PANCREATIC DISEASES BY Dr AZZA EMAM What is

PANCREATIC DISEASES BY Dr AZZA EMAM

What is the pancreas? • The pancreas is a spongy, tube-shaped organ about 6 inches long. It is located in the back of the abdomen, behind the stomach. The head of the pancreas is on the right side of the abdomen. It is connected to the duodenum, The narrow end of the pancreas, called the tail, extends to the left side of the body. • The pancreas secretes digestive enzymes into the small intestine through a tube called the pancreatic duct. These enzymes help digest fats, proteins, and carbohydrates in food. The pancreas also releases the hormones insulin and glucagon into the bloodstream. These hormones help the body use the glucose it takes from food for energy.
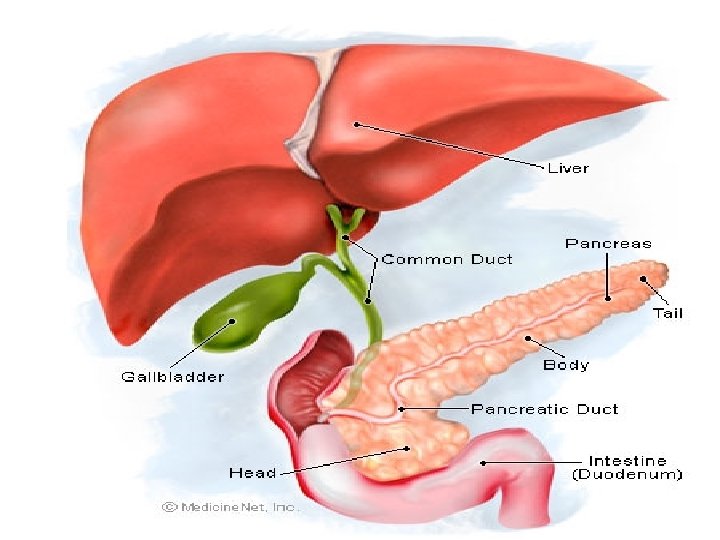

What is pancreatitis? • Pancreatitis is an inflammation of the pancreas. • As pancreatic juices are made, they flow into the main pancreatic duct. This duct joins the common bile duct, which connects the pancreas to the liver and the gallbladder. The common bile duct, which carries bile (a fluid that helps digest fat), connects to the small intestine near the stomach. • Normally, digestive enzymes do not become active until they reach the small intestine, where they begin digesting food. But if these enzymes become active inside the pancreas, they start "digesting" the pancreas itself.

• Acute pancreatitis occurs suddenly and lasts for a short period of time and usually resolves. • Chronic pancreatitis does not resolve itself and results in a slow destruction of the pancreas. Either form can be mild, moderate or severe

What are the causes of acute pancreatitis? • Acute pancreatitis occurs more often in men than women. • Acute pancreatitis is usually caused by gallstones or by drinking too much alcohol.

What are the symptoms of acute pancreatitis? • • • Pain in the upper abdomen. swollen and tender abdomen. nausea vomiting fever rapid pulse

• Severe cases may cause dehydration and low blood pressure. The heart, lungs, or kidneys may fail. If bleeding occurs in the pancreas, shock and sometimes even death follow.

How is acute pancreatitis diagnosed? • Medical history and physical exam, • Elevated serum amylase and lipase(3 time>normal). Amylase and lipase are digestive enzymes formed in the pancreas. • Changes in blood levels of glucose, calcium, magnesium, sodium, potassium, and bicarbonate. • An abdominal ultrasound to look for gallstones and a CAT scan to look for inflammation or destruction of the pancreas. CAT scans are also useful in locating pseudocysts.

How is acute pancreatitis treated? • Acute pancreatitis usually improves on its own. • Treatment, in general, is designed to support vital bodily functions and prevent complications. • In severe cases, a person may require intravenous feeding for 3 to 6 weeks while the pancreas slowly heals. This process is called total parenteral nutrition. However, for mild cases of the disease, total parenteral nutrition offers no benefit.

• If pancreatic pseudocysts occur and are considered large enough to interfere with the pancreas's healing, (drainage or surgically removal). • Before leaving the hospital, a person will be advised not to drink alcohol and not to eat large meals. After all signs of acute pancreatitis are gone, the doctor will try to decide what caused it in order to prevent future attacks.

Complications • Hypoxia, which means that cells and tissues are not receiving enough oxygen. • Treatment of hypoxia is by giving oxygen through a face mask. Or even require a ventilator. • Severe vomiting and needs to have a tube placed in the stomach to remove fluid and air. In mild cases, a person may not eat for 3 or 4 days and instead may receive fluids and pain relievers through an intravenous line. • If an infection develops, antibiotics. will be prescribed. Surgery may be needed for extensive infections. Surgery may also be necessary to find the source of bleeding, to rule out problems that resemble pancreatitis, or to remove severely damaged pancreatic tissue. • Acute pancreatitis can sometimes cause kidney failure and dialysis will be needed.

What about gallstones and pancreatitis? • Gallstones can cause pancreatitis and they usually require surgical removal. • When gallstone surgery can be scheduled depends on how severe the pancreatitis is. If the pancreatitis is mild, gallstone surgery may proceed within about a week. More severe cases may mean gallstone surgery is delayed for a month or more.

What is chronic pancreatitis? • If injury to the pancreas continues, chronic pancreatitis may develop. Chronic pancreatitis occurs when digestive enzymes attack and destroy the pancreas and nearby tissues, causing scarring and pain. The usual cause of chronic pancreatitis is many years of alcohol abuse, but the chronic form may also be triggered by only one acute attack, especially if the pancreatic ducts are damaged. The damaged ducts cause the pancreas to become inflamed, tissue to be destroyed, and scar tissue to develop. • While common, alcoholism is not the only cause of chronic pancreatitis. The main causes of chronic pancreatitis are

• Blocked or narrowed pancreatic duct because of trauma or pseudocysts • In up to 70 percent of adult patients, chronic pancreatitis appears to be caused by alcoholism. This form is more common in men than in women and often develops between the ages of 30 and 40. • Hereditary pancreatitis usually begins in childhood but may not be diagnosed for several years. A person with hereditary pancreatitis usually has the typical symptoms that come and go over time. Episodes last from 2 days to 2 weeks. A determining factor in the diagnosis of hereditary pancreatitis more than one generation. Treatment for individual attacks is usually the same as it is for acute pancreatitis. Any pain or nutrition problems are treated just as they are for acute pancreatitis. Surgery can often ease pain and help manage complications. • Other causes of chronic pancreatitis are • congenital conditions such as pancreas divisum • cystic fibrosis • high levels of calcium in the blood (hypercalcemia) • high levels of blood fats (hyperlipidemia or hypertriglyceridemia) • some drugs • certain autoimmune conditions

What are the symptoms of chronic pancreatitis? • Most people with chronic pancreatitis have abdominal pain, • Abdominal pain goes away as the condition advances, probably because the pancreas is no longer making digestive enzymes. Other symptoms include nausea, vomiting, weight loss, and fatty stools. • The weight loss occurs because the body does not secrete enough pancreatic enzymes to break down food, so nutrients are not absorbed normally. Poor digestion leads to excretion of fat, protein, and sugar into the stool. • If the insulin-producing cells of the pancreas (islet cells) have been damaged, diabetes may also develop at this stage.

How is chronic pancreatitis diagnosed? • Diagnosis may be difficult. • Pancreatic function tests help to decide whether the pancreas is still making enough digestive enzymes. • Ultrasonic imaging, endoscopic retrograde cholangiopancreatography (ERCP), and CAT scans, may show calcification of the pancreas, in which tissue hardens from deposits of insoluble calcium salts. • In more advanced stages of the disease, when diabetes and malabsorption occur, a number of blood, urine, and stool tests can be used.

How is chronic pancreatitis treated? • Relieving pain is the first step in treating chronic pancreatitis. The next step is to plan a diet that is high in carbohydrates and low in fat. • Pancreatic enzymes may be prescribed to take with meals if the pancreas does not secrete enough of its own. The enzymes should be taken with every meal to help the body digest food and regain some weight. Sometimes insulin or other drugs are needed to control blood glucose. • In some cases, surgery is needed to relieve pain. The surgery may involve draining an enlarged pancreatic duct or removing part of the pancreas. • For fewer and milder attacks, people with pancreatitis must stop drinking alcohol, stick to their prescribed diet, and take the proper medications.

What is cancer? • Cancer is a group of diseases. More than 100 different types of cancer are known, They all have one thing in common: abnormal cells grow and destroy body tissue. • Healthy cells that make up the body's tissues grow, divide, and replace themselves in an orderly way. This process keeps the body in good repair. Sometimes, however, some cells lose the ability to control their growth. They grow too rapidly and without any order. Too much tissue is made, and tumors are formed.

Tumors can be benign or malignant. • Benign tumors are not cancer. They do not spread to other parts of the body and are seldom a threat to life. Often, benign tumors can be removed by surgery, and they are not likely to return. • Malignant tumors are cancer. They can invade and destroy nearby healthy tissues and organs. Cancer cells also can break away from the tumor and spread to other parts of the body. The spread of cancer is called metastasis.

• Cancer that starts in the pancreas is called pancreatic cancer. When pancreatic cancer spreads, it usually travels through the lymphatic system. The lymphatic system includes a network of thin tubes that branch, like blood vessels, into tissues all over the body. Cancer cells are carried through these vessels by lymph, a colorless, watery fluid that carries cells that fight infection. Along the network of lymphatic vessels are groups of small, bean-shaped organs called lymph nodes. Surgeons often remove lymph nodes near the pancreas to learn whether they contain cancer cells. • Cancer cells can also be carried through the bloodstream to the liver, lungs, bone, or other organs. Pancreatic cancer that spreads to other organs is called metastatic pancreatic cancer.

Symptoms and Diagnosis • Cancer of the pancreas is hard to find (diagnose) because the organ is hidden behind other organs and is not readily felt in routine exams. The signs of pancreatic cancer are like many other illnesses, and there may be no signs in the early stages. • : • nausea • digestive problems or loss of appetite • unexplained weight loss • pain in the upper or middle of the abdomen or back • yellowing of the skin (jaundice) • Symptoms of cancer of the endocrine pancreas also include diarrhea, fatigue, faintness, and unexplained weight gain. A person who experiences any of these symptoms should see a doctor.

When symptoms do occur, they may include the following: • Pain (sometimes severe pain in the upper abdomen that can penetrate to the back). • Jaundice. • Nausea, loss of appetite. • Itching. • Weight loss. • Dizziness, weakness, diarrhea, chills, or muscle spasms. • Fatigue, and depression.

Pancreatic Cancer: Who's at Risk? – Age -- Most pancreatic cancers occur in people over the age of 60. – Smoking – Diabetes -- Pancreatic cancer occurs more often in people who have diabetes than in people who do not. – Being male -– Being African American -- African Americans are more likely than Asians, Hispanics, or whites to get pancreatic cancer. – Family history -- The risk for developing pancreatic cancer triples if a person's mother, father, sister, or brother had the disease. Also, a family history of colon or ovarian cancer increases the risk of pancreatic cancer. – Chronic pancreatitis -- may increase the risk of pancreatic cancer.

Diagnosis • If a patient has symptoms that suggest pancreatic cancer, a number of procedures, including one or more of the following will be doen: – Physical exam -– Lab tests -- to check for bilirubin and other substances. . – CT scan (Computed tomography) – – Ultrasonography --

The ultrasound procedure may use an external or internal device, or both types: • Transabdominal ultrasound. • EUS (Endoscopic ultrasound). ERCP (endoscopic retrograde cholangiopancreatography)-can show whether the ducts are narrowed or blocked by a tumor or other condition.

– PTC (percutaneous transhepatic cholangiography) -- A dye is injected through a thin needle inserted through the skin into the liver. The dye makes the bile ducts show up on x-ray pictures. From the pictures, the doctor can tell whethere is a blockage from a tumor or other condition. – Biopsy -- One way is by fine-needle aspiration, useing x-ray or ultrasound to guide the needle. – During EUS or ERCP. – Another way is to open the abdomen during an operation.

Staging • Staging is a careful attempt to find out the size of the tumor in the pancreas, whether the cancer has spread, and if so, to what parts of the body. • Tests may include blood tests, a CT scan, ultrasonography, laparoscopy, or angiography. The test results will help in deciding appropriate treatment.

Pancreatic Cancer Treatment Cancer of the pancreas is very hard to control with current treatments. For that reason, many doctors encourage patients with this disease to consider taking part in a clinical trial. • At this time, pancreatic cancer can be cured only when it is found at an early stage, before it has spread.

Getting a Second Opinion • Before starting treatment, a patient may want a second opinion about the diagnosis and the treatment plan.

Preparing for Treatment • The doctor can describe treatment choices and discuss the results expected with each pancreatic cancer treatment option. The doctor and patient can work together to develop a treatment plan that fits the patient's needs. • Treatment depends on where in the pancreas the tumor started and whether the disease has spread. When planning treatment, the doctor also considers other factors, including the patient's age and general health.

These are some questions a person may want to ask the doctor before treatment begins: – What is the diagnosis? – Where in the pancreas did the cancer start? – Is there any evidence the cancer has spread? What is the stage of the disease? – Do I need any more tests to check whether the disease has spread? – What are my treatment choices? Which do you recommend for me? Why? – What are the expected benefits of each kind of treatment? – What are the risks and possible side effects of each treatment? – What is the treatment likely to cost? Is this treatment covered by my insurance plan? – How will treatment affect my normal activities? • Would a clinical trial (research study) be appropriate for me?

Methods of Pancreatic Cancer Treatment • Surgery may be used alone or in combination with radiation therapy and chemotherapy. • The surgeon may remove all or part of the pancreas. The extent of surgery depends on the location and size of the tumor, the stage of the disease, and the patient's general health. – Whipple procedure: If the tumor is in the head (the widest part) of the pancreas, the surgeon removes the head of the pancreas and part of the small intestine, bile duct, and stomach. The surgeon may also remove other nearby tissues. – Distal pancreatectomy: The surgeon removes the body and tail of the pancreas if the tumor is in either of these parts. The surgeon also removes the spleen. – Total pancreatectomy: The surgeon removes the entire pancreas, part of the small intestine, a portion of the stomach, the common bile duct, the gallbladder, the spleen, and nearby lymph nodes.

• Radiation therapy (also called radiotherapy) uses high-energy rays to kill cancer cells. Radiation therapy may be given alone, or with surgery, chemotherapy, or both. • Radiation therapy is local therapy. It affects cancer cells only in the treated area. For radiation therapy, patients go to the hospital or clinic, often 5 days a week for several weeks.
• Chemotherapy is the use of drugs to kill cancer cells. Doctors also give chemotherapy to help reduce pain and other problems caused by pancreatic cancer. It may be given alone, with radiation, or with surgery and radiation. • Chemotherapy is systemic therapy.

Pain Control • Pain is a common problem for people with pancreatic cancer. The tumor can cause pain by pressing against nerves and other organs. – Pain medicine -- Medicines often can relieve pain. (These medicines may make people drowsy and constipated, but resting and taking laxatives can help. ) – Radiation -- High-energy rays can help relieve pain by shrinking the tumor. – Nerve block – by injecting alcohol into the area around certain nerves in the abdomen to block the feeling of pain. – Surgery -- The surgeon may cut certain nerves to block pain.

Nutrition • People with pancreatic cancer may not feel like eating, especially if they are uncomfortable or tired. Also, the side effects of treatment such as poor appetite, nausea, or vomiting can make eating difficult. Foods may taste different. Nevertheless, patients should try to get enough calories and protein to control weight loss, maintain strength, and promote healing. Also, eating well often helps people with cancer feel better and have more energy. • Careful planning and checkups are important. Cancer of the pancreas and its treatment may make it hard for patients to digest food and maintain the proper blood sugar level. The doctor will check the patient for weight loss, weakness, and lack of energy. Patients may need to take medicines to replace the enzymes and hormones made by the pancreas. The doctor will watch the patient closely and adjust the doses of these medicines.

Follow up Care • Followup care after treatment for pancreatic cancer is an important part of the overall treatment plan. Patients should not hesitate to discuss follow up with their doctor. Regular checkups ensure that any changes in health are noticed. Any problem that develops can be found and treated. Checkups may include a physical exam, laboratory tests, and imaging procedures.

Support for People with Pancreatic Cancer • Living with a serious disease such as pancreatic cancer is not easy. Some people find they need help coping with the emotional and practical aspects of their disease. Support groups can help. • Doctors, nurses, and other members of the health care team can answer questions about treatment, diet, working, or other matters. Meeting with a social worker, counselor, or member of the clergy can be helpful to those who want to talk about their feelings or discuss their concerns. Often, a social worker can suggest resources for financial aid, transportation, home care, emotional support, or other services.

The Promise of Cancer Research • In trials with people who have pancreatic cancer, doctors are studying new drugs, new combinations of chemotherapy, and combinations of chemotherapy and radiation before and after surgery. • Biological therapy is also under investigation. Scientists are studying several cancer vaccines to help the immune system fight cancer. Other studies use monoclonal antibodies to slow or stop the growth of cancer.

- Slides: 41