PatientCentered Care Unit 5 PatientProvider Communication Lecture b

Patient-Centered Care Unit 5: Patient-Provider Communication Lecture b – Trust and Respectful Interactions This material (Comp 25 Unit 5) was developed by Columbia University, funded by the Department of Health and Human Services, Office of the National Coordinator for Health Information Technology under Award Number 90 WT 0006. This work is licensed under the Creative Commons Attribution-Non. Commercial-Share. Alike 4. 0 International License. To view a copy of this license, visit http: //creativecommons. org/licenses/by-nc-sa/4. 0/.

Patient-Provider Communication Learning Objectives • Objective 1: Explain the importance, elements, and processes of patient-physician communication (Lecture a) • Objective 2: Discuss the concept of trust in the context of health care interactions (Lecture b) • Objective 3: Describe various informatics tools and the practical considerations to support patient-provider communication (Lecture c) 2

What is trust? : definitions • “Trust relationships are characterized by one party, the trustor, having positive expectations regarding both the competence of the other party (competence trust), the trustee, and that they will work in their best interests (intentional trust)” • “confidence in and reliance upon others, whether individuals, professionals, or organizations, to act in accord with accepted social, ethical, and legal norms” • (Institute of Medicine, 2001) 3

Characteristics of trust are specific to health care context • Stronger affective component (vulnerability) • Altruism, or working in best interests of patient (honesty, confidentiality, caring and showing respect) • Competence (social and technical) 4
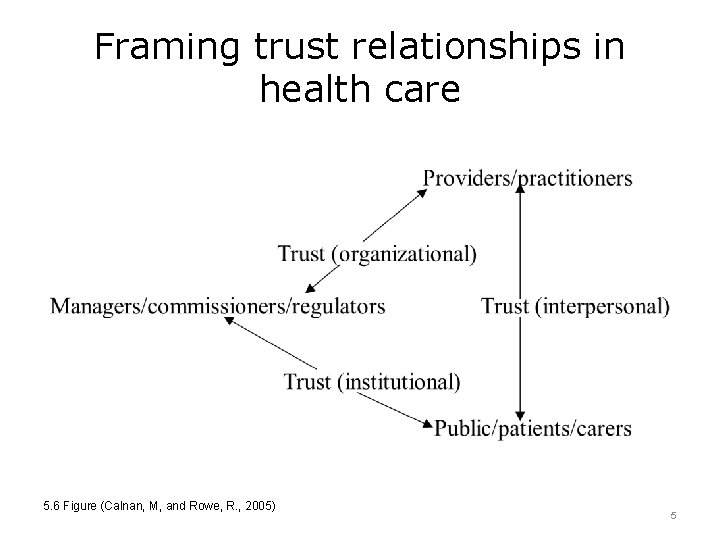
Framing trust relationships in health care 5. 6 Figure (Calnan, M, and Rowe, R. , 2005) 5

Trust: Does it matter? • Those seeking health care frequently experiencing uncertainty • Patients are vulnerable and dependent on the provider for quality care • There is an indirect influence on health outcomes through a direct therapeutic effect of empathy and caring • Trust is also an important characteristic of employees and health care staff in the workplace • Trust exhibited on the part of the employer contributes to job satisfaction and a culture of trust • (Calnan and Rowe, 2005) 6

Transactional Trust Model • Competence Trust – Trust of capability • Contractual Trust – Trust of character • Communication Trust – Trust of disclosure • (Hoylton-Rushton, Reina, & Reina, 2007) 7

Developing a trusting and connected relationship • • • Understanding the patient’s needs Displaying caring actions and attitudes Providing holistic care Acting as the patient’s advocate (Mok and Chiu, 2004) 8

The costs or dangers of trust • Abuse of trust with vulnerable patients, particularly those with limited resources • Easier to trust if powerful and wealthy • Tension between development of trust and patient empowerment 9

Drivers of change • Top down policy initiatives – E. g. performance management • Wider social and cultural change – E. g. decline in deference to authority • Negative media coverage of ‘medical scandals’ – E. g. the Tuskegee study by U. S. Public Health Service 10

How are trust relations changing? • There is high trust in professional self-regulation, such as the American Medical Association (AMA) • Patients trust clinical recommendations for treatment • Patients’ passively trust primary care providers to determine access to specialist services • Greater external regulation and monitoring decreases trust • Increased expectations of patient self-care requires more clinical trust 11

New forms of trust relations • • • Shift from affect to more cognition-based Greater interdependence in trust relations Role of information in trust creation Importance of institutional trust More informed, but conditional, trust 12
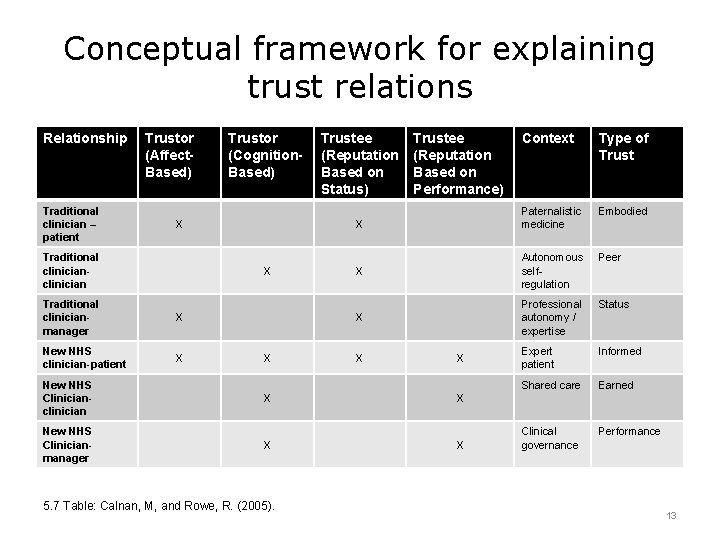

Conceptual framework for explaining trust relations Relationship Traditional clinician – patient Trustor (Affect. Based) X Traditional clinician X New NHS clinician-patient X New NHS Clinicianmanager Trustee (Reputation Based on Status) Trustee (Reputation Based on Performance) Context Type of Trust Paternalistic medicine Embodied Autonomous selfregulation Peer X Professional autonomy / expertise Status X Expert patient Informed Shared care Earned Clinical governance Performance X X Traditional clinicianmanager New NHS Clinicianclinician Trustor (Cognition. Based) X X X 5. 7 Table: Calnan, M, and Rowe, R. (2005). X X 13

Conditional trust behavior • • • Managing expectations Establishing boundaries Delegating appropriately Encouraging mutually serving intentions Keeping agreements and consistency (Calnan and Rowe, 2005) 14

Conditional trust behavior (Cont’d) • High trust behavior – Minimal checking – Informal, unwritten rules – Significant professional – – autonomy Willingness to take risks Willingness to divulge information Passive, deferent role Advice is accepted unquestioningly (Calnan and Rowe, 2005) • Low trust behavior – Constant monitoring – Detailed and prescriptive – – regulations Intense supervision and little delegation of authority Information is withheld Questioning, possibly skeptical, role Request for a second opinion or alternative source of treatment 15

Contractual trust attitudes 5. 8 Table (Calnan, M, and Rowe, R. , 2005). 16

Patients’ beliefs and behaviors if there is embodied trust • Patients have a more passive, deferent role • Information is valued for the respect it shows rather than its content • Advice / recommendations are accepted unquestioningly • Trust relates to ‘family’ / ‘personal’ experience of doctor • There is an association between the level of direct contact and level of trust (Calnan and Rowe, 2005) • There is minimal checking or monitoring with managers and clinicians being given considerable autonomy in decision-making • Rules are unwritten and informal and processes are not prescriptive • There is an assumption that the other party is wellintentioned towards you • A clinician’s altruism is unquestioned • Willingness to take risks is based on the reputation of the organisation or individual 17

Patients’ beliefs and behaviors if there is informed trust • Information is used to calculate whether trust is warranted • Careful monitoring, supervision, and checking (possibly covert) • Patients want to play a more equal role in decisionmaking • Patients expect doctors to trust their ability / competence to self-manage (Calnan and Rowe, 2005) • Patients may be more questioning of treatment recommendations • They may express greater suspicion and scepticism about other’s intentions • Willingness to take risks is based on careful weighing up of the situation 18

Providers’ beliefs and behaviors if there is peer trust • An individual clinician’s authority and reputation are based on their position in the medical hierarchy, personal networks and word of mouth recommendation. • Senior clinicians’ views and decisions are unquestioned. • Clinical freedom is unquestioned • Performance is selfregulated, individually assessed and not publicly reported (Calnan and Rowe, 2005) • Complex patients are only seen by senior doctors • ‘Successful’ relations between clinicians are based on conforming to traditional roles • Trust is generally higher between clinicians of the same profession and specialism 19

Providers’ beliefs and behaviors if there is “earned” trust • An individual clinician’s authority and reputation are based on their proven skills and competence, and being up-to-date with medical technology • Clinical freedom may be limited and trust gained by following agreed protocols and an ability to work well in a team • Careful performance monitoring against targets • Both complex and easy patients may be seen by junior clinicians on the basis that they are following agreed protocols (Calnan and Rowe, 2005) • ‘Successful’ relations between clinicians are based on mutual respect for their different skills • Trust may be higher between clinicians who have experience of working together, irrespective of their profession or specialism • Communication skills and providing information are important in building trust. • Junior clinicians may question the views of their seniors. 20

Managers’ beliefs and behaviors if there is status trust • A clinician’s authority relates to their position and role within the hospital / organization • Rules are unwritten and there is minimal monitoring of clinical activity • Trust is one way – clinicians have little need to trust managers, whereas managers have to trust clinicians • In decision-making, managers act as administrators, trusting clinicians with strategic decisions about service development • Managers are not involved in monitoring or checking clinical activity • (Calnan and Rowe, 2005) 21

Managers’ beliefs and behaviors if there is performance trust • A clinician’s authority relates to their ability to meet targets, as well as their position within the organization • Trust is likely to be higher in those clinicians who have some managerial role • A willingness to provide information on clinical activity and to engage with managerial agendas creates trust • In ‘successful’ clinician-manager relations trust is important because it reduces the need for checking and monitoring • Trust is two-way – clinicians need to work with managers to secure resources and to develop services • In decision-making, managers work with clinicians to make strategic decisions about services • An evidence-based approach to clinical practice using guidelines and protocols encourages trust • (Calnan and Rowe, 2005) 22

Trust: recap • Transactional trust – – • • • 5. 9 Figure (Axium Healthcare, 2014) Competence trust Contractual trust Communication trust Conditional trust Embodied trust Informed trust Peer trust Earned trust Status trust Performance trust 23

Unit 5: Patient-Provider Communication, Summary – Lecture b, Trust and Respectful Interactions • Listen carefully; patients will feel understood and cared for • Treat patients respectfully; patients will feel like valuable human beings • Be honest and consistent; patients will feel that providers are trustworthy • Follow through on commitments; patients will feel their care is predictable and dependable • Have an accepting attitude; patients will be more comfortable sharing information about themselves 24

Patient-Provider Communication References – Lecture b References Calnan, M, & Rowe, R. (2005). Trust relations in the “new” NHS: theoretical and methodological challenges. https: //www. kent. ac. uk/scarr/events/Calnanand%20 Rowe%20 paper. pdf Institute of Medicine. (2001). Crossing the Quality Chasm: A New Health System for the 21 st Century. Committee on Quality of Health Care in America. Mok, E, & Chiu, PC. (2004). Nurse-patient relationships in palliative care. J Adv Nurs. . 48(5): 475 -83. 25

Patient-Provider Communication References – Lecture b (Cont’d) Charts, Tables, Figures 5. 6 Figure: Calnan, M, and Rowe, R. (2005). Trust relations in the ‘new’ NHS: theoretical and methodological challenges. ‘Taking Stock of Trust’ E. S. R. C Conference London School of Economics December 2005. https: //www. kent. ac. uk/scarr/events/Calnanand%20 Rowe%20 paper. pdf 5. 7 Table: Calnan, M, and Rowe, R. (2005). Table 1: Conceptual framework for explaining trust relations in the new “NHS”. ‘Taking Stock of Trust’ E. S. R. C Conference London School of Economics December 2005. https: //www. kent. ac. uk/scarr/events/Calnanand%20 Rowe%20 paper. pdf 5. 8 Table: Calnan, M, and Rowe, R. (2005). Table 2: Attitudes that reflect felt trust. ‘Taking Stock of Trust’ E. S. R. C Conference London School of Economics December 2005. https: //www. kent. ac. uk/scarr/events/Calnanand%20 Rowe%20 paper. pdf 5. 9 Figure: Axium Healthcare. (2014). http: //www. axiumhealthcare. com/patient-providertrust/ 26

Unit 5: Patient-Provider Communication, Lecture b – Trust and Respectful Interactions This material was developed by Columbia University, funded by the Department of Health and Human Services, Office of the National Coordinator for Health Information Technology under Award Number 90 WT 0006. 27
- Slides: 27