Pathobiochemistry of liver LIVER STRUCTURE sinusoids central vein

Pathobiochemistry of liver
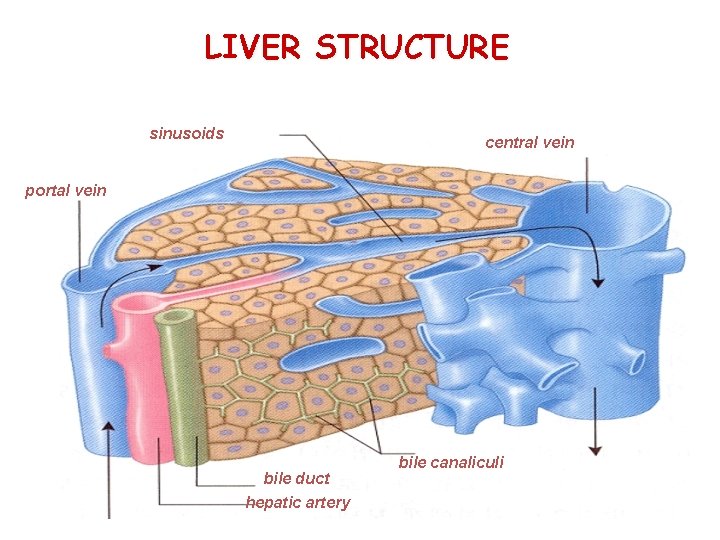
LIVER STRUCTURE sinusoids central vein portal vein bile duct hepatic artery bile canaliculi

LIVER FUNCTIONS • Distribution of nutrients • All types of metabolism (protein, lipid, carbohydrate, vitamin, mineral) • Excretory (bile acids, urea synthesis) • Destruction of toxic substances • Depot of iron, vitamins

METABOLISM OF CARBS IN LIVER § glycolisis § metabolism of fructose and galactose § gluconeogenesis § release of glucose into blood (maintain the stable glucose concentration in blood) § conversion of pyruvate into acetyl Co. A § tricarboxylic acid cycle § pentose phosphate pathway § glycogenolysis, glycogenesis

METABOLISM OF LIPIDS IN LIVER § synthesis of lipoproteins § synthesis of triacylglyserols § synthesis of phospholipids § synthesis of fatty acids, elongation of fatty acids chain, desaturation § synthesis of cholesterol § ketone bodies formation § lipolysis § fatty acids oxidation

METABOLISM OF PROTEINS IN LIVER § protein synthesis, including blood plasma proteins § protein decomposition; urea synthesis § conversion of proteins into carbs and lipids § interconversion of aminoacids § conversion of proteins into low molecular weight nitrogen containing substances

VITAMIN METABOLISM IN LIVER • Formation of active form of vitamin D • Formation of vitamin A from carotins • Depo of cyanocobalamine and folic acid • Depo of vitamin E • Phosphorilation of vitamins B, formation of coenzyme forms

DETOXIFICATION OF TOXIC SUBSTANCES IN LIVER Phase I and phase II. Phase I: Ø hydrolysis, Ø reduction, Ø oxidation. These reactions introduce functional group (—OH, — NH 2, —SH, or —COOH) and usually result in a little increase of hydrophylic properties

Phase II includes: Ø glucuronation, Ø sulfation, Ø acetylation, Ø methylation, Ø conjugation with glutathione, Øconjugation with aminoacids (glycin, taurin, glutamic acid) Phase II results in the marked increase of hydrophylic properties of xenobiotic.
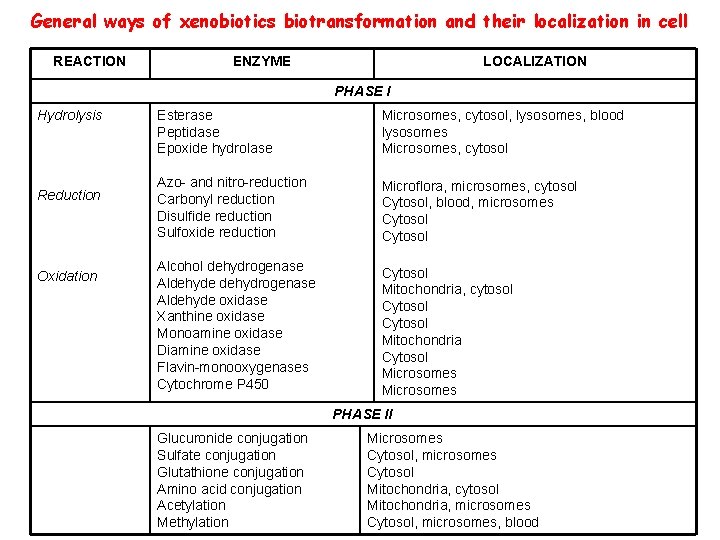
General ways of xenobiotics biotransformation and their localization in cell REACTION ENZYME LOCALIZATION PHASE I Hydrolysis Reduction Oxidation Esterase Peptidase Epoxide hydrolase Microsomes, cytosol, lysosomes, blood lysosomes Microsomes, cytosol Azo- and nitro-reduction Carbonyl reduction Disulfide reduction Sulfoxide reduction Microflora, microsomes, cytosol Cytosol, blood, microsomes Cytosol Alcohol dehydrogenase Aldehyde oxidase Xanthine oxidase Monoamine oxidase Diamine oxidase Flavin-monooxygenases Cytochrome P 450 Cytosol Mitochondria, cytosol Cytosol Mitochondria Cytosol Microsomes PHASE II Glucuronide conjugation Sulfate conjugation Glutathione conjugation Amino acid conjugation Acetylation Methylation Microsomes Cytosol, microsomes Cytosol Mitochondria, cytosol Mitochondria, microsomes Cytosol, microsomes, blood

PHASE I Hydrolysis Esterases (carboxyesterases, cholinesterases, phosphatases) Peptidases Reduction Metals and xenobiotics containing aldehyde, keto, disulfide, alkyn, azo, or nitro group are often reduced Reducing agents: ØReduced glutathione, ØFADH 2, ØFMN, ØNADH ØNADPH.
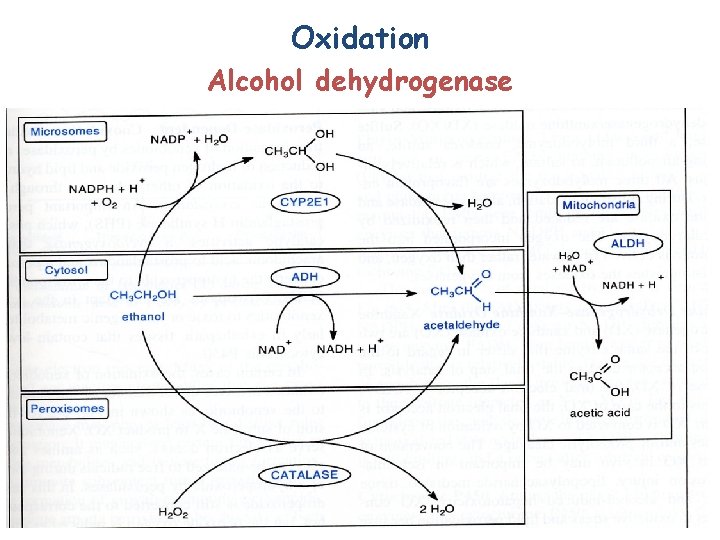
Oxidation Alcohol dehydrogenase

Aldehyde dehydrogenase Oxidizes aldehydes to carbonic acids Xanthine dehydrogenase-Xanthine oxidase Monoaminooxidase Oxidative deamination of amines (serotonin) and many xenobiotics

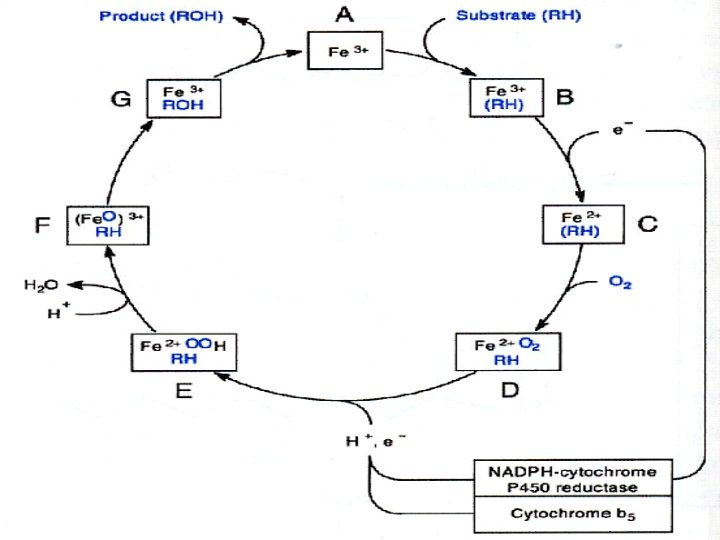
Cytochrom P 450 The highest concentration – in endoplasmic reticulum of hepatocytes (microsomes). Hem containing protein. Catalyzes monooxigenation of oxygen atom into substrate; another oxygen atom is reduced to water Electrons are transferred from NADPH to cytochrome P 450 through flavoprotein NADPH-cytochrome P 450 reductase.
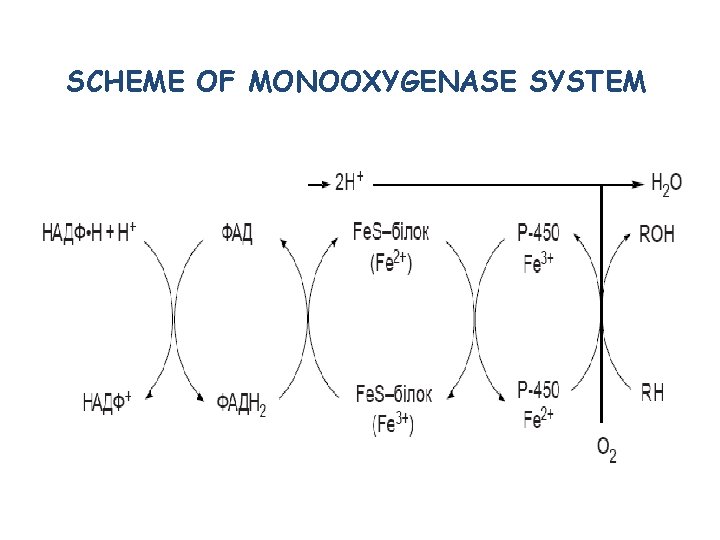
SCHEME OF MONOOXYGENASE SYSTEM
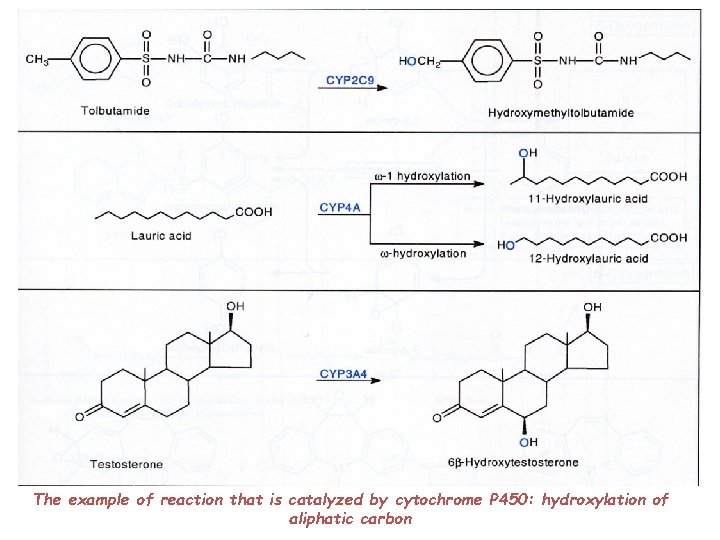
The example of reaction that is catalyzed by cytochrome P 450: hydroxylation of aliphatic carbon
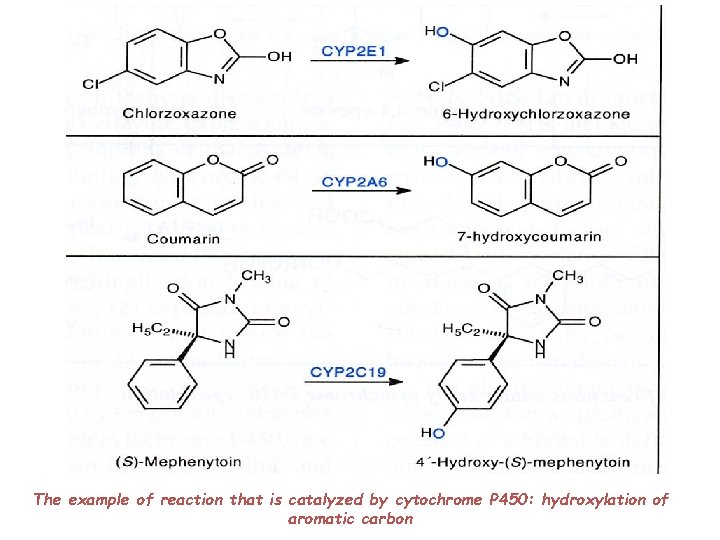
The example of reaction that is catalyzed by cytochrome P 450: hydroxylation of aromatic carbon
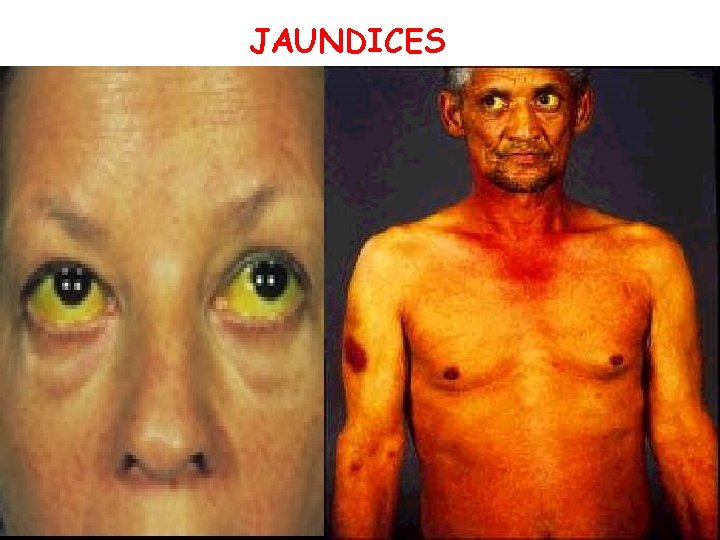
JAUNDICES
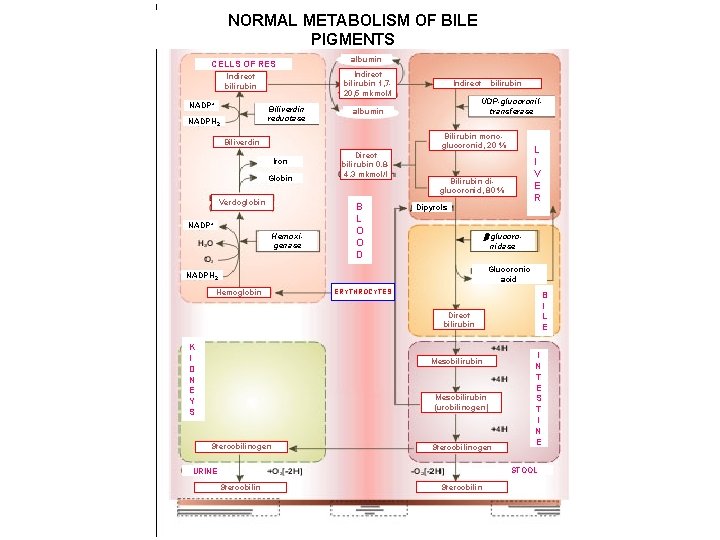
NORMAL METABOLISM OF BILE PIGMENTS CELLS OF RES Indirect bilirubin 1, 720, 5 mkmol/l Indirect bilirubin NADP+ Biliverdin reductase NADPH 2 albumin Indirect bilirubin UDP-glucoroniltransferase albumin Bilirubin monoglucoronid, 20 % Biliverdin Iron Globin Verdoglobin NADP+ Hemoxigenase Direct bilirubin 0. 84. 3 mkmol/l B L O O D L I V E R Bilirubin diglucoronid, 80 % Dipyrols -glucoronidase Glucoronic acid NADPH 2 Hemoglobin ERYTHROCYTES B I L E Direct bilirubin K I D N E Y S Mesobilirubin (urobilinogen) Stercobilinogen I N T E S T I N E STOOL URINE Stercobilin
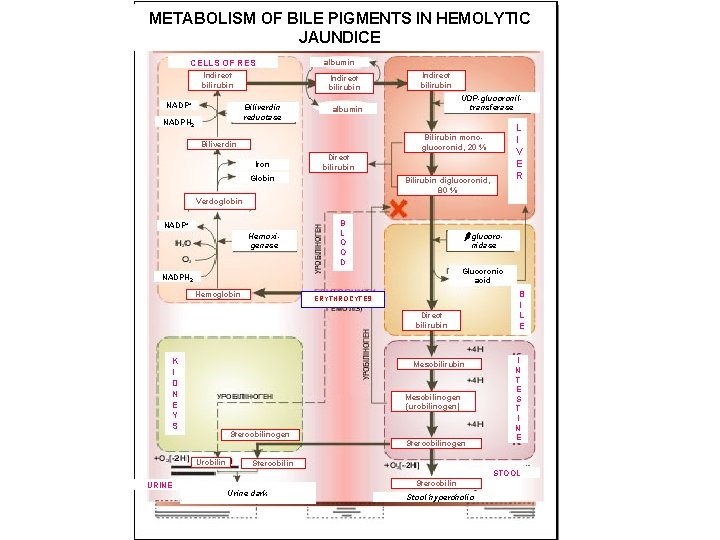
METABOLISM OF BILE PIGMENTS IN HEMOLYTIC JAUNDICE CELLS OF RES Indirect bilirubin NADP+ Indirect bilirubin Biliverdin reductase NADPH 2 albumin Indirect bilirubin UDP-glucoroniltransferase albumin L I V E R Bilirubin monoglucoronid, 20 % Biliverdin Iron Direct bilirubin Globin Bilirubin diglucoronid, 80 % Verdoglobin NADP+ Hemoxigenase B L O O D -glucoronidase Glucoronic acid NADPH 2 Hemoglobin ERYTHROCYTES Direct bilirubin K I D N E Y S Mesobilirubin Mesobilinogen (urobilinogen) Stercobilinogen Urobilin Stercobilinogen B I L E I N T E S T I N E Stercobilin STOOL URINE Stercobilin Urine dark Stool hypercholic
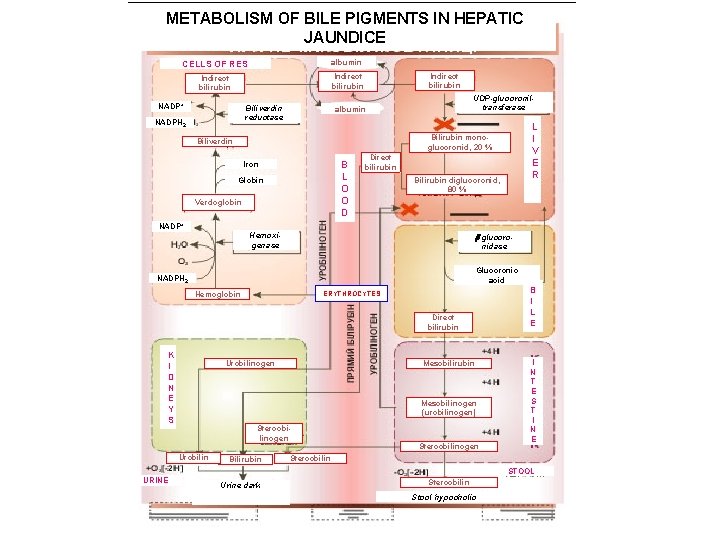
METABOLISM OF BILE PIGMENTS IN HEPATIC JAUNDICE CELLS OF RES albumin Indirect bilirubin NADP+ Biliverdin reductase NADPH 2 Indirect bilirubin UDP-glucoroniltransferase albumin L I V E R Bilirubin monoglucoronid, 20 % Biliverdin B L O O D Iron Globin Verdoglobin Direct bilirubin Bilirubin diglucoronid, 80 % NADP+ Hemoxigenase -glucoronidase Glucoronic acid NADPH 2 ERYTHROCYTES Hemoglobin Direct bilirubin K I D N E Y S Mesobilirubin Urobilinogen Mesobilinogen (urobilinogen) Stercobilinogen Urobilin Bilirubin Stercobilinogen B I L E I N T E S T I N E Stercobilin STOOL URINE Urine dark Stercobilin Stool hypocholic
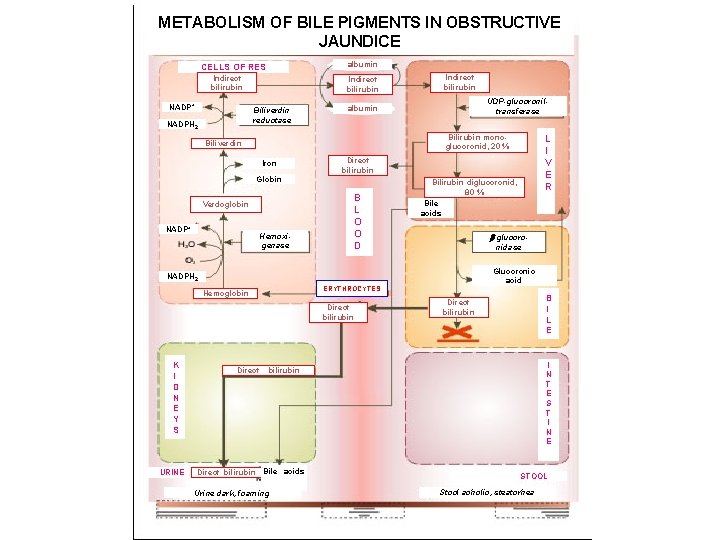
METABOLISM OF BILE PIGMENTS IN OBSTRUCTIVE JAUNDICE albumin CELLS OF RES Indirect bilirubin NADP+ Indirect bilirubin Biliverdin reductase NADPH 2 Indirect bilirubin UDP-glucoroniltransferase albumin Iron Globin Verdoglobin NADP+ Hemoxigenase Direct bilirubin B L O O D Bilirubin diglucoronid, 80 % Bile acids -glucoronidase Glucoronic acid NADPH 2 ERYTHROCYTES Hemoglobin Direct bilirubin K I D N E Y S URINE L I V E R Bilirubin monoglucoronid, 20 % Biliverdin Direct B I L E Direct bilirubin I N T E S T I N E bilirubin Direct bilirubin Bile acids Urine dark, foaming STOOL Stool acholic, steatorhea

Etiology and pathogenesis of liver insufficiency • Infectious agents (hepatitis B virus, tuberculosis bacillus, helmints) • Hepatotropic poison (drugs - tetracycline, sulfonamides, industrial poisons - carbon tetrachloride, arsenic, chloroform, vegetable poisons - aflatoxin, muscarine) • Physical impacts (ionizing radiation) • Biological drugs (vaccines, serums) • Violation of blood circulation (thrombosis, embolism, venous congestion) • Endocrine pathology (diabetes mellitus, hyperthyroidism) • Tumors • Hereditary ensymopathy
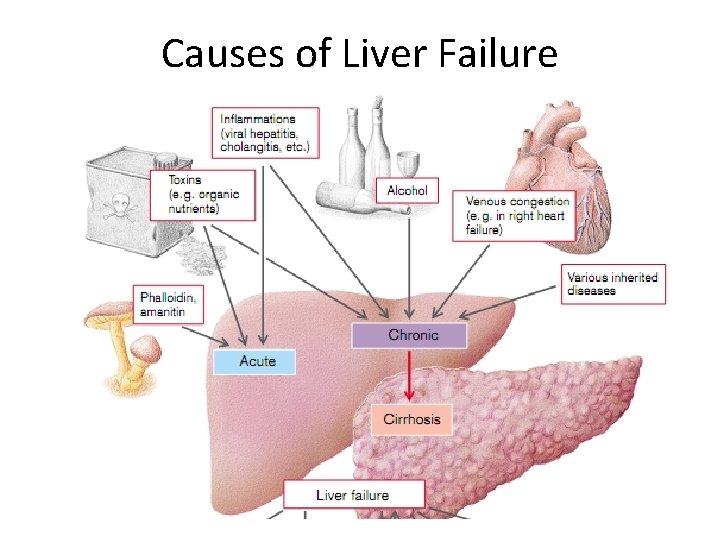
Causes of Liver Failure
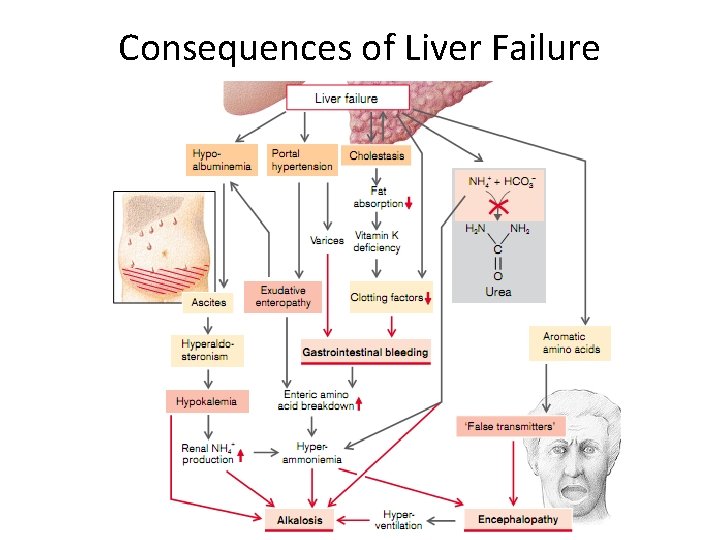
Consequences of Liver Failure
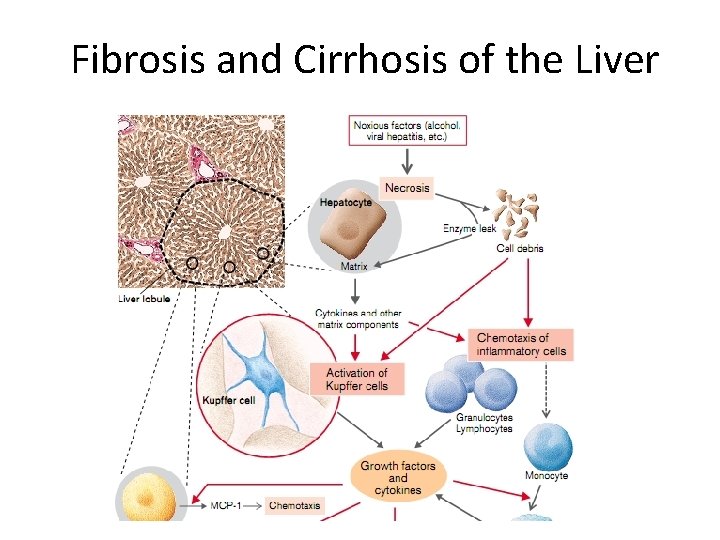
Fibrosis and Cirrhosis of the Liver
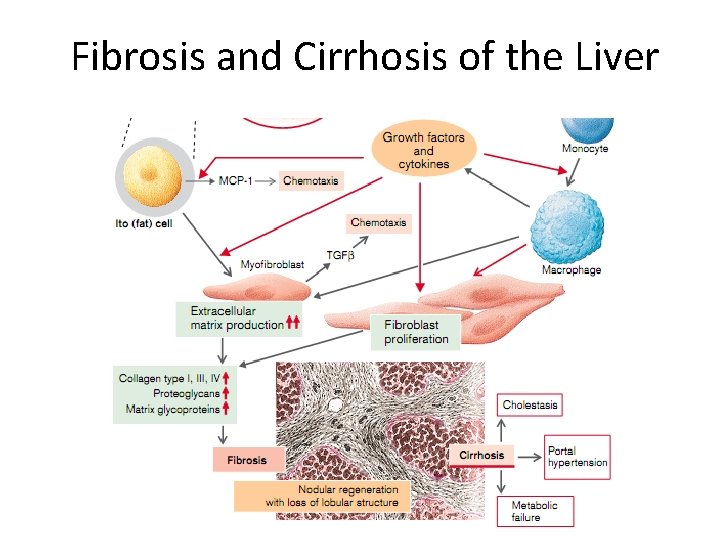
Fibrosis and Cirrhosis of the Liver

Clinical syndromes in liver injury Lack of liver disorders manifested its functions lesion: • metabolic (involved in carbohydrate, fat, protein metabolism, metabolism of vitamins, hormones, biologically active substances) • protection (phagocytic and antitoxic) • digestive and excretory (the formation and release of bile) • hemodynamic (involved in maintaining systemic circulation).
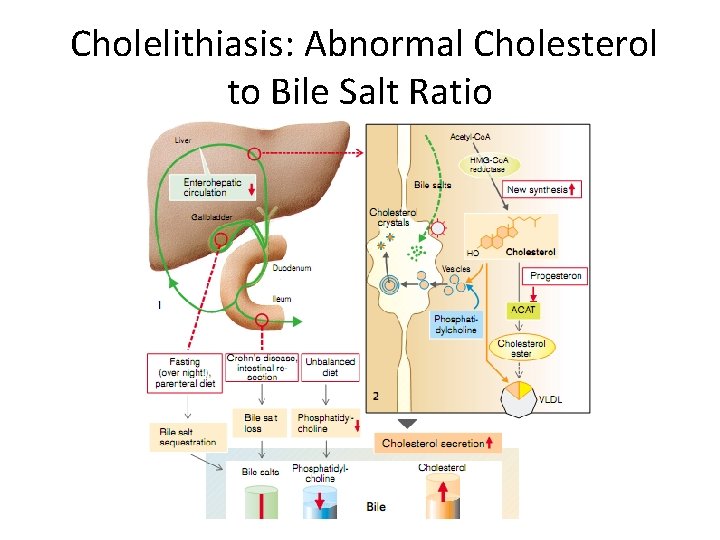
Cholelithiasis: Abnormal Cholesterol to Bile Salt Ratio

Clinical syndromes of jaundice • Acholia associated with non-receipt of bile in the intestine due to violations of the formation and outflow of bile. Acholia manifested disorders of digestion and absorption of fats, hypovitaminosis A, E, K, decreased intake of unsaturated fatty acids of phospholipids to build cell membranes, intestinal motility violation, increasing decay and fermentation. • Dyscholia - violation of the physical-chemical properties of bile, causing it acquires the ability to form stones (due to genetic predisposition, poor nutrition, metabolic disorders, infectious-inflammatory processes, cholestasis).
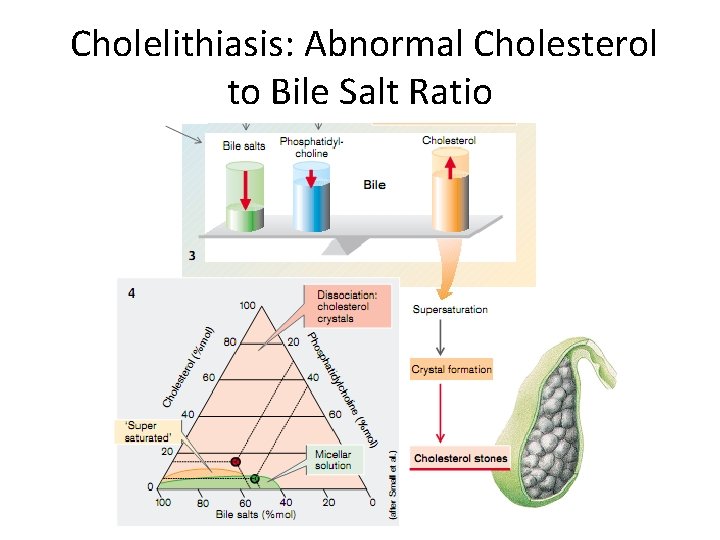
Cholelithiasis: Abnormal Cholesterol to Bile Salt Ratio
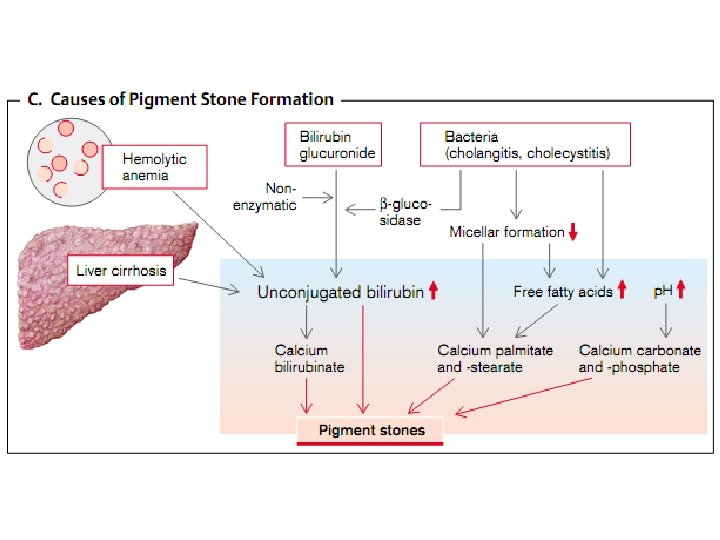
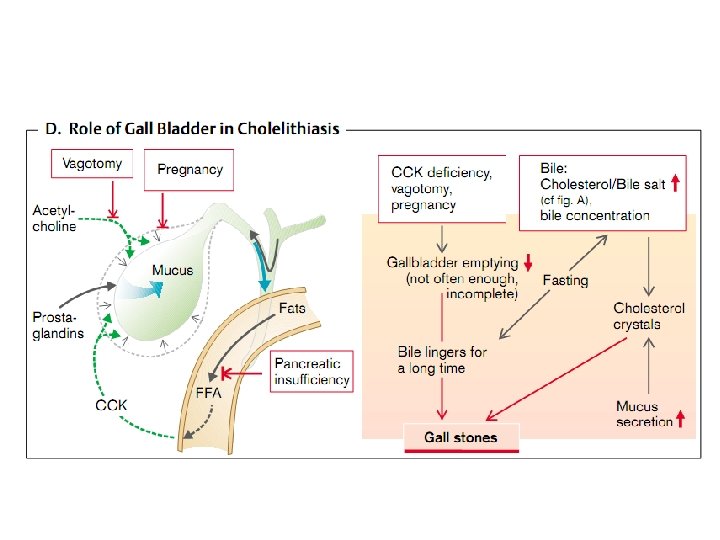
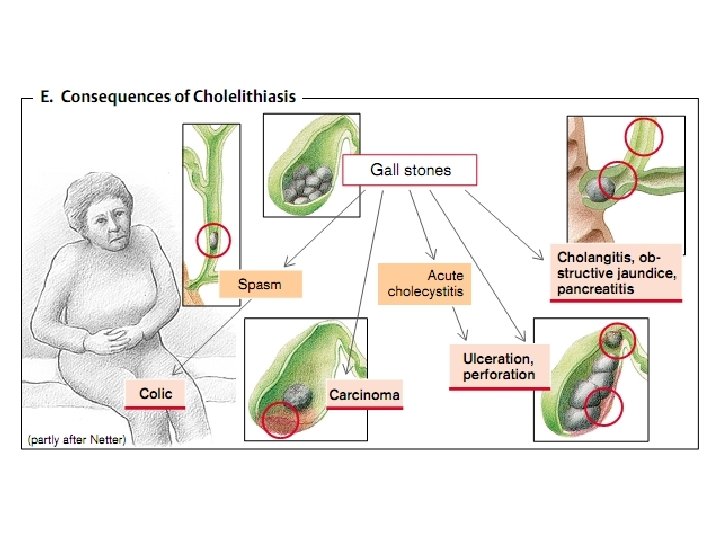
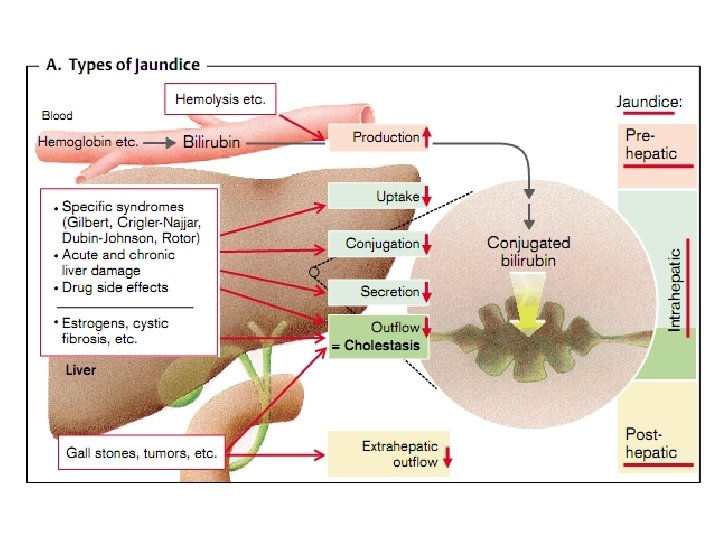

Etiology and pathogenesis of jaundice • Jaundice - a syndrome caused by an increase in blood bilirubin (hemolytic, parenchymal, mechanical). • In hemolytic jaundice due to destruction of a large number of red blood cells accumulate indirect, protein bound bilirubin. • When parenchymal jaundice disturbed capture, and excretion of bilirubin in hepatocytes due to their injuries. • In mechanical jaundice occurs outflow obstruction of bile, compression of biliary tract tumor or scar, closing within a stone, worms, thick bile.
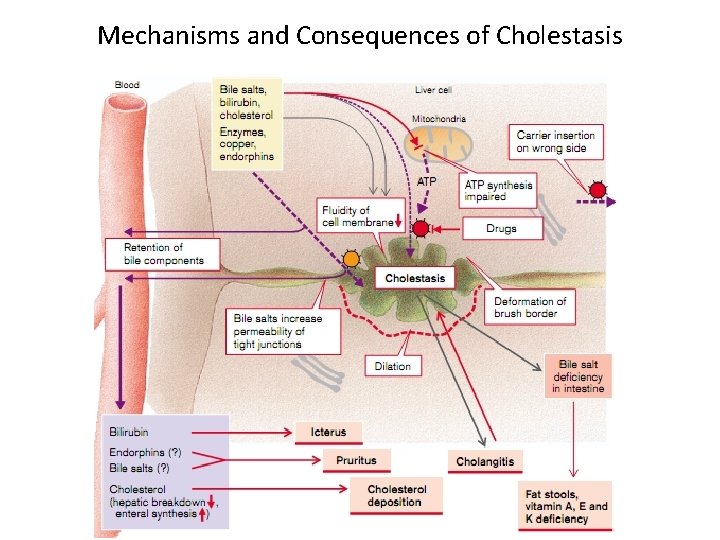
Mechanisms and Consequences of Cholestasis

Methods of experimental study of liver pathology • hepatic-cell failure simulating full or partial removal of the liver, the introduction of poisons (carbon tetrachloride, chloroform, trinitrotoluene); • cholestatic model obtained by squising bile ducts by ligature; • hepatic vascular insufficiency simulating by overlapping portocaval anastomosis, ligation portal vein, hepatic artery.
- Slides: 39