Parotid region It is a fascial lined space












- Slides: 37

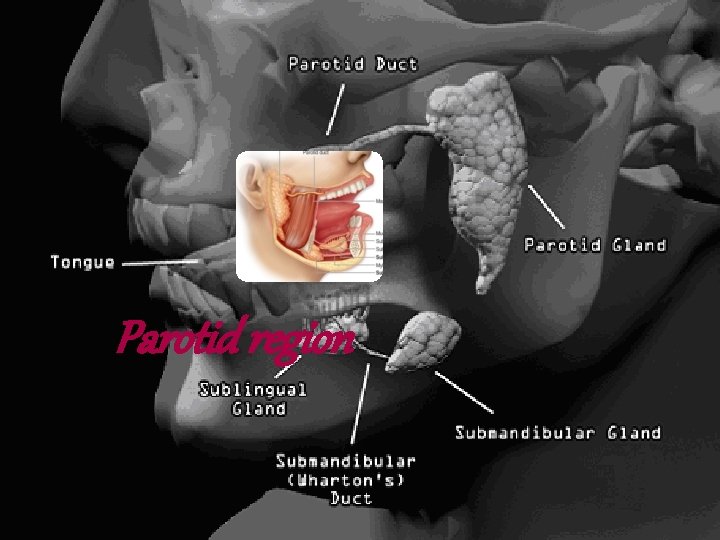
Parotid region

It is a fascial lined space which forms the mould or bed for the parotid gland. Boundaries: Front – post. Border of ramus with masseter and med. pterygoid Behind- mastoid process and sternomastoid. Above- ext. acoustic meatus and post. part of TMJ Below- post. Belly of digastric and stylohyoid Medially- styloid process with muscles.

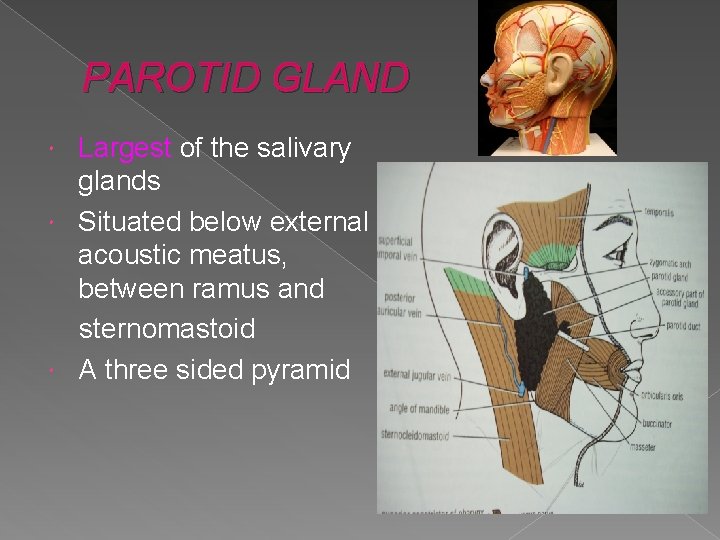
PAROTID GLAND Largest of the salivary glands Situated below external acoustic meatus, between ramus and sternomastoid A three sided pyramid

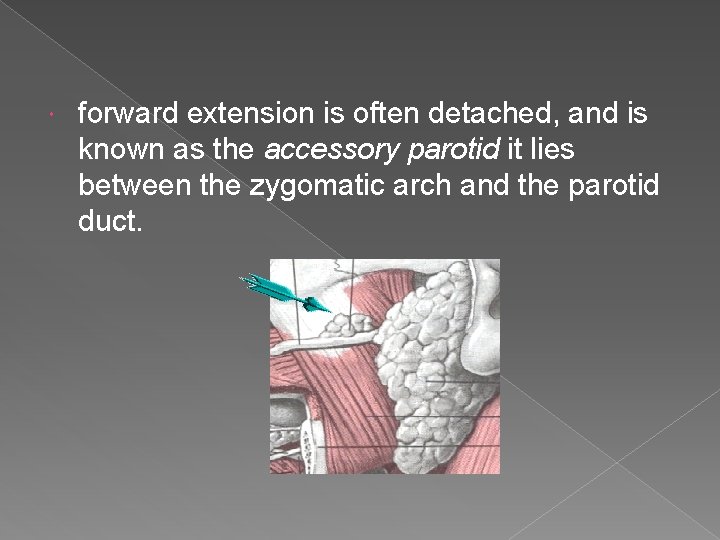
forward extension is often detached, and is known as the accessory parotid it lies between the zygomatic arch and the parotid duct.

Parotid Capsule : The investing layer of the deep cervical fascia forms a capsule for the gland. The superficial lamina, thick and adherent to the gland, is attached above to the zygomatic arch. The deep lamina is thin and is attached to the styloid process, the mandible and the tympanic plate. A portion of the deep lamina, extending between the styloid process and the mandible, is thickened to form the stylomandibular ligament which separates the parotid gland from the submandibular salivary gland.

The gland has four surfaces: (1) superior (base of the pyramid); (2) superficial; (3) anteromedial; and (4) posteromedial. The surfaces are separated by three borders: (1) anterior; (2) posterior; and (3) medial.

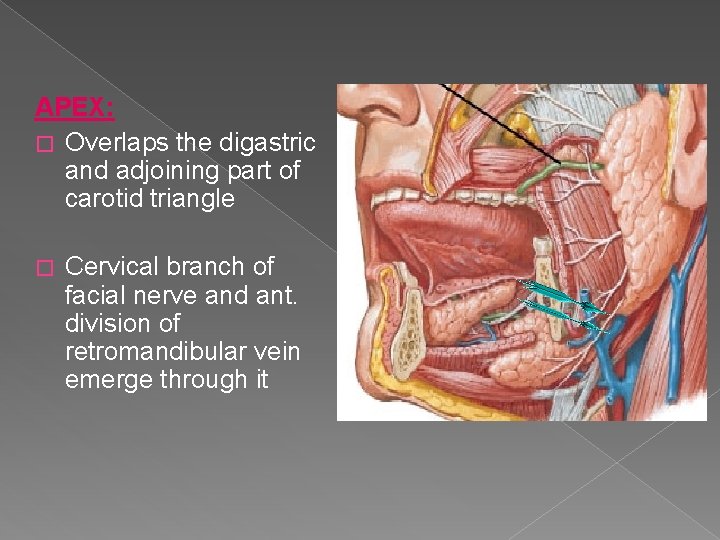
APEX: � Overlaps the digastric and adjoining part of carotid triangle � Cervical branch of facial nerve and ant. division of retromandibular vein emerge through it

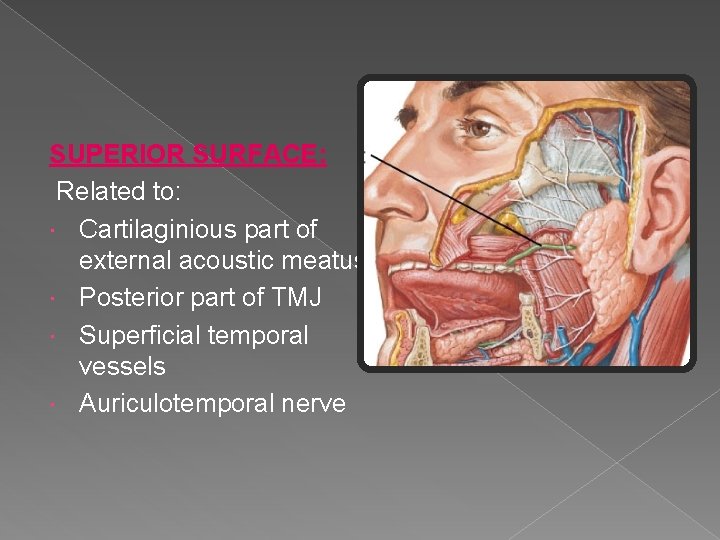
SUPERIOR SURFACE: Related to: Cartilaginious part of external acoustic meatus Posterior part of TMJ Superficial temporal vessels Auriculotemporal nerve

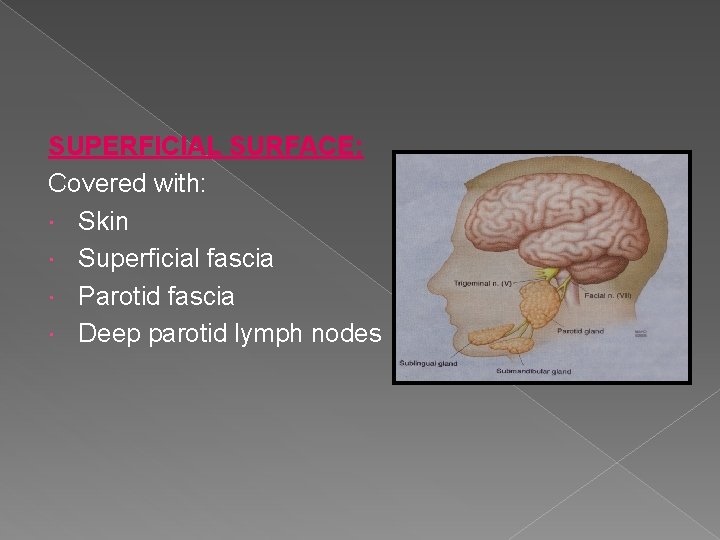
SUPERFICIAL SURFACE: Covered with: Skin Superficial fascia Parotid fascia Deep parotid lymph nodes

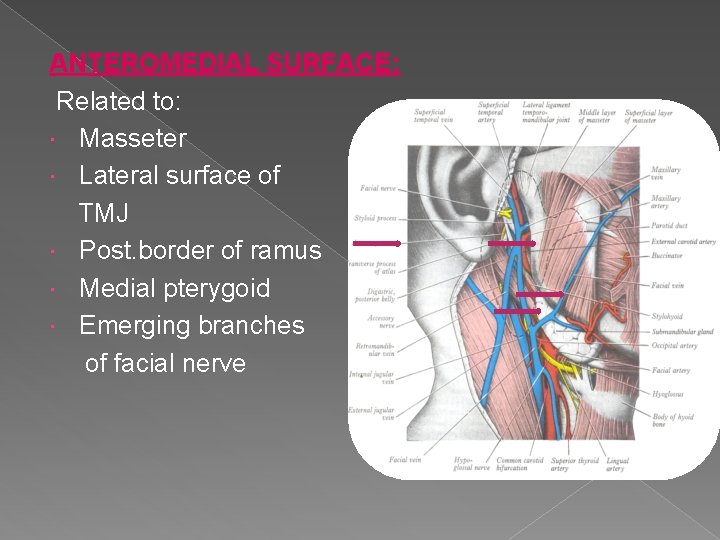
ANTEROMEDIAL SURFACE: Related to: Masseter Lateral surface of TMJ Post. border of ramus Medial pterygoid Emerging branches of facial nerve

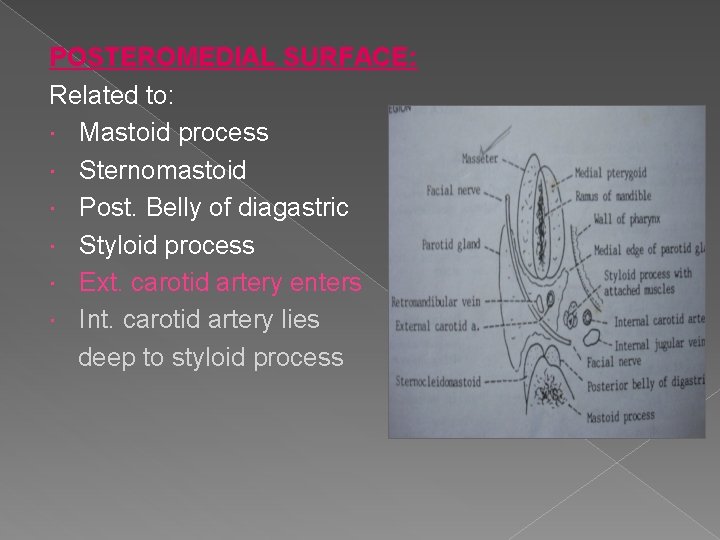
POSTEROMEDIAL SURFACE: Related to: Mastoid process Sternomastoid Post. Belly of diagastric Styloid process Ext. carotid artery enters Int. carotid artery lies deep to styloid process

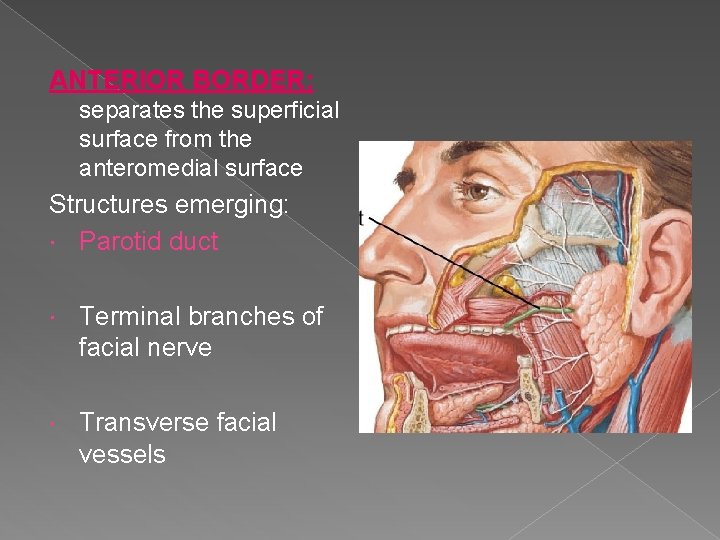
ANTERIOR BORDER: separates the superficial surface from the anteromedial surface Structures emerging: Parotid duct Terminal branches of facial nerve Transverse facial vessels

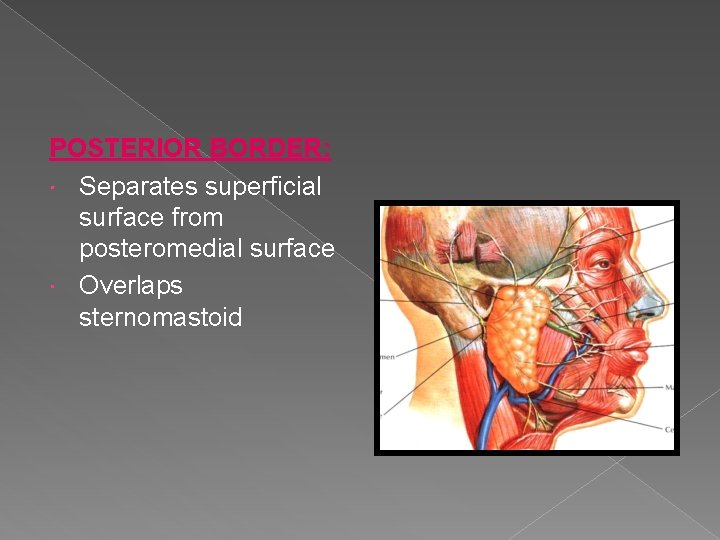
POSTERIOR BORDER: Separates superficial surface from posteromedial surface Overlaps sternomastoid

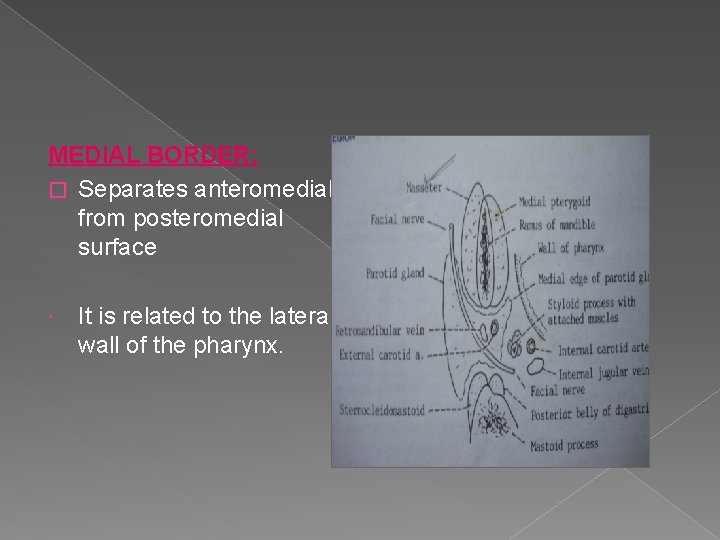
MEDIAL BORDER: � Separates anteromedial from posteromedial surface It is related to the lateral wall of the pharynx.

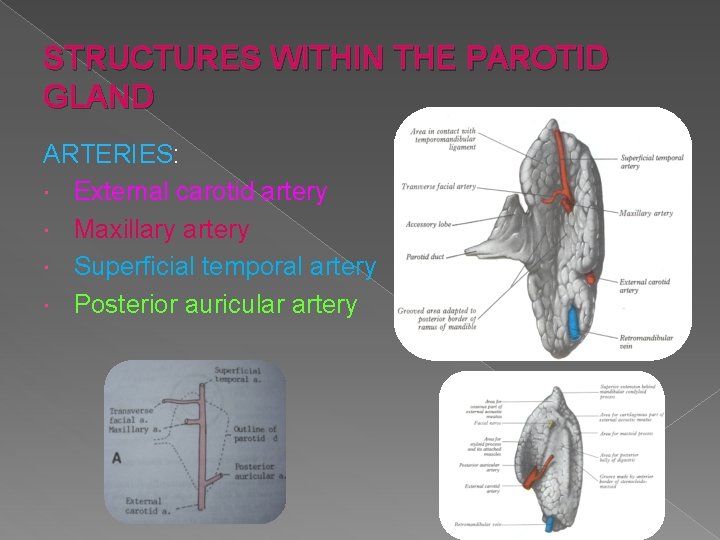
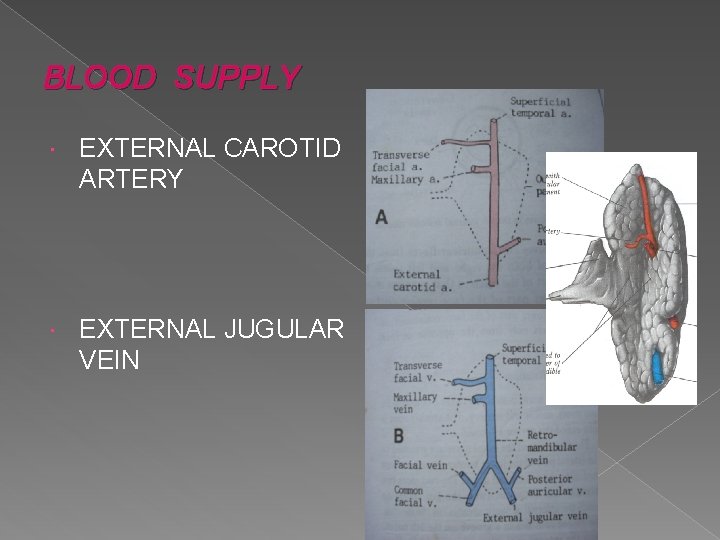
STRUCTURES WITHIN THE PAROTID GLAND ARTERIES: External carotid artery Maxillary artery Superficial temporal artery Posterior auricular artery

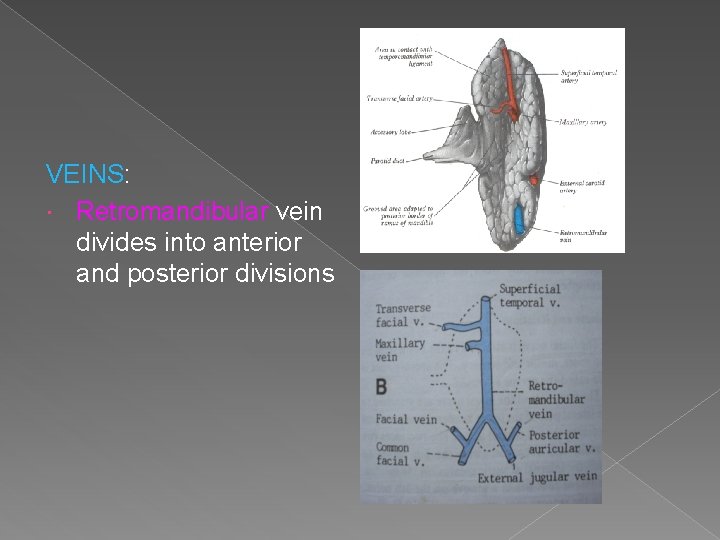
VEINS: Retromandibular vein divides into anterior and posterior divisions

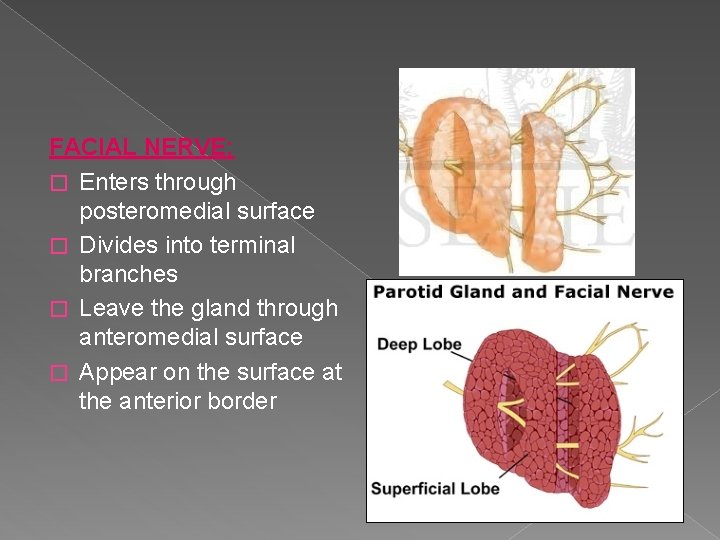
FACIAL NERVE: � Enters through posteromedial surface � Divides into terminal branches � Leave the gland through anteromedial surface � Appear on the surface at the anterior border

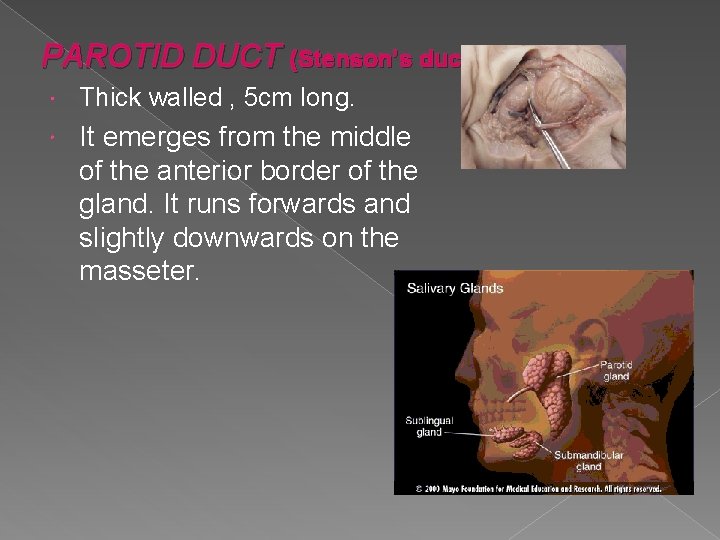
PAROTID DUCT (Stenson’s duct) Thick walled , 5 cm long. It emerges from the middle of the anterior border of the gland. It runs forwards and slightly downwards on the masseter.

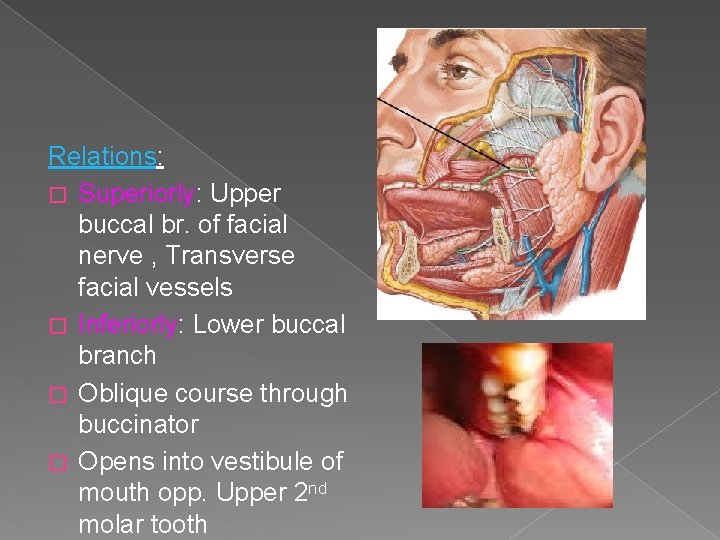
Relations: � Superiorly: Upper buccal br. of facial nerve , Transverse facial vessels � Inferiorly: Lower buccal branch � Oblique course through buccinator � Opens into vestibule of mouth opp. Upper 2 nd molar tooth

BLOOD SUPPLY EXTERNAL CAROTID ARTERY EXTERNAL JUGULAR VEIN

NERVE SUPPLY Parasympathetic nerves are secretomotor. They reach the gland through the auriculotemporal nerve. Sympathetic nerves: vasomotor Derived from plexus around middle meningeal artery Sensory nerves: Auriculotemporal nerve Parotid fascia by sensory fibres of greater auricular nerve(C 2)

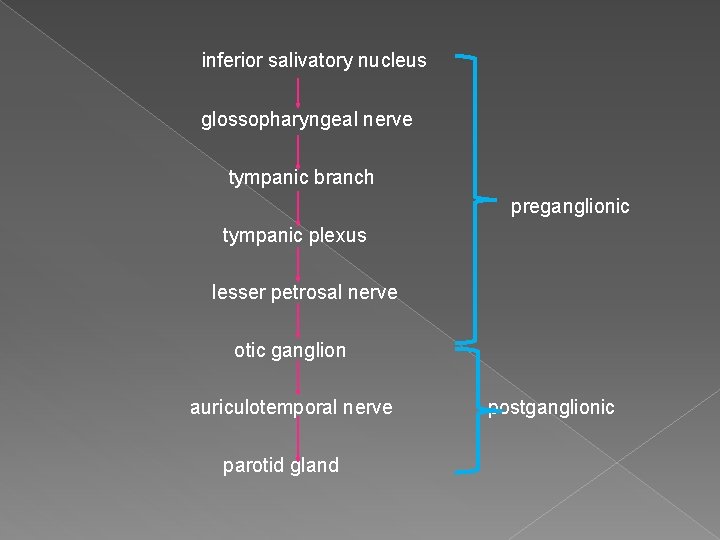
inferior salivatory nucleus glossopharyngeal nerve tympanic branch preganglionic tympanic plexus lesser petrosal nerve otic ganglion auriculotemporal nerve parotid gland postganglionic

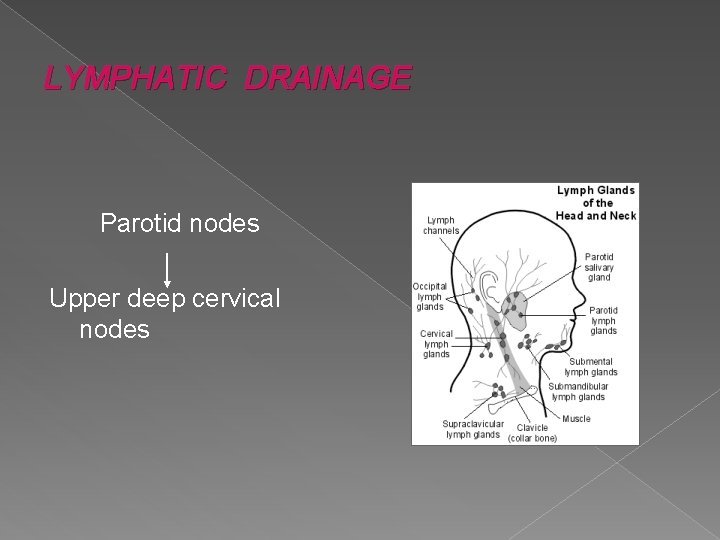
LYMPHATIC DRAINAGE Parotid nodes Upper deep cervical nodes

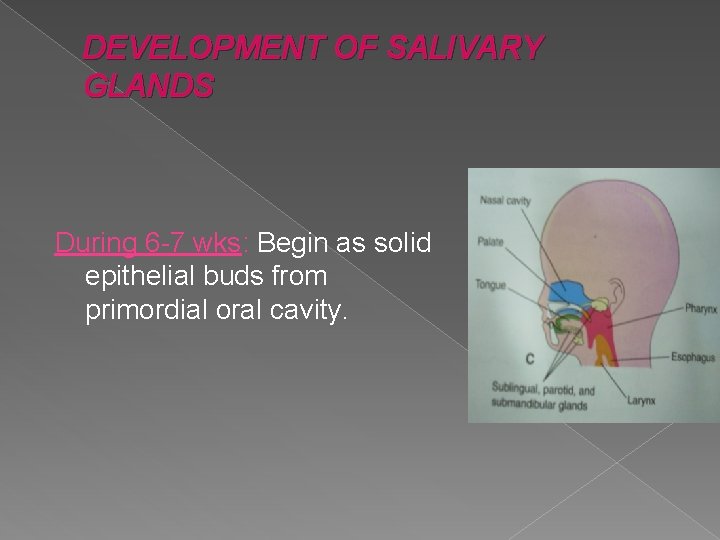
DEVELOPMENT OF SALIVARY GLANDS During 6 -7 wks: Begin as solid epithelial buds from primordial oral cavity.

Parotid gland: 1 st to appear (early in 6 th-7 thwk) Buds arise from oral ectodermal lining near stomodeum. Cords- Canalize- develop Lumina- become duct by 10 th weeks Rounded ends- develop into acini Secretion commence at 18 th wk Capsule: surrounding mesenchyme

APPLIED ANATOMY 1. Parotid swellings are very painful due to the unyielding nature of the parotid fascia 2. Mumps is an infectious disease of the salivary glands (usually the parotid) caused by a specific virus. 3. A parotid abscess may be caused by spread of infection from the oral cavity. An abscess may also form due to suppuration of the parotid lymph nodes draining an infected area. It is drained by small horizontal incision. Hilton’s method.

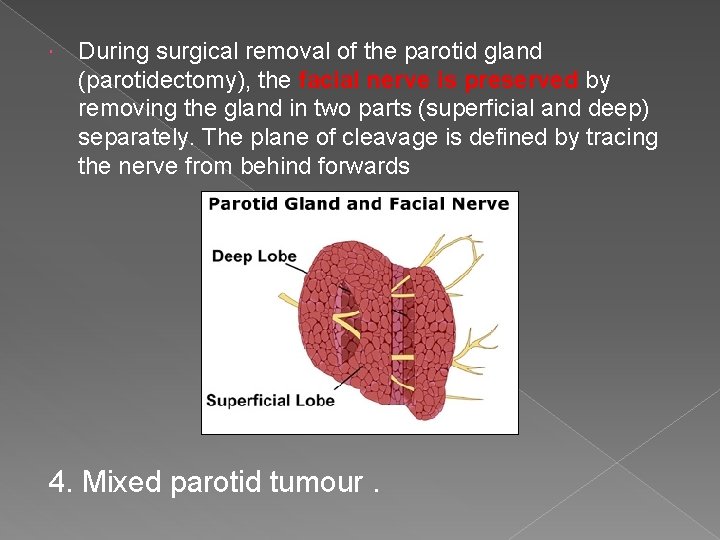
During surgical removal of the parotid gland (parotidectomy), the facial nerve is preserved by removing the gland in two parts (superficial and deep) separately. The plane of cleavage is defined by tracing the nerve from behind forwards 4. Mixed parotid tumour.

5. Sometimes penetrating wound of the parotid gland damages the auriculotemporal and great auricular nerves. During the process of healing, the secretomotor fibres of auriculotemporal nerve grow out and join with the distal end of the great auricular nerve, through which the fibres reach the sweat glands in the facial skin. Therefore, when the patient eats beads of perspiration appear on the skin covering the parotid, because the stimulus intended for salivary secretion produces sweat secretion instead. Such an interesting complication during the healing of penetrating wound of parotid gland is known as the Frey's syndrome. .

Obstructive Salivary Gland Disorders Sialolithiasis Mucous retention/extravasation

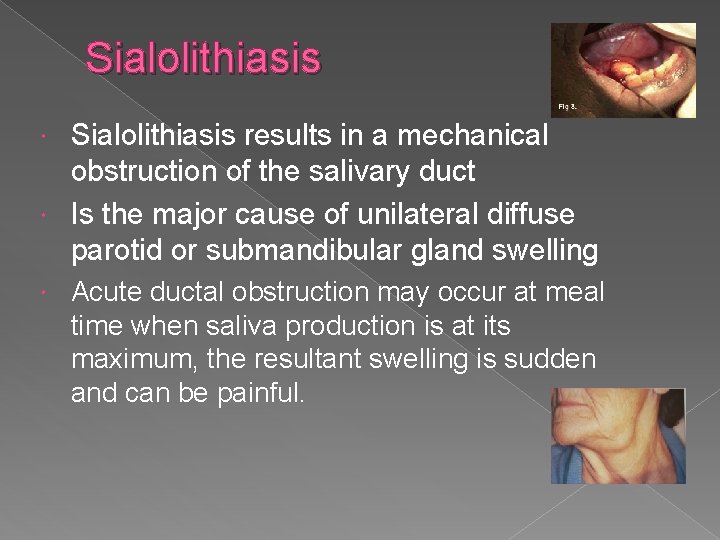
Sialolithiasis results in a mechanical obstruction of the salivary duct Is the major cause of unilateral diffuse parotid or submandibular gland swelling Acute ductal obstruction may occur at meal time when saliva production is at its maximum, the resultant swelling is sudden and can be painful.

Sialography Consists of opacification of the ducts by a retrograde injection of a water-soluble dye. Provides image of stones and duct morphological structure May be therapeutic, but success of therapeutic sialography never documented

Diagnostic Sialendoscopy Allows complete exploration of the ductal system, direct visualization of duct pathology Success rate of >95% Disadvantage: technically challenging, trauma could result in stenosis, perforation

Salivary Gland Infections Acute bacterial sialadenitis Chronic bacterial sialadenitis Viral infections

Sialadenitis represents inflammation mainly involving the acinoparenchyma of the gland.

Mumps 2 -3 week incubation after exposure (the virus multiplies in the URTor parotid gland) 3 -5 day viremia Then localizes to biologically active tissues like salivary glands, germinal tissues and the CNS.

Clinical presentation 30% experience prodromal symptoms prior to development of parotitis Headache, myalgias, anorexia, malaise Onset of salivary gland involvement is heralded by earache, gland pain, dysphagia and trismus

SALIVARY GLAND NEOPLASMS Benign Neoplasms Malignant Neoplasms