PATIENT CARE NETWORK OF OKLAHOMA PCNOK Oklahoma Healthcare












- Slides: 17

PATIENT CARE NETWORK OF OKLAHOMA (PCNOK) Oklahoma Healthcare Authority ABD Care Coordination RFI Response August 17, 2015

2 Patient Care Network of Oklahoma • Care coordination network of 20 Federally Qualified Health Centers (FQHCs) • Serve over 160, 000 patients • Operate over 50 primary care sites in 77 counties • Patient Centered Medical Homes that currently target chronically ill and medically complex patients • Strategic investment in infrastructure including Electronic Health Records, Health Information Exchange (connectivity to My. Health), and data analytics and performance measurement (i. e. Sooner. Verse)

3 FQHCs in Oklahoma

4 FQHCs in Oklahoma ealth H l a t n e M d Medical an Pharmacy Mobile Services Optometry Dental

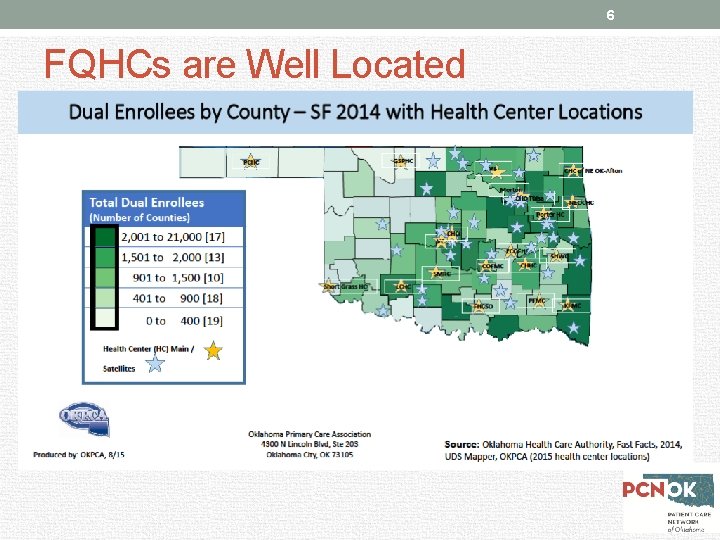
5 FQHCs are Uniquely Positioned “Many FQHCs and CHCs are uniquely positioned to coordinate care for dual-eligible beneficiaries because they provide primary care, behavioral health services, and care management services, often at the same clinic site. ” The Medicare Payment Advisory Commission: June 2013 Report to the Congress: Medicare and the Health Care Delivery System

6 FQHCs are Well Located

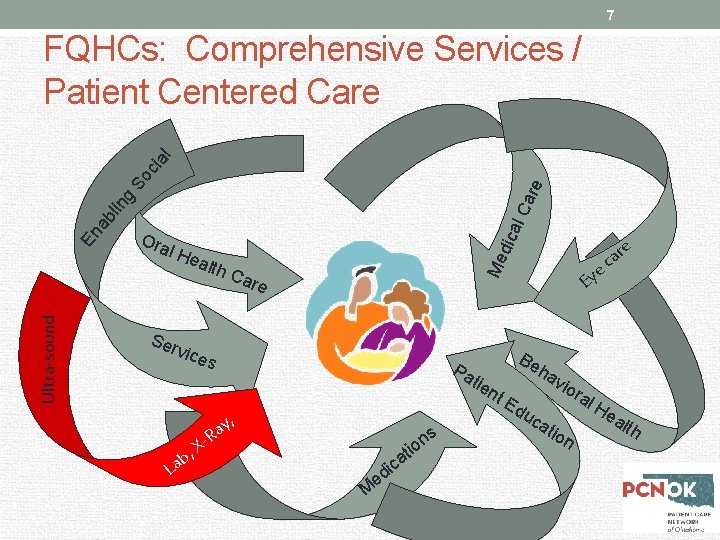
7 Ultra-sound l He alth Ser vice dic Ora Car e s Pa y, a R s n tio a ic La M ed Ey Be h tie - X b, e Me En ab lin g al C are So cia l FQHCs: Comprehensive Services / Patient Centered Care e r ca nt Ed u av ior a ca l. H tio n ea lth

8 FQHC: Care Model for Complex Patients Integrated Delivery Model Data Driven Patient Centered Better Outcomes………AND Lower Costs

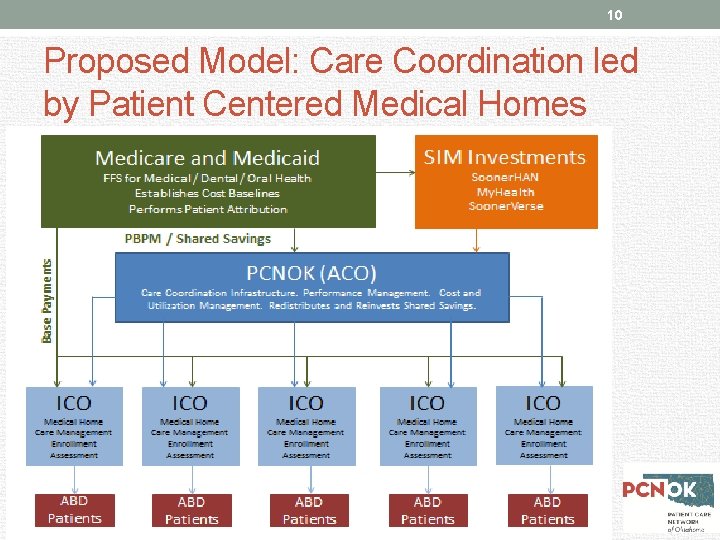
9 Proposed Model: Care Coordination led by Patient Centered Medical Homes • Develop an Accountable Care Organization structure that will manage the cost and quality outcomes of the target population through a managed fee-for-service payment mechanism • Employ a care coordination model that includes local, dedicated care managers to work with the highest complexity patients • Through investments from the State, establish a robust technology and data infrastructure for the creation of statewide care coordination and claims-based risk assessments and interventions

10 Proposed Model: Care Coordination led by Patient Centered Medical Homes

11 Best Practices for Complex Patients • High-contact, on the ground intensive care management • Focus on coordinating communication across provider care settings (i. e. hospitals, primary care, social service agencies) • Leverage community-based resources, including FQHCs • Many FQHCs are uniquely positioned to coordinate care for dual-eligible beneficiaries because they provide primary care, behavioral health services, and care management services, often at the same clinic site Source: The Medicare Payment Advisory Commission: June 2013 Report to the Congress: Medicare and the Health Care Delivery System

12 Proposed Model: Flexibility and Scalability • Builds upon existing community based, managed FFS pilots already underway in Oklahoma • Leverages existing infrastructure among FQHCs • Allows for flexibility and innovation over time • Risk sharing models could change as model matures • PCNOK can interact with a variety of payers • Model can expand to include patients beyond Duals • Includes proven best practices of approaches in other states that target Duals and other high-need patients

13 Financial Model Overview • Maintenance of the payment relationship between Sooner. Care and Medicare as payers; PCNOK FQHCs maintain all base, contracted services within the current covered benefits and services. • Tiered PBPM payment based on acuity to the PCNOK to cover the cost of the Care Management function. • “Shared Savings” payments paid to the PCNOK, and correspondingly shared to the Health Centers. • Quality measures that demonstrate no use of “care rationing” to achieve cost goals. • No impact on patient’s right to choose where to seek care or payment terms to providers outside of the PCNOK. • Alignment with State and Federal Regulations.

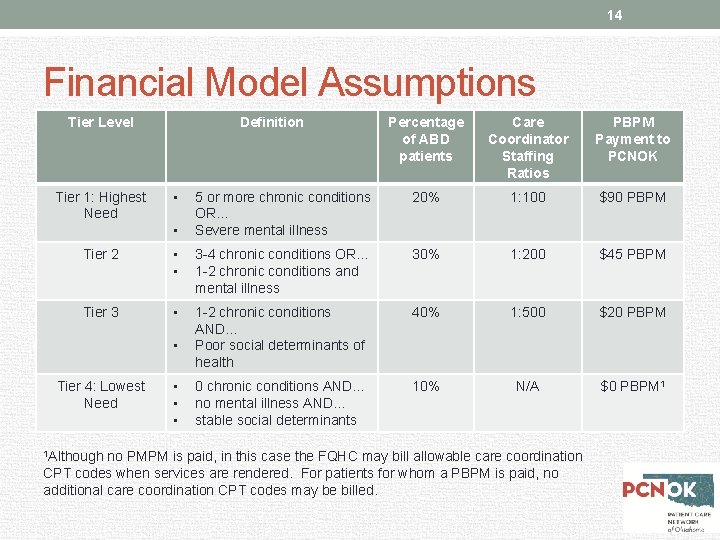
14 Financial Model Assumptions Tier Level Tier 1: Highest Need Definition • • Percentage of ABD patients Care Coordinator Staffing Ratios PBPM Payment to PCNOK 5 or more chronic conditions OR… Severe mental illness 20% 1: 100 $90 PBPM Tier 2 • • 3 -4 chronic conditions OR… 1 -2 chronic conditions and mental illness 30% 1: 200 $45 PBPM Tier 3 • 1 -2 chronic conditions AND… Poor social determinants of health 40% 1: 500 $20 PBPM 0 chronic conditions AND… no mental illness AND… stable social determinants 10% N/A $0 PBPM 1 • Tier 4: Lowest Need 1 Although • • • no PMPM is paid, in this case the FQHC may bill allowable care coordination CPT codes when services are rendered. For patients for whom a PBPM is paid, no additional care coordination CPT codes may be billed.

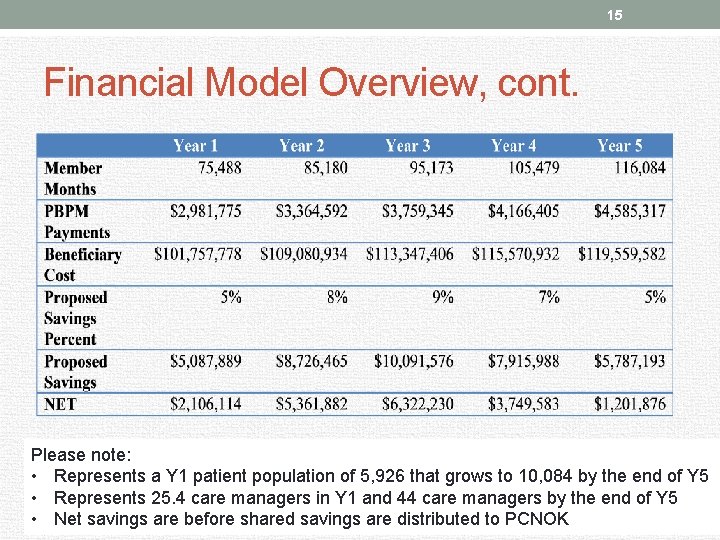
15 Financial Model Overview, cont. Please note: • Represents a Y 1 patient population of 5, 926 that grows to 10, 084 by the end of Y 5 • Represents 25. 4 care managers in Y 1 and 44 care managers by the end of Y 5 • Net savings are before shared savings are distributed to PCNOK

16 Efficient, Effective, Patient-Centered Hospital Admission Social Services Out Patient Care Specialty Care

17 QUESTIONS