Patient Assessment Objectives Students will Identify normal and

Patient Assessment

Objectives Students will: Identify normal and abnormal V/S measurements. Measure and record vital signs according to industry standards. Measure and record height and weight according to industry standards. Describe factors that would lead to error in V/S measurement Describe health factors that would affect vital signs Determine which methods to use when measuring vitals for patients in various scenarios.

Vital Signs Are important indicators of health Detect changes in normal body function May signal life-threatening conditions Provide information about responses to treatment

Vital Signs Temperature (T) Pulse (P) –same as HR Respirations (R) Blood Pressure (BP) Weight (Wt) Height (Ht) Additional Measures – Sp. O 2, CRT

When Are Vital Signs Measured: Upon admission Before & after surgery and other procedures After a fall or accident When prescribed drugs that affect the respiratory or circulatory system When there are complaints of pain, dizziness, shortness of breath, chest pain As stated on the care plan (min 8 hrs at hosp)

When Measuring Vital Signs Usually taken with the person sitting or lying The person is at rest Always report (immediately): A change from a previous measurement Vital signs above or below the normal range If you are unable to measure the vital signs

Temperature • Measurement of balance between heat lost and produced by the body. – Heat is produced by: • • – Heat may be lost through: • • Muscle and gland activity Metabolism of food Perspiration, Respiration, Excretion Measured with the Fahrenheit (F) or Celsius (C) scales

Body Temperature Factors that body temperature Illness Starvation or fasting Infection Sleep Exercise Decreased muscle activity Excitement, Stress Exposure to cold in the High temperatures in the environment Body t Temperature is usually emper ature i a. s usua in the l b. higher in the evening evenin ly the lowes t: g n c. d. Age- Younger=hotter Time- T varies up to 2 degrees during the day the aft in the ernoon m at bed orning time

Temperature Sites Oral - by mouth – most common method May be affected by hot or cold food, smoking, oxygen, chewing gum Wait 15 minutes or use alternate site Also avoid if patient is under 5, on oxygen, sedated, had oral surgery or otherwise cannot control their bite. Rectal - in the rectum –highly accurate but uncomfortable Do not use if patient has rectal surgery or bleeding Axillary - under arm – less reliable site Used when other sites are inaccessible, takes 10 min Do not use immediately after bathing

Temperature Sites Tympanic or aural - in the ear Measures in 1 to 3 seconds Temporal Artery (TA/TEMP) – temporal artery on the forehead-highly accurate Record route temperature was taken Ax – Axillary T - Oral R- Rectal A – Tympanic /Aural) TA- Temporal

Normal Body Temperature Oral 98. 6 ( 97. 6 - 99. 6) Rectal 99. 6 (98. 6 - 100. 6) Axillary 97. 6 (96. 6 - 98. 6) Typmanic 98. 6 (98. 6 - 100. 6) Temporal 99. 6 (98. 6 - 100. 6) Hypothermia – temperature below normal (<95) Hyperthermia – overheating, temperature above normal (heat stroke? ) (febrile-T(O)=1004°F and up for adults, hyperthermia=103 -105 °F) Afebrile- no fever Hyperpryexia- High fever above 106. 7 F

Types of Thermometers Clinical (glass) mercury. thermometer no longer contain Oral or rectal. (rectal are thicker/longer & labeled) Disposable covers are usually used. Electronic can be used for oral, rectal, or axillary and use disposable probe covers. Tympanic placed in auditory canal and uses disposable cover. Strips that contain special chemicals or dots that change colors can also be used.

Pulse (HR/ P) The pressure of blood pushing against the wall of an artery as the heart beats and rests. Measured for one minute while noting: rate - beats per minute rhythm - regular or irregular volume - strength or intensity - described as strong, weak, thready, bounding

Clicker question You are taking Mr. James' pulse. The beats are not spaced evenly. How would you describe his pulse when reporting to the doctor or nurse? A. thready and bounding B. weak and feeble C. strong and full D. irregular
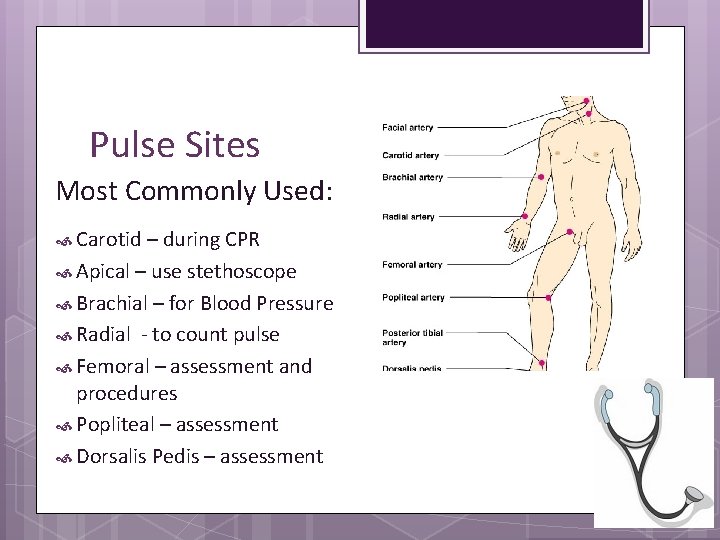
Pulse Sites Most Commonly Used: Carotid – during CPR Apical – use stethoscope Brachial – for Blood Pressure Radial - to count pulse Femoral – assessment and procedures Popliteal – assessment Dorsalis Pedis – assessment

Review Question Which is the most common site for taking the pulse? A. radial B. brachial C. apical D. carotid
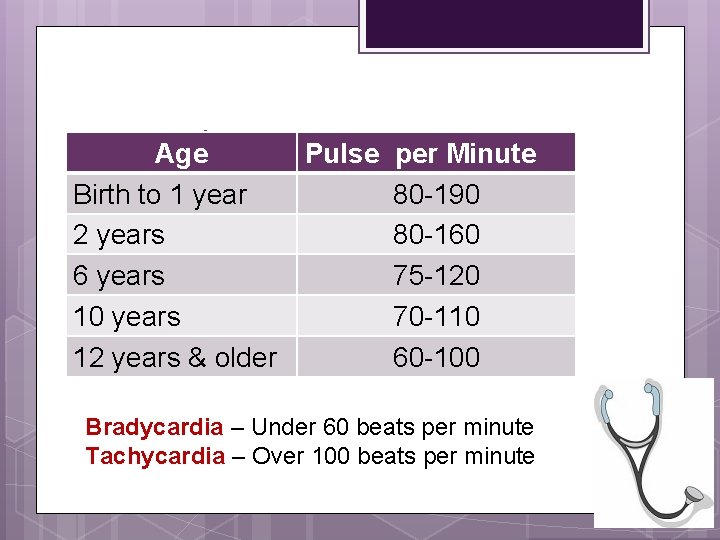
Normal Age Ranges Pulse Birth to 1 year 2 years 6 years 10 years 12 years & older per Minute 80 -190 80 -160 75 -120 70 -110 60 -100 Bradycardia – Under 60 beats per minute Tachycardia – Over 100 beats per minute
Factors that Affect Pulse Factors that pulse Exercise Stimulant drugs, caffeine Excitement, stress Fever/Illness Shock For an adult, which pulse rate is immediately reported to the doctor or nurse? a. 80 beats per minute b. 62 beats per minute c. 48 beats per minute d. 74 beats per minute Factors that pulse Sleep Depressant drugs (digoxin- cardiac medication), diuretics (decrease volume) Heart disease Coma Blood loss Position

Pulse deficit Any observed difference between Apical and radial pulse. Caused by cardiac arrhythmia

Review question To take an apical pulse rate, you must: A. count for only 15 seconds B. feel for the artery on the side of the neck C. have the patient sit or lie down D. use a stethoscope
Capillary Refill Time (CRT) For adults hold hand above heart level. Press on unpolished fingernail w/moderate pressure for 5 sec. On infants-test on sternum Observe time to reflush with color Normal CRT is LESS than 2 sec Slow CRT may indicate dehydration, hypoxia, or sepsis

Respirations Process of breathing air into (inhalation) and out of (exhalation) the lungs. Oxygen enters the lungs during inhalation. Carbon dioxide leaves the lungs during exhalation. The chest rises during inhalation and falls during exhalation. Normal rate 12 -20 breaths per minute

Assessing Respirations is measured when the person is at rest. Rate may change is patient is aware that it is being counted. To prevent this, count respirations right after taking a pulse. Keep your fingers or stethoscope over the pulse site. To count respirations, watch the chest rise and fall.

Assessing Respiration Character and quality of respirations is also assessed: Deep Shallow Labored or difficult Noises – wheezing, stertorous (a heavy, snoring type of sound) Moist or rattling sounds Dyspnea – difficult or labored breathing Apnea – absence of respirations Cheyne-Stokes – periods of dyspnea followed by periods of apnea; often noted in the dying patient Rales – bubbling or noisy sounds caused by fluids or mucus in the air passages

Blood Pressure Measure of the pressure blood exerts on the walls of arteries Blood pressure is controlled by: The force of heart contractions weakened The heart drop in BP amount of blood pumped with each heartbeat loss of blood drop in BP How easily the blood flows through the blood vessels (resistance) Narrowing of vessels increase in BP Dilatation of vessels decrease in BP

Factors that Affect Blood Pressure Factors that blood pressure Excitement, anxiety, nervous tension Stimulant drugs Exercise and eating Factors that blood pressure Rest or sleep Depressant drugs Shock Excessive loss of blood

Measuring BP A sphygmomanometer is used to measure BP Aneroid – has a round dial and needle Mercury – has a column of mercury Electronic – automated device BP is measured in millimeters (mm) of mercury (Hg). The systolic pressure is recorded over the diastolic pressure.
Normal Range of Blood Pressure Systolic: Pressure on the walls of arteries when the heart is contracting. Normal adult range – 90 - 120 mm Hg Diastolic: Constant pressure when heart is at rest Normal range – 60 - 80 mm Hg Hypertension—BP that remains above a systolic of 140 mm Hg or a diastolic of 90 mm Hg Hypertensive crisis- BP >180 systolic or 110 diastolic (emergency care needed) Hypotension—Systolic below 90 mm Hg and/or a diastolic below 60 mm Hg

Clicker response question A persistent systolic pressure above 140 mm. Hg or a diastolic pressure above 90 mm. Hg is called: A. hypertension B. hypotension C. bradycardia D. tachycardia

Measuring Height and Weight Used to estimate if a patient population is underweight or overweight BMI or Body Mass Index a statistical measure of body weight based on a person's weight and height. Wt in lbs/ (Height”x Height” x 703) BMI from 18. 5 to 24. 9 is considered normal Used to estimate pop health and resource allocation, not great for indiv. Assessment Does not account for differences in weight of body tissues Circumference is more accurate for body fat

Measuring Height and Weight General Guidelines: Use the same scale every day Make sure the scale is balanced before use Weigh the patient at the same time each day Remove jacket, robe, and shoes before weighing OBSERVE SAFETY PRECAUTIONS! Prevent injury from falls and the protruding height lever. Some people are weight conscious. Make only positive comments when weighing patients

Types of Scales Clinical scales contain a balance beam and measuring rod Bed scales or Chair scales are used for patients unable to stand Infant scales come in balanced, aneroid, or digital When weighing an infant…keep one hand slightly over but not touching the infant A tape measure is used to measure infant height.
- Slides: 32