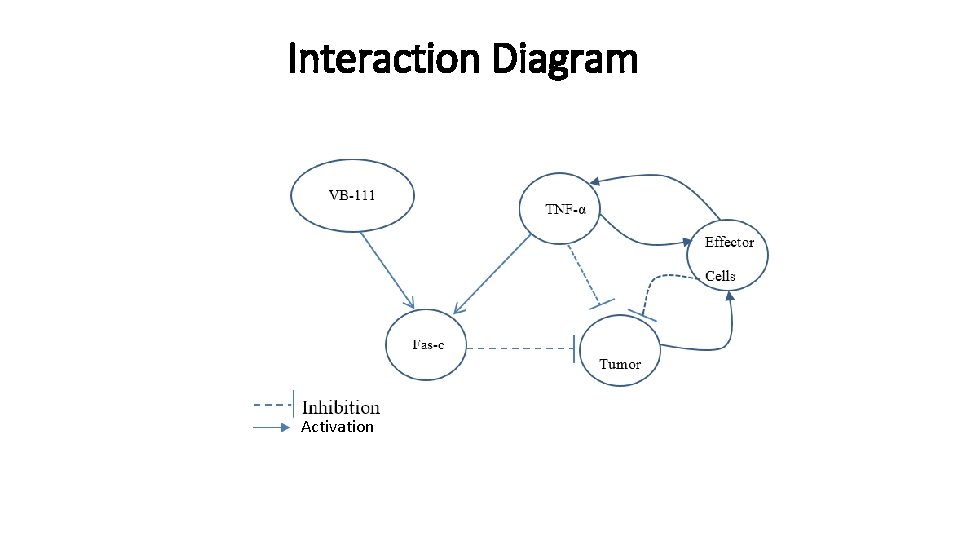
Interaction Diagram Activation
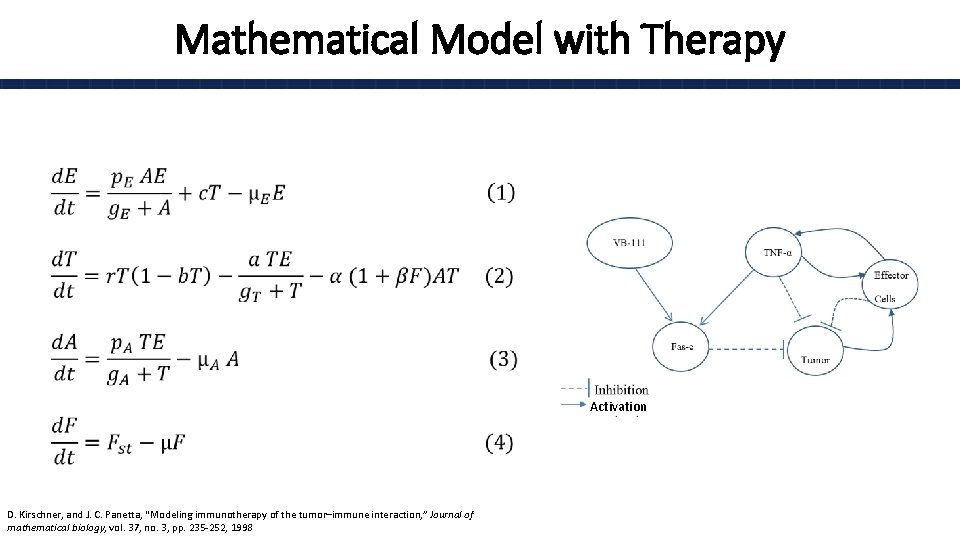
Mathematical Model with Therapy • Activation D. Kirschner, and J. C. Panetta, “Modeling immunotherapy of the tumor–immune interaction, ” Journal of mathematical biology, vol. 37, no. 3, pp. 235 -252, 1998
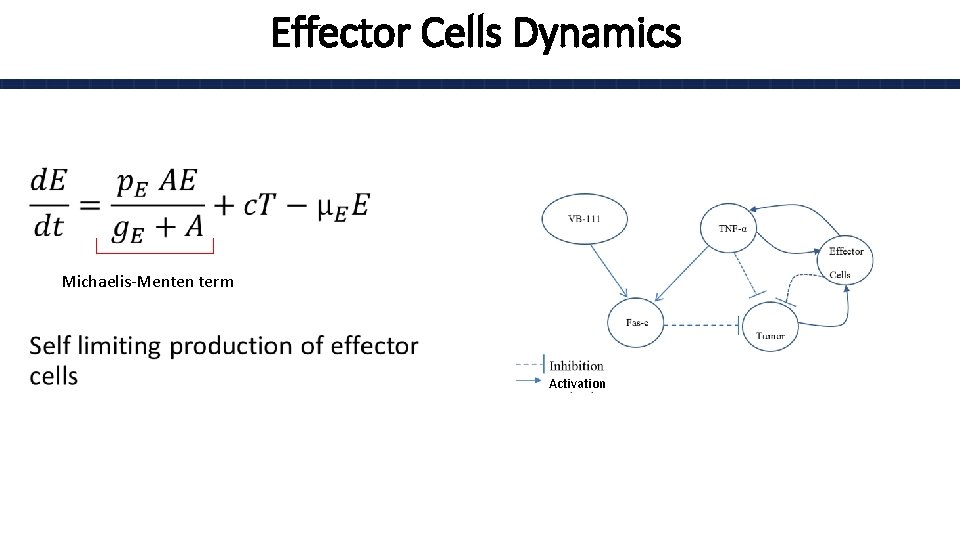
Effector Cells Dynamics • Michaelis-Menten term Activation
![Michaelis-Menten Equation • Hence: Michaelis constant or Half saturation constant [S] Michaelis-Menten Equation • Hence: Michaelis constant or Half saturation constant [S]](http://slidetodoc.com/presentation_image/244a505130e0cd4f977275cf0051432c/image-31.jpg)
Michaelis-Menten Equation • Hence: Michaelis constant or Half saturation constant [S]
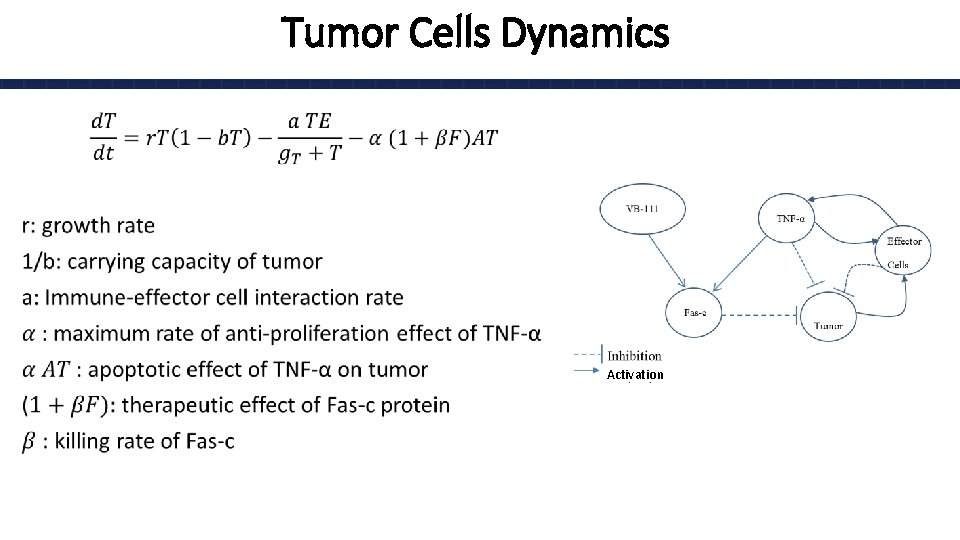
Tumor Cells Dynamics • Activation
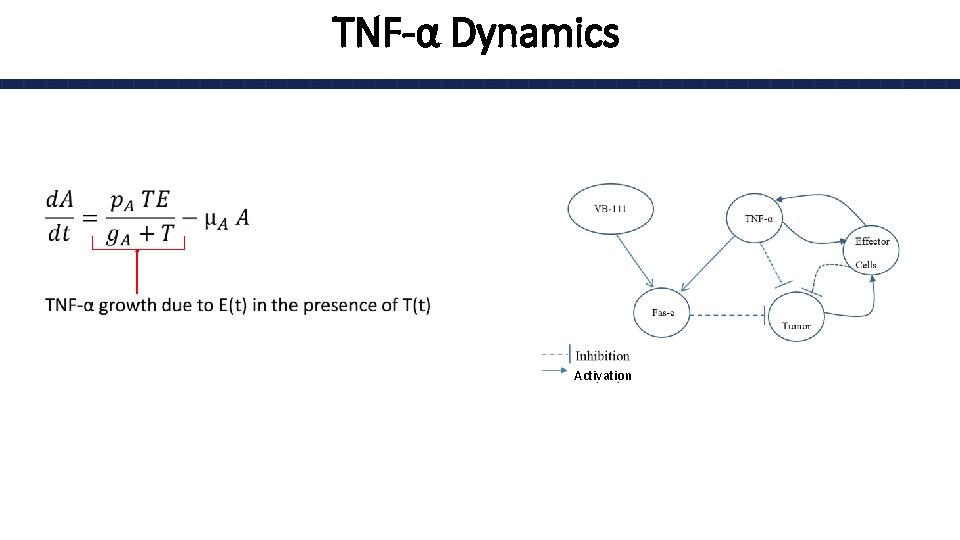
TNF-α Dynamics • Activation
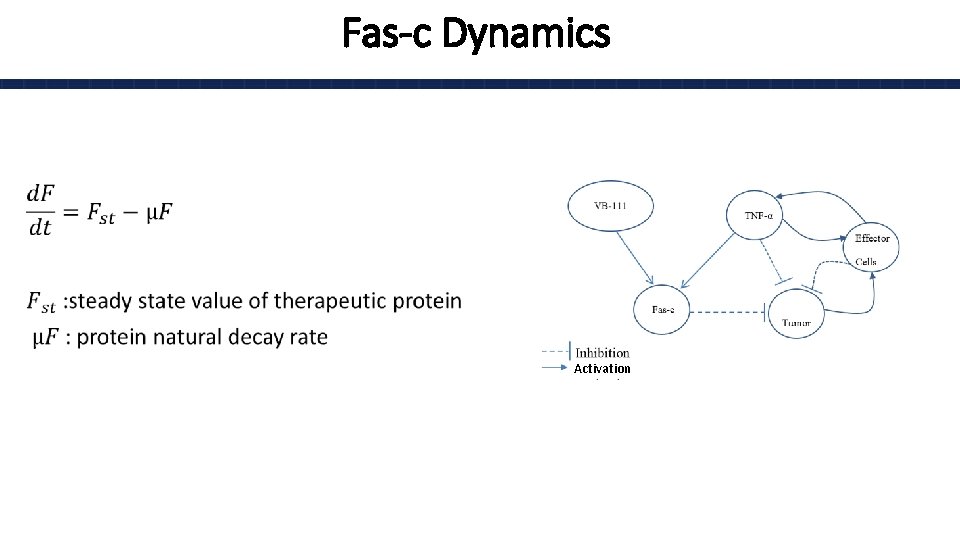
Fas-c Dynamics • Activation
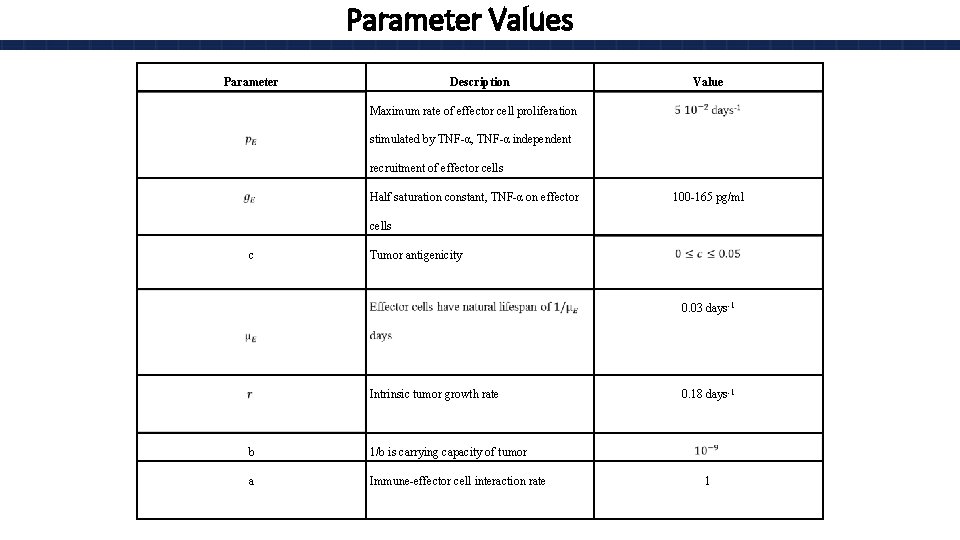
Parameter Values Parameter Description Value Maximum rate of effector cell proliferation stimulated by TNF-α, TNF-α independent recruitment of effector cells Half saturation constant, TNF-α on effector 100 -165 pg/ml cells c Tumor antigenicity 0. 03 days-1 Intrinsic tumor growth rate 0. 18 days-1 b 1/b is carrying capacity of tumor a Immune-effector cell interaction rate 1
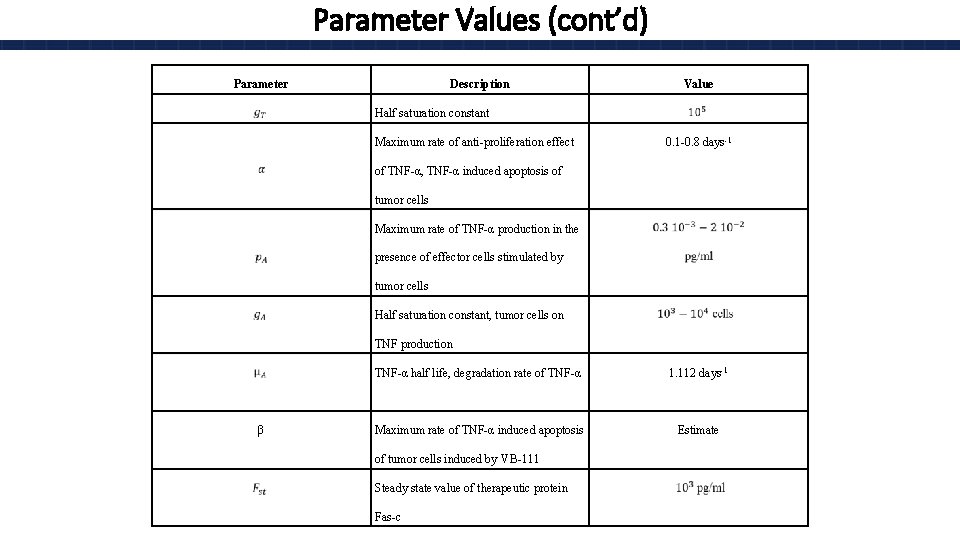
Parameter Values (cont’d) Parameter Description Value Half saturation constant Maximum rate of anti-proliferation effect 0. 1 -0. 8 days-1 of TNF-α, TNF-α induced apoptosis of tumor cells Maximum rate of TNF-α production in the presence of effector cells stimulated by tumor cells Half saturation constant, tumor cells on TNF production TNF-α half life, degradation rate of TNF-α 1. 112 days-1 β Maximum rate of TNF-α induced apoptosis of tumor cells induced by VB-111 Steady state value of therapeutic protein Fas-c Estimate

Case 1: Stability Analysis without VB-111 virotherapy •

Stability of Equilibrium Points •

Stability of Equilibrium Points •

Biologically realistic equilibrium points •

Tumor persistent equilibrium

Parameter Sensitivity Analysis • Parameters vary over a range of values • Our model is most sensitive to : • α: maximum rate of anti-proliferation effect of TNF α • c: tumor antigenicity


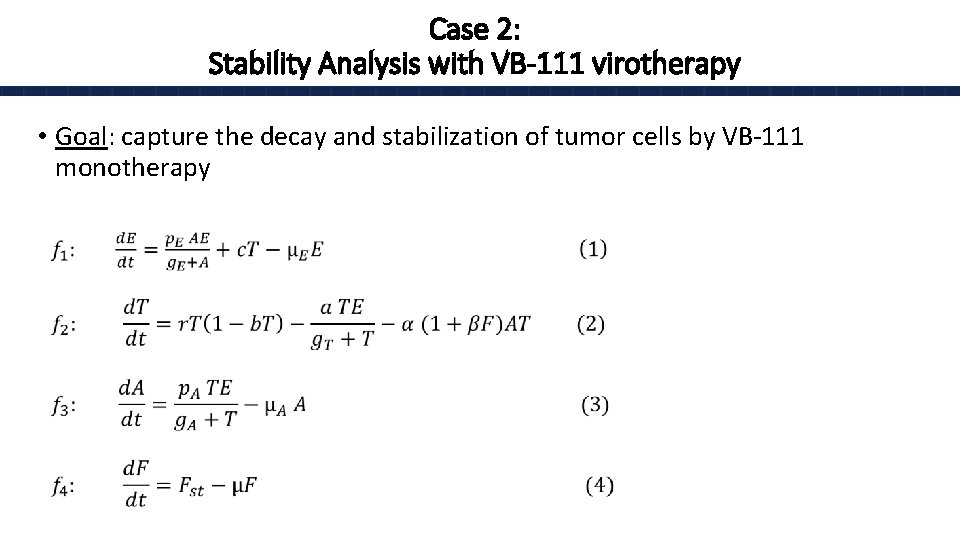
Case 2: Stability Analysis with VB-111 virotherapy • Goal: capture the decay and stabilization of tumor cells by VB-111 monotherapy

Equilibrium Points

Stability of Equilibrium Points •
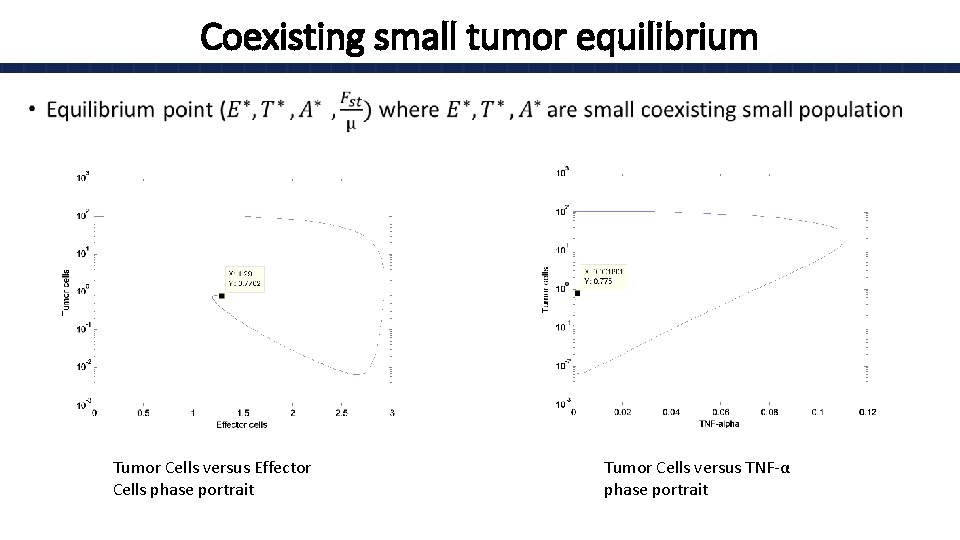
Coexisting small tumor equilibrium • Tumor Cells versus Effector Cells phase portrait Tumor Cells versus TNF-α phase portrait

Rise of therapeutic protein Fas-c
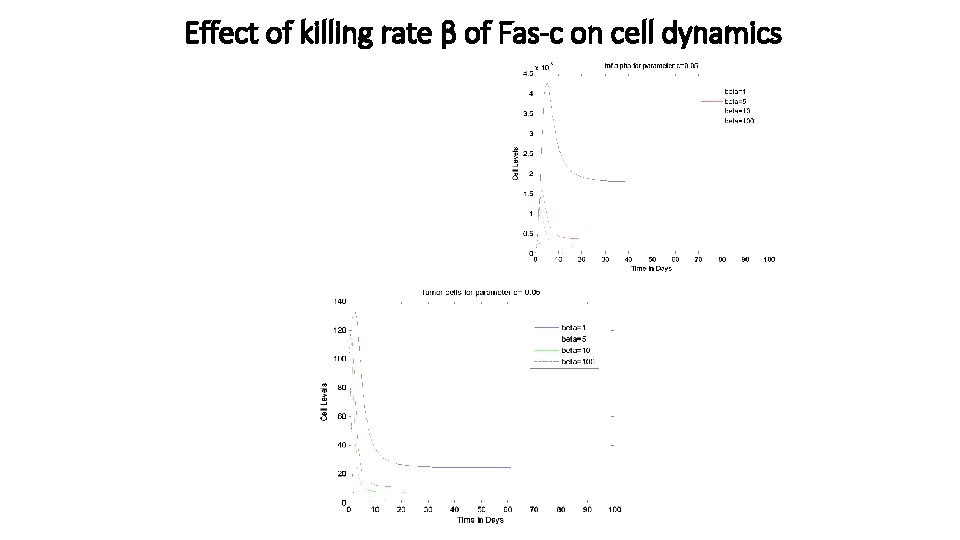
Effect of killing rate β of Fas-c on cell dynamics
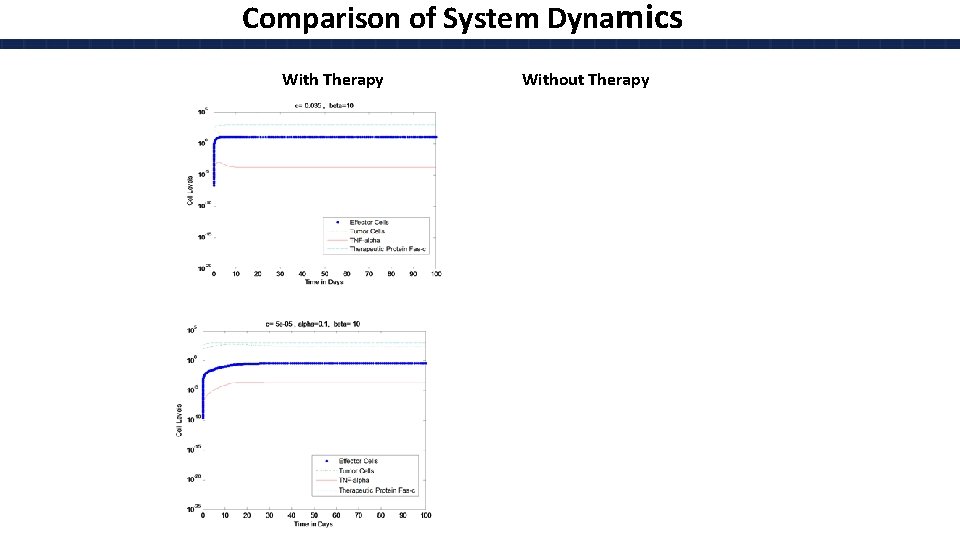
Comparison of System Dynamics With Therapy Without Therapy
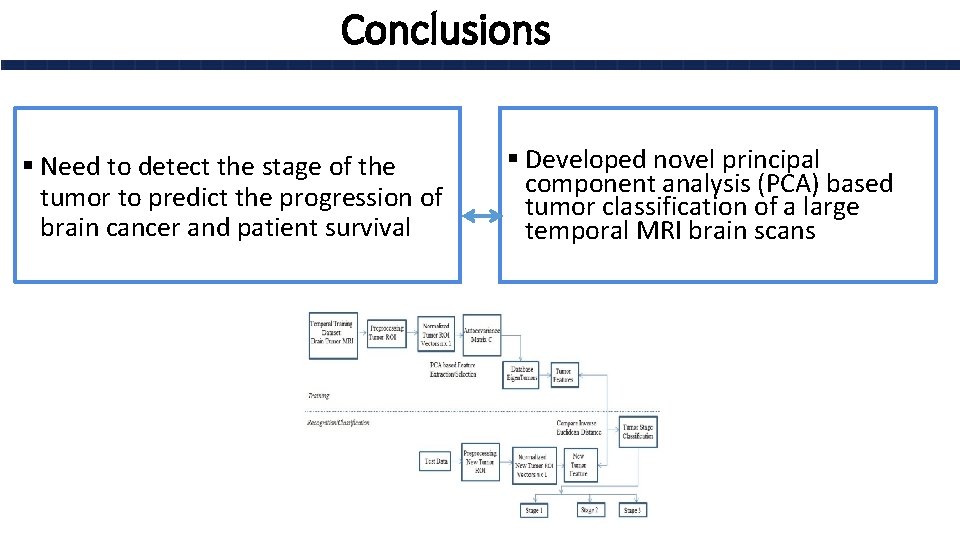
Conclusions § Need to detect the stage of the tumor to predict the progression of brain cancer and patient survival § Developed novel principal component analysis (PCA) based tumor classification of a large temporal MRI brain scans
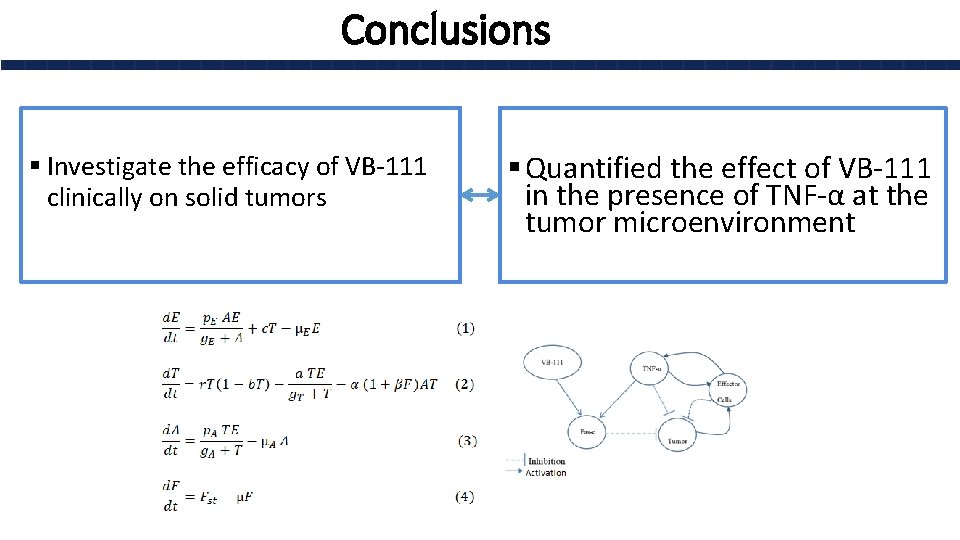
Conclusions § Investigate the efficacy of VB-111 clinically on solid tumors § Quantified the effect of VB-111 in the presence of TNF-α at the tumor microenvironment

Future Work § Image based modeling approach § Patient Specific and Disease Specific Parameters estimated from different imaging modalities -Examples: tumor growth, the diffusion tensor for tumor cells…. § One major challenge: lack of available human MRI time series data
![Publications [1] A. W. Daali, Y. Huang, and M. Jamshidi, "A system based approach Publications [1] A. W. Daali, Y. Huang, and M. Jamshidi, "A system based approach](http://slidetodoc.com/presentation_image/244a505130e0cd4f977275cf0051432c/image-55.jpg)
Publications [1] A. W. Daali, Y. Huang, and M. Jamshidi, "A system based approach to construct a Kaposi sarcoma-associated herpesvirus (KSHV) specific pathway crosstalk network“. System of System Engineering, IEEE 2013 pp. 273 -278 [2] A. W. Daali, M. Jamshidi, A. Brenner and A. Seifi, “A PCA based algorithm for longitudinal brain tumor stage recognition and classification. ” Engineering in Medicine and Biology Society (EMBC), 2015 37 th Annual International Conference of the IEEE. 25 -29 Aug. 2015. Milano, Italy [3] A. W. Daali, M. Jamshidi, A. Brenner and A. Seifi, “Mathematical model of dynamical behaviour of tumor system in response to VB-111 Virotherapy” IEEE Transactions on Biomedical Engineering, 2015 (submitted) [4] A. W. Daali, A. Kaissi, “Telemedicine: Opportunities & Challenges ”, Engineering in Medicine and Biology Society (EMBC), 2015 37 th Annual International Conference of the IEEE. 25 -29 Aug. 2015. Milano, Italy (submitted)
![References: [1] [2] [3] [4] [5] [6] [7] [8] [9] [10] [11] [12] [13] References: [1] [2] [3] [4] [5] [6] [7] [8] [9] [10] [11] [12] [13]](http://slidetodoc.com/presentation_image/244a505130e0cd4f977275cf0051432c/image-56.jpg)
References: [1] [2] [3] [4] [5] [6] [7] [8] [9] [10] [11] [12] [13] [14] [15] [16] A. Webb, and G. C. Kagadis, “Introduction to biomedical imaging, ” Medical Physics, vol. 30, no. 8, pp. 2267 -2267, 2003. M. Poustchi-Amin, S. A. Mirowitz, J. J. Brown, R. C. Mc. Kinstry, and T. Li, “Principles and Applications of Echo-planar Imaging: A Review for the General Radiologist 1, ” Radiographics, vol. 21, no. 3, pp. 767 -779, 2001. J. Hennig, A. Nauerth, and H. Friedburg, “RARE imaging: a fast imaging method for clinical MR, ” Magnetic Resonance in Medicine, vol. 3, no. 6, pp. 823 -833, 1986. D. Carr, J. Brown, G. Bydder, R. Steiner, H. Weinmann, U. Speck, A. Hall, and I. Young, “Gadolinium-DTPA as a contrast agent in MRI: initial clinical experience in 20 patients, ” American Journal of Roentgenology, vol. 143, no. 2, pp. 215 -224, 1984. A. B. T. Association, “Glioblastoma and Malignant Astrocytoma ”, 2012. A. Jain, J. C. Lai, G. M. Chowdhury, K. Behar, and A. Bhushan, “Glioblastoma: Current Chemotherapeutic Status and Need for New Targets and Approaches, ” Brain Tumors: Current and Emerging Therapeutic Strategies, In. Tech, Rijeka, pp. 145 -176, 2011. M. C. Tate, and M. K. Aghi, “Biology of angiogenesis and invasion in glioma, ” Neurotherapeutics, vol. 6, no. 3, pp. 447 -457, 2009. V. Therapeutics. "Phase I/II study shows safety and efficacy of VB-111 in patients with r. GBM, " http: //www. news-medical. net/news/20130603/Phase. III-study-shows-safety-and-efficacy-of-VB-111 -in-patients-with-r. GBM. aspx. A. J. Brenner, Y. C. Cohen, E. Breitbart, L. Bangio, J. Sarantopoulos, F. J. Giles, E. C. Borden, D. Harats, and P. L. Triozzi, “Phase I Dose-Escalation Study of VB-111, an Antiangiogenic Virotherapy, in Patients with Advanced Solid Tumors, ” Clinical Cancer Research, vol. 19, no. 14, pp. 3996 -4007, 2013. A. Brenner, Y. Cohen, E. Breitbart, J. Rogge, and F. Giles, "Antivascular activity of VB 111 in glioblastoma xenografts. " p. e 13652. B. A. Draper, W. S. Yambor, and J. R. Beveridge, “Analyzing pca-based face recognition algorithms: Eigenvector selection and distance measures, ” Empirical Evaluation Methods in Computer Vision, Singapore, pp. 1 -15, 2002. J. Zhou, E. Tryggestad, Z. Wen, B. Lal, T. Zhou, R. Grossman, S. Wang, K. Yan, D. -X. Fu, and E. Ford, “Differentiation between glioma and radiation necrosis using molecular magnetic resonance imaging of endogenous proteins and peptides, ” Nature medicine, vol. 17, no. 1, pp. 130 -134, 2011. C. Solomon, and T. Breckon, Fundamentals of Digital Image Processing: A practical approach with examples in Matlab: John Wiley & Sons, 2011. A. d’Onofrio, and A. Gandolfi, “Tumour eradication by antiangiogenic therapy: analysis and extensions of the model by Hahnfeldt et al. (1999), ” Mathematical biosciences, vol. 191, no. 2, pp. 159 -184, 2004. P. Hahnfeldt, D. Panigrahy, J. Folkman, and L. Hlatky, “Tumor development under angiogenic signaling a dynamical theory of tumor growth, treatment response, and postvascular dormancy, ” Cancer research, vol. 59, no. 19, pp. 4770 -4775, 1999. U. Ledzewicz, and H. Schättler, “Antiangiogenic therapy in cancer treatment as an optimal control problem, ” SIAM Journal on Control and

Thanks to: § Mo Jamshidi, Ph. D. , Chair § Chunjiang Qian, Ph. D. § Artyom Grigoryan, Ph. D. § David Akopian, Ph. D § Ali Seifi, M. D. UTHSCSA § Dr. Andrew Brenner, M. D. , Ph. D. § Dr. John Floyd, M. D.

Questions?
- Slides: 58