Patient Abuse Neglect and Exploitation A Necessity to

Patient Abuse, Neglect and Exploitation A Necessity to Identify AVA Regional Academy Health and Resilience Symposium October 15, 2014 Kathy Franchek-Roa MD Assistant Professor of Pediatrics University of Utah School of Medicine

Objectives • Explain why violence is a health care issue • Describe the process in preparing your health care setting to screen for violence, abuse and exploitation • Integrate trauma-informed care throughout your health care setting

Objectives • Explain why violence is a health care issue • Describe the process in preparing your health care setting to screen for violence, abuse and exploitation • Integrate trauma-informed care throughout your health care setting

Morbidity Mortality Disease, Disability, and Social Problems Adoption of Health Risk Behaviors Social, Emotional, Cognitive Impairment Disrupted Neurodevelopment Adverse Childhood Experiences Felitti 2001; www. cdc. gov/ACE

How does this happen, this reverse alchemy, turning the gold of a newborn into the lead of a depressed, diseased adult? Felitti 2001

Morbidity Mortality Disease, Disability, and Social Problems Adoption of Health Risk Behaviors Social, Emotional, Cognitive Impairment Disrupted Neurodevelopment Adverse Childhood Experiences Felitti 2001; www. cdc. gov/ACE

Morbidity Mortality Disease, Disability, and Social Problems Adoption of Health Risk Behaviors Social, Emotional, Cognitive Impairment Disrupted Neurodevelopment Adverse Childhood Experiences Felitti 2001; www. cdc. gov/ACE

Morbidity Mortality Disease, Disability, and Social Problems Adoption of Health Risk Behaviors Social, Emotional, Cognitive Impairment Disrupted Neurodevelopment Childhood Sexual Abuse Felitti 2001; www. cdc. gov/ACE

Morbidity Mortality Disease, Disability, and Social Problems Adoption of Health Risk Behaviors Social, Emotional, Cognitive Impairment Disrupted Neurodevelopment leading to physical deregulation Childhood Sexual Abuse Felitti 2001; www. cdc. gov/ACE

Morbidity Mortality Disease, Disability, and Social Problems Adoption of Health Risk Behaviors Social, Emotional, Cognitive Impairment Disrupted Neurodevelopment leading to physical deregulation Childhood Sexual Abuse Felitti 2001; www. cdc. gov/ACE

Morbidity Mortality Disease, Disability, and Social Problems Adoption of Health Risk Behaviors Chronic Depression Disrupted Neurodevelopment leading to physical deregulation Childhood Sexual Abuse Felitti 2001; www. cdc. gov/ACE
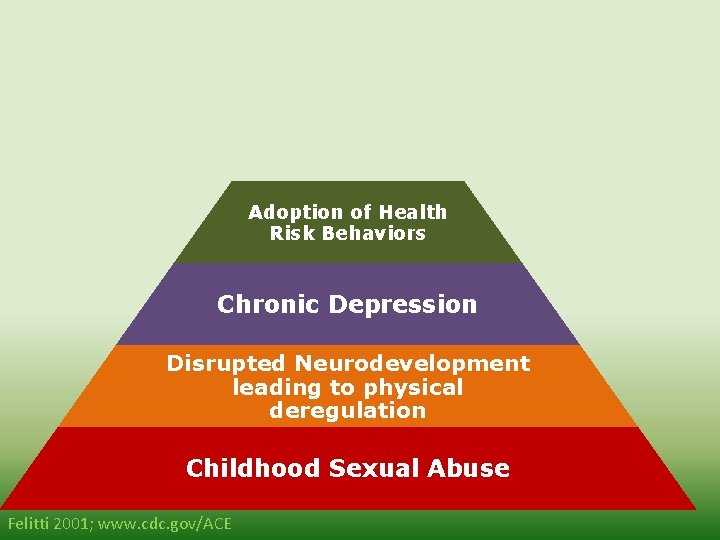
Morbidity Mortality Disease, Disability, and Social Problems Adoption of Health Risk Behaviors Chronic Depression Disrupted Neurodevelopment leading to physical deregulation Childhood Sexual Abuse Felitti 2001; www. cdc. gov/ACE
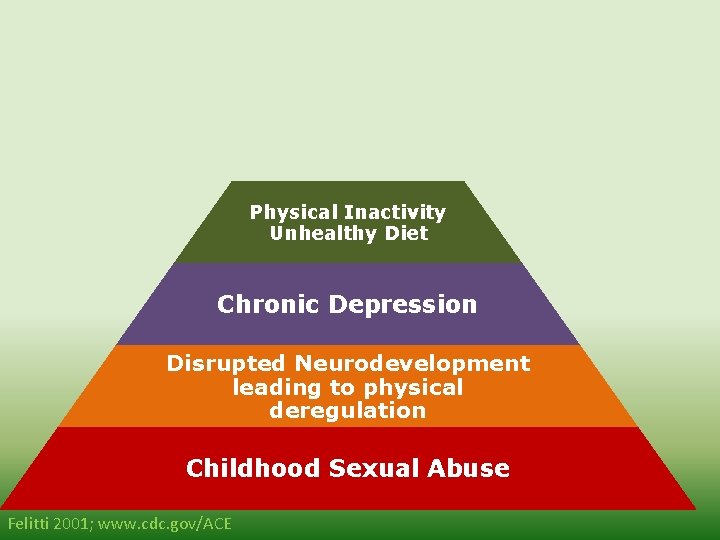
Morbidity Mortality Disease, Disability, and Social Problems Physical Inactivity Unhealthy Diet Chronic Depression Disrupted Neurodevelopment leading to physical deregulation Childhood Sexual Abuse Felitti 2001; www. cdc. gov/ACE
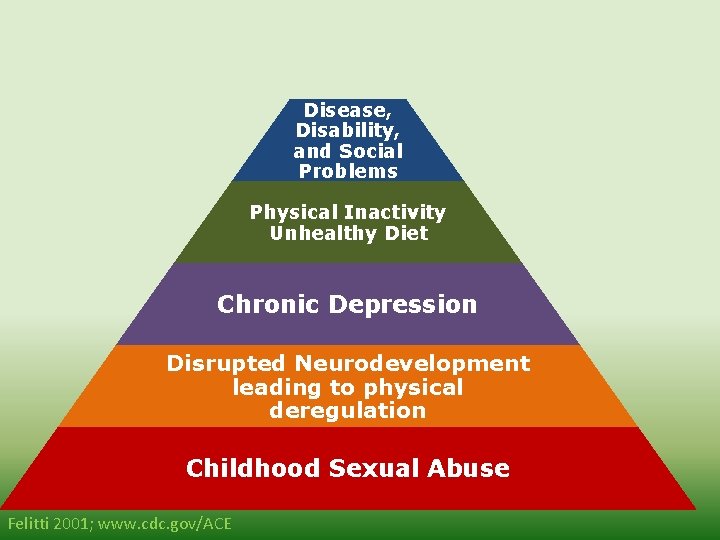
Morbidity Mortality Disease, Disability, and Social Problems Physical Inactivity Unhealthy Diet Chronic Depression Disrupted Neurodevelopment leading to physical deregulation Childhood Sexual Abuse Felitti 2001; www. cdc. gov/ACE

Morbidity Mortality HTN Diabetes Obesity Physical Inactivity Unhealthy Diet Chronic Depression Disrupted Neurodevelopment leading to physical deregulation Childhood Sexual Abuse Felitti 2001; www. cdc. gov/ACE

Morbidity Mortality HTN Diabetes Obesity Physical Inactivity Unhealthy Diet Chronic Depression Disrupted Neurodevelopment leading to physical deregulation Childhood Sexual Abuse Felitti 2001; www. cdc. gov/ACE

Morbidity Mortality HTN Diabetes Obesity Physical Inactivity Unhealthy Diet Chronic Depression Disrupted Neurodevelopment leading to physical deregulation Childhood Sexual Abuse Felitti 2001; www. cdc. gov/ACE

Morbidity Mortality HTN Diabetes Obesity Physical Inactivity Unhealthy Diet Chronic Depression Disrupted Neurodevelopment leading to physical deregulation Childhood Sexual Abuse Felitti 2001; www. cdc. gov/ACE

Adverse Childhood Experiences Obesity is not the problem– it is the solution. Vincent J Felitti MD

What’s Your ACE Score?

Childhood Adversity • Adversity and on-going toxic stress exposure during childhood is of critical concern because it can negatively affect brain development resulting in permanent changes to brain anatomy and function Mc. Ewen 2007; 2010

Childhood Adversity • A child’s response to stress may have originated as a biologically based adaptation to the child’s abnormal world Hibel 2011; Mc. Ewen 2007; 2010; Stirling 2008; www. developingchild. harvard. edu

Up to 30% of Children are exposed to IPV Mc. Donald 2006; Moore 2007

Child Exposure to IPV “Domestic violence…seems to be the most toxic form of violence for children… “For many children, the first lessons they learn about violence are not from television or from the streets, but from their parents. ” Groves 2002

Objectives • Explain why violence is a health care issue “Patients see doctors because of anxiety, while doctors see patients because of disease. Therein lies the problem between the two. ” Michael Balint 1972

Objectives • Explain why violence is a health care issue • Describe the process in preparing your health care setting to screen for violence, abuse and exploitation

Physical and Mental Health Consequences • • • AVA; CDC 2008; Plichta 2004; Zolotor 2009 Physical injury Permanent disability Mental illness Neurologic Cardiovascular Muscle/Joint disease Pulmonary Gastrointestinal Chronic pain syndromes Health risk behaviors

Violence as a Public Health Issue 1967 Maine opens first DV shelter 1979 SG report listing violence as a priority Dahlberg 2009 1970 “We will not be beaten” 1983 CDC Violence Epidemiology CDC Violence Branch Epidemiology Branch 1975 Most US States allow wives to bring criminal action against husbands for physical abuse 1990 2020 Healthy People addresses 2000 Healthy violence People addresses violence 1976 First marital rape law 1992 AMA recommends screening AMA women for DV recommends screening women for DV 1978 National Coalition Against Sexual Assault is formed 1993 Violence seen as a public health issue 1980 1994 VAWA Family Violence Prevention Fund is established 1994 National Violence Against Women National Survey Violence Against Women Survey 2013 USPSTF recommendations USPSTF for recommendation screening women for IPV for screening women for IPV

Screening Recommendations • • AMA AAP ACOG USPSTF recommends that – Clinicians screen women of childbearing age for IPV and provide or refer women who screen positive to intervention services – This recommendation applies to women who do not have signs or symptoms of abuse ACOG 2012; AMA 2008; Moyer 2013; Thackeray 2010; USPSTF 2013

Abuse, Neglect and Exploitation

Purpose of Policy • Policy on Abuse, Neglect and Exploitation is to ensure appropriate guidelines for physicians and staff caring for patients they suspect may be victims of abuse, neglect or exploitation

Types of Abuse Covered in the Policy Intimate Partner Violence Vulnerable Adult Abuse Trafficking in Persons Child Abuse and Neglect Any patient who presents with concerns of abuse, neglect and exploitation • Further additions: chapter specific to sexual assault • • •

Chapter Organization • • • Definitions Public Health Impact Standards Health Consequences Risk Factors/Presenting Signs and Symptoms Procedure for Identifying Victims Procedure Once Victim Identified Resource and Referral Information Additional Considerations

INTIMATE PARTNER VIOLENCE
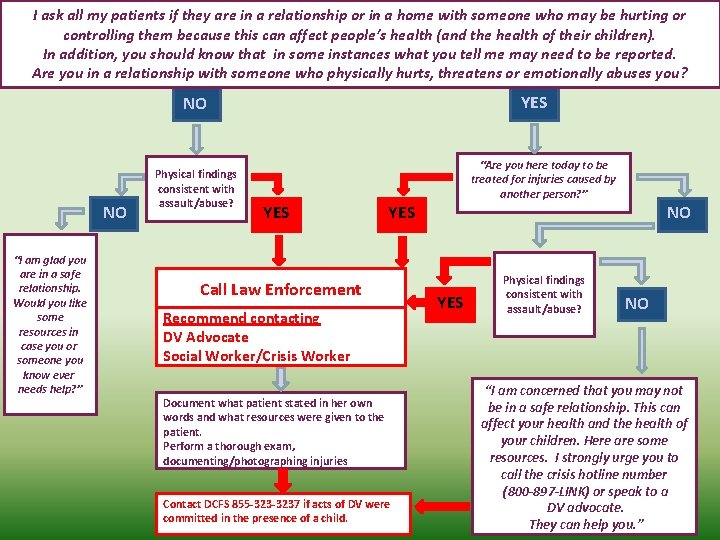
I ask all my patients if they are in a relationship or in a home with someone who may be hurting or controlling them because this can affect people’s health (and the health of their children). In addition, you should know that in some instances what you tell me may need to be reported. Are you in a relationship with someone who physically hurts, threatens or emotionally abuses you? YES NO NO “I am glad you are in a safe relationship. Would you like some resources in case you or someone you know ever needs help? ” Physical findings consistent with assault/abuse? “Are you here today to be treated for injuries caused by another person? ” YES Call Law Enforcement Recommend contacting DV Advocate Social Worker/Crisis Worker Document what patient stated in her own words and what resources were given to the patient. Perform a thorough exam, documenting/photographing injuries Contact DCFS 855 -3237 if acts of DV were committed in the presence of a child. NO YES Physical findings consistent with assault/abuse? NO “I am concerned that you may not be in a safe relationship. This can affect your health and the health of your children. Here are some resources. I strongly urge you to call the crisis hotline number (800 -897 -LINK) or speak to a DV advocate. They can help you. ”

VULNERABLE ADULT ABUSE
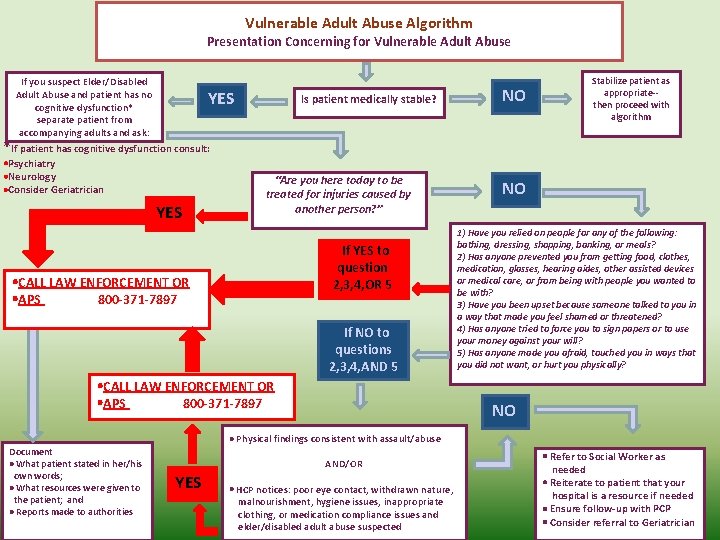
Vulnerable Adult Abuse Algorithm Presentation Concerning for Vulnerable Adult Abuse If you suspect Elder/Disabled Adult Abuse and patient has no cognitive dysfunction* separate patient from accompanying adults and ask: YES Is patient medically stable? NO Stabilize patient as appropriate-then proceed with algorithm *If patient has cognitive dysfunction consult: Psychiatry Neurology Consider Geriatrician YES “Are you here today to be treated for injuries caused by another person? ” If YES to question 2, 3, 4, OR 5 CALL LAW ENFORCEMENT OR APS 800 -371 -7897 If NO to questions 2, 3, 4, AND 5 CALL LAW ENFORCEMENT OR APS 800 -371 -7897 NO 1) Have you relied on people for any of the following: bathing, dressing, shopping, banking, or meals? 2) Has anyone prevented you from getting food, clothes, medication, glasses, hearing aides, other assisted devices or medical care, or from being with people you wanted to be with? 3) Have you been upset because someone talked to you in a way that made you feel shamed or threatened? 4) Has anyone tried to force you to sign papers or to use your money against your will? 5) Has anyone made you afraid, touched you in ways that you did not want, or hurt you physically? NO Physical findings consistent with assault/abuse Document What patient stated in her/his own words; What resources were given to the patient; and Reports made to authorities AND/OR YES HCP notices: poor eye contact, withdrawn nature, malnourishment, hygiene issues, inappropriate clothing, or medication compliance issues and elder/disabled adult abuse suspected Refer to Social Worker as needed Reiterate to patient that your hospital is a resource if needed Ensure follow-up with PCP Consider referral to Geriatrician

TRAFFICKING IN PERSONS
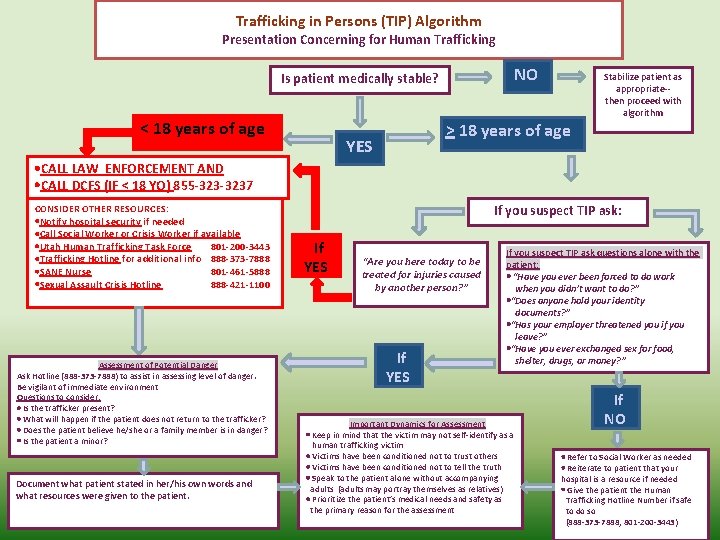
Trafficking in Persons (TIP) Algorithm Presentation Concerning for Human Trafficking NO Is patient medically stable? < 18 years of age > 18 years of age YES Stabilize patient as appropriate-then proceed with algorithm CALL LAW ENFORCEMENT AND CALL DCFS (IF < 18 YO) 855 -3237 CONSIDER OTHER RESOURCES: Notify hospital security if needed Call Social Worker or Crisis Worker if available Utah Human Trafficking Task Force 801 -200 -3443 Trafficking Hotline for additional info 888 -373 -7888 SANE Nurse 801 -461 -5888 Sexual Assault Crisis Hotline 888 -421 -1100 Assessment of Potential Danger Ask Hotline (888 -373 -7888) to assist in assessing level of danger. Be vigilant of immediate environment Questions to consider: Is the trafficker present? What will happen if the patient does not return to the trafficker? Does the patient believe he/she or a family member is in danger? Is the patient a minor? Document what patient stated in her/his own words and what resources were given to the patient. If you suspect TIP ask: If YES “Are you here today to be treated for injuries caused by another person? ” If YES If you suspect TIP ask questions alone with the patient: “Have you ever been forced to do work when you didn’t want to do? ” “Does anyone hold your identity documents? ” “Has your employer threatened you if you leave? ” “Have you ever exchanged sex for food, shelter, drugs, or money? ” Important Dynamics for Assessment Keep in mind that the victim may not self-identify as a human trafficking victim Victims have been conditioned not to trust others Victims have been conditioned not to tell the truth Speak to the patient alone without accompanying adults (adults may portray themselves as relatives) Prioritize the patient’s medical needs and safety as the primary reason for the assessment If NO Refer to Social Worker as needed Reiterate to patient that your hospital is a resource if needed Give the patient the Human Trafficking Hotline Number if safe to do so (888 -373 -7888; 801 -200 -3443)

CHILD ABUSE AND NEGLECT
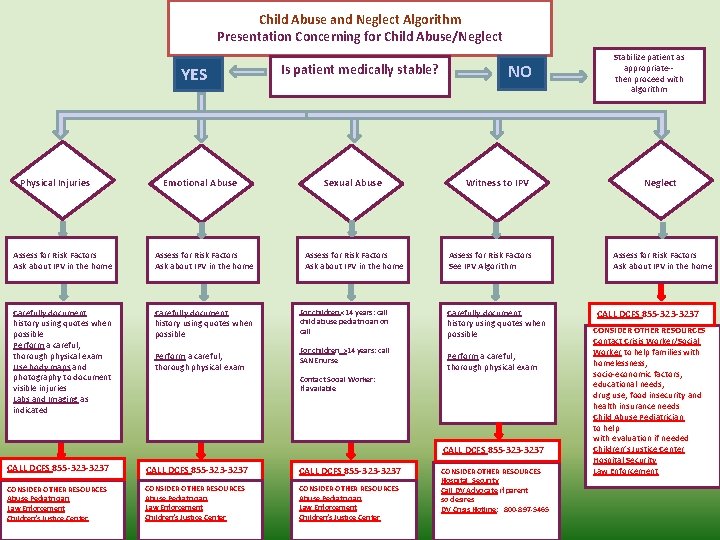
Child Abuse and Neglect Algorithm Presentation Concerning for Child Abuse/Neglect YES Physical Injuries Emotional Abuse Assess for Risk Factors Ask about IPV in the home Carefully document history using quotes when possible Perform a careful, thorough physical exam Use body maps and photography to document visible injuries Labs and Imaging as indicated Carefully document history using quotes when possible Perform a careful, thorough physical exam Is patient medically stable? Sexual Abuse Assess for Risk Factors Ask about IPV in the home For children <14 years: call child abuse pediatrician on call For children >14 years: call SANE nurse NO Witness to IPV Assess for Risk Factors See IPV Algorithm Carefully document history using quotes when possible Perform a careful, thorough physical exam Contact Social Worker: If available CALL DCFS 855 -323 -3237 CONSIDER OTHER RESOURCES Abuse Pediatrician Law Enforcement Children’s Justice Center CONSIDER OTHER RESOURCES Hospital Security Call DV Advocate if parent so desires DV Crisis Hotline: 800 -897 -5465 Stabilize patient as appropriate-then proceed with algorithm Neglect Assess for Risk Factors Ask about IPV in the home CALL DCFS 855 -3237 CONSIDER OTHER RESOURCES Contact Crisis Worker/Social Worker to help families with homelessness, socio-economic factors, educational needs, drug use, food insecurity and health insurance needs Child Abuse Pediatrician to help with evaluation if needed Children’s Justice Center Hospital Security Law Enforcement

Reminders • Activate your policy by – Making it a useful document – Making it relevant

Objectives • Explain why violence is a health care issue • Describe the process in preparing your health care setting to screen for violence, abuse and exploitation If you don’t ask—they won’t tell health care setting

Objectives • Explain why violence is a health care issue • Describe the process in preparing your health care setting to screen for violence, abuse and exploitation • Integrate trauma-informed care throughout your health care setting

Trauma-informed Care • Realization that many patients seeking behavior services and many other public health services have a history of physical and sexual abuse and other forms of trauma • Trauma-informed care approach to patients provides a more therapeutic interaction and avoids re-traumatization • “What is wrong with you? ” • “What has happened to you? ” http: //store. samhsa. gov/shin/content//SMA 14 -4816. pdf

Trauma-informed Care • Realization that many patients seeking behavior services and many other public health services have a history of physical and sexual abuse and other forms of trauma • Trauma-informed care approach to patients provides a more therapeutic interaction and avoids re-traumatization • “What is wrong with you? ” • “What has happened to you? ” http: //store. samhsa. gov/shin/content//SMA 14 -4816. pdf

Trauma-informed Care SAMHSA TIP Series 57, 2014; Harris 2001 • What happened is not nearly as important as what the trauma means to the individual • Screening to identify patients who have histories of trauma and experience trauma-related symptoms is a prevention strategy • With a history of trauma so common it has been suggested that we should use ‘universal precautions’ when interacting with patients

10 Principles of TIC Trauma-informed services 1 2 3 4 5 6 7 8 9 10 Recognize the impact of violence and victimization on development and coping strategies Identify recovery from trauma as the primary goal Employ an empowerment model Strive to maximize a patient’s choices and control over her recovery Are based in a relational collaboration Create an atmosphere that is respectful of survivors’ need for safety, respect, and acceptance Emphasize patient’s strengths, highlighting adaptations over symptoms and resilience over pathology Goal is to minimize the possibilities of retraumatization Strive to be culturally competent Solicit consumer input and involve patients in designing and evaluating services Elliott 2005

10 Principles of TIC Trauma-informed services 1 2 3 4 5 6 7 8 9 10 Recognize the impact of violence and victimization on development and coping strategies Identify recovery from trauma as the primary goal Employ an empowerment model Strive to maximize a patient’s choices and control over her recovery Are based in a relational collaboration Create an atmosphere that is respectful of survivors’ need for safety, respect, and acceptance Emphasize patient’s strengths, highlighting adaptations over symptoms and resilience over pathology Goal is to minimize the possibilities of retraumatization Strive to be culturally competent Solicit consumer input and involve patients in designing and evaluating services Elliott 2005

10 Principles of TIC Trauma-informed services 1 2 3 4 5 6 7 8 9 10 Recognize the impact of violence and victimization on development and coping strategies Identify recovery from trauma as the primary goal Employ an empowerment model Strive to maximize a patient’s choices and control over her recovery Are based in a relational collaboration Create an atmosphere that is respectful of survivors’ need for safety, respect, and acceptance Emphasize patient’s strengths, highlighting adaptations over symptoms and resilience over pathology Goal is to minimize the possibilities of retraumatization Strive to be culturally competent Solicit consumer input and involve patients in designing and evaluating services Elliott 2005

10 Principles of TIC Trauma-informed services 1 2 3 4 5 6 7 8 9 10 Recognize the impact of violence and victimization on development and coping strategies Identify recovery from trauma as the primary goal Employ an empowerment model Strive to maximize a patient’s choices and control over her recovery Are based in a relational collaboration Create an atmosphere that is respectful of survivors’ need for safety, respect, and acceptance Emphasize patient’s strengths, highlighting adaptations over symptoms and resilience over pathology Goal is to minimize the possibilities of retraumatization Strive to be culturally competent Solicit consumer input and involve patients in designing and evaluating services Elliott 2005

10 Principles of TIC Trauma-informed services 1 2 3 4 5 6 7 8 9 10 Recognize the impact of violence and victimization on development and coping strategies Identify recovery from trauma as the primary goal Employ an empowerment model Strive to maximize a patient’s choices and control over her recovery Are based in a relational collaboration Create an atmosphere that is respectful of survivors’ need for safety, respect, and acceptance Emphasize patient’s strengths, highlighting adaptations over symptoms and resilience over pathology Goal is to minimize the possibilities of retraumatization Strive to be culturally competent Solicit consumer input and involve patients in designing and evaluating services Elliott 2005

Objectives • Explain why violence is a health care issue • Describe the process in preparing your health care setting to screen for violence, abuse and exploitation • Integrate trauma-informed care throughout your health care setting “Trauma-informed care embraces a perspective that highlights adaptation over symptoms and resilience over pathology. ” al. 2005 Elliott et

IN CONCLUSION

In Conclusion • Explain why violence is a health care issue – “One of the essential qualities of the physician is interest in humanity, for the secret of the care of the patent is in caring for the patient. ” Francis Weld Peabody • Describe the process in preparing your health care setting to screen for violence, abuse and exploitation – “I will remember that there is an art to medicine as well as a science, and that warmth, sympathy, and understanding may outweigh the surgeon’s knife or the chemist’s drug. ” Louis Lasagna MD • Integrate trauma-informed care throughout your health care setting – “I wonder how different my life would have been if someone in a white lab jacket had sat down, listened to my story, and seen the health issues lurking in my tomorrows. ” Survivor

Thank you

References • Academy on Violence and Abuse. Consequences of Lifetime Experiences of Violence and Abuse – The COLEVA Project. 2009. Available at www. avahealth. org • American College of Obstetricians and Gynecologists. Committee Opinion. Intimate Partner Violence. February 2012, Number 518. http: //www. acog. org/Resources-And-Publications/Committee. Opinions/Committee-on. Health-Care-for-Underserved-Women/Intimate. Partner-Violence • American Medical Association. Opinion 2. 02 – Physicians’ Obligations in Preventing, Identifying, and Treating Violence and Abuse. Available http: //www. ama-assn. org/ama/pub/physician-resources/medicalethics/code-medical-ethics/opinion 202. page • Centers for Disease Control and Prevention. Intimate Partner Violence Consequences. Available http: //www. cdc. gov/violenceprevention/intimatepartnerviolence/conse quences. html

References • Dahlberg LL, Mercy JA. History of violence as a public health issue. AMA Virtual Mentor, February 2009. Volume 11, No. 2: 167 -172. Available on-line at http: //virtualmentor. amaassn. org/2009/02/mhst 1 -0902. html. 1976 • Elliott, D. E. , Bjelajac, P. , Fallot, R. D. , Markoff, L. S. , & Reed, B. G. (2005). Trauma-informed or trauma-denied: Principles and implementation of trauma-informed services for women. Journal of Community Psychology, 33, 461– 477 • Felitti VJ. Reverse alchemy in childhood: Turning gold into lead. Health Alert. Vol 8 No 1. 2001 • Groves BM. Children Who See Too Much: Lessons from the Child. Boston, MA: Beacon Press; 2002 • Harris, M. , & Fallot, R. D. (Eds. ). (2001). Using trauma theory to design service systems. New Directions for Mental Health Services, 89. San Francisco, CA

References • Hibel LC, et al. Maternal sensitivity buffers the adrenocortical implications of intimate partner violence exposure during early childhood. Develop Psychopath. 2011; 23: 689 -701 • Mc. Ewen BS. Physiology and neurobiology of stress and adaptation: central role of the brain. Physiol Rev 2007; 87: 873– 904. • Mc. Ewen BS, Gianaros PJ. Central role of the brain in stress and adaptation: links to socioeconomic status, health and disease. Ann NY Acad Sci 2010; 1186: 190 -222. • Mc. Donald, R. , Jouriles, E. N. , Ramisetty-Mikler, S. , Caetano, R. , & Green, C. E. (2006). Estimating the number of American children living in partner-violent families. Journal of Family Psychology, 20(1), 137 -142 • Moore, C. G. , Probst, J. C. , Tompkins, M. , Cuffe, S. , & Martin, A. B. (2007). The prevalence of violent disagreements in US families: Effects of residence, race/ethnicity, and parental stress. Pediatrics, 119(S 1), S 68 S 76

References • Moyer VA. Screening for intimate partner violence and abuse of elderly and vulnerable adults: U. S. Preventive Services Task Force Recommendation Statement. Ann Intern Med. 2013; 158: 478 -486 • Plichta SB. Intimate partner and physical health consequences: policy and practice implications. J Interpers Violence 2004; 19: 1296– 323 • Shonkoff JP et al. Technical Report—The lifelong effects of early childhood adversity and toxic stress. Pediatrics. 2012: 129: e 232 -e 246 • Stirling J et al. Understanding the behavioral and emotional consequences of child abuse. Pediatrics. 2008; 122: 667 -673 • Substance Abuse and Mental Health Services Administration. Trauma. Informed Care in Behavioral Health Services. Treatment Improvement Protocol (TIP) Series 57. HHS Publication. No. (SMA) 13 -4801. Rockville, MD: Substance Abuse and Mental Health Services Administration, 2014

References • Thackeray JD et al. Intimate partner violence: The role of the pediatrician. Pediatrics 2010; 125: 1094 -1100 • U. S. Preventive Services Task Force Recommendations on Screening for Intimate Partner Violence and Abuse of Elderly and Vulnerable Adults. Available http: //www. uspreventiveservicestaskforce. org/Page/D ocument/Recommendation. Statment. Final/intimatepartner-violence-and-abuse-of-elderly-and-vulnerableadults screening • Zolotor AJ et al. Intimate partner violence. Obstet Gynecol Clin N Am. 2009; 36: 847 -860
- Slides: 61