Pap smears and Cultures Maria Horvat MD FACOG

























- Slides: 37

Pap smears and Cultures Maria Horvat, MD, FACOG

Objectives Know how and when to perform Pap smear Know how and when to perform cultures

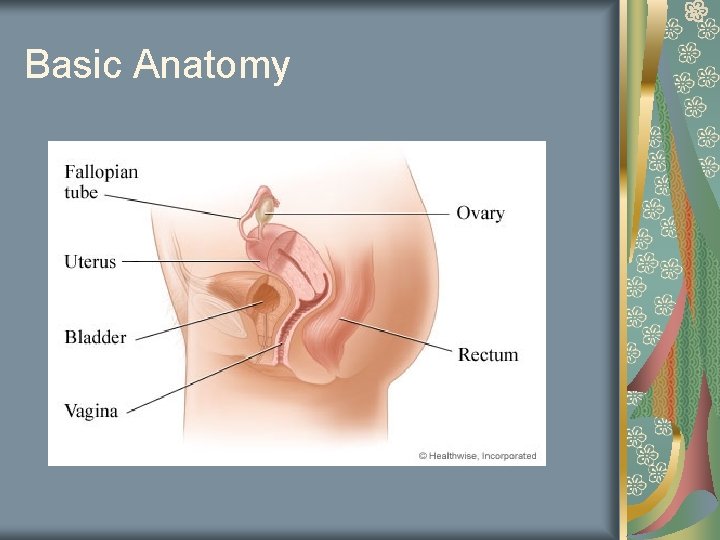
Basic Anatomy

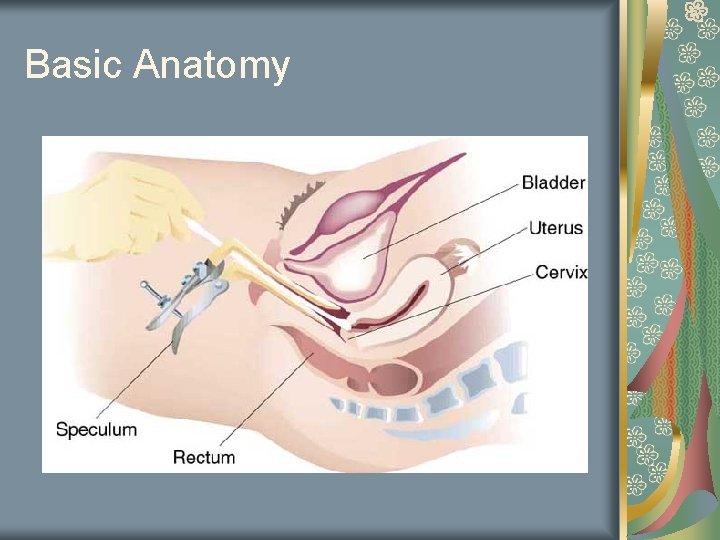
Basic Anatomy

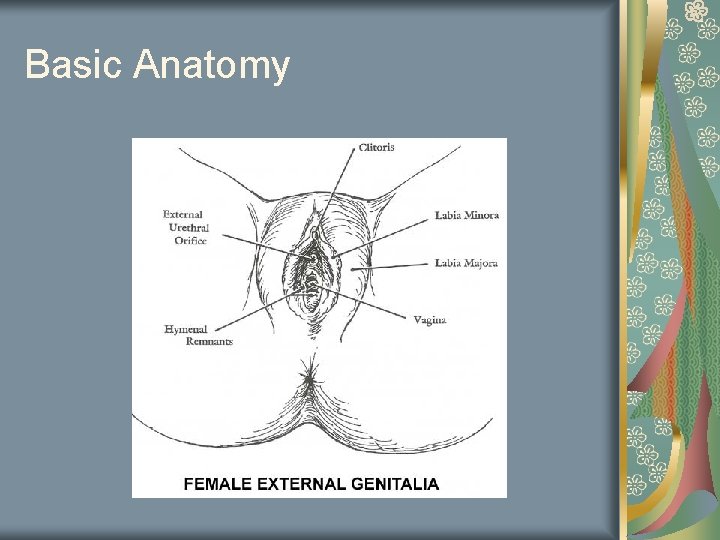
Basic Anatomy

The Basics Graves Speculum Pederson Speculum Pediatric Speculum

Pelvic Exam Note Vulva: Skin discoloration Erythema Labia normal or fused Scarring Nodularity Masses Inguinal lymph nodes Bartholins glands

Terminology used to describe: Cervix Discharge – note color, amount, odor Multiparous vs nulliparous Lesions – note size, location Vulva Color - normal or erythmatous Lesions – size, location, macerated, ulcerated, crusted, clustered

To perform Pap: Pick appropriate speculum Warm speculum with water Neutral touch on inner thigh Introduce speculum Note color, odor, amount of discharge Wipe away excess mucous Perform Pap Perform cultures

Tips: Correct positioning Have Pap and cultures ready Correct speculum size Medical assistant chaperone especially for males Litmus ph paper ready

Thin prep: Liquid based More effective in detecting LSIL’s and more severe lesions Use spatula and brush Conventional Pap Slide Must be fixed in timely manner Sensitivity 50%

Current recommendations on Pap and cultures 1 st Pap within 3 years of 1 st sexual intercourse By the age of 21 if no sexual activity Annual Pap when women are into their 20’s Pap and Gonorrhea/Chlamydia culture for sexually active females until age 2 At age 30 if you have 3 consecutive normal pap tests or recent pap and HPV is negative – can space out to q 2 -3 years

Recommendations are always changing ACS APGO (Association of Professors of Gynecology and Obstetrics) ACOG American college of Physicians

There always variations Post-menopause: Some guidelines require – no pap ACOG still advocates periodic pap q 3 -5 years Patient has had a hysterectomy If for benign reason pap may be performed q 35 years Yearly if: Cervix present History of abnormal paps History of gyne cancer History of DES exposure History of cervical cancer Smoking (increases chances of vaginal cancer)

Risk factors for cervical dysplasia Sexual activity at early age Multiple partners History of abnormal pap’s Smoking History of STD’s Immune status (HIV, chemotherapy) HPV infection Alcoholism Poor diet

Remember! Any obvious lesion needs to be biopsied!

Infection Herpes Trichomonas Gonorrhea Chlamydia Bacterial Vaginosis Yeast Vaginitis Syphilis

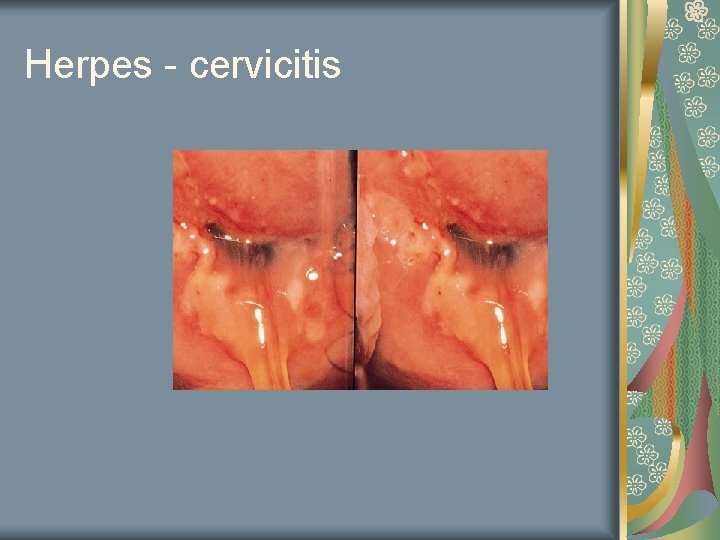
Herpes Painful vulvar lesion Clusters with a superficial crust 10 – 20% cultures give false negative 22% of adults have antibodies Other associated symptoms Pain, fever, headaches, malaise, itching, tingling Tends to be recurrent

Herpes - cervicitis

Herpes - vulva

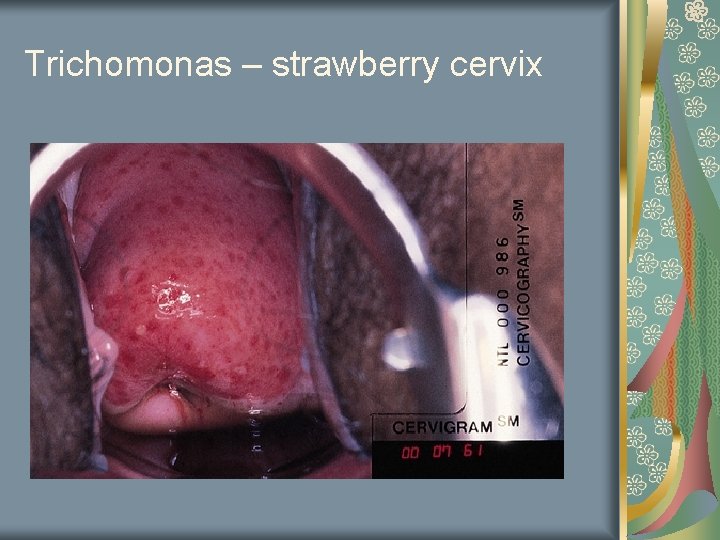
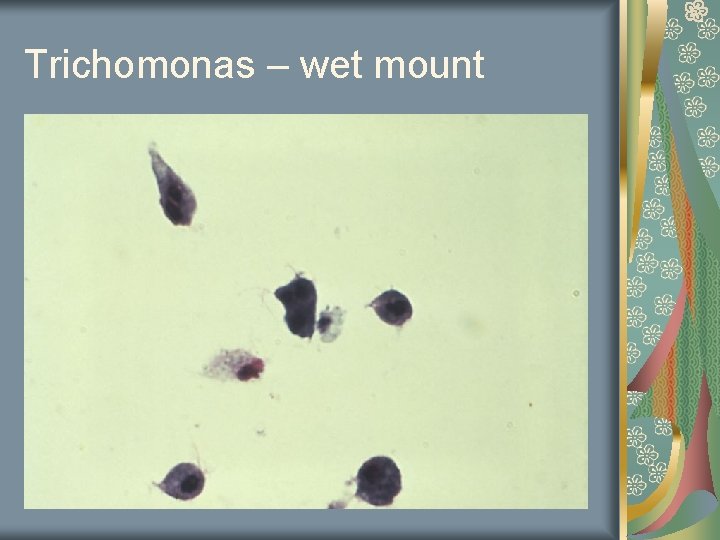
Trichomonas Most common curable STD in young women Flagellated protozoans under normal saline wet mount slide “frothy” discharge Erythematous patches on ectocervix Discharge may be yellow and copious “strawberry cervix” ph 5 -7 Incubation 3 -28 days

Trichomonas – strawberry cervix

Trichomonas – wet mount

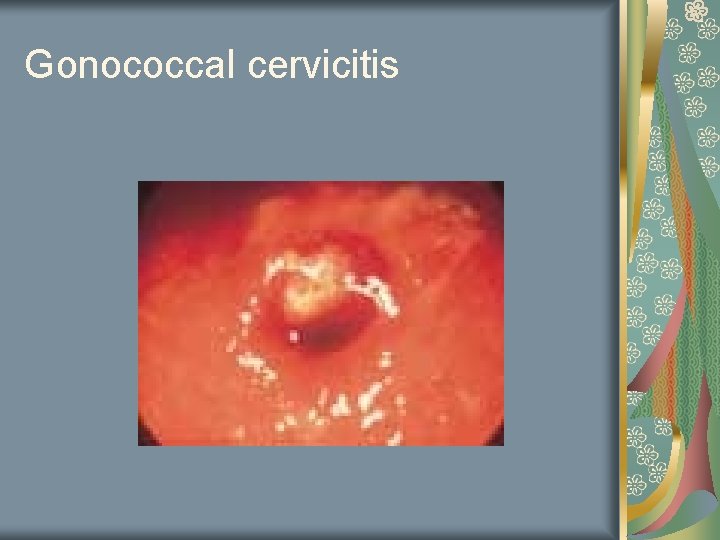
Gonorrhea Profuse discharge, odorless, creamy white to yellow Gram negative diplococci Culture to diagnose (DNA probe) Numerous WBC’s 40% of persons with gonorrhea also have Chlamydia

Gonococcal cervicitis

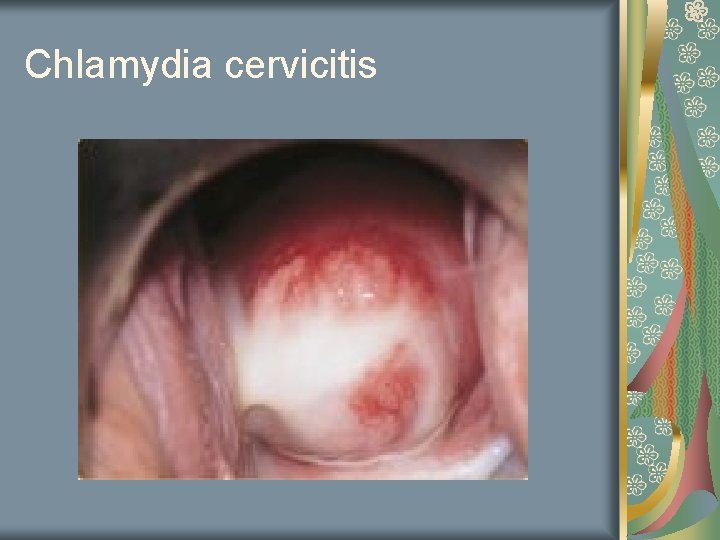
Chlamydia Mucopurulent discharge 60% Intracellular parasite Most prevalent venereal disease in US Post coital bleeding 8% are asymptomatic

Chlamydia cervicitis

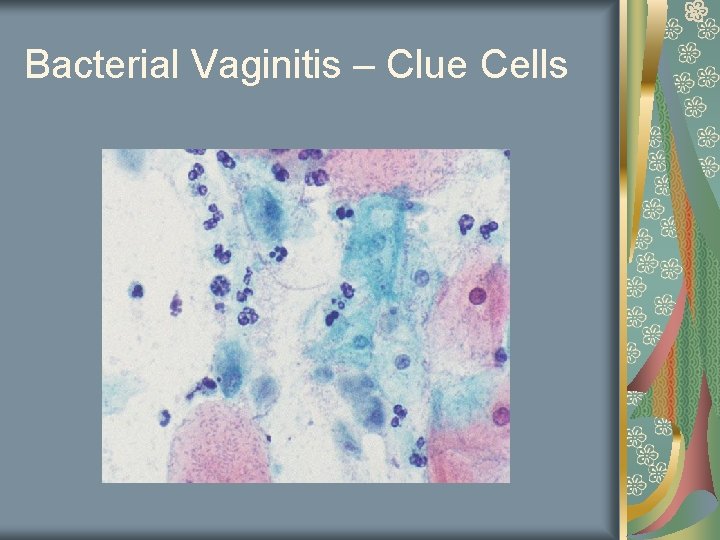
Bacterial Vaginitis Patient complains of fishy odor or general vaginal discomfort Diagnose by saline wet mount ph>4. 5 Positive whiff test Clue cells (bacteria cling to edge of epithelial cells) Caused by decreased hydrogen peroxide producing lactobacilli and increased gardnerella

Bacterial Vaginitis – Clue Cells

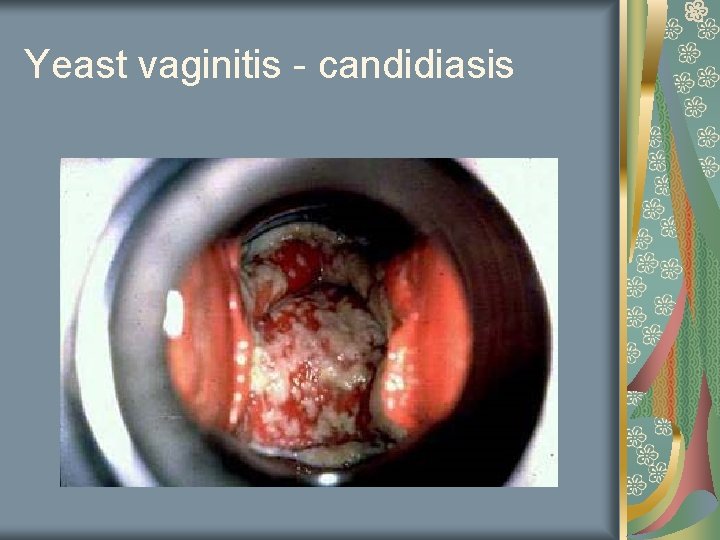
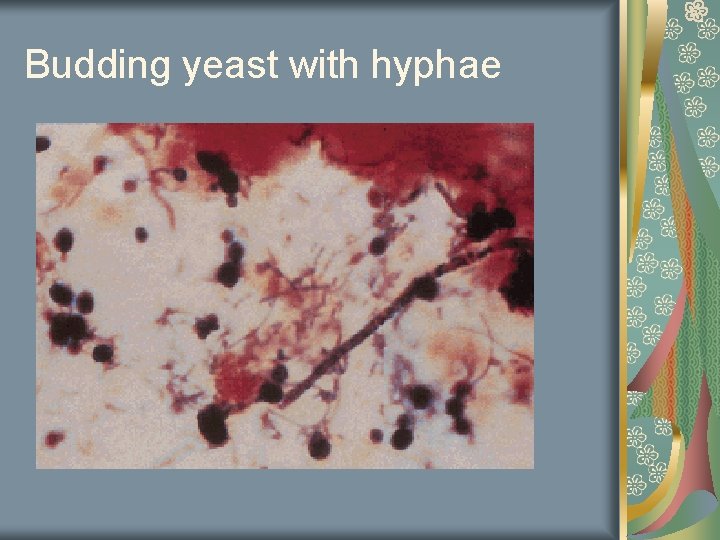
Yeast Vaginitis KOH slide Budding yeast with hyphea Erythmatous vagina White discharge

Yeast vaginitis - candidiasis

Budding yeast with hyphae

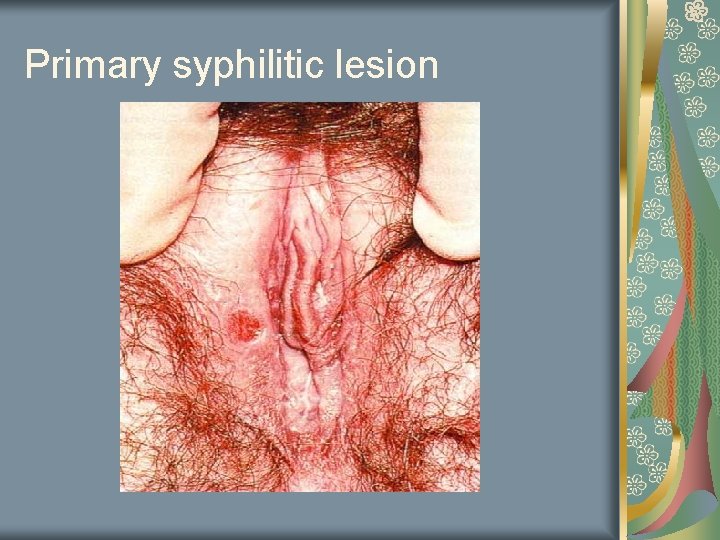
Syphilis Ulcer develops 2 -6 weeks after initial infection Papule, then it ulcerates to a 1 cm lesion Diagnosed by dark field microscopy Specimen taken from scraped and oozing syphilitic skin lesion organism: treponema pallidum, corkscrew in shape

Primary syphilitic lesion

Other recommendations Pap test as previously discussed Annual breast exam Baseline mammogram at age 35 -40 Annual mammogram starting at age 40 Annual pelvic exam Annual rectal, heme-occult starting at age 50 Dexa screen q 2 -3 years Colonoscopy q 10 years starting at age 50

References www. chups. jussieu. fr/polys/gyneco/sy philis. jpg www. kcom. edu www. usc. edu www. images. md commons. wikimedia. org/wiki/Imag e: Trichomonas
