Patient Controlled Analgesia Pain Management of Post Operative

























- Slides: 26

Patient Controlled Analgesia Pain Management of Post. Operative Patients

My Patient • • • CS Age: 59 Gender: M Medical History: DJD/Osteoarthritis, Hypothyroid, Kidney Stones, BPH Social: Kids moved out, lives at home with wife Barriers to care? Surgery Total R hip replacement TKA vs THA (RTHR) NOT BKA or AKA

Patho • Osteoarthritis/DJD • Kidney Stones • Hypothyroidism • Benign Prostatic Hyperplasia

Treatment/Medications *Tylenol • Maalox • Dulcolax • Tums • MOM • Naloxone • Zofran • Oxycodone • Miralax • Ambien • Finasteride • • • Tamsulosin Xarelto Levothyroxine Cefazolin Morphine PCA

CS’s Morphine Order • • • Dilaudid, Fentanyl, Morphine Loading dose 3 mg Demand dose 0. 5 mg Lockout interval 10 mins One hour limit 8 mg Background infusion • 0. 5/10/8

Assessment • • • Muscles are “tired and stiff” upon movement Fatigue Limited ROM in the R hip Bowel sounds hypoactive Cell-Saver Drain Foley SCDs RAC 20 G Dressing CDI

Three Good Nursing Dx for CS • Acute pain related to hip surgery as evidenced by use of PCA pump, patient report of pain, and moaning upon movement. • Risk for infection related to surgical incision and antibiotic therapy. • Risk for situational low self-esteem related to functional impairments, unfamiliar environment, and social role changes (unable to attend work. )

CARE PLAN • Nursing Dx: Acute pain related to hip surgery as evidenced by use of PCA pump, patient report of pain, and moaning upon movement. • Assessment: Patient reports pain. (Subjective) Patient moans upon movement and has restlessness. Pt is two hours post-op from total right hip replacement (Objective)

GOALS • Patient will report pain is relieved as soon as possible. (Short-term) • Patient will follow pain med regimen at home and verbalize three ways to have the best pain control upon discharge. (Long-term)

INTERVENTIONS • 1. Assess intensity, location, characteristics, and severity of pain throughout shift. • 2. Determine patient’s pain on a 0 to 10 scale. • 3. Discard PCA syringe, vials, or containers after use. • 4. Assess the patient’s LOC and mental status.

INTERVENTIONS • 5. Nurse will double check that the PCA order is correctly put into the machine • 6. Nurse will assess respiratory status (rate, depth, oxygenation) for a baseline and throughout shift in addition to using continuous pulse oximetry recording while the PCA is in use. • 7. Nurse will monitor for side effects of nausea, vomiting, dizziness, sedation. • 8. Nurse will educate patient and patient visitors to not press the PCA button

INTERVENTIONS • 9. Assess patient’s age and monitor how this can make a difference. • 10. Note that elderly patients may under-report pain as opposed to younger patients aged 20 -39. • 11. Assess precipitating and aggravating factors of pain. • 12. Note the patient’s attitude towards pain including any tolerance or history of substance abuse.

INTERVENTIONS • 13. Nurse will note cultural and developmental influences affecting pain response. • 14. Nurse will observe nonverbal cues • 15. Nurse will provide comfort measures. • 16. Nurse will instruct the client to report pain as soon as it begins. • 17. Nurse will identify ways of avoiding/minimizing pain.

EVALUATION • Short term goal met! Patient reports relief of pain from PCA bolus. • Long term goal met! Patient repeats back three ways to control pain and repeats back the instructions for his discharge pain meds.

Why do we care about pain control? • Patient education • Participation in activites/therapy • Psychological Health • GI health • Stable Vitals • Promotes early mobility • Infection

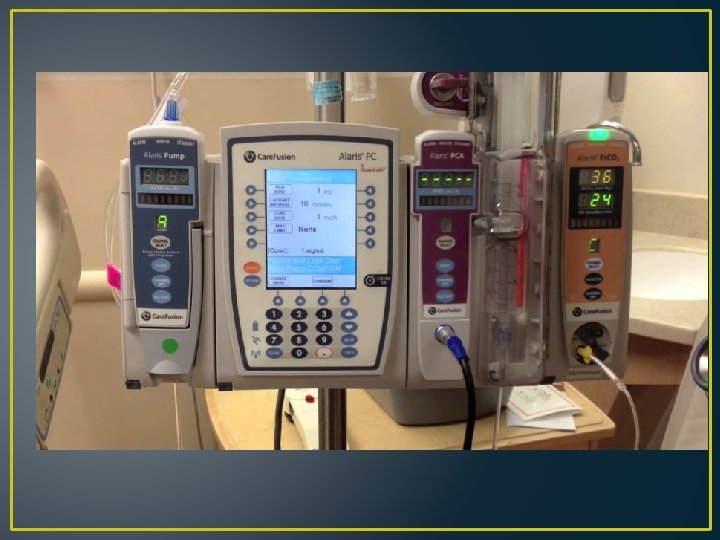
Equipment • • Is locked Cannot change settings without the key Bugs have been fixed Light Clear Pump $$$ Concentration-Standard for Safety


Who gets a PCA?

PCA-Safety Precautions • Transcribing • Dispensing • Administering • Monitoring

WARNING • Do not occlude the line or turn off alarms! • New patients need continuous pain assessment! • High Risk Patients • Sleep apnea • Kidney/Liver failure • Hypovolemia • PCA can mask complications of: • • Urinary retention Compartment Syndrome PE MI

Age/Sex Differences • Younger patients had a shorter duration of anesthesia, they required rescue analgesics more than the older patients even though they had larger doses of the fentanyl (53% vs 47. 9%) • Using ketorolac alongside with PCA resulted in less breakthrough pain • Females needed more rescue analgesics than males. • Females had higher incidence of N/V

Side Effects • The likelihood of PONV decreases by 13% for each 10 year increase in age. • Incidence of nausea and vomiting were greater in younger patients Sedation occurred more with the older patient group • N/V: 23. 8% young, 20. 6% old • Headache: 2. 3% young, 1. 7% old • Dizziness: 9. 8% young, 6. 5% old • Sedation: 0. 1% young, 0. 7% old

Perks of PCA • Don’t have to bother nurse • Don’t have to wait for med administration process (five rights, narc counts, waiting for machine, nurse interruptions, signing into computer and scanning) • Faster action • It takes less meds to prevent pain than to treat it • Don’t need food (but will probably need an antiemetic)

Problems of PCA • 22% of patients are afraid of addictions and 30% fear overdose • The control can fall off the bed or be accidentally pressed • Some patients are unable to use • IV meds don’t last as long • More side effects

Patient and Use Factors to Note • • • Previous education/experiences Anxiety or psychological conditions Age Sex Type of surgery/block (general anesthesia vs a nerve block) • Previous tolerance • Background Infusions-0. 1 to 0. 8% without and 1. 1 to 3. 9% with • Adjuvants

Conclusion • Sedation always precedes respiratory depression • Each patient is unique and should be assessed and treated as such • Careful planning and programming of a PCA pump can NOT replace careful assessment and evaluation of a nurse!!