PBC and PSC Michael Nunez MD September 20

PBC and PSC Michael Nunez, MD September 20, 2004

PBC and PSC Cholestatic Liver Disease • • • medication induced TPN infections sepsis choledocholithiasis pancreatic malignancy pregnancy related infiltrative liver diseases primary biliary cirrhosis (PBC) primary sclerosing cholangitis (PSC) secondary sclerosing cholangitis graft vs. host disease

PBC and PSC Autoimmune Liver/Biliary Diseases • • PBC PSC autoimmune hepatitis autoimmune cholangitis (AMA-negative PBC)

PBC and PSC Primary Biliary Cirrhosis • misnomer – actually a nonsuppurative autoimmune cholangitis • autoimmune disease of the liver • predominantly affects middle-aged women • results in destruction of interlobular bile ducts • causes cholestasis and, eventually, cirrhosis • no cure

PBC and PSC PBC: Epidemiology • • worldwide distribution 90% of patients are female (9: 1 ratio) median age at presentation is 50 years (range 21 -91) prevalence of 20 -400 patients per million population - up to 650 per million in US women • possible genetic association based on familial studies

PBC and PSC PBC: Pathogenesis • cause or trigger remains unknown (alloantigen? ) • immune (T-cell) mediated attack that targets the epithelial cells of interlobular bile ducts • see B-cell elaboration of autoantibodies that may not be pathogenic - AMA is not pathogenic • intrahepatic bile duct destruction leads to cholestasis and fibrosis
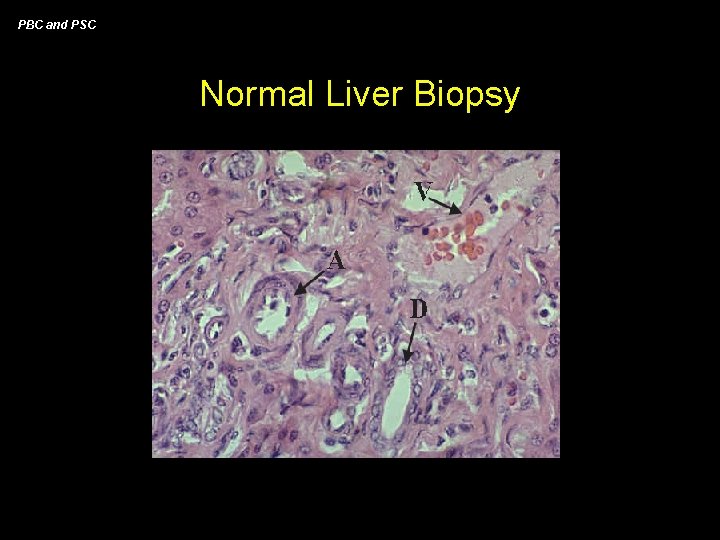
PBC and PSC Normal Liver Biopsy
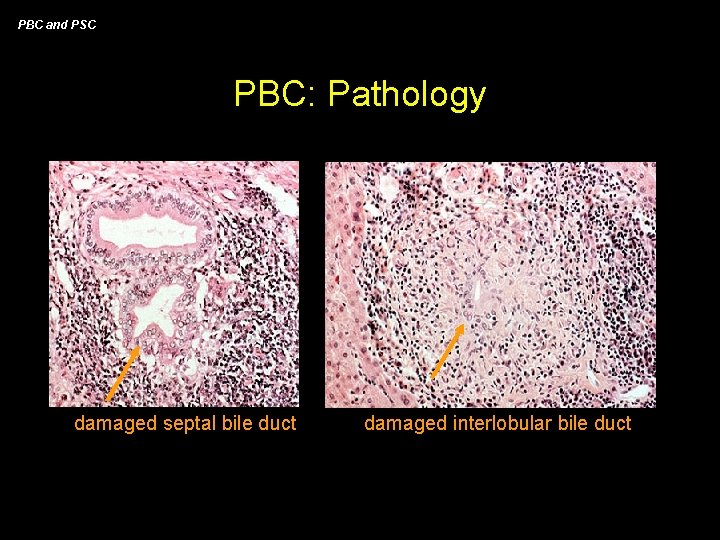
PBC and PSC PBC: Pathology damaged septal bile duct damaged interlobular bile duct
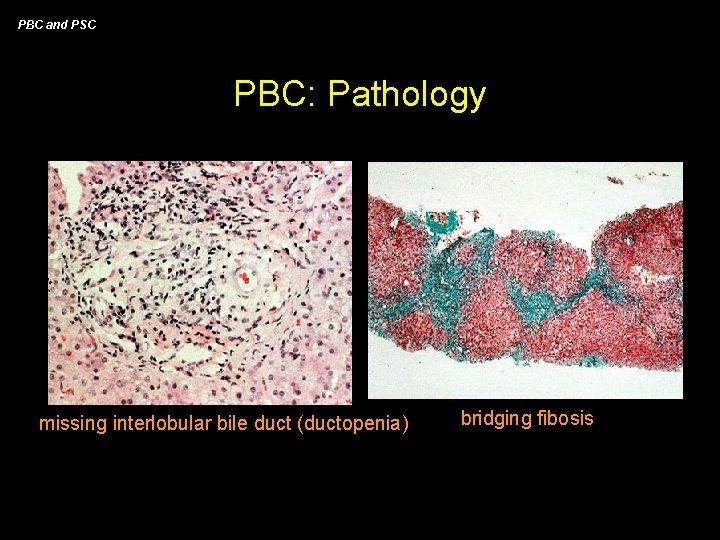
PBC and PSC PBC: Pathology missing interlobular bile duct (ductopenia) bridging fibosis
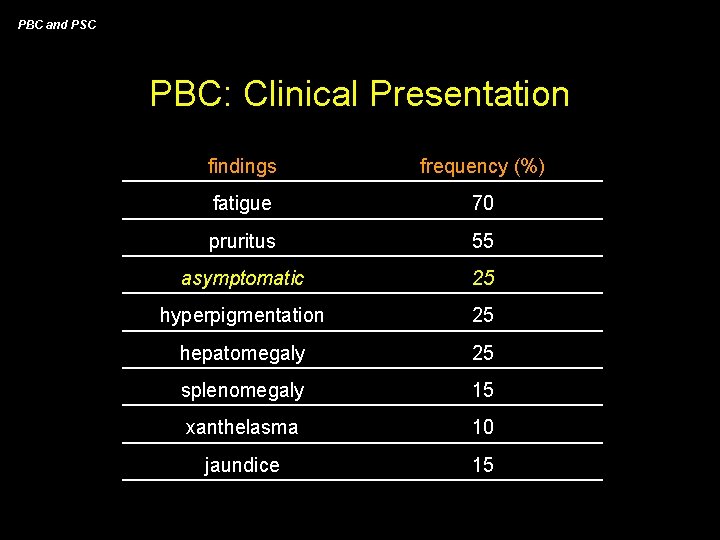
PBC and PSC PBC: Clinical Presentation findings frequency (%) fatigue 70 pruritus 55 asymptomatic 25 hyperpigmentation 25 hepatomegaly 25 splenomegaly 15 xanthelasma 10 jaundice 15
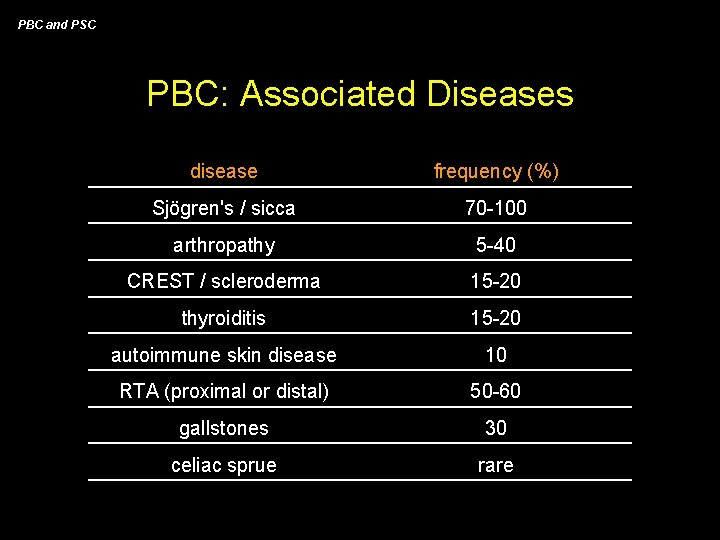
PBC and PSC PBC: Associated Diseases disease frequency (%) Sjögren's / sicca 70 -100 arthropathy 5 -40 CREST / scleroderma 15 -20 thyroiditis 15 -20 autoimmune skin disease 10 RTA (proximal or distal) 50 -60 gallstones 30 celiac sprue rare

PBC and PSC PBC: Diagnosis • abnormal liver function tests - alkaline phosphatase usually 3 -4 times elevated normal or minimally elevated transaminases (<3 x) elevated serum cholesterol and Ig. M often seen jaundice, hypoalbuminemia, and coagulopathy seen in later stages of the disease • serologic testing - AMA present in 90 -95% (the best have sens=98%, spec=96%) - RF found in 70% - ASMA in 66% - anti-thyroid in 40% - ANA in 35%

PBC and PSC PBC: Diagnosis • liver biopsy - gold standard to make diagnosis and exclude other diagnoses - stage 1 - portal triad inflammation - stage 2 - parenchymal (interface) hepatitis - stage 3 - fibrosis - stage 4 – cirrhosis • imaging studies - main utility in excluding biliary obstruction - can see increased hepatic echogenicity - can see lymphadenopathy in 25%

PBC and PSC PBC: Natural History and Prognosis • AMA positive with normal LFTs and asymptomatic - 29 patients followed (18 years average) • • • 24 with PBC on biopsy (83%) 2 with normal biopsies 24 developed abnormal LFTs at average of 5. 6 years 22 developed symptomatic disease no progression to cirrhosis or death from liver disease • asymptomatic PBC (AMA and biopsy) with abnormal LFTs - 40% develop symptoms in 5 -7 years - once symptomatic, life expectancy falls (median survival 10 years but a large range)

PBC and PSC PBC: Natural History and Prognosis • symptomatic PBC patients - independent predictors of poor prognosis • • advanced age bilirubin level (>10 portends 2 year avg. survival) poor synthetic function hepatomegaly ascites or edema variceal bleed advanced biopsy stage - prognostic models have been developed and validated http: //www. mayoclinic. org/gi-rst/mayomodel 2. html

PBC and PSC PBC: Treatment • traditional glucocorticoids - one controlled trial with benefits on biochemistry and histology - no change in mortality • colchicine - in 3 controlled trials, no prognostic or survival benefit • azathioprine - 248 patients without biochemical, histologic or survival benefit • cyclosporine - 349 patients without histologic or survival benefit • methotrexate - only one controlled trial with worse outcomes at 6 years

PBC and PSC PBC: Treatment • ursodeoxycholic acid (UDCA) - improves biochemistry, histology, and survival - 13 -15 mg/kg/day divided TID - FDA approved for PBC • budesonide and UDCA - well studied only in UDCA non-responders; no benefit in prognosis models - in naïve patients, improved biochemistry and histology (vs. UDCA alone), but no information on prognosis AMA-negative PBC seems to behave and respond the same as PBC, but may overlap with autoimmune hepatitis.

PBC and PSC PBC: Management • osteopenia and osteoporosis - lose bone mass at twice rate of controls risk of osteoporosis 8 times matched controls 50% of post transplant PBC patients suffer fractures treatment: exercise, calcium and vitamin D (25, 000 -100, 000 IU/week) - bisphonates need further study • fat soluble vitamins - monitor vitamins D, A and E - trial of vitamin K for prolonged prothrombin time • pruritus - cholestyramine 4 -16 gm/day divided before and after breakfast - rifampin or oral naltrexone can be useful in non-responders - can require transplantation

PBC and PSC PBC: Transplantation • survival is better if transplanted before a life-threatening complication or patient is on life support • common indications - portal hypertensive bleeding refractory ascites encephalopathy hepatorenal syndrome disabling fatigue disabling pruritus severe muscle wasting • one-year survival rates 90%; 5 -year >80% • post-transplant recurrence (by biopsy) in 30 -50% by 10 years but usually takes a benign course

PBC and PSC Primary Sclerosing Cholangitis • • most common type of sclerosing cholangitis in U. S. autoimmune disease of the biliary tree chronic inflammation and fibrosis of the bile ducts may occur in association with other diseases (IBD, scleroderma, SLE, sprue…) • but lacks a specific etiology (AIDS infections, parasites, operative injury, cystic fibrosis, RPC…) • no cure

PBC and PSC: Epidemiology • prevalence of 6 -8 per 100, 000 • up to 44% are asymptomatic at diagnosis • 80% of patients have concomitant IBD and 90% of those have ulcerative colitis (some years before symptoms) • 3 -6% of UC patients and 1% of Crohn’s patients have PSC • PSC and IBD progress independently • median age at diagnosis is 39 (neonates to octogenarians) • male: female ~ 1. 5: 1

PBC and PSC: Pathogenesis • theory: unknown trigger (toxin, infection, ischemia) in a genetically susceptible host - familial clustering reported class II and III HLA associations common autoantibodies (ANCA in 65 -85%) humoral and cellular immune dysfunction • intra- and extra-hepatic bile duct inflammation and fibrosis • stricture formation and obliteration - intra- and extra-hepatic ducts usually involved - 5% predominantly extra-hepatic - 25% predominantly intra-hepatic • leads to cholestasis and cirrhosis
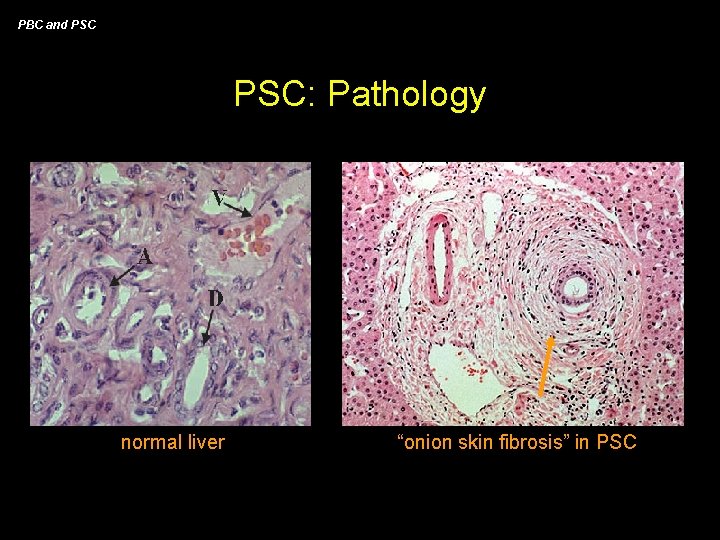
PBC and PSC: Pathology normal liver “onion skin fibrosis” in PSC
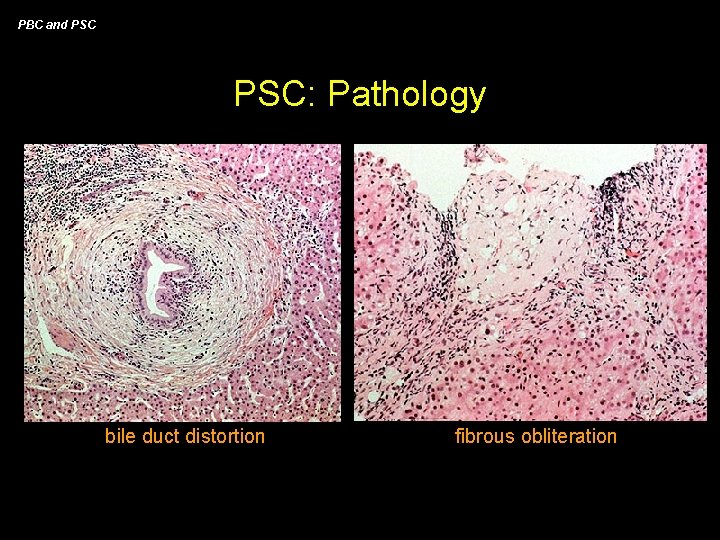
PBC and PSC: Pathology bile duct distortion fibrous obliteration
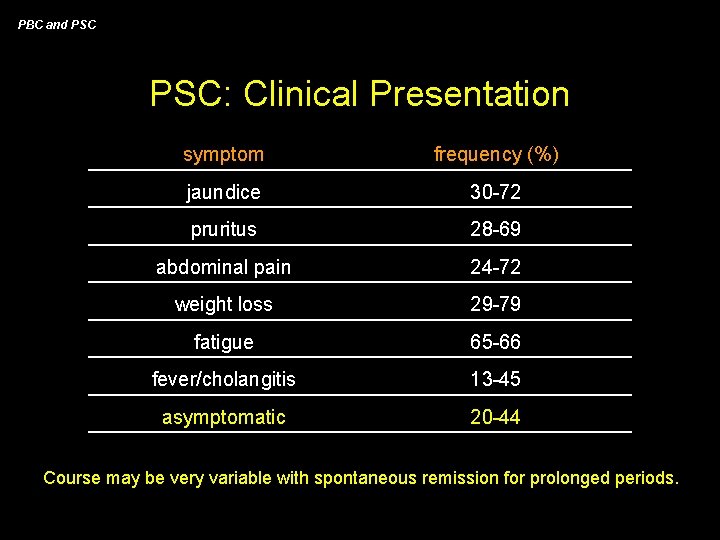
PBC and PSC: Clinical Presentation symptom frequency (%) jaundice 30 -72 pruritus 28 -69 abdominal pain 24 -72 weight loss 29 -79 fatigue 65 -66 fever/cholangitis 13 -45 asymptomatic 20 -44 Course may be very variable with spontaneous remission for prolonged periods.

PBC and PSC: Diagnosis • symptoms - high index of suspicion in IBD patients • physical findings - hepatomegaly - splenomegaly • laboratory - alkaline phosphatase elevation (usually 3 -fold or higher) • 6% have normal alkaline phosphatase - modest transaminase elevations (usually < 3 -fold) bilirubin may be normal small subset have marked eosinophilia 65 -85% are ANCA positive

PBC and PSC: Diagnosis • liver biopsy - “onion skin” fibrosis is most common (50% patients) - “obliterative fibrous cholangitis” is pathognomonic (10%) - most findings can be confused with chronic hepatitis or auto-immune hepatitis • imaging studies - non-specific findings variably present - dilated intra-hepatic ducts may be seen • cholangiography - ERCP considered the “gold standard” - MRCP reported to have PPV of 90% and sens/spec of ~85% compared to ERCP - 75% will have strictures at the bifurcation
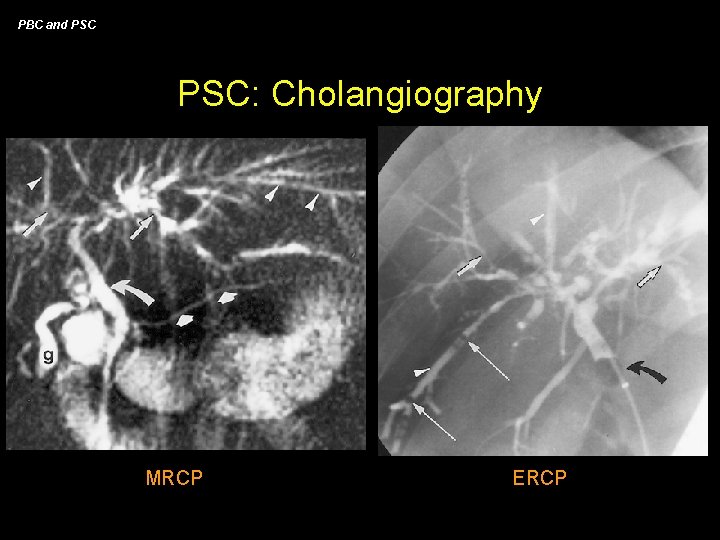
PBC and PSC: Cholangiography MRCP ERCP
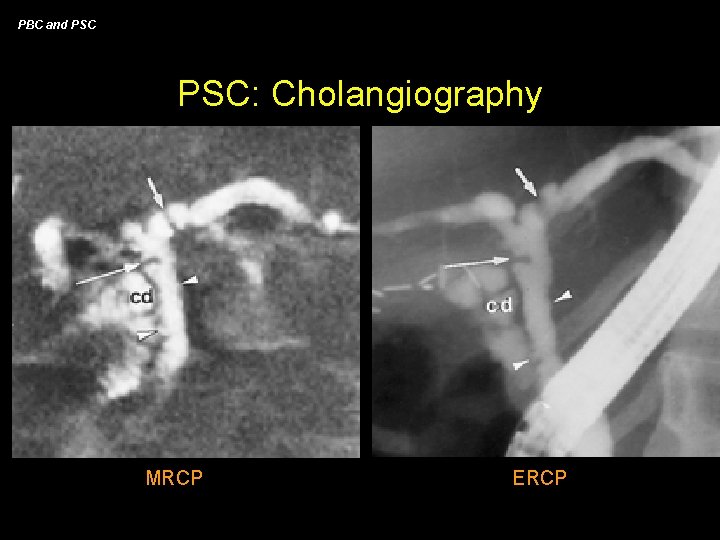
PBC and PSC: Cholangiography MRCP ERCP
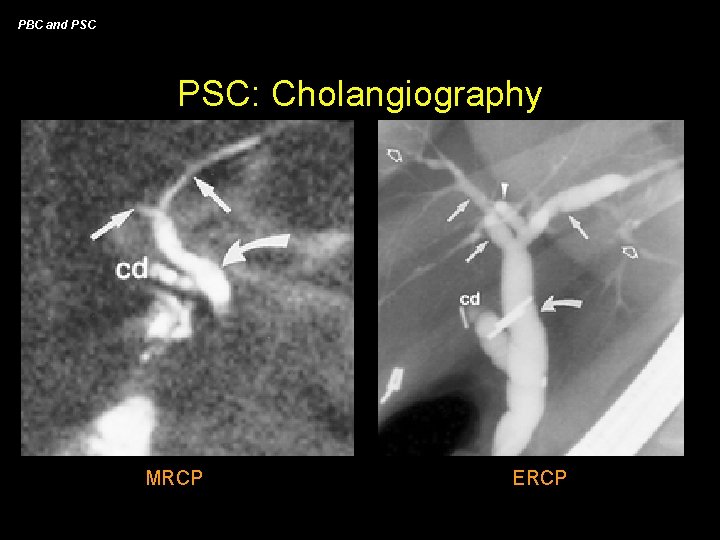
PBC and PSC: Cholangiography MRCP ERCP

PBC and PSC: Natural History and Prognosis • median survival or time to transplant is 12 years, but very variable and less predictable than PBC • some predictors of poor prognosis (Mayo model) - advanced age degree of bilirubin elevation low albumin high AST level variceal bleeding • Child-Pugh classification is used by UNOS (transplant listing) - class A: 90% 7 year survival - class B: 68% 7 year survival - class C: 25% 7 year survival

PBC and PSC: Natural History and Prognosis • malabsorption - steatorrhea - calcium malabsorption and osteoporosis - fat-soluble vitamin deficiencies • portal hypertension - bleeding - ascites • cholangiocarcinoma - median survival of 5 months diagnosed in 3 -20% of patients found in 30 -40% of PSC patients at autopsy found in 23 -33% of PSC patients at transplant tumor markers unproven as screening tools

PBC and PSC: Management • medical palliation - pruritus • cholestyramine • cholestipol • rifampin - bacterial cholangitis • antibiotics (gram neg bacilli, enterococci, bacteroides) - steatorrhea • fat-soluble vitamins • medium-chain triglycerides • interventional palliation - ERCP • dilation of dominant strictures • short-term stenting (7 -14 days) • stone removal

PBC and PSC: Transplantation • indications - complications of portal hypertension hepatic dysfunction disabling refractory symptoms recurrent cholangitis • usually done with a Roux-en-Y biliary anasamosis • excellent patient and graft survival rates • if cholangiocarcinoma is found in native liver, survival drops to 30% at one year • PSC recurs in 15 -20%
- Slides: 34