Paroxysmal Nocturnal Hemoglobinuria New ideas about an old

Paroxysmal Nocturnal Hemoglobinuria New ideas about an old disease Ahmad Shihada Silmi Msc, FIBMS Staff Specialist in Hematology Medical Technology Department Islamic University of Gaza

Objectives n Try to answer some of the frequently asked questions about: The cause of the PNH n The clinical presentation of PNH n Diagnosing PNH n The complications of PNH n New treatments for PNH n

What is PNH? n A disorder of blood affecting all the cells which come the bone marrow. n Prevalence 1 -4 per million n The disease is quite rare, only 10, 000 patients in the US and Europe. n There is no ethnic preference for the disorder. n It may present early or late in life. n The manifestations may be “classic” or obscure.

PNH Prognosis n Significant morbidity and mortality n Patients have lived for extended periods of time and have seen spontaneous recovery n Report of 80 patients showed that 60% of deaths due to venous thrombosis or bleeding n Retrospective study of 220 patients n Kaplan-Meier survival 78, 65, and 48% at 5, 10, and 15 years n 8 year rates of major complications of PNH (pancytopenia, thrombosis, MDS) 15, 28, and 5% n Up to 5% of patients can develop acute leukemia; onset about 5 years after Dx of PNH n Likely incident of leukemia lower than 5%

What is PNH Mutation? n n PNH is due to a mutation in a gene in a blood stem cell. The gene is called the PIG-A gene (phosphatidylinositol glycan complementation group A) and is located on the X chromosome. n >100 mutations in PIG - A gene known in PNH n The mutations (mostly deletions or insertions) generally result in stop codons - yielding truncated proteins which may be non or partially functional - explains heterogeneity seen in PNH

What is PNH? n In most cases of PNH, the change in the gene (mutation) is acquired, not something you are born with. When and why is unknown. n The gene contains the genetic information for the GPI anchors which link proteins to the cell membrane

What is PNH? A mutation is a “mistake” or a “change” in the gene that arises during copying and is not corrected n When the cell divides, the mutation is transmitted to daughter cells n The effect of a mutation: n None n An altered protein (sickle hemoglobin) n No protein is produced as in PNH, hemophilia etc n
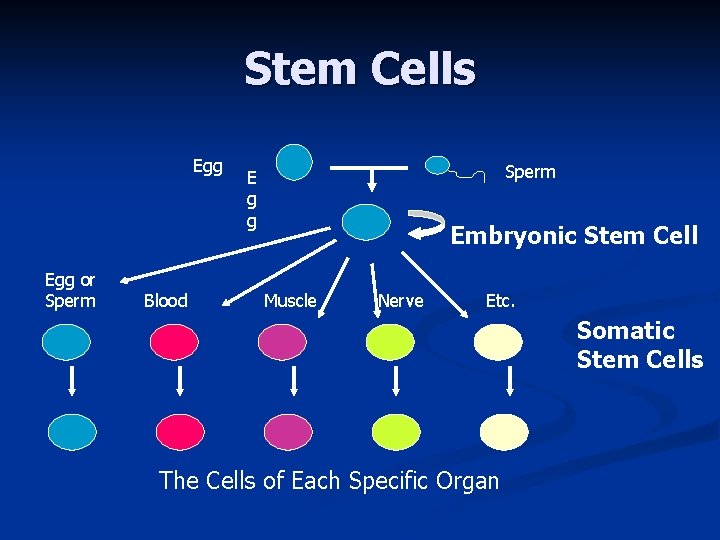
Stem Cells Egg or Sperm Blood Sperm E g g Embryonic Stem Cell Muscle Nerve Etc. Somatic Stem Cells The Cells of Each Specific Organ
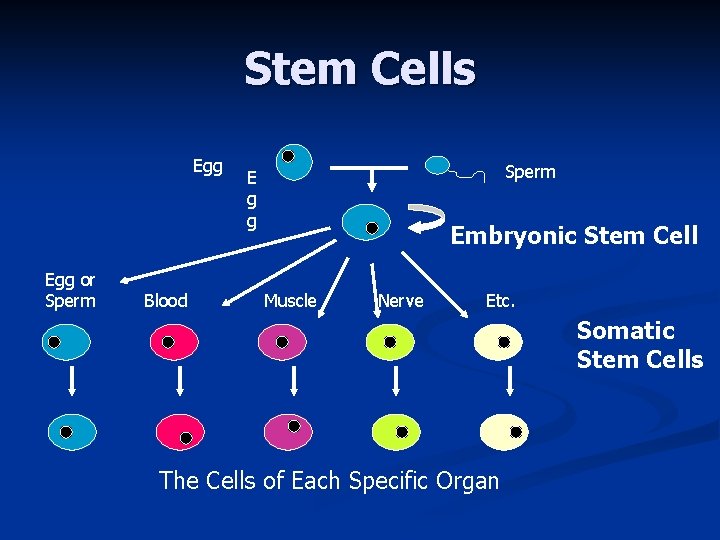
Stem Cells Egg or Sperm Blood Sperm E g g Embryonic Stem Cell Muscle Nerve Etc. Somatic Stem Cells The Cells of Each Specific Organ
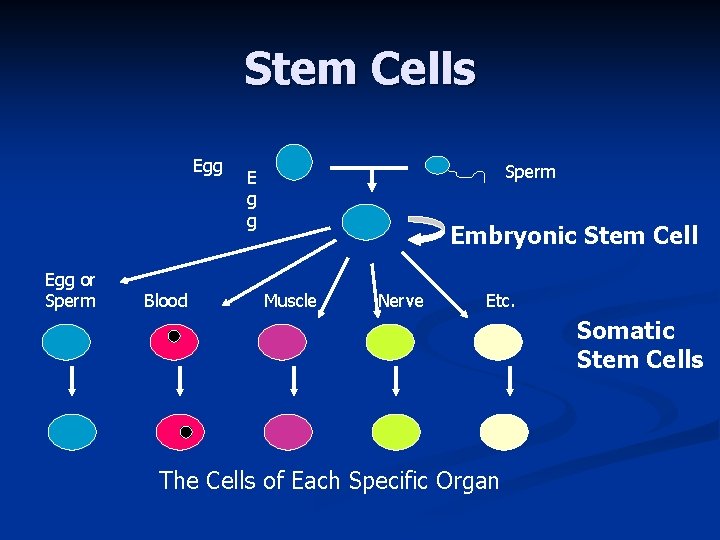
Stem Cells Egg or Sperm Blood Sperm E g g Embryonic Stem Cell Muscle Nerve Etc. Somatic Stem Cells The Cells of Each Specific Organ
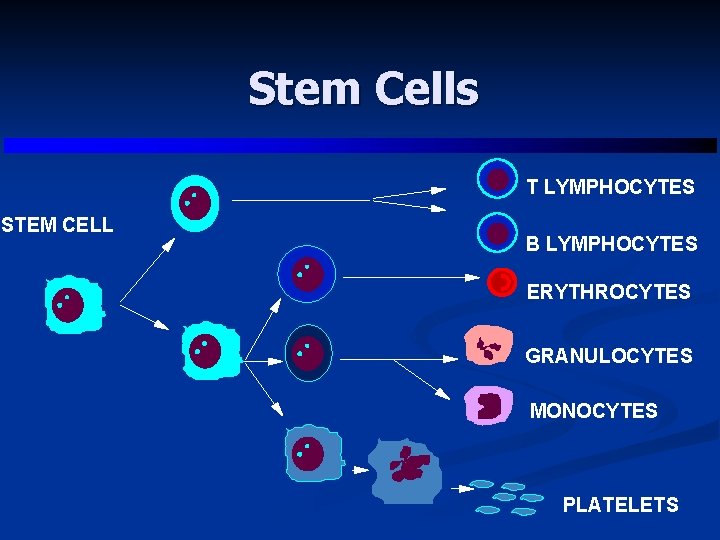
Stem Cells T LYMPHOCYTES STEM CELL B LYMPHOCYTES ERYTHROCYTES GRANULOCYTES MONOCYTES PLATELETS
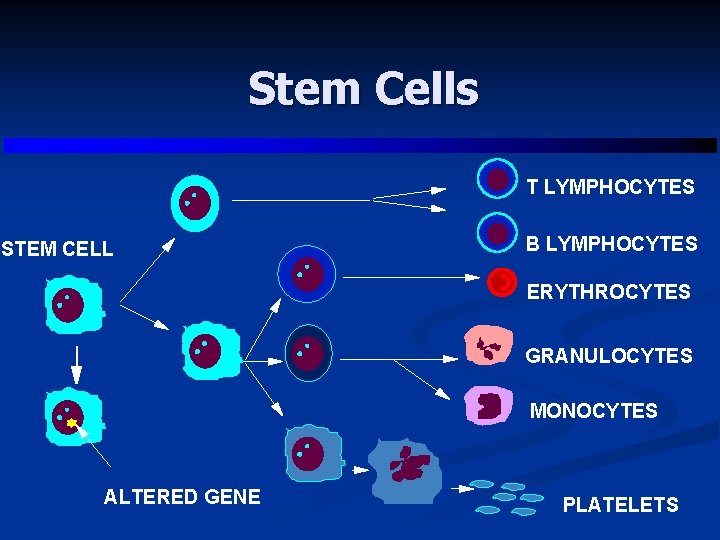
Stem Cells T LYMPHOCYTES STEM CELL B LYMPHOCYTES ERYTHROCYTES GRANULOCYTES MONOCYTES ALTERED GENE PLATELETS
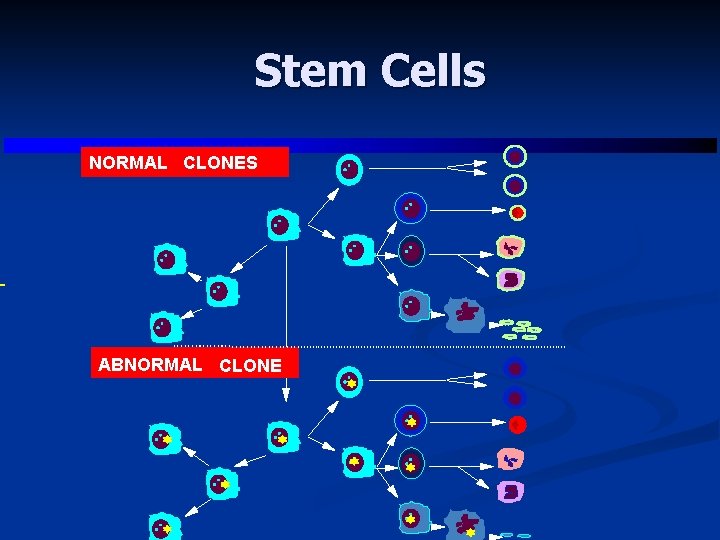
Stem Cells NORMAL CLONES ABNORMAL CLONE
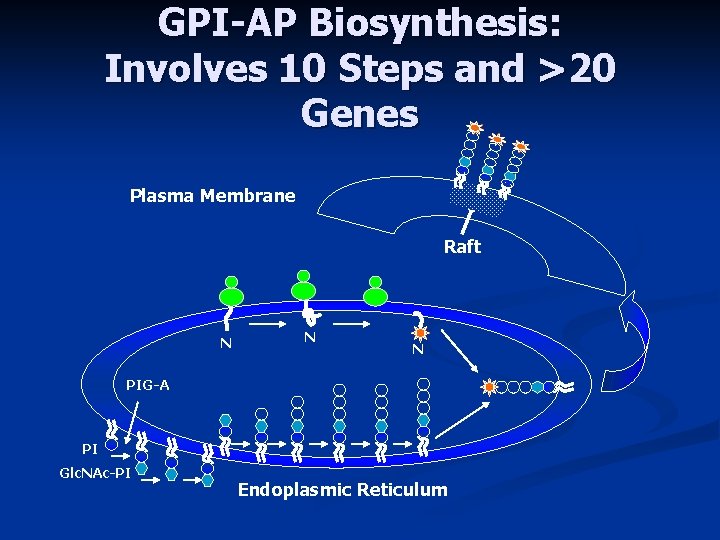
GPI-AP Biosynthesis: Involves 10 Steps and >20 Genes Plasma Membrane Raft N N N PIG-A PI Glc. NAc-PI Endoplasmic Reticulum

The Beginning of PNH n The change that occurs in PNH stops the production of an anchor that ties protein molecules to the cell n Sometimes the stop is only partial and PNH II cells occur

The GPI Anchor Defect in PNH PROTEIN Asp NORMAL PNH C=O NH CH 2 O O=P=O O ( 1 -2) ( 1 -6) ( 1 -4) O N O O-P=O O CH 2 NH 2 O O-P-O CH 2 O CH CH O 2 O-P-O O CH C=O 2 O (22: 4, 5) CH O C=O (18: 0, 1) CH (16: 0) (18: 0, 1) (22: 4, 5) 2 O

Pathogenesis - The Defect GPI Anchor n PIG - A gene codes for 60 k. Da protein glycosyltransferase which effects the first step in the synthesis of the glycolipid GPI anchor (glycosylphosphatidylinositol). Results in clones lacking GPI anchor - in turn, attached proteins PIG - A protein

What is PNH? n As a result of the PIG-A mutation, there is little of no GPI anchor produced. PNH II cells- mild reduction n PNH III cells- severely reduced. n When the anchor is reduced, certain proteins can’t attach to the cells. n The most important proteins for PNH are CD 59, CD 55. n

Proteins anchored by GPI Anchor and Surface Proteins Missing on PNH Blood Cells Antigen Enzymes Acetylcholinesterase (Ach. E) Ecto-5'-nucleotidase (CD 73) Neutrophil alkaline phosphatase(NAP) ADP-rybosyl transferase Adhesion molecules Blast-I/CD 48 Lymphocyte functionassociated antigen-3(LFA-3 or CD 58) CD 66 b Complement regulating surface proteins Decay accelerating factor (DAF or CD 55) Homologous restriction factor, Membrance inhibitor of reactive lysis (MIRL or CD 59) Expression Pattern Red blood cells Some B- and T-lymphocytes Neutrophils Some T-lymphs, Neutrophils Lymphocytes All blood cells Neutrophils All blood cells

Surface Proteins Missing on PNH Blood Cells Antigen Receptors Fc- receptor III (Fc Rlll or CD 16) Monocyte differentiation antigen (CD 14) Urokinase-type Plasminogen Activator Receptor (u-PAR, CD 87) Expression Pattern Neutrophils, NK-cells, macrophages, some T-lymphocytes Monocytes, macrophages Monocytes, granulocytes Blood group antigens Comer antigens (DAF) Yt antigens (Ach. E) Holley Gregory antigen John Milton Hagen antigen (JMH) Dombrock reside Red blood cells, lymphocytes Red blood cells Neutrophil antigens NB 1/NB 2 Neutrophils

Surface Proteins Missing on PNH Blood Cells Antigen Other surface proteins of unknown functions CAMPATH-1 antigen (CDw 52) CD 24 p 5 O-80 GP 500 GPI 75 Expression Pattern Lymphocytes, monocytes B-lymphocytes, Neutrophils, eosinophils Neutrophils Platelets

Pathogenesis CD 55 n Also known as decay accelerating factor n Accelerates decay of enzyme that destroys red cell membranes n CD 55 inhibits the formation or destabilizes complement C 3 convertase (C 4 b. C 2 a) n When GPI anchor absent, CD 55 not available and RBC membranes hemolyze

Pathogenesis CD 59 n Also known as membrane inhibitor of reactive lysis, protectin, homologous restriction factor, and membrane attack complex inhibitory factor n CD 59 Protects the membrane from attack by the C 5 -C 9 complex n Absence or reduction of CD 59 leads to increased hemolysis and perhaps thrombosis

Pathogenesis of CD 55 & CD 59 n Inherited absences of both proteins in humans have been described n Most inherited deficiencies of CD 55 - no distinct clinical hemolytic syndrome n Inherited absence of CD 59 - produces a clinical disease similar to PNH with hemolysis and recurrent thrombotic events

Pathogenesis n Many normal people have very small numbers (perhaps 6 per 1, 000 bone marrow cells) n In PNH, the abnormal cells have an advantage and become a major population in the marrow and blood (anywhere from 1% to over 90%) n This may be a result of change in the immune system –inability to recognize something foreign. n Or it may be related to aplastic anemia, a disease of poor production of blood from the marrow. WHY?

Pathogenesis - Clonal evolution and cellular selection n Expansion of abnormal hematopoietic stem cell required for PNH disease expression n Theories for expansion n n Blood cells lacking GPI-linked proteins have intrinsic ability to grow abnormally fast n In vitro growth studies demonstrate that there are no differences in growth between normal progenitors and PNH phenotype progenitors n In vivo - mice deficient for PIG -A gene also demonstrates no growth advantage to repopulation of BM. Additional environmental factors exert selective pressure in favor of expansion of GPI anchor deficient blood cells n Close association with AA - PNH hematopoitic cells may be more resistant to the Immune System than normal hematopoitic cells. n Evidence in AA is that the decrease in hematopoitic cells is due to increased apoptosis via cytotoxic T cells by direct cell contact or cytokines (escape via deficiency in GPI linked protein? ? ? )

PNH Clinical Features Aplastic Anemia n Some PNH patients have aplastic anemia or a history of aplastic anemia n Many PNH patients have evidence of a bone marrow that doesn’t work well or well enough to maintain normal blood counts n Therefore, whatever causes aplastic anemia (immune suppression or dysregulation or damage to the stem cells) may allow PNH to develop

What is PNH? Complement n Complement is a group of blood proteins that act together to help the body get rid of microbiological invaders n One of the ways it does this is by penetrating the membrane (outside surface) of the invading bacteria or viruses. n When this happens to PNH blood cells, the cells are destroyed.

What is PNH? Complement circulates in an inactive form n It is activated spontaneously and by a variety of events It is normally activated more at night n It is more active with infections, trauma, vaccinations, surgery, immune complexes, autoimmune diseases n

What is PNH? Complement n n Complement activity is regulated by proteins in the blood and on the membranes of the cell. Proteins on the cell surface interfere with complement to prevent breakdown (lysis) of the cell membrane The most important of these is CD 59, which is missing on the abnormal cells of PNH n For this reason, PNH red cells are extremely sensitive to very small amounts of activated complement n
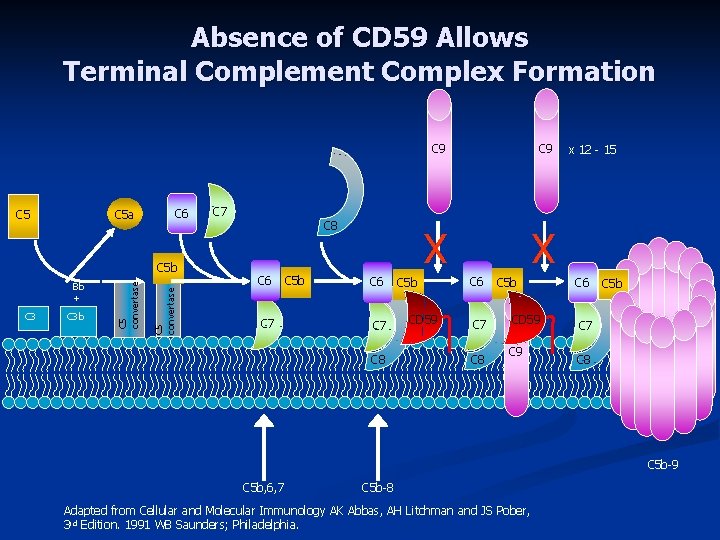
Absence of CD 59 Allows Terminal Complement Complex Formation C 5 a C 5 C 6 C 3 b C 5 convertase Bb + C 5 convertase C 5 b C 7 C 8 C 6 C 7 C 5 b C 6 C 7 C 8 C 9 X X C 5 b CD 59 C 6 C 7 C 8 C 5 b CD 59 C 9 x 12 - 15 C 6 C 5 b C 7 C 8 C 5 b-9 C 5 b, 6, 7 C 5 b-8 Adapted from Cellular and Molecular Immunology AK Abbas, AH Litchman and JS Pober, 3 rd Edition. 1991 WB Saunders; Philadelphia.
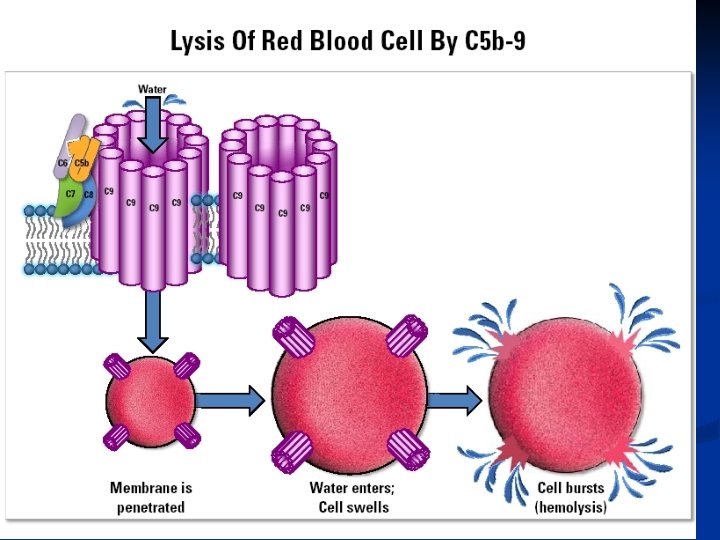

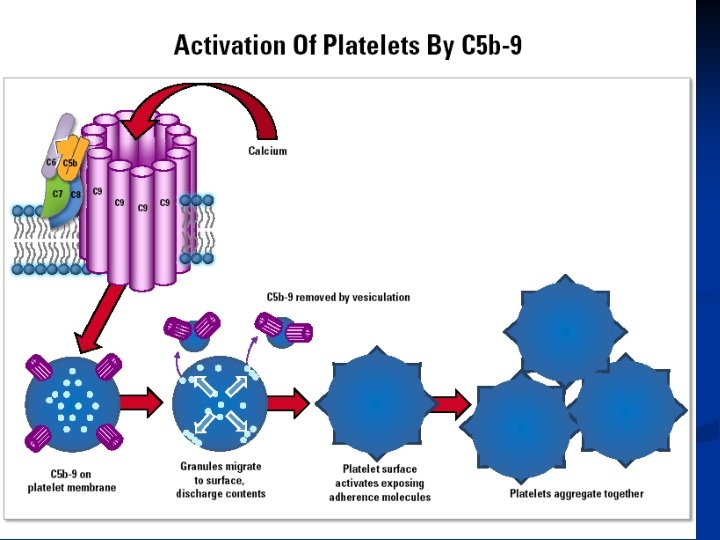
What is PNH? n Complement successfully attacks the red cells and they break up (hemolysis) This releases hemoglobin (the red pigment in red cells) into the plasma n Causes anemia n Pieces of the membrane come off. n The white cells release granule contents and change to express other proteins. n The platelets form vesicles (membrane blisters) and activate. n
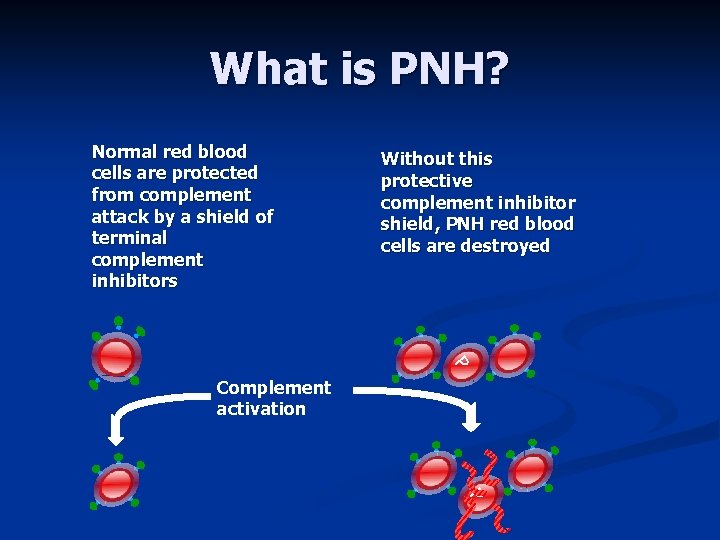
What is PNH? Normal red blood cells are protected from complement attack by a shield of terminal complement inhibitors Without this protective complement inhibitor shield, PNH red blood cells are destroyed P Complement activation P

What is PNH? Clinical Features n n n Some of the hemoglobin passes through the kidneys and into the urine, causing red to dark brown urine (hemoglobinuria) n This causes a loss of iron from the body n In the long run, this may damage the kidney Free hemoglobin binds nitric oxide causing vascular and smooth muscle spasm Causes inflammation
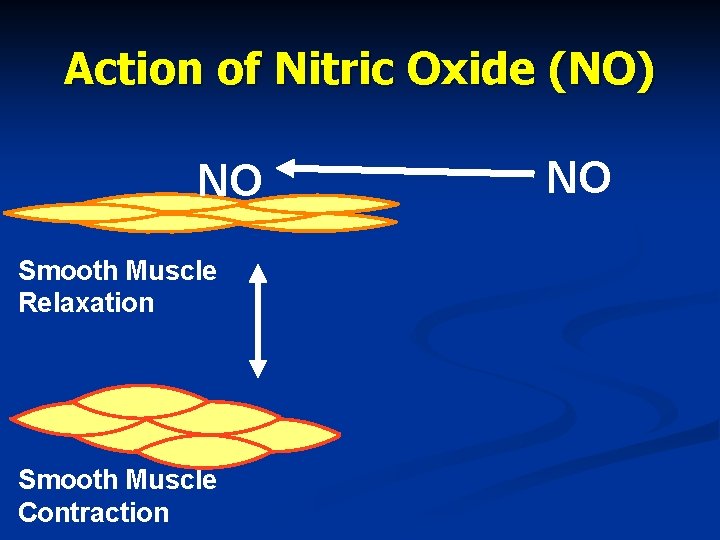
Action of Nitric Oxide (NO) NO Smooth Muscle Relaxation Smooth Muscle Contraction NO
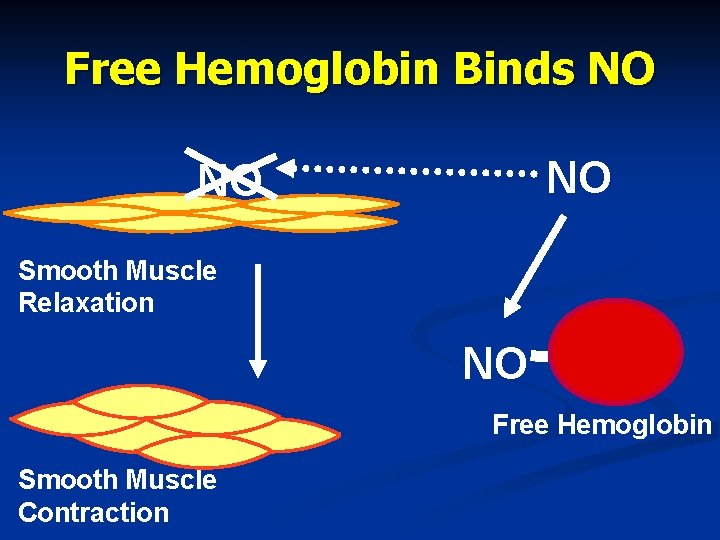
Free Hemoglobin Binds NO NO NO Smooth Muscle Relaxation NO Free Hemoglobin Smooth Muscle Contraction

What Are The Effects of Nitric Oxide Trapping by Hemoglobin Spasm of the esophagus n Abdominal pain n Erectile dysfunction n Other symptoms such as “fatigue” n

What is PNH Clinical aspects Vascular (arterial constriction, HBP) n Pulmonary artery pressure increase (PHTN) n Spasm of the esophagus n Abdominal pain n Erectile dysfunction n Other symptoms such as “fatigue” n Platelets are more “reactive” n

What is PNH? Clinical Features n WBC: n n n Granulocytes - release content stimulating inflammation Monocytes - activate expressing TF which leads to blood clots. TF-Microvesicles Platelets become “activated” They stick together and form clumps n The membrane changes, allowing them to bind to monocytes n Pieces of the membrane come off (microvesicles) n

What is PNH? Clinical Features n Hemolytic anemia due to complement activation Hemoglobinuria and, eventually, kidney damage n Anemia to a variable degree n Effects of NO depletion- HBP, smooth muscle dystonia, reduced blood flow to the kidney and lungs n n Impaired bone marrow function

What is PNH? Clinical Features Thrombosis (Blood clots) § Often in unusual places (liver veins, abdominal veins, cerebral veins, dermal veins) § Fatigue – overwhelming, poor correlation to level of hemoglobin § inflammation § anemia § Portal hypertension (PHTN). §
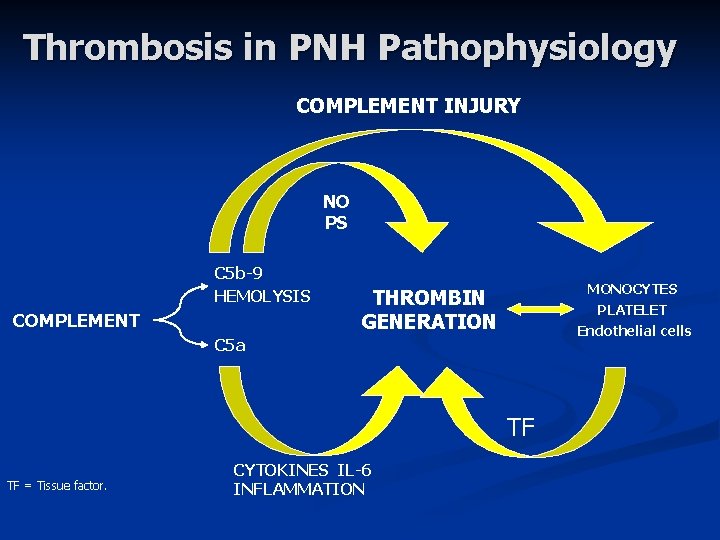
Thrombosis in PNH Pathophysiology COMPLEMENT INJURY NO PS C 5 b-9 HEMOLYSIS COMPLEMENT MONOCYTES PLATELET Endothelial cells THROMBIN GENERATION C 5 a TF TF = Tissue factor. CYTOKINES IL-6 INFLAMMATION

Laboratory Evaluation of PNH n Acidified Serum Test (Ham Test 1939) n n Acidified serum activates alternative complement pathway resulting in lysis of patient’s rbcs May be positive in congenitial dyserythropoietic anemia Still in use today Sucrose Hemolysis Test (1970) n n n 10% sucrose provides low ionic strength which promotes complement binding resulting in lysis of patient’s rbcs May be positive in megaloblastic anemia, autoimmune hemolytic anemia, others Less specific than Ham test

Laboratory Evaluation of PNH n PNH Diagnosis by Flow Cytometry (1986) n Considered method of choice for diagnosis of PNH (1996) n Detects actual PNH clones lacking GPI anchored proteins n More sensitive and specific than Ham and sucrose hemolysis test

PNH Diagnosis by Flow Cytometry Of the long list of GPI anchored protein, monoclonal antibodies to the following antigens have been used in the diagnosis of PNH The most useful Abs are to CD 14, 16, 55, 59, and 66. Are all required? Probably not - more studies needed Antigen Cell Lineage Function CD 14 monocytes LPS receptor, MDF CD 16 neutrophils Fc III receptor CD 24 neutrophils B-cell differentiation marker CD 55 all lineages DAF CD 58 all lineages possible adhesion CD 59 all lineages MIRL, HRF, protectin CD 66 b neutrophils CEA-related glycoprotein

PNH Diagnosis by Flow Cytometry n Antigen expression is generally categorized into three antigen density groups n type I Normal Ag expression n type II Intermediate Ag expression n type III No Ag expression n Patient samples that demonstrate cell populations with diminished or absent GPI-linked proteins (Type II or III cells) with multiple antibodies are considered to be consistent with PNH. n Should examine multiple lineages (ie granulocytes & monocytes)
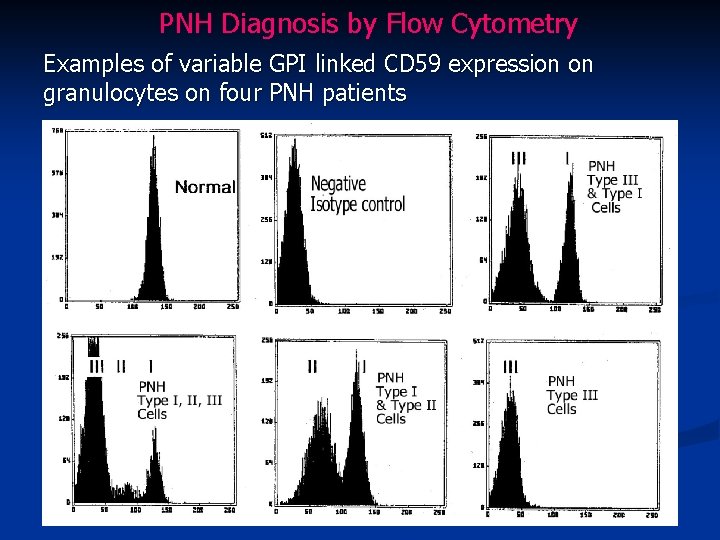
PNH Diagnosis by Flow Cytometry Examples of variable GPI linked CD 59 expression on granulocytes on four PNH patients
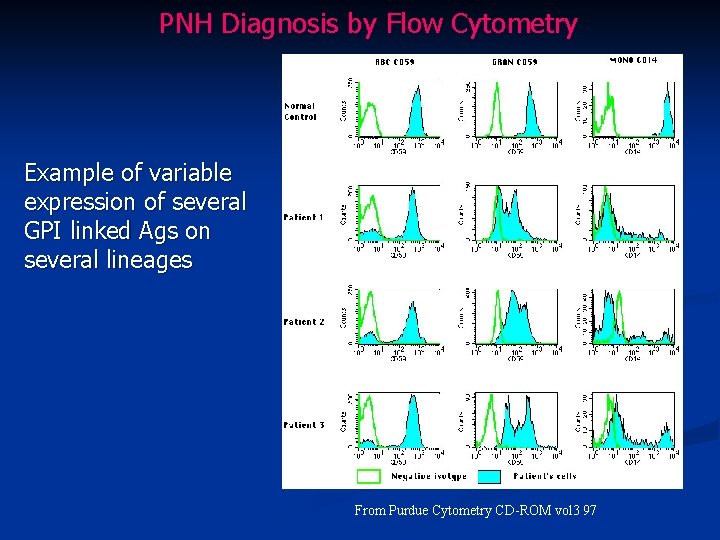
PNH Diagnosis by Flow Cytometry Example of variable expression of several GPI linked Ags on several lineages From Purdue Cytometry CD-ROM vol 3 97

PNH Diagnosis by Flow Cytometry n Flow Cytometry is method of choice but only supportive for/against diagnosis n More studies are needed to better define whether the type (I, II, or III), cell lineage, and size of the circulating clone can provide additional prognostic information. n Theoretically - should be very valuable

Historical Management Options for PNH Generally conservative, supportive, and dependent on symptom severity 1, 2 n n n Transfusions Anticoagulants Supplements n Folic acid n Iron n Erythropoiesis stimulating agents Steroids/androgen hormones Allogeneic bone marrow transplant (limited eligibility)

What is Soliris®? Monoclonal antibody (protein) that blocks complement at C 5 preventing the formation of the terminal complement complex n Quickly and markedly reduces hemolysis n Stops hemoglobinuria n Increases hemoglobin level n n Reduces transfusions n Hematocrit may not be quite normal

Microorganisms SOLIRIS Blocks Terminal Complement Proximal Classical C 3 Terminal Lectin Antigen-Antibody Complexes C 5 Constitutive/ Microorganisms C 3 a • SOLIRIS binds with high affinity to C 5 • Terminal complement activity is blocked C 3 b C 5 b SOLIRIS Alternative C 5 a C 5 b-9 Cause of Hemolysis in PNH • Proximal functions of complement remain intact • Weak anaphylatoxin • Immune complex and apoptotic body clearance Figueroa, et al. Clin Microbiol Rev. 1991; 4: 359 -395. • Microbial Walport. N Engl J Med. 2001; 344: 1058. SOLIRIS™ (eculizumab) [package insert]. Alexion Pharmaceuticals; 2007. opsonization
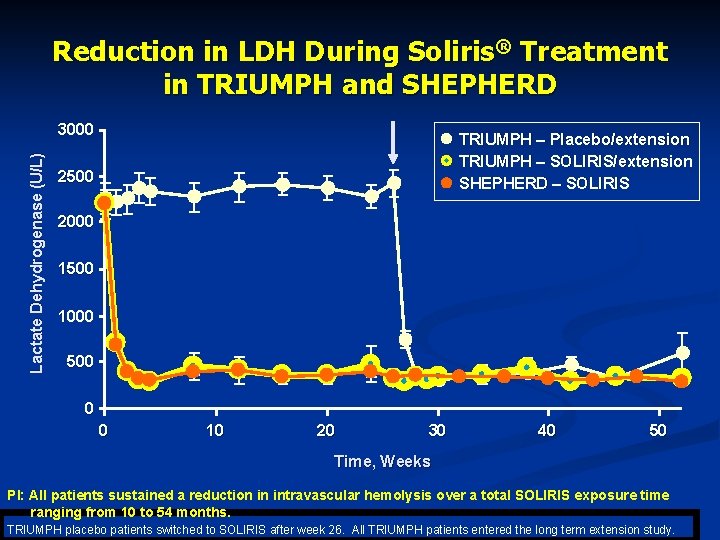
Reduction in LDH During Soliris® Treatment in TRIUMPH and SHEPHERD Lactate Dehydrogenase (U/L) 3000 TRIUMPH – Placebo/extension TRIUMPH – SOLIRIS/extension SHEPHERD – SOLIRIS 2500 2000 1500 1000 500 0 0 10 20 30 40 50 Time, Weeks PI: All patients sustained a reduction in intravascular hemolysis over a total SOLIRIS exposure time ranging from 10 to 54 months. TRIUMPH placebo patients switched to SOLIRIS after week 26. All TRIUMPH patients entered the long term extension study.
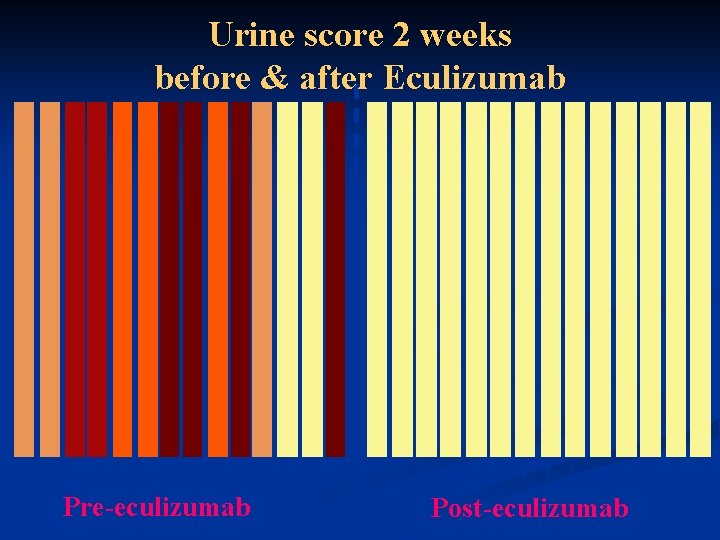
Urine score 2 weeks before & after Eculizumab 4 4 7 7 5 5 8 8 5 8 4 Pre-eculizumab 1 1 8 1 1 1 1 Post-eculizumab
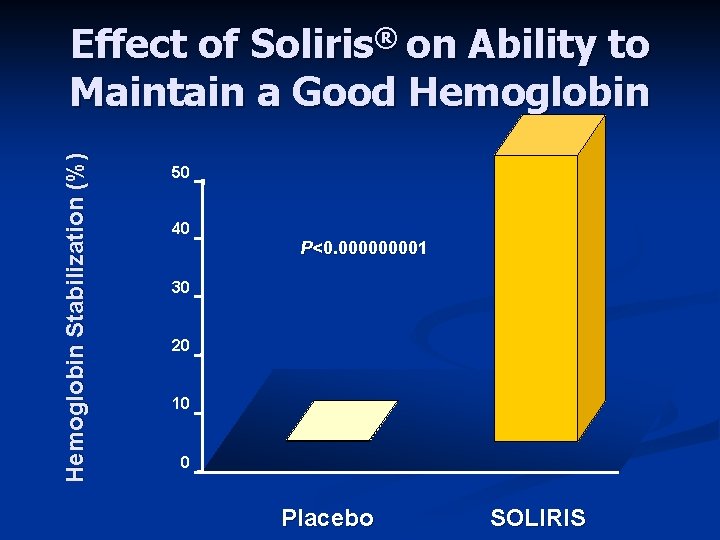
Hemoglobin Stabilization (%) Effect of Soliris® on Ability to Maintain a Good Hemoglobin 50 40 P<0. 00001 30 20 10 0 Placebo SOLIRIS
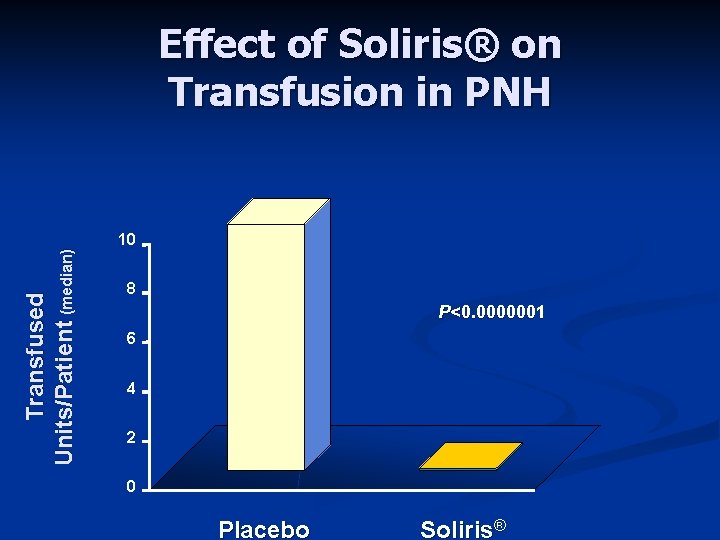
Transfused Units/Patient (median) Effect of Soliris® on Transfusion in PNH 10 8 P<0. 0000001 6 4 2 0 Placebo Soliris®

What is the effect of Soliris® in PNH n Stops the symptoms associated with hemolysis “Fatigue” n Esophageal and abdominal spasm n Erectile dysfunction n Improves sense of well being n Reduced the need for transfusion n n Appears to reduce thrombosis (blood clots)
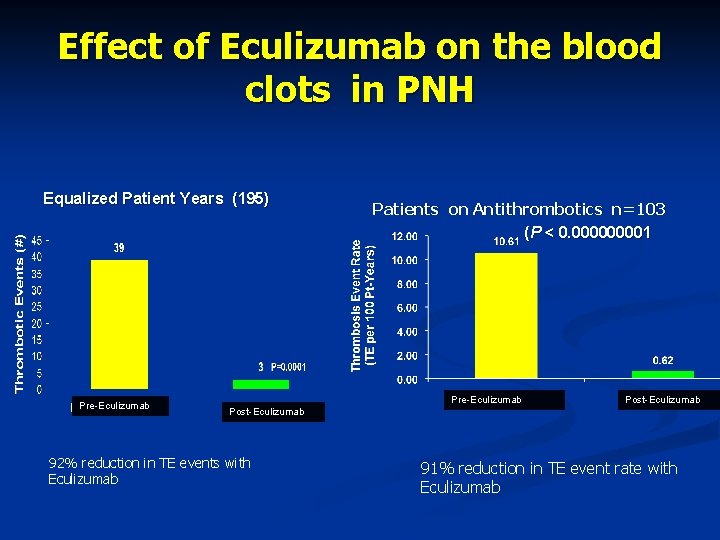
Effect of Eculizumab on the blood clots in PNH Equalized Patient Years (195) Pre-Eculizumab Patients on Antithrombotics n=103 (P < 0. 00001 Pre-Eculizumab Post-Eculizumab 92% reduction in TE events with Eculizumab 91% reduction in TE event rate with Eculizumab

What is the Effect of Soliris®? Improves kidney function reduced hemoglobinuria and iron deposition n Reduced thrombosis n Improves hypertension May in part be due to availability of nitric oxide

Side Effects of Soliris® Treatment n Susceptibility to sepsis by meningococcal organism n n n All patients must be vaccinated at least 2 weeks before starting Soliris All patients must know to seek medical help at once when fever happens All patients must carry cards describing this complication Headache – first week or 2 Cost Inconvenience n Must be given every 12 -14 days by vein

What Soliris® Cannot Do n Does not appear to improve impaired bone marrow function Low white count or low platelet count may persist in some patients, especially if it is due to aplastic anemia n Other treatments may be indicated n n Bone n marrow transplantation immunosuppressives

When is Soliris Ineffective or Less Effective § § Patient has been incorrectly diagnosed with PNH. Patient has a very small PNH clone (less than 10%) bone marrow failure- AA Breakthrough – infections, increased clearance, delayed dosing Extravascular hemolysis

Which PNH Patients are Candidates for Soliris? n n n n Patients with hemolysis (LDH ) Patients with large CD 59 deficient clones- RBC , WBC Patients with hemolysis with evidence of renal impairement GRF<90, proteinuria etc Patients with history of thrombosis Patients with hemolysis and elevated Ddimers Patients with hemolysis with fatigue Patients with hemolysis and transfusion dependence Patients prior to ? BMT, surgery, ? ? ? pregnancy

Who Should Get Soliris®? In all cases, the decision should be made by a physician that understand PNH, its complications and its treatment in conjunction with the patient, whose life is affected by the disorder.
- Slides: 67