Patient exposure trends and problems in implementing ALARA

Patient exposure trends and problems in implementing ALARA Barry Wall Medical Exposure Department Radiation Protection Division Health Protection Agency Chilton, UK Centre for Radiation, Chemical and Environmental Hazards Radiation Protection Division formerly the National Radiological Protection Board
Uses of radiation in medicine Medical radiology • X-ray imaging for diagnosis • X-ray imaging to guide therapeutic interventions • Radionuclide imaging (nuclear medicine) • Radiotherapy Together 99% of man-made population dose © HPA Centre for Radiation, Chemical and Environmental Hazards - Radiation Protection Division. Formerly the National Radiological Protection Board
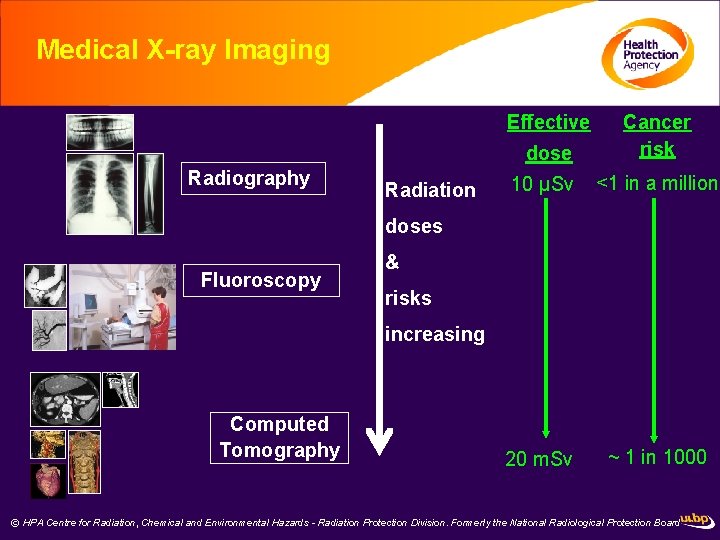
Medical X-ray Imaging Effective dose Radiography Radiation Cancer risk 10 µSv <1 in a million 20 m. Sv ~ 1 in 1000 doses Fluoroscopy & risks increasing Computed Tomography © HPA Centre for Radiation, Chemical and Environmental Hazards - Radiation Protection Division. Formerly the National Radiological Protection Board
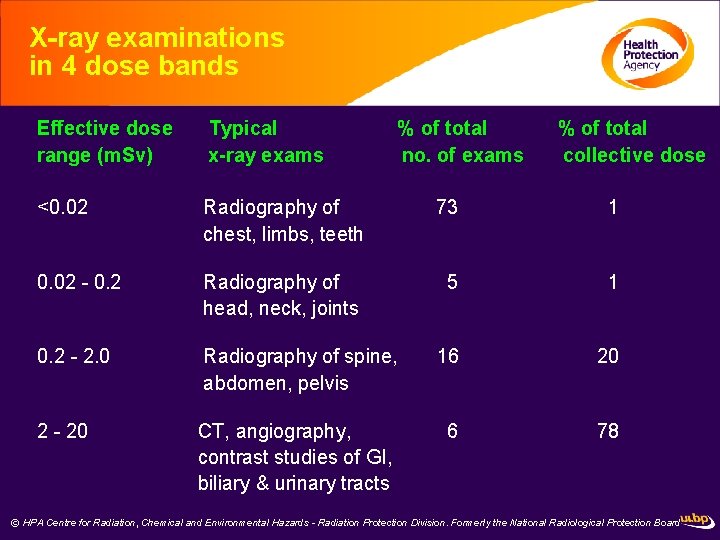
X-ray examinations in 4 dose bands Effective dose range (m. Sv) Typical x-ray exams % of total no. of exams % of total collective dose <0. 02 Radiography of chest, limbs, teeth 73 1 0. 02 - 0. 2 Radiography of head, neck, joints 5 1 0. 2 - 2. 0 Radiography of spine, abdomen, pelvis 16 20 2 - 20 CT, angiography, contrast studies of GI, biliary & urinary tracts 6 78 © HPA Centre for Radiation, Chemical and Environmental Hazards - Radiation Protection Division. Formerly the National Radiological Protection Board

Typical Effective Doses from X-ray Procedures Interventional Angiography CT body Ba enema (colon) Ba meal (stomach) IVU (urinary tract) CT head Lumbar spine Thoracic spine Pelvis / hip Abdomen Highest dose band Skull Chest 0 5 10 15 Effective dose, m. Sv 20 © HPA Centre for Radiation, Chemical and Environmental Hazards - Radiation Protection Division. Formerly the National Radiological Protection Board
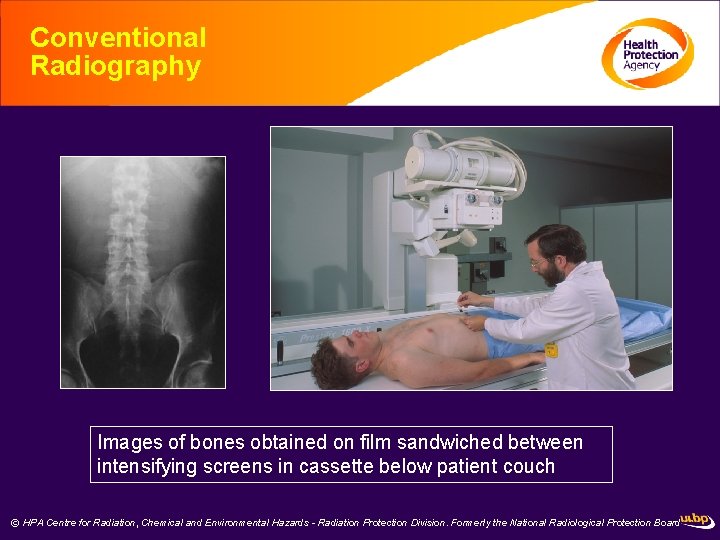
Conventional Radiography Images of bones obtained on film sandwiched between intensifying screens in cassette below patient couch © HPA Centre for Radiation, Chemical and Environmental Hazards - Radiation Protection Division. Formerly the National Radiological Protection Board
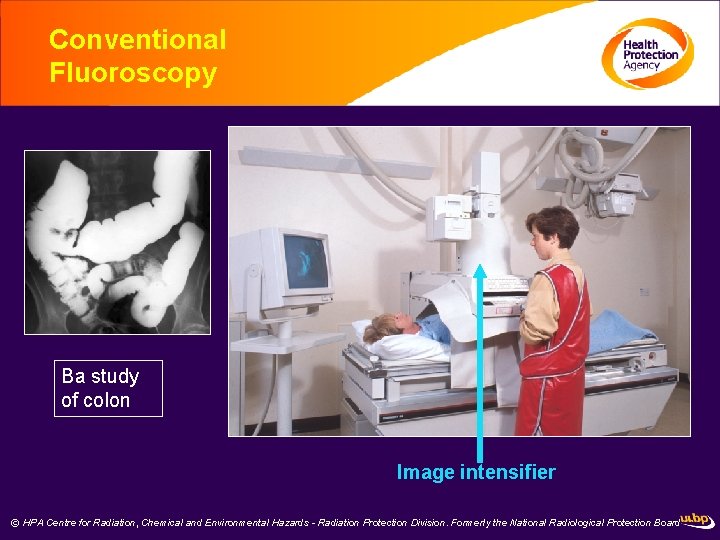
Conventional Fluoroscopy Ba study of colon Image intensifier © HPA Centre for Radiation, Chemical and Environmental Hazards - Radiation Protection Division. Formerly the National Radiological Protection Board
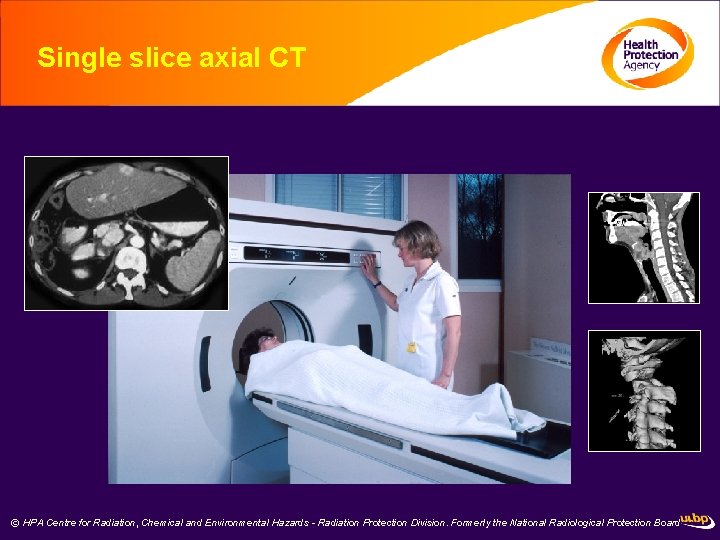
Single slice axial CT © HPA Centre for Radiation, Chemical and Environmental Hazards - Radiation Protection Division. Formerly the National Radiological Protection Board

Recent developments in medical imaging Digital radiography Storage phosphors or flat-panel detectors static digital images Amorphous selenium coating over TFT matrix Digital fluoroscopy Image intensifier or flat panel detector moving digital images and DSA © HPA Centre for Radiation, Chemical and Environmental Hazards - Radiation Protection Division. Formerly the National Radiological Protection Board
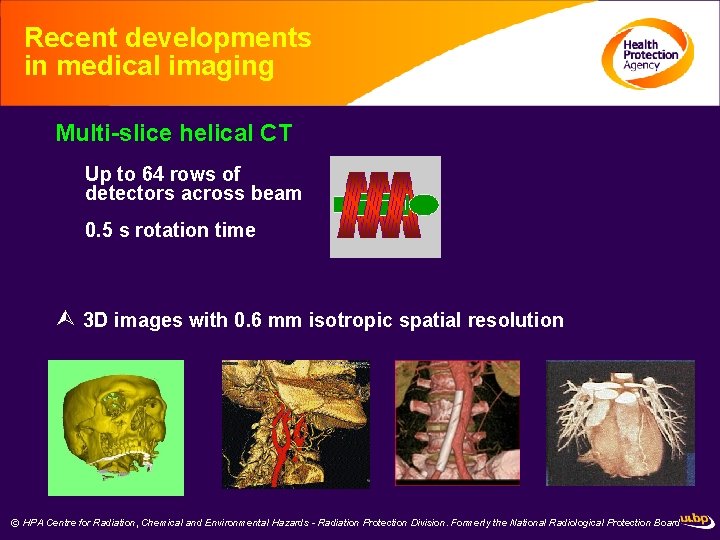
Recent developments in medical imaging Multi-slice helical CT Up to 64 rows of detectors across beam 0. 5 s rotation time 3 D images with 0. 6 mm isotropic spatial resolution © HPA Centre for Radiation, Chemical and Environmental Hazards - Radiation Protection Division. Formerly the National Radiological Protection Board
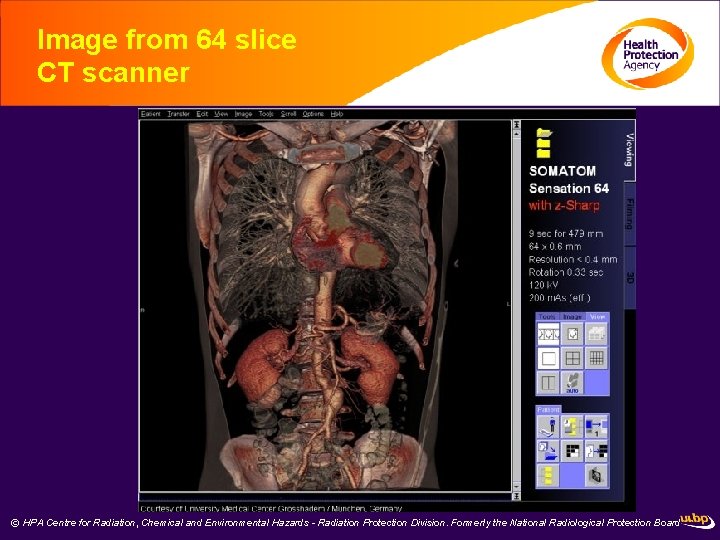
Image from 64 slice CT scanner © HPA Centre for Radiation, Chemical and Environmental Hazards - Radiation Protection Division. Formerly the National Radiological Protection Board
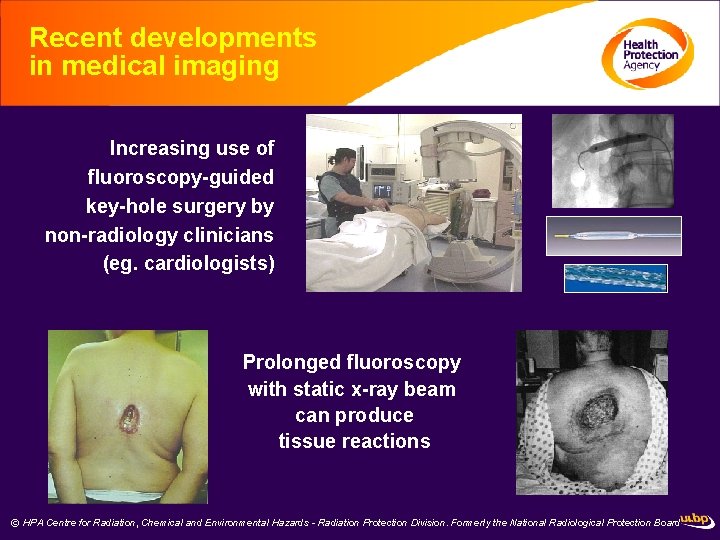
Recent developments in medical imaging Increasing use of fluoroscopy-guided key-hole surgery by non-radiology clinicians (eg. cardiologists) Prolonged fluoroscopy with static x-ray beam can produce tissue reactions © HPA Centre for Radiation, Chemical and Environmental Hazards - Radiation Protection Division. Formerly the National Radiological Protection Board

Patient Dose Measurement Methods Radiography Direct measurements can only be made in x-ray Entrance surface dose (ESD) Fluoroscopy Dose-area product (DAP) beam outside the patient CT CT dose index (CTDI) © HPA Centre for Radiation, Chemical and Environmental Hazards - Radiation Protection Division. Formerly the National Radiological Protection Board 38507, 29033, 29037
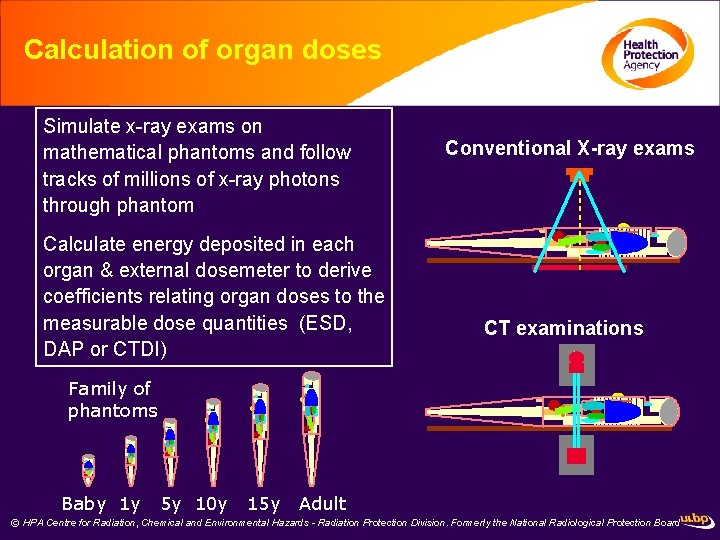
Calculation of organ doses Simulate x-ray exams on mathematical phantoms and follow tracks of millions of x-ray photons through phantom Calculate energy deposited in each organ & external dosemeter to derive coefficients relating organ doses to the measurable dose quantities (ESD, DAP or CTDI) Conventional X-ray exams CT examinations Family of phantoms Baby 1 y 5 y 10 y 15 y Adult © HPA Centre for Radiation, Chemical and Environmental Hazards - Radiation Protection Division. Formerly the National Radiological Protection Board
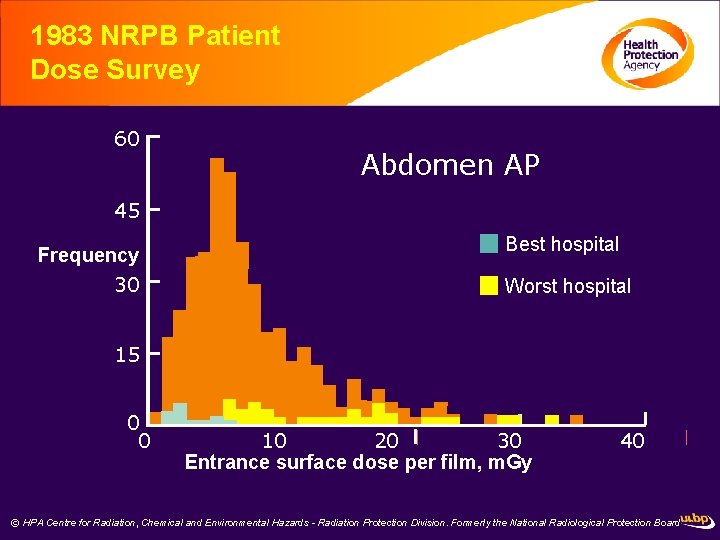
1983 NRPB Patient Dose Survey 60 Abdomen AP 45 Frequency 30 Best hospital Worst hospital 15 0 0 10 20 30 Entrance surface dose per film, m. Gy 40 © HPA Centre for Radiation, Chemical and Environmental Hazards - Radiation Protection Division. Formerly the National Radiological Protection Board 22834

Radiation protection principles for medical exposures Justification Optimisation But no dose limits © HPA Centre for Radiation, Chemical and Environmental Hazards - Radiation Protection Division. Formerly the National Radiological Protection Board
Optimisation of medical exposures X-ray equipment and techniques should be selected to ensure that patient exposures are ALARA consistent with obtaining the required diagnostic information How? © HPA Centre for Radiation, Chemical and Environmental Hazards - Radiation Protection Division. Formerly the National Radiological Protection Board

DRLs - the first step to ALARA Patient exposures cannot be reduced indefinitely without impact on image quality Radiologists subjectively assess the adequacy of their images every time they report on them but they cannot intuitively assess the patient dose (particularly with modern digital systems) DRLs provide a means for alerting radiologists when their patient doses become unusually high © HPA Centre for Radiation, Chemical and Environmental Hazards - Radiation Protection Division. Formerly the National Radiological Protection Board

DRLs - the first step to ALARA Concept of DRLs recognised in: - ICRP Publications 60 (1991) & 73 (1996) - IAEA BSS (1994) - EC Medical Exposure Directive (1997) DRLs usually set at 3 rd quartile of dose distributions seen in national patient dose surveys Hospitals with mean doses > DRL should investigate why and take corrective action, if not clinically justified DRLs are ‘investigation levels’ triggering further optimisation where most urgently needed. © HPA Centre for Radiation, Chemical and Environmental Hazards - Radiation Protection Division. Formerly the National Radiological Protection Board

DRLs - the first step to ALARA On exceeding DRL, the subsequent investigation will involve detailed analysis of existing routine performance tests on the x-ray equipment (that include simple image quality checks) [e. g. IPEM Report 91] and reference to international guidance on good imaging techniques: e. g. in European Guidelines on Quality Criteria for adult and paediatric radiography and CT © HPA Centre for Radiation, Chemical and Environmental Hazards - Radiation Protection Division. Formerly the National Radiological Protection Board
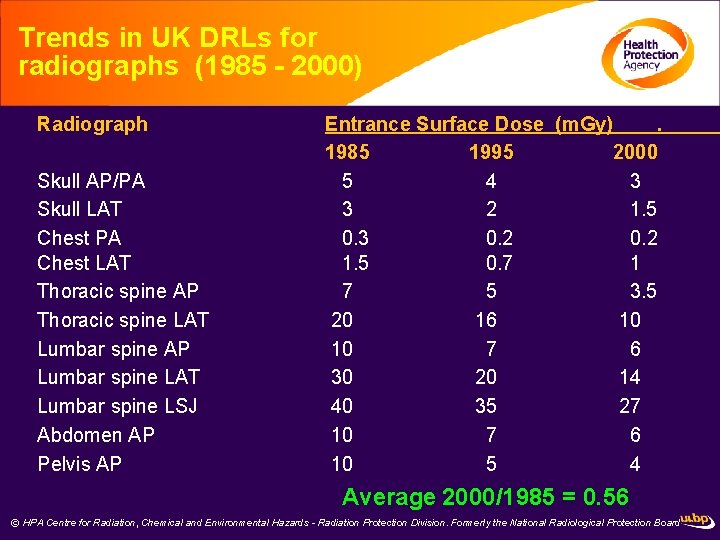
Trends in UK DRLs for radiographs (1985 - 2000) Radiograph Skull AP/PA Skull LAT Chest PA Chest LAT Thoracic spine AP Thoracic spine LAT Lumbar spine AP Lumbar spine LAT Lumbar spine LSJ Abdomen AP Pelvis AP Entrance Surface Dose (m. Gy). 1985 1995 2000 5 4 3 3 2 1. 5 0. 3 0. 2 1. 5 0. 7 1 7 5 3. 5 20 16 10 10 7 6 30 20 14 40 35 27 10 7 6 10 5 4 Average 2000/1985 = 0. 56 © HPA Centre for Radiation, Chemical and Environmental Hazards - Radiation Protection Division. Formerly the National Radiological Protection Board
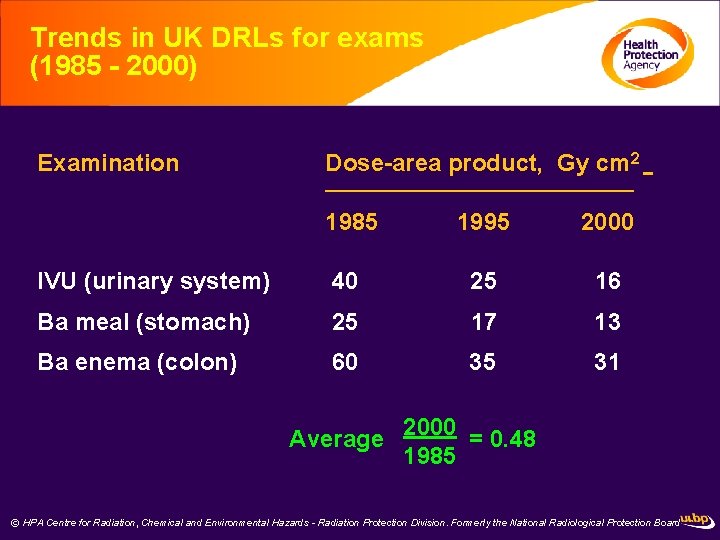
Trends in UK DRLs for exams (1985 - 2000) Examination Dose-area product, Gy cm 2 __________________ 1985 1995 2000 IVU (urinary system) 40 25 16 Ba meal (stomach) 25 17 13 Ba enema (colon) 60 35 31 Average 2000 = 0. 48 1985 © HPA Centre for Radiation, Chemical and Environmental Hazards - Radiation Protection Division. Formerly the National Radiological Protection Board
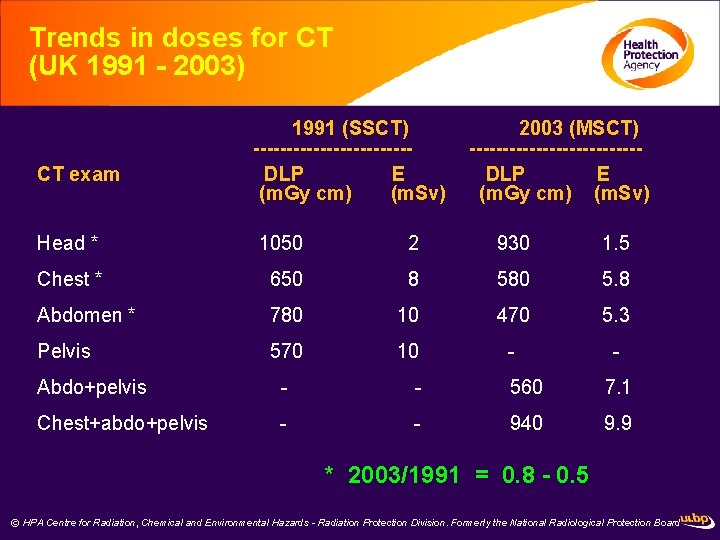
Trends in doses for CT (UK 1991 - 2003) CT exam 1991 (SSCT) ------------DLP E (m. Gy cm) (m. Sv) 2003 (MSCT) -------------DLP E (m. Gy cm) (m. Sv) Head * 1050 2 930 1. 5 Chest * 650 8 580 5. 8 Abdomen * 780 10 470 5. 3 Pelvis 570 10 - - Abdo+pelvis - - 560 7. 1 Chest+abdo+pelvis - - 940 9. 9 * 2003/1991 = 0. 8 - 0. 5 © HPA Centre for Radiation, Chemical and Environmental Hazards - Radiation Protection Division. Formerly the National Radiological Protection Board

Future problems in implementing ALARA Although doses are coming down for ‘old routine’ CT exams scanning speeds have increased and whole trunk scans (with higher doses) are becoming the ‘new routine’. Only radiologists can decide whether these increasing patient doses are ‘reasonable’ in relation to the extra diagnostic information obtained. BUT they need to be reminded regularly to consider if the doses are ALARA - through the use of DRLs. The major problems arise in trying to keep abreast of all these rapid developments in medical imaging and their impact on patient exposures, so that appropriate DRLs can be established to implement ALARA - ASAP © HPA Centre for Radiation, Chemical and Environmental Hazards - Radiation Protection Division. Formerly the National Radiological Protection Board
- Slides: 24