Patient feedback Exeter Engaging or empowering service users

Patient feedback: Exeter Engaging or empowering service users Nigel Starey 1

Objectives • By the end of this talk I hope you will have a clearer idea of the context, purpose and potential of service user engagement. • You might also understand the breadth, if not the depth of user engagement activities and how CQC values them • You will have a better understanding of how our understanding of the sector’s culture can support evaluation and rating of the providers performance by engaging with service users. • You will appreciate the possibility that the context within which we are inspecting and rating the sector means that engagement may be blending with empowerment as professional partnerships federate and transform. 2

Engaging service uses • In every consultation – patient centred approach, monitored through surveys and inspected as part of caring and responsive domains. • Volunteering – carer support, voluntary visiting, running walking groups or transporting for appointments. • Group participation - the PPG, community groups • Interviews, comment cards, feedback, surveys, friends & family, NHS choices, • National GP Patient survey – Ipsos MORI, twice per yr, random - % & response 3

National GP patient survey -Caring Results from the national GP patient survey showed patients felt they were treated with compassion, dignity and respect. The practice scored higher when compared to the CCG and national averages for satisfaction scores on consultations with GPs, nurses and interactions with reception staff. For example: 95% of patients said the GP was good at listening to them (CCG average 86%, national average 89%). 90% of patients said the GP gave them enough time (CCG average 84%, national average 87%). 98% of patients said they had confidence and trust in the last GP they saw (CCG average 94%, national average 95%). 94% of patients said the last GP they spoke to was good at treating them with care and concern (CCG average 83%, national average 85%). 96% of patients said the last nurse they spoke to was good at listening to them (CCG average 88%, national average 91%). 89% of patients said they found the receptionists at the practice helpful (CCG average 84%, national average 87%). 4

Outstanding in caring • People are truly respected and valued as individuals and are empowered as partners in their care • Feedback from people who use the service, those who are close to them and stakeholders is continually positive about the way staff treat people. People think that staff go the extra mile and the care they receive exceeds their expectations. • There is a strong, visible, person-centred culture. Staff are highly motivated and inspired to offer care that is kind and promotes people’s dignity. Relationships between people who use the service, those close to them and staff are strong, caring and supportive. These relationships are highly valued by all staff and promoted by leaders. • Staff recognise and respect the totality of people’s needs. They always take people’s personal, cultural, social and religious needs into account. • People who use services are active partners in their care. Staff are fully committed to working in partnership with people and making this a reality for each person. Staff always empower people who use the service to have a voice. They show determination and creativity to overcome obstacles to delivering care. People’s individual preferences and needs are always reflected in how care is delivered. • People’s emotional and social needs are seen as important as their physical needs 5

Context • The changing world – remember consanguinity and orphans • • • Changing Healthcare – towards a literate population Primary care – or “Out of hospital” care General practice - - EG, registration, time, personal CQC – Accountability and regulation Engaging Service users –understanding and responding to the changing relationship with patients 6

APPG Primary care & Public health The Care Quality Commission (CQC)’s statement to the inquiry that: “raising the level of health literacy is currently seen as a peripheral activity in many general practices” is of concern. RECOMMENDATION 13: A system-wide approach to improving health literacy should be taken. 7

5 QUESTIONS Is the practice 1. 2. 3. 4. 5. Safe? Effective? Caring? Responsive? Well Led? ALL with a set of prompts that we refer to as Key Lines of Enquiry (KLOEs) 8
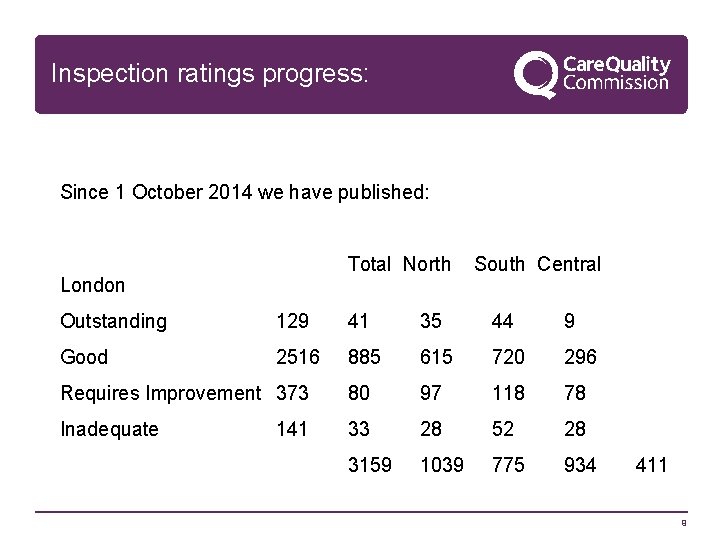
Inspection ratings progress: Since 1 October 2014 we have published: London Total North South Central Outstanding 129 41 35 44 9 Good 2516 885 615 720 296 Requires Improvement 373 80 97 118 78 Inadequate 33 28 52 28 3159 1039 775 934 141 411 9
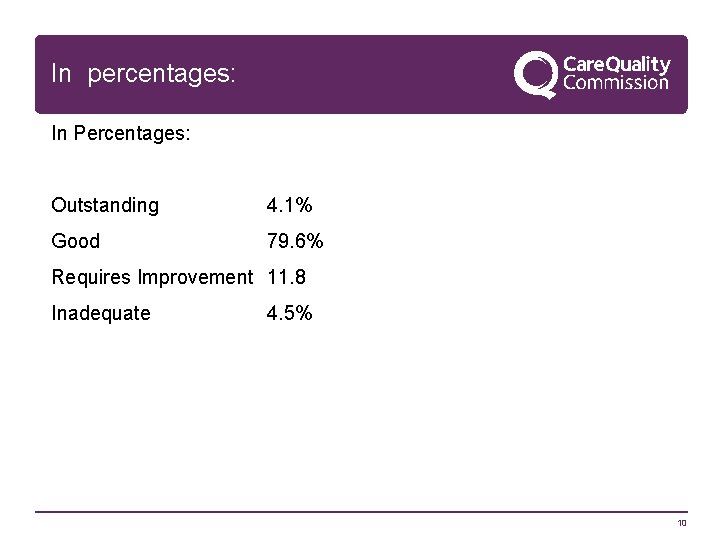

In percentages: In Percentages: Outstanding 4. 1% Good 79. 6% Requires Improvement 11. 8 Inadequate 4. 5% 10

The CQC Challenge to Practices • First comprehensive inspection of every practice in England – Fear of the unknown • • • Open and Accountable Rating Needs v wants- Learning v Reacting – Inward v Outward Drowning – Surviving – Thriving To what extent is the practice meeting the Health Needs of the community it serves? • To what extent is the practice challenging the “Inverse care law? ” • To what extent are the services provided designed to respond to the needs and views of patients? 11

The Challenge to PPGs 1. • • • Where do you fit in? Fan club League of friends Patients voice Critical friend Non executive director 2. How do you influence the practice? • • • Through or with? Hard or soft evidence Now then or when? 12

How to Influence the CQC Inspection The role of the PPG • • • Know yourself Know where you fit in Know the CQC inspection format Before the day On the day After the day – The outstanding organisation, The Good practice, The Requiring improvement finding, Inadequacy and special measures. 13

PPG+ Recent examples • • Ottery St Mary – School year “Health reps” on PPG Court Thorn Surgery - Basic life support session+ Defibs Victoria – 8 -900 members, 2000 Twitters Feedback Patient learning sessions Newsletter Exercise & “Shape up” group 14

Things change 15

Empowering (1) 16

Empowering (2) 17

Empowering(3) Conclusion In sum, our evidence shows that despite a wave of consolidation, most healthcare systems have not yet realized the potential scale efficiencies from these mergers. Scale efficiencies are possible, yet capturing those efficiencies requires a change in management philosophy, an emphasis on standardization and integrated operations, and an investment in cultural transformation. Collectively, such elements could lead to cost reductions as high as 15 to 30 percent. This is an ambitious effort, and it will require much hard work on the part of executive teams. Yet it is certainly worth the effort if the ultimate prize is more satisfied patients and higherquality care at lower costs. Price Waterhouse –”Realising the benefits of scale - size should matter“ US 2016 18

In short: • Engaging service users matters and we have found outstanding examples. • How we understand value the product of engagement needs more research • As in personal relationships, engagement is best seen as as an indicator or stepping stone to partnership. 19

Finally Thank you 20
- Slides: 20