Patient Protection and Affordable Care Act PPACA The

Patient Protection and Affordable Care Act (PPACA)

The information contained in this presentation has been collected from multiple documents and presentations. It is not intended to contain any legal advise. Please consult with you legal advisors for specific information that may apply to you and your company.


Editorial Moment

Insurance Companies Lawyers Consumer Doctors Agents Who is at fault?



The Law �The President signed the health care legislation into law on March 23, 2010. �The regulations defining the law are being written by HHS, DOL and IRS. �IRS & OSHA have monitoring responsibility �CMS has responsibility for most of the implementation, including that of the Marketplace

You can keep your insurance Grandfathered Plans

Grandfathered Plan Benefits of Retaining Status ◦ Exemption from rating restrictions based on age variation ◦ Ability to continue coverage based on class ◦ Exemption from implementing Essential Health Benefits (e. g. pediatric dental)

A Grandfathered Plan �Increase Deductible up to 15% �Increase Co pays up to 15% �Increase Co insurance more than 15% �Decrease employer contributions by more than 5%

�Most plans have lost Grandfather status. Those who have retained status must: ◦ Plans must provide a statement to participant that it believes it is a “grandfathered” plan ◦ Do you have your documents? Grandfathered Plan

Dependents Coverage

• Coverage for children must be available until the child reaches age 26 �Do you have proof of the notice to employees? (Penalty up to $100 per day) Age 26

Minimum Loss Ratio MLR

Minimum Loss Ratio MLR (2011) �The MLR is 85% for large group plans and 80% for individual and small group plans (50 and below). �Carriers will have to issue a premium rebate to individuals for plans that fail to meet the minimum MLR requirements.

Large Groups 51 or More Full Time Employees
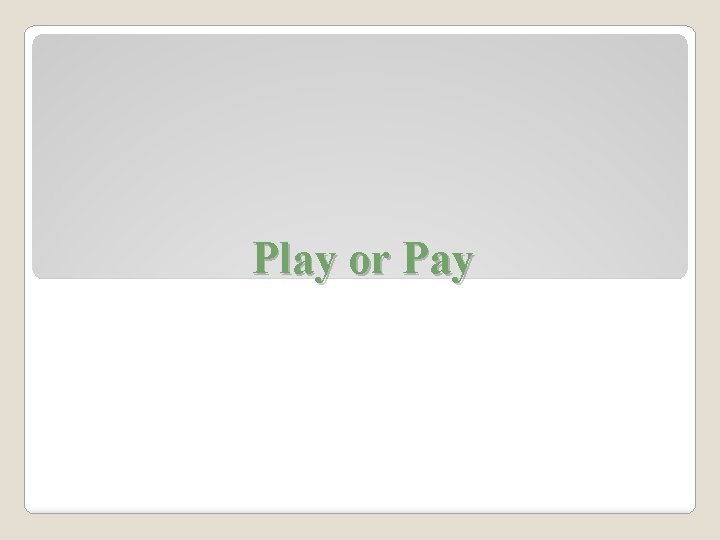
Play or Pay
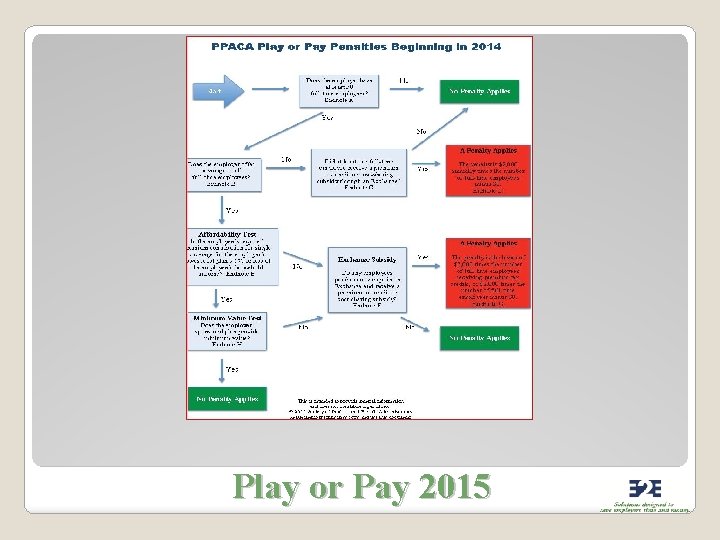
Play or Pay 2015

�Effective starting January 1, 2015 �Employer must count all full-time employees and part-time employees – on a full-time equivalent basis in determining if they have 50 or more employees Employer Responsibility

�If an employer fails to provide its full-time employees (and their dependents) the opportunity to enroll in “minimum essential coverage, ” and �One or more full-time employees enrolls for coverage in an exchange and qualifies for a premium tax credit, then �Employer penalty = $2, 000 for each of its full-time employees in the workforce ◦ This penalty is non-deductible ◦ Penalty does not offset the cost of employee coverage No Coverage

�Total number of full time employees = 30 �Part time employees = 40 �Total hours worked by each part time employees in a calendar month = 20 hrs / week X 40 = 3, 200 hrs � 3, 200 / 120 = 27 Part time equivalent employees �Total full time and full time equivalent employees = 57 �Play or Pay penalties apply Calculating Full Time Equivalent Employees

Affordable Coverage �If employer offers its full-time employees (and their dependents) the opportunity to enroll in minimum essential coverage, and �One or more full-time employees enrolls for coverage in an exchange and qualifies for a premium tax credit or cost sharing reduction because

◦ The employee’s share of the premium exceed 9. 5% of income, or ◦ The actuarial value of the coverage was less than 60%, then • Employer penalty = $3, 000 for each full-time employee who receives a tax credit or cost-sharing reduction • If the employer has many employees in this category, the alternative penalty reverts to $2, 000 per FT employee Affordable Coverage

�Employee hourly wage $9. 50 per hour �$9. 50 X 40 hours = $380. 00 �$380 X 9. 5% = $36. 10 per week �Employee cost of health insurance $156. 43 Affordable Coverage Example

�Start tracking part time hours now �Start tracking full time hours now �Learn about the safe harbor for seasonal employees Tracking Time

�If employee is covered by spouses plan there is no penalty to employer unless 50+ and employer does not provide coverage or provides unaffordable coverage. �Employers are not required to cover spouses. Definition of a dependent does not include the spouse Miscellaneous Requirements

Small Groups 1 to 50 Full Time Employees
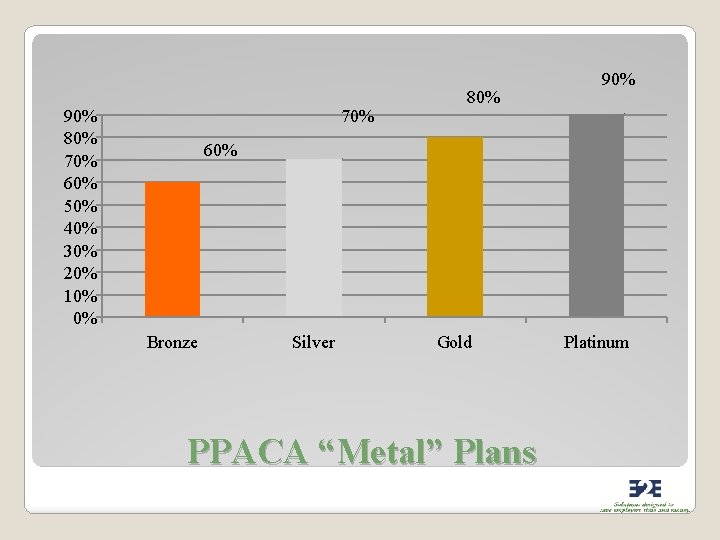
90% 80% 70% 60% 50% 40% 30% 20% 10% 0% 70% 80% 90% 60% Bronze Silver Gold PPACA “Metal” Plans Platinum

Minimum Value Standards �Minimum value - actuarial value threshold of 60% �Small group plans in the bronze level of coverage meet minimum value requirements. �Beginning in 2014, summaries of benefits and coverage must indicate whether the plan meets applicable minimum value requirements

Minimum Essential Coverage �The type of coverage an individual needs to have to meet the individual responsibility requirement ◦ Individual market policies ◦ Job-based coverage ◦ Medicare, Medicaid, CHIP, TRICARE �The law does not specify the details of what this coverage has to be, other than it has to cover preventive care with no cost-sharing and can’t be dental-only or vision-only (limited benefit)

Minimum Value Calculator

Essential Health Benefits The 10 categories of benefits individual and small employer plans have to provide: ◦ Outpatient care ◦ Emergency room ◦ Treatment in the hospital ◦ Maternity ◦ Mental health and substance use disorder services ◦ Prescription drugs ◦ Rehabilitative and habilitative services. ◦ Lab tests ◦ Preventive services ◦ Pediatric dental and vision

� Censuses must provide every dependent’s date of birth and the quotes will be lined out with a rate for each belly button. So a quote might look like this on a 3 -person group: � John Brown � Joe Smith � Jane Smith (wife) � Danny Smith (12) � Jennifer Smith (14) � Joey Smith (22) � Susie Smith (24) � Bobby Jones � Anna Jones (wife) $328. 95 $358. 23 $429. 29 $158. 77 $167. 23 $253. 97 $260. 09 $598. 98 $555. 23 Employee/Spouse/Children Employee/Spouse Age Rated Plan Small Group

Health Insurance Marketplace (The Exchange)

Primary component of the law affected by �Age band limitations (7: 1 goes to 3: 1) �No health underwriting �Cost-sharing limits (e. g. $2, 000 ded) �Essential health benefits �No pre-existing conditions Community Rating

�Smaller provider networks �Smaller hospital network �No out of network benefits on some plans �Gatekeeper plans (no open access) Health Insurance Marketplace The Exchange

Health Insurance Market Place The Exchange Federal subsidies only available through the Exchange are based on: ◦ The premium cost of the second-lowest silver Exchange plan ◦ The household income of the applicant
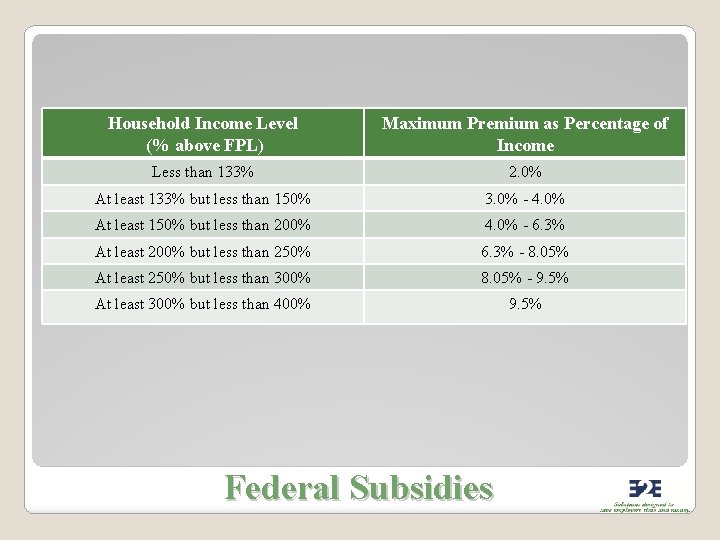
Household Income Level (% above FPL) Maximum Premium as Percentage of Income Less than 133% 2. 0% At least 133% but less than 150% 3. 0% - 4. 0% At least 150% but less than 200% 4. 0% - 6. 3% At least 200% but less than 250% 6. 3% - 8. 05% At least 250% but less than 300% 8. 05% - 9. 5% At least 300% but less than 400% 9. 5% Federal Subsidies
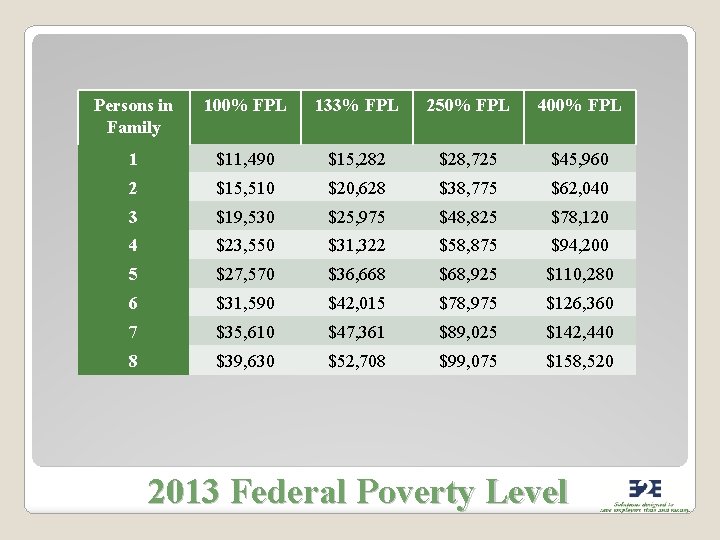
Persons in Family 100% FPL 133% FPL 250% FPL 400% FPL 1 $11, 490 $15, 282 $28, 725 $45, 960 2 $15, 510 $20, 628 $38, 775 $62, 040 3 $19, 530 $25, 975 $48, 825 $78, 120 4 $23, 550 $31, 322 $58, 875 $94, 200 5 $27, 570 $36, 668 $68, 925 $110, 280 6 $31, 590 $42, 015 $78, 975 $126, 360 7 $35, 610 $47, 361 $89, 025 $142, 440 8 $39, 630 $52, 708 $99, 075 $158, 520 2013 Federal Poverty Level

� For individuals (whichever is greater) � For families (whichever is greater) � 2014 $95 or 1% of income � 2014 $285 or 1% of income � 2015 $325 or 2% of income � 2015 $975 or 2% of income � 2016 $695 or 2. 5% of income � 2016 $2085 or 2. 5% of income above tax filing threshold ($9, 500 in 2011) above tax filing threshold Note: Penalty for dependents under age 18 is one half of the individual amount. above tax filing threshold Individual Mandate Penalties

Real Life Examples �Family of three – 63 male, 59 female, 18 son ◦ Current $2500 deductible plan $819. 32 ◦ 2014 $2500 deductible plan $1, 397. 29 �Family of four – 49 male, 50 female, 14 son, 12 daughter ◦ Current $5, 000 deductible plan $423. 93 ◦ 2014 $2500 deductible plan $965. 51 Community Rating

For a small business to qualify to purchase coverage on a SHOP they must: �Be in a SHOP service area �Have at least one common law employee (not owners) �Have 50 or fewer total FTE employees �Pay a consistent percentage or amount toward the premium (at least 50%) �Receive tax credit An employer can use a defined contribution to pay for an employee to purchase individual coverage only if that coverage is purchased through a SHOP plan. Small Business Marketplace (SHOP)

Planning is Essential

Increasing Premiums 3% to 4%

�PCORI Tax-$2. 00 per covered individual-Self Admin HRA, per employee (belly button tax) �Re insurance Tax-$63. 00 per year (belly button tax) Funds large claims in the individual marker �HIT Tax- $8 B divided by premiums collected in prior year 2014. $15 B 2015, $18 B 2016 - Paid by insurers to help fund health care reform �All are pass through taxes Taxes

�Medicare Tax increase for high income earners an additional 0. 9 to employees earning over $200, 000 ($250, 000 joint filers). January 1, 2013

Miscellaneous Requirements

�DOL ran a contest for the best software to inform employee about their labor laws. �Award winner on November 4 �$14 M effort to educate employees Government Initiative

�Many employers have said the will move employees to 1099 status. �The IRS is on to this and will be conducting audits. �An employee can contact IRS and ask about their status and you could receive an audit notice. �Engage an independent contractor for a year or more. �Be very careful with this!!!!!!! 1099 Independent Contractors

�You are not an independent contractor if you perform services that can be controlled by an employer (what will be done and how it will be done). This applies even if you are given freedom of action. What matters is that the employer has the legal right to control the details of how the services are performed. Independent Contractor

�Guarantee Issue �State Exchanges/Federal Exchange �Modified Community Rating (Groups 50 or less) �Redefines Small Group at 1 -100 in 2016 �Employer Mandate �Waiting Periods 90 Days Max. January 1, 2014

�Full Time Employee for health insurance purposes-30 hours per week �There is no requirement to pay the health insurance for part time employees Miscellaneous Requirements

W-2 Reporting �Employers who issue 250, or more W-2 s are required to list the value of the health insurance on the W-2.

�Employers will report employees and the hours worked each month. 2015 �Exempt employees can be calculates at 8 hours per day, 40 hours per week, or actual hours worked. �Form 1095 -C �Information must also be provided to each employee Reporting

Flexible Spending Accounts FSA �Flexible Spending Accounts (FSA)-Over the counter drugs are not eligible. $2, 500 cap

Required Notices

Summary of Benefits and Coverage SBC �Uniform Explanation of Benefits ◦ Maximum 4 pages ◦ Minimum 12 point font �Penalty up to $1, 000 per affected individual.

SBC �Developed and provided by the insurance company �Delivered during Open Enrollment �At a Qualifying Event � 60 days prior to a plan change during the plan year �When an employee qualifies for coverage during the plan year �Upon request

Employee Notice Requirement �Employers must issue a notice to employees about the Health Insurance Marketplace (Exchanges) availability and premium assistance by October 1, 2014. �No penalty Health Insurance Marketplace (Exchange) Notice

�Distributed by October 15 th �Distributed to all employees age 65 and older �States the company health pan has drug coverage equal to or better than Medicare Part “D” �Online verification to CMS within 60 days of renewal Medicare Creditable Coverage Notice

Health Reimbursement Arrangement (HRA) �No stand alone, except for retirees

Possible Strategies

Will employers drop coverage to save cost? �Some will and force their employees to the Exchange. �In some cases, the penalties are lower than the cost of coverage, but what about the soft cost of competition?

�Keeps current plan design in place until December 1, 2014 �Avoids age rates plans for all groups under 50 �Avoids community rates �Avoids PPACA plan designs Early Renewals

�Employer liability limited to the monthly premiums �Monthly claims reports �If plan develops a surplus the employer can receive a refund �If plan runs in a deficit, no deficit recovery Level Funded Partially Self Funding

�Places the insurance buying decision in the hands of the employee. �Must still comply with affordability. �Wide range of options for the employee. �Must be equal to all Defined Contribution

�Employer Allowance $300 �Medical $250 �Dental $25 �Vision $10 �Total $285 �Employee $15 Defined Contribution

Summary

�You will be exposed to every concept you can imagine. �Some old concepts, some new �Some will survive, and some will cause the employer bigger problems �caveat emptor (May the buyer beware) �Select a trusted advisor

�Document

�DOL. gov �HHS. gov �IRS. gov �Healthcare. gov �CMS. gov-search “minimum value calculator” �EEOC. gov �e 2 eresources. com Websites

Thank You
- Slides: 73