Parasomnias Wahba W Wahba M D Director of

Parasomnias Wahba W. Wahba, M. D. Director of Sleep-Wake Disorder Center Daytona Beach, FL Family Medicine Spring Forum Hollywood, Florida

Objectives n n n Definition of Parasomnias Classification of Parasomnias Pathophysiology of Parasomnias Diagnosis of Parasomnias Medicolegal Implications of Parasomnias Treatment of Parasomnias

What are Parasomnias? n n A group of disorders exclusive to sleep and wake -to-sleep transition They encompass arousals with abnormal motor, behavioral or sensory experiences n n Sensory experiences often involve perceptions, dream -like hallucinatory experiences, and autonomic symptoms When excessive motor-activity is present, can be disruptive to patient and patient’s bed partner
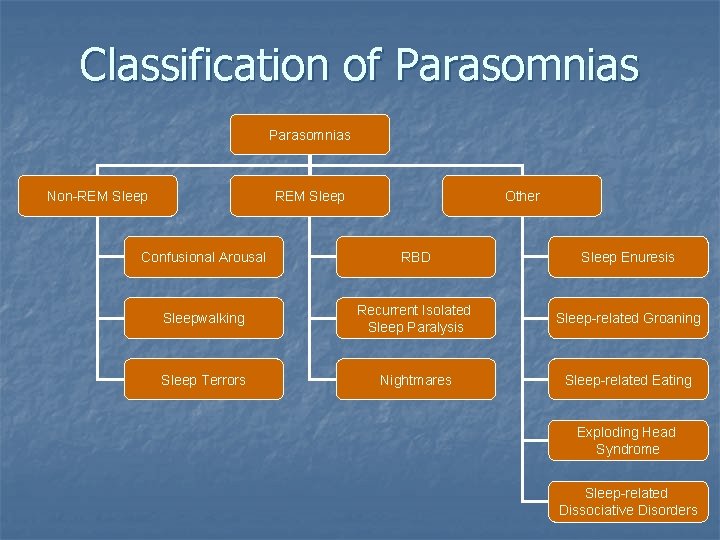
Classification of Parasomnias Non-REM Sleep Other Confusional Arousal RBD Sleep Enuresis Sleepwalking Recurrent Isolated Sleep Paralysis Sleep-related Groaning Sleep Terrors Nightmares Sleep-related Eating Exploding Head Syndrome Sleep-related Dissociative Disorders
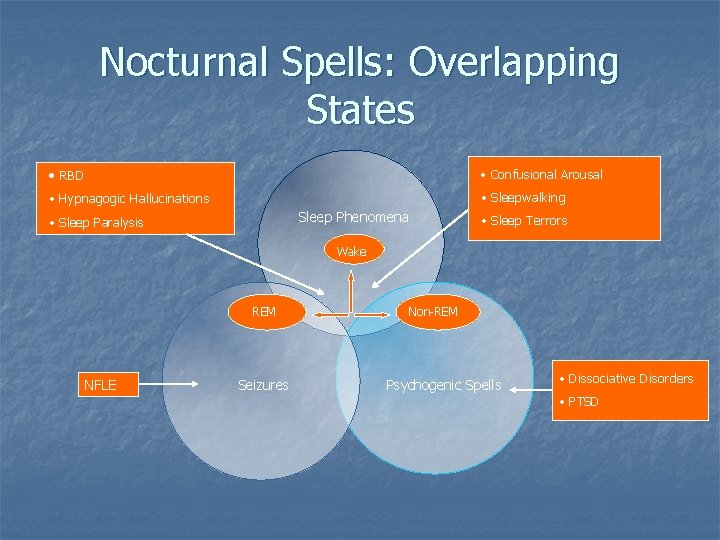
Nocturnal Spells: Overlapping States • RBD • Confusional Arousal • Hypnagogic Hallucinations • Sleepwalking Sleep Phenomena • Sleep Paralysis • Sleep Terrors Wake REM NFLE Seizures Non-REM Psychogenic Spells • Dissociative Disorders • PTSD

Pathophysiology n n Abnormal brain electro-chemical activity during sleep Disordered arousals from sleep Over-activation and release (disinhibition) phenomena Mixed states of sleep and wakefulness
PATHOPHYSIOLOGY n n De-afferentiation of the locomotor centers from the generator of the different sleep states Locomotor sensors are present at spinal and supraspinal levels and explain motor activity or ambulation

Pathophysiology n n NOT caused by psychiatric disorders Stress, Sleep Deprivation and OSA/SDB can trigger sleep aggression and violence in a person already predisposed to certain sleep disorders

Non-REM Parasomnias Confusional Arousal 1. • Including sleeprelated abnormal sexual behaviors 2. Sleepwalking 3. Sleep Terrors § § § Increased predilection in children Decreased predilection with age Occur in the first half of the night (typically first two hours of sleep)

Confusional Arousal n n n n Confusion during and following arousals from sleep Patient is disoriented in time and space Slow of speech and mentation Responds poorly to commands or questions Major memory impairment both retrograde and anterograde Behavior may last for several minutes to hours May be precipitated by forced awakening or OSA

Case History – Confusional Arousal n n n 56 -year-old man history of traumatic brain injury and OSA poor compliance with CPAP complains of night spells Described as sudden arousal with confusion and singing n n PSG Multiple spells of arousal and confusion with arm flapping and talking from NREM sleep In one event, technician reported quacking like a duck 20 episodes recorded with and without preceding respiratory effort No seizure activity Diagnosis: Confusional Arousal, Resolved with CPAP therapy

Criminal Cases – Confusional Arousal A sleeping person stabbed a friend to death after the friend tried to awaken him A boy tried to pick up an object next to a sleeping person 1. 2. • Person was aroused by the noise, grabbed a knife and stabbed the boy Person was awakened by a noise at midnight 3. • Person grabbed an axe and attacked a “stranger in the room, ” killing his wife Sleep 2007; 30: 1039 -1947

Night shift supervisor fell asleep in his office and 30 minutes later an employee entered the office to wake the supervisor 4. • Supervisor immediately pulled out his gun in confusion and fired the gun, killing the employee A porter entered a darkened hotel room unannounced and awakened the defendant 5. • Defendant shot the porter 3 times, killing the porter


Sleepwalking: Non-REM Sleep Parasomnia n n A series of complex behaviors that emerge abruptly during sudden arousals from slow -wave sleep Walking around with an altered state of consciousness and impaired judgment Eyes are open Inappropriate interaction with the environment

Sleepwalking: Diagnostic Criteria n n n Ambulation that occurs in sleep Onset typically in prepubertal children Associated features Difficulty arousing patient during an episode n Amnesia following an episode n n n Typically in first third of sleep episode PSG onset of episode during N 3

Sleepwalking & Confusional Arousal n Major Predisposing Factor: n n 22% - neither parent has the disorder 45% - one parent has the disorder 60% - both parents have the disorder Major Precipitating Factors: n n n Genetic Sleep Deprivation Stress Sleep Disordered Breathing Alcohol Use (? ) Thioridazine, Chloral Hydrate, Lithium, Prolixin, Perphenazine & Desiparmine

Case – Canada v. Parks n n n 24 -year-old Parks arose from couch where he fell asleep watching TV, put on his shoes, took car keys, left front door and garage door open, and drove 23 km in Toronto to his in-laws home Parks unlocked the door, walked to in-laws bedroom, strangled father-in-law, beat mother-in -law with tire iron, stabbed both with knife from the kitchen Parks cut his own flexor tendons in both hands and felt no pain then, or later when he was observed in a sleepwalking-like state

Canada v. Parks n Parks picked-up kitchen phone and took it off the hook, ran upstairs to children's’ bedrooms n n n Grunting stopped, after which Parks left Parks turned himself in to police stating: n n Children described hearing screaming and animal-like grunting “I killed someone with my bare hands. ” Distressed and shaking, Parks asked policeman: n “What happened? I was sleeping on the couch. I just woke up. I had a dream. I had a knife in my hand. I was killing them. I choked them, then I went to the police station…How could I drive there and not know? ”

Canada v. Parks n According to police, Parks did not appear to be in pain despite his severed tendons Striking example of dissociative analgesia (i. e. profound blunting of pain) found in sleepwalking n This observation by police provides compelling evidence supporting a grossly impaired state of consciousness n
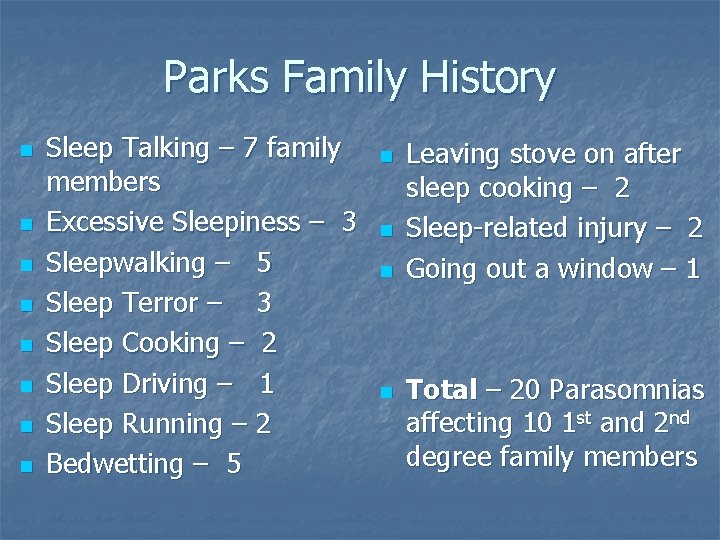

Parks Family History n n n n Sleep Talking – 7 family members Excessive Sleepiness – 3 Sleepwalking – 5 Sleep Terror – 3 Sleep Cooking – 2 Sleep Driving – 1 Sleep Running – 2 Bedwetting – 5 n n Leaving stove on after sleep cooking – 2 Sleep-related injury – 2 Going out a window – 1 Total – 20 Parasomnias affecting 10 1 st and 2 nd degree family members

Violent OSA-Triggered Confusional Arousal & Sleepwalking Baron J. Auckley. Sleep and Breathing 2005 n 55 -year old morbidly obese man, n n n Known OSA Progressive cognitive and psychological deterioration due to suboptimal treatment of OSA On night of admission, patient reached for bi-pap mask accidently picking up pistol with the mask and straps Unaware of gun in his hand, patient fired the pistol attempting to pull the straps of the mask Result: tangential scalp wound

Parasomnia & OSA Lateef O, Wyatt J, Cartwright R. Chest 2005 n 54 -year-old female n n n Found by police wandering in nearby town n n No childhood parasomnia, 5 year history of parasomnias, Sleep-driving from naps 5 times per month, Sleepwalking barefoot in the snow Chopped up her cat on cutting board in kitchen Awoke at 6 AM, hands covered in blood, cats remains next to trash can Sleep History: load snoring, EDS, weight gain PSG: severe OSA w/ marked hypoxia 4 month follow-up on CPAP: No Parasomnia

Sexsomnia n Other Terms: n n n Sleepsex Atypical sexual behavior during sleep Abnormal sleep-related sexual behaviors (ICSD-2) Problematic sexual behaviors emerging during sleep Two Most Common Causes: 1. Non-REM Parasomnias • 2. Confusional Arousal and Sleepwalking OSA

Sexsomnia in NREM Parasomnias n n Usually a history of Parasomnias Often childhood onset: sleepwalking, n sleep terrors, n Confusional arousals, n sleep-related eating disorder, n sleep talking n etc. n

Sexsomnia in OSA n “Snorgasm” n Typical History: n “Sexapnea” Onset or Increase of Snoring occurs with the onset of Sexsomnia

Sexsomnia: 31 Published Cases n Gender n n n Age n n 80. 6% 19. 4% 31. 9 ± 8. 0 years Duration n n Males Females 9. 5 ± 6. 1 years Behaviors may include: n n masturbation Sexual vocal/verbal Fondling Sexual Intercourse 22. 6% 19. 3% 45. 2% 41. 9 %

Sexsomnia: 31 Published Cases n n n n Amnesia of Sleepsex Assaultive Sleepsex behaviors Sleepsex with Minors Legal Repercussions Polysomnography performed Total # of Parasomnias Mean # of Parasomnias/Pt 100% 45. 2% 29. 0% 35. 5% 83. 9% 71 2. 2± 1. 0

Sexsomnia: Forensic Cases n n A case of Sexsomnia where there is no current documented OSA, and no past history of (observed) Parasomnias should be considered with skepticism A 1 st time Sexsomnia episode resulting in legal consequences should be considered doubtful

REM SLEEP BEHAVIOR DISORDER n n n Complex and elaborate motor activity Associated with agitated and violent dream mentation Wide range of activity: n n n n Verbalization Shouting Screaming Walking Running § Singing § Yelling § Kicking § Punching § Violent Agitated Behaviors PSG with elevation of limb or chin EMG during REM sleep The injury associated with these spells is often what triggers the patient to seek help

RBD: DIAGNOSTIC CRITERIA (ISCD 2) n POLYSOMNOGRAPHIC Excessive chin tone during REM sleep and/or n Excessive limb twitching during REM sleep n Absence of EEG epileptiform activity during REM sleep n n BEHAVIORAL CRITERIA History of problematic sleep related behaviors (Often, but not necessarily, dream enacting behaviors) that are injurious, potentially injurious, or disruptive of sleep And/Or n Documented REM sleep behaviors during PSG n

CAUSES ASSOCIATED WITH CHRONIC RBD n n n n n Idiopathic Neurologic disorders Medication induced SSRIs, Venlafaxine, mitazepine, TCAs, MAOIs, (not bupropion) B-Blockers ACE inhibitors Selegeline Caffiene, chocolate: excessive consumption

RBD: Sleep-Related Injury n n n n Bruises Subdural hematomas Lacerations Fractures Dislocations & Sprains Abrasions Tooth Chipping Hair Pulling

RBD n n The only parasomnia in ICSD-2 requiring PSG confirmation. 3 Reasons: PSG findings are present every night n RBD is NOT the only dream-enacting disorder n n n DOA, OSA, Nocturnal Seizures RBD is strongly linked to future Parkinson’s Disease making objective diagnosis crucial

POTETILY LETHAL BEHAVIORS ASSOCIATED WITH RBD Review of the Literature and Forensic Implications Journal of Forensic Sciences 2009; 54: 6

Published Cases of RBD Associated with Potentially Lethal Behaviors (Usually during Dream. Enactment) n Choking/Headlock Punching a pregnant bed partner Defenestration Near-Defenestration Diving from Bed n Total: n n n=22 -24 n=2 n=1 n=6 n=10 n= 41 -43

RBD & PARKINSONS DISEASE n n Reviewed medical records from 2002 -2006 Entry Criteria n n n Idiopathic RBD at time of RBD onset ≥ 15 yrs between RBD onset and onset of a neurodegenerative disorder (NDD) Results n n 27 patients satisfied entry criteria 23 yrs median interval between RBD onset and NDD n n 50 yrs greatest interval Conclusion n n The pathologic process may start decades before the first symptom of PD Long period has important implications for furture epidemiologic studies and interventions to slow or halt the NDD process

RBD Protects Against Obstructive Sleep Apnea (OSA)!!! n Correlation study 71 RBD patients n Loss of REM atonia and severity of OSA in RBD patients n n Case control study: 28 RBD/OSA patients; 27 OSA patients n Compare sleep related respiratory events between RBD/OSA patients and OSA patients n

RBD Protects Against (OSA) RESULTS n Correlation Study: increased REM sleep EMG activity was significantly associated with lower severity of OSA in RBD patients n n n Total AHI NREM AHI Obstructive AHI Mean apnea duration Case Control Study: RBD/OSA patients had significantly lesser severity of sleep apnea parameters than OSA controls n n n O 2 saturation (86% vs 81%) Shorter max hypopnia duration (54 vs 60 sec) Mean apnea duration (22 vs 26 sec)

Sleep-Related Eating Disorder (SRED)

SRED: Essential Features n n Recurrent episodes of involuntary eating and drinking during arousals from sleep with problematic consequences Episodes of eating always occur in an involuntary manner after an interval of sleep and usually during partial arousals with partial recall Some patients cannot be awakened (as in classic sleepwalking) Some patients have considerable alertness and substantial recall

SRED: Predominant Associations n n n Sleepwalking RLS/PLMD OSA Medication: Zolpidem, Olanzapine, Risperidone, Mitrazapine, Lithium, Anticholinergics Idiopathic, Indeterminate Onset childhood adolescents n early-mid adulthood

SRED n n n Appears to be a “final common pathway” disorder that can emerge from a broad range of clinical conditions Once SRED emerges, regardless of origin, SRED demonstrates a rather stereotypical course Classifies as a parasomnia (ICSD-2)

SRED: Diagnostic Criteria (ICSD-2) Recurrent episodes of involuntary eating and drinking during the main sleep period One of the following must be present: 1. 2. a. b. Consumption of peculiar forms or combination of food or inedible or toxic substances (frozen pizza, buttered cigarettes, raw bacon, cat food or salt/sugar peanut butter sandwich, amonia) Insomnia related to sleep disruption from repeated episodes of eating with a complaint of non-restorative sleep, daytime fatigue or somnolence Sleep-related injury: 3. n n n laceration from careless use of kitchen utensils, internal or external burns from consuming or spilling hot foods or beverages, poisoning and internal injuries from ingesting toxic substances

SRED: Diagnostic Criteria 4. Dangerous behaviors performed while in pursuit of food or while cooking food n 5. 6. e. g. Driving, kitchen fires Morning Anorexia often with abdominal distention Adverse health consequences from recurrent binge eating of high caloric foods n n n Excessive weight gain Destabilization or precipitation of Diabetes Mellitus Hyperlipidemia Overnight fasting before next day surgery can be compromised Consuming foods to which one is allergic Dental complication: tooth chipping and caries

SRED (ICSD-2) n n Female predominant disorder (60 -83%) Mean age of onset: 22 – 40 years In reported series n Nightly frequency of nocturnal eating very common n > 50% in reported cases

ASSOCIATION BETWEEN RLS & SRED n n 100 RLS patients in Northern Italy and 100 matched controls Two phone interviews about nocturnal eating, EDS, sleep quality, social demographics, health status, psychopathological traits

RESULTS n n n SRED: 33% in RLS versus 1% in controls (P=0. 001) Medication Use, Obsessive Compulsive Inventory more prevalent in RLS/SRED patients compared to RLS patients with out SRED Use of dopaminergic or hyptnotic medications in RLS patients did not corrolate with the presence of SRED

CONCLUSION n n A strong association of RLS with SRED was demonstrated in the aforementioned study Prospective studies are needed to establish the mechanisms underlying such association and whether it is causal Movement Disorders 2009 24 (6: 871 -877) Provini F. et al and Brotherhood (Univ. Of Bologna Italy)

COMMENTS n n SRED patients should be carefully questioned about RLS (including family history) RLS patients should be questioned about SRED (initially and longitudinally)

PARASOMNIA AMONG PHSYCHIATRIC OUTPATIENTS A Clinical, Epidemiologic, Cross-Sectional Study n n Subjects 18 -65 yrs old psych outpatient clinic, May-June 2006 Cross sectional study with three phase design n I. Structured questionare on parasomnias II: Clinical interview III: PSG n Patients with active parasomnias over the previous 1 yr Chinese University of Hong Kong Department of Psychiatry. Journal Clinical Psychiatry 2008

RESULTS n n n n 1, 235 completed Phase I (61% participation rate) Mean Age: 42 (+/- 11. 3) 68. 1% female SRED: 4% estimated lifetime prevalence SRED: 2. 4% estimated 1 year prevalence SRED patients had significantly greater depressive spectrum disorders compared to non. SRED patients had significantly less psychotic/bipolar disorders compared to non-SRED patients

PARASOMNIA AMONG PSYCHIATRIC OUTPATIENTS RESULTS CONTINUED n n Zolpidem (but not Zolpiclone) and antidepressants (SSRIs) were found to pose a risk for SRED Anti-psychotic medication had a negative association with SRED Polypharmacy was more common in the SRED group compared to the non-SRED group CONCLUSION: SRED and other parasomnias are common and under recognized in psychiatric outpatients in this study

Sleepwalking v. SRED Including patients with SW who evolve into SRED n n n SW: Slow wave sleep arousals predominately Episodes often occur early in sleep Benzodiazepine at bedtime usually effective n n n SRED: Distributed across all stages of NREM and rarely REM Episodes throughout most of sleep period Rarely effective as monotherapy – may aggravate SRED by deepening level of unconsciousness

ZOLPIDEM: SRED n n n n 19 patients SRED Females 84% (16/19) Mean Age: 47 (Range 17 -78) 84% recent and/or recurrent depression 89% taking anti-depressants when Zolpidem induced SRED Majority of patients were taking other drugs for varying psychiatric disorders N = 2 : started kitchen fires related to Zolpidem N = 2 : sleep driving related to Zolpidem n In both patients sleep driving occurred when patients took Zolpidem at home Sleep 2005: 28 suppl: A 259

ZOLPIDEM INDUCED AMNESTIC SRED n n n No patient had past history of SRED All patients had persistent insomnia 42% (8/19) had ≥ 1 other sleep disorder N=3 : OSA n N=2 : narcolepsy n N=2 : SW, RLS, RBD, n N=1 : DSPS n n Cessation of Zolpidem promptly stopped the SRED

ZOLPIDEM INDUCED AMNESTIC SRED CONCLUSIONS § § Zolpidem appears to be the most common drug that can induce amnestic SRED; only a small percent of patients treated with Zolpidem will develop SRED ZOPICLONE, ESZOPLICONE & ZALEPLON: similar to Zolpidem BUT do not have these effects

ZOLPIDEM AND AMNESTIC SRED Najar M. J. Clin Sleep Medicine 2007; 3: 637 8 n n 46 yr old female Ambien CR, 6. 25 mg hs After 3 weeks: almost nightly SRED Warmed leftovers and ate them n Left kitchen messy n Gained 50 lbs n n Sleep center evaluation: switched to Lunesta. n SRED immediately and completely stopped

CASE 1: ZOLPIDEM AND AMNESTIC SRED n n n 75 yr old patient: Zolpidem 10 mg hs taken for 3 yrs. No Parasomnia Switched to Zolpidem CR 12. 5 mg hs IMMEDIATELY developed amnestic SRED 4 consecutive nights Switched back to Zolpidem 10 mg hs NO FURTHER SRED or other Parasomnia for 6 months CHIANG A AND CRYSTAL A JOURNAL CLINICAL SLEEP MEDICINE 2008: 4: 155 -156

CASE 2: n n 70 yr old female: Zolpidem 10 mg hs for many years NO SRED or other parasomnia Soon after being switched to Zolpidem CR 12. 5 hs, developed nightly SRED for several consecutive nights Switched back to Zolpidem 10 mg hs; SRED immediately stopped with no recurrence one year follow up

ZOLPIDEM INDUCED AMNESTIC SRED n n n Neither patient (case 1 or 2) had any history or family history of SRED or other parasomnia or eating disorder Therefore in some vulnerable patients a relatively small adjustment in pharmacotherapy could increase the likelihood of inducing a parasomnia The more complex the sleep medical and physchiatric history and their therapies the greater the apparent risk for Zolpidem induced SRED

RISK PREDICTORS FOR HYPNOSEDATIVE-RELATED COMPLEX SLEEP BEHAVIOURS (CSBs) RETROSPECTIVE CROSS-SECTIONAL PILOT STUDY Journal of Clinical Psychiatry 2010 WONG H WANG TJ et al n n National Taiwan University Hospital Objective: Explore the risk predictors for complex sleep related behavours (CSBs) in subjects taking hynosedative drugs Methods: 125 subjects using hypnosedatives were enrolled from phsychiatric outpatient clinics of a medical center in Taiwan from May-July 2006

RESULTS n 19 of 125 subjects (15. 2%) reported CSBs; n n N=19 with CSBs (106 without CSBs) n n Comparing n=19 with Zolpidem CSBs and n=48 Zolpidem without CSBs In the 19 with Zolpidem CSBs: n n 89. 5% vs 49. 1% female in 1 st and 2 nd group respectively Mean dose of Zolpidem: 15. 3 mg (+/-5) vs 9. 4 mg (+/3. 7) n n ALL OF WHOM TOOK ZOLPIDEM 6 sleepwalking 7 SRED 6 SRED with hallucination Thus 68. 4% of CSBs involved SRED
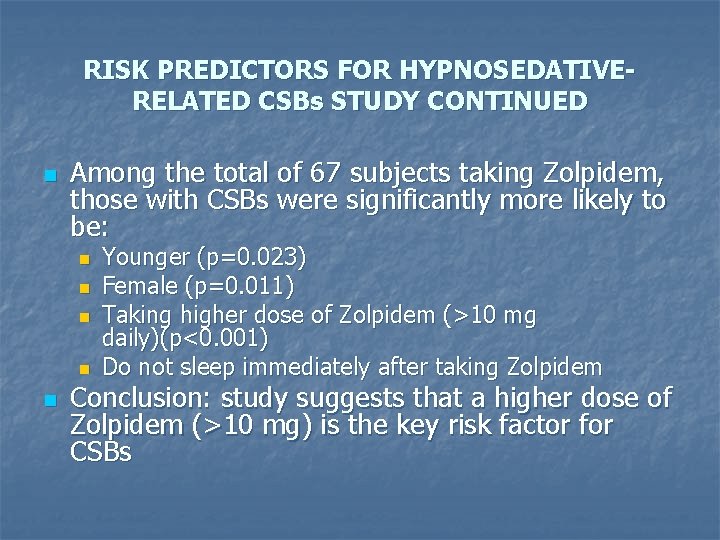

RISK PREDICTORS FOR HYPNOSEDATIVERELATED CSBs STUDY CONTINUED n Among the total of 67 subjects taking Zolpidem, those with CSBs were significantly more likely to be: n n n Younger (p=0. 023) Female (p=0. 011) Taking higher dose of Zolpidem (>10 mg daily)(p<0. 001) Do not sleep immediately after taking Zolpidem Conclusion: study suggests that a higher dose of Zolpidem (>10 mg) is the key risk factor for CSBs

Zolpidem Induced Amnestic SRED Atypical Features n n 100% Amnesia is atypical for SRED (many patients exhibit some recall) 100% Amnesia is atypical for sleep walking in adults (many patients exhibit some recall)

Final Comments n n n Zolpidem is usually a highly effective and safe hypnotic medication Zolpidem is the most commonly prescribed hypnotic medication in the USA and so its side effects will become more commonly known All sedative hypnotics carry a risk for inducing SRED (the basis for the FDA 2007 warning)
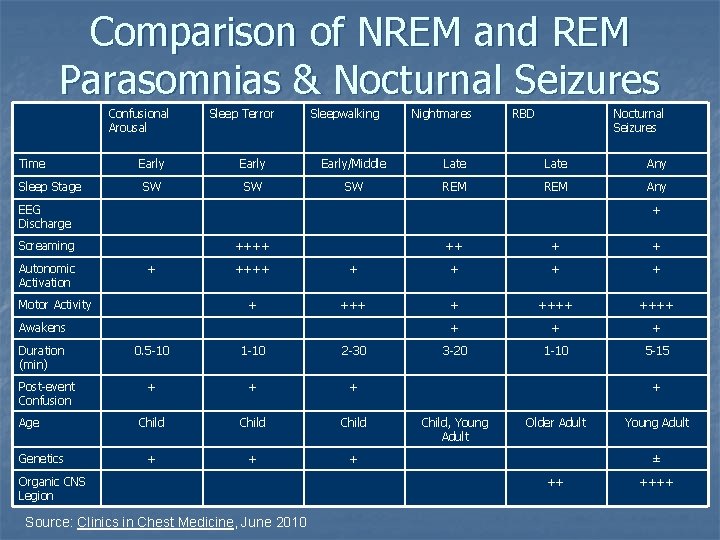
Comparison of NREM and REM Parasomnias & Nocturnal Seizures Confusional Arousal Time Sleep Stage Sleep Terror Sleepwalking Nightmares RBD Nocturnal Seizures Early/Middle Late Any SW SW SW REM Any EEG Discharge + Screaming Autonomic Activation ++++ + Motor Activity Post-event Confusion Age Genetics + + ++++ + ++++ + 3 -20 1 -10 5 -15 Awakens Duration (min) ++ 0. 5 -10 1 -10 2 -30 + + + Child + + + Organic CNS Legion Source: Clinics in Chest Medicine, June 2010 + Child, Young Adult Older Adult Young Adult ± ++ ++++
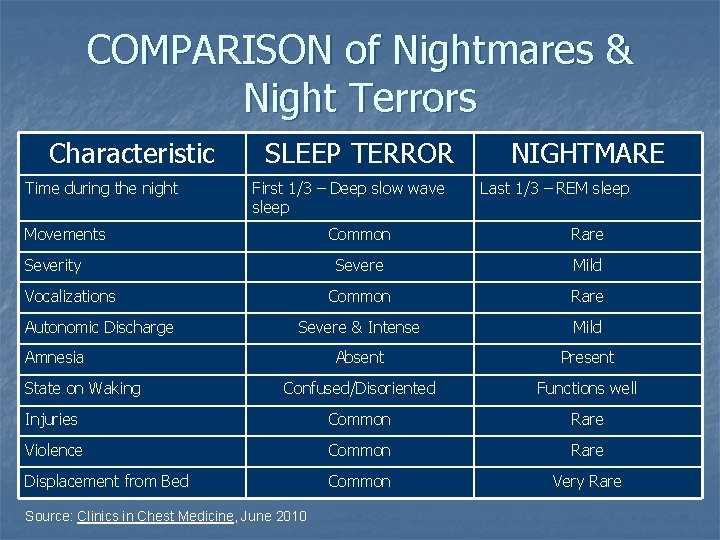
COMPARISON of Nightmares & Night Terrors Characteristic Time during the night SLEEP TERROR First 1/3 – Deep slow wave sleep Movements NIGHTMARE Last 1/3 – REM sleep Common Rare Severe Mild Common Rare Severe & Intense Mild Absent Present Confused/Disoriented Functions well Injuries Common Rare Violence Common Rare Displacement from Bed Common Very Rare Severity Vocalizations Autonomic Discharge Amnesia State on Waking Source: Clinics in Chest Medicine, June 2010

Criminal Cases – Sleep Terrors and Sleepwalking n A man dreamt that he was being attacked, n n Sleeping man saw vivid image of soldiers attacking his daughter n n “defended” himself, stabbing another man to death Left house, grabbed an axe, entered daughter’s room, “defended her” by hitting her twice, killing her While sleeping around a camp fire, man dreamt he was being burned n Man jumped up, grabbed an axe, killing another man sleeping nearby

Sleep Violence & Forensics n n Criminal behavior can occur while sleeping Criminal intent cannot occur while sleeping The brain-mind sleep state is incompatible with wakeful intent, for any behavior Sleep Violence: non-culpable behavior

Medical-Legal Guidelines for Helping Establish the Role of an Underlying Sleep Disorder in a Violent Act Journal of Forensic Sciences 1990; 35: 413 -32 Introduction n Guidelines, NOT rigid criteria Some striking exceptions found in innocent cases n n n e. g. Kenneth Parks case (1988) in Toronto n n Long, complex SW episode Guidelines 1. Presence of Underlying Sleep Disorder n n Solid evidence supporting the diagnosis Previous occurrence of similar episode

Guidelines Cont. 2. Characteristics of the Act n n n 3. On Return to Consciousness n n 4. Occurs on awakening or immediately after falling asleep Abrupt onset and brief duration Impulsive, senseless, no apparent motivation Lack of awareness of the victim during event Victim coincidentally present – may have been the arousal stimulus Perplexity, horror, no attempt to escape or to cover up the action Amnesia (partial or complete) for the event Presence of Precipitating Factors n n Attempts to awaken the subject Intake of sedative or hypnotic drugs Prior sleep deprivation Alcohol or drug intoxication disallows use of legal parasomnia defense

TREATMENT OF PARASOMNIAS n n n Safety of the environment maximized Sharp objects should be removed from bedside area Bed should not be placed near window

TREATMENT OF RBD n n n Clonazepam 0. 25 mg to 2 mg at bedtime up to 4 mg if needed 87% to 90% response rate usually no dose tolerance seems to suppress phasic motor activity rather than restore REM atonia No double blind studies given injury risk

TREATMENT OF RBD n Melatonin 3 to 15 mg co-therapy with clonazepam n n Pramipexole effective 63 -89% n n n n 0. 125 -4 mg ACE inhibitors n n About 50% reduction in REM atonia Effective in some cases of idiopathic RBD Can also trigger RBD Clonadine (a potent supressor of REM sleep) Desipramine/Imipramine (TCAs may aggravate RBD or trigger RBD) Peroxetine (in Japanese patients) MAOIs, Carbamazepine, Gabapentin, Zopiclone, Temazepam, Sodium Oxybate Immunosuppresive Therapy n Immunoglobulin + Corticosteroid for more than one year induced complete resolution of RBD with remission of associated autoimmune limbic enchephalitis (in 3 patients)(failed in 2)

NIGHT TERRORS!!!

TREATMENT OF: CONFUSIONAL AROUSALS, SLEEP WALKING & SLEEP TERRORS n n n n n Prevalence: 1 -4% in USA Asses severity Eliminate any presumed inducing medication Treat any comorbid sleep disorders Use bedroom dual alarm (inexpensive) Reassurance Avoid irregular sleep schedule Proper management of stress Pharmacotherapy n n n Violent/injurious behavior Main stay: benzodiazapines (clonazapam 0. 5 -1. 0 mg)(alprazolam 0. 251. 0 mg bedtime) Anti-depressant medication with seratolinergic activity (TCA and SSRI common). Eg. Imipramine and Peroxitine (and SSRIs in general) uniquely effective for sleep terrors Hypnotherapy: Conflicting Reports

TREATMENT OF SEXOMNIA n n n Treat comorbid condition (eg. OSA) Benzodiazapines (eg. Clonazapam) SSRIs (escitalopram 10 mg daily)

TREATMENT OF SRED n n n n CPAP therapy effective in SRED with OSA Benzodiazapines typically ineffective as monotherapy Dopaminergics: effective eliminated nocturnal eating associated with RLS and PLMD Anticonvulsants SSRIs Topiramate: positive results in 4 patients with nocturnal eating Discontinue offending medication

SUMMARY n n n Parasomnia is comprised of a set of sleep disorders generally amiable to effective and safe therapy (usually pharmacologic) This is usually gratifying to the treating physician Complications of parasomnias may be significant including sleep disruption, injuries, various health and psychosocial consequences Association with other sleep disorders not uncommon especially OSA, RLS, narcolepsy. When treated, may resolve SRED There is increasing awareness of medication induced or aggravated parasomnias such as RBD and SRED and sexomnia. Eliminating the offending agent must be carefully considered
- Slides: 80