Palliative Care Toolkit Pain management By Roshni Guerry

Palliative Care Toolkit: Pain management By Roshni Guerry, MD Supportive and Palliative Care Inpatient Medical Director

Objectives • Describe four classifications of opioids and their preferred indications • List which opioids are preferred for renal and liver patients • Describe the timeline for opioid withdrawal and how to manage symptoms • Develop a plan for tapering opioids when appropriate

“There is no pain that can not be made worse with inappropriate therapy. ”

Analgesics Classifications • Opioids are classified by their interaction with the opioid receptors. – pure agonist: morphine, hydromorphone (Dilaudid ®) oxycodone, codeine, meperidine, fentanyl, methadone – mixed agonist-antagonist: butorphanol (Stadol ®), pentazocine (Talwin ®), nalbuphine (Nubain ®), Buprenophine/naloxone(Suboxone ®) – partial agonist: buprenorphine – pure antagonist: naloxone, naltrexone

Agonist-Antagonists • Mixed Agonist-Antagonists – Claim to be less addicting—not substantiated – Will potentiate withdrawal in patients being treated with pure agonists—need to dose higher for first 72 hours then lower – Have an analgesic ceiling – Are psychotomimetic—can cause psychosis – Suboxone—need special DEA

Oral Opioids—Duration of Action A. Ultra short A. Short A. Long

A. Ultra short acting opioid • Fentanyl – Very potent (given IV, it has 50 -100 times the potency of morphine) – Transmucosal (buccal) delivery systems are available for breakthrough pain: • Actiq ® (Lozenge), Fentora TM (Buccal tablet) • Onset of analgesia within ~10 minutes; peak effect ~20 -40 mins; duration of analgesia 2 -3 h • NOTE: Should only be used in opioid tolerant patients by clinicians familiar with the pharmacology of transmucosal systems.

B. Oral Short Acting Opioids • Parenteral or Oral – morphine – hydromorphone (Dilaudid ®) – oxymorphone (Opana ®) – meperidine (Demerol ®) – codeine – fentanyl • Oral only – oxycodone (Percocet ® , Tylox ® 0) – hydrocodone (Vicodin ® Lortab ®, Lorcet ®)

Oral Short Acting Opioids • Oral dosing: – onset in 20 -30 min – peak effect in 60 -90 minutes – duration of effect 2 -4 hours (6 -8 hours for oxymorphone) – Can be dose escalated or re-administered every 2 -4 hours for poorly controlled pain

Combination Products

Opioid combination products • The following opioids are available as combination products with acetaminophen, aspirin, or ibuprofen – Codeine; hydrocodone; oxycodone; tramadol • Typically used for – Moderate, episodic (PRN) pain – Breakthrough pain in addition to a long-acting opioid (for moderate, and for some patients severe, pain). • Never prescribe more than one combination drug at any one time. • Keep acetaminophen dosing: < 4 grams/day for combination products

Which combination product? • Analgesic potency of combination meds – Aspirin < Codeine < Hydrocodone = Oxycodone • Toxicity: – All the combination products can cause opioid toxicities: nausea, sedation, constipation, etc. – There is little published data that supports the use of one product over another in terms of routine toxicity; – however … • Codeine is probably the most emetogenic opioid.

Tramadol (Ultram ®) • A synthetic analog of codeine • Analgesic effect roughly equivalent to Tylenol #3 ® – Efficacy variable; has an analgesic ceiling and maximum 24 hour dose of 400 mg • No anti-inflammatory effects • Side effects similar to opioids at high dose--nausea, confusion, dizziness, constipation • Does have abuse potential • Lowers seizure threshold

C. Long Acting Opioids • Oral – Extended-release morphine: • MS Contin® • Kadian® • Oramorph SR – ER oxycodone • Oxycontin® • Oxycodone SR – ER oxymorphone • Opana SR – Methadone (pain expert involvement recommended) ** CAN DOSE EXTENDED RELEASE Q 12 H or Q 8 H • Transdermal – Fentanyl Patch (Duragesic®)

KETAMINE • Ketamine is a dissociative amnestic – NMDA receptor antagonist • Benefits – Pain Relief – Minimal effect on ventilatory drive or blood pressure – Bronchodilation – Extremely Potent Anti-Depressant

Ketamine for who? For who not? • GOOD candidates: – with acute pain – Opioid Tolerant, Chronic Pain – Refractory Major Depression – Severe Lung Disease • POOR candidates – Intracranial trauma – previous psychotic illness – severe uncontrolled heart failure or severe hypertension

Downside of Ketamine Adverse Reactions – Dose dependent psychomimetic effects – Visual Hallucinations, vivid dreams, psychosis, dysphoria, frank psychosis – Increased Intracranial Pressure – Salivation • Treating Side Effects – Usually occur in the first 30 min – Sedation – Usually secondary to opioids – Dysphoria / Hallucinations – 10 -20% use benzos, antipsychotics, or discontinue infusion

Dosing Ketamine • Adults: – Recommended duration 24 -72 hrs – Ordering based on IDEAL Body Weight – 0. 1 -0. 2 mg/kg bolus and 0. 1 -0. 2 mg/kg/hr infusion
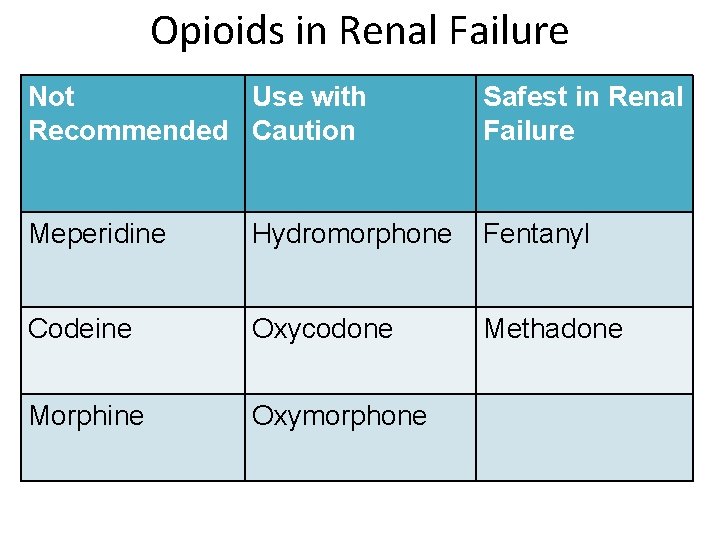
Opioids in Renal Failure Not Use with Recommended Caution Safest in Renal Failure Meperidine Hydromorphone Fentanyl Codeine Oxycodone Methadone Morphine Oxymorphone
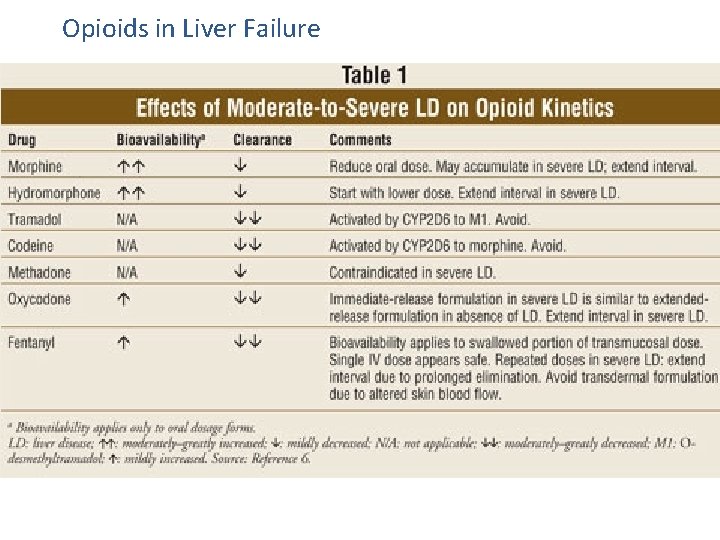
Opioids in Liver Failure

Assessing Sedation—PASERO SCALE

Treating Extreme Sedation with Naloxone (Narcan®) • In palliative care, naloxone is indicated when: – The goals of care such that reversing CNS depression is appropriate to patient’s goals – Patients have decreased respirations and decreased level of consciousness (arousal) • Adult dosing: – Administer naloxone— 1 amp (0. 4 mg) diluted in 9 cc saline —push 1 cc per minute until level of consciousness improves. Naloxone’s effects last only ~20 mins, so continued monitoring will be necessary after initially reviving the patient

Opioid Induced Hyperanalgesia • Proposed mechanisms: – Toxic effect of opioid metabolites? – Central sensitization due to activation of NMDA receptors? • Features – Increasing sensitive to painful stimuli – Worsening pain despite increasing opioids • PE exam – Allodynia, myoclonus, delirium, seizures • Therapies – Reduce of discontinue opioid, opioid rotation, use ketamine infusion

Withdrawal • Early symptoms – Agitation, anxiety, muscle aches, increased tearing, insomnia, runny nose, sweating, yawning • Late symptoms – Abdominal cramping, diarrhea, dilated pupils, goose bumps, nausea, vomiting • Withdrawal is very uncomfortable but NOT life threatening

Withdrawal • Onset: – Varies – 6 -12 hours for short acting drug – 72 -96 hours following methadone • Duration – 5 -10 days and more intense for short acting – Less severe but longer for methadone

How to Taper • Education on what it will look like– discomfort, anxiety, restlessness, nausea, sweating etc. • Speed depends on clinical circumstances– – slow taper (reduce dose by 10% every 2 weeks or even longer) – Rapid taper– can be done but will need additional med management for withdrawal • Clonidine- alpha 2 agonist can be used to help withdrawal

Learning Points Write down 3 new things you learned from this presentation. 1. 2. 3.


References Breitbart W, Chandler S, Eagle B, et al. An alternative algorithm for dosing transdermal fentanyl for cancer pain. Oncology 2000: 14: 695 -702. Davis, MP, Lasheen, W, Gamier, P. Practical guide to opioids and their complications in managing cancer pain. What oncologists need to know. Oncology. 2007; 21(10): 1229 -38. Jensen, MK et al. 10 -year follow-up of chronic non-malignant pain patients: opioid use, health related quality of life and health care utilization. Eur J Pain. 2006; 10(5): 423 -33. Jost, L, Roila, F. Management of cancer pain: ESMO clinical recommendations. Ann Oncol. 2009; 20 (suppl 4): iv 170 -iv 173. Management of Cancer Pain, Structured Abstract. January 2001. Agency for Healthcare Research and Quality, Rockville, MD. http: //www. ahrq. gov/clinic/tp/canpaintp. htm Mercadante, S. Arcuri E. Pharmacological management of cancer pain in the elderly. Drugs Aging. 2007: 24(9): 761 -76. Smith, HS. Opioid Metabolism. Mayo Clin Proc. 2009; 84(7): 613 -24. Stevens, RA, Ghazi, SM. Routes of opioid analgesic therapy in the management of cancer pain. Cancer Control. 2000; 7(2): 132 -41.
- Slides: 30