Patient screening tools associated with prediction of depression















- Slides: 18

Patient screening tools associated with prediction of depression remission at six months Kurt B. Angstman, MS MD Professor of Family Medicine Vice Chair of Education Mayo Clinic Rochester, Minnesota, USA WONCA Europe Conference, 16 June 2016 © 2016 MFMER | slide-1

Disclosures • No financial disclosures © 2016 MFMER | slide-2

Unipolar Depression • Common • Lifetime prevalence of 16. 6% in U. S. A. • 12 month incidence of 6. 6% • Strine TW, Mokdad AH, Balluz LS, et al. Depression and anxiety in the United States: findings from the 2006 behavioral risk factor surveillance system. Psychiatr Serv 2008; 59: 1383 -90. • Difficult to treat • Only about half of depressed adults get treated • Kessler RC, Chiu WT, Demler O, Walters EE. Prevalence, severity, and comorbidity of 12 -month DSM-IV disorders in the national comorbidity survey replication. Arch Gen Psychiatry 2005; 62: 617 -27. • Only 20 -40% of these show substantial improvement over 12 months • Unützer J, Katon W, Callahan CM, et al. Collaborative care management of late-life depression in the primary care setting: a randomized controlled trial. JAMA 2002; 288: 2836 -45. • Katon W, Robinson P, Von Korff M, et al. A multifaceted intervention to improve treatment of depression in primary care. Arch Gen Psychiatry 1996; 53: 924 -32. © 2016 MFMER | slide-3

Persistent Depressive Symptoms in collaborative care management • PRIOR STUDY • 1, 110 care management patients from primary care, retrospectively reviewed. • Three patient self assessment screening tests at baseline and clinical diagnosis were predictive of which patients would have PHQ-9 ≥ 10 at six months. • PHQ-9 (depression) • GAD-7 (generalized anxiety) • MDQ (bipolar disorder) • Recurrent vs. First episode of depression • Angstman KB, Shippee ND, Mac. Laughlin KL, Rasmussen NH, Wilkinson JM, Williams MD, Katzelnick DJ. Patient self-assessment factors predictive of persistent depressive symptoms 6 months after enrollment in collaborative care management. Depress Anxiety. 2013 Feb; 30(2): 143 -8. doi: 10. 1002/da. 22020. © 2016 MFMER | slide-4

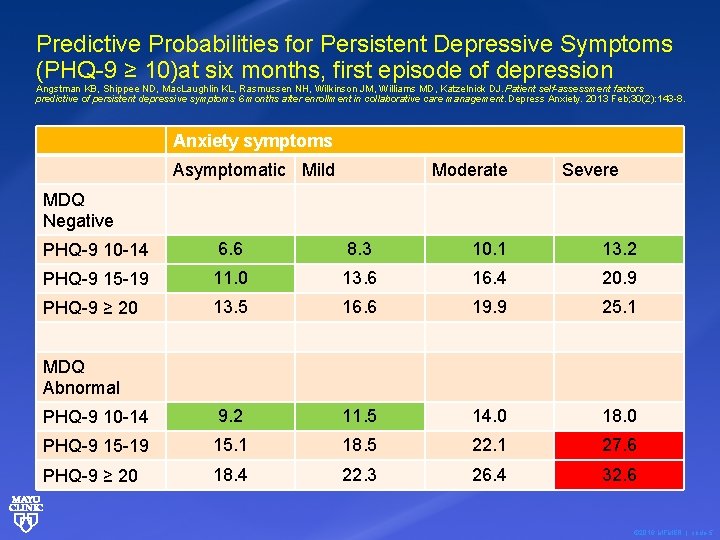
Predictive Probabilities for Persistent Depressive Symptoms (PHQ-9 ≥ 10)at six months, first episode of depression Angstman KB, Shippee ND, Mac. Laughlin KL, Rasmussen NH, Wilkinson JM, Williams MD, Katzelnick DJ. Patient self-assessment factors predictive of persistent depressive symptoms 6 months after enrollment in collaborative care management. Depress Anxiety. 2013 Feb; 30(2): 143 -8. Anxiety symptoms Asymptomatic Mild Moderate Severe MDQ Negative PHQ-9 10 -14 6. 6 8. 3 10. 1 13. 2 PHQ-9 15 -19 11. 0 13. 6 16. 4 20. 9 PHQ-9 ≥ 20 13. 5 16. 6 19. 9 25. 1 PHQ-9 10 -14 9. 2 11. 5 14. 0 18. 0 PHQ-9 15 -19 15. 1 18. 5 22. 1 27. 6 PHQ-9 ≥ 20 18. 4 22. 3 26. 4 32. 6 MDQ Abnormal © 2016 MFMER | slide-5

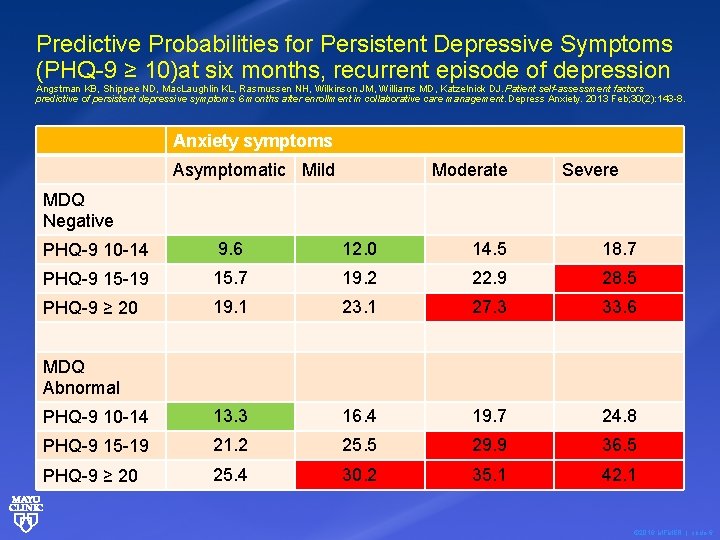
Predictive Probabilities for Persistent Depressive Symptoms (PHQ-9 ≥ 10)at six months, recurrent episode of depression Angstman KB, Shippee ND, Mac. Laughlin KL, Rasmussen NH, Wilkinson JM, Williams MD, Katzelnick DJ. Patient self-assessment factors predictive of persistent depressive symptoms 6 months after enrollment in collaborative care management. Depress Anxiety. 2013 Feb; 30(2): 143 -8. Anxiety symptoms Asymptomatic Mild Moderate Severe MDQ Negative PHQ-9 10 -14 9. 6 12. 0 14. 5 18. 7 PHQ-9 15 -19 15. 7 19. 2 22. 9 28. 5 PHQ-9 ≥ 20 19. 1 23. 1 27. 3 33. 6 PHQ-9 10 -14 13. 3 16. 4 19. 7 24. 8 PHQ-9 15 -19 21. 2 25. 5 29. 9 36. 5 PHQ-9 ≥ 20 25. 4 30. 2 35. 1 42. 1 MDQ Abnormal © 2016 MFMER | slide-6

Hypothesis • For primary care patients with a diagnosis of major depressive disorder and a PHQ-9 ≥ 10 • This study was developed to determine which screening tools might be predictive for the patient with depression being in remission or persistent depressive symptoms after six months. • Patient enrolled until 31 December 2013 • Validation of the model on patients enrolled after 01 January 2014 through 30 June 2015 © 2016 MFMER | slide-7

Study Design • Retrospective chart review • Variables • 2, 525 adult primary • Demographic care patients • Age, gender and • Unipolar depression marital status • Patients with clinical • Clinical Depression diagnosis of bipolar diagnosis depression were • Initial, recurrent or excluded dysthymia • IRB reviewed and • Initial PHQ-9, GAD-7, approved MDQ © 2016 MFMER | slide-8

Outcome variable • PHQ-9 score at six months • PHQ-9 < 5 was considered “remission” • PHQ-9 ≥ 10 was considered “persistent depressive symptoms” (PDS) © 2016 MFMER | slide-9

Odds of PHQ-9 < 5 at six months after enrollment in CCM (regression modeling) © 2016 MFMER | slide-10

Odds of PHQ-9 ≥ 10 at six months after enrollment in CCM (regression modeling) © 2016 MFMER | slide-11

Validation • Logistic Regression model developed on pre-2014 patients using significant variables • Validated on separate cohort of 1098 patients • Enrolled in CCM 01 Jan 2014 to 30 Jun 2015 • 95%CI found by bootstrapping with 1000 random samples • ROC curves plotted for predicting: • Remission (AUC = 0. 62, 95%CI 0. 57 - 0. 66) • Persistent depression (AUC = 0. 67, 95%CI 0. 61 - 0. 72) © 2016 MFMER | slide-12

© 2016 MFMER | slide-13

© 2016 MFMER | slide-14

Clinical Utility • Able to stratify patients at time of enrollment based on readily available demographic and clinical data as to: • Predictive probability of clinical remission or PDS • For example is patient was a high likelihood of remission with low likelihood of PDS- this might suggest different clinical care than a patient who was a low likelihood of remission and high likelihood of PDS. © 2016 MFMER | slide-15

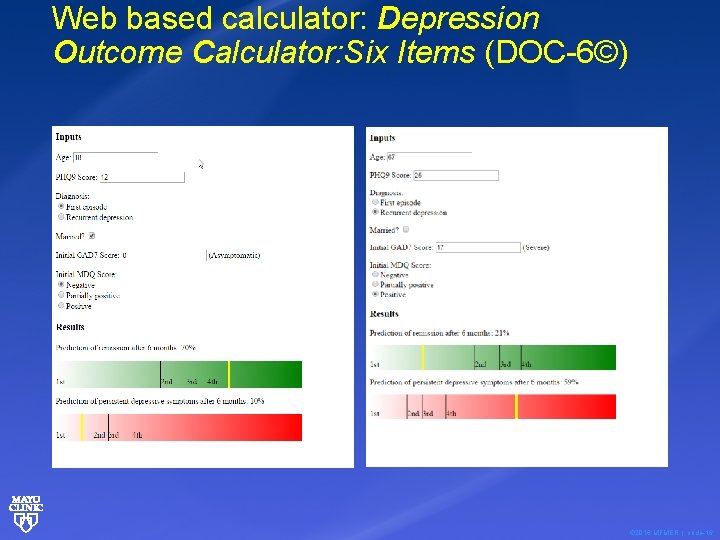
Web based calculator: Depression Outcome Calculator: Six Items (DOC-6©) © 2016 MFMER | slide-16

Study discussion Advantages Limitations • Prior studies in our • Patients who have been institution have enrolled in CCM demonstrated significant • Thus have all improvement in outcomes measures listed with CCM vs. usual primary care. • Treatment is different than usual primary • These predicted care probabilities are a “best case scenario” • Model doesn’t include other variables that may • Real world patients with multiple co-morbidities have an impact on six month outcomes © 2016 MFMER | slide-17

Questions? ? • angstman. kurt@mayo. edu • Co-author • Gregory Garrison, MD © 2016 MFMER | slide-18