Pancreas diabetes eljka Kuter Mentor A mega Horvat

Pancreas & diabetes Željka Kušter Mentor: A. Žmegač Horvat

Anatomy • Retroperitoneal abdominal organ • Exocrine and endocrine cells lobules ducts pancreatic duct
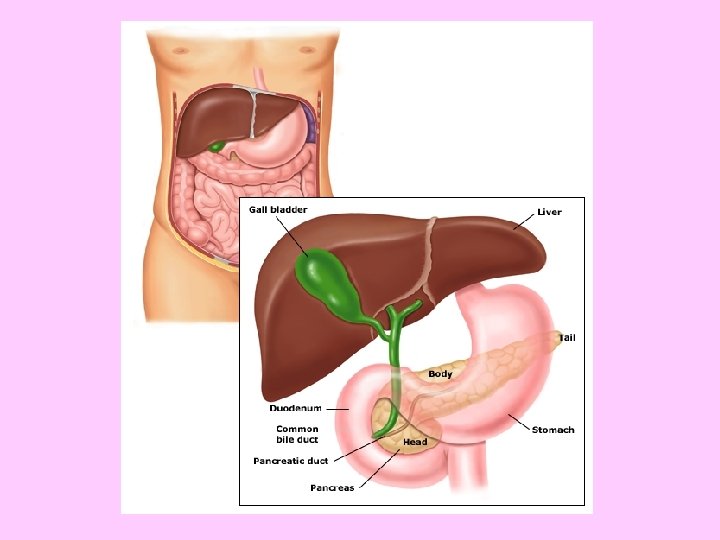

Exocrine function • Acinar cells - exocrine cells of the pancreas that produce and transport digestive enzymes • Amylase, lipase, phospholipase, proteases (trypsinogen, chymotrypsinogen)

Endocrine function • Islets of Langerhans - endocrine cells of the pancreas that produce and secrete hormones into the bloodstream • Glucagon - Alpha cells (A cells) - raises the level of glucose (sugar) in the blood • Insulin - Beta cells (B cells) - stimulates cells to use glucose • Somatostatin - Delta cells (D cells) - regulate the secretion of glucagons and insulin
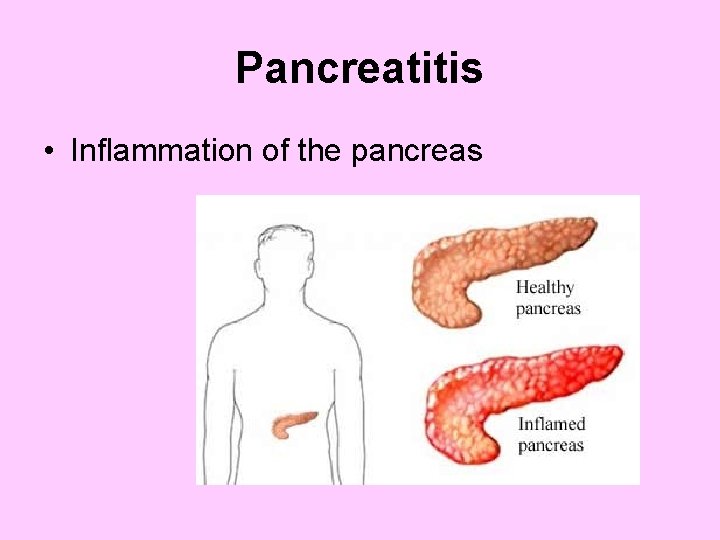
Pancreatitis • Inflammation of the pancreas

Acute pancreatitis • Pancreas suddenly becomes inflamed • Causes: Gallstones Ethanol Trauma Steroids Mumps Autoimmune Scorpion venom Hyperlipidaemia, hypothermia ↑Ca 2+ ERCP Drugs
Symptoms • • • epigastric and central abdominal pain vomiting and nausea swollen and tender abdomen fever dehydration and low blood pressure Diagnosis • medical history and physical exam • blood test: ↑ amylase, lipase • abdominal ultrasound, EUS, CT scan

Treatment • • nothing to eat or drink intravenous fluids analgesia ERCP and gallstone removal Complications • shock, ARDS, renal failure, DIC, sepsis, ↓Ca 2+ • pancreatic necrosis, pseudocyst, abscesses, bleeding, thrombosis

Chronic pancreatitis • inflammation of the pancreas - gets worse over time and leads to permanent damage Causes: many years of alcohol use hereditary disorders of the pancreas cystic fibrosis haemochromatosis autoimmune conditions

Symptoms • • nausea and vomiting weight loss diarrhea steatorrhea Diagnosis • medical history and physical exam • abdominal ultrasound, CT scan, MRCP, ERCP

Treatment • drugs - analgesia, lipase, fat-soluble vitamins • diet • surgery – pancreatectomy pancreaticojejunostomy Complications • pseudocyst, diabetes, biliary obstruction, local arterial aneurysm, splenic vein thrombosis


Diabetes • increased level of glucose in the blood (normal blood glucose level 3. 5 -6. 0 mmol/l) Type 1 ( insulin-dependent DM, IDDM) • destruction of insulin-secreting pancreatic β cells • juvenile diabetes • patient always needs insulin

Type 2 (non-insulin dependent DM, NIDDM) • insulin resistance • Β cell dysfunction, ↓insulin secretion Causes of insulin resistance: • metabolic syndrome (central obesity, hyperglycaemia, hypertension, ↓HDL cholesterol, ↑triglycerides) • • renal failure pregnancy cystic fibrosis polycystic ovarian syndrome
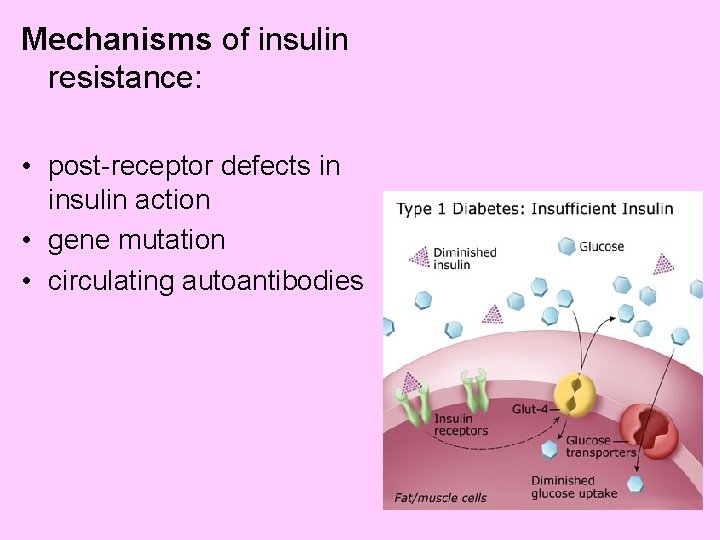
Mechanisms of insulin resistance: • post-receptor defects in insulin action • gene mutation • circulating autoantibodies

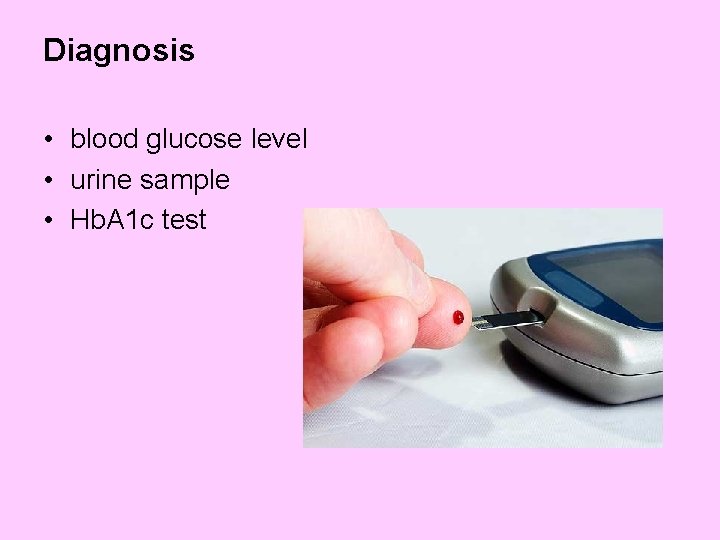
Diagnosis • blood glucose level • urine sample • Hb. A 1 c test
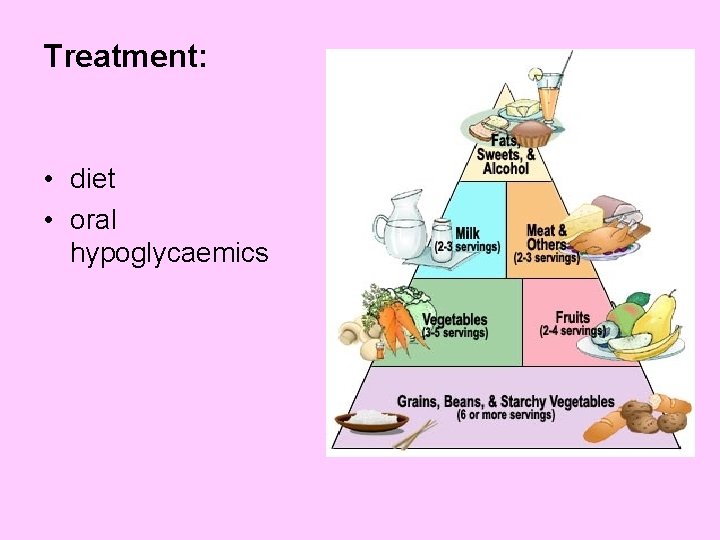
Treatment: • diet • oral hypoglycaemics
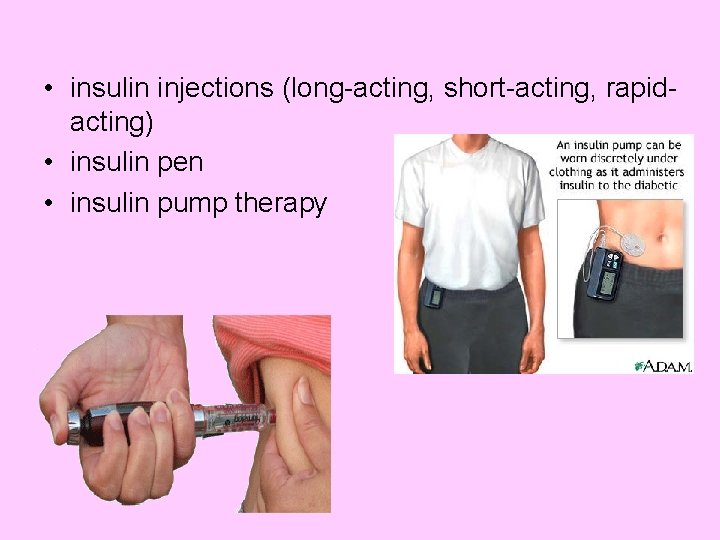
• insulin injections (long-acting, short-acting, rapidacting) • insulin pen • insulin pump therapy

Complications
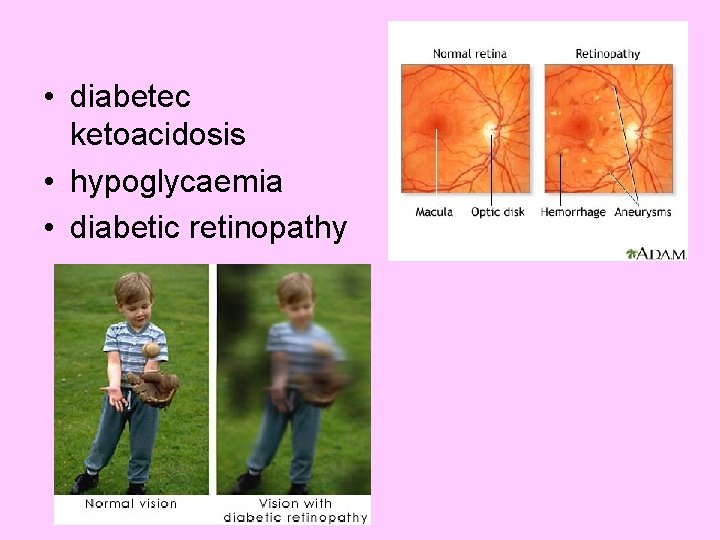
• diabetec ketoacidosis • hypoglycaemia • diabetic retinopathy
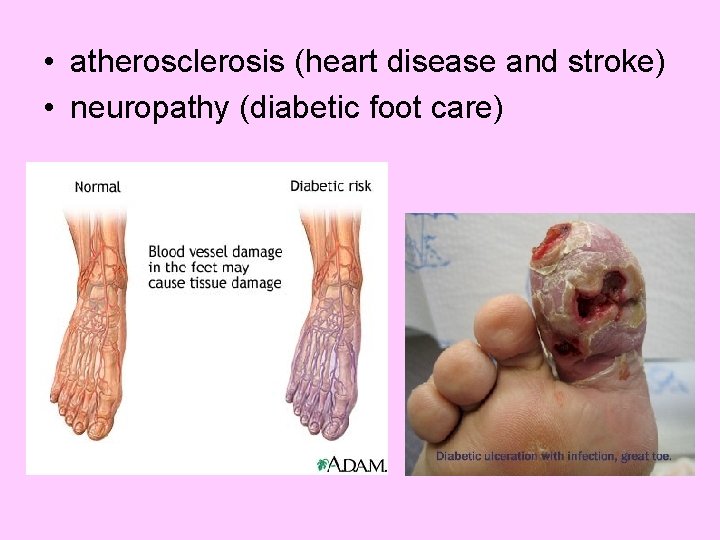
• atherosclerosis (heart disease and stroke) • neuropathy (diabetic foot care)

Diabetes risk factors • • • Age over 45 years Diabetes during a previous pregnancy Excess body weight Family history of diabetes Dyslipidaemia Hypertension Low activity level Metabolic syndrome Polycystic ovarian syndrome Acanthosis nigricans
- Slides: 24