Patient Safety for Medics Obstetrics and Anaesthesiology Amarin

Patient Safety for Medics: Obstetrics and Anaesthesiology Amarin Narkwichean, MD. Ph. D. Clinical Lead Team (CLT) Department of Obstetrics and Gynaecology Faculty of Medicine, Srinakharinwirot University

Learning objective 1. Understand the discipline of patient safety 2. Understand human factors and its relationship to patient safety 3. Understand how systems thinking can improve health care and minimize patient adverse events 4. Understand the nature of error and how health care can learn from error to improve patient safety 5. Know how to apply risk management principles by identifying, assessing and reporting hazards and potential risks in the workplace 6. Understand the importance of teamwork in health care and learn how to be an effective team player as a medical student



Harm caused by health-care errors and system failures • Extent of adverse events • Categories of adverse events • Economic costs • Human costs

Topic 2: What is human factors? Human factors definition • The study of all the factors that make it easier to do the work in the right way • Apply wherever humans work • Also sometimes known as ergonomics

Human factors • Acknowledgement: ○ the universal nature of human fallibility ○ the inevitability of error • Assumption that errors will occur • Design things in the workplace to try to minimize the likelihood of error or its consequences

Because the human brain is …. • very powerful • very flexible • good at finding shortcuts (fast) • good at filtering information • good at making sense of things Sometimes though our brain is “too clever” …

Are the lines crooked or straight? Optillusions. com

Look at the chart Say the colour of the word, not the word itself Why is it hard? Optillusions. com

The fact that we can misperceive situations despite the best of intentions is one of the main reasons that our decisions and actions can be flawed such that … Making Clinical Judgment within a second From various sources of input Seems inevitably making errors!!!

Human factors experts • Design improvements in the workplace and the equipment to fit human capabilities and limitations • Make it easier for the workers to get the work done the right way • Decrease the likelihood of errors occurring The design of tools, machines, systems, tasks, jobs, and environments for productive, safe, comfortable and effective human use.
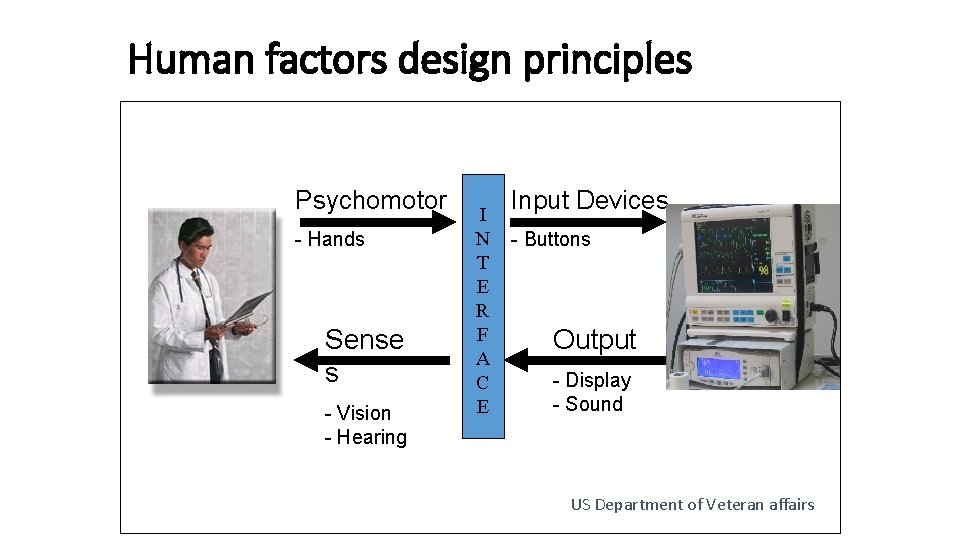
Human factors design principles Psychomotor - Hands Sense s - Vision - Hearing I N T E R F A C E Input Devices - Buttons Output - Display - Sound US Department of Veteran affairs
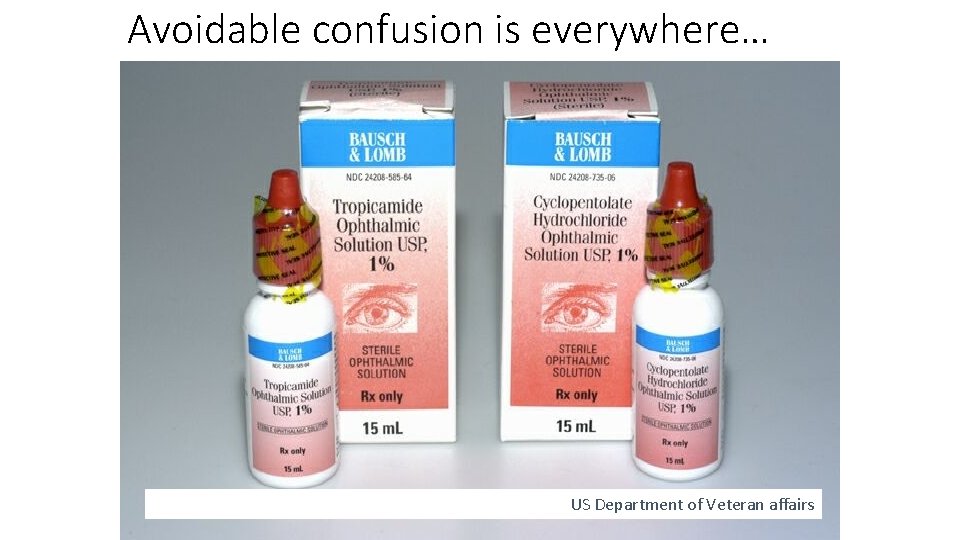
Avoidable confusion is everywhere… US Department of Veteran affairs

One definition of “human error” is “human nature” Error is the inevitable downside of having a brain!

What is an error? • The failure of a planned action to achieve its intended outcome • A deviation between what was actually done and what should have been done Reason A definition that may be easier to remember is: ○ “Doing the wrong thing when meaning to do the right thing. ”

Note: violation A deliberate deviation from an accepted protocol or standard of care

Error and outcome • Error and outcome are not inextricably linked: • Harm can befall a patient in the form of a complication of care without an error having occurred • Many errors occur that have no consequence for the patient as they are recognized before harm occurs Harm/AEs Errors

Health-care context is problematic • When errors occur in the workplace the consequences can be a problem for the patient • a situation that is relatively unique to health care • In all other respects there is nothing unique about “medical” errors • they are no different from the human factors problems that exist in settings outside health care

Situations associated with an increased risk of error • Unfamiliarity with the task* • Inexperience* • Shortage of time • Inadequate checking • Poor procedures • Poor human equipment interface * Especially if combined with lack of supervision Vincent

Individual factors that predispose to error • Limited memory capacity • Further reduced by: ○ fatigue ○ stress ○ hunger ○ illness ○ language or cultural factors ○ hazardous attitudes

Fatigue 24 hours of sleep deprivation has performance effects ~ blood alcohol content of 0. 1% Dawson – Nature, 1997
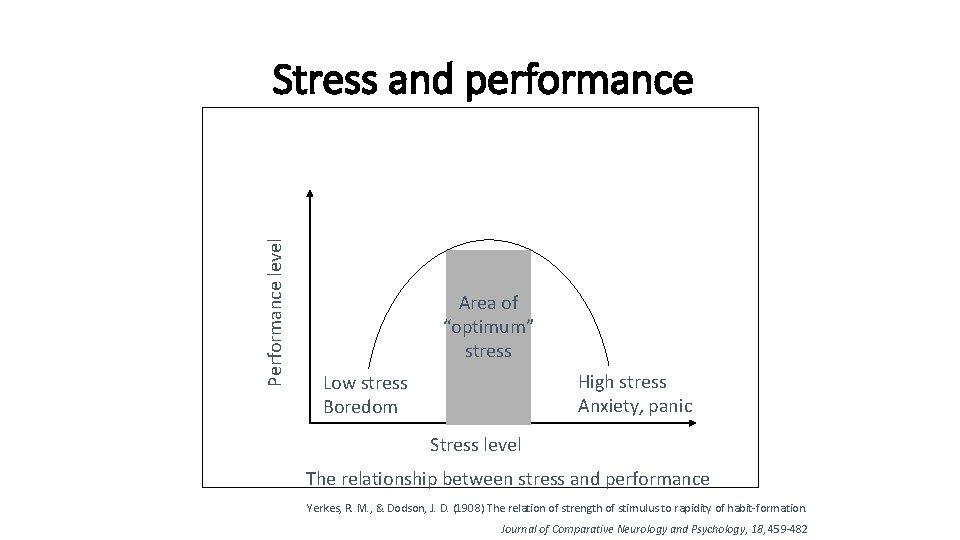
Performance level Stress and performance Area of “optimum” stress High stress Anxiety, panic Low stress Boredom Stress level The relationship between stress and performance Yerkes, R. M. , & Dodson, J. D. (1908) The relation of strength of stimulus to rapidity of habit-formation. Journal of Comparative Neurology and Psychology, 18, 459 -482

Don’t forget …. If you’re • H ungry • A ngry • L ate or • T ired …. . H A L T

A performance-shaping factors “checklist” • I • M Illness Medication • prescription, alcohol & others • • S A F E Stress Alcohol Fatigue Emotion Jensen, 1987

Apply human factors thinking to your work environment 1. 2. 3. 4. Avoid reliance on memory Make things clearly visible Review and simplify processes Standardize common processes and procedures 5. Routinely use checklists 6. Decrease the reliance on vigilance

Topic 3 : Understanding systems and the impact of complexity on patient care Health care is a complex system Increased chance of something going wrong!

Two schools of thought regarding iatrogenic injury o Traditional or person approach * the “old” culture * “just try harder” o Systems approach * the “new look” You may encounter a bit of both in your “journey”

Person approach See an errors as the product of carelessness Remedial measures directed primarily at the error-maker o o Naming Blaming Shaming Retraining Perspectives on error

An individual failing? Doesn’t work! o People don’t intend to commit errors only a very small minority of cases are deliberate violations o o Won’t solve the problem - it will make it worse Countermeasures create a false sense of security “we’ve ‘fixed’ the problem” o o Clinicians will hide errors May destroy many clinicians inadvertently the second victim

Why investigate? • The more we understand how and why these things occur, the more we can put checks in place to reduce recurrence • Strategies might include: • Education • New protocols • New systems

Multiple factors usually involved • patient factors • provider factors • task factors • technology and tool factors • team factors • environmental factors • organizational factors
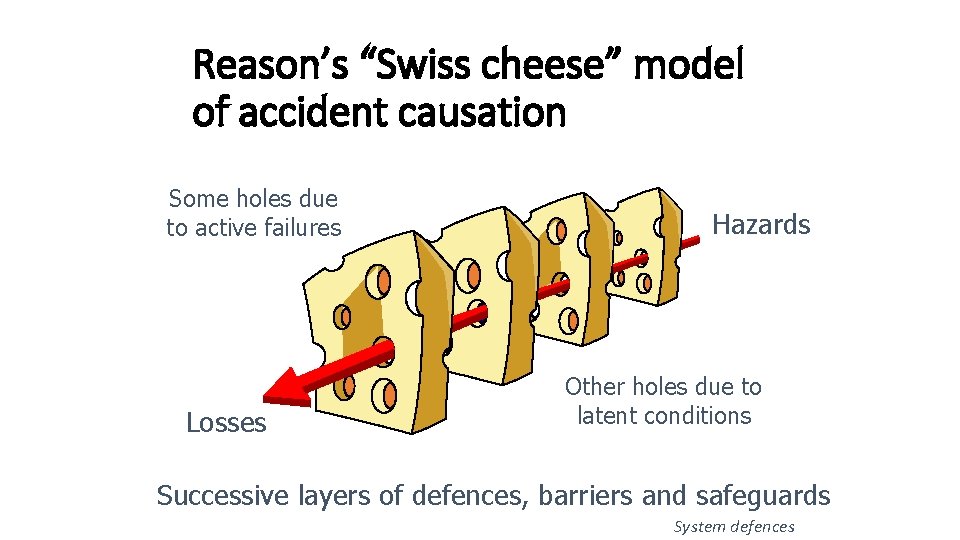
Reason’s “Swiss cheese” model of accident causation Some holes due to active failures Losses Hazards Other holes due to latent conditions Successive layers of defences, barriers and safeguards System defences
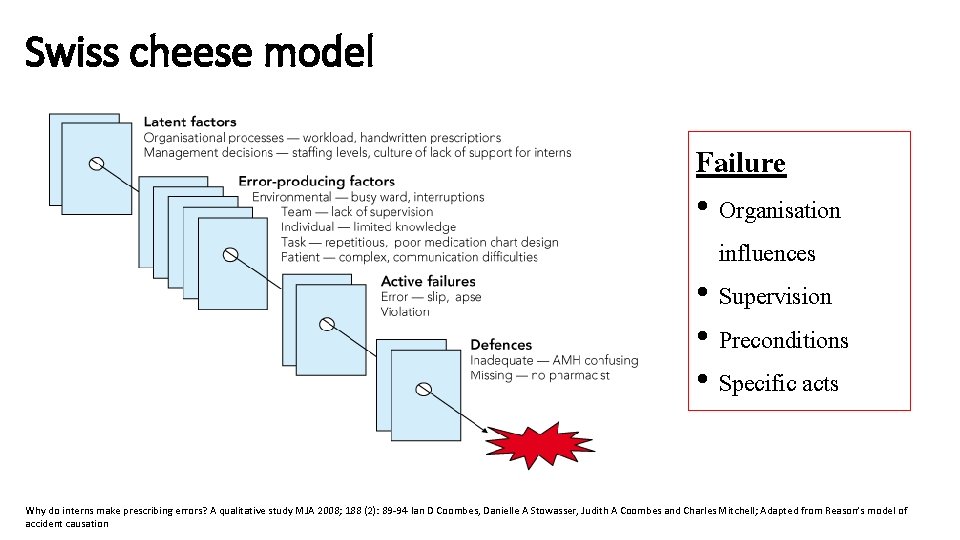
Swiss cheese model Failure • Organisation influences • Supervision • Preconditions • Specific acts Why do interns make prescribing errors? A qualitative study MJA 2008; 188 (2): 89 -94 Ian D Coombes, Danielle A Stowasser, Judith A Coombes and Charles Mitchell; Adapted from Reason’s model of accident causation
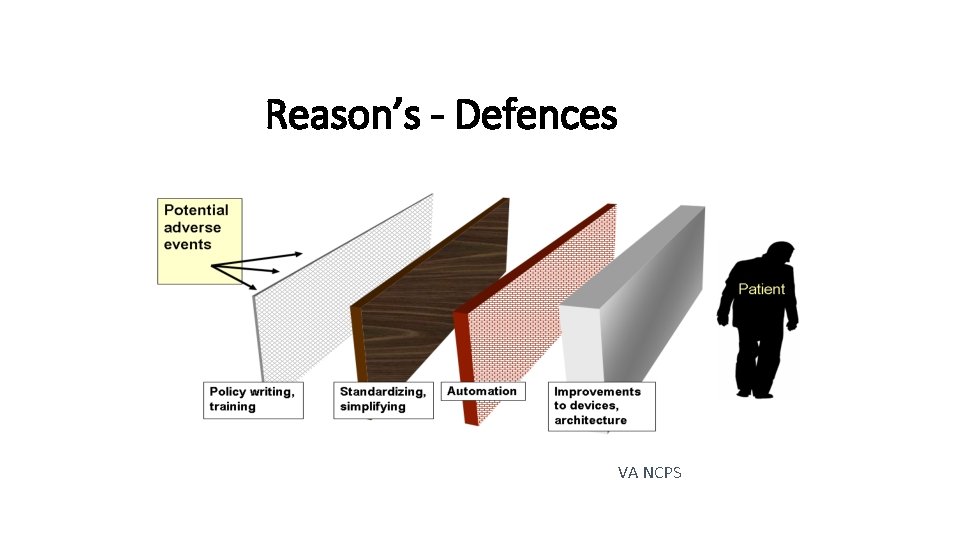
Reason’s - Defences VA NCPS

Characteristics of high reliability organizations (HROs) o Preoccupation with failure o Commitment to resilience o Sensitivity to operations o A culture of safety

Key principles from HRO theory o Maintain a powerful and uniform culture of safety o Use optimal structures and procedures o Provide intensive and continuing training of individuals and teams o Conduct thorough organisational learning and safety management

The aircraft carrier: The prototypical HRO Carriers achieve nearly failure-free record despite multiple hazards Gaba

Health care can learn many lessons from HROs Although health care is different from other industries (e. g. people are not airplanes) we can learn: from their successes: o What factors make them work so well? from their failures: o How do disasters occur even in typically high reliability settings?

Topic 4: Understanding and learning from error Incident monitoring • Involves collecting and analysing information about any events that could have harmed or did harm anyone in the organization • A fundamental component of an organization’s ability to learn from error

Removing error traps • A primary function of an incident reporting system is to identify recurring problem areas - known as “error traps” (Reason) • Identifying and removing these traps is one of the main functions of error management Error traps
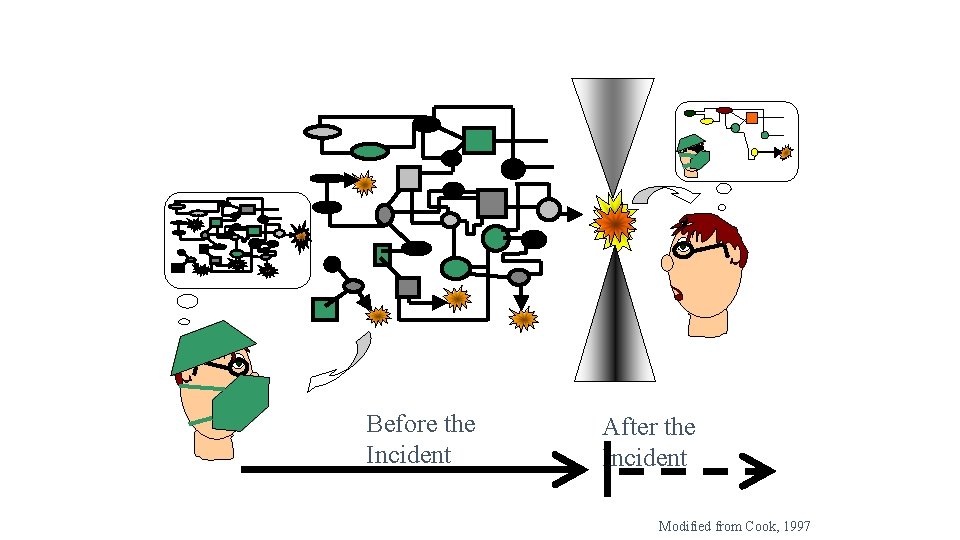
Hindsight Bias Before the Incident After the Incident Modified from Cook, 1997

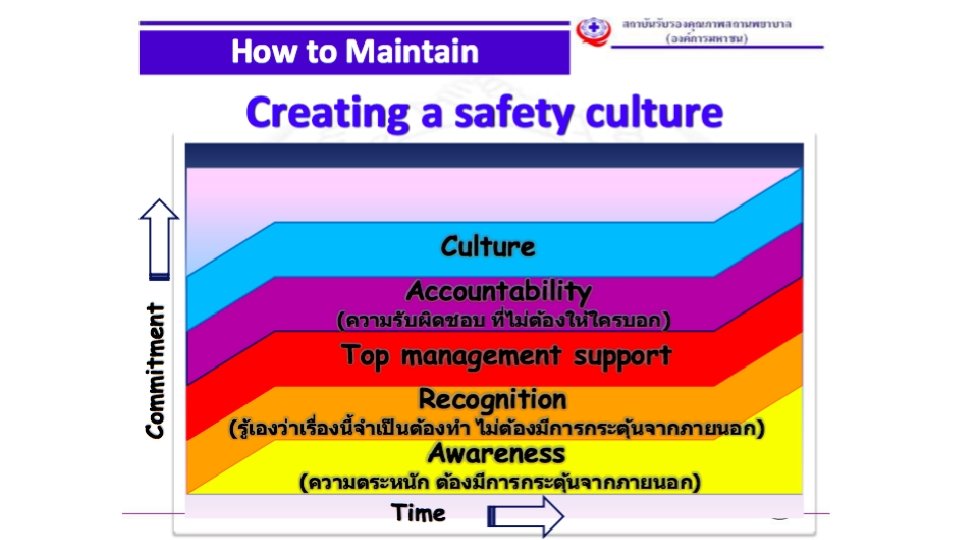
Culture: a workable definition (Reason) Shared values (what is important) and beliefs (how things work) that interact with an organization’s structure and control systems to produce behavioural norms (the way we do things around here) Safety culture

Culture in the workplace • It is hard to “change the world” as a junior doctor • but … • You can be on the look out for ways to improve the “system” • You can contribute to the culture in your work environment

Incident reporting and monitoring strategies • Others include: • Anonymous reporting • Timely feedback • Open acknowledgement of successes resulting from incident reporting • Reporting of near misses • “Free lessons” can be learned • System improvements can be instituted as a result of the investigation but at no “cost” to a patient Larson

Complaints • Assist in maintaining standards • Reduce the frequency of litigation • Help maintain trust in the profession • Encourage self-assessment • Protect the public

Root cause analysis • A rigorous, confidential approach to answering: • What happened? • Why did it happen? • What are we going to do to prevent it from happening again? • How will we know that our actions improved patient safety? Established by the US Department of Veterans Affairs National Center for Patient Safety http: //www. va. gov/NCPS/curriculum/RCA/index. html

RCA model • Focuses on prevention, not blame or punishment • Focuses on system level vulnerabilities rather than individual performance - Communication - Training (Experience) - Fatigue/scheduling - Environment/equipment - Rules/policies/procedures/management - Barriers

Sentinel events • unexpected occurrence involving death or serious physical or psychological injury and includes any process variation for which a recurrence would carry a significant chance of serious adverse outcome JCAHO, 1999

Topic 5: Being an effective team player What is a team? A team is a group of two or more individuals who: o o interact dynamically have a common goal/mission have been assigned specific tasks possess specialized and complementary skills

What makes for a successful team? Effective teams possess the following features: o o o o a common purpose measurable goals effective leadership and conflict resolution good communication good cohesion and mutual respect situation monitoring self-monitoring flexibility

Communication A number of techniques have been developed to promote communication in health care including: o SBAR (Situation, Background, Assessment, Recommendation) o call-out o check-back o handover/handoff

Resolving disagreement and conflict A number of techniques have been developed to help all members of a team speak out including: o The two challenge rule o CUS (I am Concerned, I am Uncomfortable and this is a Safety Issue) o DESC script (Describe, Express, Specify, Consequence)

Example of team mutual support • https: //youtu. be/yr 6 rxdq. Ly 2 M

Barriers to teamwork o changing roles o medical hierarchies o individualistic nature of medicine o instability nature of teams

Incidents in other industries Failures in the following team behaviours have been identified as being responsible for accidents in other industries: o roles not being clearly defined o lack of explicit coordination o miscommunication/communication

Performance requirements… Practical tips medical students can start practising now to improve teamwork include: o o o o always introducing yourself to the team reading back/closing the communication loop stating the obvious to avoid assumptions asking questions, checking and clarifying delegating tasks to people not to the air clarifyng your role using objective (not subjective) language

Performance requirements… Practical tips medical students can start practising now to improve teamwork include: o learning and using people’s names o being assertive when required o if something doesn’t make sense, finding out the other person’s perspective o doing a team briefing before undertaking a team activity and a debriefing afterwards o when conflict occurs, concentrating on “what” is right for the patient, not “who” is right

Performance requirements • know how to report known risks or hazards in the workplace • keep accurate and complete medical records • self-assess to reduce the risk of errors caused by inadequate knowledge and skills • participate in meetings that discuss risk management and patient safety • respond appropriately to patients and families after an adverse event • respond appropriately to complaints

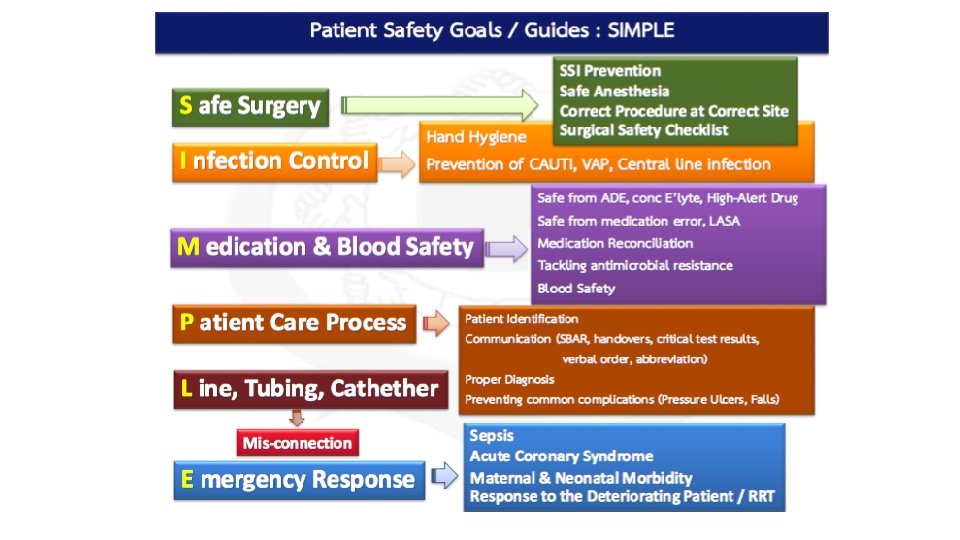

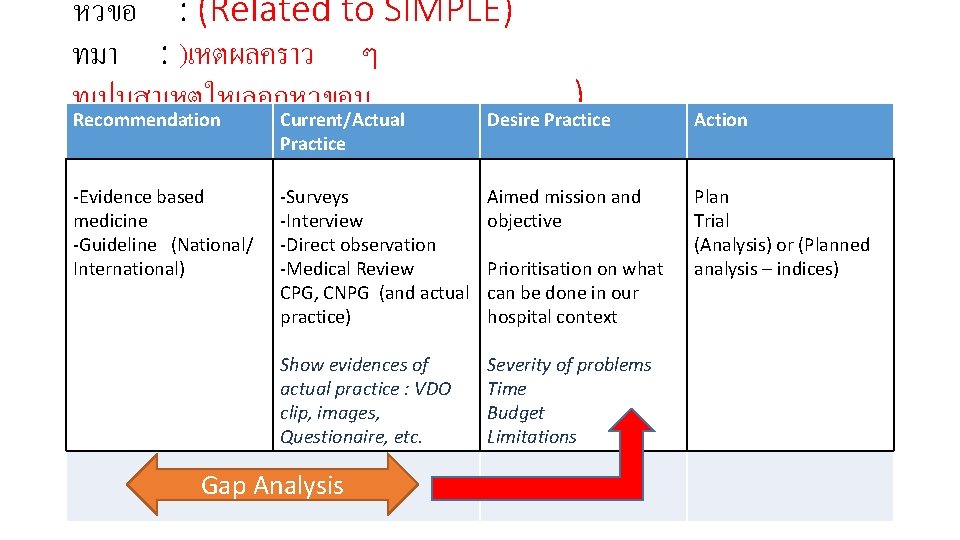
หวขอ : (Related to SIMPLE) ทมา : )เหตผลคราว ๆ ทเปนสาเหตใหเลอกหวขอน ) Recommendation Current/Actual Desire Practice Action -Evidence based medicine -Guideline (National/ International) Plan Trial (Analysis) or (Planned analysis – indices) Practice -Surveys -Interview -Direct observation -Medical Review CPG, CNPG (and actual practice) Aimed mission and objective Show evidences of actual practice : VDO clip, images, Questionaire, etc. Severity of problems Time Budget Limitations Gap Analysis Prioritisation on what can be done in our hospital context
- Slides: 64