Patientspecific Cardiovascular Modeling System using Immersed Boundary Technique
Patient-specific Cardiovascular Modeling System using Immersed Boundary Technique Yu-Heng Tsenga, Wee-Beng Taya, Liang-Yu Linb, Wen-Yih Tsengc a. High Performance Computing & Environmental Fluid Dynamic Laboratory, Department of Atmospheric Sciences, National Taiwan University, Taipei, Taiwan (yhtseng@as. ntu. edu. tw) b. National Taiwan University Hospital, Taipei, Taiwan c. Center for Optoelectronic Biomedicine, National Taiwan University College of Medicine, Taipei, Taiwan * Special thanks to Peskin and Mcqueen for providing the CFD code

Outlines • Introduction • Patient-specific Cardiovascular Modeling System • 4 -D MRI system • Numerical methods • Results and discussions • Conclusion and future work 10/19/2021 2

Introduction • Develop a CFD based, patient-specific • • • cardiovascular modeling system Facilitate physicians’ diagnosis at early stage through hybrid CFD simulation and 4 -D MRI Use Immersed boundary method (IBM) to simulate fluid-elastic interaction of heart Investigate the vortex dynamic and effects of reservoir pressure boundary condition (RPBC) on the flows in Left Ventricle (LV) 10/19/2021 3
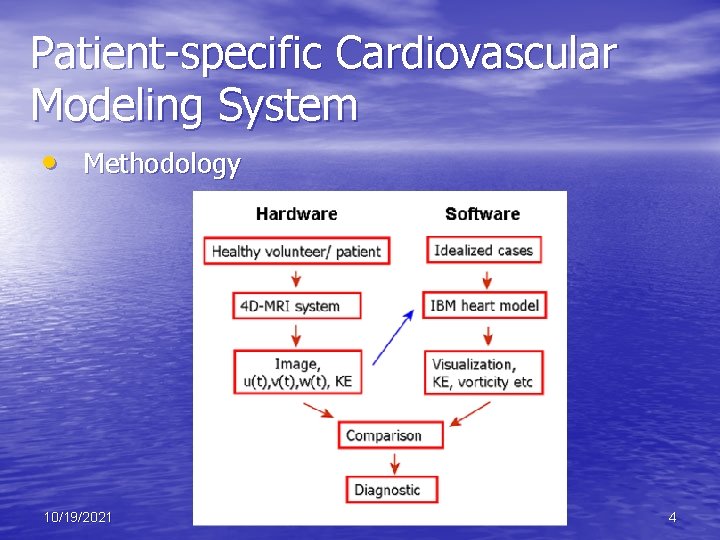
Patient-specific Cardiovascular Modeling System • Methodology 10/19/2021 4

Patient-specific Cardiovascular Modeling System • 4 -D phase contract magnetic resonance imaging (PC-MRI) system – – – Currently at the National Taiwan University Hospital Images acquired using an eight-channel phased-array body coil Time-resolved 3 D hemodynamic velocity fields – Allows one to reconstruct the 3 D images of the heart over a cardiac cycle – Data comprises of both healthy volunteer as well as patients with cardiac problems for comparison 10/19/2021 5
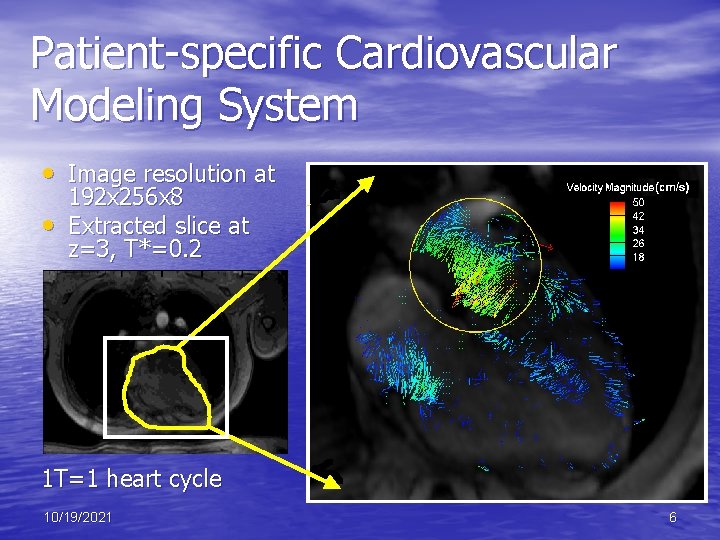
Patient-specific Cardiovascular Modeling System • Image resolution at • 192 x 256 x 8 Extracted slice at z=3, T*=0. 2 1 T=1 heart cycle 10/19/2021 6

Numerical Method – IBM (Lai and Peskin, 2000) • Incompressible Navier-Stokes equations (f represents force density) • Interaction between immersed boundary, fluid and boundary forces 10/19/2021 7

Numerical Method - IBM 10/19/2021 8
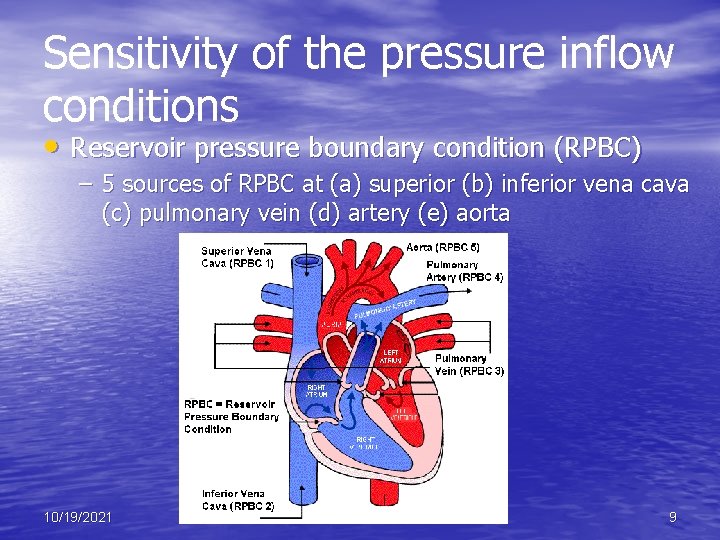
Sensitivity of the pressure inflow conditions • Reservoir pressure boundary condition (RPBC) – 5 sources of RPBC at (a) superior (b) inferior vena cava (c) pulmonary vein (d) artery (e) aorta 10/19/2021 9

Sensitivity of the pressure inflow conditions • Influence of reservoir pressure boundary condition (RPBC) – Investigate the effects/impacts of different pressure BC on the simulation results – Study vortex dynamics of left ventricle (LV) Run Description 1 Constant RPBC, unmodified 2 Similar to Run 1, except that the pulmonary vein (PV) pressure is 25% smaller 3 Similar to Run 1, except that the PV pressure is 25% larger 4 Varying RPBC, realistic data of a healthy volunteer over a heartbeat cycle (Abdallah, 2009) 10/19/2021 10
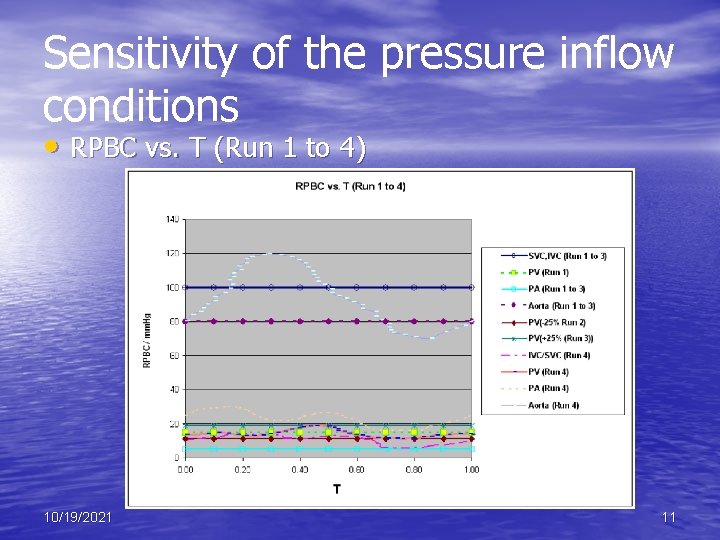
Sensitivity of the pressure inflow conditions • RPBC vs. T (Run 1 to 4) 10/19/2021 11
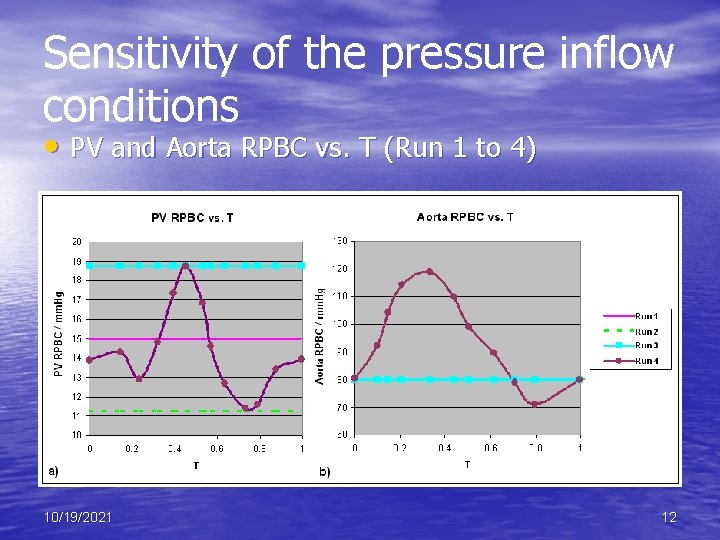
Sensitivity of the pressure inflow conditions • PV and Aorta RPBC vs. T (Run 1 to 4) 10/19/2021 12
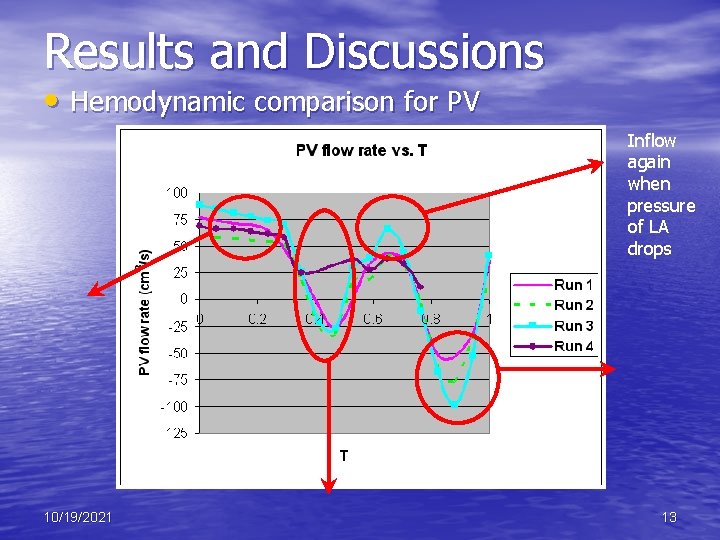
Results and Discussions • Hemodynamic comparison for PV Inflow again when pressure of LA drops 10/19/2021 13
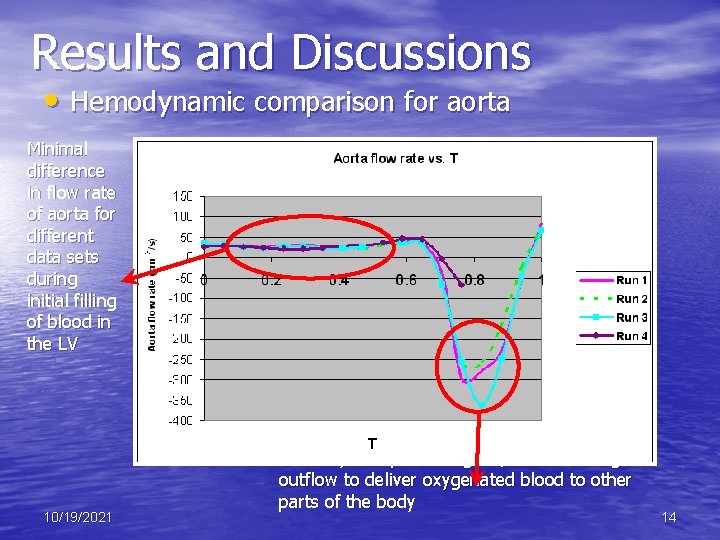
Results and Discussions • Hemodynamic comparison for aorta Minimal difference in flow rate of aorta for different data sets during initial filling of blood in the LV 10/19/2021 When systole phase begins , there is a large outflow to deliver oxygenated blood to other parts of the body 14
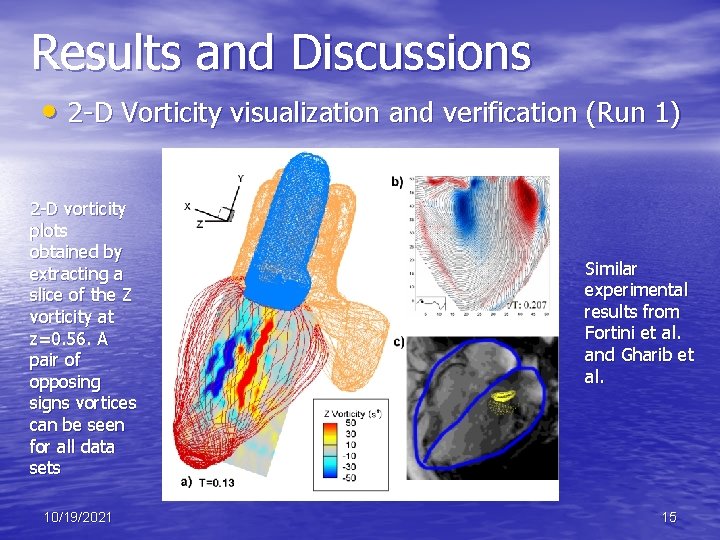
Results and Discussions • 2 -D Vorticity visualization and verification (Run 1) 2 -D vorticity plots obtained by extracting a slice of the Z vorticity at z=0. 56 A pair of opposing signs vortices can be seen for all data sets 10/19/2021 Similar experimental results from Fortini et al. and Gharib et al. 15
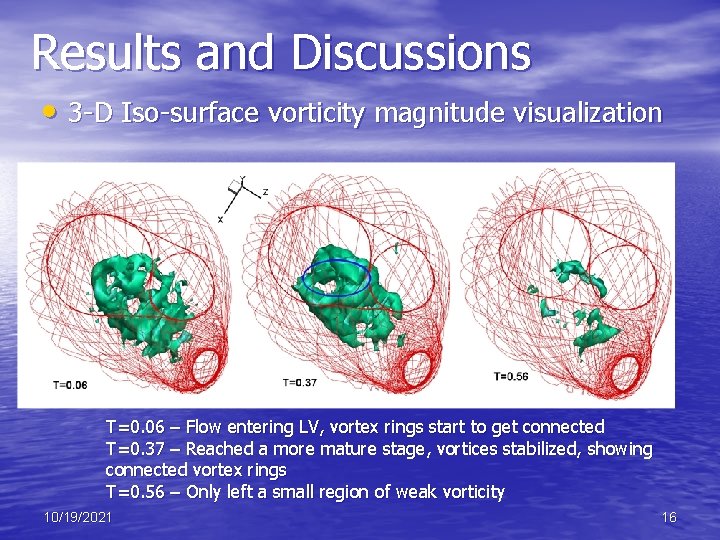
Results and Discussions • 3 -D Iso-surface vorticity magnitude visualization T=0. 06 – Flow entering LV, vortex rings start to get connected T=0. 37 – Reached a more mature stage, vortices stabilized, showing connected vortex rings T=0. 56 – Only left a small region of weak vorticity 10/19/2021 16

Results and Discussions • Vortex formation time Tv (Gharib et al. , 2006) – A good indicator of the cardiac health of the patient – – – EDV = LV end-diastolic volume (LV filling), = time-averaged mitral (annulus) valve diameter, EF = ejection fraction, ESV = LV volume at the end of systole (LV ejection), SV = the stroke volume, difference between ESV and EDV 10/19/2021 17
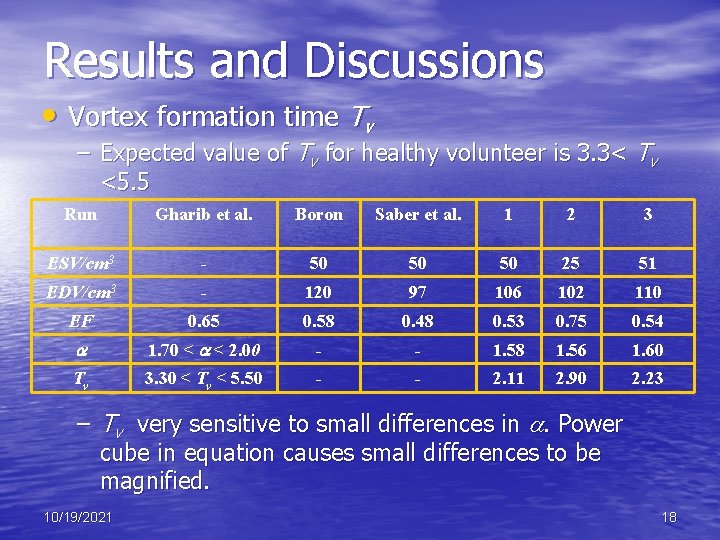
Results and Discussions • Vortex formation time Tv – Expected value of Tv for healthy volunteer is 3. 3< Tv <5. 5 Run Gharib et al. Boron Saber et al. 1 2 3 ESV/cm 3 - 50 50 50 25 51 EDV/cm 3 - 120 97 106 102 110 EF 0. 65 0. 58 0. 48 0. 53 0. 75 0. 54 1. 70 < < 2. 00 - - 1. 58 1. 56 1. 60 Tv 3. 30 < Tv < 5. 50 - - 2. 11 2. 90 2. 23 – Tv very sensitive to small differences in . Power cube in equation causes small differences to be magnified. 10/19/2021 18
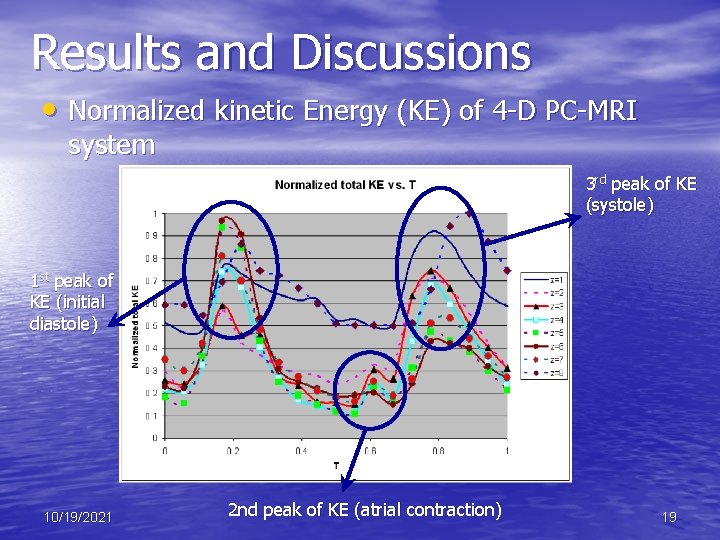
Results and Discussions • Normalized kinetic Energy (KE) of 4 -D PC-MRI system 3 rd peak of KE (systole) 1 st peak of KE (initial diastole) 10/19/2021 2 nd peak of KE (atrial contraction) 19
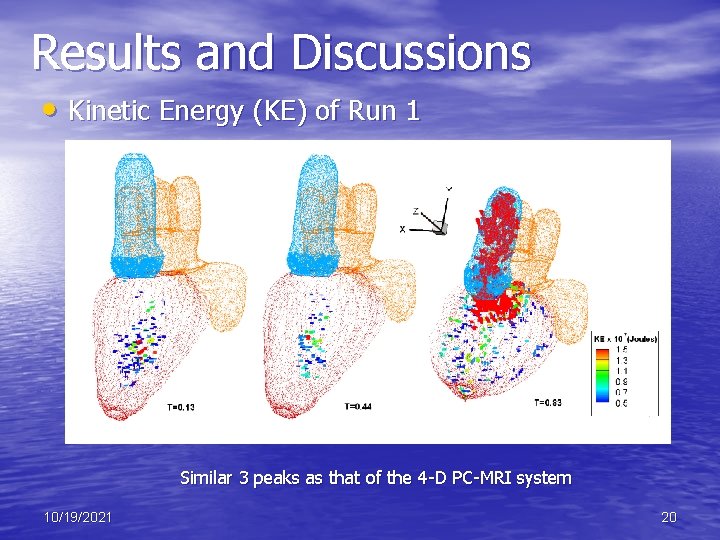
Results and Discussions • Kinetic Energy (KE) of Run 1 Similar 3 peaks as that of the 4 -D PC-MRI system 10/19/2021 20
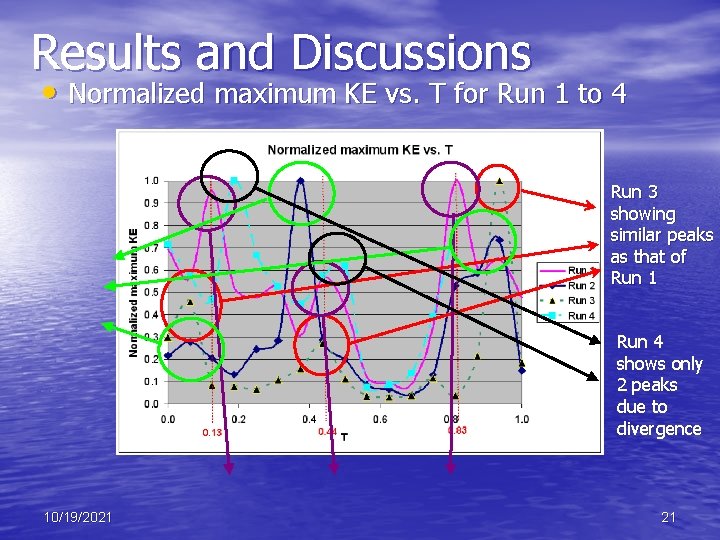
Results and Discussions • Normalized maximum KE vs. T for Run 1 to 4 Run 3 showing similar peaks as that of Run 1 Run 4 shows only 2 peaks due to divergence 10/19/2021 21
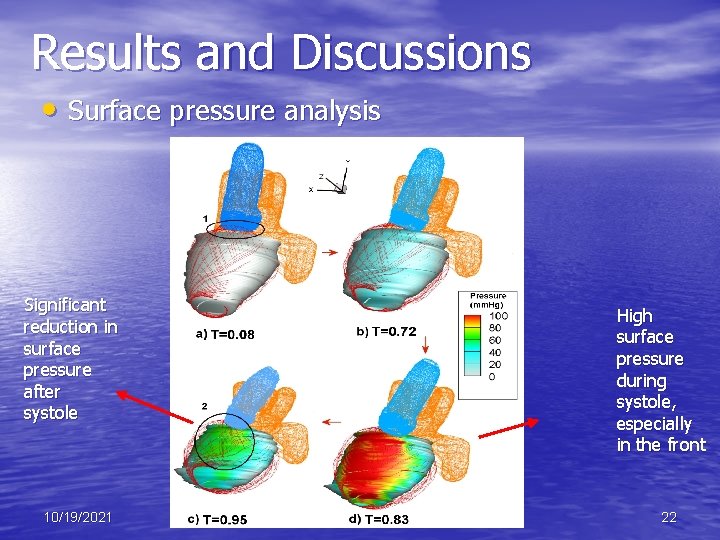
Results and Discussions • Surface pressure analysis Significant reduction in surface pressure after systole 10/19/2021 High surface pressure during systole, especially in the front 22
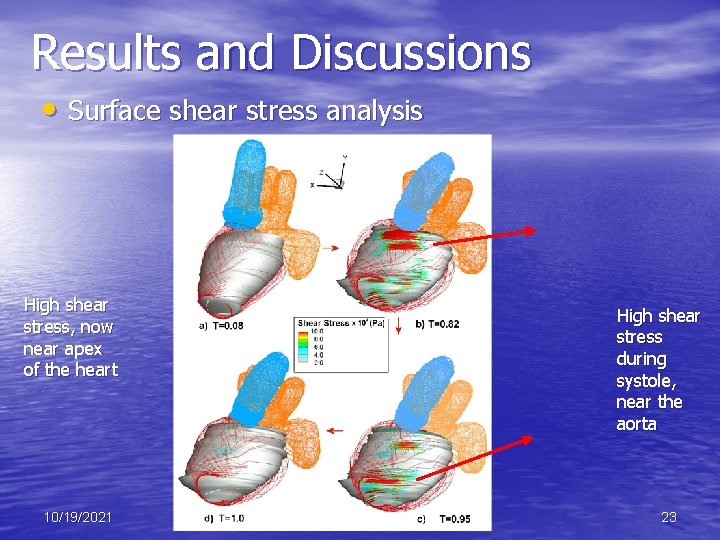
Results and Discussions • Surface shear stress analysis High shear stress, now near apex of the heart 10/19/2021 High shear stress during systole, near the aorta 23

Conclusions and future work • Patient specific cardiovascular modeling system • Simulation of heart using IBM • 4 -D PC-MRI system • Investigate the effect of RPBC on different variables such • • as KE, vorticity etc Verified with experimental results from MRI and other means through KE, vorticity Visualization of pressure and shear stress distribution on heart surface Further investigation of the realistic reservoir pressure BC is required Future work to include input of patient specific data in CFD code 10/19/2021 24

Questions? 10/19/2021 25
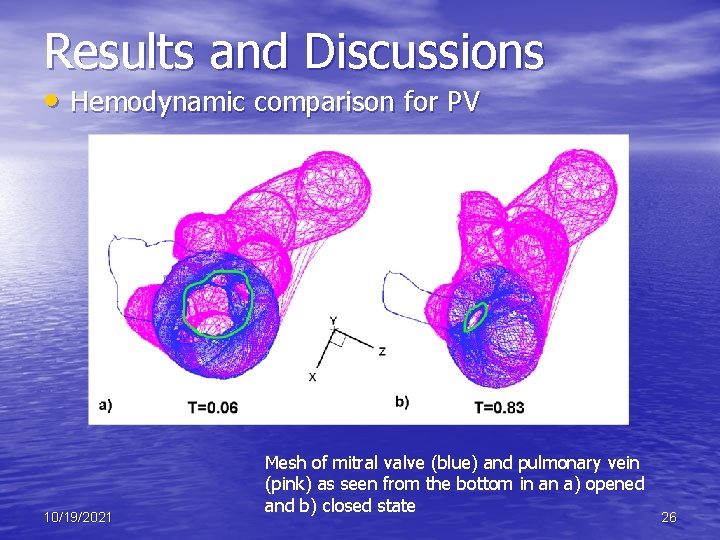
Results and Discussions • Hemodynamic comparison for PV 10/19/2021 Mesh of mitral valve (blue) and pulmonary vein (pink) as seen from the bottom in an a) opened and b) closed state 26
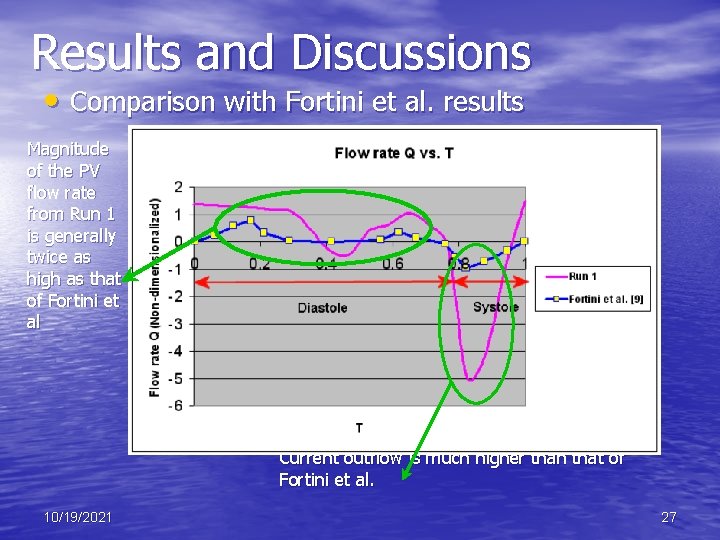
Results and Discussions • Comparison with Fortini et al. results Magnitude of the PV flow rate from Run 1 is generally twice as high as that of Fortini et al Current outflow is much higher than that of Fortini et al. 10/19/2021 27
- Slides: 27