Pathophysiology of Stroke Wanda Lovitz APRN Objectives Stroke

Pathophysiology of Stroke Wanda Lovitz, APRN

Objectives: Stroke Describe the risk factors, early identification and treatment associated with acute brain attack. Differentiate the pathologies of ischemic stroke, hemorrhagic stroke, lacunar stroke, and transient ischemic attack. Compare the arrhythmias atrial fibrillation and ventricular fibrillation. Cite the most common causes of hemorrhagic stroke. Describe the clinical manifestations associated with subarachnoid hemorrhage. State the progression of sensory and motor deficits, and speech and language problems that occur as a result of stroke

Stroke (Brain Attack) Definition PAn acute focal neurologic deficit from a vascular disorder that injures brain tissue and results in deficits as well as causing motor & sensory, and language and speech problems PAlso known as a cerebral vascular accident (CVA) or“ brain attack” P About 600 people admitted to UK yearly with stroke, 25% under the age of 55 P 3 rd leading cause of death P #1 cause of nursing home admission

Primary Injury vs Secondary Injury Primary Injury = SUDDEN cessation of blood flow to an area of brain tissue resulting in IRREVERSIBLE ISCHEMIA to some cells Secondary Injury = development of further neurologic damage, may progress over days or weeks TIME IS TISSUE!

Risk Factors Associated with Stroke Age: Increases with age (increases 1%/year between 65 -74) Also can see stroke in infants & children Gender: males > females Race: African-Americans > Caucasians (60% greater risk) Also Asians have increased risk Hx: Heart disease, HTN, smoking, high cholesterol levels, DM

What is a thrombus? Is NORMAL in cases of injury ABNORMAL : a blood clot that forms in a blood vessel may be arterial or venous Pathological thrombus = THROMBOSIS May be caused by fatty deposits that build up in arteries Damage to the endotheilum (often r/t poorly controlled HTN) fosters buildup of fatty deposits and cholesterol Body responds to the vessel wall injury by forming plaque which can rupture and form clots
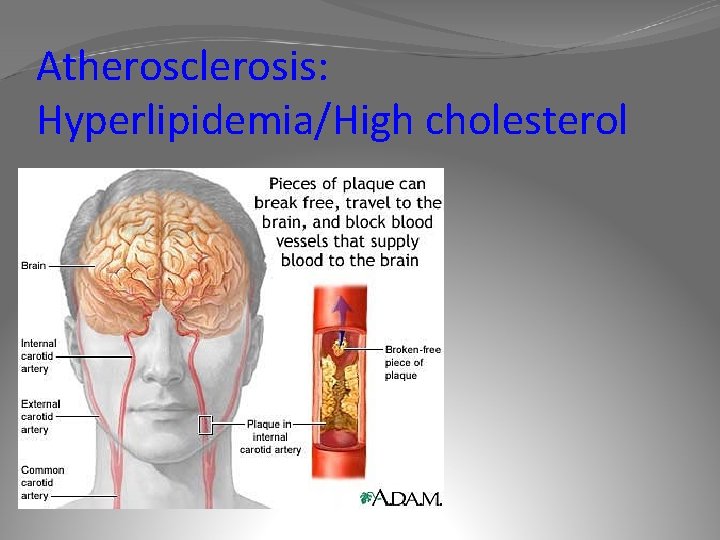
Atherosclerosis: Hyperlipidemia/High cholesterol
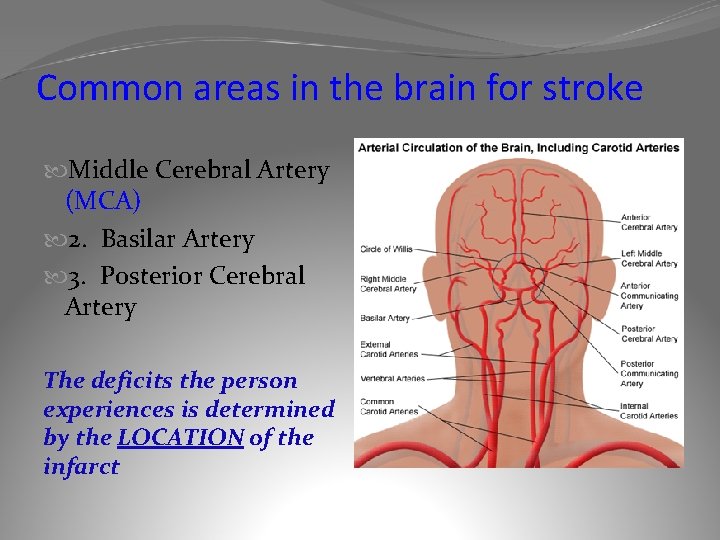
Common areas in the brain for stroke Middle Cerebral Artery (MCA) 2. Basilar Artery 3. Posterior Cerebral Artery The deficits the person experiences is determined by the LOCATION of the infarct
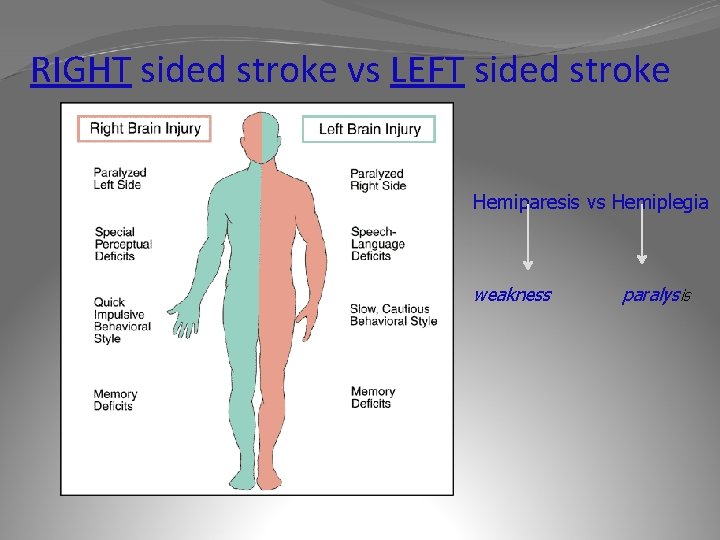
RIGHT sided stroke vs LEFT sided stroke Hemiparesis vs Hemiplegia weakness paralysis
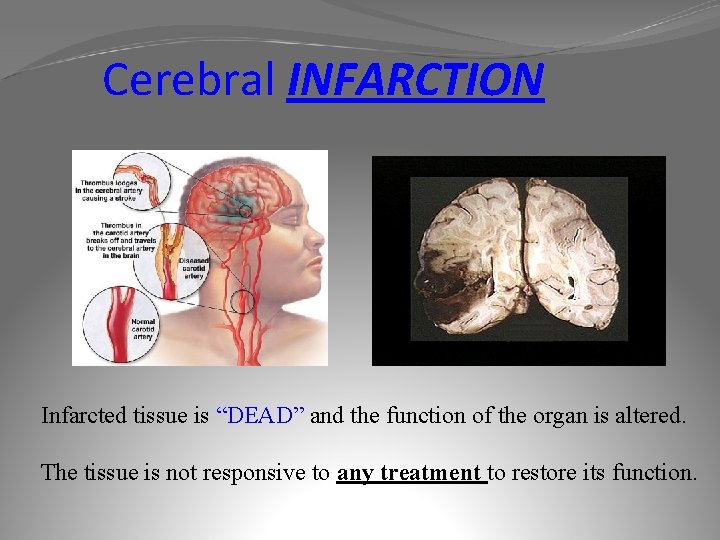
Cerebral INFARCTION Infarcted tissue is “DEAD” and the function of the organ is altered. The tissue is not responsive to any treatment to restore its function.

Cerebral ISCHEMIA Ischemic tissue is POTENTIALLY ‘salvageable’ Current treatment is directed toward restoring blood flow to injured tissue “TIME IS TISSUE” Angiogram showing a blocked cerebral artery
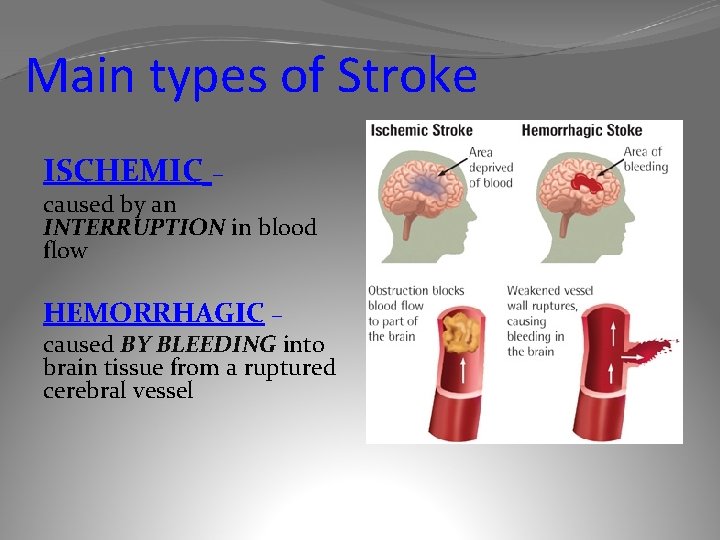
Main types of Stroke ISCHEMIC – caused by an INTERRUPTION in blood flow HEMORRHAGIC – caused BY BLEEDING into brain tissue from a ruptured cerebral vessel

Stroke Categories 1. Ischemic (slow event) (70 -80% of all strokes) Ì Thrombotic Ì Embolic 2. Hemorrhagic (fast, sudden event) Usually occurs as result of rupture of blood vessel from HTN, aneurysm, or head injury

Ischemic Stroke Think Supply and Demand Crisis! ØISCHEMIA – results in greatly reduced or interrupted blood flow in a vessel Ø A THROMBUS OR EMBOLUS is PARTIALLY blocking the blood supply.

Ischemic Penumbra “Bull’s Eye Central core of dead or infarcted tissue Ischemic Penumbra Small blood flow Cells maintain some integrity ? ? Salvageable Thrombolytics Clot busting drugs may be effective during penumbra window TIME IS TISSUE! Coronary (heart) = 6 H Stroke (brain)= 3 H

Ischemic Penumbra 70 -80% of all strokes are ISCHEMIC strokes. And the majority of ischemic strokes are d/t a thrombus. Ischemic zone = greatly reduced blood flow POTENTIAL to salvage tissue

Ischemic Penumbra Cells in the penumbra receive a SMALL amount of blood flow allowing some metabolic function The injured cells undergo ELECTRICAL FAILURE Goal of tx – MINIMIZE damage to penumbra Support cells – – Oxygen – Improved circulation with “clot busting” thrombolytics drugs

What is the Penumbra device? The Penumbra is a recently approved device (2008) that can be used to “vacuum” out the cerebral blood clot A tiny vacuum cleaner for the brain Can be tried up to 8 hours after a stroke strikes or after failure of thrombolytic therapy FDA approved 12/08
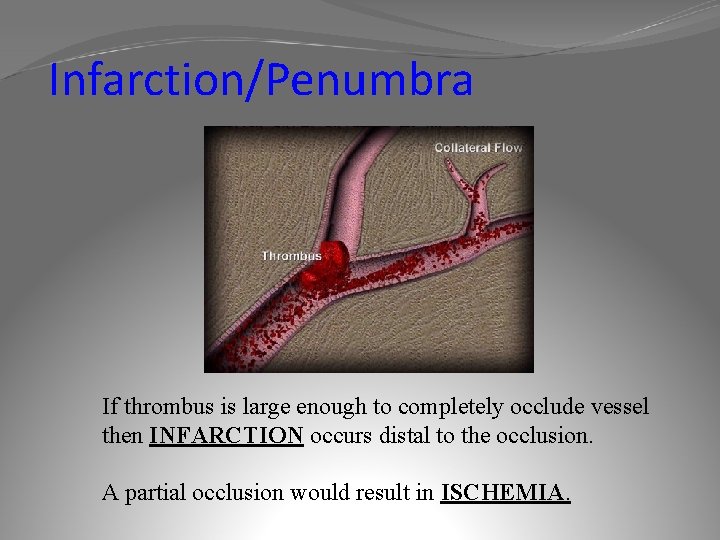
Infarction/Penumbra If thrombus is large enough to completely occlude vessel then INFARCTION occurs distal to the occlusion. A partial occlusion would result in ISCHEMIA.

Alexa Eleanor Ehlers • • • Went to school in Argyle, TX (North Texas) Born in Glenwood Springs, CO (October 2, 1994) & my family lives there again now. I live on and manage my family’s farm, Clear View Equestrian Center, behind Keeneland. I have one dog, three cats, and 5 horses of my own. I have represented the U. S. in international team competitions here in the States four times, winning team gold and bronze, and have represented the U. S. in international team competition once in Australia, winning team bronze. Last, but not least, I’m blessed with an amazing family that loves to travel. • My mom, Stacy; father, Jeff; older sister, Kelsey (25); older brother, Robbie (24)

Types of Ischemic Stroke ÌSmall Vessel (Lacunar) Ìsmall vessels deep in the brain affected ÌLarge Vessel (Thrombotic) Ì r/t hyperlipidemia with unstable plaque ÌCardiogenic (Embolic) ÌClot moves from the heart and lodges in a vessel in the brain

Small Vessel (LACUNAR) Stroke (20% of strokes) KEY CONCEPTS TINY and in DEEP brain structures basal ganglia or pons Cause: occlusion of small branches of cerebral arteries Form small cavities “lacunae” Specific manifestations based on location of injury Generally less deficits Diagnosed: by symptomatology Usually too small to be seen on CT scan
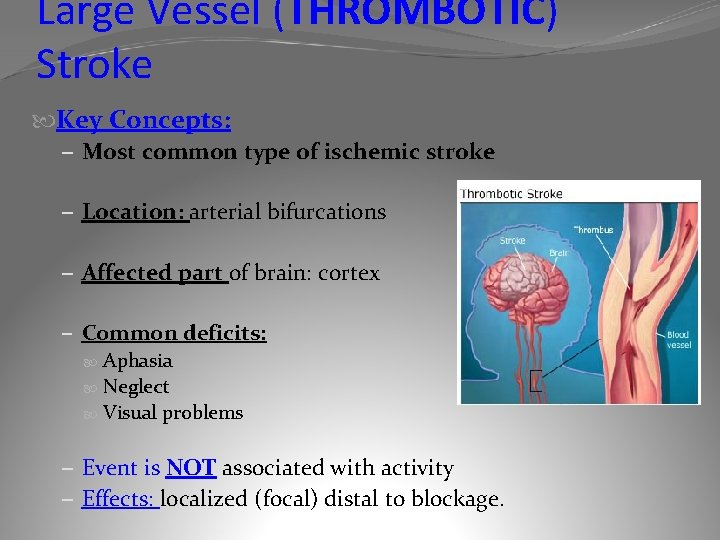
Large Vessel (THROMBOTIC) Stroke Key Concepts: – Most common type of ischemic stroke – Location: arterial bifurcations – Affected part of brain: cortex – Common deficits: Aphasia Neglect Visual problems – Event is NOT associated with activity – Effects: localized (focal) distal to blockage.

Cardiogenic (Embolic) Stroke Key Concepts – Most common location: middle cerebral artery (MCA) – A MOVING blood clot travels from its origin (heart/cardiogenic) to the brain – Usual location Lodge -- larger proximal cerebral vessels often at bifurcations – RAPID onset of symptoms.
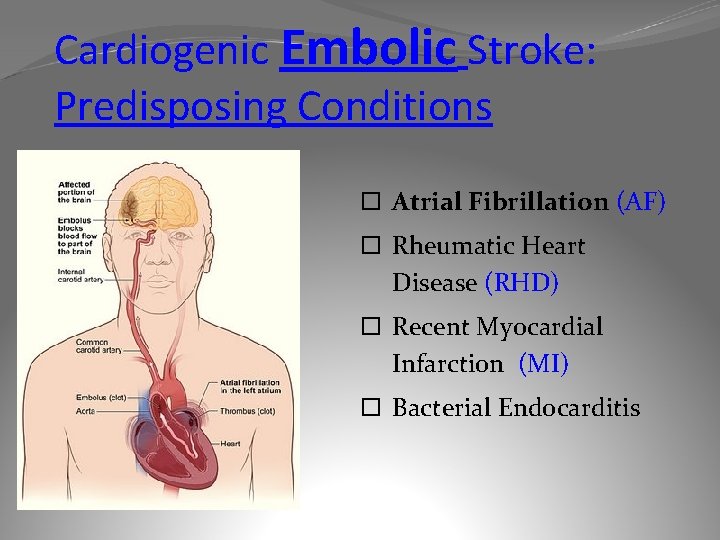
Cardiogenic Embolic Stroke: Predisposing Conditions Atrial Fibrillation (AF) Rheumatic Heart Disease (RHD) Recent Myocardial Infarction (MI) Bacterial Endocarditis
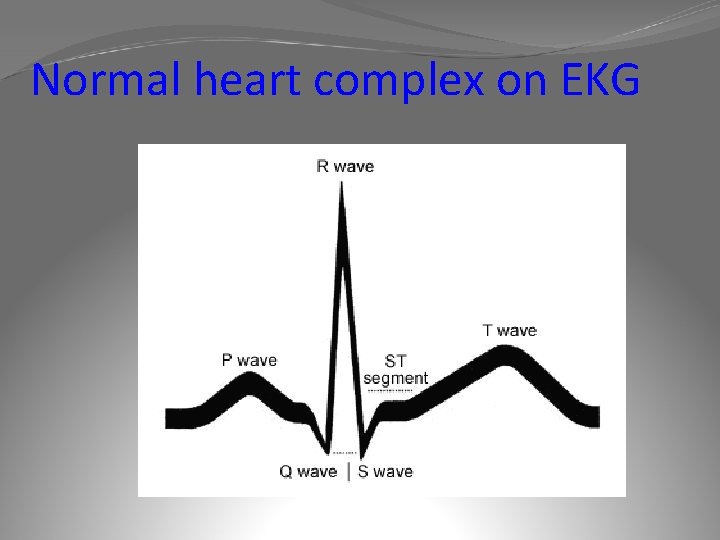
Normal heart complex on EKG
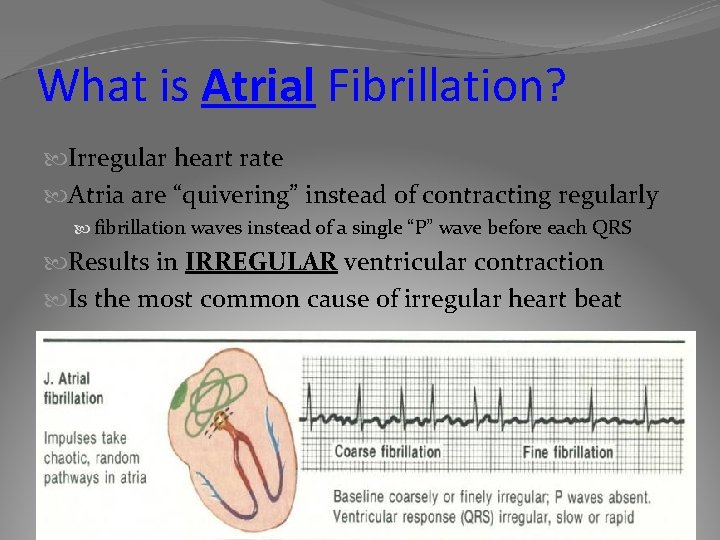
What is Atrial Fibrillation? Irregular heart rate Atria are “quivering” instead of contracting regularly fibrillation waves instead of a single “P” wave before each QRS Results in IRREGULAR ventricular contraction Is the most common cause of irregular heart beat
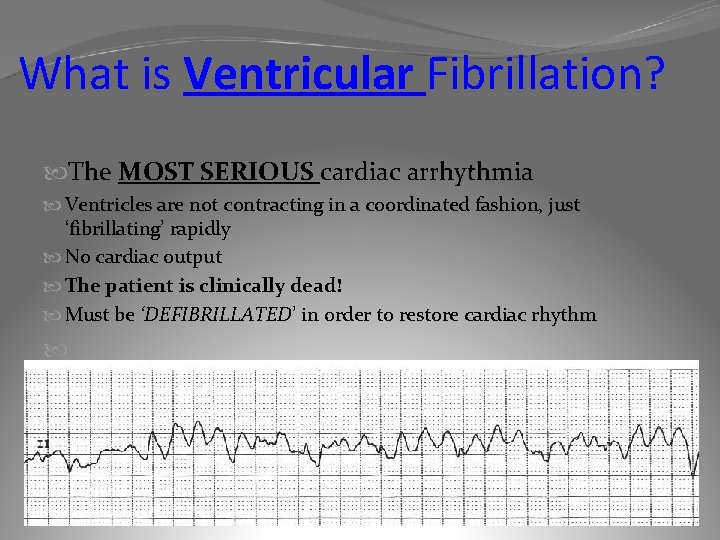
What is Ventricular Fibrillation? The MOST SERIOUS cardiac arrhythmia Ventricles are not contracting in a coordinated fashion, just ‘fibrillating’ rapidly No cardiac output The patient is clinically dead! Must be ‘DEFIBRILLATED’ in order to restore cardiac rhythm
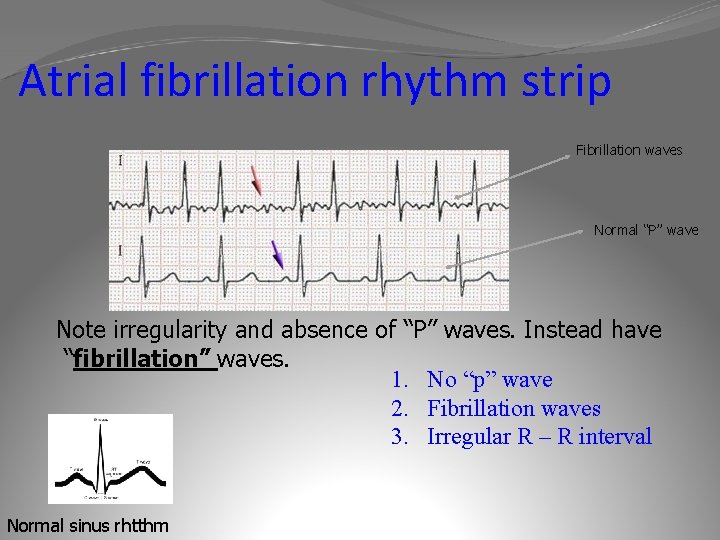
Atrial fibrillation rhythm strip Fibrillation waves Normal “P” wave Note irregularity and absence of “P” waves. Instead have “fibrillation” waves. 1. No “p” wave 2. Fibrillation waves 3. Irregular R – R interval Normal sinus rhtthm
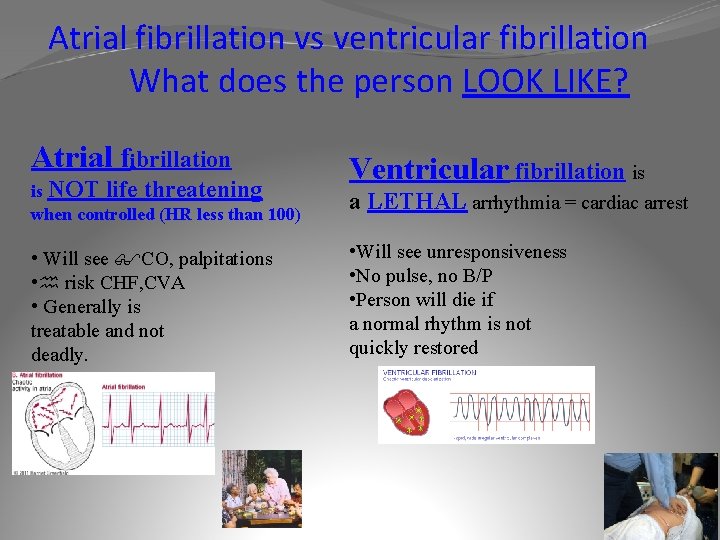
Atrial fibrillation vs ventricular fibrillation What does the person LOOK LIKE? Atrial fibrillation is NOT life threatening when controlled (HR less than 100) • Will see CO, palpitations • risk CHF, CVA • Generally is treatable and not deadly. Ventricular fibrillation is a LETHAL arrhythmia = cardiac arrest • Will see unresponsiveness • No pulse, no B/P • Person will die if a normal rhythm is not quickly restored

What is a TIA? TRANSIENT ischemic attack ÏKey concepts Ï Focal event, due to ischemia Ï TRANSIENT - Sx relieved by 24 hours post onset! Ï Think of it as “angina of the brain!” ÏA WARNING SIGN OF IMPENDING STROKE Ï Is A TEMPORARY disturbance and IS REVERSIBLE Ï Is a “mini-stroke” Ï Area of penumbra, but no infarcted tissue

What is a Hemorrhagic Stroke? Ï Key Concepts Ï Most common cause of FATAL STROKE, why? Ï Causes cerebral edema Ï Causes compression of brain contents Ï Causes spasm of adjacent blood vessels Ï Usually occurs with ACTIVITY Ï BP and pressure in cerebral vessels
Hemorrhagic Stroke Worst headache of my life!!! Most of the brain is affected here. Would see death or severe brain dysfunction and have a sudden onset
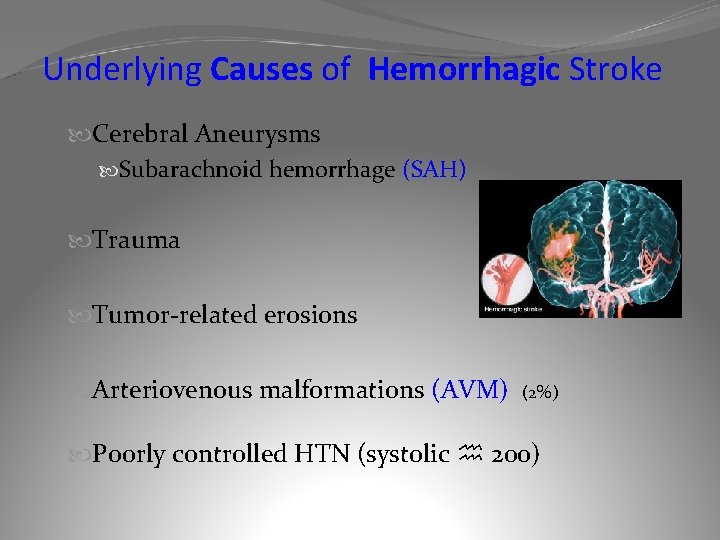
Underlying Causes of Hemorrhagic Stroke Cerebral Aneurysms Subarachnoid hemorrhage (SAH) Trauma Tumor-related erosions Arteriovenous malformations (AVM) (2%) Poorly controlled HTN (systolic 200)
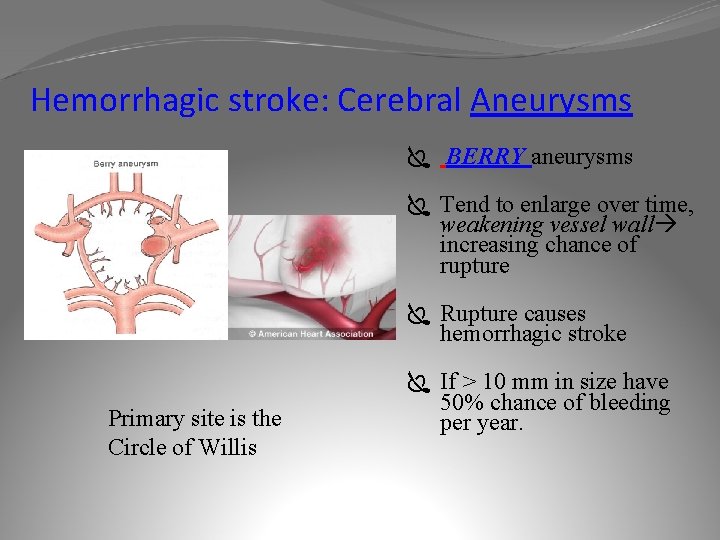
Hemorrhagic stroke: Cerebral Aneurysms Ï BERRY aneurysms Ï Tend to enlarge over time, weakening vessel wall increasing chance of rupture Ï Rupture causes hemorrhagic stroke Primary site is the Circle of Willis Ï If > 10 mm in size have 50% chance of bleeding per year.
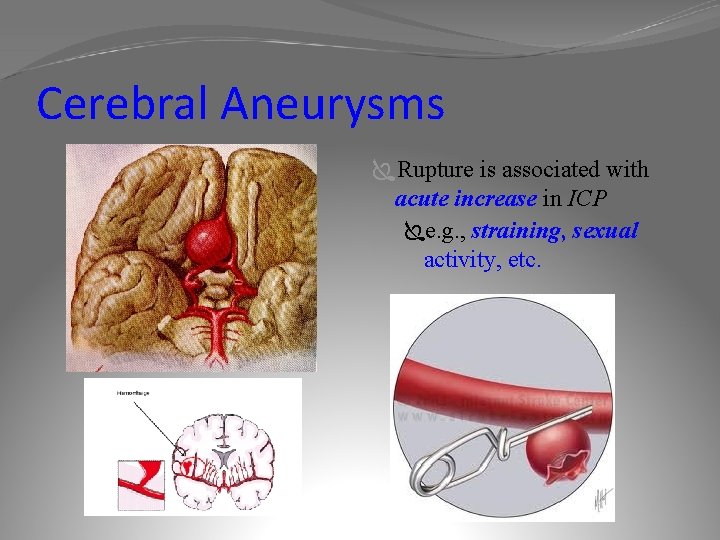
Cerebral Aneurysms ÏRupture is associated with acute increase in ICP Ïe. g. , straining, sexual activity, etc.
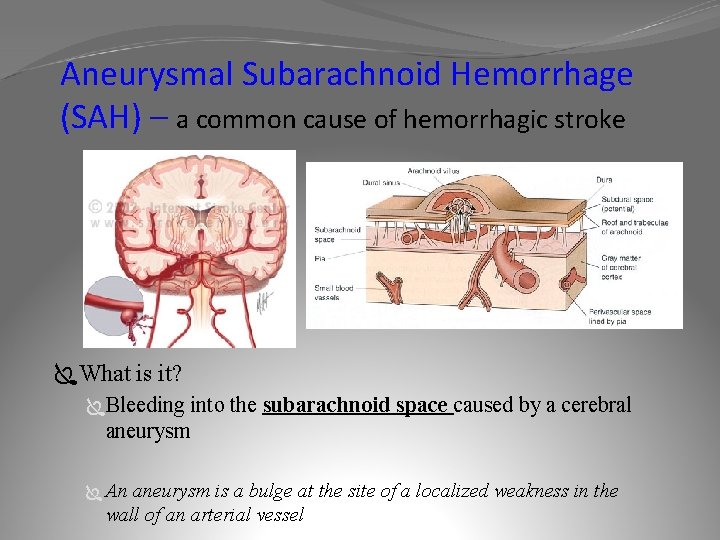
Aneurysmal Subarachnoid Hemorrhage (SAH) – a common cause of hemorrhagic stroke ÏWhat is it? ÏBleeding into the subarachnoid space caused by a cerebral aneurysm Ï An aneurysm is a bulge at the site of a localized weakness in the wall of an arterial vessel
SAH Factoids ÏUsual age: 30 -60 years ÏMortality/morbidity = high ÏAbout 50% die within 3 months Ͻ of survivors have serious disabilities ÏBleeding follows along CSF channels, so SAH extends rapidly over a large area
“Classic” Manifestations of SAH Ï Sudden onset of SEVERE headache Ï “Worse headache ever!” Ï Deteriorating LOC – Rapid Ï Meningeal irritation Ï Nuchal rigidity Ï Photophobia Ï Cranial nerve deficits (CN II & III most often –optic& oculomotor) Ï Visual disturbances, photophobia, cardinal fields of gage affected Ï Increased ICP
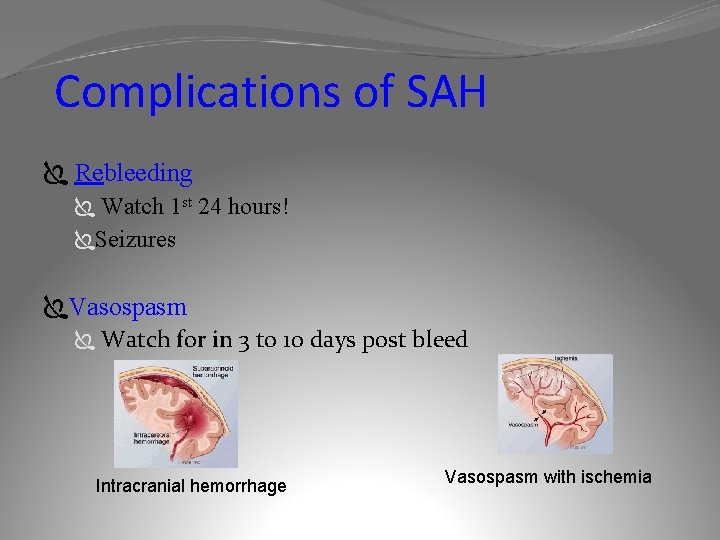
Complications of SAH Ï Rebleeding Ï Watch 1 st 24 hours! ÏSeizures ÏVasospasm Ï Watch for in 3 to 10 days post bleed Intracranial hemorrhage Vasospasm with ischemia
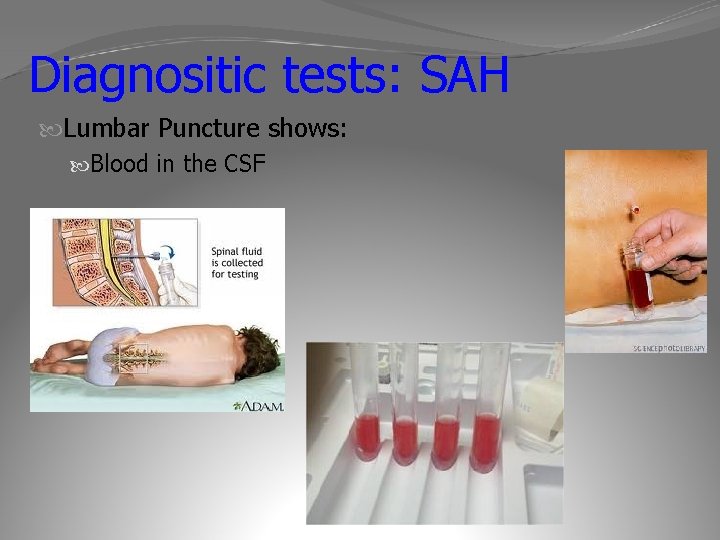
Diagnositic tests: SAH Lumbar Puncture shows: Blood in the CSF
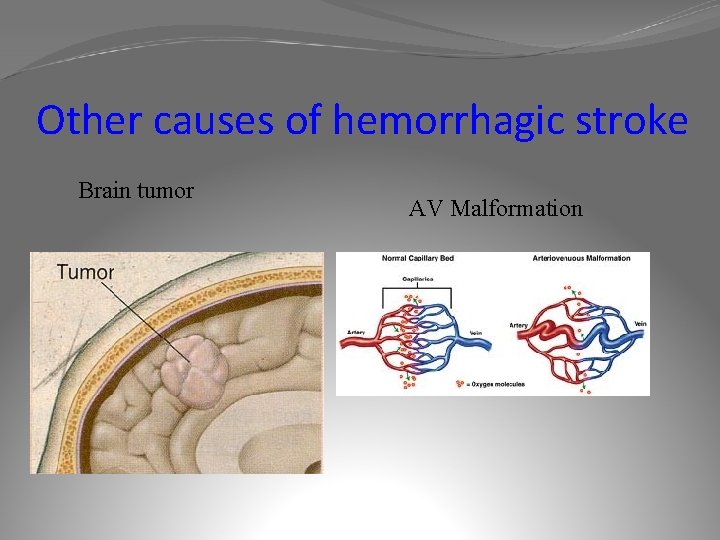
Other causes of hemorrhagic stroke Brain tumor AV Malformation
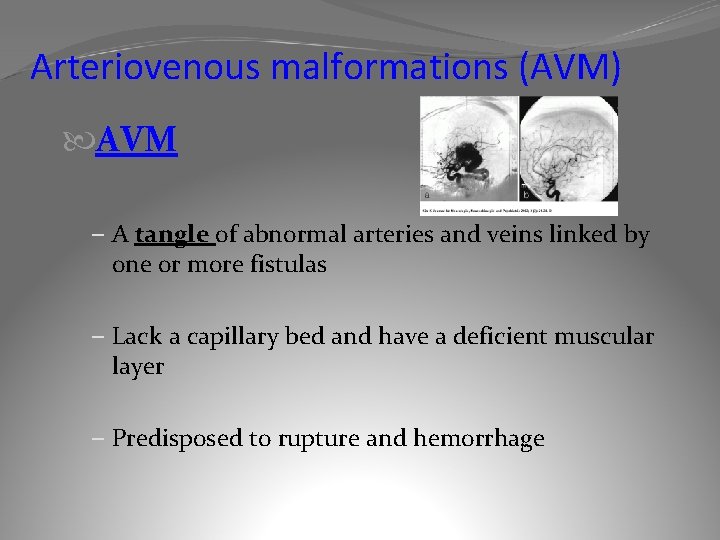
Arteriovenous malformations (AVM) AVM – A tangle of abnormal arteries and veins linked by one or more fistulas – Lack a capillary bed and have a deficient muscular layer – Predisposed to rupture and hemorrhage
You Tube Video ACT “FAST”

Diagnosis of Stroke CT scan Hx, PE Lumbar Puncture Imaging CT Shows hemorrhage or large infarct Does not pick up new ischemic damage MRI Best for new ischemic problems or small infarcts Angiography Locates exact site of abnormality – involves use of contrast dye
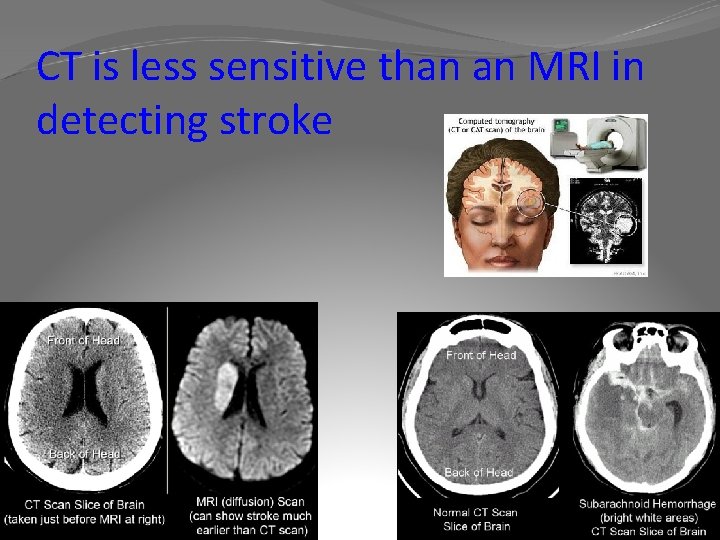
CT is less sensitive than an MRI in detecting stroke

Key Concepts: Clinical Manifestations of Acute Stroke (most common with ischemic) Symptoms depend on affected cerebral artery Symptoms occur: – Relatively rapidly, and are usually focal and unilateral Most common Sx: – Weakness of face, arm & possibly one leg (hemiparesis) = motor deficits – Weakness may be replaced by hyperflexion & spasticity

Courtney Watson

Clinical Manifestations Common with Stroke Watch the You Tube Video “ Effects of Stroke”
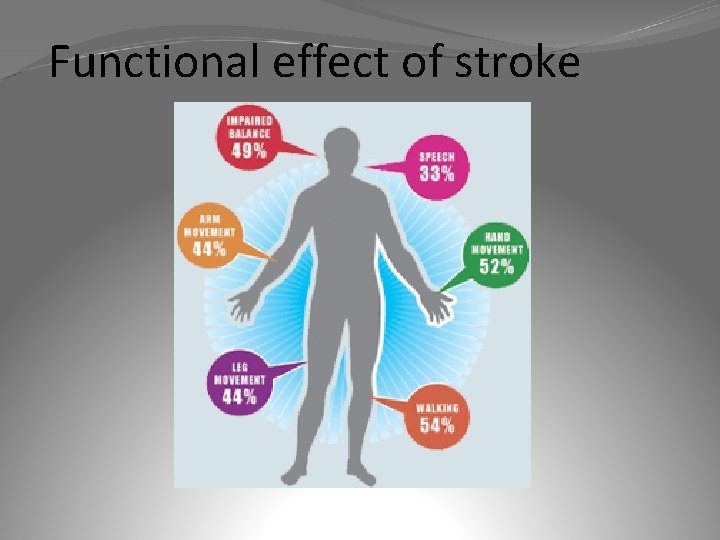
Functional effect of stroke
Stroke Presentation Affected Artery Signs Internal carotid artery Unilateral blindness Contralateral hemiplegia, hemianopia Aphasia with left hemisphere Middle cerebral artery Communication, cognition difficulties Contralateral hemiplegia or hemiparesis Anterior cerebral artery Emotional lability, confusion, amnesia, personality changes Urinary incontinence Posterior cerebral artery Cortical blindness Memory deficts

Effects of Stroke: Movement Issues (motor impairment) Movement Problems Hemiparesis/hemiplegia Mild-profound weakness on CONTRALATERAL side Clumsiness in fine motor skills Facial droop Apraxia (inability to carry out learned activity) Verbal apraxia…. person cannot say words they intend to say Foot drop Outward rotation of leg Initial flaccidity followed by spasticity

Effects of Stroke: PERCEPTION issues Perception Problems – Unilateral neglect (d/t inability to analyze/interpret incoming sensory information – May deny illness or deny one half of body and environment on affected side) – Flat affect – Hemianopsia/visual problems – awareness of one side of the body – Inability to distinguish directional concepts (up/down)
Effects of Stroke: SENSATION issues Sensation Problems – awareness of touch/temperature – proprioception – Balance problems – Vertigo

Effects of Stroke: LANGUAGE problems Language Problems – Aphasia/dysphasia (some degree of inability to speak or to comprehend) – Dysphasia (impairment of speech) – Dysarthria (imperfect speech sounds) – Word finding problems – Incorrect use of verbs or nouns – Expressive aphasia (comprehension intact but cannot express) – Receptive aphasia (can communicate but cannot comprehend what is being said ”can’t receive”

Consequences Aphasia

Effects of Stroke: VISUAL problems Visual disturbances Contralateral field blindness Homonymous Hemianopsia
Effects of Stroke: Movement Issues Flaccidity – contralateral side Spasticity – within 6 weeks

Effects of Stroke: MEMORY and BEHAVIORAL Issues Memory problems – Most memory problems are with remembering names, words, objects Behavioral problems – emotional response – Judgment is usually intact – May underestimate own abilities – Slow reaction times – Hesitant and cautious – May be apathetic, confused, disoriented

FAST……. Recognizing the symptoms of a stroke

Treatment

Be a good nurse…. Know how to recognize a stroke Act FAST…. Know how to assess for stroke 80% of strokes are preventable 500 thousand Americans will have their first stroke this year There is a 4 times greater risk of stroke for women who smoke and take the Pill

The End
- Slides: 63