Palliative care for end stage respiratory disease Aileen






















- Slides: 23

Palliative care for end stage respiratory disease Aileen Mc. Cartney Senior Physiotherapist Wisdom Hospice, Rochester, Kent June 2007

Objectives To understand what palliative care and specialist palliative care is and what happens at the hospice v To identify common problems for people in their final year of life with end stage respiratory disease v To understand medical and physiotherapy management and treatment in the last year of life for people with end stage respiratory disease v To have a knowledge of management of people with end stage respiratory disease in the terminal phase v

Palliative care What is it? “An approach that improves quality of life of patients and their families facing the problems associated with life threatening illness, through the prevention and relief of suffering by means of early identification and impeccable assessment and treatment of pain and other problems, physical, psychoscocial and spiritual. ” WHO definition 2003 v Palliative care affirms life and regards dying as a normal process and intends neither to hasten or postpone death.

Palliative care It is provided by 2 distinct categories of health and social care professionals v Those providing day to day care to patients and their carers in their homes and in hospitals v Those who specialise in palliative care Everyone can provide palliative care with the right support It is not just for people in the very last days of life – therefore please don’t walk away if you hear they are for palliative care!

End stage respiratory disease What conditions? v COPD v Lung cancer v Mesothelioma When are they end stage? v Lung cancer and mesothelioma are generally aggressive conditions with low 1 year survival rate after diagnosis. v COPD patients are more difficult to predict as can have disease for many years with many relapses – identifying “end stage” very difficult

Lung Cancer Around 37000 new cases per year with a similar number of deaths (33465 in 2005) v One of lowest survival rates of all cancers, in England Wales around 25% of patients alive 1 year after diagnosis, dropping to 7% at 5 years v Cough, haemoptysis, dyspnoea and chest pain are common symptoms v

Mesothelioma Around 2000 new cases per year and almost always fatal, rates are due to peak between 2010 and 2015 v Estimated between 2006 and 2020 up to 30, 000 people will die from mesothelioma v Estimated around 1% of all males born between 1940 and 1950 will die of mesothelioma v Time between exposure to asbestos and development of disease is an average of 30 years v Medway has one of the highest mortality ratios in England v Poorly recognised disease in public v

Palliative care Potentially large population requiring palliative care for end stage respiratory disease v Not all these patients will require specialist palliative care, but palliative care is a right for all patients at the end of life v Relies on team work and education with other specialist teams/professionals v

Care in the final year of life

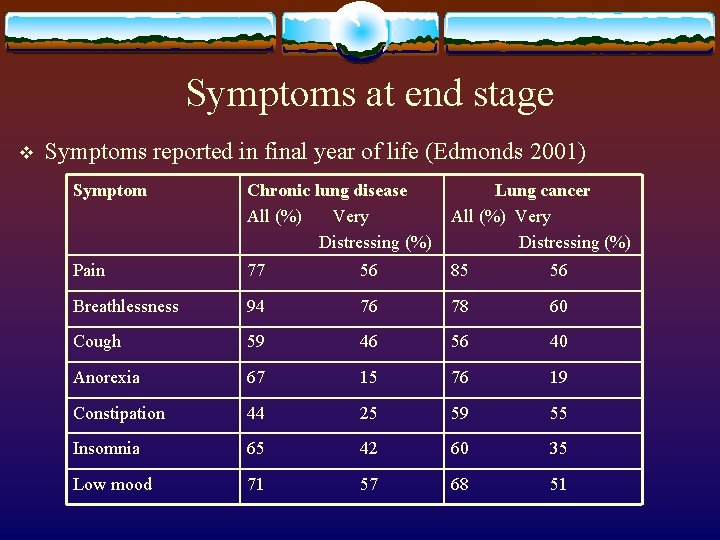
Symptoms at end stage v Symptoms reported in final year of life (Edmonds 2001) Symptom Chronic lung disease All (%) Very Distressing (%) Lung cancer All (%) Very Distressing (%) Pain 77 56 85 56 Breathlessness 94 76 78 60 Cough 59 46 56 40 Anorexia 67 15 76 19 Constipation 44 25 59 55 Insomnia 65 42 60 35 Low mood 71 57 68 51

Physiotherapy management of fatigue and reduced mobility Work closely with OT to provide equipment to ease ADL’s v Advice on pacing v Walking aid provision v Advice on gentle exercise and maintaining mobility and exercise tolerance v

Physiotherapy management of dyspnoea Education and reassurance v Breathing control v Diaphragmatic breathing v Secretion clearance if appropriate v Positioning advice v Pacing and fatigue management v Work with OT to help ADL’s v Relaxation v

Medical management of dyspnoea v v Assessment and diagnosis of cause of dyspnoea Treat reversible causes: • Infection (antibiotics) • Reversible bronchoconstriction (bronchodilators) • Pleural effusion (drainage, pleurodesis) • Anaemia (transfuse) • Cardiac failure (diuretics, ACE inhibitors etc) • Lymphangitis carcinomatosis (dexamethasone) • SVCO (dexamethasone, radiotherapy, stent)

Medical management of dyspnoea v v Opioids: • Reduce sensation of breathlessness • Improvements at doses that do not cause respiratory depression (important for COPD patients) • Starting dose: morphine 2. 5 mg PRN or increase by one increment if already on morphine for pain Benzodiazepines: • Helps manage fear and anxiety • E. g. lorazepam 500 micrograms – 2. 5 mg daily or diazepam 5 -10 mg daily • Sublingual lorazepam 0. 5 mg – 1 mg or oxazepam 10 mg – 20 mg PRN is useful in management of panic attack

Medical management of dyspnoea Oxygen – useful in some patients but there is no correlation with the degree of hypoxia. It has no role of saturation is normal. v Pareneteral medication – if patient unable to take oral medication, morphine or diamorphine and midazolam can be given. v

Physiotherapy management of retained secretions and cough ACBT v Airway clearance techniques including assisted cough where appropriate v Advice on hydration v Nebulisers v Advice on stopping smoking if patient wants to v

Medical management of respiratory secretions Nebulised saline v Refer to physiotherapist! v Fruit juice with mucolytic enzymes (pineapple, grape) v Anticholinergic medication generally not used at this earlier stage (occasionally in bulbar MND patients) v

Management in the last few days of life

Recognising the dying patient v v Treatable causes for deterioration have been excluded or refused or treatment deemed inappropriate/ineffective The multiprofessional team agree the patient is dying The following criteria may apply: • Patient is bedbound • Patient is semi-conscious • Patient is no longer able to take tablets • Patient is only able to take sips of fluid Commence the LCP for the dying. If any doubts or concerns please contact the HPCT

Respiratory secretions at the end of life v v v It is important to distinguish terminal secretions from conditions which may require alternative treatments e. g. ventricular failure or pneumonia General interventions: • Repositioning of the patient • Avoiding over hydration • Addressing family distress Drug treatment: • Drugs can reduce death rattle in up to 80% of patients • Treatment should commence when symptoms become apparent

Respiratory secretions at the end of life v v Glycopyrronium is the preferred drug because: • No central side effects • Potency and efficacy • Dose: 0. 2 mg – 0. 4 mg SC prn and 1. 2 mg – 2. 4 mg/ 24 hours by CSCI Other medications that can be used are: • Hyoscine butylbromide: 20 mg SC prn and 40 mg – 120 mg over 24 hours by CSCI • Hyoscine hydrobromide: 0. 4 mg SC prn and 1. 2 mg – 2. 4 mg over 24 hours by CSCI

Respiratory secretions at the end of life Other measures: Antibiotics (where infected secretions are distressing) Diuretics (where there is evidence of ventricular failure) Agents to reduce awareness of secretions e. g. midazolam Suctioning usually only has a role in severe cases v

Checklist for the dying patient v v v v v Assess medications and discontinue non-essentials Precribe prn SC medications: analgesia, anti-emetic, sedative and antimuscarinic. Consider commencing a syringe driver if more than one dose of these medications is required Discontinue inappropriate nursing interventions such as monitoring vital signs, replace with observations of symptom control. Ensure mouthcare and bowel and bladder care regimes are in place. Discontinue inappropriate medical interventions such as IV’s and blood tests Assess patients/familys insight into situation and give appropriate information Assess patients religious/spiritual needs Ensure DNAR forms completed Handover condition of the patient to the on call team